Dental Implants in Aesthetic Areas: Surgical Approaches and Prosthetic Considerations for Optimizing Results, A Review
Olívia Francescato1*, Frederico Santos Lages2 and Dennis Malta Guimarães3
1Master’s Degree student, area of concentration of Dental Clinic, School of Dentistry, Universidade Federal de Minas Gerais, Belo Horizonte, Minas Gerais, Brazil
2Adjunct Professor, Division of Dental Clinic, School of Dentistry, Universidade Federal de Minas Gerais, Belo Horizonte, Minas Gerais, Brazil
3PHD Student, area of concentration of Implantology at ILAPEO-PR Faculty, Belo Horizonte, Minas Gerais, Brazil
Submission: February 12, 2023; Published: February 21, 2023
*Corresponding author: Olívia Francescato, Master’s Degree student, area of concentration of Dental Clinic, School of Dentistry, Universidade Federal de Minas Gerais, Belo Horizonte, Minas Gerais, Brazil
How to cite this article: Olívia Francescato, Frederico Santos Lages and Dennis Malta Guimarães. Dental Implants in Aesthetic Areas: Surgical Approaches and Prosthetic Considerations for Optimizing Results, A Review. Adv Dent & Oral Health. 2023; 16(1): 555926. DOI: 10.19080/ADOH.2023.16.555926
Abstract
Treatment with dental implants is a clinical reality in dentistry. Several implants’ systems were introduced in the market aiming at improvements to the materials, however, there are still a lot of different surgical approaches for solving cases where there is a high aesthetic demand, especially in the anterior maxilla region. For a treatment with dental implants to be considered a success, it must present satisfactory aesthetic outcomes, with a prosthesis that is visibly pleasant and with peri-implant tissues with adequate volume. Some qualitative indexes were created where parameters related to “pink esthetic” and “white esthetic” are evaluated. The aim of this review was to elucidate different surgical and tissue manipulation protocols in order to explore new possibilities that optimize treatment using dental implants in anterior regions. The results are not conclusive regarding the pragmatic determination of the best surgical time, however, there is a tendency to obtain better aesthetic outcomes when the dental implants are early or immediately placed, from the point of view of papilla formation and maintenance of bone and soft tissue architecture. It is algo suggested that guided bone regeneration should be done simultaneously with the installation of the implants and also as soft tissue grafting. Can be concluded the important role of the implant-supported provisionals for proper conditioning of the peri-implant soft tissues. The literature confirms that each case must be evaluated individually, considering certain criteria when defining the treatment plan, such as the patient’s smile line, gingival biotype and soft tissue level, so that procedures that may lead to aesthetics failure are eliminated and consequently achieve the expectations of the patient.
Keywords: Dental implants; Dental implants in aesthetic areas; Aesthetic outcomes in dental implants
Abbreviations: CTG: Connective tissue graft; IIP: Immediate implant placement; MSI: Mucosal scarring index, ModPes: Modified pink esthetic score; PES: Pink esthetic score; SCTG: Subepithelial connective tissue graft; WES: White esthetic score
Introduction
Rehabilitating edentulous maxilla, especially in aesthetic areas is a surgical and prosthetic challenge required for the specialist, who needs to deal with a mostly medullary bone (presenting low trabecular density)[1], pre-existing conditions in the soft tissue such as absence of papillae, low buccal gingival volume, soft tissue margin level [2], thin gingival biotype, as well as the visibility of the peri-implant mucosa and the future crown on implant during smile and speech (such as patients with a high smile line, for example [3]. Therefore, when planning implants in aesthetic areas, especially in the anterior maxilla region, many risk factors that can lead to aesthetic failure are usually already present. Residual alveolar bone undergoes a remodeling process even when tooth loss is atraumatic, along with other anatomical changes. The appearance of the soft tissue represents an important aspect of the success of the implant, especially in aesthetic zones, and can be considered one of the main reasons for the patient to seek treatment with implants in this area [4].
For treatment with dental implants to be considered successful in aesthetic terms, it must have a visually pleasing prosthesis and complete (i.e., no dehiscences and fenestrations) and healthy soft tissue around this prosthesis. The aggregate of what is considered harmonic depends on both pink and white aesthetics [5]. Among several treatment approaches with dental implants in anterior regions, cases must be carefully studied and individually planned, mainly in view of the functional damage that poor execution of these procedures can cause, taking into account mainly the patient’s expectations. The expertise of the dentist responsible for the rehabilitation is decisive for obtaining aesthetically pleasing results, regardless of the surgical technique chosen for that specific treatment. The aim of this work is to carry out a literature review on the main surgical and prosthetic aspects when performing implants in aesthetic regions in order to optimize the final results.
Materials and Methods
The articles selected in this review were searched on pubmed and scielo databases between December 2020 and January 2023 with the keywords “dental implants”; “aesthetic implants”; “dental implants in aesthetic areas”; “aesthetic outcomes in dental implants”. In the analysis of the publications, the information was grouped in order to establish the relationship between the surgical techniques used (implant installation time, manipulation of the peri-implant tissue and previsualization) and the results obtained when performing dental implants in aesthetic areas.
Eligibility criteria
Studies that appeared after entering the search criteria “dental implants” were included; “aesthetic implants”; “dental implants in aesthetic areas”; “Aesthetic results in dental implants”. The articles should be in English, and in the appropriate period of time comprising December 2020 to January 2023. There were no limitations regarding the study design. Thirty-seven published papers were included in this review. Articles that did not meet the inclusion criteria were removed and duplicate articles were removed manually.
Review of surgical approaches and prosthetics considerations
Implants in anterior regions in healed and healing sites: The first implant installation protocols advocated that the implant should only be performed after a period of alveolar bone healing after tooth extraction in order to favor osseointegration [6] (Figure 1).
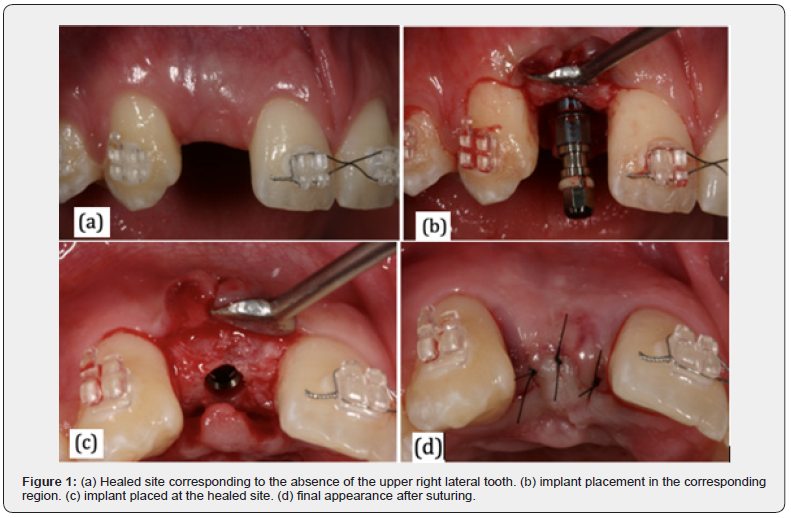
The installation of implants immediately after tooth extraction is considered a recent surgical protocol [7], which aims to reduce treatment time, reduce the number of surgical interventions, minimize alveolar bone resorption after tooth extraction, in addition to promote a positive psychological impact on the patient [8] (Figure 2). In 2005, Schropp, Isidor and Wenzel [9] developed a study where 45 patients underwent treatment with dental implants in aesthetic regions (maxilla and anterior mandible and premolar region) in two different protocols: early and late installation of implants, with the aim of evaluating the papilla interproximal and the length of the final clinical crown. An evaluation index was used with photos taken one week after the completion of the cases, as well as with 18 months of follow-up. The results showed that the risk of not having a papilla or a negative papilla was seven times greater in cases where the implants were performed late when compared to their early installation (33% versus 8%). The length of the clinical crown was also significantly more acceptable in cases with an early placement protocol compared to a late placement of implants after the 18-month follow-up. Therefore, this study suggests that the early installation of implants may be preferable to late installation, especially if the early formation of the interproximal papilla and the length of the clinical crown are analyzed, even if 18 months after the crown is placed on the implant, the dimensions of the papilla showed no difference between both protocols.
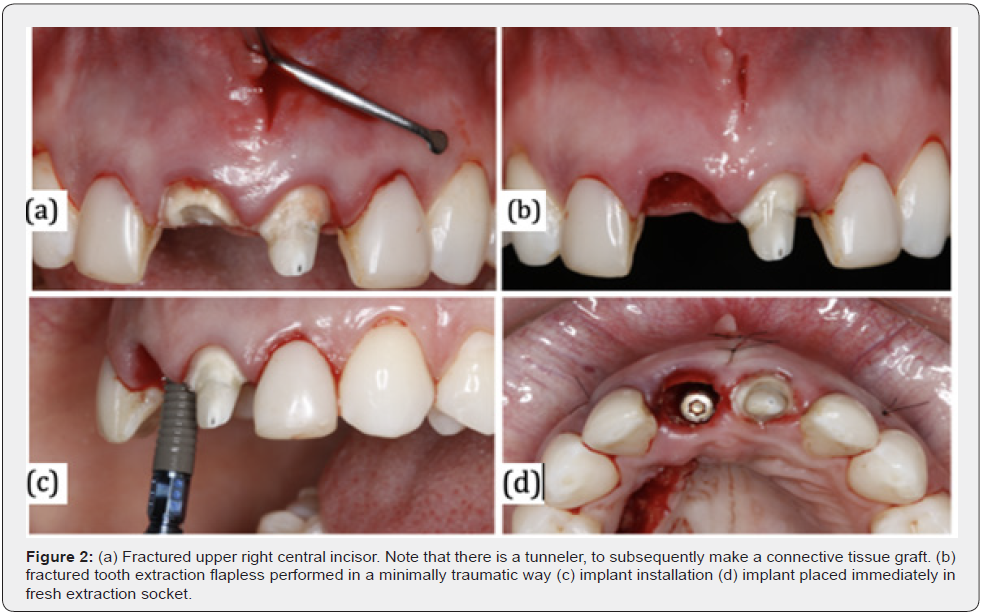
The retrospective study proposed by Mangano et al. [10] aimed to evaluate the final aesthetics results of single morse taper implants installed in fresh sockets in the anterior maxilla region using the pink and white esthetic evaluation indexes (PES/ WES). The study concluded that the immediate installation of single implants in an esthetic region with a morse connection appears to represent a successful procedure from an esthetic point of view. However, the authors suggest that further studies are required to evaluate the aesthetic results of this surgical approach as a treatment option. The work conducted by Cosyn, Eghbali, Bruyn, Dierens and Rouck [11] aimed to compare the aesthetics of implants installed in healing sites (6-8 weeks after tooth extraction) and completely healed sites (at least 6 months after tooth extraction), both in the anterior maxilla. Cases in which a soft and/or hard tissue graft had been performed previously or during implant installation were excluded. The PES [2] was used to evaluate the aesthetics of the peri-implant soft tissue, as well as the WES [12] proposed to evaluate the aesthetics of the visible part of the crown of the implant. There was no statistically significant difference in any of the parameters between the two treatment modalities in the evaluation of peri-implant soft tissue esthetics (PES) or in the evaluation of implant crown esthetics (WES).
Arora and Ivanovski [13] carried out a retrospective study whose aim was to investigate the aesthetic results of different times of installation of single implants in the anterior region of the maxilla. Four implant installation times were determined: T1, right after extraction; T2, 4-8 weeks after extraction; T3, 8-16 weeks after extraction and T4, more than 16 weeks after extraction. The PES and WES indexes were used for the evaluations. There was no statistical difference between treatment modalities (times) in pink aesthetics. In immediate implants, a trend towards better aesthetics was found in cases where they were performed flapless surgeries and whose buccal bone was intact (mean PES 11). It was concluded that the implant installation time did not significantly influence the aesthetic result, although immediate implants presented higher mean PES values. In 2021, Ibraim and Chrcanovic [8] conducted a systematic review and metaanalysis comparing dental Implants Inserted in Fresh Extraction Sockets versus Healed Sites, the review included 163 publications. Altogether, there were 17,278 and 38,738 implants placed in fresh extraction sockets and healed sites, respectively. The results showed that implants placed in fresh extraction sockets present a 34.9% higher risk of failure than implants placed in healed sites, when results from all study designs are considered. It also concluded that implant failure between the groups was statistically significant in the maxilla (higher for fresh extraction socket implants), but not in the mandible. In terms of loading, the difference in implant failure between groups was statistically significant for both implants submitted to immediate and delayed loading, but the difference was greater when immediate loading was applied. The treatment strategy to reduce the risk of gingival tissue recession in immediate implants should include maneuvers to contain dimensional tissue changes, including slow-resorptive bone grafts, flapless surgery, and connective grafting [14]. Only the expert clinician takes into account all the variables mentioned above and then combines them in order to determine an adequate and individualized treatment plan.
Bone augmentation prior to or simultaneously with the implant’s placements: Although bone resorption can be reduced, it cannot be completely extinguished. According to Pommer, Heuberer, Nahler and Watzek [15] procedures aimed at preserving the bone crest decrease vertical and horizontal alveolar resorption by an average of 1mm.
Rocuzzo, Gaudies’, Bunino and Dalmasso [16] carried out a long-term analysis for 10 years in which it was possible to observe the effectiveness of preservation of the alveolar bone crest. The peri-implant soft tissue margin supported by regenerated bone showed adequate stability with a low risk of gingival recession. The prospective study conducted by Chu et al. [17] aimed to evaluate the dimensional changes of the peri-implant soft tissue when immediate implants were performed in fresh sockets in the anterior region of the maxilla in four treatment modalities: without bone graft and provisional restoration, without bone graft but with provisional restoration, with bone graft and without provisional restoration and with bone graft and with provisional restoration. It was concluded that performing bone grafting and provisional restoration on immediate implants increased both the vertical and buccolingual dimensions by between 0.5-1.0mm when compared to the installation of immediate implants without bone graft and provisional simultaneously.
A 10-year prospective study was carried out by Chappuis et al. [18] which aimed to examine the effectiveness of early implant placement (4-8 weeks after tooth extraction) simultaneously with volume augmentation through guided bone regeneration in 20 patients. The mean peri-implant bone loss was 0.35mm between the 1st and 10th year assessment. A success rate of 95% was obtained, with pleasant aesthetic results and a high PES average (8). Buccal bone dimensions were measured with cone-beam computed tomography preoperatively and then at the 6th and 10th year of follow-up. Mean buccal bone wall thickness increased significantly from 0mm (at the time of surgery) to 1.67mm (after 10 years). Vertical bone loss from the peak of crestal bone was 0.02mm between the 6th and 10th year of follow-up. Some modulating factors that influenced the regenerative results in 10 years were the width of the preoperative interproximal bone crest and the thickness of the soft tissue. The study concluded the longterm efficacy of early implant placement while augmenting bone contour through guided bone regeneration, providing stable bone conditions with low risk of mucosal recessions over a 10-year observation period (Figure 3).
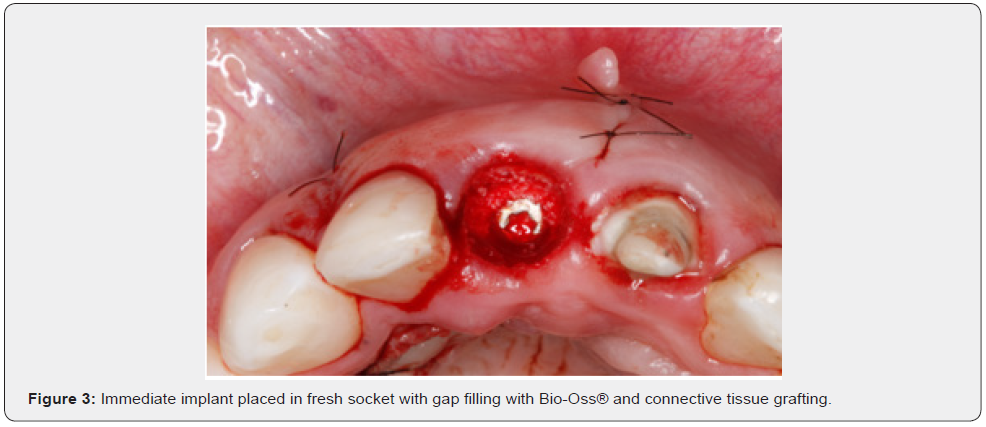
The work conducted by Hingsammer et al. [19] aimed to test the hypothesis that the socket volume increase performed at the time of tooth extraction followed by flapless implant installation using surgical guides obtained from computed tomography obtains satisfactory aesthetic results in most cases. The conclusion of this work was that although marginal bone loss cannot be avoided, the concept of crestal bone preservation and subsequent late implant placement (both flapless surgeries) has the potential to improve the esthetic results of single implants in the anterior maxillary region (Figure 4). The retrospective study carried out by Chen, Gu, Lai, and Gu [20] aimed to evaluate the three-dimensional stability of peri-implant hard tissue around single implants installed simultaneously with a guided bone regeneration using deproteinized bovine mineral bone in the anterior maxilla region and to explore possible influencing factors. Changes in the volume and thickness of the buccal hard tissue were analyzed and, in order to explore the possible influencing factors, the healing protocol, area and thickness of the graft that were performed were recorded. The secondary parameters evaluated were peri-implant marginal bone loss, bleeding on probing, and the PES score. The conclusion of this study was that, although the installation of single implants combined with guided bone regeneration using deproteinized bovine mineral bone in the anterior maxilla has presented satisfactory aesthetic and functional results, after a 03- year follow-up there was a significant decrease in the volume and thickness of the implant hard tissue of the grafted sites, mainly in the first 9 postoperative months. This phenomenon may be related to the moment of implant placement (immediate or late) and the thickness of the graft performed.
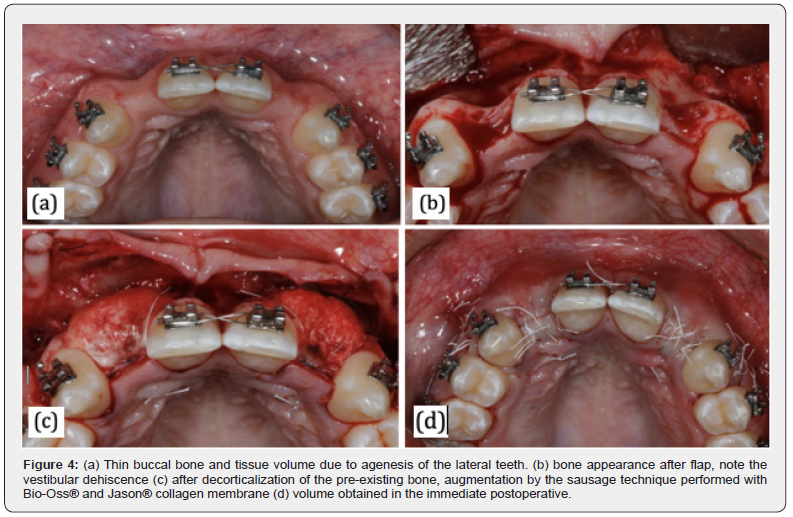
Connective tissue grafting: As previously mentioned, the appearance of the peri-implant mucosa is an important aspect in the final aesthetics of implants in the aesthetic area and usually is the main reason for the patient to seek treatment with implants in this area [4]. A thin gingival architecture is frequently observed in the anterior maxilla [11] and the use of soft tissue grafts and soft tissue substitutes to convert a thin-scalloped gingival type to a thick biotype when placing implants in the anterior maxilla is strongly recommended [21]. Furthermore, recessions following immediate implant insertion are frequently reported in the literature [22].
The systematic review and meta-analysis conducted by Seyssens, De Lat and Cosyn [23] aimed to assess the effect of connective tissue graft (CTG) in terms of vertical mid-facial soft tissue change when applied at the buccal aspect following single immediate implant placement (IIP). The review found 1814 registers but only one randomized controlled trial showed low risk of bias. Meta-analysis revealed a significant difference in favor of soft tissue grafting. This outcome was clinically relevant since the risk for ≥1 mm asymmetry in mid-facial vertical soft tissue level was 12 times lower following IIP + CTG. Soft tissue grafting also resulted in a trend towards less bleeding on probing. However, meta-analyses did not reveal significant differences in terms of PES, marginal bone level change and probing depth. The authors concluded CTG contributes to mid-facial soft tissue stability following IIP. Therefore, CTG should be considered when elevated risk for mid-facial recession is expected in the aesthetic zone (thin gingival biotype, <0.5 mm buccal bone thickness) (Figure 5).
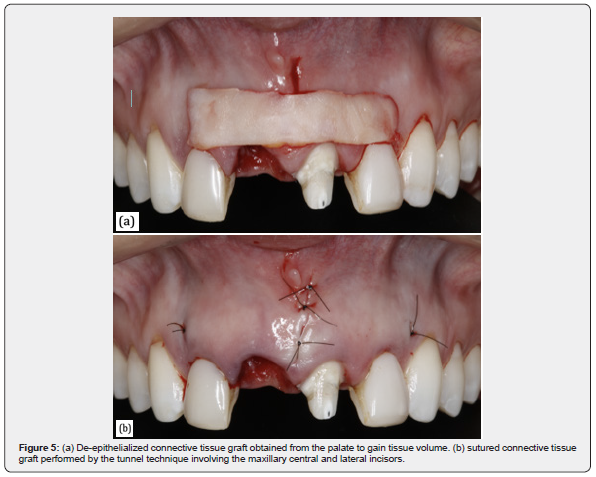
Abdelwahab, AlArab and El Nahass [24] performed a randomized controlled trial with the aim to evaluate the periimplant soft tissue aesthetics of delayed implants immediately provisional zed with or without subepithelial connective tissue graft (SCTG). The patients were randomized into two groups: the test group (immediate previsualization with SCTG) and a control group (immediate previsualization without SCTG). The soft tissue esthetics were assessed by the PES index and Mucosal Scarring Index (MSI), at 6 and 12 months, following final implant restoration. The results did not show significant differences in PES and MSI between both groups. This pilot study concluded that the soft tissue grafting around delayed implants immediately provisional zed could exhibit comparable results to immediate provisionalization without subepithelial connective tissue graft in terms of peri-implant soft tissue esthetics using PES and MSI. According to Noelken, Megrel, Pausch, Kunkel and Wagner [22], the simultaneous use of soft tissue grafts during immediate implant placement might reduce the risk of midfacial mucosal recession and improve the esthetic outcomes by reinforcement of the marginal tissues. They performed a retrospective study with 8 years of follow up. Twenty-six patients with marginal gingival recessions, which were designated for extraction and immediate implant insertion in the anterior zone of the maxilla were included. They were divided into two groups: In thirteen of the patients the recessions were grafted with autogenous bone graft additionally by connective tissue grafting, in the remaining 13 patients no soft tissue grafting was performed. The conclusion was that the results provide evidence that immediate implant placement can improve the level of facial soft tissues. In a more evident way in cases with greater recession and additional treatment with connective tissue grafts.
Use of implant-supported provisional restoration: In 1999, Jemt [25] separated 55 patients who were treated with 63 implants where the soft tissue was healed in two different ways: one group receiving provisional resin crowns at the time of reopening the implants (n = 25) and another only healing abutment (n = 38) prior to installing the final crowns. The follow-up time was 2 years. The results indicated that the use of temporary crowns was able to restore the soft tissue contour more quickly than with the healing abutments alone, however, the papilla adjacent to the crowns of the single implants presented similar volume in both groups after 2 years. Despite this result, Jemt stated that further studies were needed to elucidate different clinical procedures aimed at optimizing aesthetic results in implant dentistry.
Wittneben, Buser, Belser and Brägger [26] introduce in their article the clinical method named dynamic compression technique, which aims at conditioning the soft tissue around implants with the use with the use of provisional implant-supported restoration in the esthetic zone (anterior maxilla). Among the objectives of these techniques, they mentioned the need to establish an adequate emergence profile, to recreate a level of balanced mucosa and in harmony with the gingiva of the adjacent tooth, including papilla height and thickness and gingival zenith location, as well as establishing an accurate proximal contact point area to the adjacent implant tooth/crown (Figure 6).
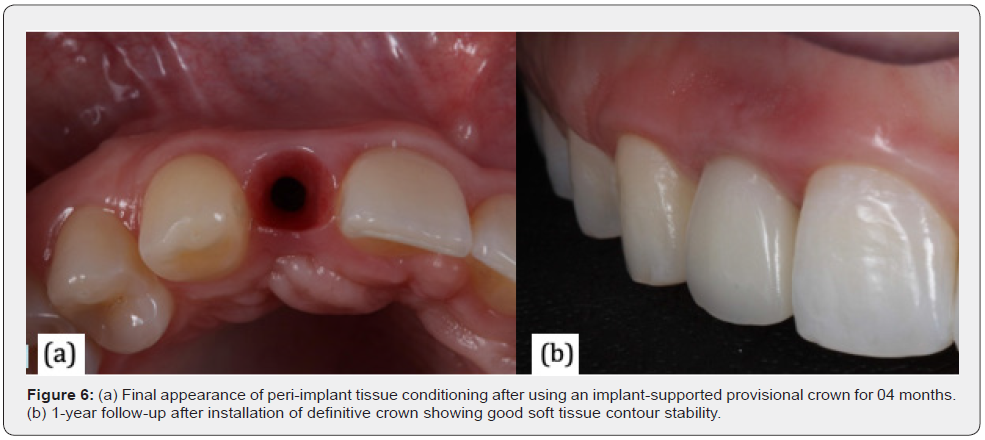
Furze et al. [27] conducted a randomized clinical trial whose objective was to investigate whether the use of an implantsupported provisional crown generated better final aesthetic results in anterior regions. To carry out this study, 20 implants were installed in the region from 13 to 23. In the reopening procedure, based on a randomization process, group 1 was defined, where soft tissue conditioning was performed using the dynamic compression technique with the use of a temporary crown and group 2, without the use of it. The final ceramic crowns were screw-retained, and the follow-up was 36 months. The results showed that the Modified Pink Esthetic Score (ModPes) showed a statistical difference between groups 1 and 2, while the WES showed no statistical difference between the two groups. The conclusion of the study was that implant-supported provisionals improve the final esthetics of the peri-implant mucosa (Figure 7 & Figure 8).
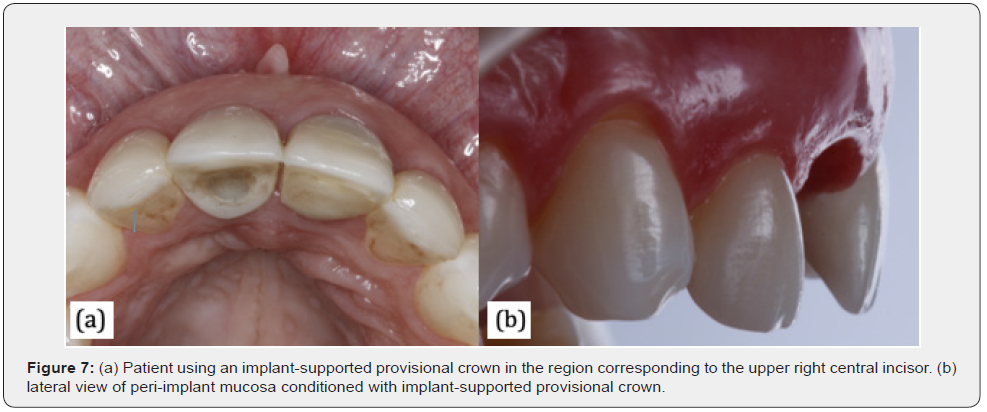
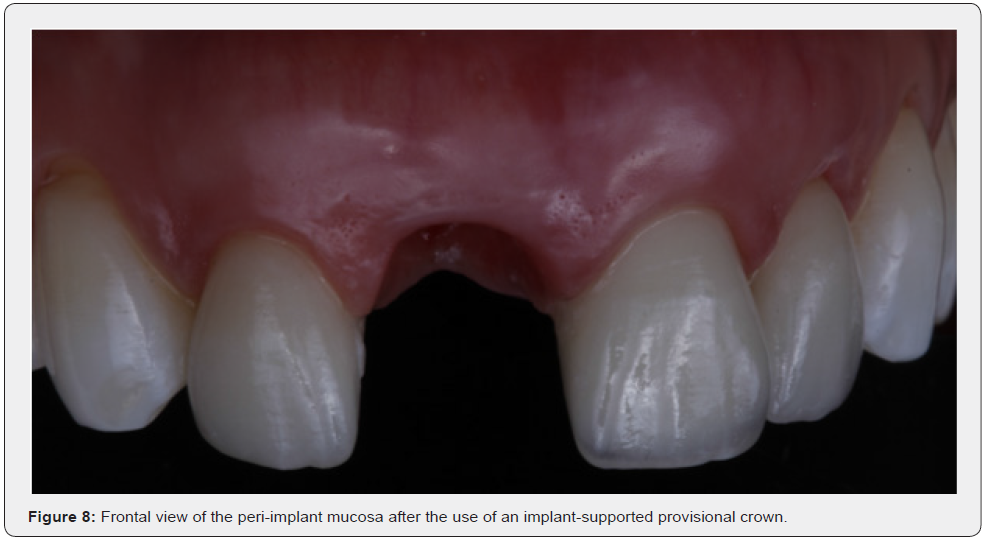
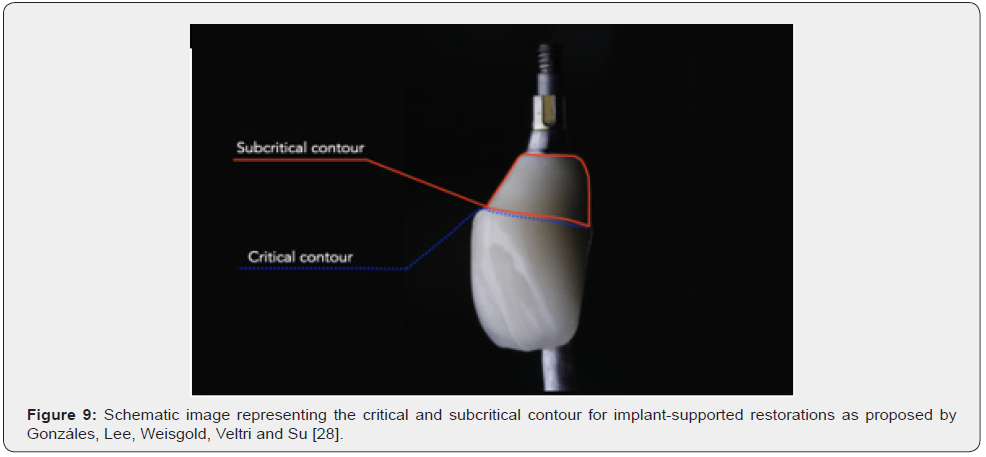
Gonzáles-Martín, Lee, Weisgold, Veltri and Su [28] start from the premise of the importance of obtaining excellent aesthetic results in implant-supported restorations. The authors emphasize the relevance of developing the transgingival area for maintaining and/or modifying the appearance of peri-implant soft tissues and how this can be achieved through an appropriate provisional restoration. To the authors maintaining the regenerated space and at the same time avoiding soft and hard tissue compression is mandatory when placing a provisional crown on an immediate implant. Therefore, they highlight the existence of two distinct areas between the implant prosthetic component and the crown: critical and subcritical contour zone (Figure 9).
Discussion
Patient satisfaction is a key factor in classifying a dental implant treatment as a success and, for this success to be achieved, the final result of the treatment must have an acceptable aesthetic appearance. Recently, indices for evaluating pink and white esthetics (PES/WES scores) have been applied to measure the final esthetic result of implant-supported crowns in the anterior region [2,12]. Dental treatments with implants show satisfactory and predictable results in single cases in the esthetic zone. However, the final result related to this procedure seems to vary according to the surgical and prosthetic approach selected for the treatment [29]. It is well known the importance of adequate management of the peri-implant soft tissue in anterior regions, for this reason, patients with a thin gingival biotype are more susceptible to esthetic complications [3]. A critical assessment of the smile line, gingival architecture (periodontal biotype) and soft tissue level (height) are essential to ensure good peri-implant esthetics [11].
Cosmetic complications can be classified into two groups: those affecting the “white aesthetic”, usually related to color and shape, and the “pink aesthetic” also called the “transition zone”, defined as the interface of the soft tissue margin around the cervical portion of the prosthesis. The major flaws found in the transition zone are associated with loss of papillae, marginal mucosal recession, dyschromia, and deficiency/lack of tissue volume. These are complications that are difficult to resolve and, when present, there are many clinical limitations in trying to restore a natural and ideal appearance [30]. For these reasons, some authors suggest that clinicians exclude patients with a “thin” gingival profile when performing high-risk procedures such as the installation of immediate implants associated with temporary implants. The same applies to sites with reduced bone volume or anatomical restrictions such as dehiscence or fenestrations. These defects require bone reconstruction in order to obtain more predictable long-term results [31,32].
Changes in soft and hard tissues after extraction of a natural tooth are a physiological and structural response that lead to bone remodeling. This, in turn, leads to dimensional, horizontal and vertical changes of the alveolar ridge, which can significantly impact esthetic results. The immediate installation of an implant right after tooth extraction does not prevent this physiological process from happening [4]. An effective regenerative protocol is the key to restoring and maintaining soft and hard tissue dimensions around the implant over the years [18]. The immediate installation of implants associated with professionalization aims at maintaining the bone and periodontal framework to achieve long-term osseointegration together with the reestablishment of a peri-implant mucosa with a natural appearance and satisfactory pink aesthetics [13]. Even though the concept of immediate implants has existed for over 20 years, there are still controversial discussions regarding the long-term results because it is something relatively “new” [7].
When using the surgical method of immediate installation of implants in fresh alveoli in anterior regions, the number of surgical steps is reduced, as well as the total treatment time is reduced, which sounds very attractive to the patient and, therefore, can It is said that there is a psychological benefit for these [8]. Factors such as the ideal three-dimensional positioning of the implant and preservation of the alveolar bone in the region of the extracted tooth have been considered advantages of immediate implantation [33].
Another point to be considered is the bone level of the adjacent tooth to the implant, an imperative factor for the presence of papilla. The reason for tooth loss is also very important to be evaluated. Tooth loss due to periodontal disease is directly related to the levels of papillae and this can negatively impact the final result of pink esthetics, explaining the absence of papillae in some cases [22].
Guided bone regeneration is currently the most used technique to reconstruct the peri-implant hard tissue architecture. Dental implants installed simultaneously with guided bone regeneration using deproteinized bovine mineral bone granules have been shown to achieve satisfactory long-term aesthetic and functional results [16,17]. The rate of resorption of this type of graft happens very slowly, which can be considered an advantage in maintaining the dimensions of the grafted region [20]. Another treatment option is the early implant placement protocol, within 4-8 weeks of tissue healing after extraction. Since the soft tissue is completely healed after this period, there is an increase in the amount of keratinized mucosa, which facilitates flap closure and favors bone regeneration [34]. Furthermore, the peak of osteoclastic and macrophage activity due to bone resorption from the socket during the initial healing phase decreases after 4-8 weeks [35] and there is an increase in levels of osteocalcin and bone morphogenetic proteins with high activity of endothelial cells [36], providing a favorable environment for regenerative procedures, especially in aesthetic areas, in order to compensate for dimensional changes in the buccal bone wall [37].
An early implant installation protocol offers minimal bone resorption in the region near to the post-extraction socket, according to the study by Chappuis, Engel, Reyes, Shahim, Nolte and Buser [18] who measured the dimensions of the sockets using computed tomography. post extraction of single teeth without flap opening. Regarding provisionalization, all authors cited in this review are in common agreement on the importance of this step; an implant-supported provisional prosthesis has the ability to modify the architecture of the peri-implant mucosa, as well as the formation of an adequate emergence profile (which will allow correct hygiene and, consequently, peri-implant health) and also improves the formation of the interdental papilla. Its only “disadvantage” would be the increased cost and time of treatment for the patient, yet, considering all the benefits that provisionalization brings, it is an investment that is certainly worth making [25-28].
Conclusion
This review showed that there is no consensus regarding the best surgical time for installing implants in anterior regions, however, there seems to be a tendency to obtain better results when dental implants are placed immediately or early (4-8 weeks after extraction) in flapless surgeries. It is also suggested that guided bone regeneration should be performed simultaneously with the installation of implants, as a strategy for maintaining the architecture of the peri-implant hard tissues. Connective tissue grafts proved an important role in maintaining vestibular tissue volume, ensuring higher scores on the PES index, reducing the risk of midfacial mucosal recession, and promoting better esthetic results by reinforcing the marginal tissues, since a thin gingival architecture is the clinical reality of most patients. It can be inferred that when it comes to the provisionalization, there is an agreement on the relevance of this stage, since it’s fundamental in the conditioning of the peri-implant soft tissues, favors the formation of interproximal papilla and provides an adequate emergence profile for the prosthesis, favoring the correct hygiene of the region and, consequently, adding peri-implant health. Despite all these considerations, the specialist must be careful when choosing the treatment plan, especially in the patient with a high smile line and final gingival biotype. This patient profile should be “excluded” from high-risk procedures. All these approaches aim to achieve a treatment with good aesthetic results, and satisfaction and fulfillment of the patient’s expectations is the key factor to classify a treatment with dental implants as successful or unsuccessful.
References
- Marković A, Mišić T, Janjić B, Šćepanović M, Trifković B, et al. (2022) Immediate Vs Early Loading of Bone Level Tapered Dental Implants with Hydrophilic Surface in Rehabilitation of Fully Edentulous Maxilla: Clinical and Patient Centered Outcomes. J Oral Implantol 48(5): 358-369.
- Fürhauser R, Florescu D, Benesch T, Haas R, Mailath G, et al. (2005) Evaluation of soft tissue around single-tooth implant crowns: the pink esthetic score. Clin Oral Implants Res 16(6): 639-644.
- Cho SC, Froum SJ, Kamer AR, Loomer PM, Romanos G, et al. (2015) Implants in the Anterior Maxilla: Aesthetic Challenges. Int J Dent 2015: 152420.
- Farmer M, Darby I (2014) Ridge dimensional changes following single-tooth extraction in the aesthetic zone. Clin Oral Implants Res 25(2): 272-277.
- Tettamanti S, Millen C, Gavric J, Buser D, Belser UC, et al. (2016) Esthetic Evaluation of Implant Crowns and Peri-Implant Soft Tissue in the Anterior Maxilla: Comparison and Reproducibility of Three Different Indices. Clin Implant Dent Relat Res 18(3): 517-526.
- Brånemark P I, Hansson B O, Adell R, Breine U, Lindström J, et al. (1977) Osseointegrated implants in the treatment of the edentulous jaw. Experience from a 10-year period. Scand J Plast Reconstr Surg Suppl 16: 1-132.
- Schulte W, Kleineikenscheidt H, Lindner K, Schareyka R (1978)The Tübingen immediate implant in clinical studies. Dtsch Zahnarztl 33: 348-359.
- Ibrahim A, Chrcanovic BR (2021) Dental Implants Inserted in Fresh Extraction Sockets versus Healed Sites: A Systematic Review and Meta-Analysis. Materials (Basel) 14(24): 7903.
- Schropp L, Isidor F, Kostopoulos L, Wenzel A (2005) Interproximal papilla levels following early versus delayed placement of single-tooth implants: a controlled clinical trial. Int J Oral Maxillofac Implants 20(5): 753-761.
- Mangano F, Mangano C, Ricci M, Sammons RL, Shibli JA, et al. (2012) Single-tooth Morse taper connection implants placed in fresh extraction sockets of the anterior maxilla: an aesthetic evaluation. Clin Oral Implants Res 23(11): 1302-1307.
- Cosyn J, Eghbali A, De Bruyn H, Dierens M, De Rouck T (2012) Single implant treatment in healing versus healed sites of the anterior maxilla: an aesthetic evaluation. Clin Implant Dent Relat Res 14(4): 517-526.
- Belser UC, Grütter L, Vailati F, Bornstein MM, Weber HP, et al. (2009) Outcome evaluation of early placed maxillary anterior single-tooth implants using objective esthetic criteria: a cross-sectional, retrospective study in 45 patients with a 2- to 4-year follow-up using pink and white esthetic scores. J Periodontol 80(1): 140-151.
- Arora H, Ivanovski S (2018) Evaluation of the influence of implant placement timing on the esthetic outcomes of single tooth implant treatment in the anterior maxilla: A retrospective study. J Esthet Restor Dent 30(4): 338-345.
- Barone A, Toti P, Marconcini S, Derchi G, Saverio M, et al. (2016) Esthetic Outcome of Implants Placed in Fresh Extraction Sockets by Clinicians with or without Experience: A Medium-Term Retrospective Evaluation. Int J Oral Maxillofac Implants 31(6): 1397-1406.
- Pommer B, Heuberer S, Nahler L, Watzek G (2012) How much bone loss can be prevented by alveolar ridge preservation? Systematic literature review and meta-analysis. ImplantNews (2012): 795-799.
- Roccuzzo M, Gaudioso L, Bunino M, Dalmasso P (2014) Long-term stability of soft tissues following alveolar ridge preservation: 10-year results of a prospective study around no submerged implants. Int J Periodontics Restorative Dent 34(6): 795-804.
- Chu SJ, Salama MA, Garber DA, Salama H, Sarnachiaro GO, et al. (2015) Flapless Postextraction Socket Implant Placement, Part 2: The Effects of Bone Grafting and Provisional Restoration on Peri-implant Soft Tissue Height and Thickness- A Retrospective Study. Int J Periodontics Restorative Dent 35(6): 803-809.
- Chappuis V, Engel O, Reyes M, Shahim K, Nolte LP, et al. (2013) Ridge alterations post-extraction in the esthetic zone: a 3D analysis with CBCT. J Dent Res 92(12 Suppl): 195S-201S.
- Hingsammer L, Pommer B, Fürhauser R, Mailath-Pokorny G, Haas R et al. (2018) Single tooth implants in the esthetic zone following a two-stage all flapless approach: A retrospective analysis. Clin Implant Dent Relat Res 20(6): 929-936.
- Chen H, Gu T, Lai H, Gu X (2022) Evaluation of hard tissue 3-dimensional stability around single implants placed with guided bone regeneration in the anterior maxilla: A 3-year retrospective study. J Prosthet Dent 128(5): 919-927.
- Seyssens L, De Lat L, Cosyn J (2021) Immediate implant placement with or without connective tissue graft: A systematic review and meta-analysis. J Clin Periodontol 48(2): 284-301.
- Noelken R, Moergel M, Pausch T, Kunkel M, Wagner W (2018) Clinical and esthetic outcome with immediate insertion and provisionalization with or without connective tissue grafting in presence of mucogingival recessions: A retrospective analysis with follow-up between 1 and 8 years. Clin Implant Dent Relat Res 20(3): 285-293.
- Seyssens L, De Lat L, Cosyn J (2021) Immediate implant placement with or without connective tissue graft: A systematic review and meta-analysis. J Clin Periodontol 48(2): 284-301.
- Abdelwahab D, Ezz AlArab A, El Nahass H (2023) Soft tissue esthetics around immediately provisionalized delayed implants with and without connective tissue graft: A randomized clinical trial pilot study. Clin Implant Dent Relat Res 25(1): 11-22.
- Jemt T (1999) Restoring the gingival contour by means of provisional resin crowns after single-implant treatment. Int J Periodontics Restorative Dent 19(1): 20-29.
- Wittneben JG, Buser D, Belser UC, Brägger U (2013) Peri-implant soft tissue conditioning with provisional restorations in the esthetic zone: the dynamic compression technique. Int J Periodontics Restorative Dent 33(4): 447-455.
- Furze D, Byrne A, Alam S, Brägger U, Wismeijer D et al. (2019) Influence of the fixed implant-supported provisional phase on the esthetic final outcome of implant-supported crowns: 3-year results of a randomized controlled clinical trial. Clin Implant Dent Relat Res 21(4): 649-655.
- González-Martín O, Lee E, Weisgold A, Veltri M, Su H (2020) Contour Management of Implant Restorations for Optimal Emergence Profiles: Guidelines for Immediate and Delayed Provisional Restorations. Int J Periodontics Restorative Dent 40(1): 61-70.
- Pollini A, Morton D, Arunyanak SP, Harris BT, Lin WS (2020) Evaluation of esthetic parameters related to a single implant restoration by laypeople and dentists. J Prosthet Dent 124(1): 94-99.
- Mesquita De Carvalho PF, Joly JC, Carvalho Da Silva R, González-Martín O (2019) Therapeutic alternatives for addressing pink esthetic complications in single-tooth implants: A proposal for a clinical decision tree. J Esthet Restor Dent (5): 403-414.
- Darby I, Chen ST, Buser D (2009) Ridge preservation techniques for implant therapy. Int J Oral Maxillofac Implants 24 Suppl: 260-271.
- Misch CE, Silc JT (2008) Socket grafting and alveolar ridge preservation. Dent Today (10): 146, 148, 150 passim.
- Cafiero C, Annibali S, Gherlone E, Grassi FR, Gualini F, et al. (2008) Immediate transmucosal implant placement in molar extraction sites: a 12-month prospective multicenter cohort study. Clin Oral Implants Res 19(5): 476-82.
- Buser D, Chen ST, Weber HP, Belser UC (2008) Early implant placement following single-tooth extraction in the esthetic zone: biologic rationale and surgical procedures. Int J Periodontics Restorative Dent 28(5): 441-451.
- Araújo MG, Lindhe J (2005) Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol 32(2): 212-218.
- Chappuis V, Gamer L, Cox K, Lowery JW, Bosshardt DD, et al. (2012) Periosteal BMP2 activity drives bone graft healing. Bone 51(4): 800-809.
- Sanz I, Garcia-Gargallo M, Herrera D, Martin C, Figuero E, et al. (2012) Surgical protocols for early implant placement in post-extraction sockets: a systematic review. Clin Oral Implants Res 23(Suppl 5): 67-79.






























