Chronic Ileocolic Intussusception Caused by a High Grade Non-Hodgkin B cell Lymphoma in a 36-Year-Old Patient
WGP Kanchana1*, S Hediwatta1, B Samarasinghe1 and E Siriweera2
1Department of Surgery, Teaching Hospital Peradeniya, Sri Lanka
2Department of Pathology, Teaching Hospital Peradeniya, Sri Lanka
Submission: March 20, 2017; Published: June 16, 2017
*Corresponding author:WGP Kanchana, Department of Surgery, Teaching Hospital Peradeniya, Sri Lanka, Email: pulasthi@live.com
How to cite this article: WGP Kanchana, S Hediwatta, B Samarasinghe, E Siriweera. Chronic Ileocolic Intussusception Caused by a High Grade Non-Hodgkin B cell Lymphoma in a 36-Year-Old Patient. Adv Res Gastroentero Hepatol 2017; 6(2): 555681. DOI: 10.19080/ARGH.2017.05.55581
Abstract
Case Presentation: Here we present a case of 36-year-old patient, who presented with recent history of altered bowel habits and constitutional symptoms. Endoscopy revealed invagination of distal ileum into caecum. CT scan showed a mass lesion in the caecum. Intra- operatively, an ileo-caecal intussusception with associated mesenteric lymph node mass was evident. Patient underwent right hemicolectomy with an end to end ileo-colic anastomosis. Histology revealed a high grade non-hodgkin B cell lymphoma of the caecum. Tumour had involved the full circumference of the caecum.
Discussion: Chronic Intussusception is a rare entity and its presentation is atypical to that of an acute one. This entity in adults is even rarer and accurate diagnosis is challenging. Surgical treatment allowed accurate diagnosis, reduction of tumour volume and relieving of gastrointestinal symptoms.
Introduction
Intussusception can be defined as telescoping of a proximal bowel loop into a more distal bowel segment [1-5]. It is commonly seen in infants and toddlers [5]. Chronic Intussusception is a rare entity and its presentation is atypical to that of an acute one [4]. This entity in adults is even rarer and accurate diagnosis is challenging [6,7].
Case Presentation
Thirty-Six-year-old patient was investigated for 4 months' history of alteration of bowel habits, Loss of weight and Loss of appetite. He had no significant past medical history. Clinical examination revealed a mass lesion in the right ileac fossa. General examination and other system examinations were unremarkable.
Investigations
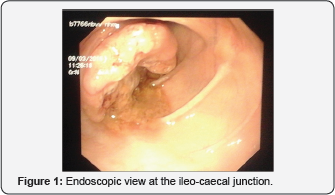
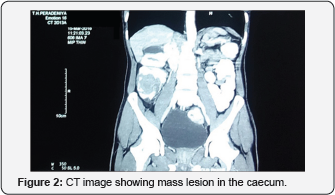
Colonoscopy revealed an invagination of the ileal mucosa or a growthat the ileocaecal junction with mucosal ulceration (Figure 1). Biopsy returned as chronic benign mucosal ulcerations. Contrast enhanced CT of the abdomen showed a mass lesion in the caecum with an adjacent mesenteric lymph node enlargement. Figure 2 shows the mass lesion involving the caecum. All other routine blood and serological investigations were unremarkable.
Treatment
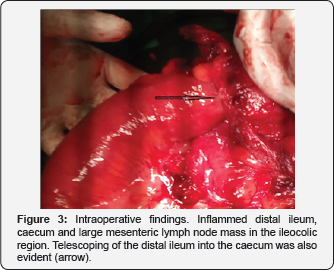
Taking into account the mass lesion seen on CT and Colonoscopy, a Laparoscopy assisted right Hemicolectomy was performed. Intraoperatively an ileocolic intussusception was evident with distal ileal segment telescoping into the caecum (Figure 3). There was an associated enlarged mesenteric lymph node mass. Distal ileum, caecum, ascending colon and proximal transverse colon was resected with adjacent mesentery to include the lymph node mass. End to end ileo-colic anastomosis was performed. Post-operative period was uneventful. Patient was discharged home on 5th postoperative day
Outcome and follow-up
Histology revealed a high grade non-hodgkin lymphoma of the colon with Ki 67 index of 80%. Tumour was 7cm in length with involvement of the full circumference of the caecal wall. Proximal and distal resection margins were away from the tumour. Tumour was invading the sub-serosa and laminapropria of the mucosa. Only one out of twenty six lymph nodes had tumour deposits. Patient was seen in the clinic at 2 weeks following surgery. He was completely symptom free. Patient was referred to the oncologist forchemotherapy.
Discussion
Intussusception in adults account only for 5% of all cases of intussusception and are commonly associated with a pathological lead point [1]. Clinical presentation of adult intussusception varies considerably [6]. Chronic partial obstruction is one of the major presenting problems as seen in this case report as well as elsewhere in literature [1,6,7]. Most common extra nodal site for non-Hodgkin type of lymphoma is gastrointestinal tract [8]. Most frequent sites of involvement are stomach followed by small intestine and ileocaecal region as in this case [2]. Treatment strategy for patients with gastrointestinal lymphomas vary with their clinical presentation, extent of the disease, age and other co-morbidities. Combination of treatment modalities such as surgery, chemotherapy, radiotherapy, immunotherapy can be used in treatment [2,9,10]. Initial surgical approach to this patient is well justified due to presence of chronic partial obstruction. Although gastrointestinal lymphomas can be managed non-surgically, surgery in this case has aided in diagnosis and reduction of tumourvolume [3].
Disclosure
The author(s) declare(s) that there is no conflict of interest regarding the publication of this paper.
Conset
Written and informed consent was taken from the patient regarding publication of this case report.
References
- Marinis A, Yiallourou A, Samanides L, Dafnios N, Anastasopoulos G, et al. (2009) Intussusception of the bowel in adults: A review. World J Gastroenterol 15(4): 407-411.
- Ghimire P, Wu GY, Zhu L (2011) Primary gastrointestinal lymphoma. World J Gastroenterol 17(6): 697-707.
- Saka R, Sasaki T, Matsuda I, Nose S, Onishi M, et al. (2015) Chronic ileocolic intussusception due to transmural infiltration of diffuse large B cell lymphoma in a 14-year-old boy: a case report. Springerplus 4: 366.
- Sutherland DM (1932) Chronic Intussusception in Children. Arch Dis Child 7: 191-192.
- Waseem M, Rosenberg HK (2008) Intussusception. PediatrEmerg Care 24(11): 793-800.
- T Azar, Berger DL (1997) Adult intussusception, Ann Surg 226(2): 134138.
- Erkan N, Haciyanli M, Yildirim M, Sayhan H, Vardar E, et al. (2005) Intussusception in adults: an unusual and challenging condition for surgeons. Int J Colorectal Dis 20(5): 452-456.
- Paryani S, Hoppe RT, Burke JS, Sneed P, Dawley D, et al. (1983) Extralymphatic involvement in diffuse non-Hodgkin's lymphoma. J ClinOncol 1(11): 682.
- Hitchcock S, Ng AK, Fisher DC, Silver B, Bernardo MP, et al. (2002) Treatment outcome of mucosa-associated lymphoid tissue/marginal zone non-Hodgkin's lymphoma, Int J Radiat Oncol Biol Phys 52(4): 1058-1066.
- Salar A, Domingo-Domenech E, Estany C, Canales MA, Gallardo F, et al. (2009) Combination therapy with rituximab and intravenous or oral fludarabine in the first-line, systemic treatment of patients with extranodal marginal zone B-cell lymphoma of the mucosa-associated lymphoid tissue type. Cancer 115(22): 5210-5217.






























