Dental Whitening at-home, in-office and Combined Techniques: Case Report and Literature Review
Danyelle Martins, Carolina Rangel, Giovana Fontanetti, Jorge Soto, Josué Junior Araujo Pierote* and Luis Alexandre Maffei Sartini Paulillo
Department of Restorative Dentistry, Piracicaba Dental School, State University of Campinas, Brazil
Submission: November 14, 2019 Published: November 20, 2019
*Corresponding author: Josué Junior Araujo Pierote, Department of Restorative Dentistry, Piracicaba Dental School, State University of Campinas, Brazil
How to cite this article: Danyelle Martins, Carolina Rangel, Giovana Fontanetti, Jorge Soto, Josué Junior Araujo Pierote, Luis Alexandre Maffei Sartini Paulillo. Dental Whitening at-home, in-office and Combined Techniques: Case Report and Literature Review. Adv Dent & Oral Health. 2019; 11(5): 555822. DOI:10.19080/ADOH.2019.11.555822
Abstract
Introduction: Smile esthetics and the quest for whiter teeth has become a main concern among patients. As a response, dental whitening techniques and materials have been developed, allowing dentist to offer a safe treatment that responds to patient´s demands. However, there is no standard consensus regarding the indicated protocol for each patient. The purpose of this article is to present the case of a patient treated with a combination of in-office and at-home whitening techniques and to clinically evaluate the color change in the patient´s teeth.
Materials and Methods: The bleaching protocol was set to include 2 sessions of in-office whitening (40% hydrogen peroxide), with prior application of a desensitizing agent (5% potassium nitrate) and a 7-day rest period between appointments, followed by 21 days of at-home whitening (10% carbamide peroxide).
Results: The applied protocol, resulted in a color change from an initial Vita A3 shade to a final A1 shade after the bleaching protocol, with no discomfort reported from the patient.
Conclusion: The combination of in-office and at-home whitening techniques, may produce quick, satisfactory and predictable results, especially when they are used with a desensitizing agent, that reduces patient discomfort, while maintaining the effectiveness of the bleaching results.
Keywords: Carbamide Peroxide; Esthetic Dentistry; Hydrogen Peroxide; Tooth Whitening
Abbreviations: OTC: Over the Counter; TS: Tooth Sensitivity; HP: Hydrogen Peroxide; CP: Carbamide Peroxide
Introduction
Improvements in dental materials have resulted in the development of tooth whitening products, that allow dental practitioners to offer dental bleaching as a safe restorative and esthetic procedure [1]. Concerns by patients over the appearance and color of their teeth appears to be a common and important topic, and in general, dissatisfaction with tooth color has been associated with an increased desire for esthetic dental procedures, including tooth whitening [2-4]. There is a wide variety of over the counter (OTC) products that claim to have a whitening effect, including toothpastes, strips, gels and whitening rinses [4], although the safety of this products has been questioned [1]. Therefore, best results are achieved when dental bleaching procedures are performed by a dentist [1,5]. Currently, dentists may offer two main types of dental bleaching techniques: at-home or in-office [3,6,7]. Traditionally, at-home bleaching has been indicated for whitening of vital teeth, although some patients reject the daily use of a plastic bleaching tray for several days or even weeks; therefore, the in-office bleaching has been increasingly indicated under the promise to offer immediate results, and a much-reduced number of applications [3,7].
However, with any of the applied techniques, tooth sensitivity (TS) remains as one of the main reported side effects of dental bleaching [1,3,4,6-9]. The mechanism of TS caused by tooth whitening, may occur in healthy teeth with no other provoking stimulus, which differs from the mechanisms of other forms of TS, usually associated with stimulus (cold or tactile) that contact the surface of exposed dentin. It has been hypothesized that bleaching associated TS occurs because of the peroxide penetrating the dental structure, which directly activates a neuronal receptor, and not because of hydrodynamic effects, that commonly explain other forms of TS [6]. In addition, morphological alteration of the enamel surface [4,5,8,10], caused by bleaching agents could leave the dentin less protected, and more susceptible to sensitivity inducing stimuli [6]. To address the issue of TS, new dental whitening products have attempted to modify its formulations. Such modifications include decreasing the concentration of peroxide products, administration of analgesics, and the application of desensitizing agents, which seem to be effective options to reduce tooth sensitivity, commonly associated with dental whitening procedures [6]. The aim of the present paper is to clinically evaluate the color change in a patient´s teeth, through the application of a combined bleaching technique
Literature Review
The active ingredient in most whitening products is hydrogen peroxide (HP) [1], that is a molecule with low molecular weight, that allows it to penetrate into dentin and act as a strong oxidizing agent, releasing oxygen [5]. HP is delivered into de patients mouth in two main forms: as HP ranging in concentrations from 5 to 35%, most frequently used for in-office whitening or as carbamide peroxide (CP) in concentrations ranging from 10 to 35% [4,5], that correspond to approximately 3.5 parts of HP and 6.5 parts of urea, frequently found in at-home products. Concentration of HP on at-home whitening products ranges from 3% to 7.5% and in-office formulations contain 25% to 38% HP [1]. A recent, Metaanalysis evaluating the effectiveness of At-home and In-office bleaching techniques, failed to identify any differences between both techniques, regarding effectiveness and risk or intensity of TS [11], and concluded that studies comparing both techniques reported similar satisfaction among patients in terms of comfort and whitening results [11]. Tooth discoloration is produced by the presence of organic compounds, that accumulate on the dentinal surface, and contain conjugated double bonds [5], or metal containing compounds, which are known as chromogens [4]. It is widely considered that regardless of the present concentration of HP, it penetrates through the enamel, to reach the dentin, were it releases reactive oxygen molecules that oxidize the colorconferring compounds by breaking the present double-bonds, transforming the chromogens, into more polar, lower molecular weight, color-less compounds [4,5,9,10].
Since TS is commonly associated with dental bleaching procedures, some authors recommend applying a desensitizing agent prior to the exposition to the whitening product [6,9]. Based on the theory that whitening associated TS is produced by a direct excitation of the terminal nerve [6,12], the use of potassium salts that reduce the excitability of the intradental nerves have become the main choice for reducing TS [12]. The most commonly used desensitizing agents are potassium nitrate (KNO3) and sodium fluoride (NaF) [3,12] and are widely indicated to treat tooth sensitivity associated with dental whitening. These agents may be included in the bleaching gel formulation or applied independently into the patients mouth for a short time before bleaching is introduced [3,9]. Has been reported, that TS is significantly higher in patients undergoing in-office whitening, when desensitizing agents are not applied [3,6,9] and that application of a desensitizing agent does not reduce the efficacy of the bleaching products [9,12].
Case Report
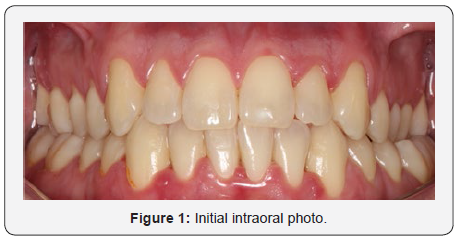
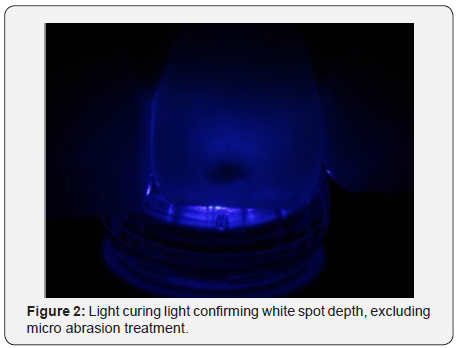
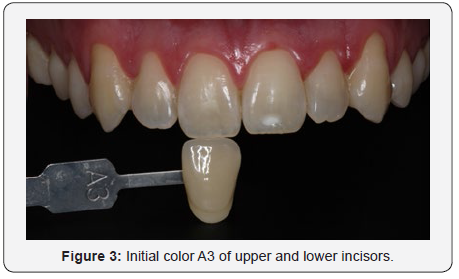
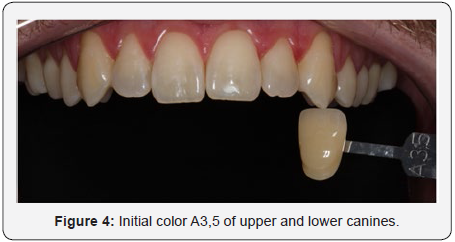
Young, non-smoking male patient was dissatisfied with his smile, mainly because of the dark staining of his teeth. A detailed clinical examination was performed, where an anamnesis form was completed to obtain data on the patient’s general health. At the first visit, an intra-oral examination identified gingival retractions in the upper and lower premolars (Figure 1). A white spot in the region of the incisal third of tooth 21 was detected and the light curing test was performed so that the depth of the lesion could be seen. As the stain was darkened by blue light, it was decided not to microabrase since it was not just a superficial stain (Figure 2). In addition, generalized and mild gingivitis was observed, causing the patient to receive oral hygiene guidelines, and the use of an extra soft toothbrush was recommended. No caries lesion was detected. With this information, the protocol chosen for the case was office whitening with the desensitizing technique. In the first whitening session, the patient was submitted to some initial photographs (T5i, Canon, USA) to record the efficiency and the result of the whitening treatment, where the initial color of the VITA scale teeth was verified, being A3 in the incisors upper and lower (Figure 3), and A3,5 in the upper and lower canines (Figure 4).
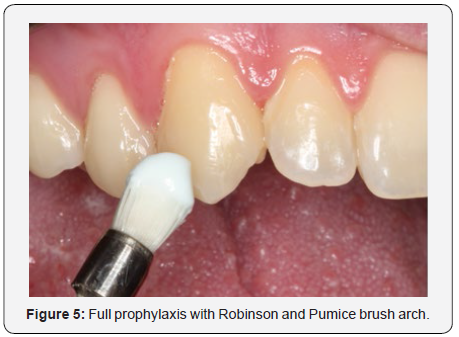
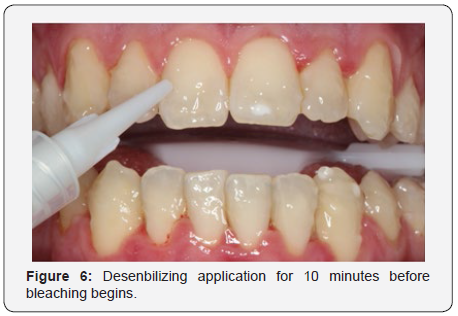
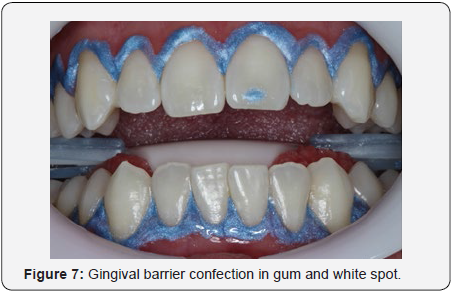
Next, Robinson Branca brush prophylaxis (MK Life, Porto Alegre, Rio Grande do Sul, Brazil) and Extra Fine Pumice Stone (SS White, São Cristóvão, Rio de Janeiro, Brazil) were performed to remove plaque (Figure 5). To remove the lips and tongue, an Arcflex retractor (FGM, Joiville, Santa Catarina, Brazil) was used, followed by a 10-minute application of Desensitize 2% desensitizing gel (FGM, Joinville, Santa Catarina, Brazil) in all the teeth that would receive the whitening treatment (Figure 6). After the elapsed time, the upper and lower arch were washed. Immediately after the teeth and gum were blown dry, the Top Dam light-curing gingival barrier (FGM, Joinville, Santa Catarina, Brazil) was applied so that the whitening gel did not come into contact with mucous membranes and soft tissues. The barrier was also applied over the white spot to protect it from the gel, and it was hoped that the gel would only reach the tooth enamel and the spot would stay the same color, giving a final result where the spot was less evident (Figure 7).
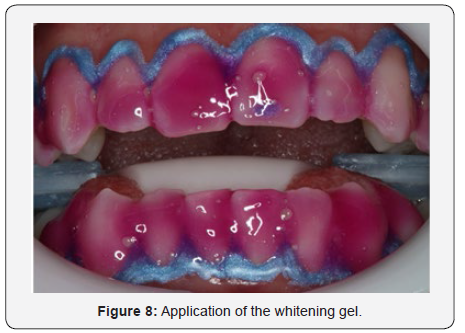
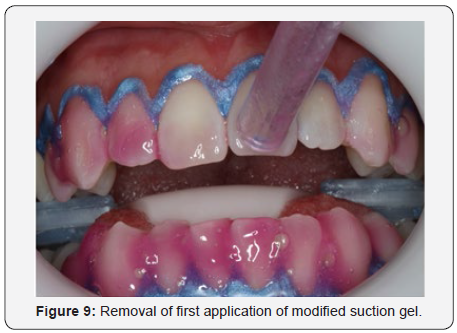
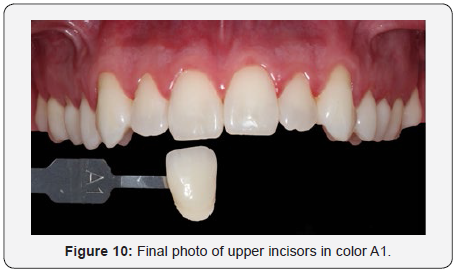
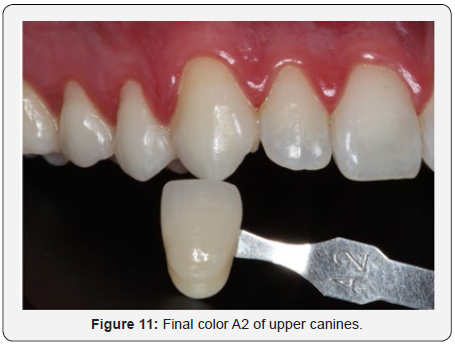
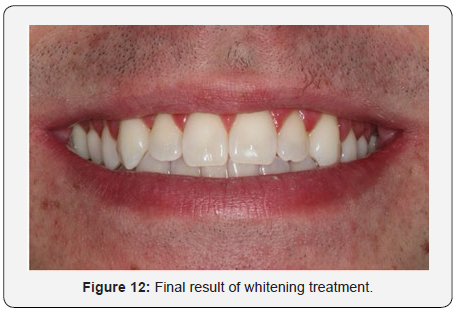
The gel chosen for the treatment was HP Whiteness 35% (FGM, Joiville, Santa Catarina, Brazil), where the manufacturer’s recommendations were followed, making the ratio of 3 drops of peroxide to 1 drop of thickener. As was done in the mouth, 4 proportions were made so that the amount of gel was sufficient in each application (Figure 8). If necessary, neutralize would be used to counteract any burn injury caused by oxygen peroxide in the gum or mucosa. A 15-minute application of the gel was made, then a modified sucker was used to suck up the excess gel and wash with water from the triple syringe (Figure 9). After this process, the procedure was repeated in that same session. The whitening treatment totaled 3 sessions, in each of them 2 applications of the gel were made. After the office whitening treatment was completed, it took 7 days for the final color to be taken due to the subtle color change after remineralization of the enamel. The upper and lower incisors were color A3 to A1 of the VITA scale (Figure 10). The upper and lower canines were color A3,5 for color A2 of VITA scale (Figure 11). The initial and final color change was very satisfactory, and the result was excellent (Figure 12). The white spot did not receive any kind of restorative treatment because the patient did not bother with its presence. After bleaching, the white spot was less evident on the incisal third.
Discussion
There is no consensual protocol regarding the indicated protocol to use either at-home or in-office dental whitening, or a potential combination of both, regarding the number of applications, product concentration, and therefore, the most appropriate bleaching protocol, must be determined individually based on the patient´s oral health, lifestyle and financial status [13]. Quicker teeth whitening can be achieved through in-office bleaching, because the products formulations, deliver higher concentrations of HP than at-home or OTC products. Consequently, gingival tissues are more prone to irritation in case of contact [1,8], and need to be protected before the whitening agent is applied by a barrier made of a light polymerized resin dam, like Top Dam, Opal Dam or similar [4], and in case there is contact of the whitening agent with the gingival tissues, it is required to apply a neutralizing agent. Considering also that the intensity of TS sensitivity after in-office bleaching is usually moderate, even though in some and in some cases may be so severe that causes patients to abandon the procedure, the application protocol of the in-office bleaching may vary, according to the patient´s needs and tolerance, and is deeply for the dentist to the manufacturer indications [11].
On the other side, at-home tooth bleaching, using carbamide peroxide containing materials has become very popular, and remains a common choice among patients, due to the low concentration of released hydrogen peroxide, which clinically translates in fewer and milder cases of dental sensitivity from the treatment [14]. In the presented case, patient´s conditions and tolerance to side effects, and due to no reported discomfort, a second application of in-office whitening agent, was made after a 7-days resting time, based on reports of reluctance about applying in-office bleaching agents during consecutive days [15]. Yet, it is important to remark, that even tough in both sessions a desensitizing agent was applied before the bleaching product, the patient reported discomfort after the second session of inoffice whitening, and therefore it was decided to apply 3 week of at-home dental whitening as a complementary treatment, looking to achieve the patient´s desired results. Considering the attained clinical success of the protocol, it was observed that both techniques have particularities, and when combined, they may offer satisfying results [16], with little to minimal discomfort for the patient [17].
Conclusion
Dentist supervised tooth whitening is a simple, safe and conservative procedure that may allow to fulfill patient´s esthetic requirements at a relatively low cost and short time. However, there is no consensus about the best protocol to be applied, therefore, a proper and profound diagnosis is necessary to determine the best protocol to be applied, reducing the risk or intensity of associated side effects. The combination of in-office and at-home whitening techniques and products allows the dentist to offer their patients quick, satisfactory and predictable results, especially when they are associated with the use of a desensitizing agent, that reduces patient discomfort, while maintaining the effectiveness of the bleaching results.
References
- Li Y (2011) Safety controversies in tooth bleaching. Dent Clin North Am 55(2): 255-263.
- Joiner A, Hopkinson I, Deng Y, Westland S (2008) A review of tooth colour and whiteness. J Dent 36(1): 2-7.
- Wang Y, Gao J, Jiang T, Liang S, Zhou Y, et al. (2015) Evaluation of the efficacy of potassium nitrate and sodium fluoride as desensitizing agents during tooth bleaching treatment - A systematic review and meta-analysis. J Dent 43(8): 913-923.
- Carey CM (2014) Tooth whitening: What we now know. J Evid Based Dent Pract 14: 70-76.
- Kwon SR, Wertz PW (2015) Review of the mechanism of tooth whitening. J Esthet Restor Dent 27(5): 240-257.
- Pintado-Palomino K, Filho OP, Zanotto ED, Tirapelli C (2015) A clinical, randomized, controlled study on the use of desensitizing agents during tooth bleaching. J Dent 43(9): 1099-1105.
- Bruzell EM, Pallesen U, Rygh Thoresen N, Wallman C, Dahl JE (2013) Side effects of external tooth bleaching: A multi-centre practice-based prospective study. Br Dent J 215(9): 466-467.
- Dahl J, Pallesen U (2003) Tooth Bleaching: A Critical Review of the Biological Aspects. New York 14(4): 292-304.
- Do Carmo Publio J, D’Arce MBF, Ambrosano GMB, Aguiar FHB, Lovadino JR, et al. (2015) Efficacy of tooth bleaching with the prior application of a desensitizing agent. J Investig Clin Dent 6(2): 133-140.
- Zanolla J, Marques ABC, Da Costa DC, De Souza AS, Coutinho M (2017) Influence of tooth bleaching on dental enamel microhardness: a systematic review and meta-analysis. Aust Dent J 62(3): 276-282.
- De Geus J, Wambier L, Kossatz S, Loguercio A, Reis A (2016) At-home vs In-office Bleaching: A Systematic Review and Meta-analysis. Oper Dent 41(4): 341-356.
- Markowitz K (2010) Painful: Why does tooth bleaching hurt? Med Hypotheses 74(5): 835-840.
- (2009) American Dental Association (ADA). Tooth whitening/bleaching: treatment considerations for dentists and their patients. Chicago: ADA Council on Scientific Affairs.
- Matis B, Hamdan YS, Cochran M, Eckert GJ (2002) A clinical evaluation of a bleaching agent used with and without reservoirs. Oper Dent 27(1): 5-11.
- Deliperi S, Bardwell DN, Papathanasiou A (2004) Clinical evaluation of a combined in-office and take-home bleaching system. J Am Dent Assoc 135(5): 628-234.
- Auschill TM, Hellwig E, Schmidale S, Sculean A, Arweiler NB (2005) Efficacy, side-effects and patients’ acceptance of different bleaching techniques (OTC, in-office, at-home). Oper Dent 30(2): 156-163.
- Mokhlis GR, Matis BA, Cochran MA, Eckert GJ (2000) Clinical Evaluation of Carbamide Peroxide and Hydrogen Peroxide Whitening Agents During Daytime Use. J Am Dent Assoc [Internet] 131(9): 1269-1277.






























