Invasive Klebsiella Pneumoniae Liver Abscess Syndrome. Analysis of Three Cases in Angola
Wilson Laffita Labañino1*, Márcio Teodoro da Costa Gaspar2, Cándido Satiro Abilio Luciano3, Lynda Dorene Galiano Cos4 and Maria das Neves Imaculada P Jardim5
1General Surgeon, Master of Emergency Medicine, Angola
2Department of Surgery, Head of Surgical Center, Angola
3Department of Surgery, Multiperfil Clinic, Angola
4General surgeon. Department of Surgery, Angola
5Department of Intensive Care, Multiperfil Clinic, Angola
Submission:October 13, 2021; Published:October 21, 2021
*Corresponding author:Wilson Laffita Labañino, General Surgeon, Master of Emergency Medicine, Medical and Surgical Department of Investigation in Angola, Multiperfil Clinic, 21 Janeiro, Morro Bento, Luanda, Angola
How to cite this article:Wilson L L, Márcio T d C G, Cándido S A L, Lynda D G C, Maria d N I P J. Invasive Klebsiella Pneumoniae Liver Abscess Syndrome. Analysis of Three Cases in Angola.Adv Res Gastroentero Hepatol, 2021; 17(5): 555975. DOI: 10.19080/ARGH.2021.17.555975.
Abstract
Liver abscess is a disease that is defined as collection bordered by a fibrotic capsule in the hepatic parenchyma and its frequency and etiology varies according to its geographic latitude. Klebsiella pneumoniae (Kp) was described for the first time in Taiwan in 1980 and it rapidly spread through the east Asia. Due to migration of people from those countries to all the continents today there are cases in Europe, North America, South America and Australia. There is an especially virulent Kp serotype that causes a syndrome with high mortality rate due to its extrahepatic complications known as Hypervirulent Invasive Klebsiella pneumoniae Syndrome (HIKPS). We describe three patients with HIKPS, there are no similar cases known in Angola but in the African continent cases were reported in South Africa, Nigeria and Morocco. The Hypervirulent Invasive Kp Syndrome is a reality in Angola, generally associated to cryptogenic origin and diabetic patients, and is characterized by bacteremia with metastatic infection and even with an adequate treatment, it has a high morbidity and mortality rate. Initially its diagnosis can go unnoticed so a high index of clinical suspicion for an early diagnosis and management is important.
Keywords: Liver abscess; Hypervirulent Klebsiella pneumoniae
Abbreviations: Ksp: Klebsiella Specie; CT: Computed Tomography; Kp: Klebsiella pneumoniae; ERCP: Endoscopic Retrograde Cholangiopancreatography; HIKPS: Hypervirulent Invasive Klebsiella pneumoniae Syndrome
Introduction
Liver abscess is a disease that is defined as collection bordered by a fibrotic capsule in the hepatic parenchyma and its frequency and etiology varies according to its geographic latitude [1-3]. Generally, they are classified into two groups, pyogenic and amebic, but there are other etiologies such as Mycobacterium tuberculosis [4,5], fungal and parasites [2]. The etiology of pyogenic liver abscess has changed in the last few years due to scientific and technical advancements and strong antibiotics; Intraabdominal infection (appendicitis, diverticulitis) via portal vein used to be the most common cause in the last century but nowadays it was replaced by biliary tract infection in the last decades of the twentieth century [1-5].
First world countries report as a primary cause the biliary tract instrumentation (ERCP), reconstructive biliary surgery, hepatic transplant, treatment of liver tumor, interventional radiology (chemoembolization) and radio ablation [1,5-8]. In Asia, the cryptogenic cause (apparently without etiological cause) is predominant, and in countries of Eastern Asia especially in Taiwan, the Klebsiella pneumoniae (Kp) substitutes the Escherichia Coli as the agent responsible of the formation of the pyogenic liver abscess in the last three decades [1-8]. Kp was described in Taiwan for the first time in 1980 and it rapidly spread through all east Asia reporting 23% in China, 52% in Hong Kong, 72% in South Korea [1]. As a result of the vast migration of people from those countries to all the continents, in nowadays series and isolated cases are reported in Europe, North America, South America and Australia [1-9].
There is a specific Kp virulent serotype that causes a syndrome with high mortality rate due to its extra-hepatic septic complications known as Hypervirulent Invasive liver Abscess Syndrome with bacteremia, metastatic infection, peculiar ultrasound and Computed Tomography (CT) findings that are associated to its cryptogenic cause and diabetic patients [1-10]. Three cases with the invasive liver abscess syndrome associated to Kp were reported in our institution, we don´t have knowledge of other similar cases reported in Angola but there were cases reported in other African countries such as South Africa [11], Nigeria [12] and Morocco [13].
The aim of the authors is to alert the medical community in the country and the rest of Africa about this dangerous syndrome responsible of high mortality rate.
Case Presentation
On table 1, described three patients with HIKPS, all Angolans, without travel background to Asian countries, all male between the ages of 39 and 65. Two of them were diabetic, the microbiological agent found was Klebsiella specie (Ksp), one of them was positive to Kp in the blood culture and pus culture collected from the liver abscess.
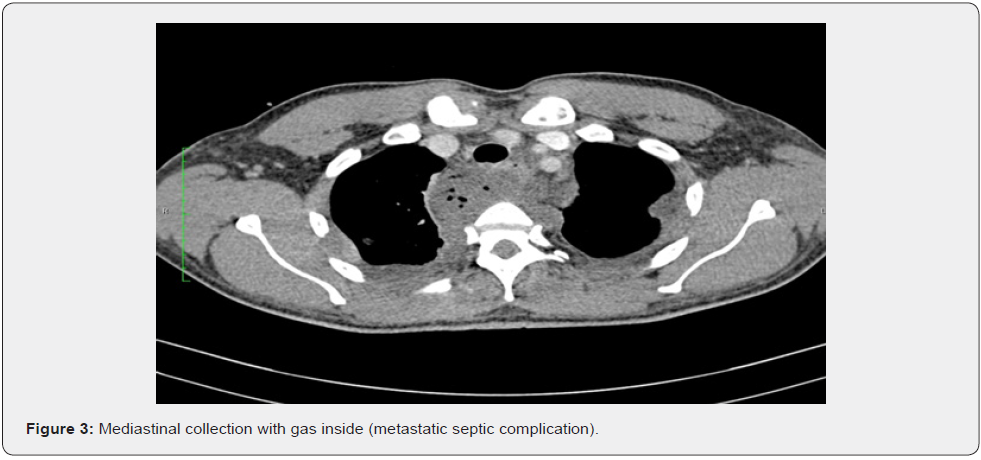
The three patients had clinically and radiologically the HIKPS, characterized by bacteremia, metastatic infection, peculiar ultrasound and tomography characteristics which are going to be explained next. From the imaging point of view (ultrasound and abdominal tomography with contrast): the wall or capsule were poorly demarcated, were single, multilocular and with presence of gas in all patients. We could also prove distant metastasis (tomography diagnosis) in the three patients, been the most frequents in the lung, mediastinum, muscle groups, bone and brain as well as the hepatic and portal vein thrombophlebitis. One patient presented septic pulmonary thromboembolism, there was not rupture of the abscess into the abdominal cavity. The therapeutic used was the ultrasound guided percutaneous drainage and there was the necessity to evolve to a laparotomy in two of them. All patients evolved to multiple organ failure that led to their death.
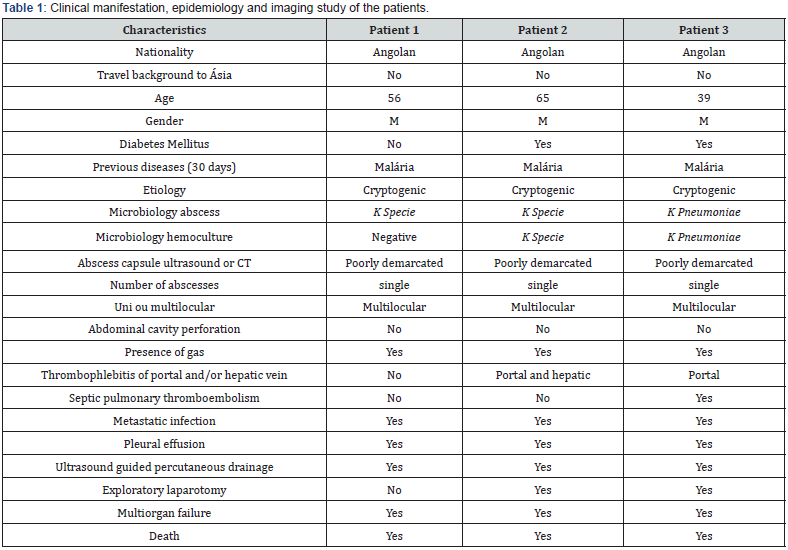
Source: Patients clinical history. Multiperfil Clinic. Luanda. Angola.
Discussion
Klebsiella pneumonia is a bacillar, Gram-negative bacteria, facultative anaerobic, non-motile and encapsulated, widely spread through the environment and it grows in mammals’ mucous surfaces; in human beings it colonizes the nasopharynx and the gastrointestinal tract [9]. Klebsiella pneumonia is responsible for the infections of a variety of systems such as respiratory, urinary and digestive, surgical site infections, cholangitis and peritonitis [14], generally associated to patients with medical history of alcohol abuse and diabetes [15].
In the majority of cases, pyogenic abscesses are polymicrobial and the Escherichia coli is the most frequent agent [16,17] and they respond well to a combined treatment of drainage with antibiotics. In the last century, mid ´80s, pyogenic liver abscesses caused by specific hypervirulent Klebsiella pneumoniae strains appeared as an important epidemiologic problem in East Asia and nowadays they constitute the cause of more than 80% of the pyogenic liver abscesses in Asia [17,18]. In the last decade, cases of hypervirulent Klebsiella pneumoniae pyogenic liver abscesses were notified in the whole world [1-18] regardless of its Asian origin like in the three patients described in our study in which all of them were Angolans without travel background to those endemic countries.
Typically, Kp pneumoniae is responsible for the severe cryptogenic liver abscesses frequently associated to uncommon distant septic metastatic locations: endophthalmitis, meningitis, myositis, osteomyelitis among others in immunocompetent hosts [16,19]. Several studies have been demonstrating that the invasive Kp strains infect the liver through the portal circulation starting from the bacterial translocation of the intestinal epithelium [14,18-20]. It is interesting to comment that the studied patients has as a past medical history malaria by falciparum 30 days before the liver abscess diagnosis and according to studies made in rats by Denny and cols [2], infection by plasmodium have different effects on the homeostasis of the intestinal microbiota that could contribute to a enteric bacteremia associated to malaria.
Diabetes mellitus is considered as a risk factor for Kp liver abscess and its complications, it is proposed that hyperglycemia interferes in the polymorphs leukocytes chemotaxis and therefore compromises the phagocytosis of the K1 and K2 encapsulated serotypes that are considered as hypervirulent strains [19] and it is related to a bad control of these patients glycemia as a possible cause of the metastatic septic complications [14,21].
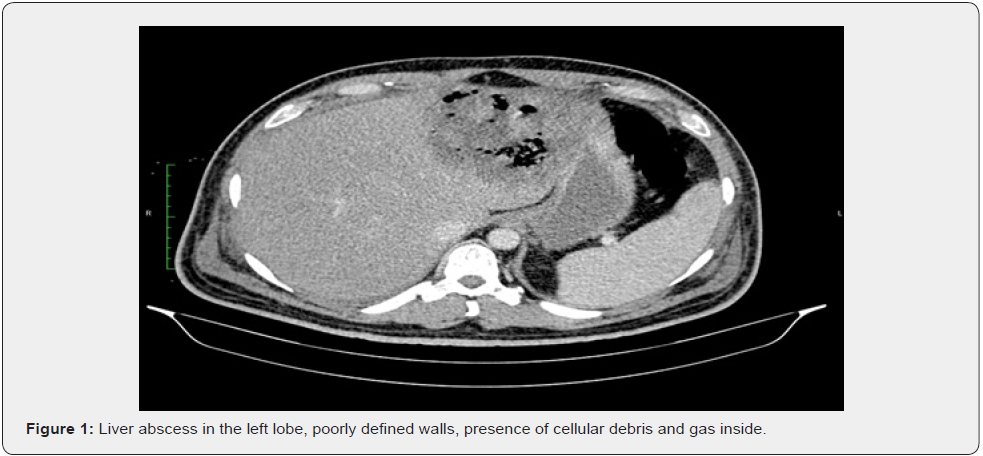
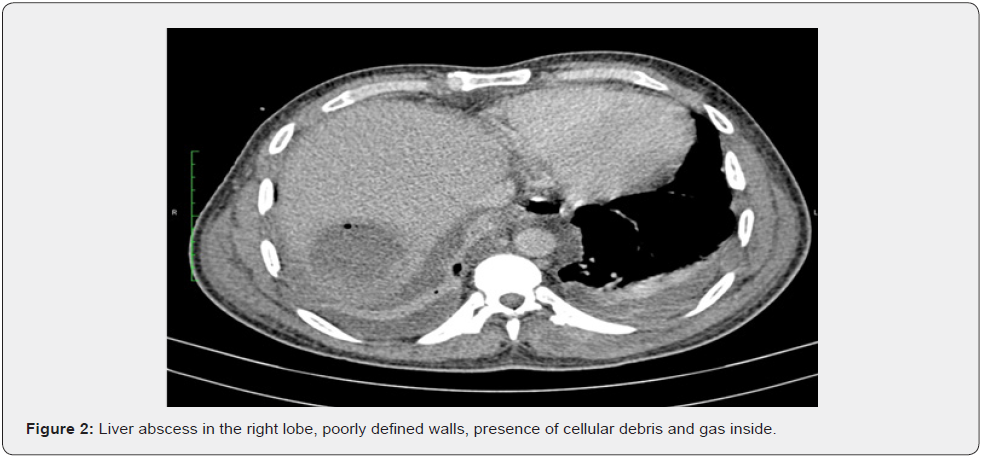
In relation to the etiology, Kp liver abscesses rarely have a biliary, portal, pos surgical, traumatic, or tumoral cause, generally they have a cryptogenic cause. Studies in animals suggests that Kp crosses the intestinal barrier and produces the liver abscess [18,22]. Although a pathognomonic image hasn´t been defined for the hypervirulent Kp liver abscess, they tend to present imaging characteristics of immaturity [6,23]. The Ultrasound shows solid masses with irregular or ill-defined margins with internal debris images and incomplete liquefaction [6,23].
The CT findings include thin walls or badly demarcated, septum ruptures, necrosed debris, presence of air that translates into a delay in the abscess maturity [6,23]. There is also described: single abscess, more solid than liquid, multilocular, with a high percentage of association to portal and hepatic vein thrombophlebitis [18,24,25]. Lee & cols [23] propose as a criteria to imaging diagnosis of Kp liver abscess, the presence of (1) thin walls, (2) necrosed debris, (3) metastatic infection and (4) absence of biliary pathology
According to their study in the Asian population, the presence of three criteria has 98% of specificity. All studied patients in this article had the Lee and cols criteria (Figure 1-3). Generally, it is suggested ultrasound guided percutaneous drainage as the gold standard treatment although this procedure might be jeopardized by a predominance of solid areas, abscess immaturity that could lead to its failure and complement it with surgery (laparotomy or laparoscopy) as it happened with two of the patients in this study. Hsieh & cols [26] suggest that an aggressive hepatic resection could have a better prognosis than a percutaneous drainage in those patients that are severely ill.
There is preference to third-generation cephalosporin, there can be also used ampicillin-sulbactam, aztreonam, and a quinolone [19]; though beta lactamase producer strains are not usual, in these cases the drug of election are the carbapenems.
The morbidity and mortality of the invasive Kp liver abscess syndrome is substantial, with a mortality between 35 and 42% [14-25]. Our study has several limitations as the sample is scarce, with limitations in isolating the Hypervirulent Kp (serotypes K1 and K2). Nevertheless, the hypervirulent invasive Kp liver abscess syndrome has a cryptogenic etiology, associated to diabetic patients, with characteristic imaging criteria (Lee criteria) with metastatic infections that were present in all three of the reported patients. Despite the appropriate treatment, including the abscess drainage percutaneous or surgical in combination with aggressive antibiotics, the result was not good. The metastatic septic complication that led to the septic shock and multiple organ failure contributed to its fatal outcome.
Conclusions
The invasive liver abscess syndrome secondary to Klebsiella pneumoniae is a reality in Angola usually associated to cryptogenic cause and diabetic patients. It is characterized by bacteremia with metastatic septic complications that even with an adequate treatment has a high morbimortality. Its diagnosis could initially go unnoticed so a high index of clinical suspicion for an early diagnosis and management is important.
Recommendations
a) It is important for the medical community not only in Angola but also in the rest of the African continent and the world to take into consideration this unusual and dangerous diagnosis in our daily practice due to the extra-hepatic complications that are generally fatal.
Microbiologists must be alert and know that a positive culture for Kp with hyper viscosity is highly suggestive of invasive Kp, same with radiologists when they write the medical reports of peculiar ultrasonography and tomography images (Lee criteria) they should immediately notify the medical doctors to consider the possibility of this syndrome.
References
- M G Mavilia, M Molina, G Y Wu (2016) The Evolving Nature of Hepatic Abscess: A Review. J Clin Transl Hepatol 4(2): 158-168.
- Yu Y, Guo L, Hu C, Chen K (2014) Spectral CT imaging in the differential diagnosis of necrotic hepatocellular carcinoma and hepatic abscess. Clin Radiol 69: 517-524.
- Lardière-Deguelte S, Ragot E, Armoun K, Piardi T, Dokmak S, et al. (2015) Hepatic abscess: diagnosis and management. J Visc Surg 152(4): 231-243.
- Bangaroo AK, Malhotra AS (2005) Isolated hepatic tuberculosis. J Ind Assoc Paediatr Surg 10(2): 105-107.
- Narwade N, Bagul A, Khan N, Murali S, Borude R (2018) What is the recent trend in the clinical study of liver abcess cases? Int Surg J 5(4): 1382-1387.
- Pinto E,Sousa M, Costa A (2013) Abcessos hepáticos piogénicos: a perspectiva do Radiologista de intervençã Rev Clin Hosp Prof Dr Fernando Fonseca 1(1): 27-33.
- Sharma A, Mukewar S, Mara KC, Dierkhising RA, Kamath PS, et al. (2018) Epidemiologic Factors, Clinical Presentation, Causes, and Outcomes of Liver Abscess: A 35-Year Olmsted County Study. Mayo Clin Proc Inn Qual Out 2(1): 16-25.
- Lu J, Zhu YH, Li ZT, Jia Z (2016) Pyogenic Liver Abscess after BileDuct Exploration Drained with Endoscopic Techniques. Surgery Curr Res 6: 277.
- Carrillo-Esper R, Díaz-Carrillo MA, Peña-Pérez C (2013) Síndrome de absceso hepático secundario a Klebsiella pneumoniae hipermucoviscosa. Una entidad emergente. Med Int Mex 29: 533-536.
- Pañella C, Flores-Pereyra D, Hernández-Martínez L, Burdío F, Grande L (2017) Absceso hepático primario por Klebsiella pneumoniae: una entidad en auge. Gastroenterol Hepatol 40: 525-527.
- Yu LV, Hansen DS, Ko WS, Sagnimeni A, Klugman KP (2007) Virulence Characteristics of Klebsiella and ClinicalManifestations of K. pneumoniae Bloodstream Infections. Emerg Infect Dis 13: 986-993.
- Bello F, Lawal Y, Bakari AG (2014) Community-acquiredprimary liver abscess due to klebsiella pneumoniae in a type 2 diabetic patient. Sub-Saharan Afr J Med 1: 104-107.
- Dédjan AH, Aziz Sel, Chadli A (2016) Liver Abscess in Diabetic Patients: A Case Series. Endocrinology, Diabetes & Metabolism 1) 1011: 1-4.
- Maheswaranathan M, Ngo T, Rockey DC (2018) Indentification and Management of the Hypervirulent Invasive Klepsiella Pneumoniae Syndrome: A unique and distinct clinical entity. Journal of investigative medicine high impact case report 6: 1- 4.
- Criales S, Lafleur A, Gervais P (2019) Liver Abscess Metastatic Syndrome Caused by Hypermucoviscous Klebsiella Pneumoniae in a Canadian Patient of Vietnamese Origin. Canadian journal of General Internal Medicine 14: 21-24.
- Brook I, Frazier EH (1998) Microbiology of liver and spleen abscesses. J Med Microbiol 47: 1075-080.
- Rossi B, Gasperini LM, Leflon-Guibout V, Gioanni A, Lastours V, et al. (2018) Hypervirulent Klebsiella pneumoniae in Cryptogenic Liver Abscesses, Paris, France. Emerging Infectious Diseases 2: 221-229.
- Jum JB (2018) Klepsiella pneumoniae Liver Abscess. Infect Chemother. 50(3): 210-218.
- Neto OCLF, Martins CLO, Lora KJB, Lacerda CM (2014) Abscesso hepático por Klebsiella pneumoniae e suas complicações sisté Gastoenterol endosc dig 33(2): 66-69.
- Denny JE, Powers JB, Castro HF, Zhang J, Joshi-Barve S, et al. (2019) Differential Sensitivity to Plasmodium yoelii Infection in C57BL/6 Mice Impacts Gut-Liver Axis Homeostasis. Cientific Reports 9: 3472.
- Siu LK, Yeh KM, Lin JC, Fung CP, Chang FY (2012) Klebsiella pneumoniae liver abscess: a new invasive syndrome. Lancet Infect dis 12(11): 881-887.
- Tu YC, Lu MC, Chiang MK, Huang SP, Peng HL, et al. (2009) Genetic requirements for Klebsiella pneumoniae induced liver abscess in na oral infection model. Infec Inmun 77: 2657-2671.
- Lee NK, Kim S, Lee JW, Jeong YJ, Lee SH, et al. (2011) CT differentiation of pyogenic liver abscesses caused by Klebsiella pneumoniae vs non-Klebsiella pneumoniae. Br J Radiol 84(1002): 518-525.
- Alsaif HS, Venkatesh SK, Chan DS, Archuleta S (2011) CT appearance of pyogenic abcesses caused by Klebsiella Pneumoniae. Radiology 260(1): 129-138.
- Maffiolo C, Novellas S, Chevallier P, Brunner P, Mourou MY, et al. (2006) Trombophlebitis of the hepatic veins: complication of a Klebsiella liver abscess. Clin Imaging 30: 63-65.
- Hsieh HF, Chen TW, Yu CY, Wang NC, Chu HC, et al. (2008) Agressive hepatic resection for patient with pyogenic liver abcess and APACHE II score ≥ or = 15. Am J Surg 196: 346-350.






























