Heyde’s syndrome: Rarely heard and often missed
Deepankar Kumar Basak1*, Richmond Ronald Gomes2 and Md Samsul Arfin3
1Specialist-Gastroenterology, Square Hospitals Ltd., Bhangladesh
2Assistant Professor, Internal Medicine, Ad-din Sakina Medical College & Hospital, Bhangladesh
3Gasroenterology, Square Hospitals Limited., Bhangladesh
Submission: November 11, 2016; Published: January 19, 2017
*Corresponding author: Deepankar Kumar Basak, MBBS, FCPS (Medicine), Specialist-Gastroenterology, Square Hospital Ltd., Dhaka, Bangladesh, Tel:0176499475; Email; deepankarbasak@gmail.com
How to cite this article:Deepankar K B, Richmond R G, Md Samsul A. Heyde’s syndrome: Rarely heard and often missed. Adv Res Gastroentero Hepatol 2017; 2(4): 555592. DOI: 10.19080/ARGH.2017.02.555592
Abstract
Bleeding from the gastrointestinal tract is very common and important problem in clinical practice. There are lots of causes of GI bleeding, but sometimes it is very difficult to locate and treat gastrointestinal bleeding. Here we discuss Heyde’s syndrome, an important cause of gastrointestinal bleeding in an elderly female patient who is also suffering from HCV related decompensated CLD with multiple myeloma. Heyde’s syndrome is now known to be gastrointestinal bleeding from angiodysplasic lesions due to acquired vWD-2A secondary to aortic stenosis, and the diagnosis is made by confirming the presence of those three things. For this, a wide range of investigations and treatment modalities are now available. One should therefore make an aggressive attempt to localize the bleeding site. Newer endoscopic technologies may prove beneficial. Aortic valve replacement is claimed to minimize or even stop the bleeding in such patients. But still there are a few reports showing gastrointestinal bleeding after aortic valve replacement. Old age and co-morbidities may create a hindrance in valve replacement or resection surgery. Some newer treatment options like hormonal and thalidomide therapy look promising but they have inadequate evidence behind them. Here, we discuss this clinical problem, strategies and evidence, areas of uncertainty, available guidelines, and our conclusions about Heyde’s syndrome.
Keywords: Heyde’s syndrome; gastrointestinal angiodysplasias; Gastrointestinal bleeding
Introduction
Angiodysplasia is the most common vascular lesion of the gastrointestinal tract, and this condition may be asymptomatic, or it may cause gastrointestinal (GI) bleeding [1]. The vessel walls are thin, with little or no smooth muscle, and the vessels are ectatic and thin. It is a degenerative lesion of previously healthy blood vessels found most commonly in the cecum and proximal ascending colon but bleeding from proximal intestinal angiodysplasias, and nasal bleeding is also reported [2,3]. After diverticulosis, it is the second leading cause of lower GI bleeding in patients older than 60 years. An association between colonic angiodysplasia and aortic stenosis was described by Edward C Heyde et al. [4]. It is caused by the induction of Von Willebrand disease type IIA (vWD-2A) by a depletion of Von Willebrand factor (vWF) in blood flowing through the nARGHowed valvular stenosis. The existence of this syndrome was debated for a considerable period of time when finally it was shown that the gastrointestinal bleeding did actually resolve after aortic valve replacement in many such patients, thereby giving a definite credence to the existence of this syndrome [2,5]. The bleeding could be severe and the patient usually requires multiple blood transfusions. We describe a case of Heyde’s syndrome with multiple angiodysplastic lesions throughout the colon, mostly at the distal part and discuss the various challenges in the diagnosis and treatment of such patients.
Case Report
Mrs. Chaina Chakraborty, 71 year old pleasant lady, known to have multiple myeloma (MULTIPLE MYELOMA-IgG Kappa Myeloma and Beta2 Microglobulin-4.2) chronic liver disease (HCV related) with Esophageal Varices (grade 2), duodenal ulcer and aortic stenosis with IHD was admitted to SHL gastroenterology department through ER with the complaints of passage of black tARGHy stool for last five days and generalized weakness for same duration. She had previous history of hospital admission for several times in the last three months with these same complaints and received 8-10 units of blood and blood products over that period. Now her hemoglobin 5 gm/dl, Haematocrit 20.9%, TC 10.5 K/uL, Platelets 40K/uL, PT, aPTT was normal. Echocardiogram shows nARGHow LVOT with Dynamic subvalvular Aortic Stenosis Gr 78/28mmHg with no AR. Endoscopy shows grade 2 esophageal varix but no active bleeding from varix. Colonoscopy shows angiodysplastic lesions through the colon with hamorrhoids.Bleeding occur most probably from angiodysplastic lesions but we don’t see any active bleeding from any angiodysplasia. Initially patient was managed with blood transfusion with fresh frozen plasma and also platelet aphaeresis (Figure 1).

Our patient is an elderly lady with multiple co-morbidities. She was treated by thalidomide for multiple myeloma that was controlled. Two times EVL was done for HCV related decompensated CLD with feature of hypersplenism with low platelet count. Her past history of multiple episodes of lifethreatening blood loss makes it necessary to do something to prevent gastrointestinal blood loss. The options available are angiographic intervention, endoscopic intervention, intestinal resection, aortic valve replacement, and estrogen-progesterone therapy/thalidomide therapy. The patient herself along with her relatives were unwilling for any major surgical intervention due to her advanced age and the multiple comorbidities that she had, further compromising the likely outcome after the surgery. There was a high chance of more angiodysplastic lesion in small gut which is not approachable on colonoscopy and there was no capsule endoscope in our country.
Angiographic intervention is also not preferable as there is a possibility of existence of multiple unnoticed angiodysplasias, possibility of gut infarction after angiography, and the deranged renal function of the patient would be a contraindication for angiography. All these problems make it difficult to choose the best and acceptable solution for this patient like aortic valve replacement (Figure 2&3).
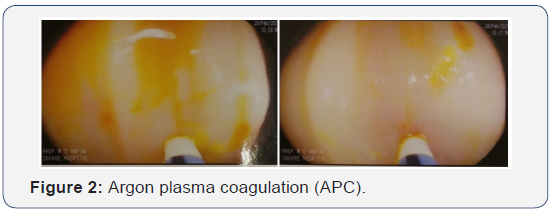
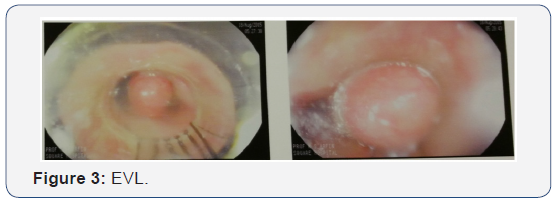
We do argon plasma coagulation (APC) of angiodysplastic lesion in colon as far as possible in 2 sessions with injection of octreotide. In this measure she was recovered well and there was no bleeding at least 1 year follow-up. After that again melaena started on/off. She was also treated by desmopressin nasal spray with cap.danazol to increase vWF with inj octreotide. This measure decreases her incidence of melaena. We offer her to do aortic valvae replacement for further management but she was not interested.
Discussion
Angiodysplasia is the most common vascular lesion of the gastrointestinal tract, and this condition may be asymptomatic, or it may cause gastrointestinal (GI) bleeding [1]. Seventyseven percent of angiodysplasias are located in the cecum and ascending colon, 15% are located in the jejunum and ileum, and the remainder is distributed throughout the alimentary tract. Nasal bleeding is also reported [2,3]. These lesions typically are nonpalpable and small (< 5 mm). Angiodysplasia may account for approximately 6% of cases of lower GI bleeding. It may be observed incidentally at colonoscopy in as many as 0.8% of patients older than 50 years. The prevalence for upper GI lesions is approximately 1-2%.Clinical presentation in patients with angiodysplasia is usually characterized by maroon-colored stool, melena, or hematochezia. Bleeding is usually low grade, but it can be massive in approximately 15% of patients. In 20-25% of bleeding episodes, only tARGHy stools are passed. Iron deficiency anemia and stools that are intermittently positive for occult blood can be the only manifestations of angiodysplasia in 10- 15% of patients. Bleeding stops spontaneously in greater than 90% of cases but is often recurrent. An association between colonic angiodysplasia and aortic stenosis was described by Edward C Heyde et al. [4].
The exact mechanism of development of angiodysplasia is not known, but chronic venous obstruction may play a role [6,7]. Increased expression of angiogenic factors, like basic fibroblast growth factor (bFGF) and vascular endothelial growth factor (VEGF), is also believed to play a role in the pathogenesis of colonic angiodysplasia [8]. In Heyde’s syndrome; it seems that bleeding occurs from pre-existing angiodysplasias in the gut. This bleeding is due to an acquired haematological defect caused by aortic stenosis [5,9]. Age-related senile tissue changes may predispose to angiodysplasia and the link between the angiodysplasia and aortic stenosis is controversial [10-12]. Various studies have described the acquired von Willebrand factor deficiency as being a reason for bleeding in Heyde’s syndrome [5,13]. The haematological defect is identified as deficiency of high molecular weight (HMW) multimers of von Willebrand factor (vWF) [14]. The high shearing force caused by blood jet in aortic stenosis uncoils the HMW multimers of vWF exposing the vWF cleavage site for ADAMST [13]. This leads to selective loss of HMW multimers of vWF due to increased proteolysis. Acquired vWF deficiency state is thus created (von Willebrand syndrome type 2A). There is an evidence showing normalisation of HMW multimers of VWF after aortic valve replacement surgery [15-18]. Heydes syndrome consists of a triad of aortic stenosis, acquired vWF deficiency and anaemia due to bleeding angiodysplasia or idiopathic bleeding [19]. The main challenge is localisation of bleeding source in these patients [17]. The bleeding source could be hidden and out of reach for conventional endoscopies.Wireless capsule endoscopy is a useful invention that helps us to visualise the small intestine. It also guides us about the route for enteroscope insertion. It is a painless and noninvasive procedure. The disadvantages of capsule endoscopy include the inability to detect all the lesions, especially in presence of active bleeding, and the inability to intervene [17,19]. The double balloon and single balloon endoscopies are described to be useful to overcome these disadvantages of capsule endoscopy [14,15]. It is claimed that double balloon and single balloon endoscopies can visualise most of the small bowel and thus enable diagnostic manoeuvres and therapeutic techniques like achieving haemostasis, performing polypectomies, stricture dilatation, and stenting. This technique produces superior quality images than capsule endoscopy. However, the cost and availability of these techniques could limit their use in developing countries. Therapeutic options for Heyde’s syndrome include aortic valve replacement, surgery, angiographic intervention, double or single balloon endoscopy,Argon plasma coagulation(APC) and medical therapy including hormonal and thalidomide therapy, octreotide [5,19]. It is claimed that aortic valve replacement reduces or even stops gastrointestinal blood loss5. Cessation of bleeding after aortic valve replacement was found to be associated with improved levels of HMW multimers of vWF after replacement. This finding strengthened the hypothesis of acquired vWF deficiency in Heyde’s syndrome. However, advanced age and co-morbidities can make this an unsuitable choice in some patients. A few case reports describe massive gastrointestinal bleeding after aortic valve replacement [16].
Thus aortic valve replacement might not be the ideal treatment in every patient of Heyde’s syndrome. Surgery and endoscopic therapy especially argon plasma coagulation are not useful in patients with diffuse angiodysplasia. Aortic stenosis and associated cardiac diseases often make patients of Heyde‘s syndrome unfit for surgery. Though double balloon endoscopy is mentioned to be able to visualise the small intestine and intervene, their cost and availability may limit their use. Angiographic intervention like embolisation of A-V malformation can lead to arterial occlusion and gangrene. It is also difficult to locate and embolise all the lesions in diffuse angiodysplasias. A few case reports, one uncontrolled trial, and recently a small double-blind, placebo-controlled, cross-over trial indicate that oestrogen-progesterone therapy may be effective in controlling severe recurrent bleeding from gastrointestinal vascular malformations [17]. Octreotide and estroprogestative treatments are the best evaluated drugs; however, no appropriate comparison on cost-effectiveness and tolerance has been performed [20]. Submucosal injection of a saline epinephrine solution followed by the application of APC has been reported [21] New endoscopic techniques such as the Olympus EVIS LUCERA variable indices of hemoglobin chart function have been developed to assess completeness of vascular mucosal ablation [22]. Super selective embolization of visceral arterial branches is central to the management of patients with lower GI bleeding, including bleeding from colonic angiodysplasia [23] Partial or complete gastrectomy for management of gastric angiodysplasia has been reported to be followed by bleeding in as many as 50% of patients. Rebleeding was attributed to other angiodysplastic lesions.Right hemicolectomy for angiodysplasia is secondline therapy after endoscopic ablation, if repeated endoscopic coagulation has failed, if endoscopic therapies are not available, and for life-threatening hemorrhage.
The mortality rate associated with surgical resection ranges from 10% to 50%. This is based on the view that surgery cARGHies a much higher risk in elderly patients, who often have multiple coexisting medical problems, including coronary artery disease, coagulopathy, and renal and pulmonary dysfunction. In a study by Meyer et al, right hemicolectomy resulted in 63% of the subjects remaining free of intestinal bleeding (mean follow-up, 3.6 y), and 37% had some degree of recurrent bleeding [24].
The Heyde’s syndrome is supposed to be one of the acquired von Willebrand factor deficiency states. The recommended guidelines for the diagnosis and management involve detection of vW factor levels, detection of antibodies against the same, and treatment with desmopressin or factor viii/vWF. These diagnostic modalities are not readily available across our country and are costly, e.g., in Bangladesh, assessment of vW factor levels may cost more than hormonal therapy for a month. There are no recommended guidelines for the management and treatment of Heyde’s syndrome. One should seek help from guidelines for management of occult gastrointestinal blood loss. Also, there should be a consideration for cardiovascular issues and haematological issues of the patient. Various treatment options are available for Heyde’s syndrome but most of them have inadequate evidence behind them. As of now, there is no universally accepted unified treatment protocol available. Recurrence of acute hemorrhage from GI angiodysplasia after hospital discharge occurred in 30% of patients after a mean follow-up (33±40 mo). In a multivariate analysis, earlier history of bleeding with a high bleeding rate, over anticoagulation, and the presence of multiple lesions were predictive factors of recurrence. Surprisingly endoscopic APC therapy was not associated with lower rates of recurrent bleeding [25].
Conclusions and Recommendations
Potentially life-threatening nature, age and co-morbidities, and poorly understood pathophysiology make Heyde’s syndrome a tough illness to treat. High index of suspicion should be kept in mind while treating aortic stenosis and gastrointestinal hemorrhage in elderly patients.Involvement of a gastroenterologist and a hematologist in treatment of such patients helps in resolving various issues pertaining to their respective fields. An aggressive attempt should be made to visualise the bleeding source. Capsule endoscopy and double balloon endoscopy may be very useful in diagnosis and treatment. Though aortic valve replacement is thought to be corrective in most of the cases, it might not be practical in all the cases. In spite of lack of strong evidence and the possibility of side-effects, hormonal therapy could prove to be an effective treatment modality in such patients. Incidentally, our patient has done well after inj octreotide & hormonal therapy with Argon plasma coagulation and her hemoglobin has been raised.
References
- Regula J, Wronska E, Pachlewski J (2008) Vascular lesions of the gastrointestinal tract. Best Pract Res Clin Gastroenterol 22(2): 313- 328.
- Warkentin TE, Moore JC (2010) Heyde’s syndrome: From controversy to mainstream. Thromb Haemost 103(2): 251-253.
- Schodel J, Obergfell A, Maass AH (2007) Severe aortic valve stenosis and nose bleed. Int J Cardiol 120(2): 21.
- Heyde EC (1958) Gastrointestinal bleeding in aortic stenosis. N Engl J
Med 259: 196.
- King RM, Pluth JR, Guiliani ER (1987) The association of unexplained gastrointestinal bleeding with calcific aortic stenosis. Ann Thorac Surg 44(5): 514-516.
- Clouse RE (1999) Vascular lesions: ectasias, tumors, and malformations. Yamada T, Alpers DH, Laine L, Owyang C, Powell DW (Eds). Textbook of Gastroenterology (3rd edn). Philadelphia, Pa: JB Lippincott 2: 2564- 2578.
- Ming SC, Goldman H. (1998) Vascular abnormalities of the gastrointestinal tract. Ming SC, Goldman H, (Eds.), Pathology of the Gastrointestinal Tract (2nd edn), Williams & Wilkins Company, Baltimore, USA, pp. 272-274.
- Junquera F, Saperas E, de Torres I, Vidal MT, Malagelada JR (1999) Increased expression of angiogenic factors in human colonic angiodysplasia. Am J Gastroenterol 94(4): 1070-1076.
- Mishra PK, Jan Kovac, John de Caestecker, Graham Fancourt, Elaine Logtens, et al. (2009) Intestinal angiodysplasia and aortic valve stenosis: lets not close the book on this association. European Journal of Cardiothoracic Surgery 35: 628-634.
- Saxena R, Sharma P (2009) Gastrointestinal Angiodysplasia and Acquired von Willebrand Syndrome: A Review of an Enigmatic Association. Journal of Coagulation Disorders 1(1): 11.
- Bhutani MS, Gupta SC, Markert RJ, Barde CJ, Donese R, et al. (1995) A prospective controlled evaluation of endoscopic detection of angiodysplasia and its association with aortic valve disease. Gastrointest Endosc 42(5): 398-402.
- Greenstein RJ, McElhinney AJ, Reuben D et al. (1986) Colonic vascular ectasias and aortic stenosis: coincidence or causal relationship? Am J Surg 151(3): 347-351.
- Massyn MW, Khan SA (2009) Heyde syndrome: a common diagnosis in older patients with severe aortic stenosis. Age and Ageing 38(3): 267- 270..
- Hui YT, Lam WM, Fong NM, Yuen PK, Lam JT (2000) Heyde’s syndrome: diagnosis and management by the novel single-balloon enteroscopy. Hong Kong Med J 15(4): 301-303.
- Yamamoto H, Sekine Y, Sato Y, Higashizawa T, Miyata T, et al. (2001) Total enteroscopy with a nonsurgical steerable double-balloon method. Gastrointest Endosc 53(2): 216-220.
- Varma P, Misra M, Radhakrishnan VV, Neelakandhan KS (2004) Fatal post-operative gastro-intestinal haemorrhage because of angiodysplasia of small intestine in aortic regurgitation. Interact Cardiovasc Thorac Surg 3(1): 118-120.
- Moshkowitz M, Arber N, Amir N, Gilat T (1993) Success of estrogenprogesterone therapy in long-standing bleeding gastrointestinal angiodysplasia. Dis Colon Rectum 36(2): 194-196.
- Pennazio M1, Eisen G, Goldfarb N; ICCE (2005) ICCE consensus for obscure gastrointestinal bleeding. Endoscopy 37(10): 1046-1050.
- Makris M (2006) Gastrointestinal bleeding in von Willebrand disease. Thromb Res 118 (Suppl 1): 13-17.
- Dray X, Camus M, Coelho J, Ozenne V, Pocard M et al. (2011) Treatment of gastrointestinal angiodysplasia and unmet needs. Dig Liver Dis 43(7): 515-522.
- Suzuki N, Arebi N, Saunders BP (2006) A novel method of treating colonic angiodysplasia. Gastrointest Endosc 64(3): 424-427.
- Hurlstone DP, Karageh M, Sanders DS (2016) The Olympus EVIS LUCERA variable indices of haemoglobin chart function: a novel technique for establishing the completeness of vascular mucosal ablation in colonic angiodysplasia. Endoscopy 38(1): 102.
- Pishvaian AC, Lewis JH (2006) Use of endoclips to obliterate a colonic arteriovenous malformation before cauterization. Gastrointest Endosc 63(6): 865-866.
- Meyer CT, Troncale FJ, Galloway S, Sheahan DG. (1981) Arteriovenous malformations of the bowel: an analysis of 22 cases and a review of the literature. Medicine (Baltimore) 60(1): 36-48.
- Saperas E, Videla S, Dot J, BayARGHi C, Lobo B, Abu-Suboh M, et al. (2009) Risk factors for recurrence of acute gastrointestinal bleeding from angiodysplasia. Eur J Gastroenterol Hepatol 21(12): 1333-1339.






























