Efficacy and Safety of Tenofovir Disoproxil Fumarate in Senegalese Patients with Chronic Hepatitis B
Murtaza Noor, Ashaq Parrey*, Mohd Ismail, Mir Sadaqat and Yasmeen Amin
Rheumatologist and Internal Medicine, Sher E Kashmir Institute of Medical Sciences Srinagar, India
Submission:November 19, 2021; Published:December 01, 2021
*Corresponding author: Ashaq Parrey, Rheumatologist and Internal Medicine, Sher E Kashmir Institute of Medical Sciences Srinagar, Srinagar, India
How to cite this article: Murtaza N, Ashaq P, Mohd I, Mir Sadaqat, Yasmeen A. Pancytopenia with Febrile Neutropenia: A Rare Presentation of Acute Viral Hepatitis A. Adv Res Gastroentero Hepatol, 2021; 18(1): 555979. DOI: 10.19080/ARGH.2021.18.555979.
Abstract
Viral Hepatitis A is a common viral infection causing a self-limited episode of acute hepatitis leading to fever, malaise, and jaundice, with rarely leading to severe illness and fulminant hepatic failure. Extra hepatic manifestations are seen in a minority involving mostly the haematological and renal systems. Some of these complications include glomerulonephritis, vasculitis, arthritis, rash, pancreatitis and haematological abnormalities like leukopenia with neutropenia, anaemia, thrombocytopenia, pure red cell aplasia, aplastic anaemia and rarely VAHS. Here we present a case of acute viral hepatitis A with pancytopenia, mild anaemia and mild thrombocytopenia, and profound neutropenia which caused febrile neutropenia.
Keywords: Hepatitis A; Leukopenia; Febrile neutropenia; Agranulocytosis
Introduction
Viral Hepatitis A is the most common cause of acute viral hepatitis worldwide. It is caused by a cytopathic single-stranded RNA virus and is transmitted by faeco oral route sometimes leading to community outbreaks. It usually presents as a self-limited episode of acute hepatitis with history of fever, malaise and jaundice, but can rarely have a prolonged or a relapsing course and occasionally lead to profound cholestasis. Extrahepatic manifestations are seen less frequently in a minority of patients including evanescent rash, arthralgias, and uncommonly leukocytoclastic vasculitis, glomerulonephritis, polyarteritis nodosa and pancreatitis. Haematological abnormalities include cryoglobulinemia, thrombocytopenia, aplastic anemia, red-cell aplasia and rarely a virus-associated hemophagocytic syndrome (VAHS).
Case Report
22 years unmarried female presented with two weeks’ history of low-grade fever and myalgia, nausea, loss of appetite and pain right upper abdomen with no past history of any jaundice, blood transfusion, or exposure to any drugs. On examination patient was haemodynamically stable (pulse 110/min, BP 110/70 Spo2 96%) febrile to touch, had muddy sclera, pallor, tender mild hepatomegaly and no other abnormal examination findings.
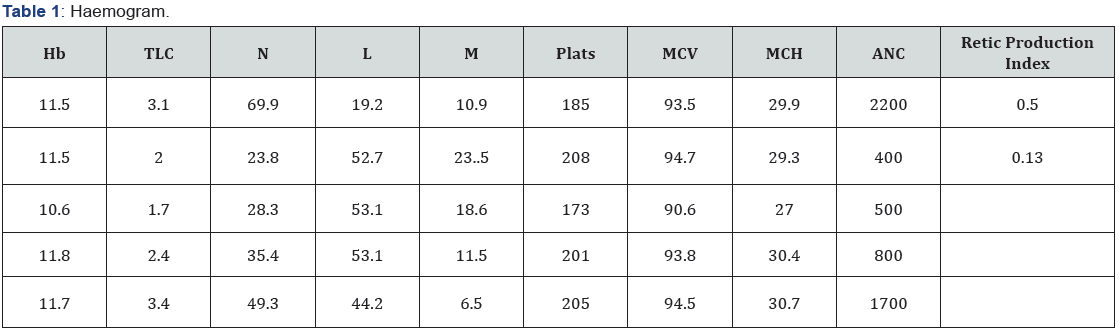
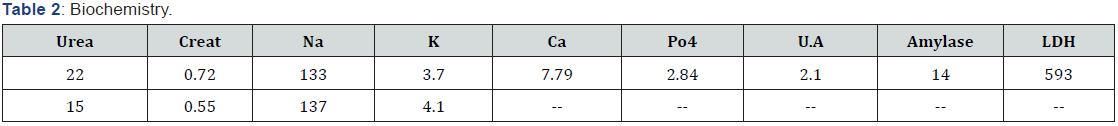
Laboratory investigations as followed over a week in the hospital are summarised as follows (Table 1-3):
a) Blood Cultures: sterile,
b) Initial Urine cultures: Sterile,
c) Widal Test: not significant
d) Brucella serology: Negative
e) Hepatitis B and C serology: Negative
f) Ig M Anti Hepatits A: POSITIVE (2.670)
g) Ig M Anti Hepatitis E: Negative (0.48).
h) Retroviral Serology: Negative
i) ICT/DCT: Negative
j) Serum ANA: Negative
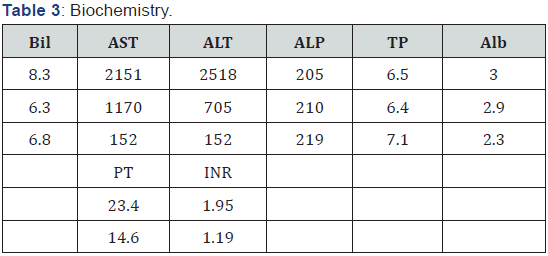
Laboratory evaluation revealed pancytopenia, low absolute neutrophil count and elevated LDH. Viral serology for acute Hepatitis A was positive, but hepatitis B, C, and E were negative. Peripheral blood smear revealed marked neutropenia and mild thrombocytopenia and mild anaemia with low corrected reticulocyte count and no abnormal cells or atypical lymphocytes. Liver function tests revealed hyperbilirubinemia, transminitis and hypoalbuminemia. Initial cultures were sterile at 24 hours. USG abdomen was suggestive of acute hepatitis. Over the next three days, patient was noticed to have jaundice and complained of passage of dark coloured urine, however she developed high grade fever and serial labs revealed a further drop in the ANC with urine culture showing Enterococcus species sensitive to Vancomycin and Linezolid.
She was managed as febrile neutropenia with iv antibiotics as per culture sensitivity, iv fluids antiemetic and thiamine for symptomatic treatment of underlying acute viral hepatitis A. There was gradual improvement in symptoms over the next 7 days with resolution of fever, and other symptoms. Labs also revealed significant improvement with near normalisation of the ANC, a decreasing trend of liver enzymes, serum bilirubin, and normalisation of coagulation profile, and was discharged after 2 weeks from the day of admission in a satisfactory condition. On follow-up over the next month, the patient became asymptomatic and the counts and liver functions have shown complete normalisation.
Discussion
Typically, viral hepatitis A is a self-limited illness with spontaneous recovery but rarely extrahepatic severe manifestations have been reported [1]. The most frequently affected extrahepatic systems affected have been found to be the haematological and the renal systems [2]. Among the haematological manifestations of acute hepatitis A leukopenia has been reported mainly in paediatric patients [3] and rarely in adults [4-6] with no reports of pancytopenia and febrile neutropenia.
In a study published by Akarsu et al. [7] haematological abnormalities were seen in nearly half of the cases with hepatitis A, with leukopenia in 0.9% of patients, neutropenia (ANC 1000- 1500) in 5.02%, anaemia in 15.52%, thrombocytopenia (<150000) in 4.10%. The likely mechanism [8] responsible for the cytopenias in acute viral illnesses has been proposed to be bone marrow suppression and peripheral immune mediated destruction of cell lines.
In Hepatitis A, bone marrow cell hypoplasia and agranulocytosis has been observed in the granulocyte parent cells [9]. Anaemia (autoimmune and AOCD) and thrombocytopenia have also been reported along with aplastic anaemia [10-13]. Aplastic anaemia and thrombocytopenia have been reported in three children with Hepatitis A [14]. In the study [7] quoted above, the haematological abnormalities in the patients with viral hepatitis A improved spontaneously without any specific treatment, and all values normalised in 6 days during which they were closely monitored for secondary infections.
Our case represents a case of acute viral hepatitis A which presented with pancytopenia and severe febrile neutropenia possibly secondary to bone marrow suppression caused by the virus leading to a hospital acquired urinary tract infection which was treated by appropriate antibiotic therapy as per culture sensitivity, after which there was resolution of the abnormally low neutrophil count and the other cell lines in the next week of hospital stay.
Conclusion
a) In conclusion, pancytopenia with moderate to severe neutropenia is a rare haematological manifestation of viral hepatitis A, caused by the bone marrow suppressing effects of the virus. It must be recognised promptly and the patient should be closely monitored for the development of secondary infections.
References
- Willner IR (1998) Serious Hepatitis A: An Analysis of Patients Hospitalized during an Urban Epidemic in the United States. Ann Intern Med 128(2): 111-114.
- Kuyucu N, Dökmen A, Yöney A, Teziç T (1998) Seroprevalence of hepatitis B infection in Turkish children. Infection 26(5): 317-318.
- Çetinkaya B, Tezer H, Özkaya Parlakay A, Revide Sayli T (2014) Evaluation of pediatric patients with hepatitis A. J Infect Dev Ctries 8(3): 326-330.
- Kivel RM (1961) Hematologic aspects of acute viral hepatitis. Am J Dig Dis 6(11): 1017-1031.
- Cunha BA, Teper RS, Raza M (2016) Fever in a traveler returning from the Amazon. Do not forget hepatitis A. ID Cases 4: 18-19.
- Gupta A, Jain P (2018). Leucopenia: A Rare Extrahepatic Manifestation of Acute Hepatitis A. J Clin Exp Hepatol 8(2): 215-216.
- Akarsu (2008) Hematological Abnormalities and Acute Viral Hepatitis A and B. J Pediatr Inf 3: 90-95.
- Rosenfeld SJ, Young NS (1991) Viruses and bone marrow failure. Blood Reviews 5(2): 71-77.
- Nishioka SD (1997) Aplastic anemia and viral hepatitis: A second look. Hepatology 26(6): 1688-1689.
- Al-Rashed SA, Al-Mugeiren MM, Al-Salloum AA, Al-Fawaz IM, Al-Sahaibani MO (1995) Acute viral hepatitis, glucose-6-phosphate dehydrogenase deficiency and prolonged acute renal failure: a case report. Ann Trop Pediatr 15: 255-257.
- Lin SM, Chu CM, Shih LY, Liaw YF (1991) Hematological abnormalities in acute viral hepatitis and acute hepatitis in HBsAg carrier]. Changgeng Yi Xue Za Zhi 14(4): 253-258.
- Smith D, Gribble TJ, Yeager AS, Greenberg HB, Purcell RH, et al. (1978) Spontaneous resolution of severe aplastic anemia associated with viral hepatitis A in a 6-year-old child. Am J Hematol 5(3): 247-252.
- Avci Z, Turul T, Catal F, Olgar S, Baykan A, et al. (2002) Thrombocytopenia and emperipolesis in a patient with hepatitis a infection. Pediatr Hematol Oncol 19: 67-70.
- Maiga MY, Oberti F, Rifflet H, Ifrah N, Cales P (1997) Hematologic manifestations related to hepatitis A virus. 3 cases. Gastroenterol Clin Biol 21: 327-330.






























