Respiratory and Gastrointestinal Involvement in Birth Asphyxia
Rohit Vohra1*, Vivek Singh2, Minakshi Bansal3 and Divyank Pathak4
1Senior resident, Sir Ganga Ram Hospital, India
2 Junior Resident, Pravara Institute of Medical Sciences, India
3 Fellow pediatrichematology, Sir Ganga Ram Hospital, India
4 Resident, Pravara Institute of Medical Sciences, India
Submission: December 01, 2017; Published: May 14, 2018
*Corresponding author: Dr Rohit Vohra, Senior resident, Sir Ganga Ram Hospital, 22/2A Tilaknagar, New Delhi-110018, India.
How to cite this article:Rohit V, Vivek S, Minakshi B, Divyank P. Respiratory and Gastrointestinal Involvement in Birth Asphyxia. Acad J Ped Neonatol. 2018; 6(4): 555751. DOI: 10.19080/AJPN.2018.06.555751
Abstract
Background:The healthy fetus or newborn is equipped with a range of adaptive, strategies to reduce overall oxygen consumption and protect vital organs such as the heart and brain during asphyxia. Acute injury occurs when the severity of asphyxia exceeds the capacity of the system to maintain cellular metabolism within vulnerable regions. Impairment in oxygen delivery damage all organ system including pulmonary and gastrointestinal tract. The pulmonary effects of asphyxia include increased pulmonary vascular resistance, pulmonary hemorrhage, pulmonary edema secondary to cardiac failure, and possibly failure of surfactant production with secondary hyaline membrane disease (acute respiratory distress syndrome).Gastrointestinal damage might include injury to the bowel wall, which can be mucosal or full thickness and even involve perforation
Material and methods:This is a prospective observational hospital based study carried out on 152 asphyxiated neonates admitted in NICU of Rural Medical College of Pravara Institute of Medical Sciences, Loni, Ahmednagar, Maharashtra from September 2013 to August 2015.
Results: Respiratory system involvement was seen in 68 (45%) neonates.112 neonates (73.6%) had no/ mild respiratory distress (Downe’s score 0-3) while 24% and 35% of children who had asphyxia had moderate and severe respiratory distress respectively. A total of 24 neonates had features suggestive of NEC out of which 17 had grade I, Grade II NEC was seen 6 neonates while only one had grade III NEC.
Conclusion: Respiratory and GIT involvement in birth asphyxia is a common and are important causes of morbidity and as well as mortality.
Keywords: Birth asphyxia; Respiratory distress; NEC; Mechanical ventilation
Introduction
Asphyxia at a pathophysiological level, is the simultaneous combination of both hypoxia and hypoperfusion, which impairs tissue gas exchange, leading to tissue acidosis. During normal labor, transient hypoxemia occurs with uterine contractions, but the healthy fetus tolerates this well.
The healthy fetus or newborn is equipped with a range of adaptive, strategies to reduce overall oxygen consumption and protect vital organs such as the heart and brain during asphyxia. Acute injury occurs when the severity of asphyxia exceeds the capacity of the system to maintain cellular metabolism within vulnerable regions.
The pulmonary effects of asphyxia include increased pulmonary vascular resistance, pulmonary hemorrhage, pulmonary edema secondary to cardiac failure, and possibly failure of surfactant production with secondary hyaline membrane disease (acute respiratory distress syndrome). Meconium aspiration if present may add to the problems [1]. The respiratory system may require support for respiratory distress syndrome or pulmonary hypertension. The goal in management of the respiratory system is moderation in oxygen and carbon dioxide levels. Hypoxia and hyperoxia can lead to further neuronal injury. Hypercarbia can lead to cerebral vasodilatation and hemorrhage, whereas hypocarbia can lead to decreased cerebral blood flow [2].
In the severely depressed infant, the necessity for very early artificial ventilation with oxygen is undisputed. However, there are differences of opinion about the advisability of a brief attempt at bag and mask ventilation prior to endotracheal intubation. There is a general agreement that respiratory stimulants are not helpful in resuscitating the severely asphyxiated infant [3].
During the initial period of asphyxia, rapid but ineffective breathing occurs within 30sec of the onset of hypoxia. These rapid respirations last for about 30sec and then stop. If asphyxia continues the heart rate falls and muscle tone is lost. Cyanosis and decreased capillary blood flow occurs secondary to vasoconstriction. This period of time is termed primary apnea. Resuscitation efforts begun during this time are usually successful and often require only supplemental oxygen and tactile stimulation to reestablish respiration.
It resuscitation does not take place, rhythmic gasping then begins and continues for 4-5min, slowly it becomes weaker and weaker until the infant takes a final gasp and enters the period called secondary or terminal apnea. Resuscitation will require artificial ventilation using positive pressure bag and mask and oxygen to establish spontaneous and effective respiration [4].
Birth asphyxia has been documented as the primary cause of respiratory distress in newborns, especially the term neonates, which resolves over a period of time with supplementary oxygen. A few having persistent respiratory distress need ventilatory support.
Gastrointestinal damage might include injury to the bowel wall, which can be mucosal or full thickness and even involve perforation. The extent of the damage influences the nutritional management, in particular when to begin feedings once recovery occur [2]. The shunting of blood away from the intestine in a fashion similar to the diving reflex in aquatic mammals has been postulated as a potential mechanism for producing the initial gut ischemia. This reflex occurs most commonly in response to asphyxia and it forms the basis of gastrointestinal involvement in birth asphyxia.
The asphyxiated infant is at risk for bowel ischemia and necrotizing enterocolitis (NEC) [5]. Probably the most serious gastrointestinal disorder occurring in neonates is necrotizing enterocolitis.
Clinical presentations vary widely. Abdominal distention usually is one of the earliest and most consistent clinical signs. Other symptoms include bloody stools, apnea, bradycardia, lethargy, shock and retention of gastric contents due to poor gastric emptying. Thrombocytopenia, neutropenia and metabolic acidosis may develop during bowel ischemia. Feeding intolerance and subtle alterations of intestinal motor activity and gastrointestinal peptides have been reported in association with perinatal asphyxia [6].
Material and Methods
Study design
Prospective Observational hospital based Study
Data collection
All asphyxiated newborns delivered at Pravara Institute of Medical Sciences, Loni from September 2013 to August 2015 who had features of birth asphyxia with Apgar score of ≤7 at 5min or/ and Umbilical cord arterial pH of <7.2 at birth or/and required more than 1 minute of positive pressure ventilation before sustained respiration or the need for mechanical ventilation at birth were included in the study.
Neonates born before 37 weeks of gestation, or born outside Pravara Institute of Medical Sciences, Loni or with congenital anomalies or with early onset sepsis were excluded from study.
Approval from the institutional ethics committee and written consent was taken from all parents before inclusion of their child in the study.
A detailed history was taken and examination performed at the time of admission to NICU. The neonatal clinical course was followed up to 14 days of birth .The data so obtained was be recorded. Natal history was taken to find out the mode of delivery and indications for interventions, if any. Complications during and prior to labour were noted.
All births were attended and resuscitated by the pediatricians. For resuscitation Neonatal Resuscitation Protocol of American Academy of Pediatrics 2010 was followed [6]. Postnatal history was obtained regarding birth asphyxia and for details of resuscitation measures done at birth, APGAR score at 1min. and 5min. was assessed.
Gestational age in completed weeks was assessed on basis of mother‘s last menstrual period and confirmed where ever necessary by routine early antenatal ultra sonography (USG) examination. In cases where ever last menstrual period (LMP) was not available and antenatal USG was not done, then gestational age was assessed by Modified Ballard Scoring system [7].
All biochemical samples were taken on admission. Special investigation like echocardiography was done at Department of Radiology at Pravara Institute of Medical Sciences, Loni.
Daily follow-up of the patient was done and overall progress was monitored till the discharge from NICU or death of the baby
Respiratory System
• Assessment of respiratory distress was done by Downe’s score.
• A score of <4 was defined as no/ mild respiratory distress,
• 4-7 was defined as moderate respiratory distress
• And >7 was defined as severe respiratory distress.
Respiratory status monitering was done in all neonates included in the study by modified downe’s score on hourly basis till 48 hrs after birth. Any child with moderate respiratory distress was started on O2 inhalation via nasal prongs to maintain a SPO2 more than 92% and children having severe respiratory distress and/ apnea was started on mechanical ventilation.
Chest X-ray was performed in all infants needing oxygen supplementation. Abnormal chest X ray was defined as any of the following features pulmonary infiltrates, patchy hyperinflation and atelectasis, air leaks, loss of lung volume, ground glass appearance or white out lungs (Figure 1).
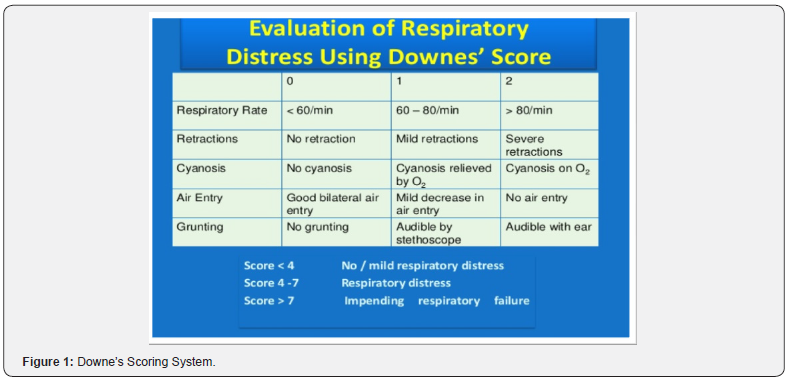
Gastrointestinal evaluation
Enteral feeding was started after 24 hours after birth in all cases via naso- gastic tube after ruling out active GI bleed. Feeds were started at a rate of 10 -20ml/kg/ day and advanced at a rate of 20ml/kg/day upto a maximum of 120ml/kg/day. All infants were started on expressed breast milk. All infants were monitered for presence of GI bleed, abdominal distension, and altered GI aspirate, or any features suggestive of NEC. Modified Bell’s criteria were used for diagnosis of necrotizing enterocolitis. If we were unable to provide enteral feeds to the child even after 72 hours after birth TPN was started (Figure 2).
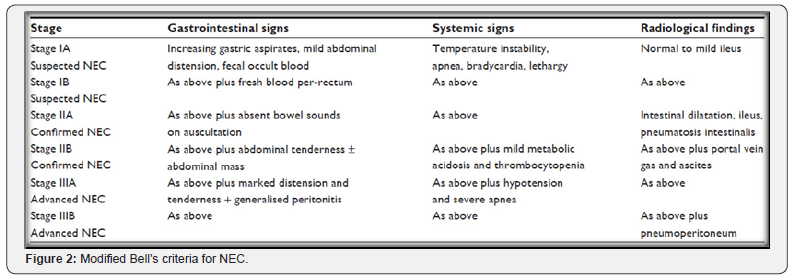
Statistical analysis
Values have been expressed as Mean±SD. The data were compiled and analyzed using descriptive statistics using student t-test. P value <0.05 was considered to be significant.
Results
Total 152 asphyxiated babies were included in the study. In this study out of 152 neonates, 84 were males and 62 females. 55.17% of our patients were delivered by vaginal delivery, while 38% of them were delivered by cesarean section.
112 neonates (73.6%) had no/ mild respiratory distress (Downe’s score 0-3) while 24% and 35% of children who had asphyxia had moderate and severe respiratory distress respectively (Table 1) (Graph 1).
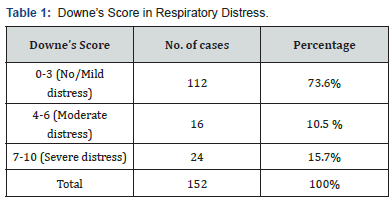
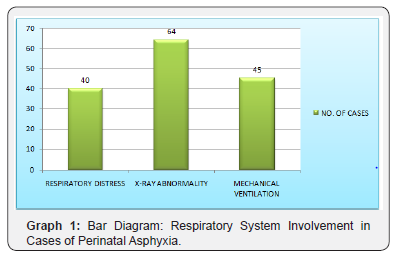
X ray abnormalities were seen in 64 (42%) of neonates. 45 (29.6%) of neonates required mechanical ventilator support (Table 2).
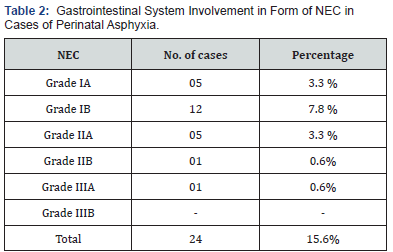
A total of 24 neonates had features suggestive of NEC out of which 17 had grade I, Grade II NEC was seen 6 neonates while only one had grade III NEC.
Discussion
Respiratory involvement
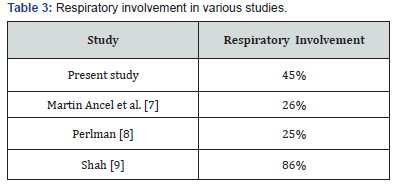
In present study is having the involvement of the pulmonary system in 68 (45%) neonates (Table 3).
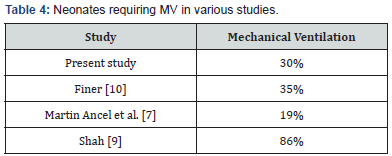
Need for mechanical ventilation
Mechanical ventilation (MV) was needed by 30% neonates in the present study. Other studies have found variable results (Table 4).
Mortality with respiratory involvement
In present study, mortality rate of 50% infants was noted among those with pulmonary dysfunction. In the study by Martin Ancel et al. [7] 6% neonates died due to respiratory involvement. Shankaran et al. [7] had mortality rate of 7% with pulmonary involvement.
In present study, mortality rate of 50% infants was noted among those with pulmonary dysfunction. In the study by Martin Ancel et al. [7] 6% neonates died due to respiratory involvement. Shankaran et al. [7] had mortality rate of 7% with pulmonary involvement.
Mortality with gastrointestinal system involvement
In present study, 29% neonates died with GIT involvement. In the study by Mohammed et al. [11] death was seen in 50% of those with GI involvement.
Conclusion
Multiorgan dysfunction, though a common feature of perinatal asphyxia, is often overlooked. The focus, most of the time, has been on the brain involvement and HIE following perinatal asphyxia. The body system gives priority to preserving the brain function, at the expense of other systems. Most research too has principally focused on the effect of hypoxia- ischemia on the brain while less attention has been paid to the effect on other systems.
Ethical Approval
Ethical Approval was taken from the institute ethics committee. Authors are required to make a disclose statement in the manuscript. Any financial (funding, stocks, the authors declare no conflicts of interest).
References
- Arora S, Evan YS (2004) Manual of neonatal care. In: Cloherty JP, Eric C, Eichenwald, Stark AR (Eds.), (5th edn), Lippincott Williams & Wilkins, USA, pp.536-555.
- Leuthner SR, Das UG (2004) Low Apgar scores and the definition of birth asphyxia. Pediatr Clin N Am 51(3): 737-745.
- Behrman RE, James LS, Klaus M, Nelson N, Oliver T (1969) Treatment of the asphyxiated newborn infant. Current opinions and practices as expressed by a panel. J Pediatr 74(6): 981-986.
- Rajakumar PS, Bhat BV, Sridhar MG, Balachander J, Konar BC, et al. (2008) Cardiac Enzyme Levels in Myocardial Dysfunction in Newborns with Perinatal Asphyxia. Indian J Pediatr 75(12): 1223-1225.
- Arora S, Evan YS (2004) Manual of neonatal care. In: Cloherty JP, Eichenwald EC, Stark AR (Eds.), (5th edn), Lippincott Williams & Wilkins, pp. 536-555.
- Turner-Gomes SO, Izukawa T, Rowe RD (1989) Persistence of atrioventricular valve regurgitation and electrocardiographic abnormalities following transient myocardial ischemia of newborn. Pediatr Cardiol 10(4): 191-194.
- Martín-Ancel A, García-Alix A, Gayá F, Cabañas F, Burgueros M, et al. (1995) Multiple organ involvement in perinatal asphyxia. J Pediatr 127(5): 786-793.
- Perlman JM, Tack ED, Martin T, Shackelford G, Amon E (1989) Acute systemic organ injury in term infants after asphyxia. Am J Dis Child 143(5): 617-620.
- Shah P, Riphagen S, Beyene J, Perlman M (2004) Multiorgan dysfunction in infants with post asphyxial hypoxic ischaemic encephalopathy. Arch Dis Child Fetal Neonatal 89(2): F152-F155.
- Finer NN, Richards RT, Peters KL (1981) Hypoxic ischaemic encephalopathy in term neonates. Perinatal factors and outcome. J Pediatr 98(1): 112-117.
- Shankaran S, Woldt E, Koepke T, Bedard MP, Nandyal R (1991) Acute neonatal morbidity and long-term central nervous system sequelae of perinatal asphyxia in term infants. Early Hum Dev 25(2): 135-148.
- Mohammed LH, Mohammed NR, Al-Hussieny NA, Rezq SH (2011) Early predictions of hypoxic-ischemic encephalopathy by umbilical cord nucleated red blood cells and lactate. Med J Cairo Univ 79: 625-631.






























