Endoscopic Treatment and Literature Review of Delayed Perforation After Colorectal Polypectomy: A Case Report
Tai-Yun Zhao, Xing-Jun Lu and Yin Wang
Department of Gastroenterology, The People’s Hospital of Bozhou, Bozhou City, Anhui Province, China
Submission:May 02, 2021; Published:May 18, 2021
*Corresponding author: Yin Wang, Department of Gastroenterology, The People’s Hospital of Bozhou, Bozhou 236800, Anhui Province, China
How to cite this article: Tai-Yun Z, Xing-Jun L and Yin W. Endoscopic Treatment and Literature Review of Delayed Perforation After Colorectal Polypectomy: A Case Report. Adv Res Gastroentero Hepatol, 2021; 17(1): 555952. DOI: 10.19080/ARGH.2021.17.555952.
Abstract
In this report, one patient developed abdominal pain in 24 hours after resection of multiple colonic polyps, and relieved after the application of symptomatic treatment. However, the patient had abdominal pain with fever and abdominal muscular tension within 40 hours. Perforation was considered in the patient based on the results of abdominal CT. Following painless colonoscopy, the patient was provided with endoscopic closure of the perforation successfully. Postoperatively, the patient was supplied with fasting of oral feeding and drinking water, anti-infectious therapy and other symptomatic therapies. The patient was discharged from the hospital successfully without the performance of surgery.
Keywords: Resection of intestinal polyps; Perforation; Endoscopic treatment
Case Report
A 51-year-old male married patient was admitted to the hospital at 11:16 on April 23, 2020. Over 10 months ago, the patient underwent colonoscopy in other hospital with the discovery of >10 polyps of 0.4-0.8cm in transverse colon, descending colon and sigmoid colon, most of which were flat in shape with relatively wider base. At present, the patient visited our hospital for further endoscopic polypectomy. During the course of the disease, the patient had no discomfort, good mental condition, no abnormality in appetite, urine and stool, and no significant change in weight. Besides, the patient reported no special medical history.
Personal history
The patient had a history of drinking, with an average of 48g per day and a history of drinking for about 30 years.
Physical examination
No obvious positive signs were found in the patient.
Preoperative laboratory examination
No obvious abnormality in routine blood test, hemagglutination test, four items of virus checking, liver and kidney function tests, and electrolyte test, with normal electrocardiogram,
Colonoscopy
There was a poor bowel preparation, with a large amount of fecal residue and yellow fecal water, which seriously affects the visual field. From the anal border to the sigmoid colon, 11 polyps can be detected, about 0.4 - 0.8cm in size. Following repeated irrigation of the intestine, the larger polyps were given submucosal injection of Meilan Glycerol Fructose and Sodium Chloride Injection at the root of the polyps, showing positive lifting sign, which were then excised by using high-frequency electrocoagulation with snare. In addition, small polyps were treated with high-frequency electric excision with hot biopsy forceps. The wound was clean in surface and white in color postoperatively, with no residual and active bleeding.
Diagnosis
Resection of multiple colonic polyps. The patient returned to the ward safely at 08:30 on April 24. The first day after operation: At 07:30 in the morning, the patient had sub-xiphoid pain and tenderness immediately after taking food by himself, with no rebound pain or abdominal muscular tension. The possibility of pain caused by ulcer required to be clarified considering the long-term drinking history and previous history of duodenal ulcer in the patient. Treatment: The patient was given intravenous injection of imported omeprazole (40mg), with improved abdominal pain 10mins later. At 20:12, the patient felt fever and shivering, with a temperature of 39.5℃, accompanied by aggravation of abdominal pain, tenderness under xiphoid process, abdominal muscular tension, showing a possibility of perforation. Chest and abdomen CT: Sub-phrenic free gas. Routine blood test: WBC of 14.48*10^9/L, ratio of neutrophils of 89.70%, and CRP of 150.5mg/L. At 23:30, with the consent of the family members, painless endoscopy was performed in the patient, and carbon dioxide air pump was used for air inflation to clarify the cause of perforation. Gastroscope: Duodenal bulb deformation, visible strip-like ulcer, about 1.5cm * 0.2cm in size, covered with white moss, accompanied by surrounding congestion and edema, with no obvious signs of perforation.
Painless colonoscopy
There was a large amount of fecal water in the intestines. After repeated irrigation, there were two postoperative ulcers in the transverse colon near the liver area, one of which was a perforation, which was deep in location, about 1.4cm in size, and about 4mm in diameter of the central part. The wound surface was clipped with 5 soft tissue clamps with an opening of 1.4cm, and the base of the 5 soft tissue clamps was ligated with nylon rope. In the rest of the colon, there were multiple postoperative ulcers (nearly 40 hours after polypectomy).
Treatment
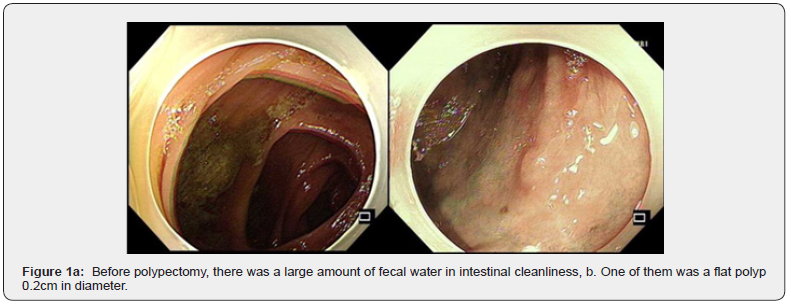
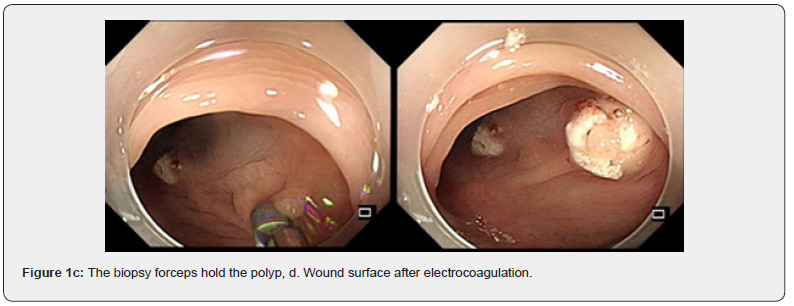
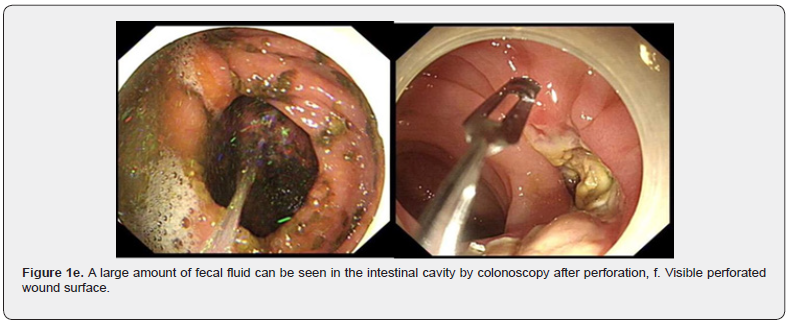
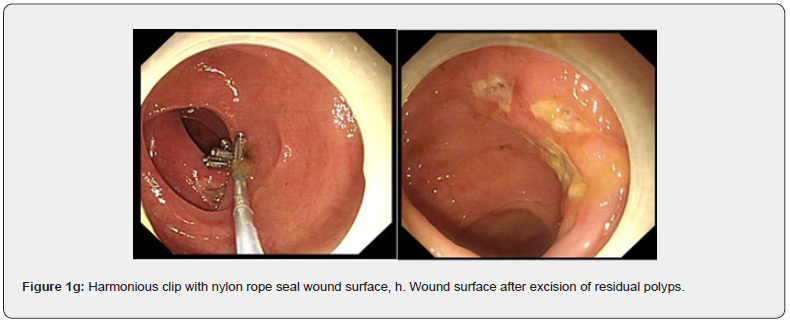
The patient was provided with fasting of oral feeding and drinking water, acid suppression, stomach protection, fluid infusion, nutritional support, inhibition of intestinal secretion, combined use of two antibiotics, and consultation of Gastrointestinal Surgery Department. As shown in the figure 1a- 1h:
The first day after repair
Symptoms: Fever, with the highest temperature of 38.9℃, accompanied by abdominal pain, abdominal distension, no anal flatus and defecation.
Signs: Epigastric eminence, tenderness, rebound pain, and abdominal muscular tension. Trans-abdominal type-B ultrasound: No obvious effusion in the abdominal cavity.
Treatment: The patient was provided with application for lowering the temperature, fasting of oral feeding and drinking water, nutritional support, as well as enhanced caring and communication to relieve the dissatisfaction of the patient. Meanwhile, the data of the patient was sent to provincial experts, and a surgical intervention was recommended as soon as possible. Despite repeated notification of the risk, the patient and his family still refused surgical intervention, and prepared to sue. At this time, the atmosphere of the whole department was depressing, and all doctors were under great pressure.
The second day after repair
Symptoms: The patient had relieved abdominal pain and distension, with the highest temperature of 37.8℃ and 3 times of anal defecation was 3 times. It was yellow watery stool. The patient showed improved symptom of abdominal distension than before. The patient had no abnormality in routine blood test, with CRP of 68.58mg/l.
Treatment: The patient was provided continuously with fasting of oral feeding and drinking water, acid suppression, stomach protection, inhibition of intestinal secretion, and other therapies.
The third day after surgery for perforation
The patient was monitored with normal temperature. However, the patient had nausea and vomiting with yellow bilelike substances, with improved symptoms of abdominal pain and abdominal distension better than before, with defecation twice of yellow watery stool.
Signs: The patient showed sub-xiphoid protrusion, tenderness and rebound pain, with no obvious abdominal muscular tension. Re-examination by using abdominal CT showed: inflammatory exudation around the perforation, with less gas accumulation and perihepatic effusion than before.
Treatment: The patient was provided with symptomatic treatment of stopping vomiting, trying drinking water, reducing rehydration, and stopping the use of somatostatin.
The fourth day after repair
Symptoms: The patient had no fever, improved abdominal pain and abdominal distension, with anal flatus and defecation, and significantly improved mental state.
Diet and treatment: The patient was given liquid diet following the principle of having more meals a day but less food at each, with enhanced symptomatic treatment of stomach protection. The patient was discharged the next day.
Discussion
Intestinal perforation is the most serious and rare complication of colonoscopy. According to statistics, the perforation rate of colonoscopy was 0.03-0.13%, and that of polypectomy was 0.08% [1]. However, with the popularity of colonoscopy and endoscopic treatment, there may be an annual increase in the incidence of iatrogenic intestinal perforation, which may be related to patient’s own condition, surgical procedures and status of polyps [2,3]. To be specific, patient factors included age (> 65 years old), female, chronic history, inflammatory bowel disease, use of anticoagulants and non-steroidal anti-inflammatory drugs, etc [4]. While polyp-related factors are diameter > 2cm, wide base, right colon polyp, abnormal morphology, etc [5-8]. From 2019 to 2020, there were 6,970 patients undergoing colonoscopy and treatment in the Digestive Center of our hospital, with 3 cases of perforation, and the perforation rate was 0.043%. Besides, there were 676 cases of polypectomy and 1 case of perforation, with the perforation rate of 0.14%. One of the patient was found in the course of colonoscopy and was occluded with soft tissue clamps. However, it caused abdominal abscess and the patient was barely discharged after 2 months of hospitalization with medical dispute. The second case was an inpatient in the Department of Obstetrics and Gynecology who underwent routine colonoscopy. The patient returned back to the ward after examination with severe abdominal pain and abdominal muscular tension. Owing to an insufficient understanding of the obstetricians and gynecologists about perforation, the patient was given pain relief treatment. Until the next morning when the obstetricians and gynecologists performed gynecological operation, the patient was found with intestinal exudate and perforation of intestinal wall. Peritoneal lavage and colostomy were performed in the patient by surgeons of the Department of Gastrointestinal Surgery.
After six months, colostomy closure operation was performed in this patient. Besides, the third case was the perforated patients after intestinal polypectomy in the present study. Based on the above two cases, perforation may be induced by many reasons. Firstly, both the 2 patients had low body mass index (BMI) that increased the difficulty to find the lumen and deliver the endoscope, part of the intestinal tract might be scratched by the endoscope itself, which easily led to intestinal mucosal traction injury, and even perforation. Similarly, it has been reported that a low BMI [9,10] is an independent risk factor for iatrogenic intestinal perforation. Secondly, the experience and personality of endoscopists are also risk factors for perforation [11-13]. Experienced endoscopists can deliver the endoscope through rotation, with rare inflation and pushing of the endoscope; by contrast, those who are impatient and easily affected by the environment are more likely to develop iatrogenic perforation.
In general, polypectomy-induced intestinal perforation is the most common complication of therapeutic colonoscopy, especially in right colon polyp with a diameter of >1cm, left colon polyp with a diameter of >2cm [14] or multiple polyps [15]. The patient with perforation in our report had multiple intestinal polyps. A membrane wall damage through electrical conduction was developed, which was attributed to a too large range of electrocoagulation resulted from long-time electrocoagulation and no action of lifting.
Conservative, endoscopic and surgical treatment are all the choices for the treatment of these patients. The use of surgical and non-surgical treatment are generally determined based on the patient’s symptoms, signs, perforation time, perforation size, intestinal cleanliness, etc. For instance, for patients with mild abdominal pain and non-obvious signs of peritonitis, it is recommended to adopt conservative fasting, fluid infusion and antibiotics for symptomatic treatment. In the case of obvious signs of peritonitis, observable signs of perforation indicated by imaging examination, clean intestinal tract, and the diagnosis time of perforation of < 24 hours, the patients can be treated with endoscopic titanium clip and/or root suture with nylon rope [16- 18]; on the contrary, surgical treatment should be applied if the diagnosis time of perforation is >24 hours and there is a poor intestinal cleanliness. In this case, the bowel preparation was poor in the patient with a large amount of fecal water during endoscopic polypectomy, producing negative affect on the field of vision of endoscopic treatment. Besides, the patient had a longterm drinking history, a history of duodenal ulcer, accompanied by sub-xiphoid pain, and no fever despite mild abdominal muscular tension. Accordingly, the possibility of whether there was pain caused by peptic ulcer or stress gastritis was considered in combination of the patient’s condition.
In this regard, the patient was supplied with intravenous injection of omeprazole for acid suppression, resulting in relieved pain of the patient. It covered up the condition of the patient to a certain extent, which indirectly resulted in misdiagnosis, and delayed the correct imaging and timely endoscopic closure. The possibility of perforation was proposed until late night when the patient had high fever and obvious signs of peritonitis. The diagnosis of perforation was confirmed by CT, which was nearly 40 hours after polypectomy. Considering that the patient was impossible to receive endoscopic treatment, surgical treatment was recommended after a consultation with the Department of Gastrointestinal Surgery. However, the patient and his family members were unable to understand with emotion and unable to accept surgical intervention. In this case, the only option was endoscopic treatment under CO2 gas pump. A large amount of fecal water was found in the intestinal cavity. After repeated washing, one ulcer with a diameter of about 1.4cm was detected with a perforation of gray in color and about 0.4cm in diameter in the center. Simultaneously, 5 soft tissue clamps were used to close the wound and nylon rope to fix the clamps at the root. Eventually, the patient did not receive surgery and discharged safely. Significantly, the successful endoscopic closure of the patient with extra-long delayed perforation also hit fresh records of endoscopic diagnosis and treatment of delayed perforation at home and abroad. At the same time, for intestinal polyp resection, the following points are worth our careful consideration. Firstly, for large intestine polyps (> 0.5cm in diameter), submucosal injection of methylene blue can be performed to separate the mucosa and muscle layer. Then, the snare can be used for assisting electrocoagulation to remove the polyps, and titanium clip can be selected for the closure of larger wound postoperatively. While polyps with smaller diameter (e.g., 0.2 - 0.4 cm) can be electrocoagulated by hot biopsy forceps. The biopsy forceps can be used to clamp the polyps. Pay attention to avoid clamping too many polyps. With the enteric cavity hung by lifting the polyp, point-type coagulation can be conducted during the process, that is, shortening the procedure time as short as possible. Closure by using titanium clips can be practicable for large wound. In addition, for beginners to avoid the problems of heat conduction and prolonged electrocoagulation in small polyps, Meilan injection is recommended for the polyp to separate the mucosa from the base layer, followed by removal using electrocoagulation with hot biopsy clamps. It can effectively reduce the damage breadth and depth of normal mucosa.
Conclusion
In conclusion, with the development of early cancer screening in China, enhanced public health awareness, and popularization of gastroscopy, there is a great increase in the detection rate of gastrointestinal polyps. It results in an increased rate of resection, which, however, is accompanied by elevated probability of bleeding and perforation. Significantly, serious complications can be avoided based on continuous summary of experience in the clinical setting.
References
- Reumkens EJ, Rondagh CM Bakker (2016) Post-colonoscopy complications: a systematic review, time trends, and meta-analysis of population-based studies. Am J Gastroenterol 111(8): 1092-1101.
- L von Karsa, J Patnick, N Segnan, W Atkin, S Halloran, et al. (2013) European guidelines for quality assurance in colorectal cancer screening and diagnosis: overview and introduction to the full supplement publication. Endoscopy 45(1): 51-59.
- Force USPST, Bibbins-Domingo K, Grossman DC, Curry SJ, Davidson KW, et al. (2016) Screening for colorectal cancer: US preventive services task force recommendation statement. JAMA 315(23): 2564-2575.
- Ryota Niikura, Hideo Yasunaga, Atsuo Yamada, Hiroki Matsui, Kiyohide Fushimi, et al. (2016) Factors predicting adverse events associated with therapeutic colonoscopy for colorectal neoplasia: a retrospective nationwide study in Japan. Gastrointest Endosc 84(6): 971-982.e6.
- Michael X Ma, Michael J Bourke (2016) Complications of endoscopic polypectomy, endoscopic mucosal resection and endoscopic submucosal dissection in the colon. Best Pract Res Clin Gastroenterol 30(5): 749-767.
- Xin Xu, Tao Wang, Zhongqing Zheng, Xin Chen, Wentian Liu, et al. (2017) Endoscopic submucosal dissection for large colorectal epithelial neoplasms: a single center experience in north China. Medicine (Baltimore) 96(36): e7967.
- W Heldwein, M Dollhopf, T Rösch, A Meining, G Schmidtsdorff, et al. (2005) The Munich Polypectomy Study (MUPS): prospective analysis of complications and risk factors in 4000 colonic snare polypectomies. Endoscopy 37(11): 1116-1122.
- SN Hong, JS Byeon, BI Lee, Seong Woo Jeon, Sung Ae Jung, et al. (2016) Prediction model and risk score for perforation in patients undergoing colorectal endoscopic submucosal dissection. Gastrointest Endosc 84(1): 98-108.
- Hamdani U, Naeem R, Haider F, Pardeep Bansal, Michael Komar, et al. (2013) Risk factors for colonoscopic perforation: a population-based study of 80118 cases. World J Gastroenterol 19(23): 3596-35601.
- Anderson ML, Pasha TM, Leighton JA (2000) Endoscopic perforation of the colon: lessons from a 10-year study. Am J Gastroenterol. Am J Gastroenterol 95(12): 3418-3422.
- Chukmaitov A, Bradley CJ, Dahman B, Umaporn Siangphoe, Joan L Warren, et al. (2013) Association of polypectomy techniques, endoscopist volume, and facility type with colonoscopy complications. Gastrointest Endosc 77(3): 436-446.
- Bielawska B, Day AG, Lieberman DA, et al. (2014) Risk factors for early colonoscopic perforation include non-gastroenterologist endoscopists: a multivariable analysis. Clin Gastroenterol Hepatol 12(1): 85-92.
- Rabeneck L, Paszat LF, Hilsden RJ, Lawrence C Hookey (2008) Bleeding and perforation after outpatient colonoscopy and their risk factors in usual clinical practice. Gastroenterology 135(6): 1899-1906.
- Heldwein W, Dollhopf M, Rosch T, A Meining, G Schmidtsdorff, et al. (2005) The Munich Polypectomy Study (MUPS): prospective analysis of complications and risk factors in 4000 colonic snare polypectomies. Endoscopy 37(11): 1116-1122.
- Hassan C, Zullo A, De Francesco V, E Ierardi, M Giustini, et al. (2007) Systematic review: endoscopic dilatation in Crohn’s disease. Aliment Pharmacol Ther 26(11-12): 1457-1464.
- Kim JS, Kim BW, Kim JI, Jeong Ho Kim, Sang Woo Kim, et al. (2013) Endoscopic clip closure versus surgery for the treatment of iatrogenic colon perforations developed during diagnostic colonoscopy: a review of 115,285 patients. Surg Endosc 27(2): 501-504.
- Han JH, Park S, Youn S (2011) Endoscopic closure of colon perforation with band ligation; salvage technique after endoclip failure. Clin Gastroenterol Hepatol 9(6): e54-e55.
- Cho SB, Lee WS, Joo YE, Hyeng Rok Kim, Sang Wook Park, et al. (2012) Therapeutic options for iatrogenic colon perforation: feasibility of endoscopic clip closure and predictors of the need for early surgery. Surg Endosc 26(2): 473-479.






























