Oral Rehabilization of Case Affected Severe Advanced Periodontitis with Furcation Involvement and Secondary Occlusal Traumatism
Guey-Lin Hou*
Former Professor, Department of Periodontics, and Graduate Institute of Dental Science, Department of Periodontal Prosthesis, Kaohsiung Medical University, Department of Periodontal & Prosthetic Therapeutic Center, Chang Gung Memorial Hospital, Kaohsiung Medical Center, Taiwan
Submission: March 17, 2022; Published: March 29, 2022
*Corresponding author: Guey-Lin Hou, Former Professor, Department of Periodontics, and Graduate Institute of Dental Science, Department of Periodontal Prosthesis, Kaohsiung Medical University, Department of Periodontal & Prosthetic Therapeutic Center, Chang Gung Memorial Hospital, Kaohsiung Medical Center, Taiwan
How to cite this article: Guey-Lin Hou. Oral Rehabilization of Case Affected Severe Advanced Periodontitis with Furcation Involvement and Secondary Occlusal Traumatism. Adv Dent & Oral Health. 2022; 15(3): 555913. DOI: 10.19080/ADOH.2022.15.555913
Abstract
The aim of this study was to retrospectively investigate the outcomes of a longitudinal study for periodontal and prosthetic therapy treatment of molar furcation Involvement (FI) using crown and sleeve-coping telescopic denture (CSCTD). The effectiveness on the clinical periodontal parameters on the molar abutments before and after periodontal and prosthetic therapy by using the CSCTD for teeth affected with secondary occlusal traumatism (SOT) and FI. The periodontal parameters, probing pocket depth (PPD), probing attachment level (PAL), and alveolar bone levels (ABL) were recorded with respective to teeth examined before and after non-surgical periodontal and prosthetic therapies in a 72-year-old male individual who was diagnosed SAP affected molar FIs and SOT, respectively. The long-term results of 5 years or more, revealed a remarkably greater improvement in the periodontal parameters and ABL in advanced class II and class III FIs on molars. It is therefore concluded that the effective therapy for SAP affected teeth with SOT and FI after using a specific design of the CSCTD combined with periodic nonsurgical periodontal therapy
Keywords:SAP; SOT; FI; CSCTD; Periodontal; Prosthetic therapy
Abbreviations:FI: Furcation Involvement; CSCTD: Crown and sleeve-coping telescopic denture; SOT: Secondary occlusal traumatism; PPD: probing pocket depth; PAL: Probing attach- ment level; ABL: Alveolar bone levels; SAP: Severe advanced periodontitis; RTTs: Root trunk types; FED: Furcation entrance dimension; NSPT: Non-surgical periodontal therapy; TPP: therapeutic provisional prosthesis; GTR: guided tissue regeneration
Introduction
The indications of CSC telescopic denture are characterized as the individuals affected severe advanced periodontitis (SAP) with secondary occlusal traumatism (SOT). These patients got more missing teeth due to SAP affected classes II and III molar FIs, heavy periodontal bone loss, and SOT, respectively. Additionally, there exist more risk factors associated with molar root morphologies, such as root trunk types (RTTs), furcation entrance dimension (FED), molar furcation groove, molar root concavity, alveolar bony defects usually that may adversely respond to non-surgical periodontal therapy (NSPT) because of these sites limited access to debride microbial bacterial plaque and calculus deposits. Former clinical studies [1, 2] reported that deep pockets within the molar FIs have prime to more attachment loss and higher mortality rate when observed over many years [1- 4]. Lindhe & Nyman [5]; Rosling [6] demonstrated that teeth which exhibit advanced destruction but existed healthy periodontium still show a continual increased mobility, splinting of the mobile teeth may be considered. In addition, the former clinical data, reported from Nyman et al. [7] indicated that permanent periodontal prosthesis can effectively improve the hypermobility of isolated abutment teeth, even the prosthesis with a cross-arch design. Predictable and effective therapy of advanced periodontitis on molars affected with SOT and FI, such as tunnel preparation, furcationplasty, root separation, hemisection, and root amputation of these techniques always exhibits discrepancies in the success rates and their complications are still controversial [8-13]. The purpose of this long-term study was to evaluate the periodontal and CSCTD prosthetic therapy for treatment of SAP affected molar with FI and SOT.
Case 1
The patient, a 72-year-old male was referred to our office with recurrent periodontal swelling with pus discharge, maxillary teeth mobility on the left canine, maxillary left second molar and mandibular molar areas (Figures 1a-b) & (Figures 2a-b) with a failed periodontal therapy on August 22, 2006. This patient complained that he had recurrent deterioration of left canine and maxillary molars including gingival swelling, bleeding, and an inability to chew due to teeth mobility during wear wrought wire clasp denture (Figures 3a-b). The past history indicated that two years prior to this time, he had visited many local dental clinics where a condition of suspected advanced adult periodontitis with severely alveolar bone loss had been diagnosed. In addition, although a serial periodontal therapy, such as scaling and root planning was continuously performed by dentists and periodontists, but still in vein. Therefore, extraction of both maxillary second molars was suggested by dentists following failures of periodontal treatment procedures. He was, therefore, introduced to the periodontal clinic of teaching hospital for further treatment.
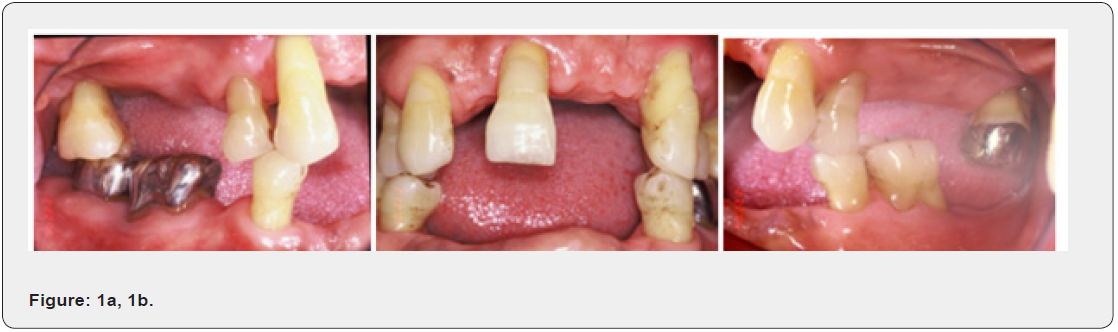
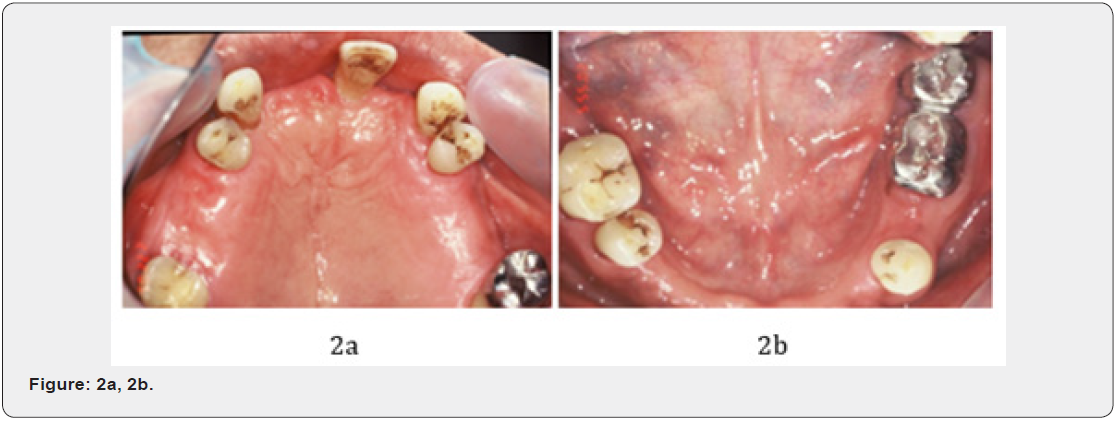
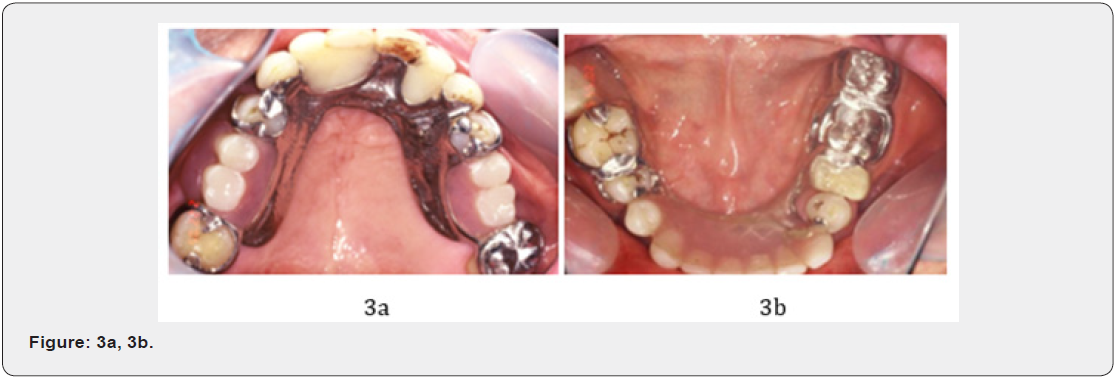
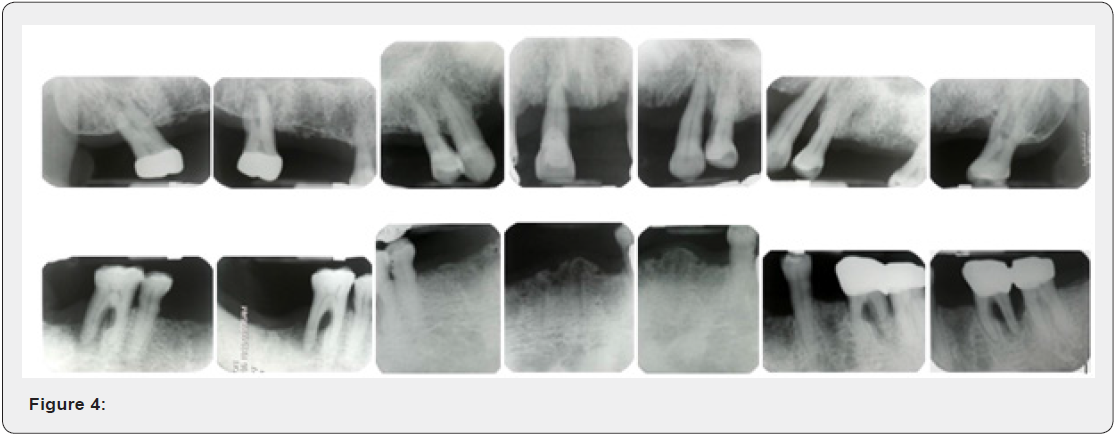
Oral examination revealed that the generalized gingival recession was found on both the maxillary and mandibular anterior and posterior teeth (Figures 1a, b) & (Figures 2a, b). Periodontal status of special chart included Gl, PLl, Cl, mobility test, PPD and PALs were recorded at the initial visit, and at first year after treatment. Periodontal probing depth revealed that molar with class III FI and deep interdental craters were noted at the right (#17) and left (#27) maxillary second molars and at the mesial and buccal furcations. In addition, deep PPD was also found in the Teeth # 14, #13, #11, #23, #24, #36, #37#34, and #45, #46, respectively. Periapical radiographs revealed that SAP with 50%~80% alveolar bone loss (ABL) occur around teeth #17, #14, #13, #11; in addition, 85%-90% ABL was noted at teeth # 23 and #27. Angular bone defect and class III FI were found on the tooth #27, where the buccal and lingual furcations to of molar #36 and #46 with angular bony defect and advanced class III FI were noted. Finally, a diagnosis of generalized severe advanced periodontitis affected SOT and molar FI was made after clinical and radiographic alveolar bone levels evaluations (Figures 1- 4).
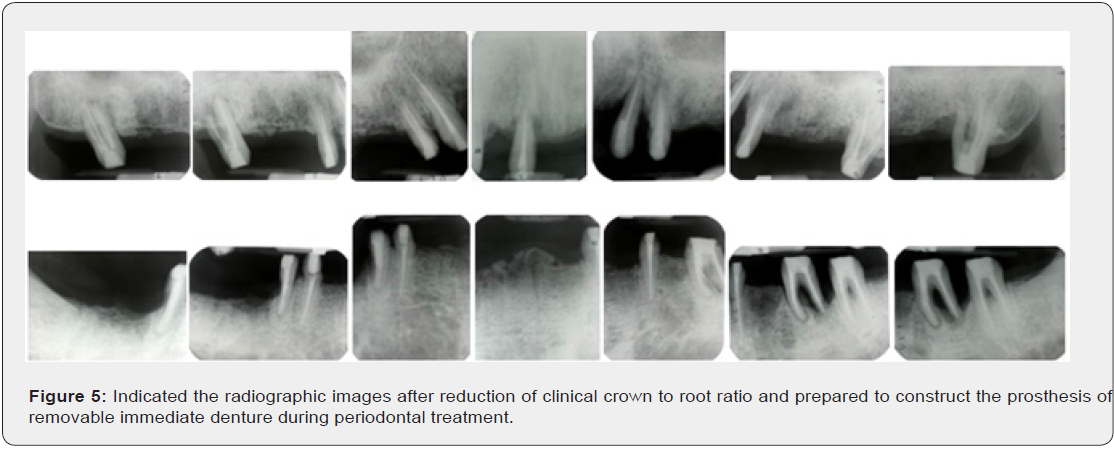
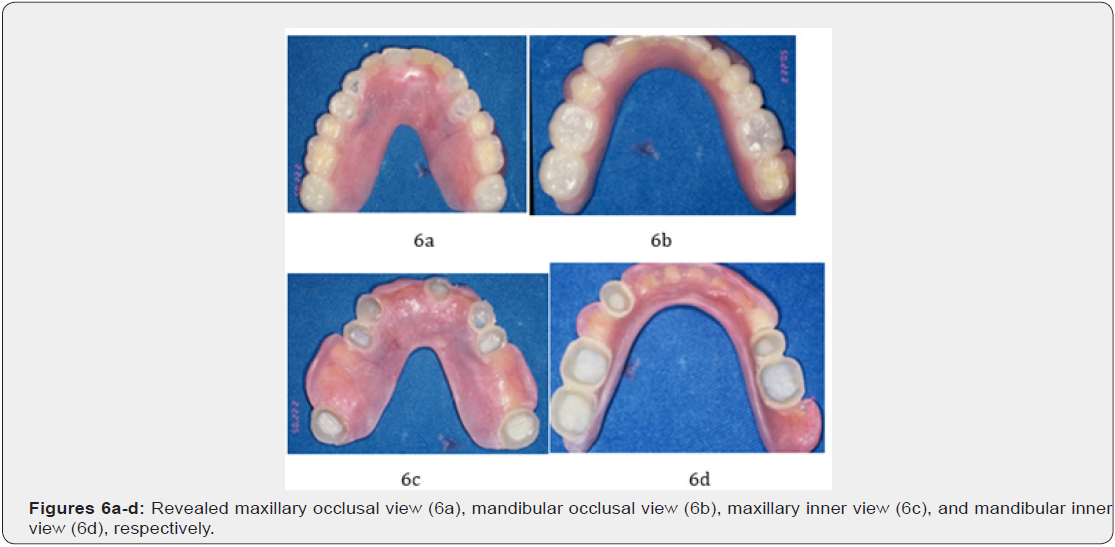
Treatment was initiated after special periodontal charting at the baseline and included oral hygiene instruction, repeated and meticulous scaling and root planning at the disease sites of #17, #14, #13, #11, #23, #24, and #27 and the other dentition during periodontal phase I stage. Reevaluation at 3 months revealed 3 mm, 4 mm, and 3 mm in probing depths for the trifurcations (buccal, mesial, and distal furcations) of the right maxillary second molar (#27) from 7mm, 5mm, 5mm to 4 mm, 3 mm, 3 mm in probing depth for the mesial and buccal furcations. In addition, the PPDs of all maxillary and mandibular teeth were remained within 3mm excepted # 23, #27 and # 36, respectively (Figure 5). The traditional prosthesis commonly used is immediate removable denture as a substituted prosthesis during periodontal treatment after reduction of clinical crown to root ratio (Figure 5) as compared to (Figure 4). In this case, the use of a removable denture design, the application of nonsurgical RSR combined with removable immediate denture (Figures 6a-6d) and other periodontal prosthesis designs for SAP affected SOT and with classes II and III molar FI, can not only effectively reduce the score of PlI, GI, PPDs and PALs, but also in the stability of tooth mobility: Clinical picture revealed a remarkable periodontal healing after periodic meticulous scaling and subgingival curettage. A remarkable healing of furcation-involved areas of #17, #27 and single root of #14, # 13, #11, #23, #24; and mandibular # 37, #34, #26, # 43 were found 5 months later, except # 36 (Figure 5). During maintain phase, the patient cooperated well, good plaque control, and subsequent visits for supportive periodontal treatment every 2 months. The removable prosthesis of maxillary and mandibular arches was constructed after intentional extirpation of right and left maxillary and mandibular teeth was formed (Figure 5), (Figures 6a-6d).
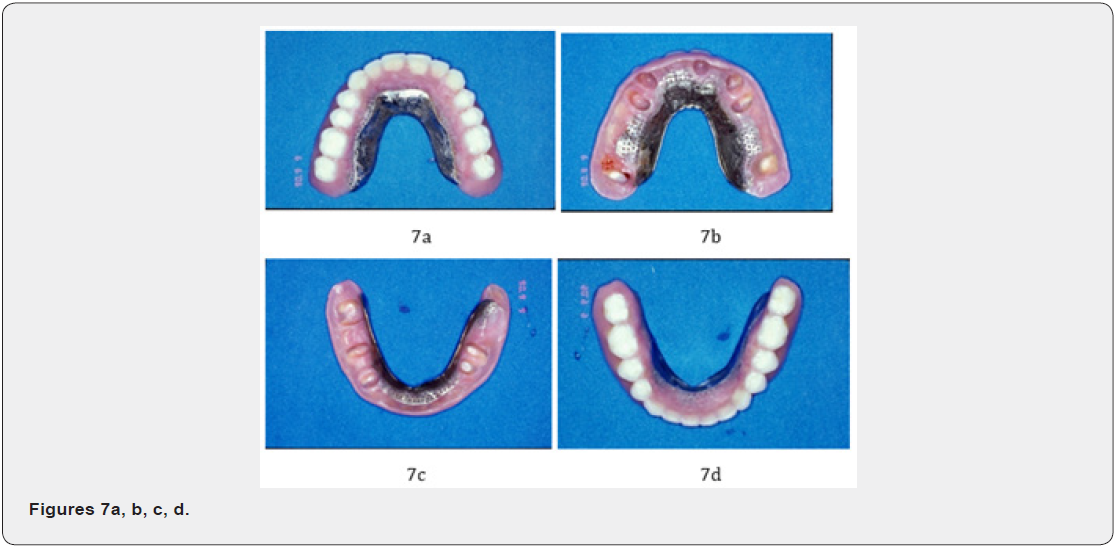
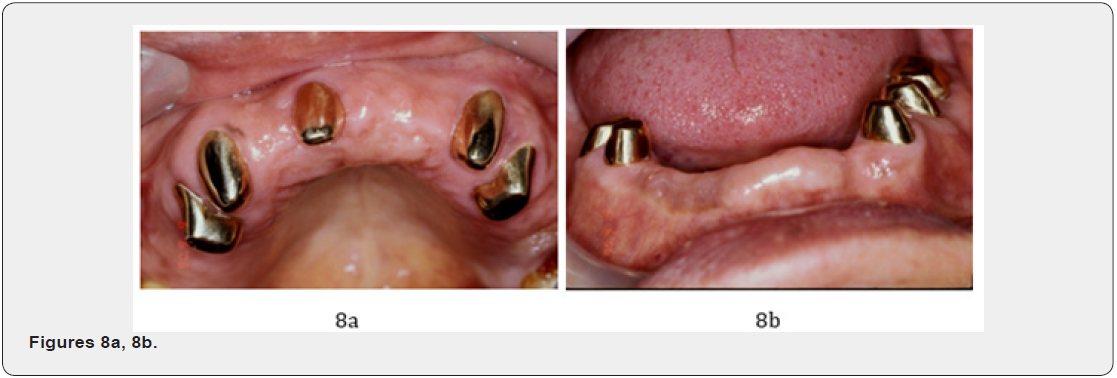
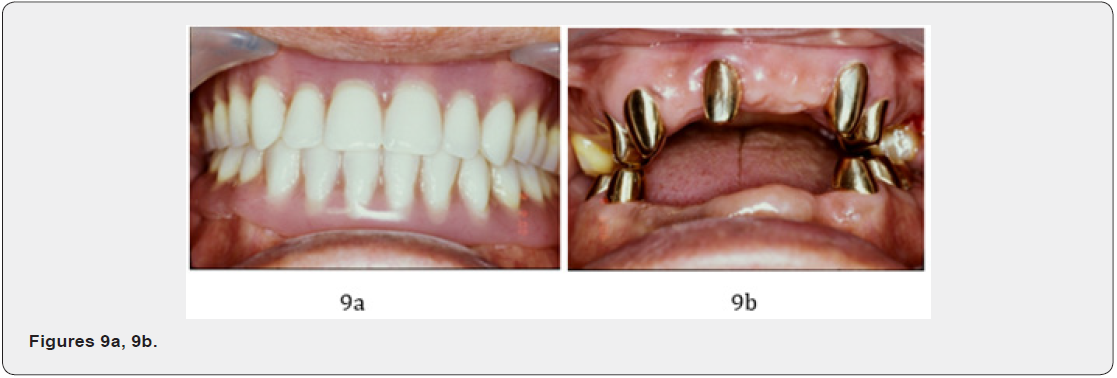
Permanent CSC telescopic denture (CSCTD) was constructed 12 months later. The prominent periodontal healing of trifurcation involvement at # 17, and # 27 was found at the end of therapy 5.3 years; (Figures 7a-d) as well as during the follow-up periods. Clinical picture revealed remarkable periodontal tissues healing around maxillary and mandibular abutments of molars and nonmolar teeth. The remarkable periodontal healing of furcationinvolved areas of the maxillary second molars was found. During maintain phase, the patient cooperated well, good plaque control, and subsequent visits for supportive periodontal treatment every 2 months. Permanent CSC telescopic denture was constructed 1 year later. The remarkable periodontal tissue healing of maxillary and mandibular arches was found at the end of therapy at 5.3 years later (Figures 7-9) as well as during the follow-up periods.
Discussion
The biomechanical theory of therapeutic provisional prosthesis (TPP) is based on the biomechanical design that a good periodontal prosthesis requires a biomechanical design. The traditional provisional prosthesis (TPP) is often designed to keep the tooth subjected to constant torque, bite force, and lateral force damage. Many studies have pointed out that CSCTD is the design that applies biomechanic principles in the current periodontal prosthesis design to overcome the least effect of the torque, bite, and lateral forces on the damage of the fragile bridge tooth [14- 16]. Originally written by Dr. Yalisove [15] proposed in 1966 as an active denture supported by hard and soft tissues, with three main biomechanical principles: 1) conical taper, 2) rotation and rotation between the inner and outer crowns when encountering greater force; 3) secondary splinting and a short lever arm. The shape of the cone is easy to clean, especially in the marginal line of the gingiva, unlike the excessive temporary crown, which is easy to cause the accumulation of dental bacteria although there is a problem of wear, but it can be handled in the way of the inner crown in the future, which not only avoids wear, but also protects the other abutments. The design of the cone, when receiving vertical force, can be borne by the top of the supporting teeth and soft tissues, has a good vertical support, and when the side force is too large, it will slide away in time to avoid directly attaching to the supporting teeth. Also, because there is still a crown, the denture can be properly stabilized than overdentures. The outer wall (or inner crown) and the outer crown and soft tissue groups of the tooth, the tooth structure and the gum can provide appropriate adhesion, and the crown/root ratio can be adjusted to reduce the effect of the lever depending on the condition of the bridge base tooth. When the denture is inserted, the abutments can provide an indirect fixation effect.
Individuals affected SAP were often involved by SOT. Once not only characterized by severe periodontal tissue destruction and reduced of alveolar bone loss but frequently also a remarkably increased teeth hyper-mobility induced a series of angular bony defects, pathological teeth migration associated with clinical and radiographic symptoms. In order to prevent a gradual mechanical loss of teeth in SAP affected SOT due to inadequate alveolar bony support, in addition, to improve the elongation of crown to root ratio to decrease the teeth mobility. The application of fixed and removal TPP or immediate denture for this case affected SAP with SOT and molar FIs after reduced crown to root ratio. The treatment is not only to exclude the source of infection for the affected area to reduce the inflammatory response, but also to alleviate or eliminate the abutment teeth of SOT, which are called occlusal therapy. Using primary or secondary splinting or with good complement design to eliminate abnormal occlusal force, lateral force, and torque force, stabilize its functional occlusion, reduce teeth mobility and reduce patient discomfort, is the treatment of teeth with SAP, especially for patients with molar FI, it is imperative. The more reliable treatment method for the serious invasion of the molar FI of the molar as mentioned in the first section is RSR, but at this time, if it is reshaped with a fixed cementum till necessary to face the problem that the molar furcation areas controlled by personal and dentist plaque, so how to apply the design of periodontal prosthesis to permanently solve the problem of molar furcation lesion treatment and prevent the problem of post-treatment complications is the main consideration in the treatment of periodontal disease.
There is often a high degree of uncertainty in the treatment of periodontitis on molar region, the main reasons include: 1) the complex anatomical morphology of the molars; 2) Clinically there is often no suitable instrument to enter this area to do root debridement; 3) When the molar furcation is involved, it is almost impossible to perform a complete debridement, or even surgically try to completely remove the root calculus and periodontal bony defects; 4) After surgical and non-surgical treatment of molar FI lesions, residual dead spaces, dentists and patients are unable to performed professional and personal plaque control. There are uncertainties in the treatment of molar with class II and III furcation involvements, and classes II and III furcation involvements are the most challenging in treatment. In general, the treatment methods can be roughly summarized as follows: guided tissue regeneration (GTR), tunnel preparation, root RSR, bone grafts of the furcal defect, and growth factors therapy. The following is a review according to the above several methods.
Pontoriero [17]; Caffesse et al. [18] have proposed that there are good treatment results in the treatment of secondary invasion areas of the molar furcations by GTR. Metzler et al. [19] have also proposed that there are good treatment results in class II molar FI invasion sites of the maxillary molars; However, in the classification and maintenance of postoperative molar FI violations, no detailed and long-term follow-up reports have been reported. A study by Becker et al. [20], Pontoriero & Lindhe [21] performing regenerative surgery on the molar affected class III FI invasion of the apical area; It uses an e-PTFE regeneration membrane to try to close the lesion area, but on average it has only a 25% occlusive effect of bone fill. Subsequent lesions may continue to produce progressive destruction. Therefore, although it is feasible to treat molars with growth factor therapy for class II and class III FI lesions, there are still many uncertainties.
Bergenholtz [22] had a long-term evaluation of 45 teeth after root resection (21 survived 2-5 years and 17 survived 5-10 years), and about 3 were removed postoperatively. Hamp et al.[23]; Klavan [24] reported that teeth after root removal could still be used normally and had a high survival rate (about 62-100% at 5 years). And the continuous periodontal destruction leads to the removal of all the extracted teeth only 0-10%, and the reason for its failure is mostly not caused by periodontal disease, but by root fracture, failure of root canal therapy, and cement washout of prosthesis [25,26]. Hou et al. [26] used non-surgical combination RSR and CSCTD (crown and sleeve-coping telescopic denture) for molar with classes II and III FI, follow-up 5 to 13 years (average 6.7±1.9 years) and showed that a remarkable reduction of periodontal pocket and clinical periodontal attachment gain, the plaque index and tooth mobility were also significantly reduced. Periodontal abscess did not recur. In addition, periodontal parameters revealed a very obvious therapeutic effect.
References
- Rampjord SP, Knowles JW, Nissle WW (1975) Results of following three modalities of periodontal therapy. J Periodontol 46(9): 522-526.
- Hirshfeld L, Wasserman B (1978) A long-term survey of tooth loss in 600 treated periodontal patients. J Periodontol 49(5): 225-237.
- McFall WT (1982) Tooth loss in 100 treatment patients with periodontal disease A long-term study. J Periodontol 53(9): 539-549.
- Hou GL, Tsai CC (1987) Relationship between periodontal furcation involvement and cervical enamel projection. J Periodontol 58(10): 715-721.
- Lindhe J, Nyman S (1975) The effect of plaque control and surgical pocket elimination on the establishment and maintenance of periodontal health A longitudinal study of periodontal therapy in case of advanced disease. J Clin Periodontol 2(2): 67-79.
- Rosling B, Nyman S, Lindhe J (1976) The effect of systemic plaque control on bone regeneration in infrabony pockets. J Clin Periodontol 3(1): 38-53.
- Nyman S, Rosling B, Lindhe J (1975) Effect of professional tooth cleaning on healing after periodonral surgery. J Clin Periodontol 2(2): 80-86.
- Muller HP, Eger T, Lange DE (1995) Management of furcation-involved teeth. A retrospective analysis. J Clin Periodontol 22(12): 911-917.
- Hou GL, Chen SF, Tsai CC (1996) Furcation entrance dimension, divergent angle and length of CEJ to furcation entrance related to periodontal therapy. Kaohsiung J Med Sci 12(12): 705-715.
- Hamp SE, Nyman S, Lindhe J (1975) Periodontal treatment of multirooted teeth. Results after 5 years J Clin Periodontol 2(3): 126-135.
- Carnevale G, Febo GD, Tonell MP, et al. (1991) A retrospective analysis of the periodontal-prosthetic treatment of molars with inter-radicular lesions. Int J Perio Restor Dent 11(3): 189-205.
- Caffesse R, Sweeny P, Smith B (1986) Scaling and root planning with and without periodontal surgery. J Clin Periodontol 13(3): 205-210.
- Parashis AO, Anagnou V, Demetrious N (1993) Calculus removal from multirooted teeth with and without surgical access (I) Efficacy on external and furcation surfaces in relation to probing depth. J Clin Periodontol 20(1): 63-68.
- Hou GL, Tsai CC (1989) Clinical observation of the effects of nonsurgical periodontal therapy on human periodontal disease (II) Ultrasonic scaling and root planning for 6 months. Kaohsiung J Med Sci 5(2): 72-86.
- Yalisove IL (1996) Crown and sleeve-coping telescopic retainers for removable partial dentures. 16(6): 1069-1085.
- Yukna RA (1992) Clinical human comparison of expanded polytetrafluoroethylene- ethylene barrier membrane and freeze-dried dura mater allografts for guided tissue regeneration of lost periodontal support(I) Mandibular molar class II furcation. J Periodontol 63(5): 431-442.
- Pontoriero R, Nyman S, Lindhe J (1987) Guided tissue regeneration in the treatment of furcation defects in mandible. J Clin Periodontol 14(10): 618-620.
- Caffesse RG, Smith BA, Duff B (1990) Class II furcations treated by guided tissue regeneration in humans: case reports. J Periodontol 61(8): 510- 514.
- Metzler D, Seamons B, Mellonig J (1991) Clinical evaluation of guided tissue regeneration in the treatment of maxillary Class II molar furcation invasions. J Periodontol 62(6): 353-360.
- Becker W, Becker BE, Berg L (1988) New attachment after treatment with root isolation procedures: report for treated Class III and Class II furcations and vertical osseous defects. Int J of Periodont and Res Dent 8(3): 9-23.
- Pontoriero R, Lindhe J (1995) Guided tissue regeneration in treatment of degree III furcaiton defects in maxillary molars. J Clin Periodontol 22(10): 810-812.
- Bergenholtz A (1972) Radectomu of multirooted teeth. J Amer Dent Assoc 85(4): 870-875.
- Klavan B (1975) Clinical observations following root amputation in maxillary molar teeth. J Periodontal 46(1): 1-5.
- Langer B, Stein SD, Wagenburg B (1981) An evaluation of root resection A ten-year study. J Periodotol 52(12): 719-722.
- Carnevale G, Pontoriero R, Febo G (1998) Long-term effects of root- resective therapy in furcation-involved molars. A 10-year longitudinal study J Clin Periodontol 25(3): 209-214.
- Hou GL, Tsai CC, Weisgold AS (1999) Treatment of molar furcation involvement using root separation and a crown and sleeve-coping telescopic denture A longitudinal study. J Periodontol 70(9): 1098- 1109.






























