Influence of various implant thread inclination on biomechanical behavior on all on four supported mandibular prosthesis
Sri Sowmya K*, BDS, MDS, Ravi Kumar C, MDS, HOD and Professor, Sujesh M, MDS, Professor, Manaswini Draksharapu, BDS, MDS
Department of Prosthodontics, Kaloji Narayan Rao University of Health Sciences, India
Submission: October 13, 2022; Published: October 26, 2022
*Corresponding author: Sri Sowmya K, BDS, MDS, Department of Prosthodontics, Kaloji Narayan Rao University of Health Sciences, India
How to cite this article: Sri Sowmya K, Ravi Kumar C, Sujesh M, Manaswini D, et al. Influence of various implant thread inclination on biomechanical behavior on all on four supported mandibular prosthesis. Adv Dent & Oral Health. 2022; 15(4): 555919. DOI: 10.19080/ADOH.2022.15.555919
Abstract
Purpose: To evaluate the influence of various implant thread inclinations (0 degree, 3 degree and 6 degree) on biomechanical behavior on all on four supported mandibular prosthesis.
Methodology: A 3D-finite element model of an edentulous mandible was constructed. Four implants were placed in the inter-foraminal region according to “All-on-Four” concept. A framework made of titanium was designed in between the bilateral first molars. A vertical load of 178N was applied between second premolar and first molar region of the distal implants, using load values similar to those of functional bite movements from patients with All-on-4 rehabilitation.
Results: Implants with six degree thread inclination showed increased stress distribution at implant bone interface compared with zero degree thread inclination. Implants with zero degree thread inclination evinced better stress distribution within the implants compared with six degree thread inclination.
Conclusions: As the thread inclination increased from zero degree to six degree better stress distribution was observed at implant bone interface whereas the stress concentration increases within the implant and vice versa.
Keywords:All-on-four concept; Thread design; Thread inclination; Finite element analysis; Biomechanical behaviour
Introduction
Edentulism is “the physical state of jaws following removal of erupted teeth and the condition of supporting structures available for reconstructive or replacement therapies”. It is a common condition seen in elderly which can be the result of many factors such as poor oral hygiene, dental caries, periodontal disease and trauma. The edentulous condition has been shown to have a negative impact on oral and general health of an individual [1]. The traditional treatment for edentulism has been conventional complete removable dentures that helps to 1) restore natural look 2) Improve chewing ability 3) Improve pronunciation and speech 4) Improve self-esteem. Many patients are dissatisfied with the dentures and the common reasons for this dissatisfaction are, areas of discomfort, poor denture stability, poor masticatory performance with reduced bite force resulting in difficulty in chewing, decreased motor control of the tongue, diminished oral sensory function and as well as compromised retention capability [1]. Since few decades, the art and science of dental implants and prosthodontic therapy have made impressive progress in the replacement of the missing dentition. Oral rehabilitation using implants is a well-established and a widely used procedure worldwide today.
Earlier one tooth is replaced using one implant. In edentulous condition desiring to have an implant supported prosthesis with multiple implants may not be feasible in many cases because of anatomical structures in the vicinity, the quality and quantity of the residual bone and increased expenses. Taking these into considerations, many researchers like Brånemark, Dr. Paulo malo focused on restoring the edentulous jaw by decreasing the number of implants without compromising the treatment outcome [2]. According to the original Brånemark protocol, five to six implants should be placed in the interforaminal region of the mandible to support a fixed dental prosthesis. Long-term clinical data on implant and prosthesis survival have con-firmed that fixed prostheses on four implants in the edentulous mandible showed similar results to those of patients treated with more implants [3]. Traditionally, it is well established that the masticatory forces must be directed along the long axis of the tooth or implant which increases the longevity and reduce the amount of bone resorption.
In severely resorbed ridges there is less amount of residual bone available and therefore researchers have been trying to find a suitable alternative to bone augmentation and sinus lift procedures so that additional surgical procedures could be avoided [4].
The “All-on-four” treatment concept advocated by Dr. Paulo Malo in 1993 was developed to maximize the use of available remnant bone in atrophic jaws, allowing immediate function and avoiding ridge augmentation procedures that increase patient morbidity and treatment costs, along with the complications inherent to these procedures. This protocol uses four implants, in the anterior part of complete edentulous jaws to support a provisional, fixed and immediately loaded prosthesis. The two most anterior implants are placed axially, whereas the two posterior implants are placed distally and angled to minimize the cantilever length, and to allow the fabrication of prostheses with up to 12 teeth, thereby enhancing masticatory efficiency [5].
Osseointegration is critical to evaluate implant success. Successful osseointegration from the clinical standpoint is a measure of implant stability, which occurs after implant integration with surrounding bone. Two terms, such as the primary and the secondary implant stability, are related to implant firmness within the bone. Primary stability is associated with the initial mechanical engagement of an implant with the surrounding bone, whereas bone regeneration and remodeling phenomena determine the secondary (biological integrity) stability to the implant. Usually secure primary stability is a precursor for positive secondary stability. Bone quantity and quality, implant geometry, and surgical technique adopted are also among the predominant clinical factors that affect primary stability [6]. The geometric features of an implant influence sufficient initial contact to facilitate primary stability of the implant. It also plays a vital role on implant capacity to withstand forces during the process of osseointegration. Therefore, optimal implant design itself can enhance potential osseointegration process thereby increasing the primary and secondary stability of the implant [7]. An important factor that affects the success of implant therapy is the way occlusal forces are transferred to the bone-implant interface. Threads on an implant body and thread inclination are so designed to maximize initial fixation and bone contact, enhance surface area, and facilitate dissipation of loads at the bone-implant interface. Implant body designs with threaded features convert occlusal loads (axial and non-axial loads) into favourable loads at the bone implant interface. Therefore, thread design plays a critical role when considering long-term load transfer to the surrounding bone [8]. Since, there is limited literature available pertaining to influence of thread inclination on stress distribution around implants, thus this study was undertaken to evaluate the influence of thread inclination on biomechanical behaviour on All on four supported mandibular prosthesis through finite element analysis.
Methodology
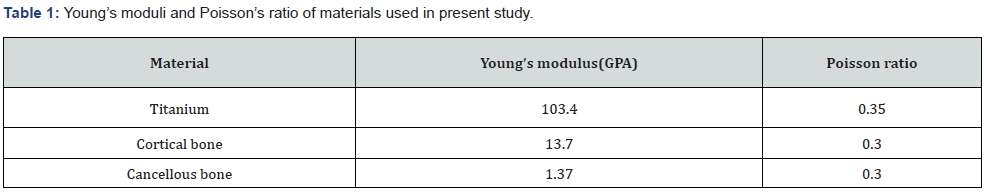
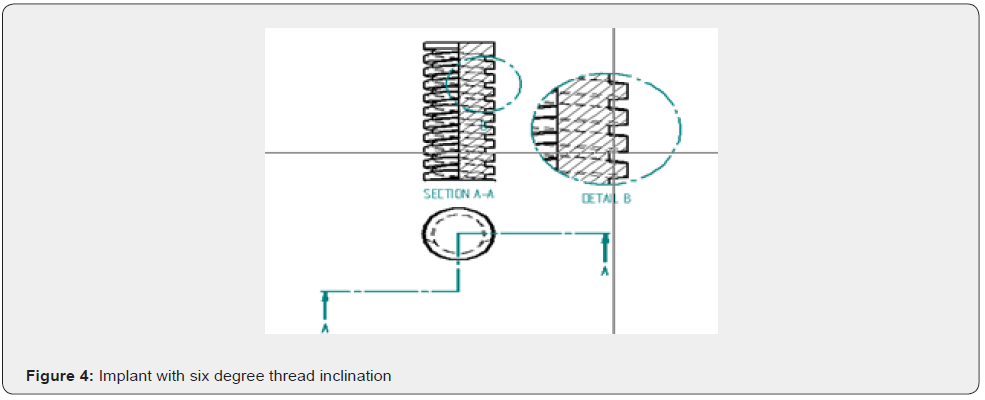
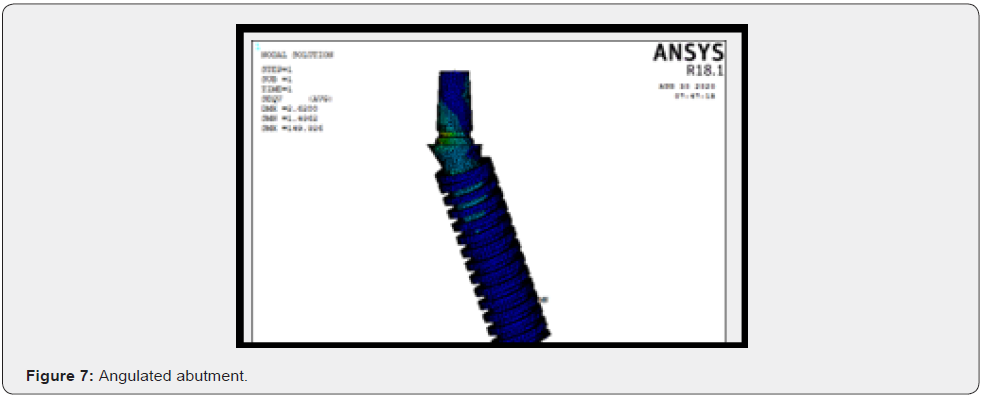
A 3D model of human mandible was simulated from computed tomographic scan data of a cadaver. The images were acquired at small slice intervals (0.5mm increments). The slices were assembled, and a 3D model was constructed by means of modelling software (autodesk fusion). Cortical bone of varying thickness (1 to 1.5mm) was defined around the cancellous core. The structure symmetry permitted the reconstruction of entire mandible. The arch was 70 mm long, 18.9 +/- 3.1 mm high, and 8.5 +/- 1.25 mm wide. A 1.8 +/- 0.4 mm cortical bone layer was established, overlaying the entire mandible, whereas cancellous bone was used in the entire internal structure, simulating type 1 bone in anterior mandible and type 2 bone in posterior mandible (Figure 1 & Table 1). A 3D model of dental implant (Branemark MKIII Groovy, Nobel biocare) was created from measurement data provided by a coordinate measuring machine (Microscribe MX System, immersion).The geometry of Noble biocare solid implants was used as a reference to bulid models of dental cylindric screw type implants with square thread configuration. To carry out a comparative analysis, 3 such models were created where the threads of implants are inclined to various degrees like 0 degree, 3 degree and 6 degree to achieve 3 different configurations in each model respectively (Figure 2-4). Four implants were placed in each model of which two anterior implants were placed bilaterally in the mandibular canine region measuring 10mm in length and 4mm in diameter. The two posterior implants are placed bilaterally measuring 13mm in length and 4mm in diameter were inserted at 4mm anterior to foramina and were tilted distally by 30 degrees relative to occlusal plane (Figure 5). Two straight abutments (multiunit abutment, Nobel biocare) were designed for the axially placed implants at the canine region and two angulated abutments (30 degree multiunit abutment, Nobel biocare) were designed for distally inclined 30 degrees implants that were measured by coordinate measuring machine and simulated in autodesk fusion. Four cylindric titanium abutments (4.30 mm high) were placed on mesial and distal implants. A solid abutment was considered as one unit with the implant (Figure 6 & 7).
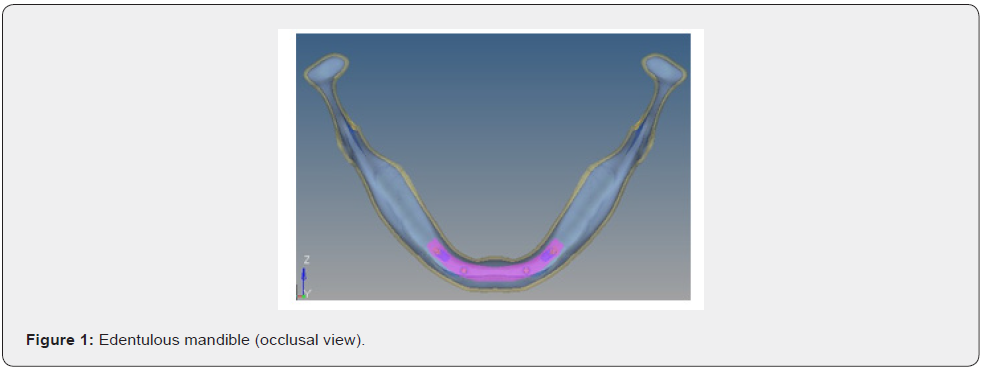
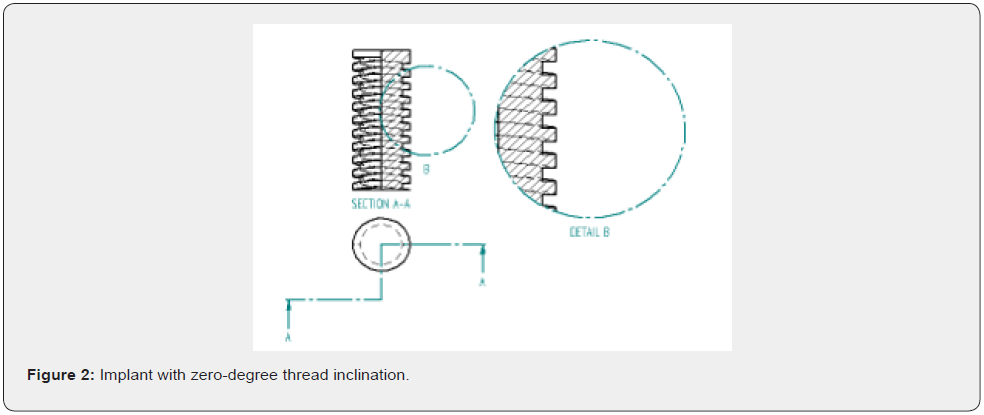
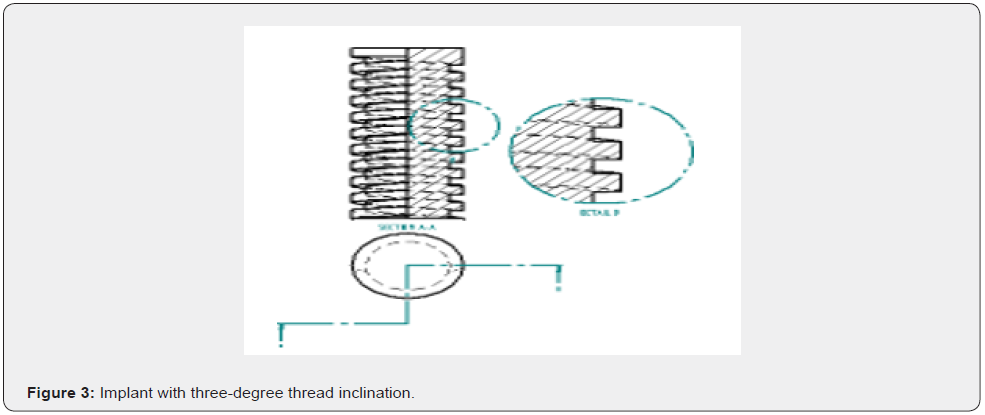


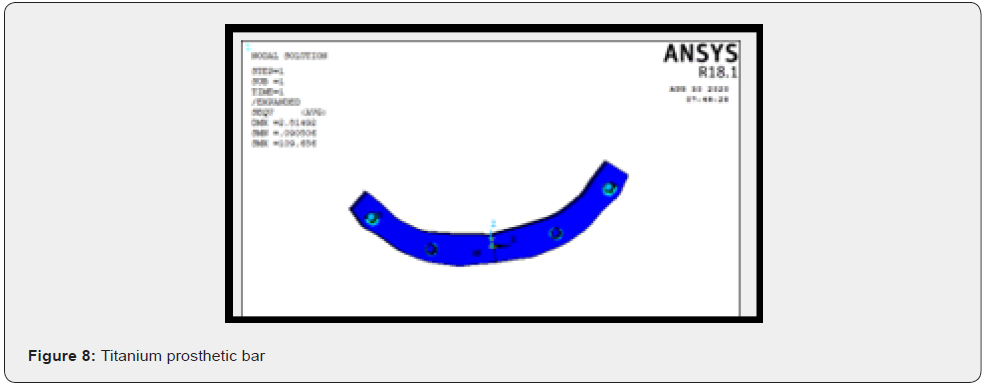
A titanium prosthetic bar measuring 70mm in length, 4mm in height, 6mm in width was designed to simulate as framework joining all the anterior and posterior abutments, including a 3.5 mm long distal cantilever for accommodating 12 masticatory units (Figure 8). Finite element analysis has been proven to be a precise and applicable method for evaluating dental implant systems. This method offers several advantages, including accurate representation of complex geometries, easy model modification and representation of internal state of stress and other mechanical quantities. Biomechanical factors play an important role to prevent undue bone resorption, on to which the implants are anchored. They deal with the stresses within and around implants as well. Bone, a plastic tissue is known to remodel its structure in response to mechanical stimulus. A minimal amount of positive stress has physiologic effect in bone remodelling but excess of stresses could lead to osseous micro damage and induce resorptive modelling and structural failure when it exceeds the tolerance limits of the bone [9].
Boundary conditions
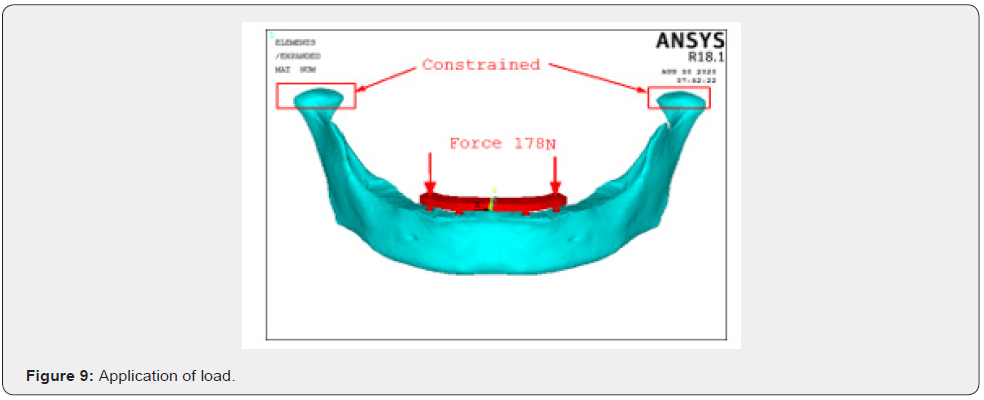
The 3D geometry was exported to FEA preprocessing software and discretized in linear tetrahedral elements. A mesh of approximately 4,79,565 elements and 5,85,089 nodes was generated for the models. All materials were assumed to be linearly elastic, homogenous, and isotropic. Table 1 shows the Young moduli and Poisson ratios of the materials used in the present study. In order to simulate a fully osseointegrated condition, the bone–implant interface was considered completely fixed, and there were no craterlike defects around the implant neck, as well as no gaps in the implant-abutment and abutmentcylinder connections. A perfect-fit situation was assumed among the implants, the bone, and the prosthetic structure. To evaluate and compare the distribution of stresses within the prosthesis, superstructure-abutment interface and bone–implant interface, a loading conditions of 178N was applied vertically in the first molar region in each of the 3 models, using load values similar to those of functional bite movements from patients with All-on-4 rehabilitation. (Figure 9). To decrease false stress concentrations in the area of load application, the load was divided into two force vectors of 89 N each (posterior loading).
To simplify the analysis, data of the mandibular rami were not incorporated into the model, and the section was removed at a 45-degree angle at the gonial angle. The cross section was assumed as the restraint and the model were considered to be fixed in this area, so that any movement or rotation in this area was impossible. The implants were assumed to be 100% osseointegrated and nodeto- node connection was considered at the bone-implant interface. The results of the mathematical solutions were converted into visual results characterized by degrees of color, ranging between red and blue, with red representing the highest stress values. The results of the simulations were evaluated in terms of von Misses equivalent stress levels within the superstructure, at the superstructure abutment interface, at the abutment implant interface, and at the bone–implant interface.
Results
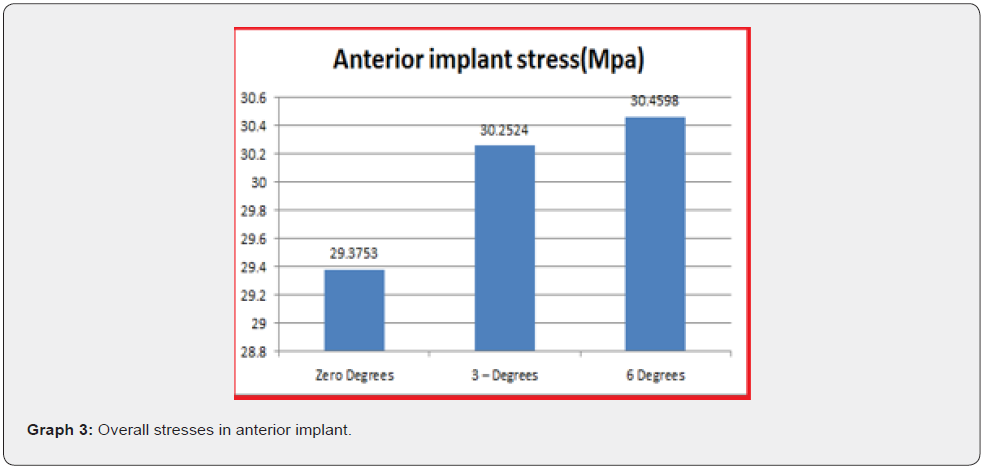
Stress distribution in finite element models comes in numerical values and in colour coding. Maximum values of von Misses stress are denoted by red colour and minimum value by blue colour. In between, the values are represented by bluish green, greenish yellow, and yellowish red in ascending order of stress distribution (Table 2-5), (Graph 3 & 4).



Stresses within superstructure
Highest stress was concentrated at the connector of the superstructure. But, in relative comparision, implants with three degree thread inclination exhibited lesser stresses when compared to zero degree and six degree thread inclinations (Figure 10).
Stress at superstructure abutment interface
Higher stresses were concentrated at superstructureabutment interface in implants with six degree thread inclination compared with implants with zero degree thread inclination followed by implants with three degree thread inclination (Figure 11).

Stresses at implant abutment interface
Stresses at implant abutment interface were found to more in distal implants with zero degree thread inclination and least stresses were exhibited by anterior implants with three degree thread inclination (Figure 12).
Stresses at implant bone interface
Stress distribution at implant bone interface under vertical loading of 178N shows highest stress concentration in distal implants with six degree inclination and comparatively lesser stresses were noticed in anterior implants with zero degree thread inclination (Figure 13).
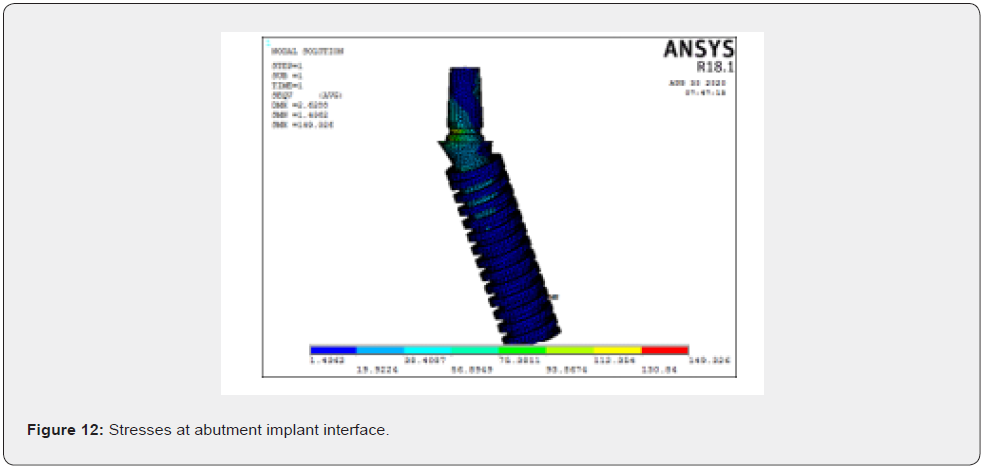
Stresses on cortical bone
Stress distribution in cortical bone under vertical loading of 178N showed highest stress concentration in distal implants with zero-degree thread inclination and comparatively lesser stresses were noted in anterior implants with six degree thread inclination (Graph 1).
Stresses on cancellous bone
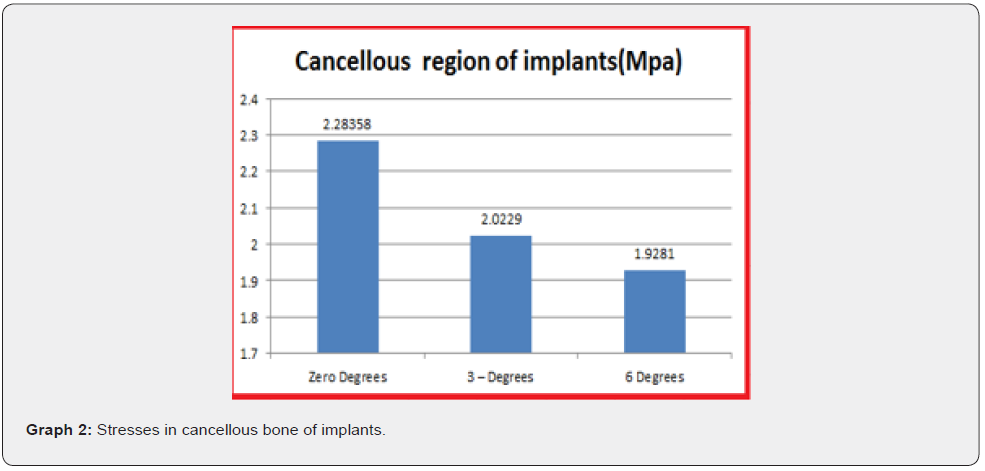
In general, the stresses in cancellous bone were lesser when compared to cortical bone. But in relative comparison anterior implants with six-degree inclination showed lesser stresses in cancellous bone when compared to distal implants with zerodegree thread inclinatioin (Graph 2).
Discussion
As reported in the literature, FE analysis has been frequently employed to study stress and strain distributions in endosteal implants, by following different approaches and analyzing different constructs. This simulation facilitates study of the interaction between the implant and bone tissues in areas which are not accessible to direct experimentation. Numerical simulations also readily allow application of various masticatory loads. The direction of load plays a significant role in the peak stress level, which could vary by up to 85%. The current study analyzed stress and strain distribution of all on four supported mandibular prosthesis with various implant thread inclinations of zero degree, three degree, six degree at various interfaces like implant bone interface, implant- abutment interface and within the superstructure.
For this 3 edentulous mandibles with 12 titanium implants were designed by the software. Each edentulous model contained four implants out of which two implants were placed in canine region at 90 degrees measuring 10mm in length and 4mm in diameter and distal implants measuring 13mm in length and 4mm in diameter tilted to 30 degrees. The thread inclinations of the implants in each model varied from zero degree, three degree, six degree respectively. 12 multiunit abutments measuring 3.5mm height and 4mm in diameter were also designed by the same software. A titanium prosthetic bar measuring 70mm in length, 4mm in height, 6mm in width was designed to simulate a framework splinting all the anterior and posterior abutments, including a 3.5 mm long distal cantilever for accommodating 12 masticatory units.
To evaluate and compare the distribution of stresses within the prosthesis, abutment – implant interface and bone–implant interface, a loading conditions of 178N was applied vertically in the first molar region in each of the 3 models, using load values similar to those of functional bite movements from patients with All-on-4 rehabilitation. The cortical bone with interposed trabecular bone is considered isotropic, homogenous, linearly elastic body. The cortical layer is taken as 2mm thick surrounding the cancellous bone and assumed as type 1 bone in anterior mandible and type 2 bone in posterior mandible. The arch was 70 mm long, 18.9 +/- 3.1 mm high, and 8.5 +/- 1.25 mm wide. While young’s modulus of cortical and cancellous bone is taken as 1.37x104 and 1.37x103 respectively and poisson’s ratio for both is considered 0.3. Young’s modulus of 11000 Mpa and poisson’s ratio of 0.35 are taken. The youngs modulus of the titanium abutment remained the same and poisson’s ratio was 0.28.
When a force of 178N was applied in between second premolar and first molar region, increased stress concentration was observed at implant bone interface in implants with zero degree thread inclination because, the force applied cannot be resolved into components since the distribution of contact force occurs only along one axis (X- axis). Moderate stresses were observed for implants with three degree thread inclination because all though the contact force is resolved into dFCos 3 degrees and dFSin 3 degrees, the sin component shows very least distribution of forces, therefore stress distribution is not that efficient with three degree thread inclination. Minimal stress concentration was observed at bone implant interface with six degree thread inclination due to dissipation of the horizontal force(contact force) resolved into vector components i.e. dFcos 6 degrees and dFsin 6 degrees and the stress is distributed between these components which was in accordance with the study conducted by Michele cali et al. [10] Generation of higher stresses was observed within the superstructure and abutment implant interface in implants with six degree thread inclination followed by implants with three degree thread inclination because of absence of dispersion medium (bone) resulting in concentration of stresses at these region. Whereas for implants with zero degree thread inclination, minimal concentration of forces were observed within the super structure which could be due to the distribution of forces occuring along the long axis of the implants. In all the implants greater stresses where observed in cortical bone than in cancellous bone because of porous nature of the latter.
Clinical implications
a) When using all- on four concept appropriate case selection is mandatory.
b) Using longer implants in all-on four concept helps to achieve better implant stability due to increased bone implant contact
c) Implants with thread inclinations helps to reduce stresses in the surrounding bone that enhances long term success of implant.
d) Implants with six degree thread inclination helps to reduce stresses better when compared to zero degree and three degree thread inclination.
Limitations of the study
Even though finite element analysis is an accurate and precise method for analyzing structures, distribution of forces, yet, the present study has some limitations.
i. The implant was assumed to be 100% osseointegrated which is never found in clinical situation.
ii. The cortical bone, cancellous bone was considered to be homogenous and isotropic which is contrary to clinical situations.
iii. Only static loads of 178N was applied between second premolar and first molar region which is far more different from dynamic loading encountered during function.
iv. In this present study only, linear forces were taken into consideration, but non- linear forces are also encountered during function.
v. The present study did not take into consideration the implants with thread inclinations above six degrees.
Conclusions
The conclusions of the present study are as follows:
a) Implants with six degree thread inclination exhibited greater stress distribution at implant-bone interface, and maximum stress concentration within the superstructure.
b) Implants with zero degree thread inclination evinced increased stress distribution within the superstructure and higher stress concentration at implant- bone interface.
Greater stress distribution was observed in cancellous bone than in cortical bone.
References
- Mukherjee S, Banerjee S, Chatterjee D, Deb S, Swamy SN, et al. All-on-Four Concept in Dental Implants.
- Thumati P, Reddy M, Mahantshetty M, Manwani R (2015) " All-On-4/DIEM 2" A concept to rehabilitate completely resorbed edentulous arches. Journal of Dental Implants 5(1): 76-81.
- Horita S, Sugiura T, Yamamoto K, Murakami K, Imai Y, et al. (2017) Biomechanical analysis of immediately loaded implants according to the “All-on-Four” concept. Journal of prosthodontic research 61(2): 123-132.
- Asawa N, Bulbule N, Kakade D, Shah R (2015) Angulated implants: an alternative to bone augmentation and sinus lift procedure: systematic review. Journal of clinical and diagnostic research: JCDR 9(3): ZE10.
- Soto-Peñaloza D, Zaragozí-Alonso R, Peñarrocha-Diago M, Peñarrocha-Diago M (2017) The all-on-four treatment concept: Systematic review. Journal of clinical and experimental dentistry 9(3): e474.
- Javed F, Ahmed HB, Crespi R, Romanos GE (2013) Role of primary stability for successful osseointegration of dental implants: Factors of influence and evaluation. Interventional Medicine and Applied Science 5(4): 162-167.
- Ryu HS, Namgung C, Lee JH, Lim YJ (2014) The influence of thread geometry on implant osseointegration under immediate loading: a literature review. The journal of advanced prosthodontics 6(6): 547-554.
- Lakha TA, Kheur MG, Kheur SM, Patankar AH, Burhanpurwala M (2016) Effect of Implant Design and Thread Geometry on Stress Distribution in the Surrounding Bone-A Photoelastic Stress Analysis Connections 13: 14.
- Geng JP, Tan KB, Liu GR (2001) Application of finite element analysis in implant dentistry: a review of the literature. The Journal of prosthetic dentistry 85(6): 585-598.
- Calì M, Zanetti EM, Oliveri SM, Asero R, Ciaramella S, et al. (2018) Influence of thread shape and inclination on the biomechanical behaviour of plateau implant systems. Dental Materials 34(3): 460-469.






























