Rate of Spontaneous Resolution of Idiopathic Ileocolic Intussusception
Roben ECZ* and Horowitz R
Northwestern University Feinberg School of Medicine, USA
Submission: May 22, 2018; Published: August 17, 2018
*Corresponding author: Emily CZR, Northwestern University Feinberg School of Medicine, USA.
How to cite this article: Roben ECZ, Horowitz R. Rate of Spontaneous Resolution of Idiopathic Ileocolic Intussusception. 2018; 7(2): 555763. DOI: 10.19080/AJPN.2018.07.555763
Keywords: Idiopathic; Ileocolic; Intussusception; Barium; Hydrostatic enema
Abbrevations: US: Ultrasound; OR: Operating Room; ED: Emergency Department
Background
Idiopathic ileocolic intussusception is a common cause of abdominal pain in young children with potential serious clinical outcomes. The gold standard for making this diagnosis is ultrasound (US) of the abdomen, and the most common next step is barium or hydrostatic enema. There is a small and underreported percentage of patients who are found to have intussusception on abdominal US but have no evidence of intussusception when they undergo enema. There is an additional small population of patients who have an irreducible intussusception with enema, who then proceed to the operating room (OR) for manual reduction and are found to no longer have intussusception. These situations are sometimes referred to as “spontaneous resolution” of intussusception and have not be thoroughly investigated. Several studies reviewing the clinical course of patients with ileocolic intussusception report on this phenomenon of spontaneous resolution and have identified spontaneous reduction rates of 0.3% to 14% [1-9]. However, these studies were retrospective reviews looking at the general outcomes of patients of all ages with all types of intussusception (ileocolic, ileoileal, and any involvement of a pathologic lead point). No specifically describes spontaneously resolved intussusceptions at the time of attempted enema, except for one small case series of four patients.10 At this time there are no studies aimed specifically at identifying the rate of spontaneous resolution of idiopathic ileocolic intussusception between the time of diagnosis and the time of attempted enema in otherwise healthy children. This information is important to know as it can inform management strategies; if there are patients whose intussusception can spontaneously reduce, this is important to identify in order to prevent those patients from receiving unnecessary invasive interventions. The objectives of this study were to identify the rate of spontaneous resolution of idiopathic ileocolic intussusception and identify features consistent among patients with spontaneous resolution.
Methods
After obtaining institutional review board approval, we performed a retrospective review of the records of all children with ileocolic intussusception seen at Children’s Memorial Hospital/Lurie Children’s Hospital from July 1, 2007 to June 30, 2015. We included all patients 3months to 36months old who had an ICD 9 or 10 diagnosis code of “intussusception,” as well as all patients who had an order in the electronic medical record for a contrast or air enema (identified by the electronic order “XR enema”). We also included all patients who were transferred to our facility with a diagnosis of intussusception or suspected intussusception using transfer diagnosis codes included the phrase “intuss.” We excluded children with a past medical history of a condition predisposing to intussusception (celiac disease, cystic fibrosis, familial polyposis syndromes), those with history of abdominal tumor or surgery, and patients who did not have intussusception diagnosed by US, CT scan, or enema. Data collected included age, gender, presence of symptoms (fever, abdominal pain, vomiting, bloody stools), presence of physical exam findings (altered mental status, abdominal tenderness, abdominal mass, knees to chest position, hemoccult positive stool), method of diagnosis (US, CT, or enema), and type of definitive management (enema, delayed repeat enema, OR reduction, OR resection, or self-resolution). The presenting symptoms and signs were compared between patients whose intussusception spontaneously reduced and those which required intervention with enema or surgery. We also compared the duration of time from symptom onset to diagnosis and ultimate outcome; symptom onset was determined using historical information documented in the medical record, and diagnosis and outcome times were determined using time stamps within the medical record.
Statistical Analysis
Demographic and clinical characteristics across outcome groups were compared using Kruskal-Wallis tests for continuous variables and chi-squared tests for categorical variables. Unknown responses for abdominal pain and vomiting were excluded from comparisons for these variables. For variables with significant omnibus tests, pairwise comparisons using Wilcoxon rank sum tests and chi-square tests were assessed. To account for multiple comparisons, Bonferroni-adjusted p-values (p<0.0167) were used to determine statistical significance. The timings of spontaneous resolution by location were compared using a two-sample test of proportions.
Results
The records of 636 children were identified and reviewed. There were 317 patients who met our inclusion criteria and we abstracted all clinical information from those records. 319 (50%) children did not meet inclusion criteria (Figure 1). The most common reason for exclusion was, absence of intussusception on imaging. An equal percentage of patients were excluded from the transferred and the directly seen groups (115/247=46% vs 204/389=52%).

Table 1 shows the main results of the chart review. Among the 317 records reviewed, the rate of spontaneous resolution of idiopathic ileocolic intussusception was 11%. Other outcomes were reduction by enema (69%), reduction in the OR (14%), and resection in the OR (6%). Overall, patients with idiopathic ileocolic intussusception were majority male (62%) and their mean age was 15.3 months. The most common presenting symptoms were abdominal pain (81%) and vomiting (72%). Interestingly, the “classic triad” of abdominal pain, vomiting, and bloody stool was only present in 17% of patients. The average time from symptom onset to diagnosis was 21hours, and the average time from diagnosis to ultimate outcome was 2.3hours.
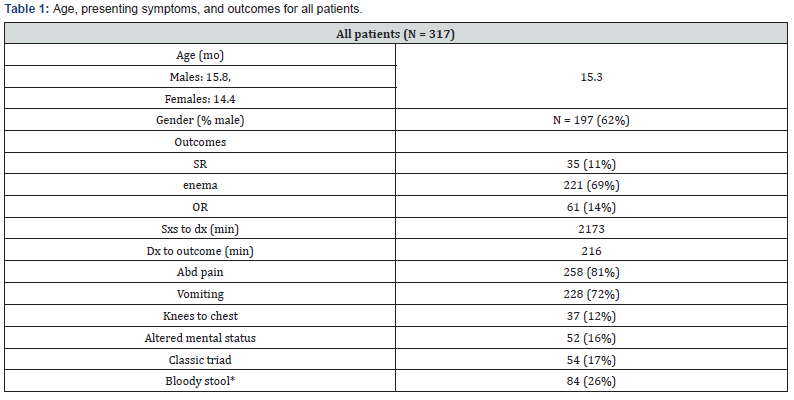
*Bloody stool refers to either a report of blood stools in the history, or documentation of hemoccult positive stool in the ED. Only 272 of 317 patients had documentation of hemoccult status, therefore this row reflects a different denominator than the other signs and symptoms.
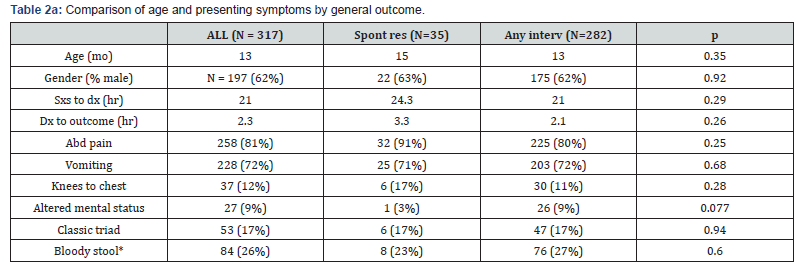
*Bloody stool refers to either a report of blood stools in the history, or documentation of hemoccult positive stool in the ED. Only 272 of 317 patients had documentation of hemoccult status, therefore this row reflects a different denominator than the other signs and symptoms.
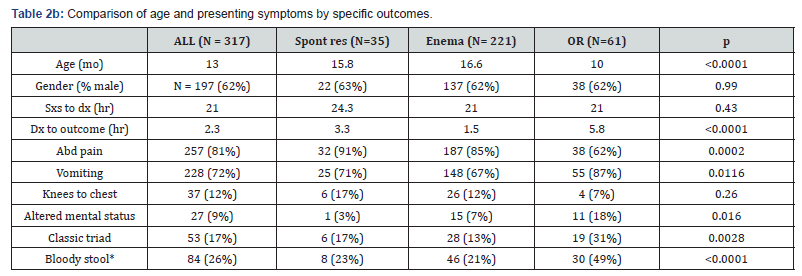
*Bloody stool refers to either a report of blood stools in the history, or documentation of hemoccult positive stool in the ED. Only 272 of 317 patients had documentation of hemoccult status, therefore this row reflects a different denominator than the other signs and symptoms.
Table 2a compares the demographic and clinical characteristics for the patients who had spontaneous resolution of their intussusception to those who required intervention of any kind. Table 2b breaks down the “any intervention” group into the two separate outcomes: enema and operative intervention. There were no statistically significant differences in age, gender, presenting symptoms, time from symptom onset to image diagnosis, and time from image diagnosis to ultimate outcome between the group that spontaneously resolved and the group that required any intervention. However, when we broke the intervention group down into its two components (enema and OR), we found some statistically significant differences. The patients who required OR intervention was younger, less commonly had abdominal pain, and more commonly had vomiting, bloody stools and altered mental status than the patients who spontaneously resolved and those whose intussusception was successfully treated by enema. They also had a longer time interval between receiving their diagnosis of intussusception and achieving their ultimate outcome.
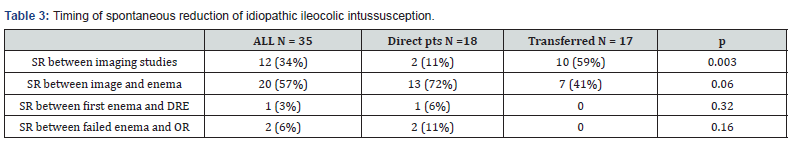
Table 3 shows the timing of spontaneous resolution relative to symptom onset, image diagnosis, and intervention. Most (57%) of spontaneous resolutions were discovered at the time of enema, after an image diagnosis had been made. The next most common time for discovery of resolution was upon obtaining a second, confirmatory, imaging study. We found a similar overall spontaneous resolution rate (10% vs 13%) between patients who presented directly to our facility compared to those who were transferred from other hospitals. However, the breakdown of the timing of the spontaneous resolution is quite different between these groups. In the patients who were transferred from outside facilities, most of the spontaneous resolutions (10/17, 59%) were discovered between the initial diagnostic imaging (at the referring hospital) and the confirmatory imaging at our hospital. The other 41% were discovered between diagnostic imaging and attempted enema. This is in contrast to the patients that were directly seen at our facility; only 11% of spontaneous resolutions were discovered between imaging studies, another 78% discovered at the time of enema, and the last 11% discovered in the OR after unsuccessful enema.
Discussion
In reviewing all patients diagnosed with idiopathic ileocolic intussusception over a 7-year period, we found a spontaneous resolution rate of 11%. There were no significant differences between the group that spontaneously resolved and the group that required either enema or OR intervention. To our knowledge, this is the first study to examine this outcome of intussusception. We believe that this rate is higher than what may have previously been assumed and has clinical significance in that it may impact the management of otherwise well children with an image diagnosis of intussusception. For example, patients with image-diagnosed intussusception who subsequently have resolution of symptoms might need to be re-imaged or observed prior to further invasive intervention. Additionally, patients who have seem to have all of the classic symptoms of intussusception but have negative imaging and no other positive findings may be considered to have had a self-resolved intussusception and be managed accordingly.
A spontaneous resolution rate of 11% is within the range of what may have been expected based on the existing literature about idiopathic ileocolic intussusception. No study has ever looked specifically at the rate of spontaneous resolution of idiopathic ileocolic intussusception in otherwise healthy individuals. Several retrospective reviews of patients undergoing enema after image diagnosis of intussusception have found spontaneous resolution rates of 0.8% - 10.9% [1-3, 6, 8-9]. However, these studies differ from ours in that they only looked at children undergoing enema and did not include any children undergoing repeat, confirmatory imaging. Additionally, several of these studies included patients with ileoileal intussusceptions, as well as those with pathologic lead points. Hryhorczuk et al. [7] found a 4.5% spontaneous resolution rate amongst children undergoing repeat US after initial US diagnosis of intussusception. This study did not include data about the management and outcomes for the diagnosed patients, and therefore does not comment on a spontaneous reduction rate between imaging and attempted enema reduction. Two studies, Ein et al. & Eklof et al. [4,5] reported on rates of spontaneous reduction between failed enema and surgical intervention, and found rates of 10% and 14%, respectively. These two studies included all types of intussusception (ileoileal and those with pathologic lead points) and did not include patients who spontaneously reduced between imaging studies or between imaging and attempted enema.
Our study found an overall enema success rate of 70% and an operative intervention rate of 19%. These figures are similar to previous studies specifically examining outcomes of intussusception, which have reported enema success rates of 40 - 85% and operative intervention rates of 6 to 42% [1-6, 9, 10-14].
There were no significant differences seen in age, presenting symptoms, or duration of symptoms between the group that selfresolved compared to the group that required enema or operative intervention. One reason for the lack of difference between groups may be that the size of the spontaneous resolution group was relatively small (N= 35). Data collected over a longer period of time, or between multiple sites, could add to the population and potentially reveal some meaningful differences between the groups. Interestingly, there were some statistically significant differences between the group who required operative intervention compared to the groups that either self-resolved or required enema. The patients who ultimately required surgery were younger, less commonly had abdominal pain, and more commonly had vomiting, bloody stools and altered mental status. They also had a longer duration of time from diagnosis to outcome. These differences seem logical; a patient who is younger might have more difficulty localizing symptoms, making it harder or take longer to ultimately make a diagnosis. They may present with the less typical or more severe symptoms, such as altered mental status and bloody stools. The longer time frame from diagnosis to outcome for patients requiring surgery is inevitable, as all patients with image-diagnosed intussusception undergo air or contrast enema as an initial treatment strategy, and only go to the OR if the enema is unsuccessful.
It is not entirely clear why the timing of self-resolution was different between patients who were transferred to our facility compared to those who presented directly to our Emergency Department (ED). Transferred patients were more commonly found to have resolution of their intussusception between an initial imaging study and a repeat imaging study. This could be because our hospital does not routinely read transferring hospitals’ US images, and therefore these patients undergo repeat US imaging to confirm their diagnosis. Another explanation is that patients who are transferred may have a change in their symptoms, such that they have improvement in their pain or other symptoms, and therefore a repeat image is performed to assess for the persistence of the intestinal abnormality. Without the actual US images to review, and without clear documentation of changes in transferred patients’ physical exam findings and symptoms both before and after their transfer, it will be impossible to know the exact reason for this difference in timing of resolution.
Regarding the presenting symptoms of intussusception, it has long been taught that a classic triad of abdominal pain, bloody stool, and vomiting are representative of ileocolic intussusception. However, our study shows that this “classic triad” is present in only 17% of cases. Individually, the most common presenting symptoms of intussusception were abdominal pain (81%) and vomiting (72%). Additionally, we discovered that 48 (15%) of patients presented with abdominal pain as an isolated complaint, and 22 (7%) with vomiting as an isolated complaint. Klein et al. [15] previously attempted to create a decision rule to identify patients at low risk for intussusception, thereby avoiding unnecessary enemas or other diagnostic tests, but unfortunately failed to find anything reliable as a decision rule. Our findings confirm this challenging aspect of idiopathic ileocolic intussusception. Emergency practitioners may take this information to mean that they should consider a diagnosis of intussusception even if the “classic triad” is not present and a sufficiently vague symptom such as abdominal pain or vomiting is the only complaint.
Limitations
Our study had several limitations. As a retrospective review, we relied on the documented history and physical for patient information, and we relied on time stamps for the documentation of timing of tests and results. We also had to rely on transport documentation for the results of imaging studies that were performed at referring facilities. Our hospital does not routinely re-read US images performed at referring hospitals, so the results of USs obtained at outside hospitals were determined based on the radiologist read at the performing hospital.
Our study did not examine recurrence rates. Previous studies have reported recurrence rates (overall, for all types of intussusception) of 6 to 20%. [1,6,11-12,14,16-17] This topic was out of the scope of the current study, but would be useful information to study in the future, as the rate of recurrence may differ amongst patients who had enema or operative intervention compared to those patients whose intussusception self-resolved.
Conclusion
We found a spontaneous resolution rate of 11% for idiopathic ileocolic intussusception in otherwise healthy children. Just as there are no specific criteria to identify patients at low risk of having intussusception, there are no clear criteria as to which patients with intussusception will likely self-resolve compared to those who will require enema or operative intervention.
We believe that this resolution rate of 11% is sufficiently high that it should be taken into consideration when approaching patients in the pediatric ED with suspected or image-confirmed diagnosis of intussusception.
References
- Al-Jazaeri A, Yazbeck S, Filiatrault D, Beaudin M, Emran M, et al. (2006) Utility of hospital admission after successful enema reduction of ileocolic intussusception. J Pediatr Surg 41(5): 1010-1013.
- Burns R, Adler M, Benya E, Guthrie B (2014) Fluoroscopy Screen Time During Contrast Enema for the Evaluation and Treatment of Intussusception. Pediatr Emerg Care 30(5): 327-330.
- Curtis JL, Gutierrez IM, Kirk SR, Gollin G, et al. ( 2010) Failure of enema reduction for ileocolic intussusception at referring hospital does not preclude repeat attempts at a children’s hospital. J Pediatr Surg 45(6): 1178-1181.
- Ein SH, Alton D, Palder SB, Shandling B, Stringer D, et al. (1997) Intussusception in the 1990s: has 25 years made a difference? Pediatric Surgery International 12(5-6): 374-376.
- Eklof OA, Johanson L, Lohr G (1980) Childhood intussusception: Hydrostatic reducibiity and incidence of lead points in different age groups. Pediatric Radiology 10: 83-86.
- Gilmore AWG, Reed M, Tenenbein M (2011) Management of childhood intussusception after reduction by enema. Am J Emerg Med 29(9): 1136-1140.
- Hryhorczuk AL, Strouse PJ (2009) Validation of US as a first-line diagnostic test for assessment of pediatric ileocolic intussusception. Pediatr Radiol 39(10): 1075-1079
- Navarro O, Daneman A (2004) Intussusception Part 3: Diagnosis and management of those with an identifiable or predisposing cause and those that reduce spontaneously. Pediatr Radiol 34(4): 305-312.
- Shekherdimian S, Lee SL, Sydorak RM, Applebaum H (2009) Contrast enema for pediatric intussusception: is reflux into the terminal ileum necessary for complete reduction? J Pediatr Surg 44(1): 247-250.
- Swischuk LE, John SD, Swischuk SD (1994) Spontaneous reduction of intussusception: verification with US. Radiology 192(1): 269-271.
- Daneman A, Alton DJ, Lobo E, Gravett J, Kim P, et al. (1998) Patterns of recurrence of intussusception in children: a 17year review. Pediatr Radiol 28(12): 913-919.
- Fecteau A, Flageole H, Nguyen LT, Laberge JM, Shaw KS (1996) Recurrent Intussusception: Safe Use of Hydrostatic Enema. J Pediatr Surg, 31(6): 859-861.
- Justice F, Auldist A, Bines J (2006) Intussusception: Trends in clinical presentation and management. J Gastroenterol Hepatol 21(5): 842- 846.
- Wiersma F, Allema JH, Holscher HC (2006) Ileoileal intussusception in children: ultrasonographic differentiation from ileocolic intussusception. Pediatr Radiol 36(11): 1177-1181.
- Klein E, Kapoor D, Shugerman R (2004) The Diagnosis of Intussusception. Clin Pediatr (Phila) 43(4): 343-347.
- Daneman A, Navarro O (2004) Intussusception: part 2: An update on the evolution of management. Pediatr Radiol 34(2): 97-108.
- Whitehouse JS, Gourlay DM, Winthrop AL, Cassidy LD, Arca MJ (2010) Is it safe to discharge intussusception patients after successful hydrostatic reduction? J Pediatr Surg 45(6): 1182-1186






























