The Role of Oesophagogastroduodenoscopy in Avoiding Unnecessary Cholecystectomies in Patients with Gallstones and Upper Abdominal Discomfort
Mohamed Alshekhani* and Juned Gafoor Mustafa
Department of Medicine, University of Sulaimaniyah, Iraq
Submission: January 08, 2018; Published: Februay 02, 2018;
*Corresponding author: Mohamed Alshekhani, Department of Medicine, University of Sulaimaniyah, Iraq, Email: shaikhanimohammad@googlemail.com
How to cite this article: Mohamed A, Juned G M. The Role of Oesophagogastroduodenoscopy in Avoiding Unnecessary Cholecystectomies in Patients with Gallstones and Upper Abdominal Discomfort. Adv Res Gastroentero Hepatol 2018; 8(5): 555747. DOI: 10.19080/ARGH.2018.08.555747.
Abstract
Background: Cholelithiasis is a common condition, 10-20% of the population will develop gallstones, the incidence increases with age. Only about 30% of asymptomatic patients will wARGHant surgery during their lifetime. Dyspeptic symptoms due to other abdominal conditions such as PUD, IBS, Functional dyspepsia, IBS & GERD are frequently attributed to Gallstones.
Aim of study: To assess the role of upper endoscopy in patients with gallstones in avoiding unnecessary cholecystectomies.
Patients and methods: 124 patients were included in sulaimanyah city hospitals from October 2015 to February 2017 complaining of upper GIT symptoms and U/S evidence of gallstones and an OGD is performed to exclude other possible explanation which may avoid unnecessary operation.
Results: Among 124 patient 99(79.8%) were females and 25(20.2%) were male; The mean age of studied patients was 46.4±14.5 years. The OGD findings of patients with Gallstones were normal 63 (50.8%), deudenal ulcer 24(19.4%), non significant findings 24(19.4%), reflux esophagi is 10(8.2%), gastrodudenitis 2(1.6%) and fungal esophagi is (10.8%), There was 12(9.6%) patients in whom surgery decision was changed while in 112(90.4%) the surgery was done.
Conclusion: OGD is a very useful tool in the preoperative evaluation of patient with Gallstones with upper GIT symptoms.
Keywords: GIT; OGD; Gallstones
Introduction
Gallstone is one of the commonest problems in GE practice [1-3]. The prevalence is 5-10% mostly among female & middle to elder age groups [4-7], rising in many countries including Iraq [8]. In England 70000 & USA > 0.5 million cholecystectomies had done each year [9]. Risk factors include; Advancing age ,Multiple pregnancies, Obesity, repeated fluctuations in body weight, rapid weight loss >1.5kg/week, high dose estrogens & Cholestyramine/fibrates [10-12]. Protective factors may include Moderate exercise, Coffee & Moderate alcohol consumption [13-15].
Presentations of Gallstones include asymptomatic& Symptomatic ones which include:
A. Biliary colic: a Moderate - Severe epigastria or right hypochondriac pain that last for 15 minutes to 6 hours or less than 24 hours , not associated with fever & can be associated with nausea/vomiting ,usually resolve spontaneously or by medications [16-18].
B.Symptomatic complications as acute pancreatitis, obstructive jaundice, cholecystitis 0.2-0.8%/ annum, 0.3-1.2% if the stones are initially asymptomatic , 0.7-2%/annum ifthe stones are initially symptomatic, Other rare symptomatic complications include Acute cholangitis, Mucocele of gallbladder, Empyema of gallbladder, Gangrenous gallbladder, Biliary peritonitis, Porcelain gallbladder, Gallbladder cancer [11,19,21,22].
Management includes:
A.Nonsurgical: Oral dissolution with bile acids successfully dissolved gallstones in an extremely limited patient population, especially in patients with symptomatic radiolucent gallstones <15 mm within a functioning gallbladder.
B. Laproscopiccholecystectomy (LC): results in a shorter hospital stay, speedier recovery, reduction of postoperative pain & better cosmetic results compared with open surgery [12,23-25].
Indications for cholecystectomy for asymptomatic Gallstones may include:
a. Age: children & young adults.
b. Very large stones >3cm.
c. Thick walled gallbladder >0.3cm.
d. Porcelain gallbladder
e. Large sessile polyps.
f. Race related like native American Indians [13,26-30].
4. Patients and Methods
A prospective study in sulaimanyahgovermental hospitals (KCGH, Shar teaching hospital & Surgical teaching hospital). A total number of 124 patients with U/S diagnosed GSs & upper GIT symptoms were referred to do OGD. A full history &clinical exam cARGHied out with emphasis on upper GIT & Biliary symptoms. Patients were followed out to see in how many patients the decision to do operation was changed in the short term follow- up of our study period. Inclusion criteria: any adult with U/S evidence of GSs & upper GIT symptoms.
Exclusion criteria: any case of complicated Gallstone including common bile duct stones, acutecholecystitis, pancreatitis, cholangitis.
Results
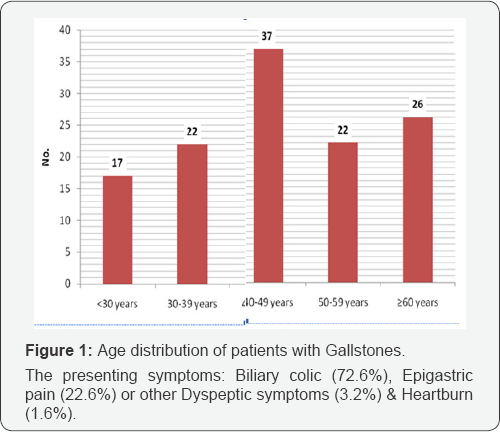
The mean age of studied patients was 46.4±14.5 years, 29.9% of them were 40-49 years, 21% of them >60 years, 17.7% ,3039 years, 17.7% ,50-59 years & 13.7% ,>10 years. Females were more than males with female to male ratio as 3.96:1(Figures 1-5 and Table 1).
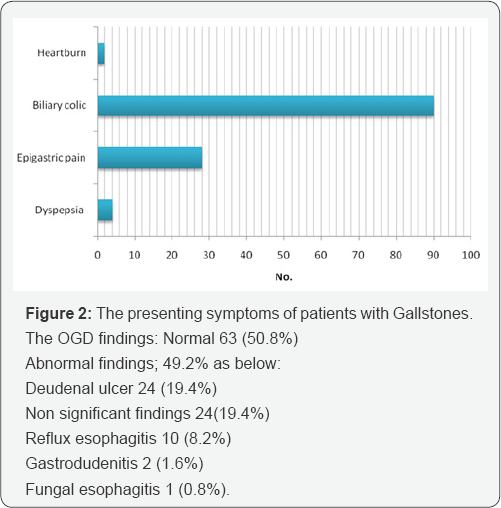
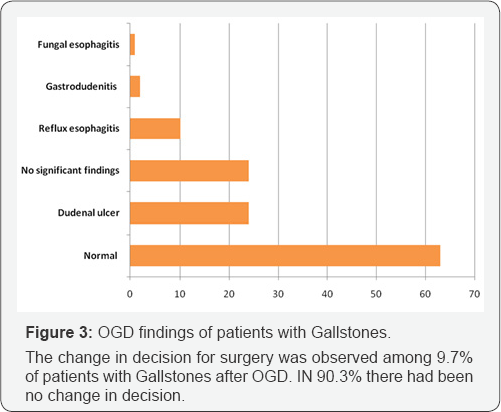
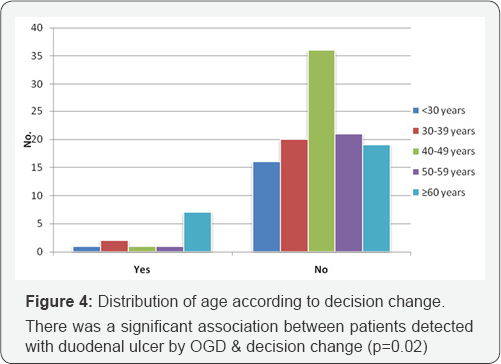
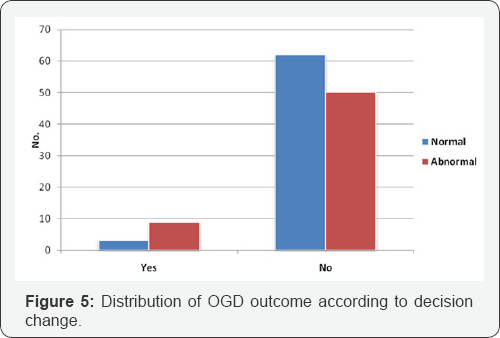
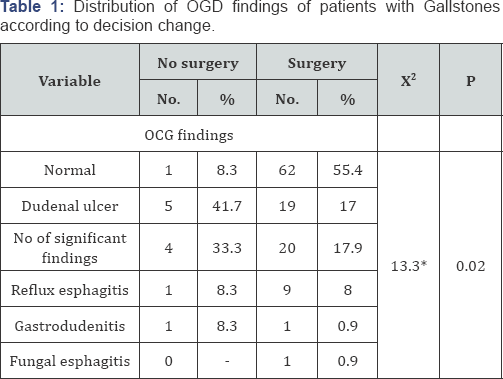
There was a significant association between Gallstone patients with abnormal OGD findings & decision change (p=0.002).
Discussion
Our patients were 124 in number, female 99 (79.8%), 25(20.2%) and a female to male ratio of 3.96/1, similar prevalence observed in a study cARGHied out in India [31-36]. In our study the OGD findings of patients with upper GIT symptoms and Gallstone were normal 63(50.8%), deudenal ulcer 24(19.4%), non significant findings 24(19.4%), reflux esophagi is 10(8.2%), gastrodudenitis 2(1.6%) and fungal esophagi is (0.8%). The results were near to results of a study cARGHied out by Thybusch et al in Germany, which showed 50% of patients had pathological findings on OGD examination [37]. Another study in Germany recommend that OGD must be done before an elective cholecystectomy &showed that out of 960 patients for elective cholecystectomy, 589 underwent gastro copy 56% had normal gastro copy [38].
In our study the change in decision for surgery was observed among 9.7% of patients with upper GIT symptoms and Gallstones after OGD while 90.3% of them had no change in decision &underwent operation. The results of OGD findings changed decision in the management plan in 8.3% and 11.7% of patients in previously mentioned study by Thybusch et al. [37] & Rassek et al. [38]. A study in Poland showed that Pathological findings were identified in 1187(42%) patients & the surgery was delayed for patients with ulcers until they finished their medical treatment , Sixteen patients had complete resolution of symptoms after medical treatment therefore cholecystectomy was not performed [39,40]. In a study done in Sudan included 108 patients with GSs & OGD was done revealed different pathological findings in 61(56%), Cholecystectomy was done for 82(76%) & 26 were treated conservatively [41]. A study in India [42] showed that in 89 patients the management plan had to be changed in 7.9% of patients based on the upper GI endoscopy findings (P value <0.001). In a meta-analysis of 12 cohort studies a total of 6317 patients with Cholelithiasis underwent OGD & in 36.3% abnormality was found in OGD but only 3.8% of patient surgery was avoided [43]. Another study by Yavorski et al. [43] recommend that patients who present with Cholelithiasis & atypical abdominal pain undergo preoperative OGD, as they found that at least 9 per cent of the patients in their study had significant findings that altered their management. In a study in india in 2016 ,216 patient with Gallstone underwent OGD, showed 100% who underwent LC, had relief of symptoms in patients with normal OGD finding while those with significant OGD findings either not went through surgery in 10(4.6%) or when surgery was done they had more gradual relief of symptoms in 6 months follow-up [44]. A study in England suggested that OGD should be considered as a routine investigation before LC especially in those, who present with overlapping upper GI symptoms [45].
Conclusion
1. Gallstones are frequently silent & upper GIT symptoms can be attributed to other pathologies in upper GIT.
2. OGD is a very useful tool which can be used in every case with Gallstone & upper GIT complains especially those with atypical symptoms.
3. OGD before elective cholecystectomy can help avoid unnecessary surgeries.
4. Biliary colic was the most important symptom that predicted negative OGDs & led to the decision of proceeding to surgery, so every effort should be done to take a good history of typical biliary colic in those patients.
Recommendations
1. We recommend evaluating patients with Gallstones very carefully to avoid doing un-necessary LC.
2. We highly recommend OGD as an appropriate evaluation of patients planned for elective cholecystectomies.
References
- Everhart J (2008) The burden of digestive diseases in the United States.
- Centers for Disease Control and Prevention. Discharges with at least one procedure in nonfederal short-stay hospitals, by sex, age, and selected procedures: United States, selected years 1990 through 20092010, www.cdc.gov/nchs/hus/contents2012.htm#098.
- Health and Social Care Information Centre. Hospital episode statistics, Admitted patient care, England-2012-13.
- Karmacharya A, Malla BR, Joshi HN, Gurung RB, Rajbhandari M (2013) The predictve value of pre-operatve symptoms including upper gastrointestnal endoscopy before laparoscopic cholecystectomy for electve symptomatc cholecystolithiasis. Kathmandu Univ Med J 44(4): 300-304.
- Huang J, Chang CH, Wang JI, Kuo HK, Zin JW, Shan WY (2009) Natonwide epidemiological study of several gallstone disease in Taiwan. BMC Gastroenterol 9: 63
- Everhart JE, KhARGHe M, Hill M, Maver KR (1999) Prevalence and ethnic differences in gallbladder diseases in the United States. Gastroenteroscopy 117(3): 632-639.
- Conte D, Fraquelli M, GiuntaM, Cont CB (2011) Gall stones and Liver disease; an overview. J Gastrointestn Liver Dis 20(1): 9-11.
- (2001) Changing Pattern and Incidence of Gallstone Diseases in Al- Kadhymia Teaching Hospital, Bashar A Abdul Hassan, Dept. of Surgery, College of Medicine, Al-Nahrain University, IRAQI J MED SCI. 9(2).
- Diehl AK (1991) Epidemiology and natural history of gallstone disease. Gastroenterol Clin North Am. 20(1): 1-19.
- Weinster RL, wilsonLJ, lee LJ (1995) Medically safe weight loss for treatment of obesity: a guideline based on the risk of gallstone formation. AM J MED 98(2): 115-117.
- Atilli AF, Capocaccia R, CarulliN, Festi D, Roda E, et al. (1997) Factors associated with gallstone disease in theMICOLexperience. Multicenter italian study on epidemiology of cholelithiasis. Hepatology 26(4): 809818.
- Leitzman MF, Rimm EB, Willet WC, Grodstein F, Colditz GA, et al. (1999) Recreation physical activity and the risk of cholecystectomy in women. N Engl J Med 341(11): 777-784.
- Veysey MJ, Thomas LA, Mallet AI, Jenkins PJ, Besser Gm, et al. (1999) Prolonged large bowel transit increase serum deoxycholic acid: a risk factor for octreotide induced gallstone. Gut 44(5): 675-681.
- Heaton KW (2000) Epidemiology of gallbladder disease-role of intestinal transit. Alimentpharmacolther 14(2): 9-13.
- Leitzman MF, Rimm EB, Willet WC, Stampfer MJ, Coldtz GA, et al. (1999) A prospective study coffee consumption and the risk of gallstone in men. JAMA 281(22): 2106-2112.
- Caroli-rose FX, Le Gall P, Puliese P, Delabre B, Demarquay JF, et al. (2001) Role of fibrates and HMG-COA reductase inhibitors in gallstone formation; epidemiological study in an unselected population. Dig Dis Sci 46(3): 540-544.
- (2005) First principles of gastroentrology fifth edition. In: ABR Thomas, EA Shaffer (Eds.), Janssen-Ortho, canada.
- (2015) HARGHisons principles of internal medicine 19th edition 1-2.
- WGO Practice Guideline: Asymptomatic Gallstone Disease, core team. In: AG Johnson, M Fried, GNJ Tytgat, JH, Krabshuis Special Advisors: Roque Saenz, Martin Carey, SP Lee.
- Heaton KW, Braddon FE, Mountford RA, Hughes AO, Emmett PM (1991) Symptomatic and silent gall stones in the community. Gut 32(3): 316320.
- Capocaccia L, Giunchi G, Pocchiari F (1984) Prevalence of gallstone disease in an Italian adult female population. Rome Group for the Epidemiology and Prevention of Cholelithiasis (GREPCO). American Journal of Epidemiology 119(5): 796-805.
- Fendrick AM, Gleeson SP, Cabana MD, Scwartz JS (1993) Asymptomatic gallstones revisited. Is there a role for laparoscopic cholecystectomy? Arch Fam Med 2(9): 959-68.
- Kurinchi S Gurusamy (2014) Gallstones. Clinical Review 348: 2669.
- Petroni ML, Jazrawi RP, Pazzi P, Lanzini A, Zuin M, et al. (2001) Ursodeoxycholic acid alone or with chenodeoxycholic acid for dissolution of cholesterol gallstones: a randomized multicentre trial. The British-Italian Gallstone Study group. Aliment Pharmacol Ther 15(1): 123-128.
- Hood KA, Gleeson D, RuppinDC, DowlingRH (1993) Gall stonerecurrence and its prevention: the British/Belgian Gall Stone Study Group's post dissolution trial. Gut 34(9): 1277-1288.
- (1992) Gallstones and laparoscopic cholecystectomy. NIH Consensus Statement 10(3): 1-28.
- Tornqvist B, Stromberg C, Persson G, Nilsson M (2012) Effect of intended intraoperative cholangiography and early detection of bile duct injury on survival after cholecystectomy: population based cohort study. BMJ 345: 6457.
- Gurusamy KS, Davidson BR (2010) Surgical treatment of gallstones. Gastroenterol Clin North Am 39(2): 229-244.
- Department of Health. NHS reference costs 2012 to 2013. www.gov.uk/ government/ publications/nhs-reference-costs-2012-to-2013.
- Keus F, Dejong JAF, Goosze HG, Van LARGHhove CJHM (2006) Laparascopic versus open cholcystectomy for patients with symptomatic colelithiasis. Chocrane database sys rev (4): CD006231.
- Patino JF, Quintero GA (1998) Asymptomatic cholelithiasis revisited. World J Surg 22(11): 1119-1124.
- Srikanth G, Kumar A, Khare R, Siddappa L, Gupta A, Sikora SS, et al. (2004) Should laparoscopic cholecystectomy be performed in patients with thick walled gall bladder? J Hepatobiliary Pancreat Surg 11(1): 40-44.
- Diehl AK (1983) Gallstone size and the risk of gall bladder cancer. JAMA 250(17): 2323-2326.
- Vitetta L, Sali A, Little P, Mrazek L (2000) Gallstones and gall bladder carcinoma. Aust N Z J Surg 70(9): 667-673.
- Lowenfels AB, Lindstrom CG, Conway MJ, Hastings PR (1985) Gallstones and risk of gallbladder cancer. J Natl Cancer Inst 5(1): 77-80.
- Kolla V, Charles N, Datey S, Mahor D, Gupta A, Malhotra S (2016) Upper gastrointestinal endoscopy prior to laparoscopic cholecystectomy: a clinical study at a tertiary care centre in central India. Int Surg J 3(2): 637-642.
- Thybusch A, Schaube H, Schweizer E, Gollnick D, Grimm H (1996) [Significant value and therapeutic implications of routine gastroscopy before cholecystectomy]. J Chir (Paris) 133(4): 171-174.
- Rassek D, Osswald J, Stock W (1988) [Routine gastroscopy before cholecystectomy]. Chir'urg 59(5): 335-337.
- Sosada K, Zurawinski W, Piecuch J, Stepien T, Makarska J (2005) Gastroduodenoscopy: a routine examination of 2,800 patients before laparoscopic cholecystectomy. Surg Endosc 19(8): 1103-1108.
- Mohamed Toum Musa M Ibrahim, Randa Zaki A M Khair, El-Hadi Y Mohamed, AbdelMagid M Massaad. Upper gastrointestinal endoscopic fndings in patients with gallstone disease. University of Khartoum, Khartoum Teaching Hospital, Omdurman Islamic University.
- Indrajit R, Jugindra S, Chandragupta C (2016) Role of upper gastrointestinal endoscopy in patients with symptomatic gallstone disease - a prospective, descriptive study. Indian Journal of Medical Research and Pharmaceutical Sciences 3(8).
- Mark PL, Wietske K, Cihan Ozdemir, Gert P Westert, Cornelis JHM van Laarhoven, Joost PH Drent. EGD in patients referred for cholecystectomy: a systematic review and meta-analysis.
- Yavorski CC, Acosta JA, Ragland JJ (1995) Precholecystectomy routine oesophagogastroduodenoscopy before cholecystectomy esophagogastroduodeno- scopy: is it of value? Am Surg 61(12): 1032- International Journal ofSurgery 8(3): 236-238.1034.
- Rashid F, Rashid N, Waraich N, Ahmed J, Iftikhar SY (2010) Role of
- http://www.intechopen.com/books/endoscopy-of-gi-tract.intech






























