Esophagitis Dissecans: A Rare Cause of Esophageal Stenosis
Gueye Mamadou Ngone*, Diallo Salamata, Fall Marème Polèle, Cissé Cheikh Ahmadou Bamba, Ndiaye El hadj Modou, Thioubou Mame Aïssé, Diouf Gnagna, Bassène Marie Louise, Dia Daouda and Mbengue Mouhamadou
Idrissa Pouye General Hospital, Senegal
Submission:April 12, 2021; Published:May 05, 2021
*Corresponding author: Gueye Mamadou Ngone, Idrissa Pouye General Hospital, Dakar, Senegal
How to cite this article: Gueye M N, Diallo S, Fall M P, Cissé C A B, Ndiaye El h M, et al. Esophagitis Dissecans: A Rare Cause of Esophageal Stenosis. Adv Res Gastroentero Hepatol, 2021; 16(5): 555950. DOI: 10.19080/ARGH.2021.16.555950.
Abstract
Chronic dissecans oesophagitis is a rare condition of recent discovery. It is the consequence of degenerative changes in the superficial layer of the oesophageal mucosa, reducing adhesion between the cells of the malpignan epithelium [1]. It can be primary or secondary. dissecans oesophagitis is recognised as one of the etiologies of chronic dysphagia. The most common endoscopic appearance is a whitish mucosa that flakes off either spontaneously or on biopsy. In rare cases, esophageal stricture may be associated. We report a case of dissecting stenosing oesophagitis in a patient treated for lichen planus.
Keywords: Esophagitis dissecans; Stenosis; Lichen plan; Chronic dissecans oesophagitis
Introduction
Chronic dissecans oesophagitis is a rare condition of poorly understood aetiopathogeny. It is the consequence of degenerative changes in the superficial layer of the oesophageal mucosa, reducing adhesion between the cells of the squamous epithelium [1].
Primary cases occur in 20% of cases. Secondary dissecans oesophagitis occurs in the context of GERD, dermatological disease (lichen planus, pemphigus vulgaris), eosinophilic oesophagitis, drug use (biphosphonates, NSAIDs) or coeliac disease [2].
Progression to oesophageal stricture is not common. We report a case of chronic dissecting oesophagitis complicated by oesophageal stricture in a patient being treated for lichen planus.
Observation
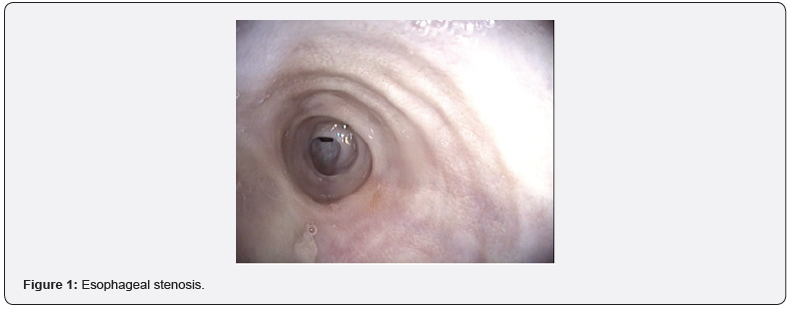
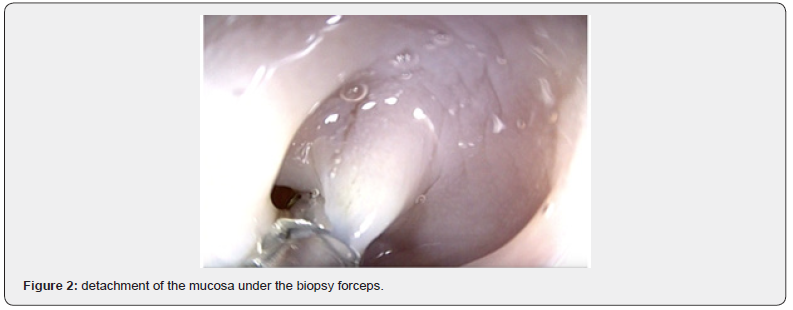
This was a 43-year-old female patient who had been treated for Lichen Plan for 8 years and who presented with mechanical dysphagia for 3 years. The dysphagia was not disabling (dysphagia score = 1). For 3 months, the patient noted a worsening of her dysphagia (dysphagia score = 3) which motivated a consultation. Esogastroduodenal endoscopy revealed a tight, whitish annular stenosis that could not be penetrated by the endoscope at 25 cm from the AD, and which was detached in flaps under the biopsy forceps (Figures 1 & 2).
A 9, 11 and 13 mm Savary Gilliard candle dilatation was performed, allowing the stenosis to be crossed with the endoscope. The sub-stenotic mucosa had a pseudo-tracheal appearance (Figure 3).
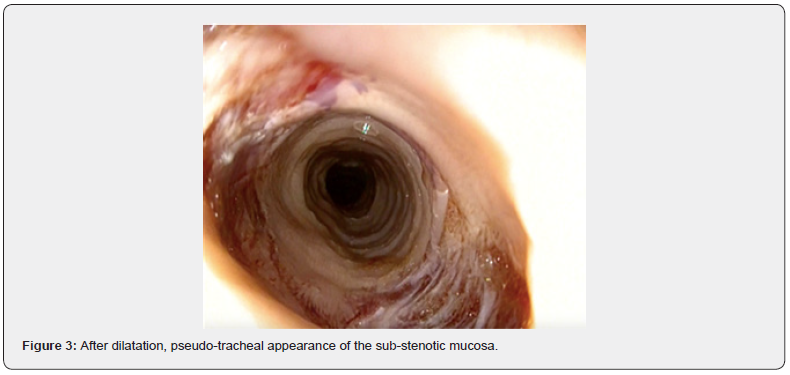
It was whitish, detached in shreds on contact with the endoscope and under the biopsy forceps. The oesophageal biopsies obtained were longer than usual. Histological analysis showed that the squamous epithelium was of normal thickness and the basal layers of the epithelium contained normal looking keratinocytes with oedematous intercellular spaces. A few inflammatory cells (mainly lymphocytes and rare neutrophils) were present. An intramucosal detachment was located in the suprabasal region. There was no inflammatory infiltrate in the lamina propria. No electron microscopic or immunohistochemical studies were performed.
The diagnosis of secondary dissecans oesophagitis complicated by stenosis was retained in view of the endoscopic and histological appearance of this patient suffering from lichen planus. A followup endoscopy at 4 weeks showed a recurrence of the stenosis but less tight and the persistence of a fragile mucosa, still detaching when rubbed with the endoscope. A new dilatation with Savary Gilliard candles was performed this time up to 15 mm. The evolution was favourable with a disappearance of the dysphagia (dysphagia score = 0).
Conclusion
Dissecans oesophagitis is a rare cause of chronic dysphagia that is often unrecognised. The diagnosis is evident from evocative endoscopic aspects. Its evolution is favourable, but it can be troublesome and require dilatations on demand. Studies are still needed to understand its pathophysiology and to define an appropriate treatment.
References
- Ponsot P, Molas G, Scoazec JY, P Ruszniewski, D Hénin, et al. (1997) Chronic œsophagitis dissecans: an unrecognized clinicopathologic entity? Gastrointest Endosc 45(1): 38-45.
- Hokama A, Ihama Y, Nakamoto M, N Kinjo, F Kinjo, et al. (2007) Esophagitis dissecans superficialis associated with bisphosphonates. Endoscopy 39(Suppl 1): E91.






























