Liver Hydatid Cyst with Rupture into Extrahepatic Right Hepatic Duct presenting as Obstructive Jaundice: A Case Report
Swamy P T1*, Jayendra Vagadia2, Jatin G Bhatt3 and Shailesh Gupta4
1Resident Doctor, Department of General Surgery, PDU Medical College and Hospital, India
2Assistant Professor, Department of General Surgery, PDU Medical College and Hospital, India
3Professor & Head, Department of General Surgery, PDU Medical College and Hospital, India
4Resident Doctor, Department of General Surgery, PDU Medical College and Hospital, India
Submission:December 01, 2021; Published:December 13, 2021
*Corresponding author: Swamy P T, Resident doctor, Department of General Surgery, PDU Medical College and Hospital, Rajkot, Gujrat, India
How to cite this article: Swamy P T, Jayendra V, Jatin G B, Shailesh G. Liver Hydatid Cyst with Rupture into Extrahepatic Right Hepatic Duct presenting as Obstructive Jaundice: A Case Report. Adv Res Gastroentero Hepatol, 2021; 18(2): 555982. DOI: 10.19080/ARGH.2021.18.555982.
Abstract
Introduction: Cystic hydatid disease is most commonly seen in liver, and it is associated with its own set of complications. Intrabiliary rupture of hydatid cyst is one of the common complications of liver hydatid disease which usually presents with jaundice. Here we bring to light a case of 62-year-old male patient of liver hydatid cyst disease having cyst rupture into extrahepatic right hepatic duct presenting as obstructive jaundice.
Keywords: Hydatid disease; Intrabiliary rupture; Jaundice; Choledochoduodenostomy
Abbreviations: ERCP: Endoscopic Retrograde Cholangiopancreatography; MRCP: Magnetic Resonance Cholangiopancreatography; CBD: Common Bile Duct; CHD: Common Hepatic Duct; CECT: Contrast Enhanced Computed Tomography
Introduction
Hydatid disease or echinococcosis is a zoonotic disease caused by tapeworm called echinococcus granuloses, with human being dead end host. It usually effects liver followed by lung, spleen, kidney, bone and the brain [1]. Liver hydatid disease is usually accompanied by complications like disseminated disease, severe anaphylactic disease, rupture into biliary tree or into peritoneum or into thorax depending on the location of the cyst and infection of the cyst lead to liver abscess. Treatment is advised for all the patients who are symptomatic and whose cyst are in risk of rupture or other complication.
Case Report
A 62-year-old male patient farmer by occupation presented to outpatient department of Department of General Surgery with complaints of abdominal pain for 1 month, weight loss in the last 1 month, fever in the past 10 days and non-bilious vomiting for 2 days. There was no history of breathlessness, changes in bowel habits. Patient is a non-diabetic, non-hypertensive with no positive medical or surgical history. On physical examination icterus (greenish yellow colour) was observed. There was mild tenderness over right hypochondrium with no palpable lump or organomegaly. Laboratory findings revealed increased total count (16,700 cells/cumm), raised total bilirubin (6.5 mg/dl) and direct bilirubin (5.2 mg/dl) suggesting obstructive type of jaundice, with elevated serum Alkaline phosphatase (631IU/L) and serum Alanine Aminotransferase (78 IU/L). All other blood investigations were normal. The ultrasound of abdomen showed large liver hydatid cyst with dilated Common Hepatic Duct with echogenic material within CBD lumen. CECT Abdomen suggested evidence of peripherally enhancing cystic lesion with internal daughter cysts involving subcapsular location of segment 7 of liver with patchy peripheral calcification and lesion was superiorly indenting into diaphragm and basal lung and compressing IVC & right atrium. Lesion measured 7.7*12.5*8.1 cm (AP*TR*CC) (Figure 1), with Similar lesion of size 4.4*4.4*3.9 cm (AP*TR*CC) located in segment 6 of liver. This lesion was causing compression over confluence of right and left hepatic duct with subsequent dilatation of bilobar IHBR (R>L), with focal defect in inferior wall of cyst with possible communication with right hepatic duct was seen (Figure 2). CHD (11mm) and CBD (15mm) are dilated upto lower end s/o distal CBD stricture. MRCP was done as CECT was inconclusive, it showed Two complex cystic area in right lobe of liver with communication between them as well as communication between lower cyst and right hepatic duct with presence of parasitic contains in biliary tree and moderate to severe asymmetric dilatation of biliary tree with benign distal CBD stricture with CBD diameter of 16mm. Patient was taken for open Deroofing of liver hydatid cyst with external drainage with cholecystectomy with choledochoduodenostomy in Right lateral decubitus position with right thoracoabdominal incision. On exploration bulge was seen posterior aspect of liver, hydatid cyst was confirmed by aspiration, Hydatid cyst deroofing done with drainage of 700cc fluid with debris. Cholecystectomy was done followed by location of CBD. A 2cm long longitudinal incision kept over CBD and cystic content were removed (Figure 3). Cystic wall was opening into Right Hepatic Duct just above confluence which was closed with PDS 3-0. Infant Feeding Tube passed from CBD through to hydatid cyst wall (Figure 4), 2 major Cystobiliary communication in medial wall of cyst were noted and closed with prolene 2-0. First part of duodenum located 2.5cm longitudinal incision kept choledochoduodenostomy performed with PDS 3-0. Omentopexy done into cyst cavity and drain was kept in cyst cavity, Cyst wall approximated with PDS 3-0. Post operative period was uneventful. Patient started orally on 2nd postoperative day with removal of Intercoastal drain. Patient discharged on post operative day 6 with normal laboratory reports.
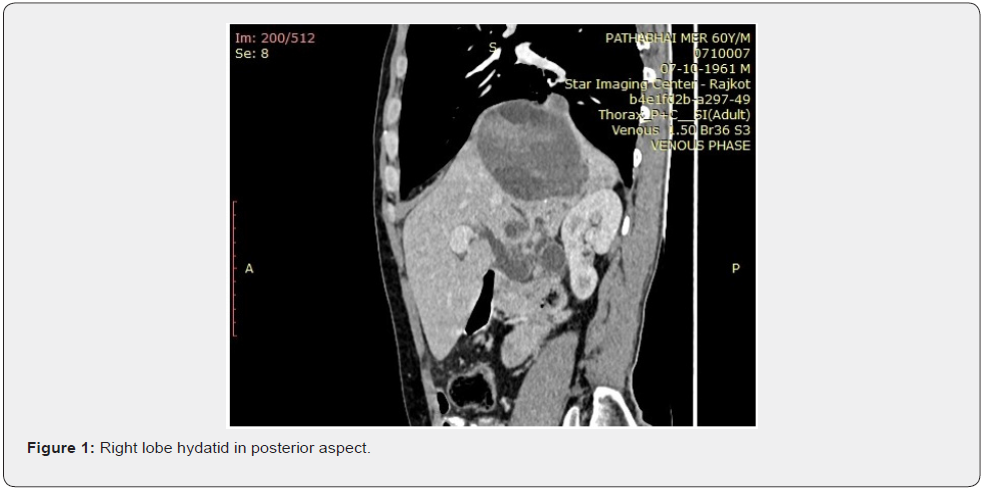
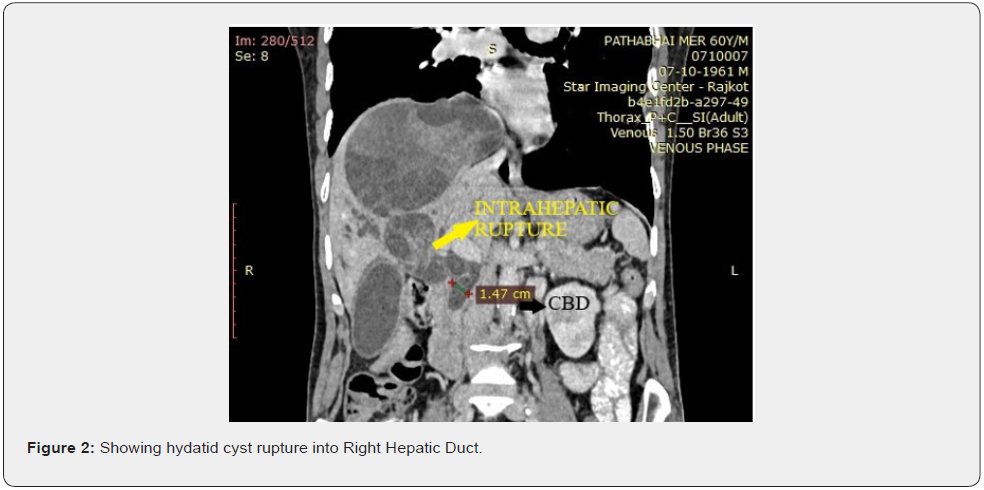


Discussion
Liver is the most obvious first site for hydatid cyst development, after organism enters bloodstream and passes into portal circulation. Hydatid cyst may present with various signs and symptoms depending on site of cyst location, most commonly in right lobe of the liver. Patient may complain from generalized upper abdominal pain or fever, jaundice due to cholangitis or intrabiliary rupture of cyst. Complications of hydatid cyst of the liver ranges upto 40% [2] of cases, most common complications include superadded infection of hydatid cyst, followed by intrabiliary rupture of hydatid cyst either in the form of occult rupture or frank rupture. In case of occult rupture, cyst fluid drains into biliary tree and in frank rupture there will be a overt passage of intracystic material into biliary tract. Incidence of intrabiliary rupture ranges from 3 to 17% [3,4]. The intrabiliary rupture of hydatid cyst leads to biliary complications such as cholangitis, hydatid biliary lithiasis or even obstructive jaundice. Diagnosis of intrabiliary rupture can be made with CECT or MRCP. The presence of dilated CBD, jaundice with cystic lesion of liver.
Other complication of hydatid cyst includes intrathoracic and intraperitoneal rupture. Some complications of the hydatid cyst of liver are very rare such as fistulisation of skin [5], can lead to portal hypertension either pre-hepatic, hepatic or post-hepatic, and in some cases may lead to vascular erosions. Diagnosing hydatid cyst of liver is very tricky, most of the cases goes unnoticed and some are incidentally noticed during investigation for other pathologies. Patients in some cases presents with complication of cyst. Surgery remains gold standard for management of liver hydatid cyst disease, aim of surgery is to inactivate the parasites in cyst and completely evacuate it, keeping in mind to avoid spillage, managing any Cystobiliary communications.
Endoscopic management is used commonly in intrabiliary rupture in the form of ERCP, it is used to clear out intrabiliary residual hydatid material [6]. In our case due to presence of large hydatid cyst an open approach was opted with thoracoabdominal incision, with clearance of biliary trunk from the residual hydatid material, Cystobiliary connections were closed with choledochoduodenostomy as CBD was dilated (15mm).
Conclusion
Intrabiliary rupture of liver hydatid cyst is one of the common complications, these intrabiliary ruptures occur in intrahepatic biliary radicles, sometimes cyst may rupture into extrahepatic biliary radicles. Prompt diagnosis and management is required for any intrabiliary rupture, but management varies from patient to patient and final judgment must always be made by taking into consideration of all imaging studies available.
References
- (2017) Blumgart's Surgery of the Liver, Biliary Tract, and Pancreas. In: Leslie H Blumgart, William R Jarnagin, Elsevier, pp. 1102-1121.
- Fethi Derbel, Mohamed Ben Mabrouk, Mehdi Ben Hadj Hamida, Jaafar Mazhoud, Sabri Youssef, et al. (2012) Hydatid Cysts of the Liver - Diagnosis, Complications and Treatment, Abdominal Surgery, Fethi Derbel, Intech Open.
- Zaouche A, Haouet K, Jouini M, El Hachaichi A, Dziri C (2001) Management of liver hydatid cysts with a large biliocystic fistula: multicenter retrospective study. Tunisian Surgical Association. World J Surg 25(1): 28-39.
- Eckert J, Deplazes P (2004) Biological, epidemiological, and clinical aspects of echinococcosis, A zoonosis of increasing concern. Clin Microbiol Rev 17(1): 107-135.
- Kehila M, Allègue M, Abdesslem M (1987) Spontaneous cutaneous-cystic-hepatic-bronchial fistula due to an hydatid cyst. Tunis Med 65(4): 267-270.
- Ozaslan E, Bayraktar Y (2002) Endoscopic therapy in the management of hepatobiliary hydatid disease. J Clin Gastroenterol 35(2): 160-174.






























