The Discovery through Dentistry of Potentially HCV-Infected Japanese Patients and Intervention with Treatment
Yumiko Nagao1,2* and MasahideTsuji2
1Department of Organ System Interactions and Information, Faculty of Medicine, Saga University, Japan
2Tsuji Dental & Oral Surgery Clinic, Shiragane-machi, Japan
Submission: September 09, 2017; Published: October 04, 2017
*Corresponding author: Yumiko Nagao, Department of Organ System Interactions and Information, Faculty of Medicine, Saga University, 5-1-1 Nabeshima, Saga 849-8501, Japan, Tel: +81-952-34-2516; Fax: +81-952-34-2516; Email: nagaoyu@cc.saga-u.ac.jp
How to cite this article: Yumiko Nagao, MasahideTsuji.The Discovery through Dentistry of Potentially HCV-Infected Japanese Patients and Intervention with Treatment. Adv Res Gastroentero Hepatol 2017; 7(3): 555711.DOI:10.19080/ARGH.2017.07.555711
Abstract
Background: Oral Lichen planus (OLP) is a representative extrahepatic manifestation of hepatitis C virus (HCV) infection. Many HCV- infected individuals remain untreated in Japan and the aim of this study was to evaluate retrospectively the frequency of encouragement of patients with HCV-associated OLP to consult a hepatologist following a visit to a dental clinic.
Materials and Methods: A total of 90 patients, who visited our dental clinic in Japan from May, 2015 to February 2017, were examined retrospectively. The subjects were 23 males and 67 females (average age, 68.9 years). We examined the discovery rate and encouragement to treatment of untreated HCV-infected individuals among OLP patients.
Results: OLP was the most common oral disease (38/90, 42.2%). Fifteen of 51(29.4%) patients who were tested for HCV infection were found to be positive. Among the 15 HCV-infected patients, the most common disease was OLP (10/15, 66.7%, P=0.0126). One patient had not been diagnosed previously with HCV Treatment with antiviral therapy at the first visit was as follows; sustained virological response (SVR), n=5(66.7%); under direct-acting antivirals (DAA) therapy, n=2 (13.3%); under maintenance interferon (IFN) therapy, n=1(6.7%); no treatment, n=7(46.5%). Five patients were encouraged to receive treatment for liver disease (4, no treatment; 1, exacerbated by IFN). Three patients received appropriate treatment and achieved SVR.
Conclusion: We report that general dentists could be the gatekeepers of the health-care system, especially for untreated HCV-infected individuals. The clinical cooperation of dentists and physicians is important for treating HCV-infected individuals early.
Keywords: Oral lichen planus (OLP); Hepatitis c virus (HCV); Interferon (IFN); Direct-acting antivirals (DAA); Dentist
Abbreviation: OLP: Oral Lichen Planus; HCV: Hepatitis C Virus; CH-C: Chronic Hepatitis C; LC-C: HCV-Related Liver Cirrhosis; HCC: Hepatocellular Carcinoma; IFN: Interferon; RBV: Ribavirin; DAA: Direct-Acting Antivirals; SVR: Sustained Virological Response; CLP: Cutaneous Lichen Planus; LDV/SOF: Ledipasvir and Sofosbuvir; DCV/ASV: Daclatasvir and Asunaprevir; SOF/RBV: Sofosbuvir and Ribavirin; NA: Not Applicable; CH-B: Chronic Hepatitis Type B; PBC: Primary Biliary Cirrhosis; NASH: Non-Alcoholic Steatohepatitis
Introduction
In 2015, 71 million people worldwide were estimated to have chronic hepatitis C virus (HCV) infection [1]. In May 2016, the World Health Organization (WHO) launched a new global strategy to eliminate viral hepatitis as a public health threat by 2030 (reducing new infections by 90% and mortality by 65%) [2]. In Japan, HCV is responsible for one of the most common infections, affecting approximately 1.5 to 2 million people, and about 30,000 deaths from hepatocellular carcinoma (HCC) occur each year [3]. The advent of direct-acting antivirals (DAAs) has been revolutionary in the advancement of HCV treatment. Interferon (IFN)-free DAAs have low side effects, short durations of treatment, and high efficacy [4-6]. However, only around 500,0 people are receiving some form of treatment within a medical institution [7]. Many HCV-infected individuals in Japan remain untreated.
HCV is also associated with extrahepatic manifestations, including glomerular disease, hematologic diseases, autoimmune disorders such as Sjögren's syndrome, and dermatologic conditions such as lichen planus (LP) and porphyria cutanea tarda (PCT) [8,9]. LP is a chronic inflammatory disease that affects the skin and mucous membranes and 0.9-1.2% of the world's population are affected [10]. Oral lichen planus (OLP) is one of the most common oral mucosal disorders and patients with OLP often visit dental offices. The rates of HCV infection in patients with OLP are high in Japan, ranging from 62% to 67.8% [11,12]. The prevalence of OLP in HCV-infected individuals increases with age [13-17]. In epidemiological studies of prospective cohorts in Japan, the prevalence was from 6.6 to 23.8% in Kyushu (X town) [13-15] and from 8.8 to 2 3.1% in Hiroshima prefecture (O town) [16,17].
There is a high prevalence of medical disorders and patients receiving polypharmacy among individuals requesting dental care [18]. In this study, we examined retrospectively the frequency of encouragement of consultation for HCV-infected liver diseases by the dentist among patients who visited a dental clinic.
Materials and Methods
Patients
We examined retrospectively oral mucosal disease and HCV infection using the information in the patients' medical records. A total of 90 consecutive patients, 23 men and 67 women, had checkups for specialized outpatient treatment for oral mucosal diseases at the Tsuji Dental & Oral Surgery Clinic in Japan from May 1, 2015 to February 28, 2017 Table 1. The 90 patients ranged in age from 35 to 89 years, with an average age of 68.9±13.1 years. We interviewed each patient to determine their major complaint, their clinical history, systemic diseases, including liver disease, offered testing for HCV and HBV infection, the medical history of family members, and primary physician.
Evaluation of liver disease
Because there were no suitable facilities in our dental clinic, we were unable to cARGHy out any blood tests. Therefore, we obtained such information in cooperation with a medical institution. As for the patients with liver disease, diagnosis of liver disease and information of viral hepatitis were provided by a hepatologist as the primary physician. The patients in whom the presence or absence of liver disease was unknown were examined carefully for liver disease by the hepatologist, with their consent. Liver function tests and ultrasonographic examinations were performed in each medical institution to investigate the shape of the liver and search for space occupying lesions. Computed tomography (CT) was performed on some patients.
Anti-HCV and serum HCV RNA was measured using a chemiluminescent enzyme immunoassay (CLEIA) kit (Lumipulse IIHCV, Fujirebio Inc., Tokyo, Japan) and a quantitative polymerase chain reaction (PCR)assay (COBAS AMPLICOR HCV MONITOR v2.0Test, COBAS AmpliPrep/COBAS Taq-Man HCV Test; Roche Molecular Systems, New Jersey, US)respectively. Hepatitis B surface antigen (HBsAg) was assayed by a chemiluminescent immunoassay (CLIA) kit (Architect™, HBsAg QT, Dainabot Co. Ltd., Tokyo, Japan).
Ethical considerations
The study was approved by the Ethics Committee of Saga University (reference number: 29-20) in accordance with the Declaration of Helsinki. The study received ethical approval for the use of an opt-out methodology, based on unbiased information.
Statistical analysis
All data are expressed as mean±standard error. Statistical analyses were performed by Welch's t test, with p<0.05 considered to be statistically significant. Statistical analyses were conducted using JMP Version 11.1.1 software (SAS Institute, Cary, NC, USA).
Results
Oral mucosal diseases in the 90 patients
A total of 120 diseases were diagnosed in the 90 patients. The most common disease was OLP (38/90, 42.2%) Table 1. The other oral diseases were: leukoplakia (7/90, 7.8%), head and neck squamous cell carcinoma (SCC) (5/90, 5.6%), aphthous stomatitis (2/90, 2.2%), xerostomia (13/90, 14.4%), Sjogren's syndrome (4/90, 4.4%), oral candidosis (8/90, 8.9%), traumatic ulcer of the tongue (6/90, 6.7%), angular stomatitis (2/90, 2.2%), cheilitis granulomatosa (1/90, 1.1%), epithelial hyperplasia (2/90, 2.2%), oral dyskinesia (2/90, 2.2%), burning mouth syndrome (13/90, 14.4%), mucous cyst (2/90, 2.2%), oral benign tumor (3/90, 3.3%), trigeminal neuralgia (1/90, 1.1%), taste disorder (3/90, 3.3%), fissured tongue (2/90, 2.2%), geographic tongue (2/90, 2.2%), disappearance of the lingual papilla (1/90, 1.1%), temporomandibular disorder (1/90, 1.1%), bruxism (1/90, 1.1%), and normal membrane (1/90, 1.1%).
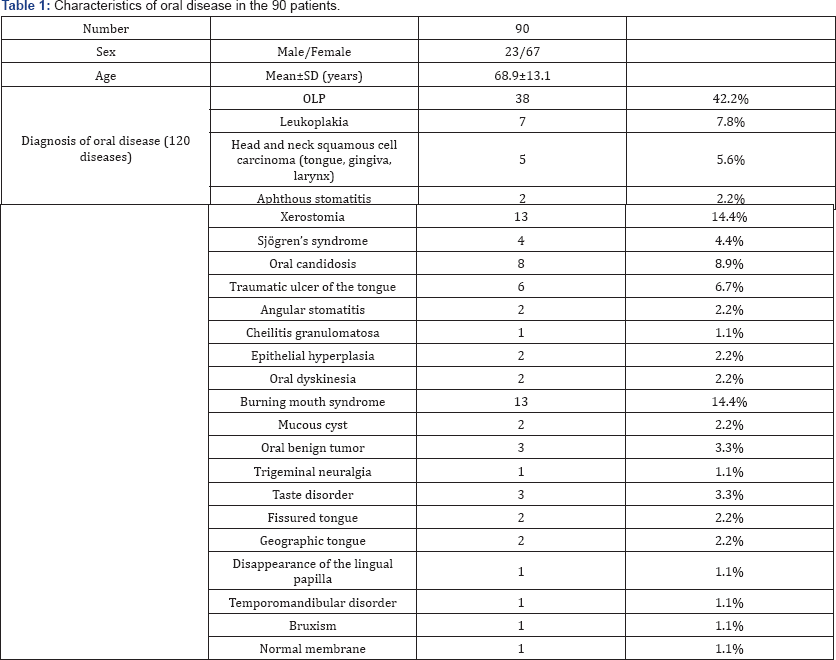
*OLP: Oral Lichen Planus
Liver diseases of the 90 patients
The numbers of patients tested for anti-HCV antibody and HBsAg were 51 (56.7%) and 47 (52.2%), respectively Table 2. The rates of anti-HCV antibody and HBsAg positivity were 29.4% (15/51) and 0% (0/47), respectively. Twenty three patients (25.6%) had some form of liver disease, of whom six (26.1%) suffered from chronic hepatitis type C (CH-C), one (4.3%) from CH-C and alcoholic liver disease, five (21.7%) from CH-C with SVR, one (4.3%) from HCV-related liver cirrhosis (LC-C), one (4.3%) from LC-C and under treatment for HCC, one (4.3%) from LC-C and post-HCC, one (4.3%) from chronic hepatitis B (CH-B), one (4.3%) from past CH-B, one (4.3%) from primary biliary cirrhosis (PBC), two (8.7%) from fatty liver, one (4.3%) from LC secondary to non-alcoholic steatohepatitis (NASH-LC), one (4.3%) from a liver cyst, and one (4.3%) from alcoholic liver disease.
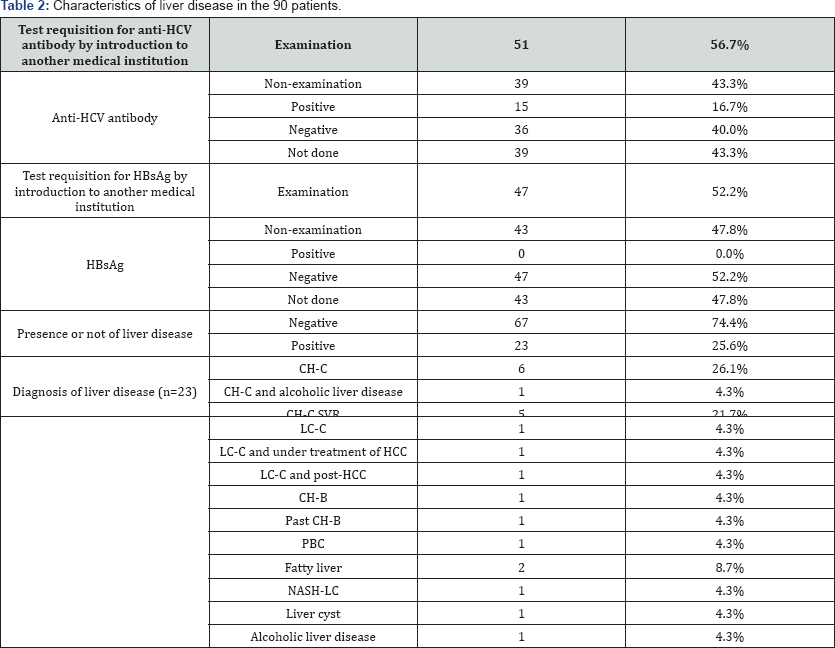
*CH-C: Chronic Hepatitis C; SVR: Sustained Virological Response; LC-C: HCV-Related Liver Cirrhosis; HCC: Hepatocellular Carcinoma; CH-B: Chronic Hepatitis Type B; PBC: Primary Biliary Cirrhosis; NASH: Non-Alcoholic Steatohepatitis.
Characteristics of the 15 anti-HCV antibody-positive patients
The anti-HCV antibody-positive patients were nine men and six women with an average age of 72.0±9.3 years Table 3. The most common disease was OLP (10/15, 66.7%, P=0.0126). One patient (an 81-year-old female, patient no.3 in Table 3) bled bilaterally from her buccal mucosa and her lower lip because of exacerbation by IFN therapy and had worsening pain with weight loss and a poor quality of life. The second most common disease was head and neck SCC (2/15, 13.3%). One patient (a 77-year-old male, patient no.6 in Table 3) was post-operative laryngeal cancer, and another (79-year-old male, patient no.11 in Table 3) was post-operative tongue cancer
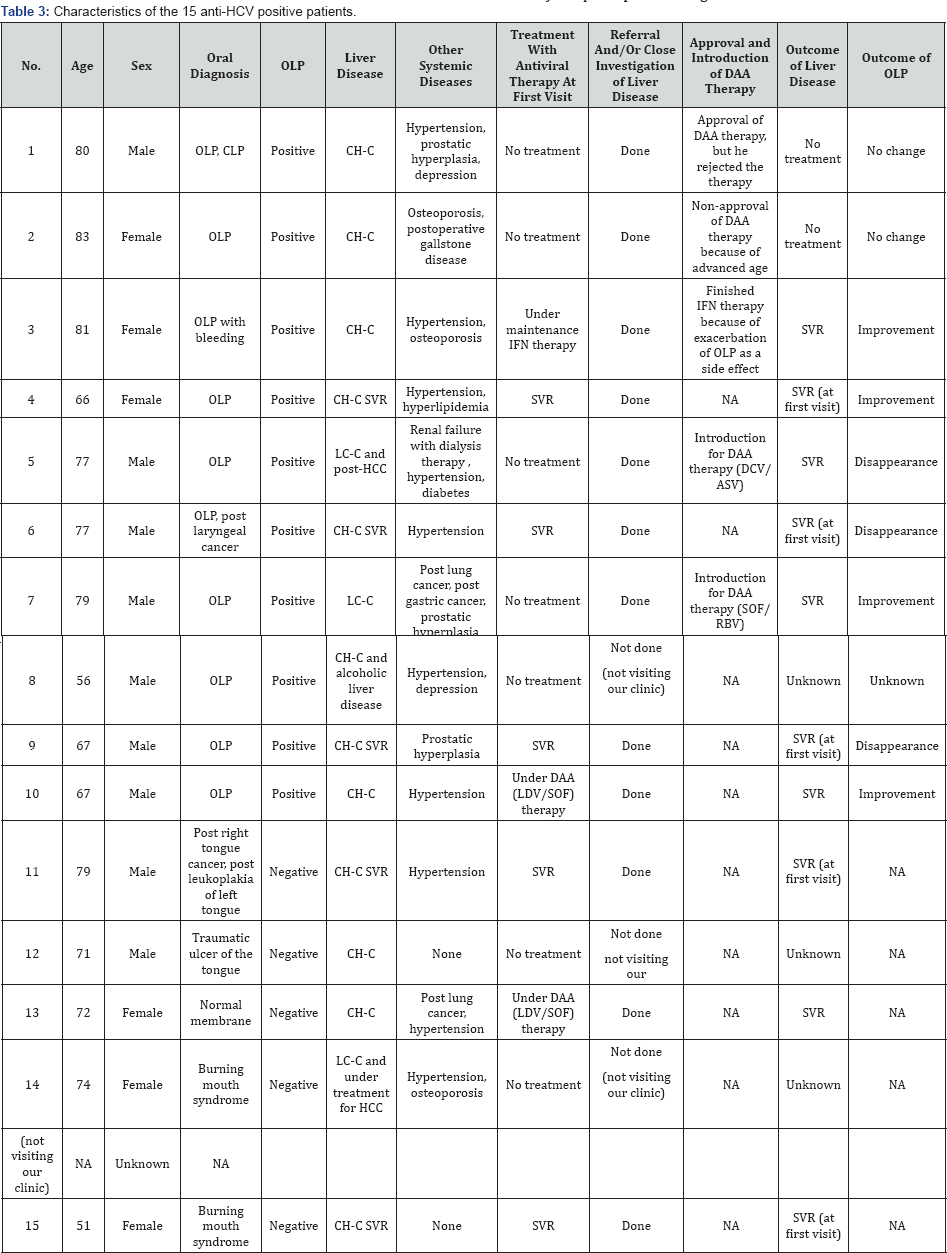
*OLP: Oral Lichen Planus; CLP: Cutaneous Lichen Planus; CH-C: Chronic Hepatitis C; SVR: Sustained Virological Response; LC-C: HCV-Related Liver Cirrhosis; HCC: Hepatocellular Carcinoma; DAA: Direct-Acting Antiviral; LDV/SOF: Ledipasvir And Sofosbuvir: DCV/ASV, Daclatasvir and Asunaprevir; SOF/RBV: Sofosbuvir and Ribavirin; NA, Not Applicable.
Their liver diseases included CH-C (n=6, 40%), CH-C and alcoholic liver disease (n=1, 6.7%), CH-C with SVR following antiviral therapy (n=5, 33.3%), LC-C (n=1, 6.7%), LC-C and under treatment of HCC (n=1, 6.7%), and LC-C and post-HCC (n=1, 6.7%). When the 15 patients were first seen at our dental clinic, treatment with antiviral therapy such as IFN or DAAs was as follows; SVR, n=5(66.7%); under DAA therapy, n=2(13.3%); under maintenance IFN therapy, n=1(6.7%); no treatment, n=7(46.5%).
Twelve patients (80%) received referral and/or close investigation of liver disease by a hepatologist. Three (20%) did not receive this because they failed to attend after consulting our clinic once. Of these 12 patients, we encouraged liver treatment for five patients; four (nos. 1, 2, 5, and 7) who did not receive antiviral therapy and one (no. 3) whose OLP was exacerbated as a side effect of IFN therapy. Two of five patients (nos. 5 and 7) received DAA therapy for the first time and one patient (no. 3) finished IFN therapy.
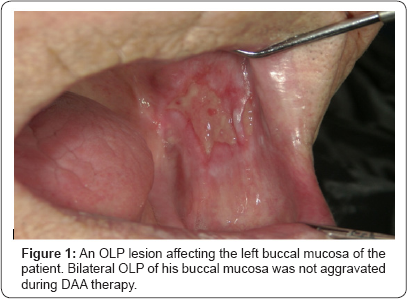
Patient no. 5 in Table 3 received DAA treatment involving a 24-week course of daclatasvir (DCV) and asunaprevir (ASV), while receiving dialysis treatment, with successful eradication of HCV. Patient no. 7 in Table 3 was diagnosed with HCV infection for the first time. He received DAA treatment involving a 12-week course of sofosbuvir (SOF) and ribavirin (RBV), and achieved SVR (Figure 1). The patient of no. 3 also achieved SVR.
The remaining two patients did not receive DAA therapy, one (no. 1) was approved for DAA therapy but rejected the therapy and the other (no. 2) was not approved for DAA therapy because of advanced age. Patient of no. 1 said that he felt insecure about remembering to take the medicine every day and declined DAA therapy.
Outcome of OLP In patients for whom treatment of liver disease was recommended, leading to SVR
When 10 HCV-infected patients with OLP were first seen at our dental clinic, treatment with antiviral therapy such as IFN or DAAs was as follows; SVR, n=3(30%); under DAA therapy, n=1(10%); under maintenance IFN therapy, n=1(10%); no treatment, n=5(50%) (Table 3). Three untreated patients for who treatment was recommended achieved SVR. The symptoms of OLP subsided in these three patients; the lesions resolved in one (no. 5, Table 3) and improved in two (nos. 3 and 7, Table 3) after SVR24.
Discussion
HCV causes extrahepatic manifestations, as well as liver disease [8,9]. OLP and oral cancer are representative extrahepatic manifestations [11,12,19,20]. Assessing the risk for head and neck cancers, researchers found that patients with HCV infection had a 2.4 times greater risk for oral cancers, 2.04 times greater risk for oropharynx cancers and 4.96 times greater risk for laryngeal cancers [20] than uninfected individuals. A metaanalysis showed a significant association between HCV infection and OLP malignant transformation [21]. We identified genetic variants associated with HCV-positive OLP in the Japanese and Italian populations: HLA class II genes, NRP2, and 1GFBP4 loci [22].
In this study, a dentist requested a detailed evaluation of potential liver disease and recommended intervention for liver treatment in another medical institution with a full-time hepatologist. As a result, among the OLP patients who consulted this dental clinic we identified a new HCV-infected patient and led an untreated HCV-infected patient to SVR. A dentist may act in the role of gatekeeper for liver disease. This study may be the first report of a dentist playing this role.
In Japan, most patients with OLP are treated in a dental clinic. However, because awareness that OLP is an extrahepatic manifestation of HCV infection is low among Japanese dentists, it is rare that a dentist requests that a patient with OLP undergoes a detailed evaluation of liver disease by a hepatologist. Furthermore, it is rare that a general dentist cooperates clinically with a hepatologist.
Until 2013, IFN-based regimens were the standard treatment for hepatitis C in Japan. OLP was reported to be frequently exacerbated by IFN treatment [23,24]. In this study we report OLP with bleeding during IFN therapy. In 2014, the first IFN-free and all-oral regimen, a nonstructural protein 3 (NS3)/nonstructural protein 4A (NS4A) protease inhibitor and a nonstructural protein 5A (NS5A) inhibitor, in combination, was initiated in Japan [4]. In Japan, DCV/ASV for 24 weeks, SOF/ ledipasvir (LDV) for 12 weeks, ombitasvir (OBV)/paritaprevir (PTV)/ritonavir (r) for 12 weeks, elbasvir/grazoprevir for 12 weeks, and DCV/ASV/beclabuvir for 12 weeks are approved to treat patients with genotype-1 HCV, whereas SOF/RBV for 12weeks and OBV/PTV/r plus RBV for 16 weeks are currently approved for genotype-2 HCV patients [25]. OLP in HCV-infected individuals was reported to be improved by these IFN-free DAAs [26-28].
Dental health care workers are at risk of contracting HCV because HCV is detectable in the saliva of patients with chronic hepatitis C [29]. Infection control is critical in dental institutions. HCV infection is the nation's most common infection. Approximately 1.5 to 2 million Japanese individuals are infected with HCV and approximately one million are untreated. In this country, a system of efficient examination has not yet been developed. If dentists encourage examination and treatment of hepatitis through dental and medical cooperation, we may discover and treat patients with untreated hepatitis. Guidelines on DAA therapy for the treatment of extrahepatic manifestations are expected to come into effect. Furthermore, it is necessary to emphasise the fact that OLP is a disease associated with HCV
Conclusion
In this study, we examined retrospectively oral mucosal disease and HCV infection using the medical record information of 90 patients who consulted a general dental clinic. Among 51 patients who could be examined for the presence or absence of HCV infection, the incidence of that infection was 29.4% (15/51). Untreated HCV cases and an OLP case exacerbated by IFN received treatment were encouraged by the dentist to seek advice regarding their liver disease. General dentists could be gatekeepers for the health-care system, especially for untreated, HCV-infected individuals. In the future, we intend to conduct further studies involving larger populations.
Acknowledgement
This study was supported in part by a Grant-in-Aid for Scientific Research (C) (No.17K12012) from the Ministry of Education, Culture, Sports, Science and Technology of Japan. We thank Dr. Michio Sata (Kurume University School of Medicine, and Nishinihon Hospital) for advice.
Conflict of Interest
YN is a member of a department funded by Nishinihon Hospital. The remaining author discloses no conflicts.
References
- WHO (2017) Global hepatitis report, World Health Organization.
- WHO (2016) Combating hepatitis B and C to reach elimination by 2030.
- Uemura M, Sasaki Y, Yamada T, Gotoh K, Eguchi H, et al. (2014) Serum antibody titers against hepatitis C virus and postoperative intrahepatic recurrence of hepatocellular carcinoma. Ann Surg Oncol 21(5): 17191725.
- Kumada H, Suzuki Y, Ikeda K, Toyota J, Karino Y, et al. (2014) Daclatasvir plus asunaprevir for chronic HCV genotype 1b infection. Hepatology 59(6): 2083-2091.
- Omata M, Nishiguchi S, Ueno Y, Mochizuki H, Izumi N, et al. (2014) Sofosbuvir plus ribavirin in Japanese patients with chronic genotype 2 HCV infection: an open-label, phase 3 trial. J Viral Hepat 21(11): 762768.
- Mizokami M, Yokosuka O, Takehara T, Sakamoto N, Korenaga M, et al.
- Tanaka J, Koyama T, Mizui M, Uchida S, Katayama K, et al. (2011) Total numbers of undiagnosed cARGHiers of hepatitis C and B viruses in Japan estimated by age- and area-specific prevalence on the national scale. Intervirology 54(4): 185-195.
- Negro F, Forton D, Craxi A, Sulkowski MS, Feld JJ, et al. (2015) Extrahepatic morbidity and mortality of chronic hepatitis C. Gastroenterology 149(6): 1345-1360.
- Ferri C, Ramos Casals M, Zignego AL, Arcaini L, Roccatello D, et al.
- Lozada Nur F, Miranda C (1997) Oral lichen planus: epidemiology clinical characteristics, and associated diseases. Semin Cutan Med Surg 16(4): 273-277.
- Nagao Y, Sata M, Tanikawa K, Itoh K, Kameyama T (1995) Lichen planus and hepatitis C virus in the northern Kyushu region of Japan. Eur J Clin Invest 25(12): 910-914.
- Nagao Y, Sata M (2012) A retrospective case-control study of hepatitis C virus infection and oral lichen planus in Japan: association study with mutations in the core and NS5A region of hepatitis C virus. BMC Gastroenterol 12: 31.
- Nagao Y, Sata M, Fukuizumi K, Tanikawa K, Kameyama T, et al. (1997) High incidence of oral precancerous lesions in a hyperendemic area of hepatitis C virus infection. Hepatol Res 8(3): 173-177.
- Nagao Y, Sata M, Fukuizumi K, Ryu F, Ueno T, et al. (2000) High incidence of oral lichen planus in an HCV hyperendemic area. Gastroenterology 119(3): 882-883.
- Nagao Y, Kawaguchi T, Tanaka K, Kumashiro R, Sata M (2005) Extrahepatic manifestations and insulin resistance in an HCV hyperendemic area. Int J Mol Med 16(2): 291-296.
- Nagao Y, Tanaka J, Nakanishi T, Moriya T, Katayama K, et al. (2002) High incidence of extrahepatic manifestations in an HCV hyperendemic area. Hepatol Res 22(1): 27-36.
- Nagao Y, Myoken Y, Katayama K, Tanaka J, Yoshizawa H, et al. (2007) Epidemiological survey of oral lichen planus among HCV-infected inhabitants in a town in Hiroshima Prefecture in Japan from 2000 to 2003. Oncol Rep 18(5): 1177-1181.
- Fernandez Feijoo J, Garea Goris R, Fernandez Varela M, Tomás Carmona I, Diniz Freitas M, et al. (2012) Prevalence of systemic diseases among patients requesting dental consultation in the public and private systems. Med Oral Patol Oral Cir Bucal 17(1): e89-e93.
- Nagao Y, Sata M, Tanikawa K, Itoh K, Kameyama T (1995) High prevalence of hepatitis C virus antibody and RNA in patients with oral cancer. J Oral Pathol Med 24(8): 354-360.
- Mahale P, Sturgis EM, Tweardy DJ, Ariza Heredia EJ, Torres HA (2016) Association between hepatitis C virus and head and neck cancers. J Natl Cancer Inst 108(8).
- Aghbari SMH, Abushouk AI, Attia A, Elmaraezy A, Menshawy A, et al. (2017) Malignant transformation of oral lichen planus and oral lichenoid lesions: A meta-analysis of 20095 patient data. Oral Oncol 68: 92-102.
- Nagao Y, Nishida N, Toyo Oka L, Kawaguchi A, Amoroso A, et al. (2017) Genome-wide association study identifies risk variants for lichen planus in patients with hepatitis C virus infection. Clin Gastroenterol Hepatol 15(6): 937-944.
- Nagao Y, Sata M, Ide T, Suzuki H, Tanikawa K, et al. (1996) Development and exacerbation of oral lichen planus during and after interferon therapy for hepatitis C. Eur J Clin Invest 26(12): 1171-1174.
- Grossmann Sde M, Teixeira R, de Aguiar MC, do Carmo MA (2008) Exacerbation of oral lichen planus lesions during treatment of chronic hepatitis C with pegylated interferon and ribavirin. Eur J Gastroenterol Hepatol 20(7): 702-706.
- Tamori A, Enomoto M, Kawada N (2016) Recent advances in antiviral therapy for chronic hepatitis C. Mediators Inflamm 2016(2016): 11.
- Nagao Y, Kimura K, Kawahigashi Y, Sata M (2016) Successful treatment of hepatitis C virus-associated oral lichen planus by interferon-free therapy with direct-acting antivirals. Clin Transl Gastroenterol 7(7): e179.
- Misaka K, Kishimoto T, Kawahigashi Y, Sata M, Nagao Y (2016) Use of direct-acting antivirals for the treatment of hepatitis C virus-associated oral lichen planus: A case report. Case Rep Gastroenterol 10(3): 617622.
- Yoshikawa A, Terashita K, Morikawa K, Matsuda S, Yamamura T, et al. (2017) Interferon-free therapy with sofosbuvir plus ribavirin for successful treatment of genotype 2 hepatitis C virus with lichen planus: a case report. Clin J Gastroenterol 10(3): 270-273.
- Nagao Y, Seki N, Tamatsukuri S, Sata M (2000) Detection of hepatitis C virus in saliva before and after scaling of dental calculus. Kansenshogaku Zasshi 74(11): 961-965.






























