Computed Tomography of the Head Prior to Lumber Puncture in Suspected Cases of Meningitis in Children, in Qatar
Wail Seleem1, Ahmed Setouhi1, Abdulaziz Farooq2, Nahla Sharaf1, Hoda Badran1, Mohamed Shoaebi1 and Khalid Ibrahim1
1Hamad General Hospital, PO BOX 3050, Doha-Qatar
2AspetarOrthopaedic and Sports Medicine Hospital, PO Box 29222, Doha-Qatar
Submission: July 14, 2017; Published: October 20, 2017
*Corresponding author: Khalid Ibrahim, Department of Pediatric, Hamad General Hospital, P.O BOX 3050, Doha, Qatar.
How to cite this article: Wail S, Ahmed S, Abdulaziz F, Nahla S, Hoda B, et al. Computed Tomography of the Head Prior to Lumber Puncture in Suspected Cases of Meningitis in Children, in Qatar. Acad J Ped Neonatol. 2017; 5(5): 555732. DOI: 10.19080/AJPN.2017.05.555732
Abstract
Introduction: Lumbar puncture (LP) to obtain cerebrospinal fluid (CSF) is an important step in the management of acute bacterial meningitis. This procedure can, however, be associated with the presumed risk of brain herniation. Performing head Computed Tomography (CT) scan before LP has become an almost a routine practice in many centers with its associated possible negative impact of radiation risk and treatment delay
Methods:A retrospective review of cases of children, age 18 months to 14 years, with suspected meningitis attending a large emergency center over two years. Demographic and clinical descriptions were recorded. Children who had CT head and lumbar punctures were recorded.
Results: 116 cases were included in the study. 55.2% were in the age group 5 to 9 years. CT of the head was done before LP on 101 (87%) of the cases. Abnormalities in the scan were reported on 6 (0.06%). LP was done on 100 (86%) of the cases, including two of the children with abnormal scans. CSF findings suggested aseptic meningitis in 85% and bacterial meningitis in 10% of the cases. There was an average delay of 7.7 hours in getting the scan, 6.3 hours in starting antibiotics and 8.9 hours in performing the LP. No complications were reported with the LP procedures.
Conclusion: This large pediatric series demonstrated the high prevalence of the practice of obtaining head CT before LP in suspected cases of meningitis. Reported abnormalities in head CT scans were extremely low. Organizing the imaging studies was associated with delay in initiating the correct treatment. Practice advices regarding LP in these cases are given.
Keywords: Bacterial Meningitis; Children; Lumbar Puncture; Computed Tomography
Introduction
Overview of pediatric bacterial meningitis
Bacterial meningitis within the pediatric age group is considered a medical emergency, because it can result in serious morbidity, mortality and significant disabling neurological consequences. Delay in establishing diagnosis and starting antibiotic poses high risk on patients. In order to positively diagnose bacterial meningitis, a cerebrospinal fluid (CSF), obtained via lumbar puncture (LP), study should be performed. Performing lumbar puncture in such cases has remained controversial, because of the presumed risk of brain herniation [1]. All cases of bacterial meningitis are associated with varying degrees of increased intracranial pressure. However, herniation is a rare complication occurring in about 5% of patients [2]. Due to the potential risks of the lumber puncture procedure, a computed tomography (CT) head scan is widely used to decide which patients in whom lumber puncture should be avoided [3]. However, with the increase of such practice, important questions should be asked such as; how sensitive is a CT head scan in detecting increases of intracranial pressure and, importantly, how detrimental could the resulting delay in initiation treatment. Many studies have demonstrated that CT head scans can be normal in cases where an increase of intracranial pressure actually exists [4]. A further concern is the potential risks of the high dose radiation associated with CT scans [5]. The decision to do a CT head scan prior to lumbar puncture remains a clinical dilemma highlighting the need for further studies in this area.
In this study we retrospectively reviewed the practice of performing head CT scans before doing lumbar punctures, in a busy tertiary pediatric center.
Methodology
Two years retrospective study of cases of suspected meningitis in children between the age of 18 months and 14 years that attended Hamada General Hospital, a tertiary hospital serving a population of 1.75 Million in Qatar. The medical notes and the electronic records of all cases with the record coding of meningitis were reviewed. All children who had head CT scans done were recorded. A neuroradiologist subsequently reviewed all the scans. All children under the age of 18 months, together with all cases where records were incomplete, were excluded from the review.
Results
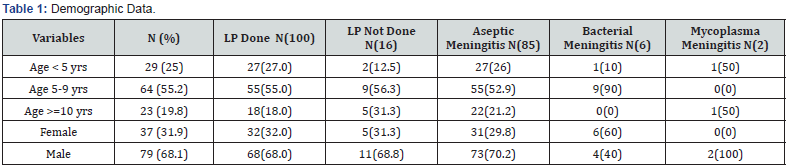
This retrospective review included 116 cases, of which, 79 (68.1%) were males and 37 (31.9%) females. The larger age groups represented were five to nine years (55.2%) followed by the under fives (25%). Lumbar puncture was done in a hundred (86%) cases. CSF studies indicated aseptic meningitis in 85 (85%) cases, ; bacterial meningitis in 10 (10%) and mycoplasma infection in two cases. Nine cases (90%) of the bacterial meningitis were in the age group five to nine years. CT scans were done in 101 (87%) of all cases within the study (70 (69.3%) were males and 31 (31.7%) females (Table 1) only 6 (0.06%) of the total scans done revealed abnormalities. Two of these scans revealed diffuse brain edema; one suggested an uncal herniation, and the fourth showed evident dilatation of the ventricular system. In of all these cases, however, lumbar puncture was not done based on the scan reports. The fifth scan revealed mild brain edema with the sixth scan showing mild ventricular dilatation. In both of these cases lumbar punctures was done. In all of these six cases, no specific symptom or sign could predict the scan result. Fever and vomiting occurring in all of these cases. In another 2 cases the LP was refused by the families.
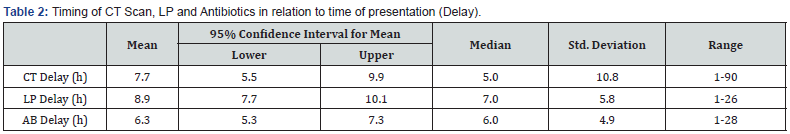
On average a lumbar puncture was conducted 8.9 hours post-presentation (CI 7,7-10.1). CT scans were completed on average 7.7 hours post-presentation (CI 5.5 -9.9). Antibiotics were commenced on average 6.3 hours post-presentation (CI 5.3 -7.3). No serious complications related to the lumbar puncture were reported in any of the study cases. (Table 2)
Discussion
Diagnosis of meningitis requires lumbar puncture to confirm the presence of inflammatory cells in the cerebrospinal fluid, to identify the infecting pathogen and to guide antimicrobial therapy. However, because of the potential risks associated with lumbar puncture, CT head scans are now widely used to identify patients in whom the procedure should be avoided. This practice of obtaining a CT head scan before performing a lumbar puncture is on the rise, particularly in facilities where CT scans are easily available. This practice has, almost, become the standard of care worldwide in such cases, especially in USA and Europe. This is likely to be attributed mostly to the lack of consensus and clear guidelines. Therefore, it has become particularly difficult for frontline physicians to decide whether or not the patient requires a CT scan of the head before having a lumbar puncture.
It is known that even a single exposure to CT head radiation is sufficient to raise the risk of malignancy, an effect that can persist for up to 25 years [5]. There is a widely accepted assumption that head CT scans can reliably predict who will and who will not experience brain herniation after a lumbar puncture. However, conversely, it is a fact that there exists considerable published data indicating the opposite. In a prospective investigation by Hasbun, et al.[6]. none of the seven patients with mild-to-moderate mass effects on CT head scans experienced brain herniation after undergoing a lumbar puncture procedure. Furthermore, four patients had a mass effect on CT head scans, which caused their treating clinicians to decide not to perform lumbar punctures. Two of those four patients experienced brain herniation despite not undergoing the lumbar puncture procedure. They, therefore, concluded that having a mass effect on a CT head scan did not predict post-lumbar puncture herniation, and in addition, not performing a lumbar puncture for patients with a mass effect, did not prevent herniation.
The results of numerous other studies are concordant. For example, ten out of seventy-five patients with streptococcus pneumonia meningitis experienced brain herniation after a lumbar puncture and only two of those patients had abnormal CT head scan findings prior to a lumbar puncture [7]. Furthermore, 26 of the 65 patients who did not experience brain herniation after a lumbar puncture had had abnormal CT head scan findings [7]. In another review, 36 patients underwent a lumbar puncture procedure despite having a mass effect on the CT head scan, and only one patient experienced brain herniation after the lumbar puncture. It was also noted that, a total of four (1.3%) of the 296 patients with focal mass effect, were found to have experienced brain herniation after a lumbar puncture [8].
In our retrospective study, all of the 116 included cases had a CT head scan, with 110 having lumbar puncture done. This indicates that CT was done on each single patient in whom LP was considered. Only six scans revealed abnormalities. Consequently, our findings demonstrate that the majority of CT head scans are normal before a lumbar puncture procedure (94.82%). The abnormalities in observed in the CT head scans were: two cases with diffuse brain edema, one evident dilatation of the ventricular system, one showed a suspected uncal herniation, and the remaining two scans showed one with mild brain edema and one with mild ventricular dilatation.
Although the number of the abnormal scans was low, we could not find any correlations between the result of the scan and age group, type of clinical presentation or the findings in the CSF studies.
The decisions not to do LP in these cases were not based on clinical findings but solely on the CT reports. An important aspect highlighted in our study is the delay in initiation of antibiotic treatment prior to conducting a CT head scans, on average it was 6.3 hours post-presentation to the emergency room. This may have serious consequences on the patient. A further observation is the unnecessary prolonged stay in the emergency room awaiting the completion of the CT head imaging (7.7hours post-presentation) before conducting the lumbar puncture. Alternatively stated, the significant delay in carrying out a lumbar puncture, caused by the decision to conduct a CT head scan first, can also affect other important management decisions such as whether or not to hospitalise the patient, in addition to unnecessarily prolonging a patient’s stay in the emergency department, occupying a much needed space for other patient’s.
The delay in therapy in our study was longer compared to the finding of Hasbun et al, of 2 hours and 20 minutes [6]. A further study in Pakistan carried out on children, showed the same pattern with more than three quarters of the scans done before LP were normal [9]. An important strength of our study, though, is the large sample size. We demonstrated the very low yield of the CT scans of the head in cases of suspected meningitis in the absence of clinical indicators of raised intracranial pressure and focal neurological deficits. In order to limit the unnecessary CT head scans, we suggest the following, modified criteria from the one referenced to by Creig and Goroszeniuk, 4 to select patients in whom a CT head scan prior to lumbar puncture is indicated [1].
Indications for mandatory CT Head Scan before LP in suspected bacterial meningitis
1. Signs of raised intracranial pressure (for example, papilledema, bradycardia occurring with hypertension)
2. Altered sensorium (Glasgow Coma Scale <11).
3. Immunosuppression.
4. Focal neurological deficit.
5. Tonic seizure or tonic posturing.
6. Unequal pupils (not deemed to be post ictal finding).
7. Suspected subdural or cerebral hemorrhage or collection.
Our findings indicate that children with suspected meningitis who have none of the significant base-line features which we identified, are good candidates for immediate lumbar puncture, with a low risk of brain herniation. Patients, who have any of the base-line clinical features we identified, should undergo a CT head scan after blood has been drawn for culture and after empirical antibiotic therapy has been initiated.
The limitation of the study is the fact that it is retrospective review. In addition there was shortage in documenting fundoscopic examination. Future studies will be needed to validate our results to determine their value with respect to the reduction of medical and legal concerns among physicians.
Conclusion
In conclusion, CT head scans are widely used in cases of children with suspected meningitis in order to decide on the safety of performing a lumbar puncture procedure. The abnormalities detected on the scans in these cases are very few. Performing the CT head scans has resulted in significant delays in performing a lumbar puncture, and most importantly has caused further delays on initiating antibiotic treatment; a practice which can lead to serious consequences in relation to the outcome of these cases.
References
- Kneen R, Solomon T, Appleton R (2002) The role of lumbar puncture in suspected CNS infection. a disappearing skill? Arch Dis Child 87: 181- 183.
- Oliver WJ, Shope TC, Kuhns LR (2003) Fatal lumbar puncture: fact versus fiction-an approach to clinical dilemma. Pediatrics 112: 174- 176.
- Mellor DH (1992) The place of computed tomography and lumbar puncture in suspected bacterial meningitis. Arch Dis Child 67: 1417- 1419.
- PR Creig, D Goroszeniuk (2006) Role of computed tomography before lumbar puncture: a survey of clinical practice. Postgrad Med 82: 162- 165.
- (2003) Royal College of Radiologists Making the best use of a department of clinical radiology, guidance for doctors. (5th edn), The Royal College of Radiologists, London, UK.
- Hasbun R, Abrahams J, Jekel J, Quagliarello VJ (2001) Computed tomography of the head before lumbar puncture in adults with suspected meningitis. N Engl J Med 345(24): 1727-1733.
- Kastenbauer S, Winkler F, Pfister HW (2002) Cranial CT before lumbar puncture in suspected meningitis. N Engl J Med 346: 1248-51.
- Tattevin P, Bruneel F, Regnier B (2002) Cranial CT before lumbar puncture in suspected meningitis. N Engl J Med 346: 1248-1251.
- Arshalooz Rehman , Muhammad Hamid, Uzma Rahim Khan (2014) CT scan in children with acute bacterial meningitis.Experience from Emergency Department of a tertiary-care hospital in Karachi, Pakistan. J Paki Med Ass 64(4):419-22






























