Herpes Simplex Virus Esophagitis in an Immunocompetent Patient with Upper Gastrointestinal Bleeding: A Case Report
Hamid-Reza Moein1*, Cale Sebald2, Dongping Shi3 and Ahmad Abu-Rashed1
1Department of Internal Medicine, Wayne State School of Medicine, USA
2Division of Gastroenterology, St. John Macomb Oakland Hospital-Oakland Center, USA
2Department of Pathology, Wayne State School of Medicine, USA
Submission:April 04, 2021; Published:May 05, 2021
*Corresponding author:Hamid-Reza Moein, Division of Gastroenterology, Department of Internal Medicine, Sinai-Grace Hospital/Detroit Medical Center, Wayne State School of Medicine, Detroit, MI, USA
Hamid-Reza M, Cale S, Dongping S, Ahmad A-R. Herpes Simplex Virus Esophagitis in an Immunocompetent Patient with Upper Gastrointestinal Bleeding: A Case Report. Adv Res Gastroentero Hepatol, 2021; 17(1): 555951. DOI: 10.19080/ARGH.2021.17.555951.
Abstract
Background: Herpes simplex virus (HSV) esophagitis is rarely seen in immunocompetent patients. Symptoms include odynophagia, dysphagia, fever, and/or extra-esophageal herpetic lesions. A male predominance is noted with individuals being inflicted with the illness in the third to fourth decade. Although HSV esophagitis has typical punch-out lesions on endoscopy, it is very similar in appearance to cytomegalovirus (CMV) and should be confirmed by tissue biopsy. Upper gastrointestinal bleeding is a rare complication of HSV esophagitis. Treatment of HSV esophagitis in immunocompetent patients is controversial.
Case presentation: A 63-year-old African American woman with past medical history of chronic obstructive pulmonary disease (COPD) presented with acute shortness of breath and productive cough despite adherence to home medications. She was admitted for the management of a COPD exacerbation. Prompt respiratory demise required intubation and transfer to the intensive care unit. She subsequently developed coffee ground emesis with associated drop in hemoglobin. An esophagogastroduodenoscopy (EGD) was performed which noted punched-out esophageal ulcers and a non-bleeding superficial antral ulcer. Cold-forceps biopsies were taken from esophageal ulcers, which showed typical HSV histologic changes (multinuclear cells with ground glass appearance nuclei). Diagnosis was confirmed by positive immunohistochemical staining for HSV and negative staining for CMV. She was treated with oral valacyclovir for 10 days. Post-extubation dysphagia, detected by speech-language pathologist, prompted a percutaneous endoscopic gastrostomy (PEG) placement. Repeat EGD for PEG placement (1 day after completion of valacyclovir therapy) demonstrated resolution of previously noted esophagitis.
Conclusion: HSV esophagitis, although rare, can occur in immunocompetent patients. A high index of suspicion is required as patients may present with upper gastrointestinal bleeding but without any systemic symptoms as in our case. HSV esophagitis should be considered in immunocompetent patients with COPD or asthma exacerbation who are receiving systemic steroid therapy and develop upper gastrointestinal bleeding. Valacyclovir may be used successfully in treatment of HSV esophagitis in immunocompetent patients.
Keywords: Herpes simplex virus; Esophagitis; Infectious esophagitis; Gastrointestinal bleed
Keywords: HSV: Herpes Simplex Virus; HIV: Human Immunodeficiency Virus; PCR: Polymerase Chain Reaction; COPD: Chronic Obstructive Pulmonary Disease; IV: Intravenous; GI: Gastrointestinal; EGD: Esophagogastroduodenoscopy; CMV: Cytomegalovirus; PEG: Percutaneous Endoscopic Gastrostomy
Background
Herpes simplex virus (HSV) esophagitis is one of the most common subtypes of infectious esophagitis with reported incidence of 0.5-2% in autopsy studies [1]. HSV esophagitis is commonly diagnosed in immunocompromised men under 40 years of age. Those with human immunodeficiency virus (HIV) infection, underlying malignancy, burns, organ transplantation, immunosuppressive therapy, or systemic corticosteroids are particularly susceptible [2,3]. HSV esophagitis, however, has been rarely reported in immunocompetent patients [2,4]. Literature search by Canalejo et al. [2] revealed only 53 cases of HSV esophagitis in immunocompetent patients from 1950 to 2009.
The most common clinical manifestations of HSV esophagitis are odynophagia, fever, dysphagia, extra esophageal herpetic lesion(s), and retrosternal chest pain [2,5]. Diagnosis is established by histopathological examination with immunohistochemical staining, viral culture, or polymerase chain reaction (PCR) [2,5]. Herein, we present a case of HSV esophagitis, with typical endoscopic and histological findings, which was found incidentally in an asymptomatic immunocompetent patient.
Case Presentation
A 63-year-old African American woman presented to the emergency room with shortness of breath, not relieved by her home inhalers, and five days history of a productive cough with yellow sputum. Past medical history included chronic obstructive pulmonary disease (COPD), hypertension, and non-insulin dependent type 2 diabetes mellitus. On initial physical examination the patient was fully conscious and in mild to moderate distress. Blood pressure 221/134 mmHg, heart rate 133 beats/minute, respiratory rate 36 breaths/minute, and Temperature 36.4°C. Lung auscultation revealed bilateral wheezing. Bilateral lower extremity pitting edema was present. The remainder of the physical exam was normal.
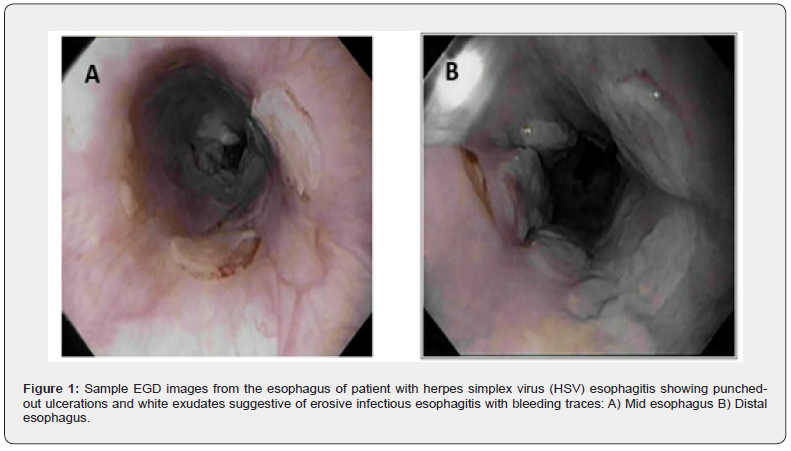
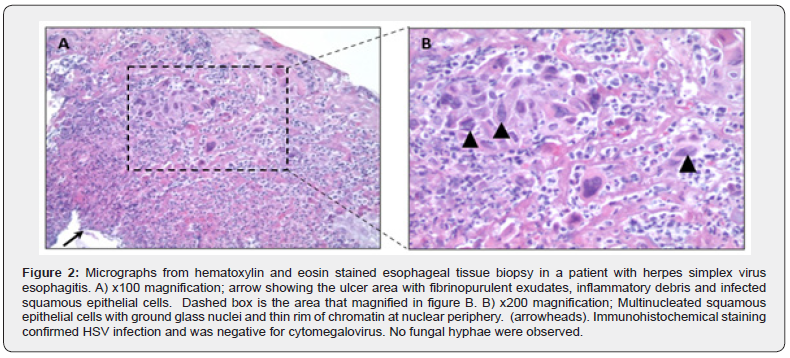
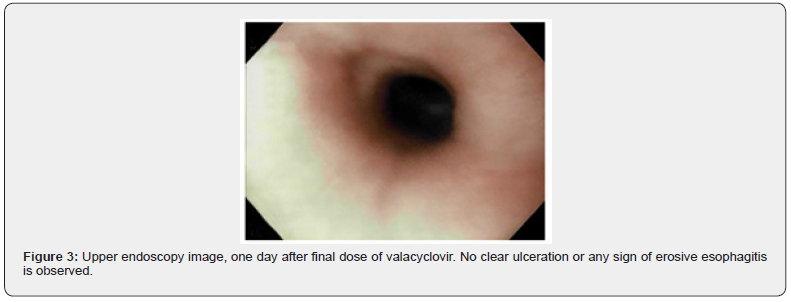
Patient was admitted to the hospital for COPD exacerbation. Initial blood work was within normal limits. except for an elevated triglyceride level (410 mg/dl) and total cholesterol level (298 mg/ dl). Rapid PCR tests for influenza and respiratory syncytial virus were negative. Chest X ray was without any infiltrate, effusion or opacity. She was treated with intravenous (IV) methylprednisolone, inhaled steroid (budesonide), bronchodilators, and doxycycline. The following day, the patient developed hypoxemic hypercapnic respiratory failure necessitating mechanical ventilation and a transfer to the intensive care unit. Gastrointestinal (GI) bleeding prophylaxis was started with IV pantoprazole. Two days after extubating, she developed coffee ground emesis. She denied symptoms of dysphagia or odynophagia. Hemoglobin decreased gradually to 6.1 g/dl from initial level of 12-13 g/dl. She received a total of 3 units packed red blood cells and her hemoglobin stabilized at 7-9 g/dl while inpatient. Additional lab work demonstrated leukocytosis (WBC, 30.1 K/mm3), mild transaminitis (AST, 69 units/L and ALT, 166 units/L), elevated lipase (1,911 units/L) and amylase (1,177 units/L). CT abdomen showed peripancreatic fluid establishing a diagnosis of acute pancreatitis. An esophagogastroduodenoscopy (EGD) was performed which demonstrated severe erosive esophagitis with multiple punchedout ulcers in mid and distal esophagus (Figure 1), a superficial nonbleeding antral ulcer, and an unremarkable duodenum. Biopsy results from the esophageal ulcers confirmed HSV esophagitis, demonstrating multinuclear cells with ground glass appearance nuclei and thin rim of chromatin at nuclear periphery (Figure 2). Immunohistochemical staining confirmed the presence of HSV and absence of cytomegalovirus (CMV). She was treated with 10 days of oral valacyclovir 500 mg daily (renally adjusted for her acute kidney injury). Speech-language pathology evaluation, postextubation, demonstrated dysphagia level II with thin liquids, which was attributed with long term intubation (13 days). Repeat EGD for percutaneous endoscopic gastrostomy (PEG) placement was performed, 1 day after completion of valacyclovir treatment course, and showed significant improvement of esophagitis and resolution of esophagitis (Figure 3).
Discussion and Conclusion
HSV esophagitis typically affects immunocompromised hosts but is occasionally observed in immunocompetent young men [2,4]. However, rarely it is reported in elderly women as well [6]. The aforementioned case describes an immunocompetent elderly woman with HSV esophagitis. Our case is unique given the atypical presentation. Our patient did not have any specific symptoms such as esophagitis or odynophagia, heartburn, fever, or dysphagia. Esophagitis was noted incidentally during an investigative EGD for upper GI bleeding. All previously reported HSV esophagitis cases were symptomatic [2,6].
HSV-1 is the primary pathogen for most cases of HSV esophagitis in immunocompetent patients. Infectious outbreaks are from reactivation of virus and rarely from primary infection [2,4]. Exposure to a family member with HSV lesions before the onset of symptoms was reported in 22% of the patients [4]. Steroid treatment is a risk factor for HSV esophagitis [2]; however, this is seen more in immunocompromised patients and with longer duration of steroid therapy [7,8]. Wiest et al. [8] presented a case series of COPD patients who were using steroids for 5 months to 10 years and some developed HSV esophagitis. Our patient received systemic and inhaled steroid therapy for COPD exacerbation during her hospital stay, which was tapered and discontinued after total of 18 days. Steroid therapy, therefore, may have had a role in development of HSV esophagitis in our patient but its association with short term steroid therapy in an immunocompetent patient is unclear and warrants further investigation.
Endoscopic appearance of HSV esophagitis includes friable mucosa and several ulcers that vary in size, depth, and type of clustering. Ulcers are mainly found in mid and distal esophagus [2,4,5]. The gross appearance may vary depending on the timing of endoscopy. Earlier lesions can present as vesicles or form circumscribed ulcers with raised edges. These lesions may be punched-out and volcano-like in appearance or may coalesce to exhibit a cobblestone or shaggy ulcerative appearance [4,5]. Circumferential punched-out ulcers are the most common feature of CMV esophagitis [9]. Our patient had multiple punched-out lesions with erosions and bleeding in the mid to distal to distal esophagus, which was suggestive of either HSV or CMV esophagitis. Histologic diagnosis is essential given that endoscopic features of HSV esophagitis are very similar to CMV esophagitis [6,9].
Eosinophilic intranuclear and cytoplasmic inclusion bodies within squamous cells, along with Cowdry type A inclusions, are pathognomonic histologic features in HSV esophagitis [5]. Additionally, HSV esophagitis can also be confirmed by immunohistovhemistry, tissue PCR or viral culture [2].
Treatment of HSV esophagitis in immunocompetent patients is controversial and can be self-limiting in most cases [2,4]. Acyclovir is the most common antiviral therapy used for treatment of HSV esophagitis and the duration of therapy ranged between 5 to 21 days (mostly 7-10 days) [2,6]. Upper GI bleeding (5.3%) and esophageal perforation (1.8%) are rare complications of HSV esophagitis [2,4]. Given the severity of the GI bleed, the patient was treated with valacyclovir with the goal to promptly heal the ulcerated esophageal mucosa. This resulted in complete resolution of lesions after 10 days of treatment. Similarly, Noda & Donatelli et al. [10,11] reported successful treatment of HSV esophagitis with valacyclovir.
In conclusion, HSV esophagitis is a rare infection in immunocompetent patients. It mostly presents with some systemic or GI symptoms. Here, we presented a case of HSV esophagitis in an immunocompetent patient who was asymptomatic but developed upper GI bleeding. This indicates that HSV esophagitis can be indolent and undiagnosed in immunocompetent patients emphasizing the need for a high index of suspicion. We also demonstrated complete resolution of esophagitis following a 10- day course of oral valacyclovir without any major side effects.
References
- Wang HW, Kuo CJ, Lin WR, Chen-Ming Hsu, Yu-Pin Ho, et al. (2016) Clinical Characteristics and Manifestation of Herpes Esophagitis: One Single-center Experience in Taiwan. Medicine (Baltimore) 95(14): e3187.
- Canalejo Castrillero E, Garcia Duran F, Cabello N, Garcia Martinez J (2010) Herpes esophagitis in healthy adults and adolescents: report of 3 cases and review of the literature. Medicine (Baltimore) 89(4): 204-210.
- Genereau T, Rozenberg F, Bouchaud O, Marche C, Lortholary O (1997) Herpes esophagitis: a comprehensive review. Clin Microbiol Infect 3: 397-407.
- Ramanathan J, Rammouni M, Baran J, Jr., Khatib R (2000) Herpes simplex virus esophagitis in the immunocompetent host: an overview. Am J Gastroenterol 95(9): 2171-2176.
- Narasimhalu T, Olson KA (2020) Educational Case: Infectious Esophagitis. Acad Pathol 7: 2374289520903438.
- Bando T, Matsushita M, Kitano M, Okazaki K (2009) Herpes simplex esophagitis in the elderly. Dig Endosc 21(3): 205-207.
- Smith LA, Gangopadhyay M, Gaya DR (2015) Catastrophic gastrointestinal complication of systemic immunosuppression. World J Gastroenterol 21(8): 2542-2545.
- Wiest PM, Flanigan T, Salata RA, Shlaes DM, Katzman M, et al. (1989) Serious infectious complications of corticosteroid therapy for COPD. Chest 95: 1180-1184.
- Jung KH, Choi J, Gong EJ, Jeong Hoon Lee, Kee Don Choi, et al. (2019) Can endoscopists differentiate cytomegalovirus esophagitis from herpes simplex virus esophagitis based on gross endoscopic findings? Medicine (Baltimore) 98: e15845.
- Noda J, Devlin S, Mahon GM, Zhu W (2014) Case report: herpes simplex esophagitis in a frail elderly patient. J Am Med Dir Assoc 15: 955-956.
- Donatelli G, Vergeau BM, Tuszynski T, Meduri B (2016) Giant, deep, well-circumscribed esophageal ulcers. Dis Esophagus 29: 684-685.






























