Bloating Abdominal Distention (BAD) is not OK!!
Suresh Kishanrao*
Karnataka State Rural Development & Panchayath Raj University (KSRDPRU), Rajiv Gandhi Institute of Public Health (RGIPH) and Indian Institute of Health Management and Research (IIHMR), India
Submission:October 28, 2021; Published:January 12, 2022
*Corresponding author: Suresh Kishanrao, Karnataka State Rural Development &Panchayath Raj University (KSRDPRU), GADAG, 582101 & Rajiv Gandhi Institute of Public Health (RGIPH) and Indian Institute of Health Management and Research (IIHMR) Bengaluru Karnataka, India
How to cite this article: Suresh K. Bloating Abdominal Distention (BAD) is not OK!!. Adv Res Gastroentero Hepatol, 2022; 18(2): 555985. DOI: 10.19080/ARGH.2022.18.555985.
Abstract
Abdominal bloating is a very common and troublesome symptom of all ages, but it has not been fully understood to date. Bloating is usually associated with functional gastrointestinal disorders or organic diseases, but it may also appear with no specific reasons. Studies have revealed that 15–30% of the general United States (US) population experiences bloating symptoms, compared with about 15% reported in an Asian population.
Tummy bloating every day, unless you have eaten too much or are menstruating, is not okay, and it amounts to a gut disorder. The pathophysiology of bloating remains ambiguous, although some evidence supports the potential mechanisms, like gut hypersensitivity, impaired gas handling, altered gut microbiota, and abnormal abdominal-phrenic reflexes have been put forth. No treatment is of unequivocally beneficial to all. Dietary intervention is important in relieving symptom in patients with bloating. Medical treatment with some prokinetics, rifaximin, lubiprostone and linaclotide could be considered in the treatment of bloating. In this manuscript I have tried to analyse 5 cases of abdominal bloating including autobiographical cases in the last 2 decades and their medical management. GI system pathological causes are kept out of the purview of this article.
Keywords: Gaseous distension of the stomach; Abdominal bloating; Irritable bowel syndrome; Food intolerance; Foods increasing or decreasing bloating and Probiotics
Introduction
Gas is the most common cause of bloating, especially after eating. Gas builds up in the digestive tract when undigested food gets broken down or when you swallow air. Everyone swallows air when they eat or drink. But some people can swallow more than others, especially if they are eating or drinking too fast in a hurry, chewing gum, smoking and those wearing loose dentures. A distended abdomen is measured by swollen tummy beyond its normal size. It’s often accompanied by the feeling of being bloated with trapped gas or digestive contents. General medical practitioners diagnose a distended abdomen in terms of the “five ‘f’s”: flatus (gas), foetus (pregnancy), faeces (trapped poop or constipation), fluid (from several causes) or fat. However, in this article I am discussing about abdominal distension from digestive processes only [1]. All of us have puffy tummies sometimes after having a heavy meal like chole Bhature or Puri, Holige (sweet rotis stuffed with cooked any pulses & jaggery), cheese burst pizza. If that feeling of discomfort becomes more routine in nature and pops up every time after we eat anything, we term it as being bloated. Most of us manage with bloating considering it a part of everyday life, but unless you have eaten way too much or are menstruating, you should not be okay with this gut disorder (Figure 1).
The major reasons for bloating are:
Abnormal gut microbiota
More than 500 different species of GI microbiota, most of them are obligate anaerobes, in adult play an important role in host immune system. Research over the past decades have shown that altered colonic flora were found in stool samples of patients with irritable bowel syndrome (IBS) that can be divided into 2
a) the luminal bacteria
b) the mucosa-associated bacteria
Luminal microbiotas form most of the GI tract flora and play a key role in bloating and flatulence through carbohydrate fermentation and gas production. The patients with IBS complain of bloating (case 2) have been reported to have increased gas production from bacterial fermentation caused by small intestinal bacterial overgrowth (SIBO).

Intestinal gas accumulation
A healthy GI tract contains only about 100 mL of gas distributed almost equally among 6 part of GI tract namely stomach, small intestine, ascending colon, transverse colon, descending colon, and pelvic colon. After a meal volume of gas increases by about 65%, in the pelvic colon. The excessive volume of intestinal gas has been proposed as the likely cause of bloating and distension. More recent studies using CT scans combined with imaging analysis have shown that excess gas was not associated with abdominal bloating, but impaired gas transit or distribution are the problem [2-4].
Altered gut motility and impaired gas handling
Many studies support ineffective anorectal evacuation as well as impaired gas handling as the possible mechanisms of abdominal distension and bloating [2-4].
Abnormal abdominal-diaphragmatic reflexes
The abdominal cavity is determined by the placement of the walls of abdominal cavity including diaphragm, vertebral column, and abdominal wall musculature. The patients with bloating have weak abdominal muscles. Intestinal gas load was associated with a significant increment in abdominal wall muscle activity in healthy subjects. Several modern studies using modern CT analysis with electromyography have demonstrated that abdomino-phrenic dyssynergia is one of main factors for abdominal distension and bloating. While in healthy adults, colonic gas infusion increases anterior wall tone and relaxes the diaphragm at the same time, but on the contrary, patients with bloating have shown diaphragmatic contraction and relaxation of the internal oblique muscle with the same gas load [2,3].
Visceral hypersensitivity
The autonomic nervous system contributes to modulation of the visceral sensitivity. It has been observed that visceral perception may be influenced by cognitive mechanism. Female patients with IBS (case 1) had worsening of abdominal pain and bloating during their peri-menstrual phase, at which time heightened rectal sensitivity contribute to bloating, taken together, altered sensory threshold combined with altered conscious perception may explain the mechanism of bloating.
Food intolerance and carbohydrate malabsorption
It is well recognized that dietary habits may be responsible for abdominal symptoms. Fiber overload has long been regarded as worsening factor of IBS symptoms through decreased small bowel motility or intraluminal bulking. Lactose intolerance also contributes to symptom development in IBS patients. In the small intestine, disaccharides are split by intestinal enzymes into monosaccharides which are then absorbed, and if this process is disturbed, the disaccharide reaches the colon, in turn is split by bacterial enzymes into short chain carbonic acids and gases, that malabsorption of lactose produces the symptom of bloating in patients with IBS. Additionally, highly fermentable but poorly absorbed short chain carbohydrates and polyols (FODMAPs- fermentable oligo-, di- and mono-saccharides and polyols) to the small intestine and colon that also contributes to the development of GI symptoms. FODMAPs are small molecules that induce relatively selective bacterial proliferation, especially of Bifidobacterium, that lead to expansion of bacterial populations in distal small intestine. The high FODMAP diet has demonstrated prolonged hydrogen production in the intestine, colonic distension by fermentation, increased colonic fluid delivery by osmotic load within the bowel lumen, and GI symptom generation [2-4].
Intraluminal contents
it has been observed that increased intra-abdominal bulk, not gaseous filling, might be a cause of abdominal bloating for example consumption of bran might give rise to symptoms such as bloating in IBS patients [3,4].
Hard stool/constipation
Many doctors have observed that most constipated patients complain of distension of the rectum by retained faeces that slows small intestinal transit as well as colonic transit, probably explaining the aggravated bloating in constipated patients. Constipation may accelerate bloating by intraluminal bulking effect in the same manner as bran [2-4].
Psychological aspects
Bloating is a frequent complaint of women with IBS. Patients with bloating reveal increased anxiety and depression, allowing the hypothesis that psychological distress may contribute to the perceived severity of bloating. It is unclear whether there is an actual relationship between bloating and psychosocial distress [4].
Gender and sex hormones
In a population-based studies in USA, UK and India, female gender was significantly associated with increased symptoms of bloating and distension in IBS. Some studies have indicated that bloating is one of the frequent symptoms of menstruation. The variation of reproductive hormones throughout the menstrual cycle and after the menopause may influence the gut motility and visceral perception Though the underlying mechanisms for these disparities remain to be determined, it seems to be possible that the hormonal fluctuation may contribute to bloating in female IBS patients [2,4].
Pathological medical conditions
Pathologic fluid accumulation in the abdominal cavity (ascites) because of cancer (e.g., ovarian cancer), liver disease, kidney failure, or congestive heart failure, celiac disease, or non-celiac gluten sensitivity, pancreatic insufficiency (unable to produce enough digestive enzymes), perforation of the GI tract with escape of gas, other contents into the abdominal cavity [4].
Medicines causing bloating
Some medicines like Aspirin, Antacids. Anti-Diarrheal medicines like Imodium, Kaopectate, Lomotil, Opioid pain medicines, Fiber supplements and bulking agents, such as Nutrova, ACTi fibre, Plant Protein, Great Gut, Glutamine and Multivitamins and iron pills may sometimes cause bloating [5].
Symptoms of Bloating
Common symptoms of bloating are stomach pain, discomfort, and gas and frequent gas passing. There may be frequent burping or belching and /or have abdominal rumbling or gurgling. Severe bloating may occur along with other serious symptoms, such as: Blood in your stool. Burping and flatulence are two ways swallowed air leaves the body. Delayed emptying of the stomach and gas accumulation can also cause bloating and abdominal distension [2,3].
Management of bloating
In most of the cases, the abdominal bloating can be managed by a few simple lifestyle changes:
a) First, check if you have food intolerance for any specific food, by item-by-item elimination process. Avoid or minimize consumption starting from avoiding dairy products like milk, butter milk, curds etc (lactose intolerance), whole-wheat bread (Gluten intolerance), lentils, bananas, onions, cabbage, cauliflower, and broccoli.
b) losing weight if you’re overweight.
c) Minimizing swallowing too much air by avoiding chewing gum, minimizing intake of carbonated drinks especially drinking fluids through a straw, alcohol, coffee etc.
d) Most importantly masticate well and eat slowly.
e) Probiotics help with repopulating healthy gut bacteria, simple curds or commercially available probiotics can be helpful
f) Staying hydrated helps in flushing out the toxins from the body which may be contributing to bloating. Detox water packed with antioxidants help cleansing all the toxins and helps improve metabolism, digestion, gut health, and promotes weight loss.
g) Magnesium rich diet- bloating often leads to constipation, a fiber and magnesium-rich diet can be effective in regularising your bowel movement. Green leafy vegetables that are rich in fiber and magnesium or take a natural supplement to meet daily magnesium needs [6].
Medications
In exceptional cases especially among women hormonal flux and mental health factors like stress, anxiety or depression secondary other medico-social causes have been blamed, and medicines like antibiotics, antispasmodics, or antidepressants may be required to treat [6] (Figure 2).
Material and Methods
Five case studies including an autobiographical case, review of literature and published articles on causes and management practices by home remedies, ISM approaches and allopathic medicines.
Case Studies
Bloating due to oral anti-diabetic drugs- Case 1
This is an autobiography. After having been diagnosed as Diabetic in a routine annual check-up in 1991, I was put on a combination of Glimepiride, Metformin and Glucobay (Acarbose). I was to take Amaryl 2 mg 30-45 minutes before, Glucobay 50 mg just before each meal and Metformin 500 mg after each meal. Within the first week I started getting flatulence and the endocrinologist said it is a known side effect of Glucobay and Amaryl drugs. The remedies suggested were to a) eat slowly masticating well, avoid eating cabbage, cauliflower, lentils especially Bengal grams, eat yoghurt 250 G /day and b) practice Yoga like Pavan Mukta Asana and Uthan Padasan and strengthen abdominal muscles. Over a period of 4- weeks the measure reduced the problem to a manageable level. Since 2018 after reading an Ayurvedic literature I am eating Papaya about 600 G (10 g/Kg body weight) for breakfast and 1 Banana (Yalakki-small variety) or boiled Sweet Potato and continued Yoga and muscle strengthening exercises. A little underripe Banana or boiled sweet potatoes high in potassium help in lining the stomach, flushing excessive sodium, and reducing inflammation and acts as a prebiotic increasing the good bacteria in the gut. Similarly, sweet potatoes are also high in potassium. For nearly a year now I have reduced my weight from 68 Kg to 59 Kg, reduced oral anti-diabetics especially stopped taking Glucobay, that have relieved my problem to almost Zero level.

Gluten intolerance- case 2
A distant relative of mine a young Engineering graduate of around 30 years working for an electronic organisation in Pune approached me in a social visit with complaints of abdominal distension and embarrassment when in official meetings for over 6 months. He had already tried the local physicians and undergone multiple investigations including scanning and Barium meal x-rays, with no relief. Taking a detailed history of his dietary practices over an hour’s time, interacting with his wife a software engineer and mother, I could narrow down that the discomfort of gas in abdomen and flatulence was associated with his eating whole wheat Pulkas (Indian homemade bread). I advised him to switch over to Jowar or Bajra roti’s for next 4 weeks instead of Chapatis / Pulkas. While he reported 50% relief at the end of a week, He was asked to try the Pulkas again and with no surprise his discomfort recurred. He reverted to non-wheat rotis, and it took him almost 4 weeks for complete relief. He continues with his diet and trying Pulkas 1-2 days a week with very little discomfort.
Irritable bowel syndrome- case 3
My younger sister a professionally busy spinster complained of pain in epigastric region of the abdomen, gaseous distension,flatulence, frequent episodes of diarrhoea and constipation and uneasiness starting in April 2020. The problem started after her retirement in 2018 from a remarkably busy schedule of heading a government Polytechnic after 30 odd years of services. Her work culture changed after retirement, and she got more leisurely time as she was unable to keep herself busy. Being a spinster lacked family support though she had shouldered our primary family back home. After multiple consultations in our home district in north Karnataka she landed in Bengaluru. After a thorough checkup by a popular and experienced Gastroenterologist and battery of investigations including, endoscopy, Colonoscopy, CT scan of abdomen and Pelvis, echocardiography, KFT, LFT, etc a final diagnosis of IBS was arrived. Endoscopy on 08/04/21, of Fundus and Body of stomach showed few polyps 5x5 mm, Gastric Polyps. Histopathology Features of the polyps were suggestive of benign fundic gland polyp with microcyst formation. Colonoscopy on 08/04/2021- showed Transverse colon incidental diverticula. She was put on i) Tab Nexpro 40 mg (Proton pump inhibitor) that reduces gastric acid secretion One tablet before food in the morning, 2. Tab Colospa Retard (for relief of pain and spasm)1 One tablet before food, iii). Tab Colospa X (an antispasmodic) 1 One tablet after food and iv) Tab Cyclopam (a combination drug Dicyclomine 20 mg and Paracetamol 500 mg) 1 SOS as needed. Having used these drugs for 3 months she is weaned of all drugs and is doing fine for 6 months.
Hormonal reflux -case 4
One of my post-graduate scholars of MPH, a girl of 24 years, nursing graduate admitted for master’s in public health (MPH) a first rank holder in the first year is suffering from Mitral Valve Prolapse (MVP) and Polycystic ovarian syndrome PCOS for over 3 years. She was put on cardiac drugs and hormones for PCOS since early 2021. She reduced her weight by 6 kg in 6 months of 2021 due to improper dietary practices (being a hostelite), mental pressure due to the worries of the consequences of MVP and PCOS and most importantly the pressure of expectation of good performance in the university final examination. She is suffering from heart burn (GERD-a spectrum of reflux diseases of the gastroesophageal junction) and flatulence for last 3 months. Oestrogen and Oestrogen receptor agonists are associated with an increased risk of gastroesophageal reflux disease symptoms among female as sex hormones can relax the lower oesophageal sphincter and increase the risk of gastroesophageal reflux symptoms. In this complex case we are not yet sure if it is the hormonal therapy or the mental stress of finding a job and other domestic problems that have exaggerated her co Figure edition. She is under treatment (basically antacids, Cyclopam and Destress tablets) for 6 weeks now and showing signs of improvement. In recent years, studies have reported have that estrogenic and its receptors serve an important role in the gastrointestinal (GI) tract and contribute to the progression of several GI diseases, including gastroesophageal reflux, peptic ulcers, gastric cancer, inflammatory bowel disease, irritable bowel syndrome.
Probiotics and lactose intolerance- case 5
Divya a newly married young lady of 25 years, had relocated to Bengaluru from a small town Harihar after marriage in early 2010. Both she a M.Sc. (Chemistry) working in a Probiotic manufacturing company and her husband a chartered accountant in a Bank were working couple. In one of couple’s weekend outing, after seeing a movie, to avoid hassles of cooking at home ate a Dosa each and an ice-cream. After reaching home both drank a big glass of milk (250 ml each) left un-used since morning. Sometime in the middle of night Divya got bloating and gaseous flatulence. However, her husband had no such problem ruling out the suspicion of food poisoning. Next day early morning, they consulted me and advised some antibiotics and anti-spasmodic that relived her symptoms. Next week they ate Cheese Pizza and faced similar but mild distension of the stomach and flatulence. However, next day morning she ate only small helping of rice and homemade curds with no consequence. She continued to consume curds regularly at home. Since she was working in a probiotic company, had access to probiotics free of cost, so, I advised her to consume the same on alternate days. After a moth she was asked to consume 30-50 ml of milk in coffee daily for about a week. In the following we she was given 100 ml of milk alone with no intolerance. In subsequent weeks I asked her to increase slowly the quantity of milk/icecream or Cheese pizza and confirmed that she was intolerant to milk more than 200 ml, second cup of ice-cream and more than a quarter of Cheese Pizza. Lactose intolerance is linked to the quantity of milk or ice cream she consumes. Now she limits her intake of these items with no recurrence of intolerance despite stopping commercial probiotics but consuming a cup of curds both in lunch and dinner.
Discussions
Abdominal bloating is suspected by symptoms of trapped gas, abdominal pressure, and fullness. It is defined as a measurable increase in abdominal girth. Abdominal bloating is a very common and troublesome symptom of all ages, yet to be understood fully. Bloating is usually associated with functional gastrointestinal disorders or organic diseases and can also occur with no specific pathology. Studies have revealed that 15–30% of the general United States (US) population experiences bloating symptoms, compared with about 15% reported in an Asian population.
In case of relative insufficient lactase activity in the small intestine, spill over into the colon will occur. In the colon it is fermented by the microbiota into glucose and galactose. Gasses such as hydrogen, methane and carbon dioxide are formed that cause bloating. There is evidence that probiotics can alleviate symptoms of lactose intolerance, by increased hydrolysis of lactose in the small intestine and by manipulation of the colonic metabolism. However, the precise mechanism how colonic metabolism influences lactose intolerance symptoms is not yet fully understood. There are some foods that reduce gassy emissions by helping to digest proteins, starches, and fats. Papaya, Banana, sweet potato containing Vitamin K are considered extremely effective in breaking down protein and help as in case 1 [7]. Other fruits like Pineapple containing digestive enzymes and Kiwi with laxative qualities and ability to increase gastric mobility have been used in AYUSH (traditional medicine) with success.
Gluten intolerance among people eating whole wheat bread is reported. Gluten is a protein naturally found in grains including Wheat, Barley and Rye. A study by Nizam’s Institute of Medical Sciences, in Hyderabad, India on the prevalence of gluten intolerance showed in 2014 showed that more than 10% of the general population suffers from the condition and if neglected may lead to intestinal cancer and heart disease. The finding was an offshoot of a diabetes research project screening 300 members of the weaver community for diabetes, hypertension, auto immunity and obesity [8]. An earlier inhouse study conducted in 2013 of 298 children and 318 adults with diabetes for gluten sensitivity showed 16% of the tested population tested positive for celiac sprue, that was presented in American Diabetes Association conference in Chicago in 2013. Our case no 2 falls in this category. Irritable bowel syndrome (IBS) is yet another condition commonly seen by gastroenterologist in India complaining of distensions, gas accumulation and flatulence to the extent of embarrassing them in meetings.as was our case no 3 [9] (Figure 3 & 4).
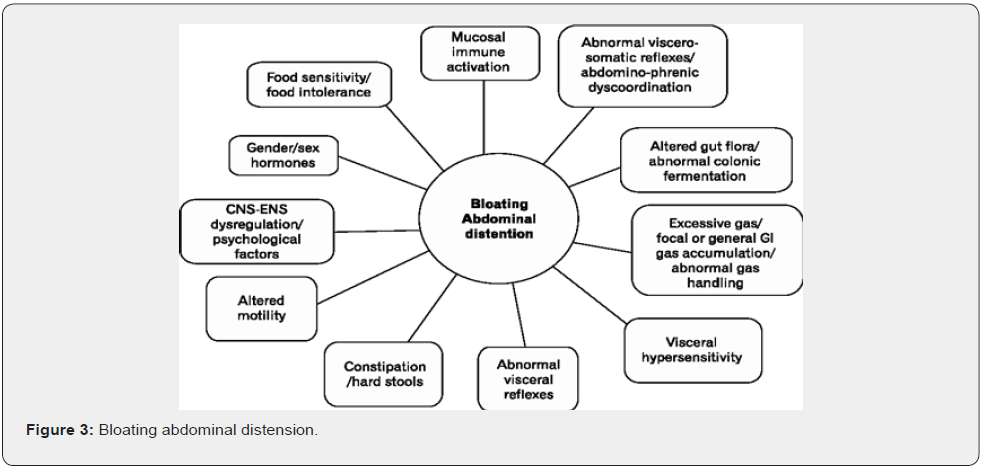
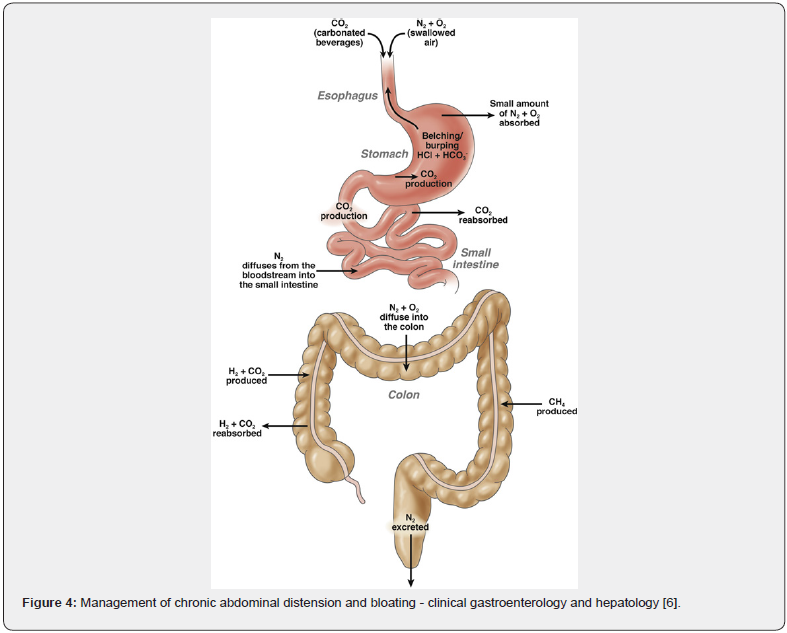
Milk has vitamin D, calcium, vitamin B2, vitamin B12, potassium and phosphorus and some vitamin A, vitamin B1, vitamin B6, zinc and magnesium. Almost, 60 to 65% of people in India are lactose intolerant, while 68% of the world’s population has lactose malabsorption. So many of them cannot digest lactose and can’t consume dairy product an important source of proteins and fats for vegetarian community [10]. A multicentered study in India to determine the incidence of lactose intolerance in healthy volunteers from different parts of the country indicated the incidence to be 66.6% in the subjects from two South Indian cities of Trivandrum and Pondicherry and in New Delhi significantly lower- 27.4% (P < 0.001). The lower incidence in the North Indian subjects is ascribed to their descendancy of the Aryans dairying for long and are known to be lactose tolerant [11]. Probiotics have been observed to be helpful in desensitizing people with lactose intolerance and so is the home-made curds as was seen in case no 5. Our case no 4 a rare condition of hormonal influx leading to bloating of abdomen is a complex case, yet to be resolved [12-14].
Conclusion
a) Ten to 25% of healthy persons experience bloating.
b) It is particularly common in persons with the irritable bowel syndrome and constipation.
c) Recent weight gain, weak or inappropriately relaxed abdominal muscles, an inappropriately contracted diaphragm and retained fluid in loops of distal small bowel are the reasons for gaseous distension of the abdomen
d) Gluten sensitivity, lactose intolerance and irritable bowel syndrome (IBS) are other common reasons in India for distended abdomen
e) No treatment is of unequivocally beneficial to all.
f) A low fermentable oligosaccharides, disaccharides, monosaccharides & polyols (FODMAPs) diet, probiotics and the non-absorbable antibiotic rifaximin offer some hope.
g) Treatment by Yoga, weight loss, abdominal exercise, prokinetics and girdles do benefit but need more study to establish the universal benefit.
References
- https://my.clevelandclinic.org/health/symptoms/21819.
- https://www.healthline.com/health.
- Young SA, Kim N, Oh DH (2013) Abdominal Bloating: Pathophysiology and Treatment. J Neurogastroenterol Motil 19(4): 433-453.
- Azpiroz F, Malagelada JR (2005) Abdominal Bloating. Gastroenterology 129(3):1060-1078.
- https://www.mottchildren.org.
- (2021) Simple remedies to reduce bloating, times of India e-paper. TOI Bangalore.
- Roel JV, Reckman GAR, Harmsen HJM, Priebe MG (2012) Probiotics and Lactose Intolerance.
- http://timesofindia.indiatimes.com/.
- K Suresh (2021) Irritable Bowel Syndrome-Running from Pillar to Post with No Cure. EC Gastroenterology and Digestive System 8: 27-33.
- https://timesofindia.indiatimes.com/life-style/health-fitness.
- Tandon RK, Joshi YK, Singh DS, Narendranathan M, Balakrishnan V, et al. (1981) Lactose intolerance in North and South Indians. American Journal of Clinical Nutrition 34(5): 943-946.
- Brian EL, Cangemi D, Roque MV (2021) Management of Chronic Abdominal Distension and Bloating. Clinical Gastroenterology and Hepatology 19(2): 219-231.
- https://www.hindustantimes.com.
- Sullivan SN (2012) Functional Abdominal Bloating with Distention. ISRN Gastroenterol.






























