Clinical Endodontic Applications of 3D Printing, A Review
Aniuska Tobin1* and Max Einbinder2
1Assistant Professor and Predoctoral Program Director, Division of Endodontology, School of Dental Medicine, UConn Health, Farmington CT, USA
2Candidate of SDM class of 2024, UConn Health, Farmington CT, USA
Submission: July 01, 2022; Published: July 13, 2022
*Corresponding author: Aniuska Tobin, DDS, University of Connecticut School of Dental Medicine, Farmington CT, USA
How to cite this article: Aniuska T, Max E. Clinical Endodontic Applications of 3D Printing, A Review Adv Dent & Oral Health. 2022; 15(4): 555917. DOI: 10.19080/ADOH.2022.15.555917
Abstract
Current research suggests an emerging value of 3D printed guides use in the endodontic field. Computer-aided design and manufacturing technologies can be used to create 3D printed guides with endodontic clinical applications. Guided endodontics is a term that has gained popularity and involves 3D planning, 3D models and 3D printed guides. The aims of this review were to asses all current applications of 3D guide usage in endodontics, determine when 3D guide use is effective in clinical endodontic settings, evaluate the possible incorporation of 3D guides in the didactic endodontics setting, and analyze the future of this technology. A literature search was conducted on PubMed, Ovid, Google Scholar, and Scopus. A total of 75 published papers were included, including one systematic review, four different reviews in planning, comparative reviews and in digital technology: one observational study, forty-three case reports, nine case series, and seventeen preclinical studies. These studies show that implementing 3D printing in endodontics opens the door to promising techniques with highly predictable outcomes and a low risk of iatrogenic damage, especially in very complex cases.
Keywords:Endodontics; 3D printing; Guided endodontics
Abbreviations:3D: Three dimensional; CAD: Computer-aided design; CAM: Computer-aided manufacturing; CBCT: Cone beam computed tomography; DICOM: Digital Imagining Communication in Medicine; MTA: Mineral trioxide aggregate; SLA: Stereolithography
Introduction
Digital imaging and 3D printing are rapidly revolutionizing dental practice. Fabrication of dental appliances such as veneers, crowns, and bridges using dental CAD-CAM technology is not new; however, new and improved systems are becoming available in the market very quickly and with that significantly increased the precision of the production of these dental appliances translating into better fit and function, and usually at a lower cost than was possible with other traditional lab methods. An emerging application for this technology is in the field of endodontics; specifically, the fabrication of 3D printed guides. A well-made guide can significantly improve the quality and safety of endodontic procedures.
Duret and Preston were the first dentists to document the use of computer-aided design/computer-aided manufacturing (CAD/CAM) in dentistry. They began their endeavors in the early 1970s and used the technology to create dental prostheses [1]. CAD/CAM technologies used to be dominated by closed systems (e.g., CEREC) which require their own proprietary data acquisition and processing software; however an important part of the rapid evolution of 3D printing is the availability of open systems, that allows the use of Digital Imagining Communication in Medicine (DICOM) files to be use for local manufacturing or printing at distant laboratories [2,3]. In the current review, most of the published literature dealt with open-source software (Blue Sky Plan, coDiagnostix, etc.), though closed system software (e.g., DENTSPLY Sirona) was also employed in some studies.
The term “guided endodontics” was first introduced in 2016 by Krast et al. and Zehnder et al. as a treatment option for calcified teeth with periapical pathosis [4]. Amid this explosion in the adaptation of 3D printing in endodontics are applications to various endodontic clinical problems that have posed severe difficulties for operators in the past. We will review a number of these clinical scenarios. Finally, given the apparent promise of 3D printed appliances, we will argue that instruction in their use should be incorporated into didactic clinical instruction. In sum, it was hoped that this review would shed light on the current, and future, utility of this fast-growing technology.
Materials and Methods
To conduct this review, we searched the following databases: PubMed, Scopus, Ovid, and Google Scholar. Search terms were:‘clinical endodontic applications of 3D printings,’ ‘endodontic surgical guide,’ ‘guided endodontic surgery,’ ‘guided endodontic access’ and ‘guided endodontic auto transplantation’. The search included publications from January 1st, 2017, until June 25th, 2022, in order to review new literature published on the application of 3D surgical guides in endodontics. The first literature review on this topic was published in February 2018 and only included one case report Anderson et al. [2]. Articles for the present review had to be published in English or were excluded. Duplicate articles were removed manually.
Eligibility criteria
Studies were included that appeared after entering the search criteria (key term, English language, and appropriate time period) and at least one of the following:
i. Explored the utility of 3D printed surgical guides in guided endodontic access, guided endodontic microsurgery, and guided endodontic auto transplantation.
ii. Compared treatment accuracy of 3D printed guides to conventional methodology,
iii. Case reports, case series, and preclinical in vitro and ex vivo studies.
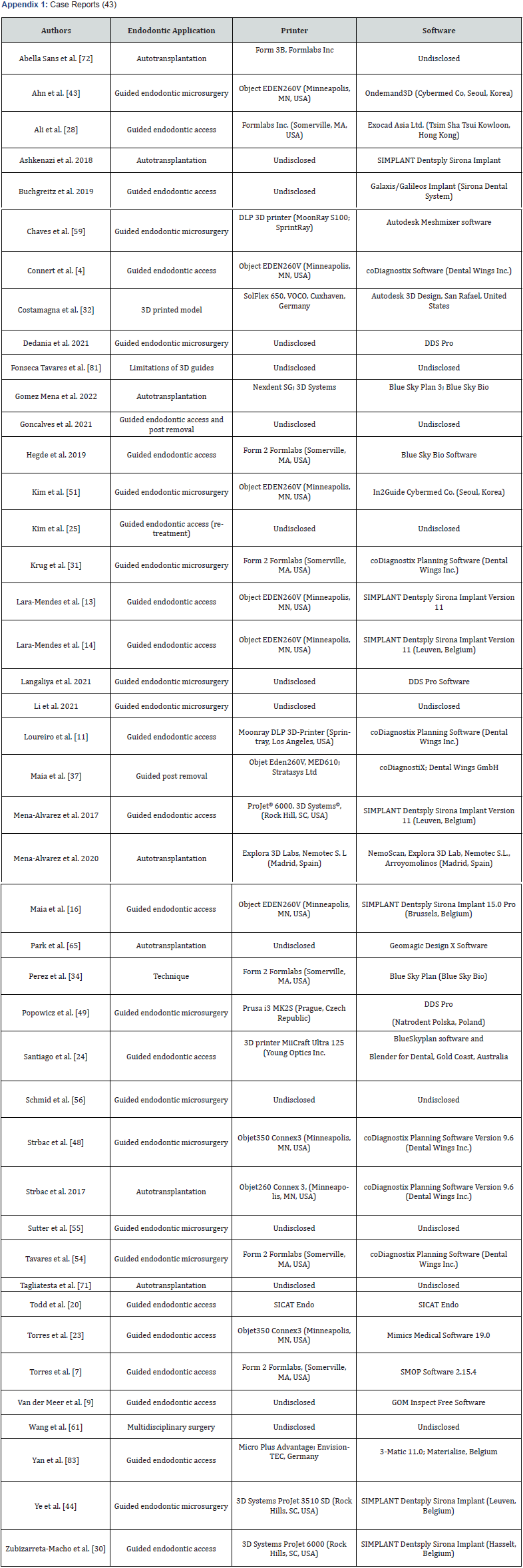
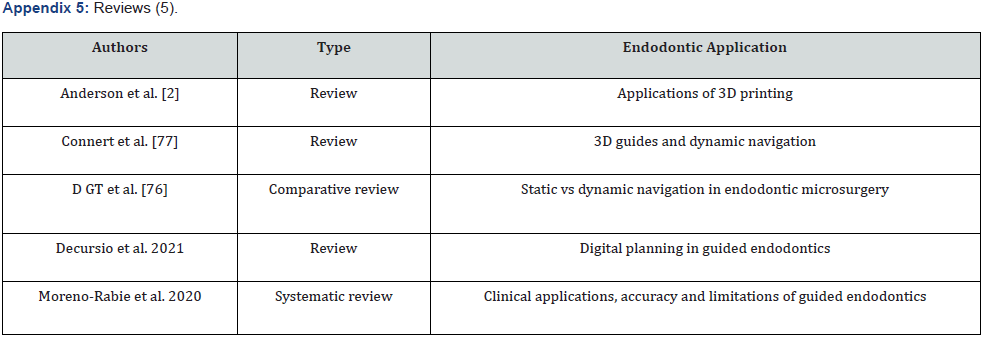
Seventy-five published papers were included in this review see Appendix 1. This included one systematic review on the application and limitations of guided endodontics Moreno-Rabie et al. 2020, four different reviews in planning, comparative reviews and in digital technology; and one observational study Buchgreitz et al. The remaining articles were case reports (forty-three), case series (nine), and preclinical studies (seventeen).
Review of clinical endodontic applications
Guided endodontic access
Pulp canal obliteration, calcific metamorphosis, and pulp canal calcification are all terms that describe increased apposition of tertiary dentin in the root canal system. Increased apposition of dentin decreases the translucency of the tooth and causes discoloration; this is the most common clinical sign of pulp canal obliteration. Orthodontic treatment, aging, dental caries, and dental trauma can increase pulp canal calcification; 15-40% of patients who undergo dental trauma will develop pulp canal obliteration [5]. Approximately 60-80% of teeth will remain asymptomatic and require no endodontic treatment. However, the remaining 20-40% of teeth will develop pulp necrosis with radiographic signs of periapical disease [6,7]. This obliteration makes it more challenging to negotiate canals, complicates root canal treatment, and increases the risk of iatrogenic events. In addition, 20% of perforations occur when trying to locate canals of severely calcified incisors [8].
Using the conventional approach to root canal treatment, the clinician relies on visualization skills and memorization of tooth anatomy to isolate canals. Abnormal pulp canal anatomy and the small size of the canals make the root canal treatment more difficult [9]. Many potential complications can arise during root canal treatment: access cavity overextension, iatrogenic perforation, missed root canals, file separation, and root canal deviation from the original path [10]. Guided endodontic access offers a safer and more predictable approach to endodontic treatment [4,5,11,12]. The access point, orientation of the bur, and depth can be predetermined; this minimizes the error inherent in conventional visualization and free-hand treatment. Current best practice emphasizes minimizing structure loss, which can be difficult to accomplish for inexperienced clinicians.
Precision guides can help significantly in these cases. In one preclinical study, Connert et al. [4] observed that severe calcified canal localization was 92% successful using guided endodontics; compare to 42% success using conventional free-hand treatment. In addition, the overall treatment time was reduced and there was less tooth structure loss while using guided endodontics, and there were no statistically significant differences in performance between the clinicians when using the guided approach [12]. The access, cleaning and shaping of severe calcified root canal systems can be simplified with this technique [13]. Several studies report similar findings, indicating that guided endodontics promotes accurate and replicable positioning, and allows access to smaller cavities regardless of the level of experience of the clinician [4,9,12,14-16].
Another ex vivo study concluded that guided endodontic access preserved a statistically significant amount of dental tissue in maxillary molars; however, there was no statistically significant difference in the amount of dental tissue preserved in mandibular incisors [17]. On the contrary, a different ex vivo study using a 3D guided protocol successfully preserved the tooth structure of anterior mandibular incisors by using a surgical guide with a stent that harbored a 0.85mm diameter bur. This allowed for optimal precision in the mandibular incisors, compared to traditional burs that are 1.2 – 2.4 mm in diameter. This diameter is too large for anterior mandibular teeth and results in excessive loss of radicular tissue [15,8]. This protocol was successfully replicated clinically one year later [4]. Other clinical case studies report successful treatment of molars and premolars at 12 months follow up, they show that guided endodontic therapy can be used to safely and effectively locate calcified root canals in posterior teeth [12,16].
Deviation from the desired drill path can cause iatrogenic damage to the surrounding tooth structure and root perforation, damaging the surrounding periodontal ligament and decreasing the tooth’s chances of survival [19,20]. There were in-vitro studies that demonstrate that guided endodontic access results in less bur deviation than the conventional free-hand method. For instance, Connert et al. had sixty mandibular teeth used and two operators. They had virtually planned the access and produced 3D guides to complete the access. The deviations between the planned- and prepared-access cavities were low, with means ranging from 0.12 to 0.13 mm and no significant difference between the operators. They concluded that microguided endodontics technique is an accurate, fast, and operator-independent tool for accessing root canals [5]. Nayak et al. using 3D endodontic guides to performed guided root canal access in extracted teeth, they found that the deviation between the axis of the planned root canal access cavity and the prepared root canal access cavity was 0.07 ± 0.02 mm [21]. Su et al. in their ex vivo study, also found very low linear deviation in all groups (anteriors, premolars, and molars); however, they found that the apical position had more deviation than the coronal (0.46 mm. vs. 0.13 mm); nonetheless, al canals were accessible and no root canal perforation was observed [22]. This review included one observational study by Buchgreitz et al. that found that guided endodontic access can be precise irrespective of sex, age, tooth number, degree of obliteration, and previous attempts to find and negotiate the root canal in single-rooted teeth [18].
Endodontic surgical guides were suggested only after conventional endodontic treatment using dental microscopes, conventional access and ultrasonic tips fail to access the obliterated canals, however in clinical cases with canal obliteration the use of guided endodontics was essential to preserve tooth structure and reach the calcified canal system without complications [16] (Figure 1). Guides have been effective in allowing treatment in a variety of complex cases, including that of a maxillary lateral incisor with pulp canal obliteration, a maxillary central incisor with root perforation in the middle third, and a pulp canal obliteration in the apical third [11,14,23]. This review included multiple case reports using guides specifically for pulp canal obliteration cases [24-27]. Guided endodontics allows clinicians to gain access to canals they may not have attempted otherwise. The result has been that teeth that might have been lost were ultimately saved [20].

Treatment of dental morphology anomalies
Dental malformations like dens invaginatus and dens evaginatus are rare malformations that create anatomical disturbances that affect the ability to prepare conservative access and, presents with an added complication during root canal treatment. Dens invaginatus is caused by an infolding of the enamel organ into the dental papilla during tooth development. This can cause pulp exposure to the oral environment and abnormal root morphology, making endodontic treatment more difficult [28]. Dens evaginatus in the other hand originates from a proliferation and folding of the inner portion of the enamel epithelium resulting in the formation of ta supernumerary tubercle that contains pulp tissue [29]. In their Endodontic Case Difficulty Assessment Guidelines, the American Association of Endodontics considers treating a tooth with significant deviation from normal tooth/ root form as ‘high difficulty’ in endodontic practice. Greater difficulty can increase the risk of iatrogenic damage during root canal treatment, such as root perforation. In addition, dental morphology anomalies can present with an increased rate of appositional dentin disposition, leading to pulp canal calcification, making it even more challenging to isolate canals.
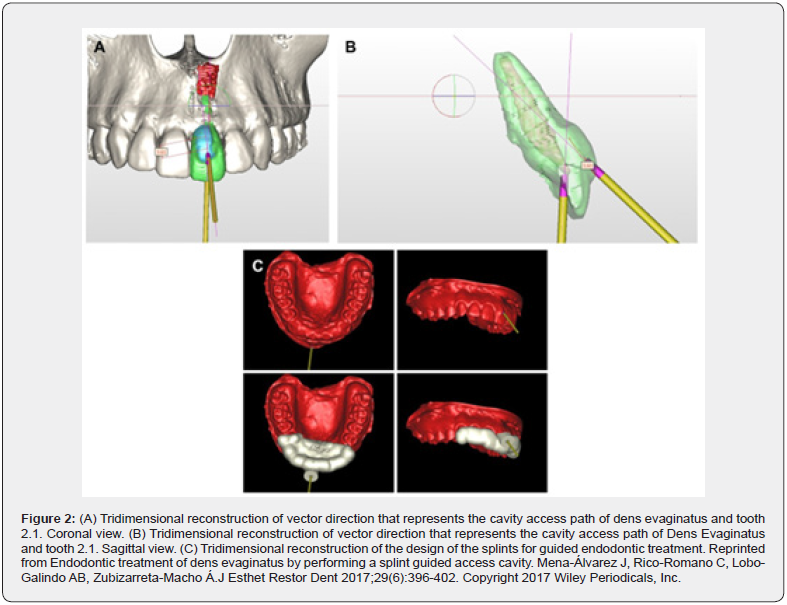
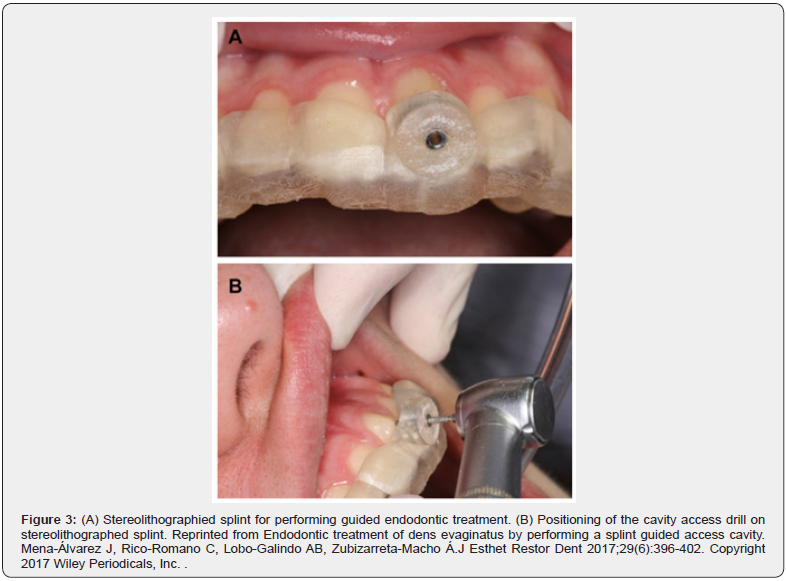
Mena-Alvarez et al. reported a clinical case showing a root canal treatment of a type V Dens evaginatus using CBCT and a 3D printed guided for a conservative access. Tooth #9 presented with a fistulous lesion and had a tubercle at the medial gingival third and on the medial buccal surface. At the 12-month follow-up the buccal defected was repaired, and there was resolution of the periapical radiolucency [29] (Figures 2-3). Another case report of a Type 2 dens invaginatus noted the successful treatment of tooth #10 using guided access. At an 18-month follow-up the authors reported radiographic reduction of the periapical lesion and an absence of clinical signs [30]. Using guided access, treating teeth with these complex root canal anatomies resulted in a successful and simplified endodontic treatment process that might not have succeeded using hands-free methods. Ali et al. presented a case series that used a guided endodontic approach for the conservative management of Type II dens invaginatus by prophylactic sealing of dens with mineral trioxide aggregate (MTA) to prevent any pulpal damage to the tooth due to deep palatal pits which are commonly vulnerable to carious lesion. They concluded that this technique can be a valuable tool for negotiating the dens part, thereby reducing chairside time and more significantly decreasing the risk of iatrogenic damage to the remaining tooth structure [28].
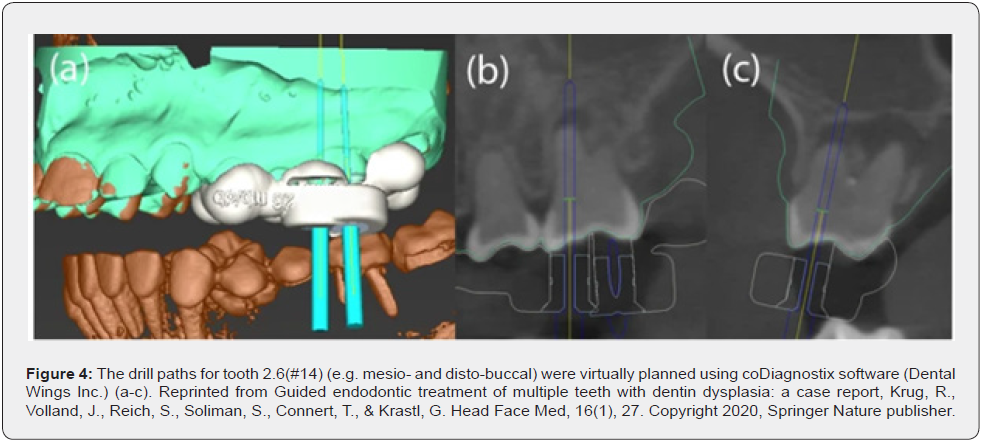
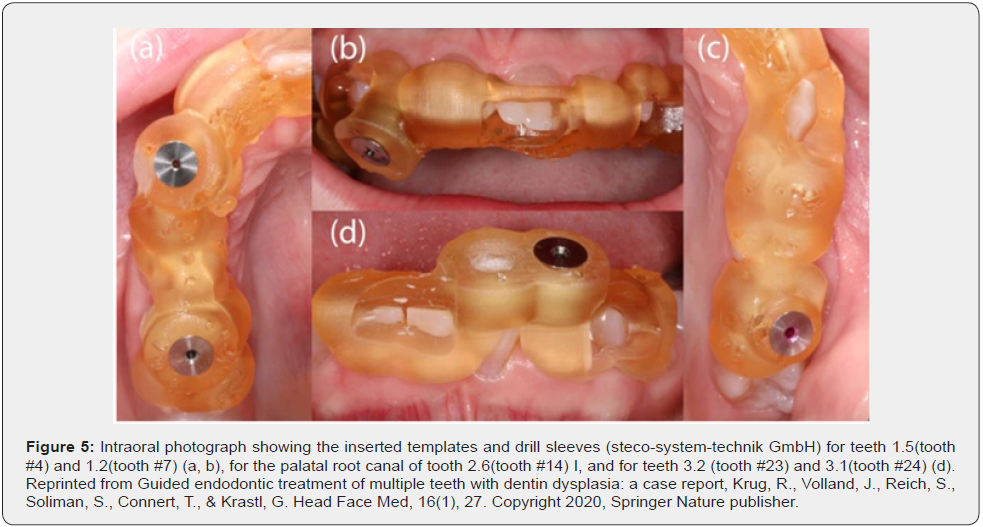
Krug et al. showed the use of the 3D-printed guide for a complex case with dentin dysplasia and pulp canal calcifications with apical radiolucencies in several teeth of a 12-year-old patient. Initially, endodontic therapy was performed on tooth #19 using the conventional approach, resulting in two perforations, whereas guided endodontic treatment on the remaining affected teeth led to a successful outcome. At the one-year follow-up examination the authors noted signs of healing of the endodontic lesions in all root canal treated teeth. They concluded that guided endodontics is a safe and clinically feasible technique that prevents root perforation and enables tooth retention [31] (Figures 4-5).
One case report by Costamagna et al. did not use a guide itself but instead used the 3D models (digital and printed) to allow the clinicians to locate and manage the unusual anatomy of the tooth. The patient presented with second upper molar that had a hidden third canal in the mesial root, the 3D model grant to improve diagnosis and treatment plan allowing the clinician a complete preclinical simulation of the treatment saving time and sound tooth structure [32].
Guided post removals
Fiber-reinforced composite resin posts are used when restoring endodontically treated teeth to provide retention of the core and for root reinforcement, sometimes the removal of these post is necessary to perform a retreatment of a root canal. The conventional method for post removal includes using drill kits specific to the type of post, drills combined with ultrasound, and long-shank endodontic burs with an operating microscope. However, even with these tools, the task remains difficult; root perforation, axis deviation, and roots’ weakening remain serious risks [33]. 3D printed surgical guides enable the clinician to maintain the axis of the drill at precisely the angle at which the post should be removed. In a case report, Perez et al. demonstrated using a surgical guide to clinically remove a fiberglass post from the palatal canal of a maxillary first molar [34]. Later in an in vitro study, Perez et al. showed the reliability of guided endodontic technique to remove bonded fiber-posts. Apical gutta-percha was accessed successfully in 87.5% of the teeth. The mean deviation between the planned and actual drill paths was 0.39 mm coronally and 0.40 mm apically; notably, no root perforations were reported [35].
Cho et al. in case series used the 3D guided to safety remove fiber posts in 4 teeth; it took less than 5 min. to remove the complete each fiberpost removal and there were no perforations. However, they do mention that using the operating microscope is still advisable even with the use of a guide as they observed a slight discrepancy between the planned and actual drilling path [36]. Maia et al. reported the successful removal of the fiberreinforced composite post while preserving the crown [37]; and Goncalves et al. reported the post removal in a molar [27]. They all agreed that removing the fiber post with virtual planning and a 3D guide resulted in a safe and faster procedure.
Guided endodontics in periapical surgery
Endodontic surgery or apicoectomy is indicated to treat apical periodontitis in cases that did not heal after nonsurgical retreatment or, in certain instances, primary root canal treatment with overfilled canals, broken instruments, posts and crown restorations with persisting apical pathosis [38]. Modern advances in surgical techniques include magnification with loupes or microscopes and the use of smaller ultrasonic instruments [39]. The procedure involves navigation through soft tissue and cortical bone, followed by resecting 3mm of the root apex [40,41]. Traditionally, the operator relies on two-dimensional imaging and corrective actions during surgery to locate and resect the apex. The procedure is performed freehanded and is dependent on the clinician’s perceptual ability and hand-eye coordination [42]. Root apices that are near anatomic structures such as the inferior alveolar nerve, greater palatine artery, mental foramen, and maxillary sinus, can complicate treatment and require a high degree of accuracy in their removal. In some instances, the risks involved can contraindicate endodontic surgery. A thick cortical plate can make it more challenging to identify the root end and often results in increased, unnecessary bone removal [43]. Endodontists can struggle to limit damage to healthy tissue and bone while trying to obtain a comfortable visual field [44]. Significant bone removal is associated with more postoperative complications and delayed healing [39].
Pinsky et al. reported the first in vitro study to use of a digitally designed guide in endodontic microsurgery in 2007. They compared access accuracy using guidance versus a conventional method. Results showed that the apex was more precisely and consistently localized utilizing computer guidance versus freehand technique. A significant difference was noted for four of the five examiners [45]. 3D imaging and printed surgical guides allow the operator to visualize the tooth and periapical lesion three-dimensionally, predetermine root access and streamline the procedure. Ackerman et al. also evaluated the accuracy of surgical access using a 3D surgical guided to access the apices of the roots. Dentists performing the access free-hand had a mean deviation of 2.36 mm; however, when performed with 3D surgical guides, they had a mean deviation of 1.73 mm, a statistically significant decrease in deviation (p < 0.001), this study was performed on 48 cadaver’s teeth, which had canals accessed within 4 mm apically [46].
Trephine burs can be incorporated with the 3D surgical guide and perform the osteotomy, root-end resection, and biopsy in a single step; this is known as targeted endodontic microsurgery [42,47]. Targeted endodontic microsurgery provides a direct pathway to the root end needing resection: the osteotomy size, the apical resection level, and the bevel angle can be defined before treatment; thus, limiting damage to the otherwise healthy alveolar bone. Furthermore, the surrounding soft tissue, neurovascular structures, and mucosa can be preserved from enduring unnecessary harm and reduce postoperative pain and swelling [43,44,48,49]. In an in vitro study, Peng et al. showed that when using targeted endodontic microsurgery both length and angle deviations of root-end resection were significantly lower than when no guide was used (P < 0.01). Additionally, when a guide was used, there were no significant differences in the deviations of root-end resection between experienced and inexperienced operators (P > 0.05), allowing inexperienced clinicians to operate at the same caliber as experienced clinicians [50]. Kim et al. also reported targeted endodontic microsurgery to be less technique sensitive [51].
Targeted endodontic microsurgery can also help reduce procedure time and patient chair time. In an ex vivo study, three board-certified endodontists operated on six maxillary and six mandibular teeth using a guided and freehand approach. Targeted endodontic microsurgery reduced surgical time from 14 minutes to 4 minutes and reduced bevel angle and volume over-resection, all with significant p-values [42]. Other authors also showed reduced surgical time in clinical scenarios [43,49]. In a clinical study, endodontic faculty and residents performed targeted endodontic microsurgery in 24 teeth with a 91.7% success rate; only one patient had radiographic evidence of failure. They concluded that targeted microsurgery had similar success to traditional microsurgery [52]. In this clinical cohort 70.8% of cases presented with anatomic complexities that may have precluded treatment without a surgical guide. These cases included a palatal approach to the palatal root of a maxillary second molar, facial roots of maxillary second molars, a mandibular second premolar in close proximity to the mental foramen, and distal roots of mandibular first molars and mandibular second molars [52].
In a series of anatomically challenging scenarios, targeted endodontic microsurgery was used successfully. One case report presented a second mandibular molar with a fractured file segment extruding beyond the apex in the distal canal, and another instrument half-way extruded from the mesial canal, with radiolucencies evident at the mesial and distal root apices. Removal of the instruments and apical surgery were completed with no complications and complete healing at the one year follow up [53]. Additional case reports and case series reported successful targeted endodontic microsurgery in a variety of clinical scenarios [43,54-57]. One in vitro study by Nagy et al. compared commercially available and custom-made trephine burs as over penetration in the bucco-lingual direction can be a risk. They concluded that the use of a custom-made endo-trephine with a stop reduced this error to a safe and acceptable level [58].
Other case reports used only the 3D guide to aid on the osteotomy for endodontic microsurgery with success outcome and simplification of the surgery. One example was a patient with overfilled root canals and extruded gutta-percha in teeth #3 and #4 in close proximity to the maxillary sinus, presented with discomfort, pain, and swelling. Root ends were successfully resected using a guide, with no perforation to the sinus membrane and no postoperative swelling [48]. Chaves et al. reported using a 3D surgical guide, planned only with CBCT, to aid in a microsurgery in tooth #19 that presented with a thick cortical buccal plate; at the one year follow up the patient presented asymptomatic and bone healing was confirmed with a CBCT scan [59].
Kim et al. also noted that a guide could be used as a soft tissue retractor to avoid iatrogenic damage to the soft tissue [51]. The guide can also improve the accuracy of endodontic microsurgery for anterior teeth, especially for complex cases with multiple teeth [44,51,60]. One case report by Wang et al. performed simultaneously endodontic microsurgery of tooth #7 and horizontal bone augmentation of the edentulous area of #8, six months later a guided implant was placed and at the one year follow up, all areas were healed with no post op complications [61]. This innovative, template-based method safely preserved the tooth, bone, and surrounding anatomic structures [53].
Tooth auto transplantation
Auto transplantation of a tooth is indicated to replace a lost tooth in cases with complex tooth fracture, deep dental caries, endodontic treatment failure, and congenitally missing teeth [62]. In young patients, auto transplantation is preferred over an implant due to the donor tooth’s ability to adapt to adjacent teeth eruption and respond to orthodontic treatment. Implants and fixed prosthetic devices are contraindicated in the developing patient, making transplantation the most viable option for patients who are still growing [63]. Additional benefits are that transplanted teeth can maintain vital periodontium, preserve alveolar bone volume, and is often less costly to the patient. Numerous factors can affect the success of auto transplantation, such as stage of donor tooth development, root morphology, and the recipient site’s condition. Iatrogenic damage to the donor’s tooth during the extraction process or implantation at the recipient site can damage the periodontal ligament and lead to progressive inflammation. This can be followed by tooth resorption, pulp necrosis, potential lack of revascularization, and arrested development of the donor’s tooth [64]. The evolution of 3D printing and cone beam computed tomography (CBCT) scanning has opened the door for modifications to the conventional auto transplantation approach. Planning the guided osteotomy utilizing CBCT imaging and specialized software to create an osteotomy guide can minimize bone loss and limit damage to soft tissue and neurovascular structures [63]. This guided approach to auto transplantation is helping to reduce iatrogenic damages that can occur during the procedure.
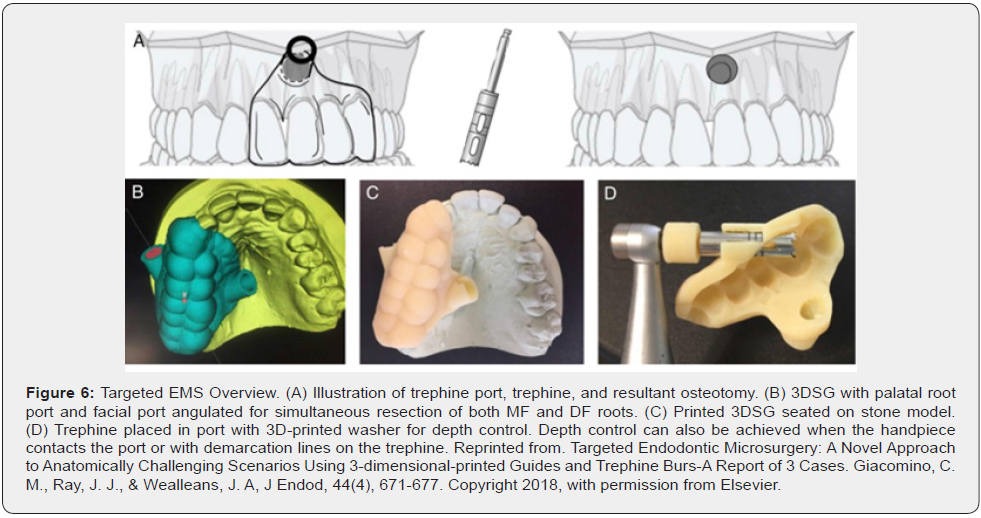
Donor teeth with root development between 1⁄2 and 1⁄3 of the way is ideal for auto transplantation. During extraction of these teeth, there is less damage to the periodontal ligament, and blood supply through the apical foramen remains intact, which aids pulpal healing [65]. Auto transplantation of developing teeth has shown a success rate of over 97% after 1 to 5 years and 96% after ten years [64]. However, adjacent teeth and anatomic structures in close proximity to the recipient site, such as the inferior alveolar nerve, can make it challenging to perform auto transplantation, which can act as a barrier for treatment. Strbac et al. devised a completely digital workflow for guided osteotomy that can be performed on severely impacted teeth in close proximity to adjacent root structures and the inferior alveolar nerve; in this case it was an impacted second premolar. This digitalized approach maintains auto transplantation as a viable treatment option even in complex situations. They also demonstrated that 3D templates for guided osteotomy could ensure an atraumatic uncovering of severely impacted donor teeth; this ensures the vitality of the attached periodontal ligament and protecting vital nerve structures in the vicinity [63] (Figure 6). Another case report of a successful auto transplant of an impacted donor tooth was described by Gomez Meda et al. in this case was a 42-yearold man with a maxillary left canine. Surgical 3D guides were used to expose the donor tooth and also a tooth replica to prepare the recipient area [66]. Guided auto transplantation is also shown to improve the safety and success rate of transplantation of teeth with fully developed roots. This is typically more complex and with a greater risk of iatrogenic damage due to increased trauma during extraction and implantation [65].
3D printed multi-drilling axis surgical guides, donor tooth replicas, and recipient site guides have modified the way auto transplantation procedures can be performed. Extra-oral time of the donor’s tooth has a significant implication on the procedure’s success. The conventional method of auto transplantation involves upwards of 10 minutes of extra-oral time. Extra-oral time greater than 18 minutes can damage donor’s periodontal ligament, decreasing host acceptance of the donor’s tooth. An extra-oral time greater than 30 minutes makes successful auto transplantation very unlikely [67]. Numerous case reports and case series have concluded that 3D printing can help reduce the extra-oral time [63,65,68,69]. Overall treatment time is also reduced; one case report found that conventional auto transplantation takes 40-90 minutes on average while a guided approach takes 30-45 minutes on average [68].
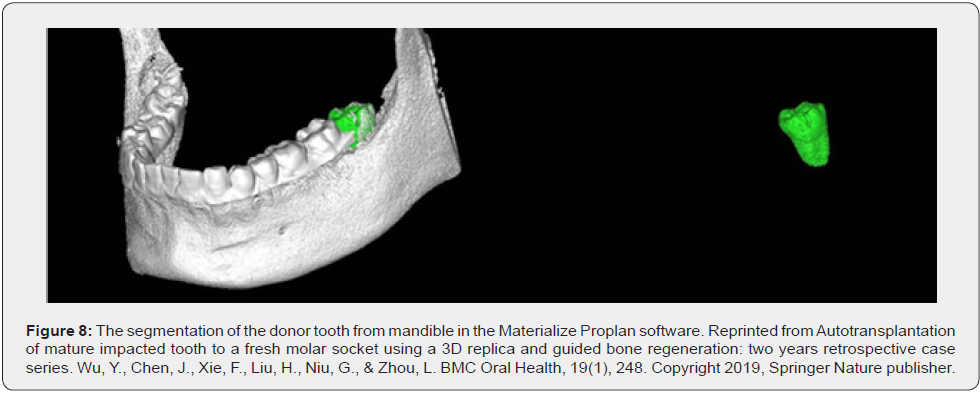
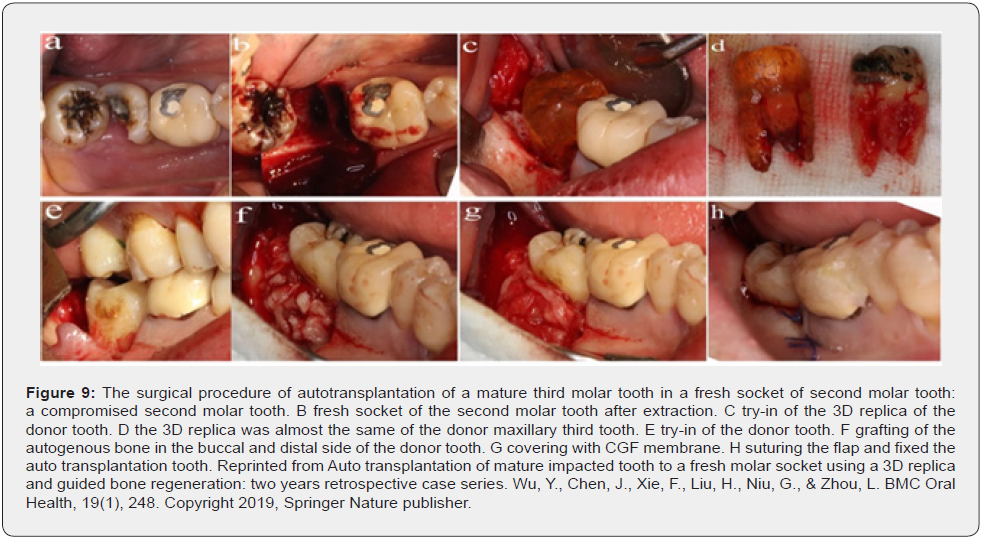
Another way to use 3D printing technology for auto transplantation is to create a replica of the donor’s tooth, this aids in accurate preparation of the recipient site and reduces fit-in attempts; bone loss is minimized as well. Each fit-in attempt damages the periodontal ligament of the donor tooth and the soft tissue surrounding the recipient site. Several clinical studies confirmed success and improved prognosis using a tooth replica [62,63,65,70,71]. Wu et al. performed a completely guided transplantation of mature third molars into fresh molar extraction sockets using 3D replicas. Ten patients underwent the procedure,and all responded normally to percussion, probing depth, mobility, radiography examination, and masticatory function of the auto transplanted tooth at two-year follow-up [69] (Figure 7-8). Abella Sans et al. also showed that guided tooth auto transplantation decreases extra-oral time of the donor tooth and intraoperative fitting attempts and facilitates the technique regardless of the patient age and recipient socket conditions [72].

Guided endodontics and 3D printing in education
Finally, the literature does shed some light on the use of 3D guides in dental education. The introduction of guided endodontic access in the pre-doctoral curriculum can help pre-doctoral students develop their manual dexterity, teach ideal access opening shape, and demonstrate how to preserve tooth structure. Students who perform guided access could also experience a reduction in operating time [5,12]. Guided exercises should complement the traditional curriculum rather than replace it.
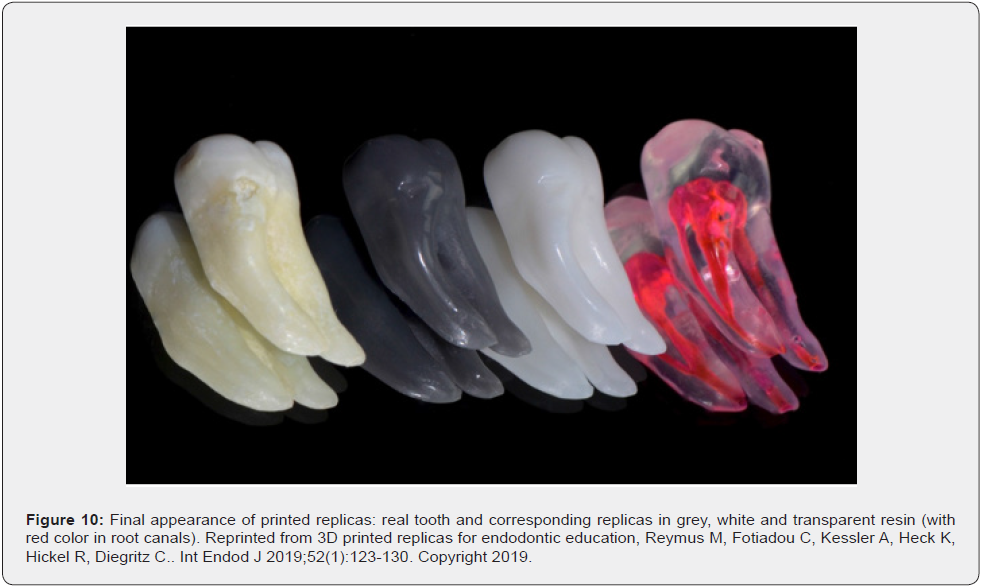
It is typically challenging to find many extracted teeth in need of a specific endodontic treatment. Also, proper disinfection, storage, and preservation of extracted teeth can be costly and time-consuming [2]. 3D printing can be used to create resin teeth with a simulated need for endodontic treatment, with numerous endodontic anatomic variations, which allows dental students to practice with a large number of endodontic procedures. Liang et al. compared root canal obturations of extracted premolars and 3D printed replicas and found that the combination of CBCT and multijet printing technology generated accurate 3D-printed artificial teeth. They concluded that the combination of CBCT and multi-jet printing technology generated accurate 3D-printed artificial teeth, which provided a master gutta-percha with a matching working length and taper for the in vivo root canal fillings [73]. Reymus et al. presented a workflow with feasible manufacturing of accurate 3D printed tooth replicas of extracted human teeth. Students in the third and fourth year of dental school who had trained on extracted molars, or who had performed root canal treatment in patients, were asked to complete root canal procedures in the replicas. Students felt they greatly benefited from using replicated teeth for endodontic training [74] (Figure 9).
This also can apply to endodontics residency training, in which intricate root canal anatomy replicas can be used for advanced training and surgical models used for pre-surgical simulation. Furthermore, the ability to print large quantities of the same prototype can be employed in preclinical research of root canal shaping, different access preparation, and different obturation techniques [2]. Dobros et al. had a review in applications of 3D-printed teeth models in teaching dentistry students. This study included fifteen articles in different areas of dentistry: two studies specific to endodontics. The 3D models were assessed as comparable, or rather comparable to natural teeth. However, in the study by Hanafi et al. the access cavities were asess as much harder than in natural teeth, but 93% of the students recommended using 3D models in teaching endodontics. In overall, the review concluded that 3D models facilitated an alternative to extracted teeth that can be used in many areas of dentistry, including embracing treatment of undue complications like separated instruments or repair of perforations [75]. The continue development in CAD/CAM and 3D printing technology will make possible the use of more realistic alternatives to extracted teeth which will open the door to enhance the students and residents training (Figure 10).
The foresight of guided endodontics
Digital systems such as CBCT, 3D printing, intra oral cameras, etc. have an important place in dentistry now a days. Technology is in constant evolution and 3D printing and guided endodontics are no exception. Dynamic navigation is another realm of guided endodontics that is taking off in modern endodontics; this recent technology, that was initially develop for implant placement, allows to dynamically guide the operator’s instruments to the correct location for root canal localization, root-end resection, etc. in realtime without the need of a guide. The basic setup of the system consists of a preop CBCT scan, stereoscopic camera, a computer platform with a screen, and the respective navigation software [76]. Guided endodontics using 3D printed guides is now known as “static guidance” to differentiate from dynamic navigation that refers to guidance in real time. D et al. in their comparative study of static vs dynamic guidance concluded that apart from the initial upfront cons dynamic navigation is simpler, efficient, errorless, and less technique sensitive than static navigation [76]. Connert et al. in their review of dynamic navigation explains how augmented reality navigation the next step towards evolution of this technology could also be. The augmented reality approach overlays radiographic images and navigation paths, with a view of the operative field in a wearable head-up display or a dedicated microscope. Therefore, the operator can simultaneously visualize the operative field and 3D navigation images without having to look up at a display; clinical implementation in endodontics has only been proposed but not yet implemented [77].
Discussion
The review presented here highlights the utility to endodontics of precision 3D guides. A few caveats should be kept in mind, however. For one thing, the 3D guide’s dimensional accuracy depends on the 3D-printer system used. Jetting-type printers have proven to be the most accurate; photopolymer jetting (PolyJet) 3D printers produced more accurate guides than SLA and Multijet printers [2]. Nonetheless, Stereolithography (SLA) and Multijet printed guides still produce accurate and replicable results when applied to dental procedures [51]. Additional clinical studies with larger sample sizes, standardized procedures, and a greater variety of 3D printers need to be conducted in order to determine what are the most accurate and reliable printers. Currently, there is no gold standard to evaluate 3D printers [2].
The accuracy and efficiency of digital workflow depend on the type of software application used. CoDiagnostiX software was originally developed for implant procedures but has an available add-on that enables the user to superimpose the drill axis over the axis of the root canal. Sicat Endo was specifically designed for complex endodontic treatment. In an in vitro study, Sicat Endo guides successfully located 16/16 root canals for guided endodontic access, and CoDiagnostiX located root canals in 15/16 of the cases (94%). Sicat Endo had less mean deviation of the bur tip compared to CoDiagnostiX. However, CoDiagnostiX required a shorter mean planning time and fewer clicks at 10 min. 50 sec., 107 clicks compared to 20 min. 38 sec., 341 clicks. All of these results had a statistically significant p-value (p < 0.001; p < 0.05, respectively) [78]. The author deemed both programming software packages accurate, effective, and reliable. This was the first study to compare the accuracy of two well-established, commercially available virtual planning software applications for endodontic procedures; specifically, guided endodontic access. Future studies are needed to compare a wider variety of virtual planning software products. Interestingly, the CoDiagnostiX configured guide was milled using additive manufacturing, while the Sicat Endo guide was milled using subtractive manufacturing. The different fabrication methods were possibly responsible for the deviations in results between the two software packages, although both have proven to be highly accurate.
Additional costs and a learning curve are required to use the data software and 3D printers necessary to implement 3D printing into endodontic practice. The turnaround time to receive an outsourced 3D template is approximately two weeks; this makes owning a 3D printer a potential advantage [20]. As of 2019, only PolyJet printers have been used to mill surgical guides used in endodontic microsurgery. However, PolyJet printers can cost over $100,000, this can limit their use in private endodontic practice. Other 3D printers (SLA, DLP, etc.) can cost much less (< $3,500) [79]. The reduced chair time, increased safety, increased procedure quality, and improved tooth prognosis should be taken into consideration. There was one in vitro study in this review by Koch et al. that evaluated the accuracy and precision of four different desktop 3D printers when fabricating stents for guided endodontics, the prices were from $2,800 to $162,500; they concluded that all of the printers tested produced stents for guided access that allowed for a high level of accuracy in obtaining access to the artificial endodontic canal [80]. Future studies should examine the accuracy of surgical guides milled by benchtop printers and used in endodontic scenarios. A cost-benefit analysis on the implementation of guided endodontics in private practice would be beneficial.
The safety and accuracy of guided endodontics rely on the surgical guide’s proper fit. There have been reports of inaccuracy when templates are solely supported by mucosa to guide implant placement; mucosal thickness and resiliency are factors; this can be a source of error in endodontics [5]. Fonseca Tavares et al. in their case report discussed the limitations and management of failures with the 3D guide, they reported that an accuracy error in the CBCT settings, low-quality images, section thickness >1 mm, and an incorrect threshold value can compromise the guided endodontic planning and lead to deviations [81].
Another concern with this technology could be the need to have a CBCT scan to create the 3D guides, which exposes patients to ionizing radiation; one ex vivo study by Leontiev et al. demonstrate that magnetic resonance imaging (MRI) is sufficiently accurate for the detection of root canals using guided endodontics [82]. More comparative studies are needed to validate this approach.
The additive size of the guide, bur, and handpiece may make treatment of posterior teeth unfeasible due to limited interocclusal space [4,14]; currently new designs in the 3D guides are coming up to counter this challenge like single-tooth templates [26] and, 3D inlay guides [83] which were less bulky than traditional 3D guides. Connert et al. stated that surgical guides are most effective on ‘straight rooted’ teeth. The curvature in molars typically occurs in the apical one-third. However, heavy calcifications are typically found in the coronal one-third where the canal is typically straight; thus, the guide can be helpful [13,84]. The heat generated by the bur and handpiece can melt the surgical guide and damage the tooth. The excessive heat can also be harmful to the surrounding periodontal ligament and alveolar bone [85]. To combat this, slow rotation may be use (approx. 250 rpm) [47,86]. As well has been reported implementing an irrigation window in the guide port that allows sterile saline into the drill site for lubrication and cooling purposes [47].
A majority of the publications included in this review were case reports and pre-clinical studies; these types of studies do not offer substantial validity. Ex vivo studies do not accurately replicate alveolar bone, oral mucosa, soft tissue, and granulation tissue well; however, they do provide a good environment for standardization of treatment. Future large-scale, randomized clinical trials with more participants and longer follow-up times are essential to solidify the validity and reliability of the novel techniques mentioned in this review [52]. The continued evolution of endodontics and integration of 3D printing in private practice is dependent on this (Appendix 2-5).
Conclusion
Implementing 3D printing in endodontics opens the door to promising techniques with highly predictable outcomes and a low risk of iatrogenic damage. Results become less technique sensitive, and more teeth could be saved. Endodontic treatment time is reduced, and procedures become less invasive, resulting in greater patient comfort and satisfaction. Larger clinical studies with more participants, longer follow-up time, and standardized methodology are required to establish the validity of the proposed techniques in this review. Further research examining the accuracy of 3D surgical guides printed by affordable, benchtop 3D printers applied to endodontic procedures is also warranted. Lastly, the success of 3D applications in endodontics is dependent on clinicians learning how to use a new design software, thus arguing for the inclusion of instruction in these procedures in dental education. In sum, all these technological advances allow for endodontics to be more precise and be able to execute more complex cases.



References
- Duret F, Preston JD (1991) CAD/CAM imaging in dentistry. Curr Opin Dent 1(2): 150-154.
- Anderson J, Wealleans J, Ray J (2018) Endodontic applications of 3D printing. Int Endod J 51(9): 1005-1018.
- Van Noort R (2012) The future of dental devices is digital. Dent Mater 28(1): 3-12.
- Connert T, Zehnder MS, Amato M, Weiger R, Kühl S, et al. (2018) Microguided Endodontics: a method to achieve minimally invasive access cavity preparation and root canal location in mandibular incisors using a novel computer-guided technique. Int Endod J 51(2): 247-255.
- Connert T, Zehnder MS, Weiger R, Kühl S, Krastl G, et al. (2017)) Microguided Endodontics: Accuracy of a Miniaturized Technique for Apically Extended Access Cavity Preparation in Anterior Teeth. J Endod 43(5): 787-790.
- McCabe PS, Dummer PM (2012) Pulp canal obliteration: an endodontic diagnosis and treatment challenge. Int Endod J 45(2): 177-197.
- Torres A, Lerut K, Lambrechts P, Jacobs R (2021) Guided Endodontics: Use of a Sleeveless Guide System on an Upper Premolar with Pulp Canal Obliteration and Apical Periodontitis. J Endod 47(1): 133-139.
- Kvinnsland I, Oswald RJ, Halse A, Grønningsaeter AG (1989) A clinical and roentgenological study of 55 cases of root perforation. Int Endod J 22(2): 75-84.
- Van der Meer WJ, Vissink A, Ng YL, Gulabivala K (2016) 3D Computer aided treatment planning in endodontics. J Dent 45: 67-72.
- De Toubes KMS, de Oliveira PAD, Machado SN, Pelosi V, Nunes E, et al. (2017) Clinical Approach to Pulp Canal Obliteration: A Case Series. Iran Endod J 12(4): 527-533.
- Loureiro MAZ, Silva JA, Chaves GS, Capeletti LR, Estrela C, et al. (2021) Guided endodontics: The impact of new technologies on complex case solution. Aust Endod J 47(3): 664-671.
- Connert T, Krug R, Eggmann F, Emsermann I, ElAyouti A, et al. (2019) Guided Endodontics versus Conventional Access Cavity Preparation: A Comparative Study on Substance Loss Using 3-dimensional-printed Teeth. J Endod 45(3): 327-331.
- Lara Mendes STO, Barbosa CFM, Santa-Rosa CC, Machado VC (2018) Guided Endodontic Access in Maxillary Molars Using Cone-beam Computed Tomography and Computer-aided Design/Computer-aided Manufacturing System: A Case Report. J Endod 44(5): 875-879.
- Lara-Mendes STO, Barbosa CFM, Machado VC, Santa-Rosa CC (2018) A New Approach for Minimally Invasive Access to Severely Calcified Anterior Teeth Using the Guided Endodontics Technique. J Endod 44(10): 1578-1582.
- Ali A, Arslan H (2021) Effectiveness of the static-guided endodontic technique for accessing the root canal through MTA and its effect on fracture strength. Clin Oral Investig 25(4): 1989-1995.
- Maia LM, de Carvalho Machado V, da Silva NRFA, Brito Júnior M, da Silveira RR, et al. (2019) Case Reports in Maxillary Posterior Teeth by Guided Endodontic Access. J Endod 45(2): 214-218.
- Loureiro MAZ, Elias MRA, Capeletti LR, Silva JA, Siqueira PC, et al. (2020) Guided Endodontics: Volume of Dental Tissue Removed by Guided Access Cavity Preparation-An Ex Vivo Study. J Endod 46(12): 1907-1912.
- Buchgreitz J, Buchgreitz M, Bjørndal L (2019) Guided root canal preparation using cone beam computed tomography and optical surface scans - an observational study of pulp space obliteration and drill path depth in 50 patients. Int Endod J 52(5): 559-568.
- Choi Y, Jeon WS, Cho JM, Jeong HG, Shin Y, et al. (2021) Access opening guide produced using a 3D printer (AOG-3DP) as an effective tool in difficult cases for dental students. J Dent Educ 85(10): 1640-1645.
- Todd R, Resnick S, Zicarelli T, Linenberg C, Donelson J, et al. (2021) Template-guided endodontic access. J Am Dent Assoc 152(1): 65-70.
- Nayak A, Jain PK, Kankar PK, Jain N (2018) Computer-aided design-based guided endodontic: A novel approach for root canal access cavity preparation. Proc Inst Mech Eng H 232(8): 787-795.
- Su Y, Chen C, Lin C, Lee H, Chen K, et al. (2021) Guided endodontics: accuracy of access cavity preparation and discrimination of angular and linear deviation on canal accessing ability-an ex vivo study. BMC Oral Health 21(1): 606.
- Torres A, Shaheen E, Lambrechts P, Politis C, Jacobs R (2019) Microguided Endodontics: a case report of a maxillary lateral incisor with pulp canal obliteration and apical periodontitis. Int Endod J 52(4): 540-549.
- Santiago MC, Altoe MM, de Azevedo Mohamed CP, de Oliveira LA, Salles LP (2022) Guided endodontic treatment in a region of limited mouth opening: a case report of mandibular molar mesial root canals with dystrophic calcification. BMC Oral Health 22(1): 37.
- Kim BN, Son SA, Park JK (2021) Endodontic retreatment of a calcified anterior tooth using a 3D-printed endodontic guide. Int J Comput Dent 24(4): 419-427.
- Velmurugan N, Sundar S, Saumya-Rajesh P, Kasabwala K, Shilpa-Jain DP, et al. (2021) Endodontic management of pulp canal obliteration using a new single-tooth template: A case series. Indian J Dent Res 32(4): 528-532.
- Gonçalves WF, Garcia LDFR, Vieira-Schuldt DP, Bortoluzzi EA, Dias-Júnior LCL, et al. (2021) Guided Endodontics in Root Canals with Complex Access: Two Case Reports. Braz Dent J 32(6): 115-123.
- Ali A, Arslan H, Jethani B (2019) Conservative management of Type II dens invaginatus with guided endodontic approach: A case series. J Conserv Dent 22(5): 503-508.
- Mena-Álvarez J, Rico-Romano C, Lobo-Galindo AB, Zubizarreta-Macho Á (2017) Endodontic treatment of dens evaginatus by performing a splint guided access cavity. J Esthet Restor Dent 29(6): 396-402.
- Zubizarreta-Macho Á, Ferreiroa A, Agustín-Panadero R, Rico-Romano C, Lobo-Galindo AB, et al. (2019). Endodontic re-treatment and restorative treatment of a dens invaginatus type II through new technologies. J Clin Exp Dent 11(6): e570-e576.
- Krug R, Volland J, Reich S, Soliman S, Connert T, et al. (2020) Guided endodontic treatment of multiple teeth with dentin dysplasia: a case report. Head Face Med 16(1): 27.
- Costamagna P, Carpegna G, Bianchi C, Baldi A, Pasqualini D, et al. (2021) Endodontic Treatment of a Molar with Peculiar Anatomy: Case Study with CBCT and 3D Printed Model. J Contemp Dent Pract 22(12): 1477-1482.
- Haupt F, Pfitzner J, Hülsmann M (2018) A comparative in vitro study of different techniques for removal of fibre posts from root canals. Aust Endod J 44(3): 245-250.
- Perez C, Finelle G, Couvrechel C (2020) Optimisation of a guided endodontics protocol for removal of fibre-reinforced posts. Aust Endod J 46(1): 107-114.
- Perez C, Sayeh A, Etienne O, Gros CI, Mark A, et al. (2021) Microguided endodontics: Accuracy evaluation for access through intraroot fibre-post. Aust Endod J 47(3): 592-598.
- Cho C, Jo HJ, Ha JH (2021) Fiber-reinforced composite post removal using guided endodontics: a case report. Restor Dent Endod 46(4): e50.
- Maia LM, Bambirra Júnior W, Toubes KM, Moreira Júnior G, de Carvalho Machado V, et al. (2021) Endodontic guide for the conservative removal of a fiber-reinforced composite resin post. J Prosthet Dent
- Kim S (2010) Contemporary Endodontic Microsurgery: Procedural Advancements and Treatment Planning Considerations. In. Endodontics: colleagues for Excellence AAE.
- Von Arx T, Jensen SS, Hänni S (2007) Clinical and radiographic assessment of various predictors for healing outcome 1 year after periapical surgery. J Endod 33(2): 123-128.
- Tsesis I, Rosen E, Taschieri S, Telishevsky Strauss Y, et al. (2013) Outcomes of surgical endodontic treatment performed by a modern technique: an updated meta-analysis of the literature. J Endod 39(3): 332-339.
- Song M, Shin SJ, Kim E (2011) Outcomes of endodontic micro-resurgery: a prospective clinical study. J Endod 37(3): 316-320.
- Hawkins TK, Wealleans JA, Pratt AM, Ray JJ (2020) Targeted endodontic microsurgery and endodontic microsurgery: a surgical simulation comparison. Int Endod J 53(5): 715-722.
- Ahn SY, Kim NH, Kim S, Karabucak B, Kim E (2018) Computer-aided Design/Computer-aided Manufacturing-guided Endodontic Surgery: Guided Osteotomy and Apex Localization in a Mandibular Molar with a Thick Buccal Bone Plate. J Endod 44(4): 665-670.
- Ye S, Zhao S, Wang W, Jiang Q, Yang X (2018) A novel method for periapical microsurgery with the aid of 3D technology: a case report. BMC Oral Health 18(1): 85.
- Pinsky HM, Champleboux G, Sarment DP (2007) Periapical surgery using CAD/CAM guidance: preclinical results. J Endod 33(2): 148-151.
- Ackerman S, Aguilera FC, Buie JM, Glickman GN, Umorin M, et al. (2019) Accuracy of 3-dimensional-printed Endodontic Surgical Guide: A Human Cadaver Study. J Endod 45(5): 615-618.
- Giacomino CM, Ray JJ, Wealleans JA (2018) Targeted Endodontic Microsurgery: A Novel Approach to Anatomically Challenging Scenarios Using 3-dimensional-printed Guides and Trephine Burs-A Report of 3 Cases. J Endod 44(4): 671-677.
- Strbac GD, Schnappauf A, Giannis K, Moritz A, Ulm C (2017) Guided Modern Endodontic Surgery: A Novel Approach for Guided Osteotomy and Root Resection. J Endod 43(3): 496-501.
- Popowicz W, Palatyńska UA, Kohli MR (2019) Targeted Endodontic Microsurgery: Computed Tomography-based Guided Stent Approach with Platelet-rich Fibrin Graft: A Report of 2 Cases. J Endod 45(12): 1535-1542.
- Peng L, Zhao J, Wang ZH, Sun YC, Liang YH (2021) Accuracy of root-end resection using a digital guide in endodontic surgery: An in vitro J Dent Sci 16(1): 45-50.
- Kim JE, Shim JS, Shin Y (2019) A new minimally invasive guided endodontic microsurgery by cone beam computed tomography and 3-dimensional printing technology. Restor Dent Endod 44(3): e29.
- Buniag AG, Pratt AM, Ray JJ (2021) Targeted Endodontic Microsurgery: A Retrospective Outcomes Assessment of 24 Cases. J Endod 47(5): 762-769.
- Akshayraj L, Chaudhari E, Patel A, Shah J (2021) Computer-aided design-CAM-guided endodontic microsurgical localization and retrieval of two separated instruments from the periapical area of a mandibular second molar. Endodontology 33(22): 112-117.
- Tavares WLF, Fonseca FO, Maia LM, De Carvalho MV, França ASNR, et al. (2020) 3D Apicoectomy Guidance: Optimizing Access for Apicoectomies. J Oral Maxillofac Surg 78(3): 351-358.
- Sutter E, Lotz M, Rechenberg DK, Stadlinger B, Rücker M, et al. (2019) Guided apicoectomy using a CAD/CAM drilling template. Int J Comput Dent 22(4): 363-369.
- Schmid C, Lotz M, Pieralli S, Valdec S (2022) Guided flapless apicoectomy of the palatal root of a maxillary molar: a case presentation. Quintessence Int 53(7): 608-614.
- Kamburoğlu K, Koç C, Sönmez G, Çapçı A (2021) 3D printing in endodontics: report of three clinical cases with innovative approaches. Int J Comput Dent 24(3): 317-328.
- Nagy E, Braunitzer G, Gryschka DG, Barrak I, Antal MA (2021) Accuracy of digitally planned, guided apicoectomy with a conventional trephine and a custom-made endodontic trephine: An in vitro comparative study. J Stomatol Oral Maxillofac Surg.
- Chaves GS, Capeletti LR, Miguel JG, Loureiro MAZ, Silva EJNL, et al. (2022) A Novel Simplified Workflow for Guided Endodontic Surgery in Mandibular Molars with a Thick Buccal Bone Plate: A Case Report. J Endod 48(7): 930-935.
- Dedania MS, Shah NC, Arora A, Pisal N (2020) Three-dimensional printing: A revealing pathway to an unpredictable maze. J Conserv Dent 23(5): 533-537.
- Wang J, Luo Y, Tan X, Wang C, Huangphattarakul V, et al. (2021) Horizontal bone augmentation of the edentulous area with simultaneous endodontic microsurgery of the adjacent tooth: A digitally driven multidisciplinary case report with a 1-year follow-up. Int J Oral Implantol (Berl) 14(4): 435-451.
- Mena ÁJ, Riad DE, Quispe LN, Rico RC, Zubizarreta MA (2020) Technology at the service of surgery in a new technique of autotransplantation by guided surgery: a case report. BMC Oral Health 20(1): 99.
- Strbac GD, Schnappauf A, Bertl MH, Vasak C, Ulm C, et al. (2020) Guided Osteotomy and Guided Autotransplantation for Treatment of Severely Impacted Teeth: A Proof-of-Concept Report. J Endod 46(11): 1791-1798.
- Czochrowska EM, Stenvik A, Bjercke B, Zachrisson BU (2002) Outcome of tooth transplantation: survival and success rates 17-41 years posttreatment. Am J Orthod Dentofacial Orthop 121(2): 110-119.
- Park J, Sangho L, Nanyoung L, Myoungkwan J (2017) Contemporary Approach to Autotransplantation of Teeth with Complete Roots Using 3D-printing Technology. KoreaScience 44(4): 461-468.
- Gómez MR, Abella SF, Esquivel J, Zufía J (2022) Impacted Maxillary Canine with Curved Apex: Three-Dimensional Guided Protocol for Autotransplantation. J Endod 48(3): 379-387.
- Andreasen JO, Paulsen HU, Yu Z, Bayer T, Schwartz O (1990) A long-term study of 370 autotransplanted premolars. Part II. Tooth survival and pulp healing subsequent to transplantation. Eur J Orthod 12(1): 14-24.
- Shahbazian M, Jacobs R, Wyatt J, Denys D, Lambrichts I, et al. (2013) Validation of the cone beam computed tomography-based stereolithographic surgical guide aiding autotransplantation of teeth: clinical case-control study. Oral Surg Oral Med Oral Pathol Oral Radiol 115(5): 667-675.
- Wu Y, Chen J, Xie F, Liu H, Niu G, et al. (2019) Autotransplantation of mature impacted tooth to a fresh molar socket using a 3D replica and guided bone regeneration: two years retrospective case series. BMC Oral Health 19(1): 248.
- Lucas TE, Llaquet M, Muñoz PJ, Somoza J, Satorres NM, et al. (2020) Fully Guided Tooth Autotransplantation Using a Multidrilling Axis Surgical Stent: Proof of Concept. J Endod 46(10): 1515-1521.
- Tagliatesta L (2021) Use of 3D printed replica for autotransplantation: Clinical case in: Oliva N (Editor.) Dental Cadmos pp. 381-388.
- Abella SF, Ribas F, Doria G, Roig M, Durán SF (2021) Guided tooth autotransplantation in edentulous areas post-orthodontic treatment. J Esthet Restor Dent 33(5): 685-691.
- Liang X, Liao W, Cai H, Jiang S, Chen S (2018) 3D-Printed Artificial Teeth: Accuracy and Application in Root Canal Therapy. J Biomed Nanotechnol 14(8): 1477-1485.
- Reymus M, Fotiadou C, Kessler A, Heck K, Hickel R, et al. (2019) 3D printed replicas for endodontic education. Int Endod J 52(1): 123-130.
- Dobroś K, Hajto BJ, Zarzecka J (2022) Application of 3D-printed teeth models in teaching dentistry students: A scoping review. Eur J Dent Educ.
- GT D, Saxena P, Gupta S (2022) Static vs. dynamic navigation for endodontic microsurgery - A comparative review. J Oral Biol Craniofac Res 12(4): 410-412.
- Connert T, Weiger R, Krastl G (2022) Present status and future directions - Guided endodontics. Int Endod J.
- Krug R, Reich S, Connert T, Kess S, Soliman S, et al. (2020) Guided endodontics: a comparative in vitro study on the accuracy and effort of two different planning workflows. Int J Comput Dent 23(2): 119-128.
- Anderson JAW (2019) Targeted Endodontic Microsurgery: A Clinically Oriented Assessment of Three 3D Printers. In: James A, (Editor.), Defense Technical Information Center.
- Koch GK, Gharib H, Liao P, Liu H (2022) Guided Access Cavity Preparation Using Cost-Effective 3D Printers. J Endod 48(7): 909-913.
- Fonseca TWL, De Oliveira MPN, Moreira RA, Braga T, De Carvalho MV, et al. (2022) Limitations and Management of Static-guided Endodontics Failure. J Endod 48(2): 273-279.
- Leontiev W, Bieri O, Madörin P, Dagassan BD, Kühl S, et al. (2021) Suitability of Magnetic Resonance Imaging for Guided Endodontics: Proof of Principle. J Endod 47(6): 954-960.
- Yan YQ, Wang HL, Liu Y, Zheng TJ, Tang YP, et al. (2021) Three-dimensional inlay-guided endodontics applied in variant root canals: A case report and review of literature. World J Clin Cases 9(36): 11425-11436.
- Shi X, Zhao S, Wang W, Jiang Q, Yang X (2018) Novel navigation technique for the endodontic treatment of a molar with pulp canal calcification and apical pathology. Aust Endod J 44(1): 66-70.
- Walton RE (1989) Principles and Practice of Endodontics. W B Saunders Co.
- Buchgreitz J, Buchgreitz M, Bjørndal L (2019) Guided Endodontics Modified for Treating Molars by Using an Intracoronal Guide Technique. J Endod 45(6): 818-823.






























