Relationship between Oral Function and Respiratory Disturbance Index in Obstructive Sleep Apnea Syndrome Patients
Hiroyuki Nakano1*, Sho Mizobuchi1, Yasuhisa Sawai1, Eri Komori1, Kei Suzuki1, Mayumi Matsumura1, Yasuyuki Sasai1, Toshiyuki Konda1, Soichiro Ikeda2, Yoichiro Nakajima1, Tomohiro Yamada3 and Takaaki Ueno1
1Department of Oral Surgery, Osaka Medical College, Japan
2Division of Internal Medicine (I), Faculty of Medicine, Osaka Medical College, Japan
3 Section of Oral and Maxillofacial Surgery, Division of Maxillofacial Diagnostic and Surgical Sciences, Faculty of Dental Science, Kyushu University, Japan
Submission: April 08, 2021; Published: May 17, 2021
*Corresponding author: Hiroyuki Nakano, Department of Oral Surgery, Osaka Medical College, 2-7 Daigaku-machi, Takatsuki City, Japan
How to cite this article: Hiroyuki N, Sho M, Yasuhisa S, Eri K, Kei S, et al. Relationship between Oral Function and Respiratory Disturbance Index in Obstructive Sleep Apnea Syndrome Patients. Adv Dent & Oral Health. 2021; 14(2): 555883. DOI: 10.19080/ADOH.2021.14.555883
Abstract
To investigate the relationship between oral function and respiratory disturbance index (RDI). This has not been reported previously. Sixtyone patients (41 males, 20 females) who were treated for obstructive sleep apnea with an oral appliance were enrolled in this study. Mean age and body mass index were 55.5±12.7 years and 24.4±4.0kg/m2, respectively. Patients were classified into groups based on body mass index (non-obese group, < 25.0kg/m2 and obese group, ≧ 25.0kg/m2) and severity of RDI (mild group, 5 ≤ RDI < 15 and moderate and severe group, RDI ≥15). RDI was measured by in-home (portable) monitoring and oral function was measured as maximum occlusal force, tongue pressure and labial closure force. A significant negative correlation was found between labial closure force and RDI in the total cohort and in non-obese cases (P<0.05). This study suggests that labial closure force may affect sleep-disordered breathing, supporting past reports. Evaluation of labial closure force thus appears very important before treating OSA.
Keywords: Respiratory disturbance index; In-home (portable) monitoring; Maximum occlusal force; Tongue pressure; Labial closure force
Abbreviations: SBD: Sleep-Disordered Breathing; OSA: Obstructive Sleep Apnea; CSA: Central Sleep Apnea; CSR: Cheyne-Stokes Respiration; RDI: Respiratory Disturbance Index
Introduction
The oral cavity, along with the nasal cavity, is one of the entrances for breathing. Many anatomical features of the oral cavity can contribute to sleep-disordered breathing (SDB). Within SDB, several subtypes of sleep disturbance have been identified, including obstructive sleep apnea (OSA), central sleep apnea (CSA) and Cheyne-Stokes respiration (CSR). OSA occurs when obstruction of the upper airway causes cessation of airflow during continued inspiratory effort and is more prevalent among heart failure patients than among the general population [1]. Research comparing the pharyngeal and maxillofacial morphology between patients with and without OSA has identified mandibular retraction, small mandible, low hyoid bone, long face, short cranial base, and long soft palate and pharynx [2,3]. However, evaluating the functions of the jaw, tongue and soft palate has been difficult. In recent years, advances in devices has enabled evaluation of oral functions such as maximum occlusal force, tongue pressure, and lip closure force. However, no reports appear to have investigated the relationship between oral function and respiratory disturbance index (RDI). This study therefore examined the relationship between oral function and RDI.
Materials and Methods
Patients
Sixty-one patients (41 men, 20 women) who were treated with an oral appliance at Osaka Medical College Hospital from August 2018 to August 2020 were enrolled in this study. Mean age was 55.5±12.7 years and mean body mass index was 24.4±4.0kg/ m2. Patients were classified into two group based on the severity of RDI, the body mass index: non- obesity group (<25.0kg/m2) and obesity group (≧25.0kg/m2), mild cases (5 ≤ RDI < 15) and moderate and severe cases (RDI ≥ 15).
RDI
RDI was measured by in-home (portable) monitoring (SAS- 2100; Teijin Medical Pharma, Tokyo, Japan) of respiration and oxygenation. RDI was defined as the total sum of apnea and hypopnea episodes divided by total sleep time.
Oral functions
Maximum occlusal force was measured once for each side using a simple occlusal force-measuring device (Occlusal Force Meter GM10; Nagano Keiki Co., Tokyo, Japan) to find maximum values for each subject. Tongue pressure was measured using a tongue pressure-measuring device (JMS tongue pressure measurement device; Morita Corporation, Tokyo, Japan). Labial closure force was measured using a labial closure device (LDC- 110R Lip De Cum lip force measurement device, Ducklings; Cosmo Instruments Co., Tokyo, Japan).
Statistical analysis
We conducted statistical analyses with Spearman’s rankorder correlation coefficient to evaluate the associations between indicators of RDI and oral function. Correlation coefficients for maximum occlusal force, tongue pressure, labial closure device and RDI were calculated. The level of significance was set as p<0.05.
Ethical considerations
This study was approved by the ethics committee at Osaka Medical College (approval number 2695) and conformed with the accepted ethical standards formulated in the Declaration of Helsinki 1964 (as revised in 2000). All participants provided informed consent for measurement of oral functions and RDI.
Results
RDI
Mean RDI for the total cohort was 20.6±10.5 times/h. Among the 18 mild cases (29.5%), mean RDI was 9.8±3.5 times/h. Among the 43 moderate and severe cases (70.5%), mean RDI was 25.2±9.0 times/h. Among the 36 non-obese cases (59.0%), mean RDI was 20.4±10.3 times/h. Among the 25 obese cases (41.0%), mean RDI was 20.9±10.7 times/h.
Oral functions
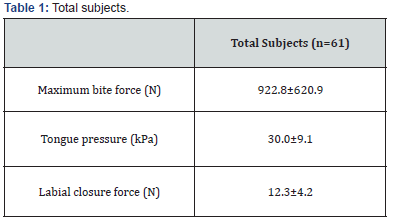
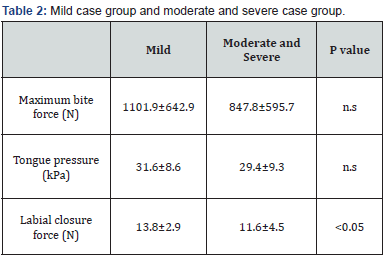
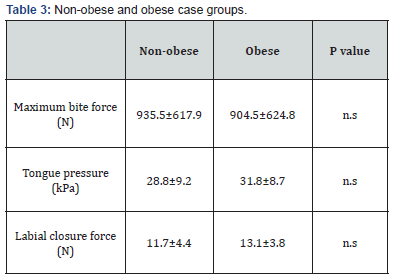
Mean maximum bite force was 922.8±620.9N for the total cohort, 1101.9±642.9N in mild cases and 847.8±595.7N in moderate and severe cases. Mean maximum bite force was 935.5±617.9N in non-obese cases and 904.5±624.8N in obese cases. Mean tongue pressure was 30.0±9.1kPa for the total cohort, 31.6±8.6kPa in mild cases, and 29.4±9.3kPa in moderate and severe cases. Mean tongue pressure was 28.8±9.2kPa in nonobese cases and 31.8±8.7kPa in obese cases. Mean labial closure force was 12.3±4.2N in the total cohort, 13.8±2.9N in mild cases and 11.6±4.5N in moderate and severe cases. Mean labial closure force was 11.7±4.4N in non-obese cases and 13.1±3.8N in obese cases (Table 1-3).
Correlations
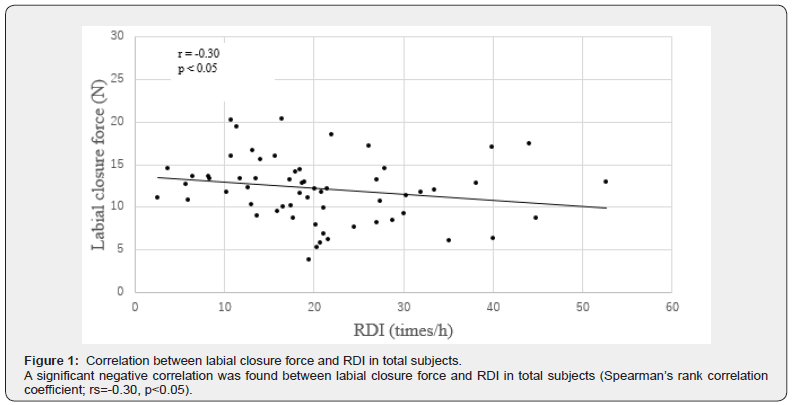
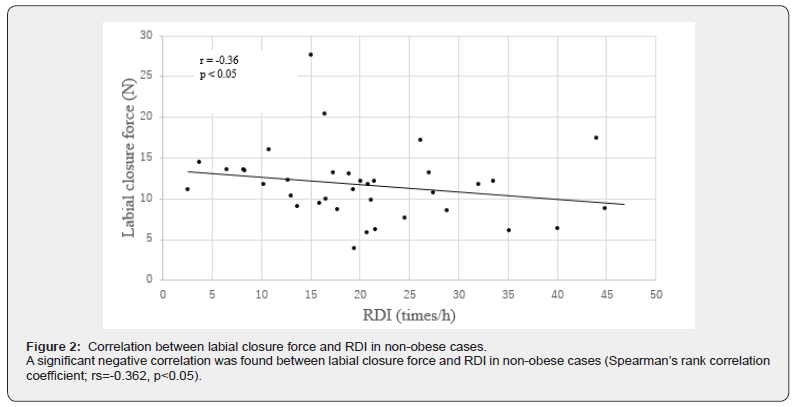
A significant negative correlation was found between labial closure force and RDI in the total cohort. (Spearman’s rank correlation coefficient: rs=-0.30: p<0.05) (Figure 1). No correlations were found with other factors, with the exception of a correlation between labial closure force and RDI in the total cohort. A significant negative correlation was found between labial closure force and RDI in non-obese cases (Spearman’s rank correlation coefficient: rs=-0.362: p<0.05) (Figure 2).
Discussion
The prevalence of sleep apnea syndrome (SAS) in the global middle-aged work force is reportedly 4% of men and 2% of women [4]. Of these, OSA is the most common cause of secondary hypertension [5] and arteriosclerosis, which exacerbates the pathologies of diabetes and dyslipidemia. The causes of OSA can be divided into functional and morphological factors [6,7]. As functional factors, hypotonia of the muscles of upper airway dilatation weakens as the upper airway relaxes with the onset of sleep, and the upper airway becomes more susceptible to pressure fluctuations, resulting in narrowing of the airway. In particular, the soft palate and tongue base sink posteriorly, narrowing the pharyngeal cavity in the supine position. In the absence of structural or functional abnormalities in the upper airway, this degree of physiological upper airway stenosis maintains the necessary ventilation during sleep with resting breathing power, resulting in sleep or occasional mild snoring.
However, when a morphologically narrowed upper respiratory tract is added to this, resting breathing during sleep interferes with the required amount of ventilation, resulting in OSA consisting of persistent snoring and hyperventilation with apnea and snoring. So far, many reports have examined the morphological characteristics of OSA patients [2,3], but few reports have examined functional factors. In recent years, the advancement of devices has allowed evaluation of oral functions such as maximum occlusal force, tongue pressure, and lip closure force. As a result, many reports have been made on the effects of oral function on the whole body [8-10]. The tongue can be easily considered to have a significant impact on OSA. We suspected that a correlation exists between tongue pressure and Apnea Hyponea Index. However, only the non-obese group showed a correlation between labial closure force and AHI in this study
We think that the factors that affect AHI in terms of lip closure force are that mouth opening shortens the space between the mandible and the hyoid bone, and that the hyoid bone retracts, causing the tongue to rise and fall into the pharyngeal cavity. When narrowing occurs to the extent that the nasopharyngeal cavity downstream of the airway is affected by turbulence, airway resistance is increased [11]. When nasal cavity resistance is further increased, Bernoulli’s principle causes the nasal cavity to become a resistance tube, and a strong negative pressure is generated in the pharynx below the nasal cavity, pulling in the soft palate, as the softest tissue in the region. Airway narrowing can thus result [12]. Takamoto et al. [13] reported on training methods and devices to increase labial closure force. Moreover, they reported that labial closure force training ameliorated eating dysfunction, decreased daytime sleepiness, and activated the prefrontal cortex in elderly individuals. That report supports our results. In patients with OSA, measuring labial closure force before treatment may be important when choosing a treatment method.
Conclusion
This study suggests that labial closure force may affect SDB, supporting previous findings. Evaluating labial closure force appears very important before treating OSA.
References
- Oldenburg O, Lamp B, Faber L, Teschler H, Horstkotte D, et al. (2007) Sleep-disordered breathing in patients with symptomatic heart failure: a contemporary study of prevalence in and characteristics of 700 patients. Eur J Heart Fail 9(3): 251-257.
- Kikuchi M, Higurashi N, Miyazaki S, Itasaka Y (2000) Facial patterns of obstructive sleep apnea patients using Ricketts method. Psychiatry Clin Neurosci 54(3): 336-337.
- Lowe AA, Ozbek MM, Miyamoto K, Pae EK, Fleetham JA (1997) Cephalometric and demographic characteristics of obstructive sleep apnea: an evaluation with partial least square analysis. Angle Orthod 67(2): 143-154.
- Young T, Palta M, Dempsey J, Skatrud J, Weber S, et al. (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328(17): 1230-1235.
- Nieto FJ, Young TB, Lind BK, Shahar E, Samet JM, et al. (2000) Association of sleep disordered breathing, sleep apnea, and hypertension in a large community-based study. Sleep Heart Health Study. JAMA 283(14): 1829-1836.
- Punjabi NM, Ahmed MM, Polotsky VY, Beamer BA, O Donnell CP (2000) Sleep-disordered breathing, glucose intolerance, and insulin resistance. Am J Epidemiol 160(6): 521-130.
- Robinson GV, Pepperell JC, Segal HC, Davies RJO, Stradling JR (2004) Circulating cardiovascular risk factor in obstructive sleep apnea: data from randomized controlled trials. Thorax 59(9): 777-782.
- Suzuki K, Kato Kogoe N, Inoue K, Omori M, Imagawa N, et al. (2020) The relationship between jaw function and cognitive function in the elderly population. Journal of Hard Tissue Biology 29(3): 169-172.
- Imagawa N, Kato Kogoe N, Suzuki K, Omori M, Suwa Y, et al. (2020) Relationship between oral function and occlusal bite force in the elderly. Journal of Hard Tissue Biology 29(3): 165-168.
- Suzuki K, Nakano H, Kato Kogoe N, Inoue K, Omori M, et al. (2020) A preliminary study of the relationship between oral and vascular function in the elderly population. Journal of Hard Tissue Biology 29(3): 161-164.
- Lee SH, Choi JH, Shin C, Lee HM, Kwon SY, et al. (2007) How does open-mouth breathing influence upper airway? Laryngoscope 117(6): 1102-1106.
- Nishimura T, Suzuki K (2003) Anatomy of oral respiration: morphology of the oral cavity and pharynx. Acta Otolaryngol Suppl 550: 25-28.
- Takamoto K, Saitoh T, Taguchi T, Nishimaru H, Urakawa S, et al. (2018) Lip closure training improves eating behaviors and prefrontal cortical hemodynamic activity and decreases daytime sleep in elderly persons. J Bodyw Mov Ther 22(3): 810-816.






























