Gallbladder Duplication, Annular Pancreas and Duodenal Stenosis in a Child with Noonan Syndrome
Izabela Jastrzebska1* and Krzysztof Fyderek2
Department of Internal Medicine and Gerontology, Jagiellonian University Medical College, Poland
2Department of Gastroenterology and Nutrition, Jagiellonian University Medical College, Poland
Submission: February 19, 2017; Published: June 26, 2017
*Corresponding author: Izabela Jastrzebska, Department of Internal Medicine and Gerontology, Jagiellonian University Medical College ul. Sniadeckich 10, 30-962 Krakow, Poland, Tel: 0048124248800; Fax: 004812 4248854; Email: izabela.l.jastrzebska@uj.edu.pl
How to cite this article: Izabela J, Krzysztof F. Gallbladder Duplication, Annular Pancreas and Duodenal Stenosis in a Child with Noonan Syndrome. Adv Res Gastroentero Hepatol 2017; 6(2): 555682. DOI: 10.19080/ARGH.2017.06.555682.
Abstract
Gallbladder duplication is rare congenital malformation. There is no report of gallbladder duplication or other gastrointestinal tract malformations in patients with Noonan syndrome. We present a child with Noonan syndrome, gallbladder duplication, annular pancreas and duodenal stenosis. The presumptive diagnosis of gallbladder duplication was established on the basis of ultrasonographic examination. Endoscopy revealed the presence of septum in stomach fundus, antrum malformation and duodenal duplication with two separate duodenal papillas. Wide spectrum of diagnostic procedures is needed to establish the diagnosis of gastrointestinal malformations. It is especially important if you plan any surgery.
Keywords: Duodenal obstruction; Gallbladder; Gastrointestinal tract; Congenital
Introduction
Noonan syndrome occurs in about one per 2000 live births [1]. The males and females are affected equally. The disorder is usually sporadic, but presents also with dominant inheritance. The main features of Noonan syndrome are characteristic facial changes, such as: triangular face, hypertelorism, epicanthus, downward palpebral fissures, ptosis, micrognathia, low-set ears with thickened helices; webbed neck; congenital heart disease (in 30-50%); short stature; chest and vertebral deformities; delayed puberty and sometimes bleeding diatheses [1,2]. Moderate mental retardation may our in 25% of the patients [1,2]. The patients with Noonan syndrome have normal kariotypes. The gene responsible for the disorder was mapped to 12q24.1 [3].
Congenital malformations presented in patients with Noonan syndrome include congenital heart diseases, renal anomalies, skeletal deformities and other but there is no report of gallbladder and duodenal duplication in a patient with Noonan syndrome. We present the first case of such gastrointestinal malformation in a child with Noonan syndrome.
Case Presentation
A 8, 5-year-old boy presented with a history of abdominal pain, nausea, vomiting, heartburn, dysphagia and anorexia. He suffers from asthma and allergy and has been treated with inhaled corticosteroids, long-acting inhaled beta 2-agonists and antihistaminics from 3 years. Physical examination showed slight growth retardation (hight <0,9SD); microcephaly (head circumference <1,5SD); facial asymmetry with characteristic facial changes prominent on the right side, such as: triangular face, downward slanted palpebral fissures, ptosis, low-set ears with thickened helices; webbed neck on the right side, scapula alata on the right side, scoliosis, heart murmur and bradycardia. Laboratory findings, which included white blood cell count, red blood cell count, transaminases, amylase clotting tests and stool examination, were normal. 24-hour pH monitoring showed mild gastroesophageal reflux. Esophageal manometry demonstrated esophageal motility disturbances, with the presence of more than 45 % of simultaneous contractions in the distal esophageal body and low-amplitude esophageal peristalsis. Ultrasonography revealed two structures in the gallbladder fossa. The presumptive diagnosis of gallbladder duplication was made. Repeated ultrasonography showed two gallbladders with two separate cystic ducts. Gastroscopy showed septum in stomach fundus, wide open pylorus, duodenal malformation, with suspicion of duodenal duplication or duodenal diverticulum and two separate duodenal papillas. Upper gastrointestinal tract radiographic examination with contrast established the diagnosis of duodenal duplication. Contrast enhanced computer tomography of the abdomen revealed the presence of annular pancreas, separated inferior part of the spleen and confirmed the diagnosis of gallbladder and duodenal duplication. Magnetic resonance cholangiography (MRCP) was made to establish the type of gallbladder duplication and to demonstrate the presentation of bile and pancreatic ducts. Because of small caliber of the cystic ducts and their openings exact determination of the type of gallbladder duplication was not possible. The evaluation of MRCP was also difficult because of abnormal anatomic presentation of the pancreas and duodenum. Since the child still suffered from abdominal pain and vomiting preparations for surgery were made. To preoperatively well establish the anatomic presentation of the gastrointestinal malformation endoscopic retrograde cholangiopancreatography (ERCP) was performed. Catheterization of one of the duodenal papillas, localized on the edge of the wide open pylorus, showed short pancreatic duct with small pancreas. Catheterization of another duodenal papilla, localized in duodenum showed two gallbladders, laying side by side. The bile outflow from both of them was good (Figure 1).
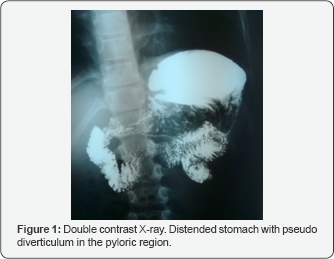
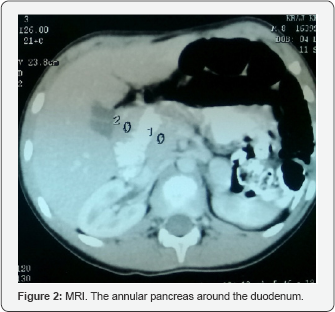
The boy's phenotypic features were consistent with Noonan syndrome. The dermatoglyphs of the boy finger tips and right hand were abnormal. The karyotype was normal. The skeletal age was 6 years of age. Echocardiography did not reveal congenital heart defects. Family history of genetic disorders or congenital malformations was negative. In the opinion of the consulting clinical geneticist the boy presented with Noonan syndrome (Figure 2). The patients has been qualified for surgical intervention due to recurrent vomiting, abdominal pain and the confirmation of duodenal obstruction in the CT and MRI scans.
The diagnosis of annular pancreas has been confirmed during the laparothomy. In accordance with the pictures obtained during the upper gastrointestinal tract radiography, the duodenal obstruction was placed in the descending part of duodenum. A duodenoplasty (Heineke-Mikulicz type) was performed. As the bile flow during ERCP was completely undisturbed and the second duodenal papilla drained the pancreas the surgical intervention do not involved the gallbladder duplication or duplication of the duodenal papillas, due to the clinical irrelevance of these congenital malformations. The postoperative recovery was uneventful and the patient was discharged on the tenth day after surgery. No recurrence of gastrointestinal tract obstruction has been observed during the one year follow-up. The patient has the growth retardation due to the Noonan syndrome, but he has no more gastrointestinal symptoms (Figure 3).
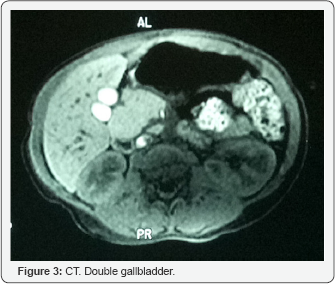
Discussion and Conclusion
Presence of feeding difficulties and failure to thrive in children with Noonan syndrome was previously described [4]. It seems to be a common finding in this group of patients. Poor growth and malnutrition of many of the children with Noonan syndrome results probably from the foregut dysmotility. Most of the patients described in this study required nasogastric tube for feeding. Gastroesophageal reflux was detected in significant percentage of the patients. Our patient also presented with mild gastroesophageal reflux and with significats disturbances of esophageal motility. The authors of cited study did not investigate esophageal motility, so there is no evidence of similar findings of esophageal dysmotility, as noted in our patient. Two of the patients described in this study had midgut malrotation, which shows that probably gastrointestinal malformations are more common in this group of patients that it is known [4].
Noonan syndrome is rather rare genetic disorder, on the other hand gallbladder and duodenal duplication is very rare congenital malformation. So the coincidence of gallbladder and duodenal duplication, and Noonan syndrome was not previously described.
Gallbladder duplication occurs in about one per 4000 autopsies [5]. According to the classification presented by Boyden there are three types of gallbladder duplications: bilobed gallbladder, duplicated gallbladder with two different cystic ducts, uniting before entering the common bile duct, known as “Y-shaped” type and two separate gallbladders with two cystic ducts emptying separately into the common bile duct, known as “H-shaped” type [5].
Previously the diagnosis of gallbladder duplication was usually made during surgery but also nowadays is happens to find unexpectedly accessory gallbladder during cholecystectomy [6].Gallbladder duplication is more frequently found in adults than in children. The common use of ultrasonography increased the incidence of accidental findings of gallbladder duplication but ultrasonography is not sufficient to establish the diagnosis
Differential diagnosis for two cystic structures in the gallbladder fossa include: gallbladder duplication, gallbladder fold, phrygian cap, focal adenomyomatosis, intraperitoneal fibrous (LADD's) bands, choledochal cyst, pericholecystic fluid, and gallbladder diverticula [8]. Especially difficult is to distinguish during ultrasonography bilobed gallbladder from true duplication [7]. Ultrasonography was also not sufficient to establish the diagnosis of gallbladder duplication in presented case report. It is especially difficult to visualize the cystic ducts and differentiate between the three known types of gallbladder duplication. It is especially important before surgery. Magnetic resonance cholangiography (MRCP) was described as a good method to differentiate the type of gallbladder duplication [7]. However in above presented patient it did not reveal the presentation of cystic ducts. Endoscopic retrograde cholangiopancreatography (ERCP) was necessary to demonstrate the opening of pancreatic and common bile duct in duodenum, as well as gallbladder and cystic ducts anatomy.
The incidence of duodenal duplication is also rare (one per 100 000 births) [9]. It is usually found in children. There are also reports of prenatal diagnosis of duodenal duplication [10].As with gallbladder duplication, exact preoperative diagnosis is necessary to avoid later complications. In our patient upper gastrointestinal tract radiographic examination with contrast and contrast enhanced computer tomography of the abdomen allowed to established the diagnosis of duodenal duplication.
The symptoms present in our patient, such as: abdominal pain, nausea,vomiting, heartburn, dysphagia could have been induced only by foregut dysmotility, earlier described in patients with Noonan syndrome [4]. However after careful examination the diagnosis of coexistent gallbladder and duodenal duplication was established. Only wide spectrum of diagnostic procedures allowed establishing the anatomic presentation of gallbladder and duodenal duplication present in our patient.
This case report shows another, not previously described, congenital gastrointestinal malformation, which can be probably find not only in patients with Noonan syndrom.
Consent
The parents of the patient have given informed consent for the case report to be published.
Competing Interest and Source of Funding
The authors declare that they have no competing interests. No financial support has been used to prepare and publish this case report.
References
- Behrman RE, Kligeman RM, Jenson HB (2000) Nelson Textbook of Pediatrics. (16th edn), W.B. Saunders Company, Philadelphia, USA.
- EMEDICINE (2002) Noonan Syndrome.
- Jamieson CR, van der Burgt I, Brady AF, van Reen M, Elsawi MM, et al. (1994) Mapping a gene for Noonan syndrome to the long arm of chromosome 12. Nat Genet 8(4): 357-360.
- Shah N, Rodriguez M, Louis DS, Lindley K, Milla PJ (1999) Feeding difficulties and foregut dysmotility in Noonan's syndrome. Arch Dis Child 81(1): 28-31.
- Boyden EA (1926) The accessory gallbladder-an embryological and comparative study of aberrant biliary vesicles occurring in man and the domestic mammals. Am J Anat 38: 177-231.
- Gui D, Magalini S, Prete F, Sermoneta D (2002) What's right when the gallbladder's left? Surg Endosc 16(11): 1637.
- Mazziotti S, Minutoli F, Blandino A, Vinci S, Salamone I, et al. (2001) Gallbladder duplication: MR cholangiography demonstration. Abdom Imaging 26(3): 287-289.
- Goiney RC, Schoenecker SA, Cyr DR, Shuman WP, Peters MJ, et al. (1985) Sonography of gallbladder duplication and differential considerations. AJR 145(2): 241-243.
- Richer JP, Faure JP, Maillot N (2000) Duodenal duplication cyst communicating with the bile duct with a long common biliary- pancreatic channel. Eur J Surg 166(6): 504-507.
- Borgnon J, Durand C, Gourlaouen D, Sagot P, Sapin E (2003) Antenatal detection of a communicating duodenal duplication. Eur J Pediatr Surg 13(2): 130-133.






























