Orthognathic Surgical Treatment of Patient with High Angle Growth Pattern and Skeletal Open Bite Malocclusion: A Case Report
Muhammed Hilmi Buyukcavus*
Akdeniz University, Turkey
Submission: February 12, 2017; Published: December 13, 2017
*Corresponding author: Muhammed Hilmi Buyukcavus, Faculty of Dentistry, Akdeniz University, Turkey, Email: mhbuyukcvs@gmail.com
How to cite this article: Orthognathyc Surgycal Treatment of Patyent wyth Hygh Angle Growth Pattern and Skeletal Open Byte Malocclusyon: A Case Report. Adv Dent & Oral Health: 2017; 7(1): 555703. DOI: 10.19080/ADOH.2017.07.555703
Abstract
Aim: The aim of this case report is to present the orthodontic and surgical treatment of an adult patient with high angle growth pattern and skeletal open bite malocclusion.
Case: A 25 years old male patient with chief complaints of prognathic mandibula and ineffective chewing of food. In clinical examination, -2,4mm overjet, -6,2mm overbite, Class III molar and canine relationship and concave profile was observed. With cephalometric measurements, it has been that evaluation of the patient's sagittal direction as SNA: 81.3° SNB: 79.3° ANB: 2°, the evaluation of vertical direction SN-Go-Me: 45.9°, FMA: 38.4°.
The treatment was performed at 3 stages:
1. Pre-surgical orthodontics involving leveling and aligning (non-extraction orthodontic treatment)
2. Surgical Treatment (Maxillary Posterior Impaction, Mandibular Set Back and Counter clockwise Rotation)
3. Post-surgical orthodontic treatment. Total treatment time 20 months.
Results: Adequate overjet and overbite were achieved after the treatment. Cephalometric analysis showed the Wits value changed by 2,5mm. The vertical plane angle decreased by 7,1° according to SN-Go-Me and decreased by 6,5° according to FMA.
Conclusion: The orthodontic and orthognathic treatment of patient with skeletally open bite and high angle growth pattern was successful. Initial chewing complaints disappeared due to the ideal occlusion ensured.
Introduction
Skeletal open bite is one of the most difficult problems to treat ortodontically [1,2]. Most patients with anterior open bites have both a dentoalveolar component and increased skeletal vertical dimension [3,4]. The true skeletal open-bite patient would require a combination of orthodontic treatment and orthognathic surgery to achieve ideal occlusion, acceptable esthetics and improved function [5]. This case shows a successful treatment of skeletal open bite, whose magnitude demanded an orthodontic - surgical treatment for reestablishment of ideal occlusion and adequate facial esthetics. In addition, this case is characterized by using only splint unlike other done double-jaw orthognathic surgery.
Diagnosis
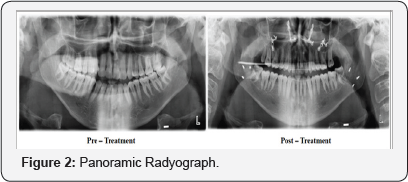
An 25-year old adult man was concerned about the unesthetic appearance of his spaced dentition localized at both upper and lower arches while smiling and forwardly placed lower jaw. The patient's medical history didn't reveal any systemic diseas. Tongue thrust habit and mouth breathing was found at the initial examination. Extraoral examination showed a symmetric face and concave lateral profile. Intraoral examination showed bilaterally Class III canine and molar relationship and 6.2mm anterior open-bite (Figure 1). Panoramic radiograph showed that all teeth were present except upper left third molar and posteroanterior cephalometric radyograph showed no skeletal asymmetry (Figure 2).
There weredentoalveoler discrepancies in both arches (maxillary:-8mm and mandibular:-3mm) according to Hays Nance Analysis. A Bolton discrepancy of 2.9mm maxillary excess in total and of 0.2mm in the anterior teeth was measured. Maxillary midline shifted 2 mm to the left side, mandibular midline shifted 1mm to the left side according to facial midline. The overjet was found to be -2.6mm and the open bite -6.2mm.
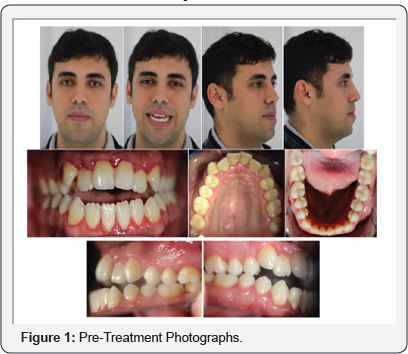

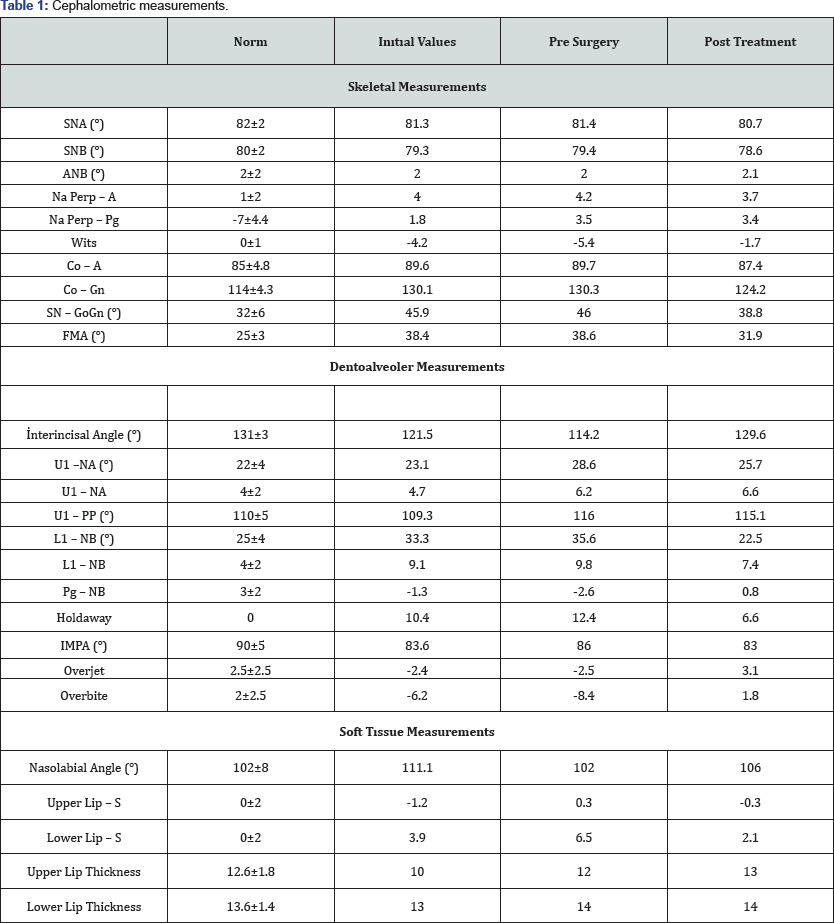
Cephalometric evaluation revealed a Class III skeletal relationship according to Wits appraisal (-4.2 mm), hyperdivergent facial growth pattern (SnGo-Gn = 45.9°, FMA = 38.4°), normal upper insicors (U1-PP = 109.3°) and retrusive lower incisors (IMPA = 83.6°). The concave soft tissue profile was accentuated with retrusion of the upper lip and protrusion of the lower lip in relation to Steiner's S line (Figure 3 and Table 1).
Treatment Objectives
The objectives in the treatment of this malocclusion were:
1) to correct the skeletal Class III malocclusion,
2) to reduce the vertical dimension of the face,
3) to achieve adequate overjet and overbite,
4) to eliminate the lower incisor retrusion and the crowding in the maxillary arch,
5) to correct midlines.
Treatment Progress
Before orthodontic treatment, the oral hygiene motivation was given to the patient and elimination of the tongue thrust habit was planned for true tongue positioning during functional movements. For this purpose, patient was given swallowing exercises. Orthodontic treatment was initiated by levelling and alignment with .014 inch NiTi archwires followed by .016, .018, .020, .017 x .025, .019 x .025 NiTi, 019 x .025 stainless steel and 0.021 x 0.025 stainless steel wires. In addition, in order to control the vertical dimension was placed lingual archwire in mandibula and transpalatal arch in maxilla. Also, upper arch was expanded with the long armes of TPA for the correction of the dental maksillary transversal deficiency.
The intercuspation was checked by occluding the plaster models that were obtained periodically until satisfactory occlusion was attained for performing the orthognathic surgery. After obtaining satisfactory intercuspation of the plaster models, crimpable hooks were placed on a 0.021 x 0.025 stainless steel archwires in all inter-bracket spaces and patient was forwarded to orthognathic surgery.Pre-surgical treatment was completed in 14 months and the patient was scheduled for surgery (Figure 4).
The orthognathic surgery included 4mm maxillary posterior impaction and 5mm backward and counterclockwise rotation (until 2mm overbite achieved) of mandible with bilateral sagittal split osteotomy. Firstly, maxillary posterior impaction was performed. Superior repositioning of the maxilla, via total or segmental maxillary osteotomies, is indicated in skeletal open bite patients with excess vertical maxillary growth. Maxillary impaction allows forward and upward rotation of the mandible, therefore decreasing the lower face height and eliminating anterior open bite. Miniplates were only used in maxilla for post-surgical fixation. Bicortical screws usedin mandible. After the surgery, the patient started to use vertical elastics with occlusal splint to settle the occlusion for a month. After the splint was removed, patient used the elastics all day for a month and 12hours for two months. Appliances were removed six months after the surgery and the total treatment time was 20 months. Retention consisted of a fixed lingual and palatinal retainer (3-3).
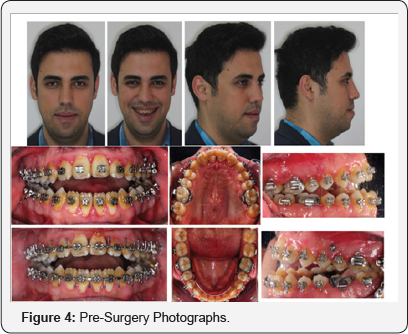
Treatment Results
Post-treatment evaluation showed that patient's complaints had been addressed. Teeth were esthetically pleasing while smiling. The posttreatment records showed a dramatic change in a facial profile and occlusion. The protruding chin and longer lower facial height were reduced resulting in a straighter profile.
An ideal ClassI dental occlusion with favorable overbite and overjet relationships, adequate intercuspation was attained. Dental alignment for the maxillary and mandibular arches was satisfactory. Upper and lower dental midlines were compatible with facial midline (Figure 5).
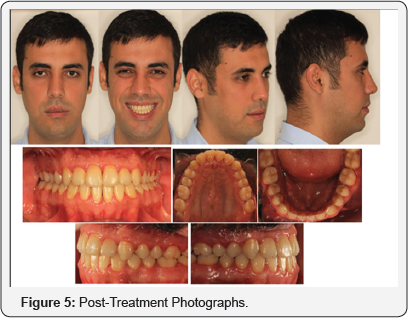
Cephalometric analysis showed that skeletally, the ANB angle was unchanged and the Wits appraisal improved 2.5mm. The amount of mandibular setback was approximately 5mm. A slight decrease of the SNB angle (from 79.3° to 78.6°) was verified. The vertical plane angle dramatically decreased (SN/Go- Gn angle decreased 7.1°, FMA angle decreased 6.5°). In general, the cephalometric changes during the treatment period were favorable and other changes are summarized in the cephalometric summary table. (Table 1) shows the results obtained with the orthognathic surgery and orthodontic finishing stage. Total and partial superimposition of initial and final cephalometric tracings revealed the changes occured with the treatment.
Discussion
Anterior open bite malocclusion is defined as the absence of contact between the maxillary and mandibular incisor edges consequently presenting a negative overbite [7]. Generally, it deteriorates the facial aspect, impairs mastication and speech, subjecting the patient to uncomfortable situations [8]. One indication for surgery obviously is a malocclusion too severe for orthodontics alone. It is possible now to be at least semiquantitative about the limits of orthodontic treatment, in the context of producing normal occlusion. The limits vary both by the tooth movement that would be needed (teeth can be moved further in some directions than others) and by the patient's age (the limits for tooth movement change little if any with age, but growth modification is possible only while active growth is occurring). Because growth modification in children enables greater changes than are possible by tooth movement alone in adults, some conditions that could have been treated with orthodontics alone in children (e.g., a centimeter of overjet) become surgical problems in adults [9].
Orthognathic surgery is considered an adjunct procedure to correct dental deformities in adults The interaction between orthodontics and orthognathic surgery expand the treatment possibilities to solve patient complaints and anxieties that could not be treated alone with orthodontics. Manipulation of the apical bases in the three planes of space can provide a better esthetic improvement in the soft tissues than tooth movement within the apical bases.
Open bite is hardest problem in orthodontics - overall 30% of open bites will return. Dr. Shapiro feels confident in treating open bite, as he knows 70-80% will be corrected and retained reasonably well [10]. Dr. Greg Huang in his new paper found that 80% of open bites whether done with surgery or with orthodontics alone will have reasonable stability, that is, will have contact or overlap. Found 0% of non-growing patients showed relapse, and 17% of growing patients showed relapse at Crib Therapy in Conjunction with Open-bite Treatment (non-surgical) [11].
The stages are the followings for orthognathic surgery cases: Treatment planning, orthodontic treatment, presurgical impression and revaluation of dental positioning, plaster model surgery and construction of an intermediary splint, orthognathic surgery, bracket rebonding and finishing, retention.
In our case,it was followed at this stage. Firstly, non-extraction orthodontic treatment was planned for aligning dental arches. During treatment, occlusion was checked by using the plaster models that were obtained periodically each month until appropriate occlusion was attained for performing the surgery It has started preparing splint stage when patient was ready for surgery. Two splint are prepared (separately for each jaw) in normal procedure of double-jaw surgery for ideal placement. The unique about this case is using only final occlusion splint.Even though double-jaw surgery is performed, no intermediate splint is used. Because, intercuspal relationship was ideal position before surgery, so it was decided to use only final splint for positioning jaws. The orthognathic surgery included 4mm maxillary posterior impaction and 5mm backward and counterclockwise rotation of mandible with bilateral sagittal split osteotomy
In the treatment of open bite, non-surgical treatment options such as molar intrusion with miniplates and mini screws, MEAW (Multiloop Edgewise Archwire) mechanics, orthodontic camouflage with premolars and molars extraction, chincup etc. are also avaiable. However, long term stability of anterior open-bite correction is a challenging problem. Several treatment protocols have been proposed to correct anterior open-bite malocclusions [12-18] that can distinctly influence long-term stability [19-21]. Conventional orthodontic treatment is marked by significant open- bite relapse [22-23]. On the other hand, some studies have shown that orthodontic-surgical correction of open-bite malocclusion has greater long term stability. Because of this, sometimes orthodontic treatment of skeletal open bite in nongrowing patients has been combined with orthognathic surgery to obtain more stable results, although acceptable facial balance and occlusion can be frequently achieved with a nonsurgical open-bite approach [12,24-30].
After the active treatment phase, a stainless steel 3x3 lingual-palatinal canine-to-canine retainers were placed in the maxillary and mandibular arches. Due to the patient s growth and development period over at the start of treatment, fixed retainer were selected for retention protocol. Besides the retainers, the patient was told to continue swallowing exercises.
Conclusion
Orthodontic treatment combined with surgery of this patient was quite successful in the correction the morphologic problem. The patient's psychological satisfaction was achieved.
The overall treatment results seem to have had a very positive impact on his personality and his self-esteem. Patient is followed for long-term results and stability.
Conflict of Interests
The authors declare that there is no conflict of interests regarding the publication of this paper.
Authors’ Contribution
MHB and AYG treated of this case and performed the cephalometric measurements and M£ drafted the manuscript. C£ operated orthognathic surgery treatment of this case. All authors read and approved the final manuscript.
References
- Erverdi N, Usumez S, Solak A (2006) zygomatic anchorage New generation openbite treatment with. Angle Orthod 76(3): 519-526.
- Tuncer C, Atac M, Tuncer B, Kaan E (2008) Osteotomy assisted maxillary posterior impaction with miniplate anchorage. Angle Orthod 78(4): 737-744.
- Kuroda S, Katayama A, Yamamoto TT (2004) Severe anterior open-bi- te case treated using titanium screw anchorage. Angle Orthod 74(4): 558-567.
- Cangialosi TJ (1984) Skeletal morphologic features of anterior open bite. Am J Orthod 85(1): 28-36.
- Cozza P, Baccetti T, Franchi L, Mucedero M, Polimeni A (2005) Sucking habits and facial hyperdivergency risk factors for anterior open bite in the mixed dentition. Am J Orthod Dentofacial Orthop 128(4): 517-519.
- Proffit W, Fields HW, Sarver DM (1983) Combined surgical and orthodontic treatment. Contemporary orthodontics. In: Proffit W, Fields HW, Sarver DM (Eds.), USA St. Louis: Mosby-Year Book; pp. 607-45.
- Nielsen IL (1991) Vertical malocclusions etiology development diagnosis and some aspects of treatment. Angle Orthod 61(4): 247-260.
- Janson G, Valarelli FP, Henriques JF, de Freitas et al. (2003) Stability of anterior open bite nonextraction treatment in the permanent dentition. Am J Orthod Dentofacial Orthop 124(3): 265-276.
- Proffit WR (2007) Contemporary Orthodontics - Elsevier Health Sciences; 4th Edition, pp. 689-690.
- Lo FM, Shapiro PA (1998) The effect of presurgical incisor extrusion on stability of anterior open bite malocclusion treated with orthognathic surgery. Int J Adult Orthodon Orthognath Surg 13(1): 23-34.
- Juang, G, Justus, R, Kennedy, D and Kokich, V (1990) Stability of anterior open bite treated with crib therapy. Angle Orthod 60(1): 17-24.
- Janson G, Valarelli FP (2014) Open bite Malocclusion Treatment and Stability. pp. 403-412.
- Maia FA, Janson G, Barros SE, Maia NG, Chiqueto K, et al. (2010) Longterm stability of surgical-orthodontic open-bite correction. Am J Orthod Dentofacial Orthop 138(3): 254.e1-254.e10.
- Ng CS, Wong WK, Hagg U (2008) Orthodontic treatment of anterior open bite. Int J Paediatr Dent 18(2): 78-83.
- Beane RA Jr (1999) Nonsurgical management of the anterior open bite: a review of the options. Semin Orthod 5(4): 275-283.
- Umemori M, Sugawara J, Mitani H, Nagasaka H, Kawamura H (1999) Skeletal anchorage system for open-bite correction. Am J Orthod Den- tofacial Orthop 115(2): 166-174.
- Epker BN, Fish L (1977) Surgical-orthodontic correction of open-bite- deformity. Am J Orthod 71(3): 278-299.
- Janson G, Crepaldi MV, de Freitas KM, de Freitas MR (2008) Evaluation of anterior open-bite treatment with occlusal adjustment. Am J Orthod Dentofacial Orthop 134(1): 10-11.
- De Freitas MR, Beltrao RT, Janson G, Henriques JF, Candado RH (2004) Long-term stability of anterior open bite extraction treatment in the permanent dentition. Am J Orthod Dentofacial Orthop 125(1): 78-87.
- Janson G, Valarelli FP, Henriques JF, de Freitas MR, Candado RH (2003) Stability of anterioropen bite nonextraction treatment inthe permanent dentition. Am J Orthod Dentofacial Orthop 124(3): 265-276.
- Espeland L, Dowling PA, Mobarak KA, Stenvik A (2008) Three-year stability of open-bite correction by 1-piece maxillary osteotomy. Am J Orthod Dentofacial Orthop 134(1): 60-66.
- Lopez-Gavito G, Wallen TR, Little RM, Joondeph DR (1985) Anterioro- pen-bite malocclusion: a longitudinal10-year postretention evaluation of orthodontically treated patients. Am J Orthod 87(3): 175-186.
- Remmers D, Van't Hullenaar RW, Bronkhorst EM, Bergé SJ, Katsaros C, et al (2008) Treatment results and long-term stability of anterior open bite malocclusion. Orthod Craniofac Res 11(1): 32-42.
- Kuroda S, Sakai Y, Tamamura N, Deguchi T, Takano-Yamamoto T (2007) Treatment of severe anterior open bite with skeletal anchorage in adults: comparison with orthognathic surgery outcomes. Am J Orthod Dentofacial Orthop 132(5): 599-605.
- Vaden JL (1998) Nonsurgical treatment of the patient with vertical discrepancy. Am J Orthod Dentofacial Orthop 113(5): 567-582.
- Hiller ME (2002) Nonsurgical correction of Class III open bite malocclusion in an adult patient. Am J Orthod Dentofacial Orthop 122(2): 210-216.
- Smith GA (1996) Treatment of an adult with a severe anterior open biteand mutilated malocclusion without orthognathic surgery. Am J Orthod Dentofacial Orthop 110(6): 682-687.
- De Cuebas JO (1997) Nonsurgical treatment of a skeletal vertical discrepancy with a significant open bite. Am J Orthod Dentofacial Orthop 112(2): 124-131.
- Kondo E, Aoba TJ (2000) Nonsurgical and nonextraction treatment of- skeletal Class III open bite: its long-term stability. Am J Orthod Dento- facial Orthop 117(3): 267-287.
- Hamamci N, Basaran G, Sahin S (2006) Nonsurgical correction of anadult skeletal Class III and open-bite malocclusion. Angle Orthod 76(3): 527-532.






























