Platelet to White Cell Count Ratio (PWR) in Prediction of Mortality Among Patients with Acute on Chronic Liver Failure (ACLF)
Raja Taha Yaseen Khan*, Abbas Ali Tasneem, Syed Mudassir Laeeq, Hina Ismail, Husnain Ali Metlo, Kiran Bajaj, Nasir Hasan Luck and Muhammad Adeel
Department of Hepatogastroenterology, Sindh Institute of Urology and Transplantation, Pakistan
Submission:December 01, 2021; Published:December 09, 2021
*Corresponding author: Raja Taha Yaseen Khan, Department of Hepatogastroenterology, Sindh Institute of Urology and Transplantation, Pakistan
How to cite this article: Raja T Y K, Abbas Ali T, Syed Mudassir L, Hina I, Husnain Ali M, et al. Platelet to White Cell Count Ratio (PWR) in Prediction of Mortality Among Patients with Acute on Chronic Liver Failure (ACLF). Adv Res Gastroentero Hepatol, 2021; 18(2): 555981. DOI: 10.19080/ARGH.2021.18.555981.
Abstract
Introduction:Impaired inflammatory response and immune dysfunction increases the susceptibility to infections and can lead to the high mortality associated with ACLF. One of the hematological markers of systemic inflammatory response is platelet to white blood cell ratio (PWR) which not only heralds risk of infectious complications, but also predicts poor outcomes of patients. Patients with ACLF have a significantly higher white cell count and low platelet count. The aim of this study is therefore to use the platelet to white blood cell ratio (PWR) in predicting outcome of patients with acute on chronic liver failure (ACLF).
Methods: This was a cross-sectional retrospective study. Patients presenting with acute-on-chronic liver disease or failure with aged >12 years were included in the study. All patients with age greater than 12 years and presenting with acute-on-chronic liver failure were included in the study. Patients having decreased platelet count from any disease other than cirrhosis or any ongoing systemic infection that may affect the white blood cell (WBC) count were excluded. The patient’s baseline characteristics were recorded including the duration of stay in the hospital and the outcome in terms of mortality. These indices were then used to calculate the platelet to white blood cell count ratio (PWR). Area under ROC(AUROC) for PWR was derived and sensitivity, specificity, positive predictive value, negative predictive value and diagnostic accuracy was calculated.
Results: Total number of patients included in the study was 63. Among them, 41(65.1%) were males. Out of 63 patients, 26 (41.3%) patients expired due to complications of ACLF while 37 (58.7%) were discharged. The most common cause of chronic liver disease was HCV in 14 (22%) patients. The most common cause of acute insult was HEV, which was seen in 12 (15%) patients. The baseline characteristics showed mean White blood cell (WBC) count of 12.96±10.1 x 103/mm3 and platelet count of 134±94.11 x 103/mm3. The age, WBC count, serum creatinine and serum total bilirubin were significantly higher in the patients who died compared to the patients who survived; while, platelet counts were lower in the former. Platelet to WBC ratio (PWR) was calculated and value of ≤ 8, was found to be significantly associated with higher risk of mortality in patients with ACLF with p value of 0.005. Area under ROC of PWR was 0.7. At a cutoff of ≤ 8, the sensitivity, specificity, NPV and PPV were 81%, 50%, 81% and 50% respectively for PWR in predicting the risk of mortality among ACLF patients. The diagnostic accuracy of PWR in predicting mortality was 70.27%.
Conclusion: PWR has an excellent sensitivity in predicting mortality in ACLF. However, further studies are required to validate the score.
Keywords: Acute on Chronic Liver Failure; Platelet; White blood cell; Mortality
Abbreviations: PWR: Platelet to White Blood Cell Ratio; ACLF: Acute on Chronic Liver Failure; WBC: White Blood Cell; AUROC: Area Under ROC; CLD: CHRONIC LIVER DISEASE; MELD: Model for End-Stage Liver Disease; ERC: Ethical Review Committee; SD: Standard Deviation; Hb: Hemoglobin; CTP: Child Turcotte Pugh
Introduction
According to the APASL criteria, Acute-on-chronic liver failure (ACLF) is a critical clinical syndrome involving acute hepatic insult manifested as jaundice and coagulopathy, complicated within 4 weeks by ascites and/or encephalopathy in a patient with previously diagnosed or undiagnosed chronic liver disease [1-3]. One of the serious problems encountered in hospital setting in Pakistan is chronic Liver disease (CLD). Around the globe, millions of people are affected by chronic hepatitis. A number of etiological factors have been recognized to cause acute on chronic liver injury including hepatotropic viruses, alcohol, hepatotoxic drugs and ischemic hepatic injury. Among the causes of chronic liver injury, the most commonly encountered are viral hepatitis (hepatitis C and hepatitis B viruses) [4-10]. ACLF occurs in about 31% of hospitalized patients with cirrhosis who have an acute complication of their liver disease and have a short-term mortality of 50-90% [11,12]. Impaired inflammatory response and immune dysfunction increases the susceptibility to infections and can lead to the high mortality associated with ACLF [13,14].
The model for end-stage liver disease (MELD) score was developed to classify patients with cirrhosis awaiting transplantation according to the severity of their liver disease and is based on variables related to both liver and renal function. Increasing MELD score is reported to be associated with increasing severity of hepatic dysfunction and increased threemonth mortality risk in patients. However, the widely used MELD score does not take into account the inflammatory aspect of liver injury [10,15]. One of the hematological markers of systemic inflammatory response is platelet to white blood cell ratio (PWR) which not only heralds risk of infectious complications, but also predicts poor outcomes of patients. Patients with ACLF have a significantly higher white cell count and low platelet count [16,17]. PWR is a dependable gauge that can help differentiate between infectious etiology and normal response to splenectomy post abdominal trauma [18].
Significant amount of research work has been performed to evaluate PWR in predicting prognosis of patients suffering from various diseases. However, little work has been done in our country to use this relatively simple tool in predicting outcome of patients suffering from ACLF. The aim of this study is therefore to use the platelet to white blood cell ratio (PWR) in predicting outcome of patients with acute on chronic liver failure (ACLF).
Methodology
This cross-sectional study retrospective was conducted in the Department of Hepatogastroenterology, Sindh Institute of Urology and Transplantation, Karachi from January 2019 to June 2020. Patients presenting with acute-on-chronic liver disease or failure were admitted in the gastroenterology ward. Acute-onchronic liver failure (ACLF) was defined according to the Asian Pacific Association for the Study of Liver (APASL, 2019) as an acute hepatic insult manifesting as jaundice (total bilirubin >5mg/ dL) and coagulopathy (international normalized ratio >1.5), complicated within 4 weeks by ascites and/or encephalopathy in a patient with previously diagnosed or undiagnosed chronic liver disease [4]. Any acute insult over an already existing CLD but not meeting the above-mentioned criteria was labelled as acuteon- chronic liver disease (ACLD). All patients with age greater than 12 years and presenting with either acute-on-chronic liver disease or failure were included in the study. Patients having decreased platelet count from any disease other than cirrhosis or any ongoing systemic infection that may affect the white blood cell (WBC) count were excluded. The study was performed after approval from the ethical review committee (ERC) of the institution. Written informed consent was taken from all patients. A thorough history was taken and complete physical examination of all patients was performed, and the findings recorded in the structured proforma. All baseline investigations were performed, including blood complete picture, liver and renal function tests.
Ultrasound abdomen was done to identify the features of chronic liver disease. In order to identify the cause of the chronic liver disease, specific tests were done comprising viral serologies (hepatitis B surface antigen and anti-hepatitis C virus antibody); and where needed, autoimmune serology, metabolic profile, doppler ultrasound and CT scan of abdomen were performed. To identify the cause of acute hepatic insult, a history of prior use of any hepatotoxic agents was taken. Moreover, a number of tests were performed including hepatotropic viral serologies (hepatitis A and E, and where indicated hepatitis B, D and C), cytomegalovirus and herpes virus. The data has been taken from a study previously performed on patients with ACLF [5].
All the data was collected through a structured proforma and the data analysis was performed by using SPSS version 22. The patient’s baseline characteristics were recorded including the duration of stay in the hospital and the outcome in terms of mortality. These indices were then used to calculate the platelet to white blood cell count ratio (PWR). Results were presented as means ± standard deviation (SD) for quantitative data or as numbers with percentages for qualitative data. Continuous variables were analyzed using the t-test or the Mann Whitney test, while categorical variables were analyzed using the Chi-square or the Fisher exact test. A p value of <0.05 was considered as statistically significant.
Results
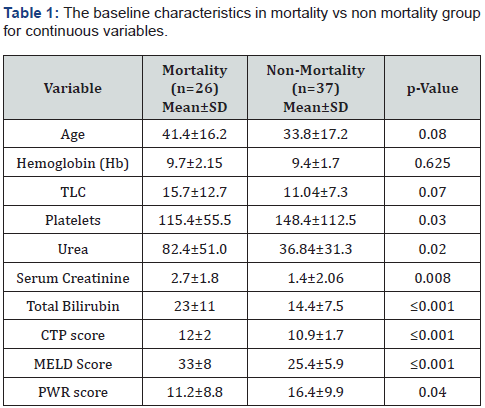
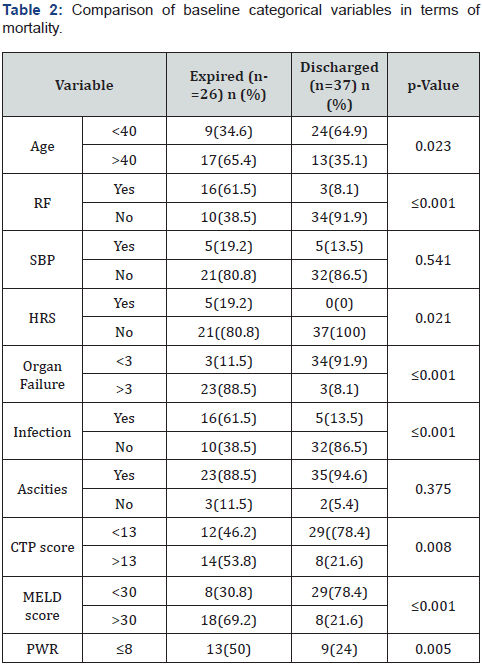
Total number of patients included in the study was 63, among which 41 were males and 22 were females. Mean age was 37.02±17.23 years. At the time of presentation, 37 patients had less than three organ failure while more than 3 organ failure was noticed in 27 patients. Out of 63 patients, 26 (41.3%) patients expired due to complications of ACLF while 37 (58.7%) were discharged. The most common cause of chronic liver disease was HCV in 14 (22%) patients while HBV was the second most common etiology seen in 12(19%) patients. The most common cause of acute insult was HEV, which was seen in 12(15%) patients. The baseline characteristics showed mean Hemoglobin (Hb) of 9.59±1.87 gm/dL; White blood cell (WBC) count of 12.96±10.1 x 103/mm3, platelet count of 134±94.11 x 103/mm3, INR of 2.2±0.7, serum creatinine of 1.9±2.01 mg/dL, total bilirubin of 17.9±10.0 mg/dL and serum albumin of 2.25±0.69gm/dL. The mean Child Turcotte Pugh (CTP) score was 11 and model for end stage liver disease (MELD) score of 28±7.86. The age, WBC count, serum creatinine and serum total bilirubin were significantly higher in the patients who died compared to the patients who survived; while, platelet counts were lower in the former (Table 1). Most of the patients who died had age greater than 40 years (p value 0.023). Hepatorenal syndrome was a frequent complication significantly associated with mortality along with infections, organ failure, advanced CTP and MELD score with p-value of (0.021), (≤0.001), (≤0.001), (0.008) and (≤0.001) respectively (Table 2). Platelet to WBC ratio (PWR) was calculated and value of ≤ 8, was found to be significantly associated with higher risk of mortality in patients with ACLF with p value of 0.005 (Table 3) (Figure 1 boxplot, 2 kaplan meier). Area under ROC of PWR was 0.7 (Figure 2 & 3 ROC). At a cutoff of ≤ 8, the sensitivity, specificity, NPV and PPV were 81%, 50%, 81% and 50% respectively for PWR in predicting the risk of mortality among ACLF patients. The diagnostic accuracy of PWR in predicting mortality was 70.27% (Table 3).

Discussion
PWR can be calculated bedside using complete blood count. Previously, it was done only in HBV patients, but in our study all etiologies leading to cirrhosis were included and HCV was found to be the most common cause of cirrhosis.16 In our study, PWR was higher in patients who were discharged compared to those who expired. PWR has been utilized previously in multiple studies to predict mortality. In one study, it has been used to predict 90-days mortality in patients with stroke and intravascular thrombolysis [19]. Multiple studies have revealed that PWR is lower in patients with ACLF and is also an independent predictor of mortality. The underlying mechanism is yet to be explained. However, the probability is that decrease platelet count is likely due to liver cirrhosis and secondly portal hypertension with hypersplenism may also lead to thrombocytopenia. The severity of liver disease has been linked inversely with decrease platelet count. On the other hand, high white blood cell count is secondary to infections which are the inciting factors leading to ACLF [16,17]. In our study, the patients who died were older with renal dysfunction, advanced bilirubin and high CTP and MELD and low PWR. Mortality was also increased in patients with more than three organ failure.
analysis of our data revealed that decreasing PWR values could serve as an important predictor of mortality in patients with ACLF. Previously available model such as model of end-stage liver disease (MELD) consists of both liver and renal confounding factors and is used for characterization and prioritization of the patients with liver disease awaiting liver transplant according to their disease severity. On the other hand, PWR is an excellent bedside tool based on only two markers, making it far more simple and easy to calculate than the MELD score. In previous studies, the combination of CTP, MELD, advanced age together with low PWR are found to be significantly associated with mortality [17]. While in our study, we reported that the combination of the PWR value together with the advanced MELD score, CTP and total bilirubin can predict 30day mortality in patients with ACLF. The prediction power of PWR (AUC = 0.71±0.054, 𝑝=0.01) was seen to be slightly higher than that of MELD score, Total bilirubin and CTP score (AUC = 0.68±0.074, 𝑝 =0.01), (0.7±0.064, 𝑝 =0.01) and (0.7±0.06, 𝑝 =0.01) in predicting 30-days mortality in patients with ACLF.
The major limitation of our study was the small sample size and limited specificity of PWR in predicting mortality in ACLF. However, the strength of the study is that it is the first study from this part of the world, particularly from Pakistan showing the role of PWR in predicting mortality in patients with ACLF. Secondly, we have included patients with all etiologies of cirrhosis and lastly, the excellent sensitivity of low PWR in ACLF.
Conclusion
PWR has an excellent sensitivity and in predicting mortality in ACLF. However, further studies comprising of large sample size are required to validate the score. And also studies showed be performed on larger scale to detect the accuracy of different scores in predicting mortality in ACLF.
References
- Shiv Kumar Sarin, Chandan Kumar Kedarisetty, Zaigham Abbas, Deepak Amarapurkar, Chhagan Bihari, et al. (2014) Acute-on chronic liver failure: consensus recommendations of the Asian Pacific Association for the Study of the Liver (APASL) 2014. Hepatol Int 8(4): 453-471.
- Shiv Kumar Sarin, Ashok Choudhury, Manoj K Sharma, Rakhi Maiwall, Mamun Al Mahtab, et al. (2019) Acute-on-chronic liver failure: consensus recommendations of the Asian Pacific Association for the study of the liver (APASL). Hepatol Int 3(1): 269-282.
- Sen S, William R, Jalan R (2002) The pathophysiological basis of acute-on-chronic liver failure. Liver 22(Suppl 2): 5-13.
- Memon MS, Zaki M (2013) Burden of chronic liver disease and liver transplantation in Sindh. J Liaquat Uni Med Health Sci 2: 1-2.
- Tasneem AA, Luck NH (2017) Acute-On-Chronic Liver Failure: Causes, Clinical Characteristics and Predictors of Mortality. J Coll Physicians Surg Pak 27(1): 8-12.
- Ullah F, Khan S, Afridi AK, Rahman SU (2012) Frequency of different causes of cirrhosis liver in local population. Gomal J Med Sci 10: 178-181
- Shan Yin, Shi Jin Wang, Wen Yi Gu, Yan Zhang, Liu Ying Chen, et al. (2017) Risk of different precipitating events for progressing to acute-on- chronic liver failure in HBV-related cirrhotic patients. J Dig Dis 18: 292-301.
- FM Lu, T Li, S Liu, H Zhuang (2010) Epidemiology and prevention of hepatitis B virus infection in China. Journal of Viral Hepatitis 17(1): 4-9.
- J Lu, A Xu, J Wang, Li Zhang, Lizhi Song, et al. (2013) Direct economic burden of hepatitis B virus related diseases: Evidence fromShandong, China, BMC Health Services Research 13(1): 37.
- Zhang F, Zhuge Y, Zou X, Zhang M, Peng C, et al. (2014) Different scoring systems in predicting survival in Chinese patients with liver cirrhosis undergoing transjugular intrahepatic portosystemic shunt. Eur J Gastroenterol Hepatol 26: 853-860.
- Moreau R, Arroyo V (2015) Acute-on-chronic liver failure: A new clinical entity. Clin Gastroenterol Hepatol 13: 836-841.
- Nava LEZ, Valadez JA, Chavez-Tapia NC, Torre A (2014) Acute-onchronic liver failure: A review. Ther Clin Risk Manag 10: 295-303.
- Malik R, Mookerjee RP, Jalan R (2009) Infection and inflammation in liver failure: Two sides of the same coin. J Hepatol 51(3): 426-429.
- Jalan R, Sen S, Williams R (2004) Prospects for extracorporeal liver support. Gut 53: 890-898.
- E Dionigi, M Garcovich, M Borzio, Gioacchino Leandro, Avik Majumdar, et al. (2017) Bacterial Infections Change Natural History of Cirrhosis Irrespective of Liver Disease Severity. Am J Gastroenterol 112(4): 588-596.
- Jie Y, Gong J, Xiao C, Zhu S, Zhou W, et al. (2018) Low Platelet to White Blood Cell Ratio Indicates Poor Prognosis for Acute-On-Chronic Liver Failure. Biomed Res Int 2018: 7394904.
- Liu LX, Zhang Y, Nie Y, Zhu X (2020) Assessing the Prediction Effect of Various Prognosis Model for 28-Day Mortality in Acute-on-Chronic Liver Failure Patients. Risk Manag Healthc Policy 13: 3155-3163.
- J Weng, CVR Brown, P Rhee, Ali Salim, Linda Chan, et al. (2005) White blood cell and platelet counts can be used to differentiate between infection and the normal response after splenectomy for trauma: Prospective validation. J Trauma 59(5): 1076-1080.
- Amalia L, Dalimonthe NZ (2020) Clinical significance of Platelet-to-White Blood Cell Ratio (PWR) and National Institute of Health Stroke Scale (NIHSS) in acute ischemic stroke. Heliyon 6(10): e05033.






























