An Unexpected Cause of Obstructive Jaundice
Oliver DWIDAR1, Michelle GRÄMIGER2,Jeremy MEYER3,Galab M HASSAN4*and Eleftherios GIALAMAS1
1Division of General Surgery, Department of Surgery, Pourtales Neuchatel Hospital, Switzerland
2Division of Urology, Department of Surgery, Pourtales Neuchatel Hospital, Neuchatel, Switzerland
3Division of Digestive Surgery, University Hospital of Geneva, Geneva, Switzerland
4Division of Gastroenterology, Department of Medicine, Neuchatel Hospital, Neuchatel, Switzerland
Submission:September 04, 2021; Published:October 20, 2021
*Corresponding author:Galab M. Hassan, Chief of Gastroenterology Division, Department of Medicine Réseau Hospitalier Neuchâtelois, 2000 Maladiére, Switzerland
How to cite this article:DWIDAR O, GRÄMIGER M, MEYER J, HASSAN GM, GIALAMAS E. An Unexpected Cause of Obstructive Jaundice.Adv Res Gastroentero Hepatol, 2021; 17(5): 555974. DOI: 10.19080/ARGH.2021.17.555974.
Keywords: Liver function; Computed tomography; Duodenal; Choledocho-duodenostomy
Case Report
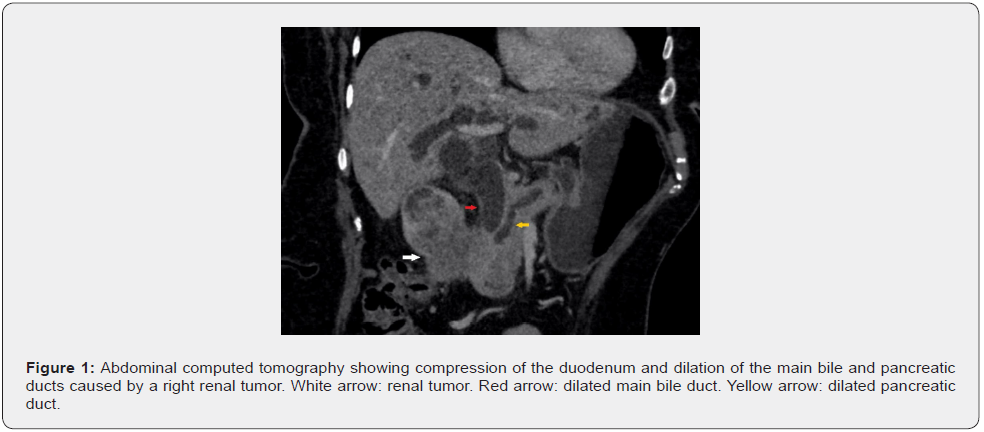
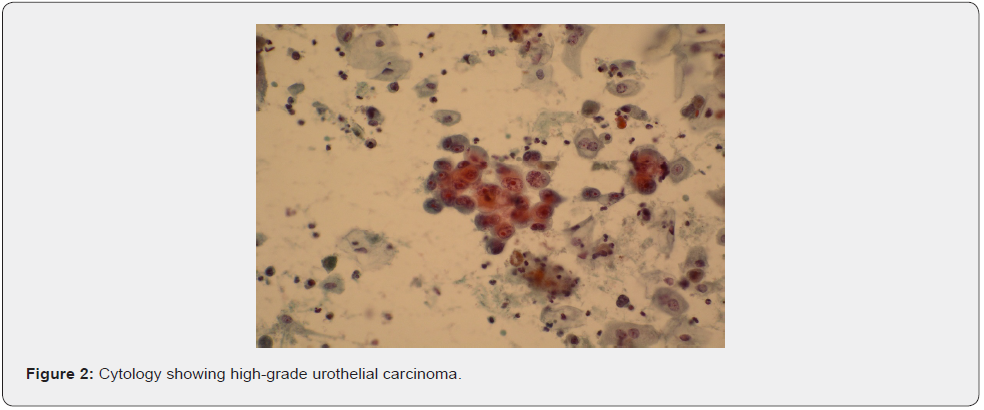
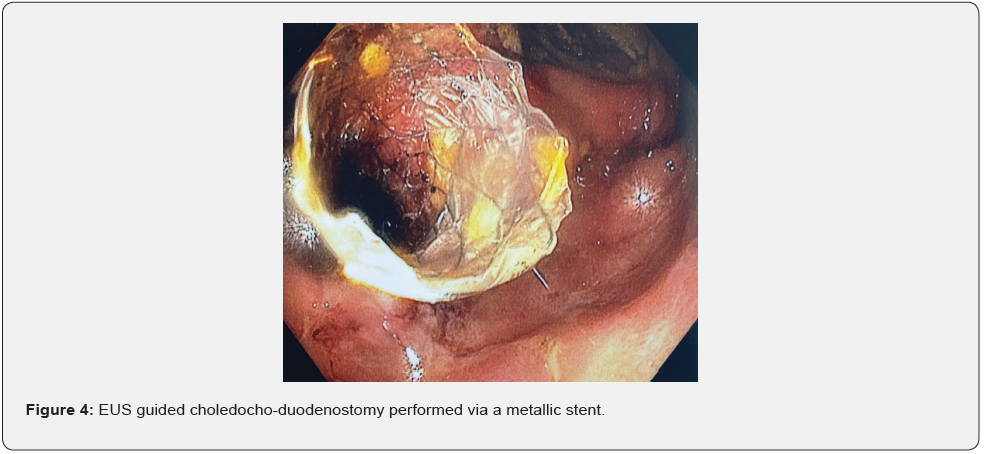
An 82-year-old healthy woman presented to the emergency department with epigastric pain, recurrent vomiting and jaundice since one week. On physical examination, she had epigastric tenderness and muco-cutaneous jaundice. Laboratory studies revealed abnormal liver function tests (alkaline phosphatase 1216 U/l, γ-glutamyl transpeptidase 1098 U/l, total bilirubin 12.4 mg/dl, conjugated bilirubin 9 mg/dl) with normal white-cell count. Computed tomography showed extrinsic compression of the duodenum (D2 part) and dilation of the main bile and pancreatic ducts caused by a right renal tumor of 6x5x8 cm (Figure 1). The tumor was invading both the renal artery and vein. Histologic examination after endoscopic ultrasound (EUS) guided fine-needle renal tumor biopsy revealed a high-grade urothelial carcinoma (Figure 2). EUS followed by endoscopic retrograde cholangio-pancreatography (ERCP) was attempted but could not be performed due to tumor infiltration (duodenal obstruction), which limited access to the bile duct (Figure 3). Endoscopic placement of a duodenal SEMS stent (12cm length/22mm diameter), followed by an EUS guided choledocho-duodenostomy via a self-expandable metallic stent (SEMS, 6cm length/10mm diameter) were therefore performed (Figure 4), resulting in improvement of jaundice and vomiting. Due to advanced age, stage of the tumor and decision of the patient, no additional treatment was undertaken. The patient passed away two months after diagnosis.
Obstructive jaundice results mostly from pancreatico-biliary tumors but can rarely have extra-digestive origins that should be considered in the differential diagnosis. Herein, we described the first case of a renal carcinoma causing extrinsic compression of the duodenum and the main bile duct. In the literature, metastatic renal cell carcinoma to the pancreas or to the ampulla of Vater has been described causing obstructive jaundice but remains a rare entity [1-5]. Treatment of this type of tumor requires extensive surgical resection which might be, in some cases, not feasible due to patients’ comorbidities and tumor extension. In such cases, palliative care should be considered either by endoscopic treatment or by interventional radiology. EUS guided choledocho-duodenostomy can be a useful alternative to percutaneous transhepatic biliary drainage in some selected cases of failed ERCP drainage for palliative care of obstructive jaundice of tumoral origin.
Contribution Details
a) All authors contributed equally to the manuscript preparation, editing and review, as well as literature search and image preparation. Conception of the article and overall integrity is guaranteed by Eleftherios Gialamas.
b) The manuscript has been read and approved by all the authors, the requirements for authorship as stated earlier have been met and each author believes that the manuscript represents honest work.
Protection of Patients’ Rights to Privacy
All identifiable information for patient’s identity was covered. Written consent form has already been obtained by the patient’s family for publication of the images and the manuscript and is available, if required, in French language.

References
- Shin TJ, Song C, Jeong CW, Cheol Kwak, Seongil Seo, et al. Metastatic renal cell carcinoma to the pancreas: Clinical features and treatment outcome. J Surg Oncol 123(1): 204-213.
- Ghavamian R, Klein KA, Stephens DH, T J Welch, A J LeRoy, et al. (2000) Renal cell carcinoma metastatic to the pancreas: Clinical and radiological features. Mayo Clin Proc 75(6): 581-585.
- Chambers M, Krall K, Hébert-Magee S (2017) Falling under the umbrella cells: A single institutional experience and literature review of urothelial carcinoma presenting as a primary pancreatic mass on endoscopic ultrasound-guided fine-needle aspiration. Cytojournal. 14(1).
- Haidong W, Jianwei W, Guizhong L, Ning L, Feng H, et al. (2014) Ampullary tumor caused by metastatic renal cell carcinoma and literature review. Urol J 11(2): 1504-1507.
- Karakatsanis A, Vezakis A, Fragulidis G, Staikou C, Carvounis EE, et al. (2013) Obstructive jaundice due to ampullary metastasis of renal cell carcinoma. World J Surg Oncol.






























