Low Window Technique: A Technical Note
Terry Zaniol1*, Tiziano Testori2 and Stephen Wallace3
1Private Practitioner, Crocetta del Montello, Italy
2IRCCS Orthopedic Institute Galeazzi, Dental Clinic, Section of Implant Dentistry and Oral Rehabilitation, Milan, Italy; Department of Biomedical, Surgical and Dental Sciences, Università degli Studi di Milano, Milan, Italy; Adjunct Clinical Associate Professor, Department of Periodontics and Oral Medicine, University of Michigan, School of Dentistry.
2Department of Periodontics, Columbia University College of Dental Medicine, New York, New York, USA.
Submission: January 01, 2022; Published: January 17, 2022
*Corresponding author: Terry Zaniol, Studio Dentistico Zaniol, Crocetta del Montello, Italy
How to cite this article: Zaniol T, Testori T, Wallace S. Low Window Technique: A Technical Note. Adv Dent & Oral Health. 2022; 15(2): 555906. DOI: 10.19080/ADOH.2022.15.555906
Abstract
This article describes a technique for performing lateral antrostomy when performing lateral sinus augmentation using a rational approach. Based on a CBCT scan, a surgical guide is designed and manufactured to allow the surgeon to draw the antrostomy flush with the anterior sinus wall and floor, with its height not exceeding 6 mm. The distal antrostomy line is placed in relation to the position of the most distal fixture. This technique facilitates sinus membrane detachment and reduces flap elevation to approximately 10 mm, and potentially prevents intraoperative and postoperative complications saving the patient from later discomfort. The technique is easily reproducible and because it involves a series of standardized steps, it reduces the likelihood of intraoperative errors.
Keywords:Lateral approach; CAD-CAM surgical technique; Membrane perforation; Guided surgery
Introduction
In lateral sinus augmentation, the design and position of the antrostomy determine the degree of elevation of the mucoperiosteal flap, and the width, height, shape, and distance of the window from the sinus floor may restrict the angles at which sinus membrane elevation instruments must operate in order to separate the membrane from the sinus floor. This may affect the likelihood of membrane perforation, the most common complication of sinus augmentation [1-6]. Currently, the position of the window seems to be chosen by surgeons mainly on the basis of personal habits [7-16]. Some authors suggest placing the inferior antrostomy line flush with the sinus floor, others prefer a position up to 2-3 mm higher, as in Simplified Antrostomy Design (S.A.D.), a planned fenestration technique that starts at the medial sinus wall and extends distally 3 mm above the sinus floor [10-17]. Standardized approaches to window preparation should be preferred because they entail fewer surgical errors, a faster learning curve, and greater reproducibility. To this end, based on rational considerations and observations, the authors have recently proposed a technique for designing the lateral window and performing window antrostomy that takes advantage of the tremendous accuracy that can be achieved with modern CAD-CAM fabrication systems. The purpose of this article is to describe this technique, termed the Low Window Sinus Lift [18,19], taking a rational approach to the steps involved.
Surgical Technique
The Low Window designs
In the Low Window antrostomy design, the window is positioned as low and mesial as possible (Figure 1). The inferior osteotomy line is always placed flush with the sinus floor and the mesial line is always flush with the anterior sinus wall. In addition, the height of the window never exceeds 6 mm to avoid intraosseous anastomosis. The distal osteotomy is positioned to correspond to the most distally planned implant. The reason for creating a low window in as coronal and mesial a position as possible is that the more apical and distal the window, the more difficult the surgical access to the sinus. Additionally, the position of this osteotomy design provides specific surgical advantages. Placement of the lower horizontal osteotomy flush with the sinus floor eliminates any residual bone wall that could hinder detachment of the sinus membrane. The position of the distal osteotomy line is optimized according to the position of the most distal implant; extending it more distally provides no advantage and may result in elevation of a wider mucoperiosteal flap.
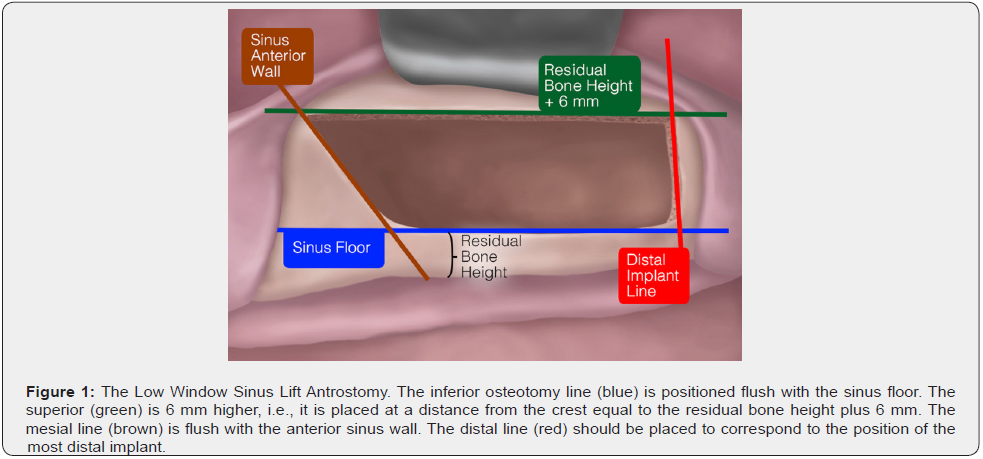
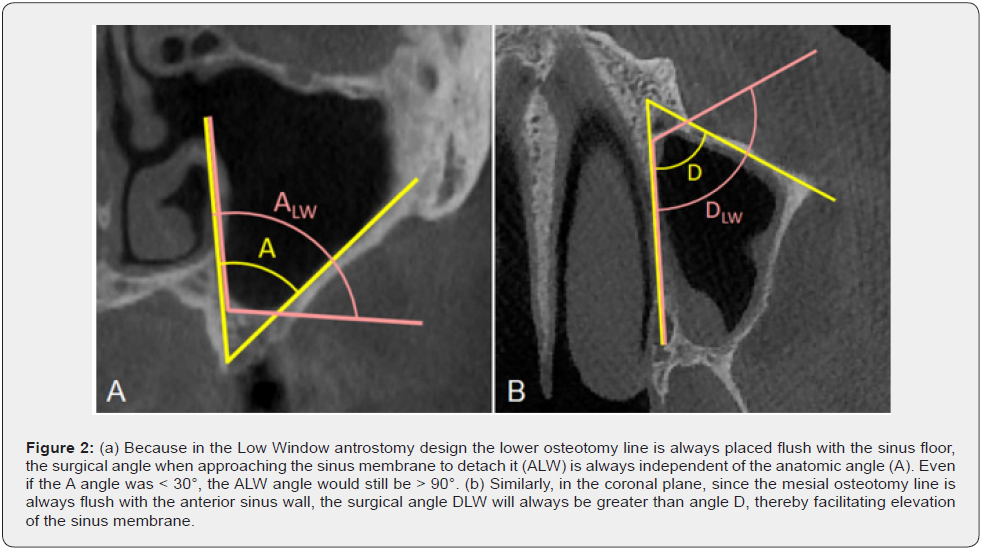
Placing it more distally forces the surgeon to detach a portion of the membrane in a “blind” condition, with no reference points. The position of the mesial osteotomy line, flush with the anterior sinus wall, allows easier access to the anterior sinus recess, i.e. the zone where detaching the sinus membrane is usually most difficult. A window height of 6 mm is the minimum that allows easy access to membrane elevators. A lower height would be an obstacle to membrane elevation, while a greater height would not confer any appreciable advantage but would require the elevation of a wider mucoperiosteal flap [16]. Low Window design may also reduce the risk of sinus membrane perforation when the A and D angles of the patient’s sinus are narrow (i.e., when A < 30°, a condition with increased risk of membrane tearing during detachment [5]). In fact, because the inferior osteotomy line is placed flush with the sinus floor, the modified surgical ALW and DLW approach angles will always be larger than their corresponding anatomic A and D counterparts (Figure 2), reducing the risk of membrane perforation.
Designing and manufacturing the surgical guide
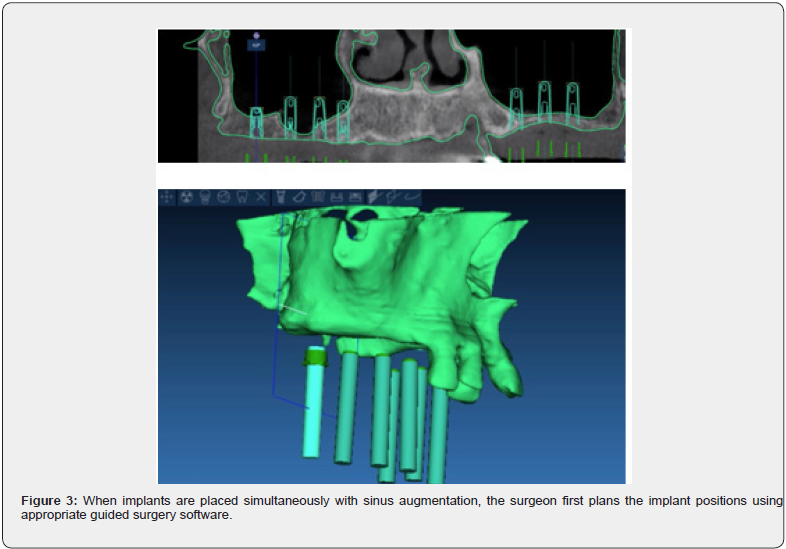
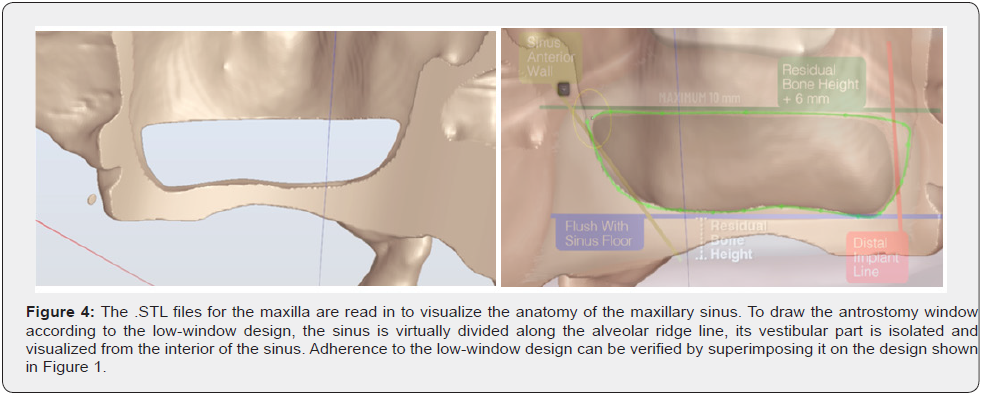
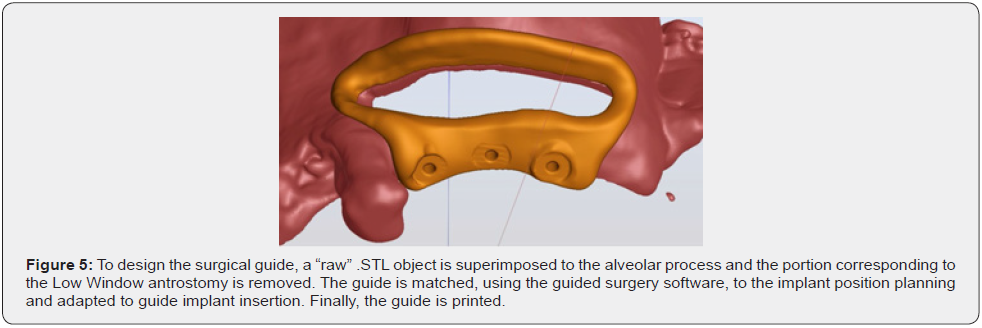
Based on a CT or a CBCT scan, the surgeon first plans the implant positions using guided surgery software (Figure 3) and then reads the .STL file corresponding to the maxilla and maxillary sinuses to visualize their anatomy. Using the same software, the surgeon then draws the window according to the Low Window design (Figure 4). Finally, to design the surgical guide, a “raw”. STL object is superimposed to the alveolar process and its portion corresponding to the Low Window antrostomy removed (Figure 5). The .STL file of the guide is then 3D-printed to manufacture the surgical guide.
Surgical steps
The patient is anesthetized locally according to standard protocols. Given the advanced and low position of the antrostomy, tissue retraction is achieved using a flexible aid (Optragate, Ivoclar Vivadent AG, Schaan, Liechtenstein). Its size is chosen according to the size of the patient’s mouth. This usually eliminates the need for the dental assistant to pull back the patient’s cheeks and lips. The incision lines are drawn using a dermographic pen. The crestal line is medial to the ridge, with no release incisions. It should be moved 1-2 mm more palatal if the buccal attached gingiva is minimal. If a residual distal tooth is present, a paramarginal line is drawn at 3-4 mm at least from the marginal gingiva, starting from its distal papilla. The attached gingiva is incised along the crestal line. A fullthickness incision is performed, going from the distal aspect of the most distal residual tooth to the tuberosity. The incision at the most distal residual tooth is a full-thickness one, up to its mesial aspect, and preserves the papilla. The flap is raised from mesial to distal, not more than 10 mm, leaving intact the attached gingiva at the most distal residual tooth. The antrostomy is first carried out using a tungsten carbide spherical blur, the surgical template acting as a guide; when the sinus membrane begins to appear, one can switch to using a piezoelectric handpiece, with appropriate inserts.
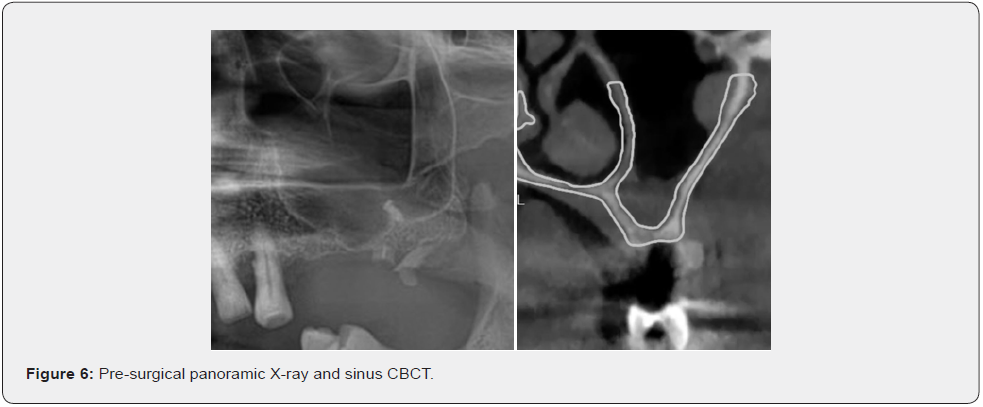
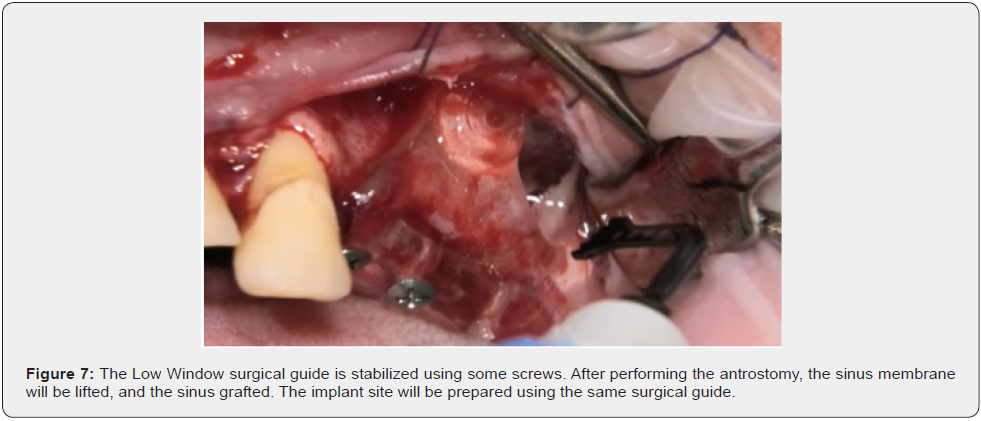
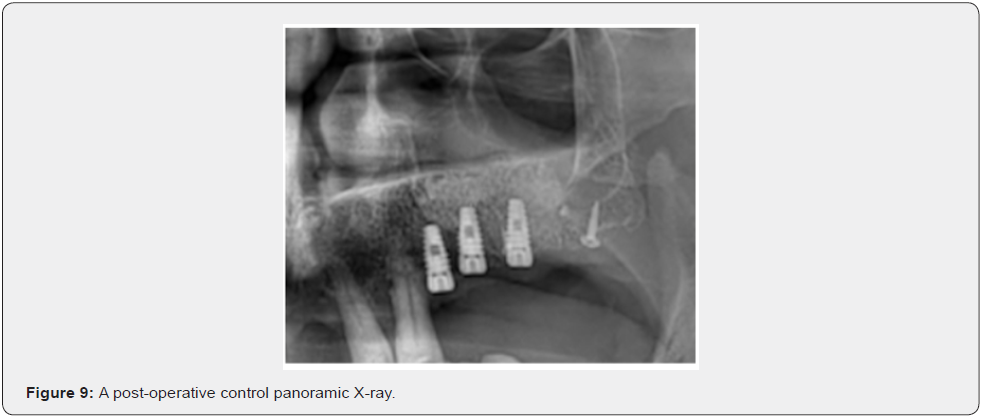
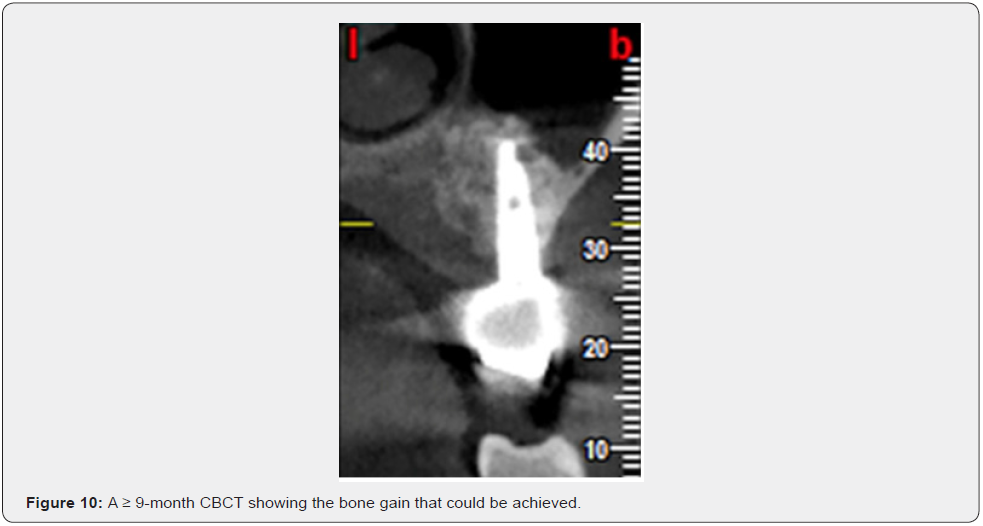
The sinus membrane is detached according to the same procedures used in the traditional approach; the detachment may be carried out using an appropriate piezoelectric insert first, to mobilize the membrane, and then using manual sinus elevators or curettes. As will be explained later, the position of the inferior line flush with the sinus floor and the mesial line flush with the anterior sinus wall facilitate detachment. This is especially true for the anterior sinus recess, a part of the sinus in which the detachment of the membrane is notoriously troublesome and difficult. The sinus is grafted according to standard procedures, using either autogenous bone and/or a bone substitute. The authors usually place a collagen membrane under the sinus membrane to protect it and graft an equine-derived xenograft. They place a collagen or equine-derived cortical bone membrane to protect the antrostomy (the latter being stabilized using taps or screws). External-internal suturing [17] using non-resorbable suture material is followed by suturing of the mucoperiosteal flaps using non-resorbable suture material. A complete clinical case is shown in Figures 6-10. Informed consent was obtained from patients.

Discussion
The Low Window Technique involves a series of standardized surgical steps and is therefore easy to learn, repeatable, and less error-prone than the traditional freehand method. Because it involves the use of digital software to create a surgical template, it helps the surgeon perform osteotomies with precision [18-21]. The Low Window Technique allows easier access to the sinus and reduces invasiveness. Detachment of the sinus membrane is facilitated and because the mesial osteotomy line is flush with the anterior sinus wall and the inferior border is flush with the sinus floor, the movements the surgeon makes with the elevators to detach the membrane are smooth and linear as they first run parallel to the anterior wall and sinus floor and then move upwards. Membrane detachment is facilitated, especially in the area of the anterior recess. This potentially reduces the risk of rupture of the membrane, a known complication of intraoperative sinus augmentation [1-6,22-25]. In the Low Window Technique, incisions are limited to a linear incision. No release incisions are made, and the flap is elevated a maximum of 10 mm. This is expected to result in a better postoperative course characterized by less pain, hematoma, and swelling than the traditional method. In addition, because of the low window height and minimal flap elevation, a flexible lip and cheek retraction device can be used, saving the patient intraoperative and postoperative discomfort. In the authors’ experience, the low-window sinus lift technique does not affect other important sinus augmentation variables, such as the volume of biomaterial required or the length of implants to be placed, and it does not preclude the possibility of simultaneous vertical/horizontal ridge augmentation through guided bone regeneration, if required.
Published evidence on the Low Window Technique is currently limited to an anecdotal case report [18] and a retrospective case series [19] analyzing the records of 28 surgeries involving 22 patients who received 79 implants and were followed-up for 38.4 ± 13.2 months. There were no cases of intraoperative perforation of the sinus membrane or other complications, and patients reported a high level of satisfaction. At final followup, all prostheses and implants were successful. Retrospective data analyses are currently being performed to assess the longterm bone gain achieved by the Low Window Technique, as well as immediate postoperative discomfort, pain, hematoma and bruising. Prospective split-mouth studies are also being planned to compare the Low Window Technique with more traditional, freehand procedures. Overall, the Low Window Technique saves chair time during clinical procedures because it consists of a series of standardized surgical steps that reduce the risk of intraoperative and postoperative complications as well as the patient’s postoperative discomfort. It is easy to learn, repeat, and less error-prone than traditional, freehand methods and reduces the level of difficulty associated with lateral wall techniques [26].
References
- Testori T, Yu SH, Tavelli L, Wang HL (2020) Perforation Risk Assessment in Maxillary Sinus Augmentation with Lateral Wall Technique. Int J Periodontics Restorative Dent 40(3): 373-380.
- Testori T, Wallace S, Monteverdi R, Baj A, Giannì AB (2009) Complications: diagnosis and management In: Testori T, Del Fabbro M, Weinstein R, Wallace S (Editors.), Maxillary Sinus Surgery and Alternatives in Treatment. Quintessence, London pp. 312-323.
- Wallace SS, Mazor Z, Froum SJ, Cho SC, Tarnow DP (2007) Schneiderian membrane perforation rate during sinus elevation using piezosurgery: clinical results of 100 consecutive cases. Int J Periodontics Restorative Dent 27(5): 413-419.
- Fugazzotto P, Melnick PR, Al-Sabbagh M (2015) Complications when augmenting the posterior maxilla. Dent Clin North Am 59(1): 97-130.
- Cho SC, Wallace SS, Froum SJ, Tarnow DP (2001) Influence of anatomy on Schneiderian membrane perforations during sinus elevation surgery: three-dimensional analysis. Pract Proced Aesthet Dent 13(2): 160-163.
- Kang SJ, Shin SI, Herr Y, Kwon YH, Kim GT, et al. (2013) Anatomical structures in the maxillary sinus related to lateral sinus elevation: a cone beam computed tomographic analysis. Clin Oral Implants Res 24(Suppl A100): 75-81.
- Khehra A, Levin L (2020) Maxillary sinus augmentation procedures: a narrative clinical review. Quintessence Int 51(7): 578-584.
- Stern A, Green J (2012) Sinus lift procedures: an overview of current techniques. Dent Clin North Am 56(1): 219-233.
- Guerrero JS, Al-Jandan BA (2013) Lateral wall sinus floor elevation for implant placement: revisiting fundamentals and the surgical technique. J Calif Dent Assoc 41(3): 185-187, 190-195.
- Jensen OT, Shulman LB, Block MS, Iacono VJ (1998) Report of the Sinus Consensus Conference of 1996. Int J Oral Maxillofac Implants 13 Suppl: 11-45.
- Zitzmann NU, Schärer P (1998) Sinus elevation procedures in the resorbed posterior maxilla. Comparison of the crestal and lateral approaches. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 85(1): 8-17.
- Jensen ST, Jensen JD (2017) Maxillary Sinus Floor Augmentation: A Review of Selected Treatment Modalities. J Oral Maxillofac Res 8(3) e3.
- Al-Dajani M (2016) Recent Trends in Sinus Lift Surgery and Their Clinical Implications. Clin Implant Dent Relat Res 18(1): 204-212.
- Lambert F, Lecloux G, Rompen E (2010) One-step approach for implant placement and subantral bone regeneration using bovine hydroxyapatite: a 2- to 6-year follow-up study. Int J Oral Maxillofac Implants 25(3): 598-606.
- Simonpieri A, Choukroun J, Del Corso M, Sammartino G, Dohan Ehrenfest DM (2011) Simultaneous sinus-lift and implantation using microthreaded implants and leukocyte- and platelet-rich fibrin as sole grafting material: a six-year experience. Implant Dent 20(1): 2-12.
- Baldini N, D'Elia C, Bianco A, Goracci C, de Sanctis M, et al. (2017) Lateral approach for sinus floor elevation: large versus small bone window - a split-mouth randomized clinical trial. Clin Oral Implants Res 28(8): 974-981.
- De Stavola L, Tunkel J (2014) The role played by a suspended external-internal suture in reducing marginal flap tension after bone reconstruction: a clinical prospective cohort study in the maxilla. Int J Oral Maxillofac Implants 29(4): 921-926.
- Zaniol T, Zaniol A (2017) A rational approach to sinus augmentation: The low window sinus lift. Case Rep Dent 2017: 7610607.
- Zaniol T, Zaniol A, Tedesco A, Ravazzolo S (2018) The Low Window Sinus Lift: A CAD-CAM-Guided Surgical Technique for Lateral Sinus Augmentation: A Retrospective Case Series. Implant Dent 27(4): 512-520.
- Goodacre BJ, Swamidass RS, Lozada J, Al-Ardah A, Sahl E (2018) A 3D-printed guide for lateral approach sinus grafting: A dental technique. J Prosthet Dent 119(6): 897-901.
- Osman AH, Mansour H, Atef M, Hakam M (2018) Computer guided sinus floor elevation through lateral window approach with simultaneous implant placement. Clin Implant Dent Relat Res 20(2): 137-143.
- Testori T, Weinstein T, Taschieri S, Wallace SS (2019) Risk factors in lateral window sinus elevation surgery. Periodontol 2000 81(1): 91-123.
- Misch CE (1999) The maxillary sinus graft and sinus graft surgery in: Misch CE (Editor.) Contemporary Implant Dentistry. Mosby, Chicago pp. 469-495.
- Danesh-Sani SA, Loomer PM, Wallace SS (2016) A comprehensive clinical review of maxillary sinus floor elevation: anatomy, techniques, biomaterials and complications. Br J Oral Maxillofac Surg 54(7): 724-730.
- Stacchi C, Andolsek F, Berton F, Perinetti G, Navarra CO, et al. (2017) Intraoperative Complications During Sinus Floor Elevation with Lateral Approach: A Systematic Review. Int J Oral Maxillofac Implants 32(3): e107-e118.
- Testori T, Tavelli L, Yu SH, Scaini R, Darnahal A, et al. (2020) Maxillary Sinus Elevation Difficulty Score with Lateral Wall Technique. Int J Oral Maxillofac Implants 35(3): 631-638.






























