Dentin Dysplasia Type I-Diagnosis and Treatment: Case Report
Carmem Dolores Vilarinho Soares de Moura1*, Lúcia de Fátima Almeida de Deus Moura2, Heloísa Clara Santos Sousa2, Markelane Santana Silva1, Graciela Maria Oliveira Sipauba1 and Marina de Deus Moura de Lima2
1Department of Restorative Dentistry, Universidade Federal does Piauí-UFPI, Brazil
2Department of Pathology and Dentistry Clinic, Universidade Federal do Piauí-UFPI, Brazil
Submission: August 22, 2017; Published: October 25, 2017
*Corresponding author: Carmem Dolores Vilarinho Soares de Moura, DDS, MSc, PhD, Adjunct Professor, Department of Restorative Dentistry, School of Dentistry, Universidade Federal do Piauí-UFPI, Bairro Ininga, 64049-550 Teresina-Piauí, Brazil, Tel: +558632371517; Email: carmemdvsm@uol.com.br
How to cite this article: Carmem D V S d M, Lucia d F A d D M, Helo�sa C S S, Markelane S S, Graciela M O S ,et al. Dentin Dysplasia Type I-Diagnosis and Treatment: Case Report. Adv Dent & Oral Health. 2017; 6(1): 555676. DOI: 10.19080/ADOH.2017.06.555676
Abstract
This paper aims to report the case of a child with dentin dysplasia type I. An 8 year old female child was referred to the Children's Dental Clinic of the Universidade Federal do Piauf with an aesthetic complaint caused by missing teeth. Four permanent first molars, premolar upper right and upper left permanent canine were present. There was satisfactory oral hygiene and no dental diseases. Anamnesis and laboratory tests did not detect any systemic disorders. Evaluations of initial panoramic radiographs and computed tomography showed permanent teeth with apparently normal crowns, with short and conical roots and obliteration of the pulp chamber, confirming the diagnostic hypothesis of Dentin Dysplasia type I. Root Dentin Dysplasia or Dentin Dysplasia type I is a rare hereditary autosomal dominant disorder, with a complex diagnosis, and the need for evaluation and interdisciplinary planning. There is no specific treatment for this genetic condition. Temporary mucosa-supported prosthesis reimbursed with resilient resin was made to preserve the sites of erupted teeth and those erupting. Monitoring is to be done until the growth of the facial structures is completed, allowing for rehabilitation with fixed prostheses on implants
Keywords: Pathology; Oral; Pediatric dentistry, Dentin dysplasia, Diagnosis, Dental care
Abbreviations: DDI: Dentina Dysplasia Type-I
Introduction
Dentin dysplasia is a rare hereditary autosomal dominant disorder, with prevalence of 1:100,000 [1,2] characterized by an altered dentin structure, aesthetic involvement and teeth that can present mobility, early exfoliation and association with abscesses or cysts [3-6].
Two phenotypes have been described [1]. Type I or root dentin dysplasia (DD I) can affect the two dentitions, and is characterized by a normal appearance of dental crowns, short, conical or missing roots, partial or total obliteration of the pulp chamber, and the presence of periodical cysts [2,3]. Type II or coronal dentin dysplasia (DD II) is more frequent in deciduous teeth, showing teeth with brown or blue amber discoloration and pulp obliteration. When DD II is present in the permanent dentition, the teeth have a normal appearance or slight discoloration and the presence of pulp nodules [2,3,7].
This paper aims to report the case of a child with dentin dysplasia type I.
Case Report

An 8 years old female was referred to the Children’s Dental Clinic of the Universidad Federal do Piauí with an aesthetic complaint caused by missing teeth (Figure 1). The teeth erupted and soon after exfoliated spontaneously. There was an alveolar ridge deficiency in the maxilla and mandible, and decreased vertical height due to missing teeth. The child presented introspective behavior and little collaborator for dental procedures.
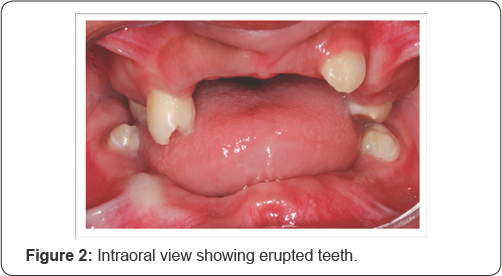
There is no report of other family members with similar dental changes. In the first examination the following fully erupted teeth were present: four permanent first molars, premolar upper right and upper left permanent canine. There was satisfactory oral hygiene and no dental diseases. The teeth had normal color and the absence of mobility ( Figure 2).
Laboratory tests such as blood count, ionic calcium, phosphorus, serum iron, 17 alpha hydroxy progesterone, and rostenedione, alkaline phosphates total protein and fractions, A/G ratio, somatomedin and GH stimulation test after coniine did not detect any systemic disorders. Radiographs of hands and wrists showed images of bone development compatible with a 6-year- old child (Gilsanz-Ratib digital atlas for bone age estimations).
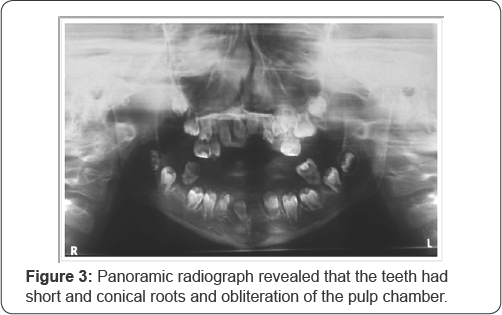
Evaluations of initial panoramic radiographs (Figure 3) and computed tomography showed permanent teeth in different stages of development, with apparently normal crowns, with short and conical roots and obliteration of the pulp chamber, confirming the diagnostic hypothesis of dysplasia dentine type I.
Due the psychological framework of the patient with social isolation behavior, which is a condition that worried the family, we opted for the placing of temporary mucosa-supported prosthesis reimbursed with resilient resin to preserve the sites of erupted teeth and those erupting. The child’s mother signed a written consent, allowing the case to be documented for publication in a scientific journal.
Moldings were made of the dental arches with Hydro gum ® (Zhermack clinical, Rovigo, Italia) and children’s trays, and then the molds were cast with a special plaster, type IV Drone (Dentsply, Petropolis-RJ, Brazil), to obtain the study design and manufacture of a custom tray in clear acrylic (Vipident plus, Pirassununga- SP, Brazil). This was used for the functional molding and to generate the working model; for this, Godiva stick type 1 (SDS Kerr, Joinville-SC, Brazil)was used in order to obtain an adequate sealing peripheral, and soft Politer Impregum™ Soft (3M ESPE, Neuss, Germany) for the molding itself. The working models were sent to the laboratory for the base-proof and wax plans.
In the second session, the base-proof and wax plans were tested, and the vertical dimension was defined using a Willis compass. This measurement was decreased 3mm to get the vertical height of occlusion. Markings were also made to set a high smile line and intercanine space, which in this case was made using the line of the pupils, and then the upper and lower planes were fixed with clips. The bases were replaced in the working model and the assembly was made in Articulator, semi-adjustable, Arson (Board) for mounting the teeth. Stock teeth 1D were selected to anterior maxillary, 3M to anterior mandible and 3M for posterior Vipident plus (VIPI, Pirassununga-SP, Brazil).
The patient returned to the proof of the teeth mounted in wax. In this session were made swallowing and phonetic tests, confirming ideal height of the vertical occlusion, without invasion of free functional space and without need for adjustments. After the choice the color of gingiva - medium pink (STG dentes ® ), the prostheses was remand to the laboratory for acrylization.
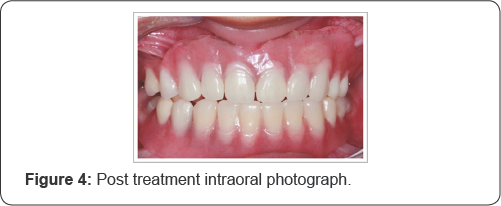
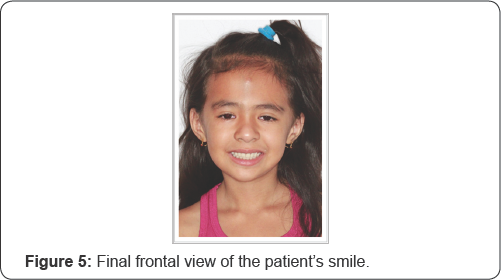
In the fourth session, the installation of the prostheses (Figure 4,5) was completed with relining with dense Soft Comfort ® resin (Decrial, Pirassununga-SP, Brazil). Small occlusal adjustments were made with Minicab Pmtungsten drills (Dedeco). After this step was completed, the prostheses were delivered and guidelines were given. The mother agreed that the patient would return bimonthly, or when the prosthesis was difficult to use, in order to make adjustments due to the eruptive process and/or tooth loss.
The patient returned three months after the making of the prosthesis for adjustments, due to tooth eruption 24. Adjustments to the prosthesis were made. Monitoring is to be done until the growth of the facial structures is completed, allowing for rehabilitation with fixed prostheses on implants.
Discussion
The absence of teeth influences the aesthetics and masticator function with consequent impairment in the quality of life of the patient5. Dentin dysplasia is a rare condition, with a complex diagnosis, and the need for evaluation and interdisciplinary planning [8]. The differential diagnosis of DDI is made with dentinogenesisimperfecta, aware autosomal dominant condition, at which teeth may exhibit color changes, hypo mineralized and exposed dentin, bulbous crowns, cervical constriction, thick and short roots and obliteration of the pulp chamber [2].
Patients with missing teeth, spontaneous exfoliation of teeth, periodical lesions without a history of pulp involvement and mandible atrophy, as in this report, dentin dysplasia type I should be considered as first hypothesis diagnostic [5]. The maxillomandibular atrophy observed commonly in patients with dentin dysplasia type I, can be considered as a sequelae of anomalous root development or early tooth loss [1]. There is no consensus regarding the clinical and radiographic findings present in patients with dentin dysplasia type I [6]. In this case, the changes observed are not characteristic of any DD I subtype described [6,9,10].
Dysplasia dentin type I has been reported in the literature as a hereditary disease of autosomal dominant character. However, in 2013, Cherkaoui et al. [1] published a study conducted on a Moroccan family in which this condition manifested itself as an autosomal recessive inheritance. In the case described, there are no reports of similar cases in the family, which excludes the dominant manifestation in this patient.
Early diagnosis is important for planning and preventive strategies [11-14]. In the case of the reported patient, preventive measures were adopted in order to preserve the healthy teeth, such as control of ingestion of sugar and adequate oral hygiene; this is because the prognosis was unfavorable due to short roots and the presence of periodical radiolucency that would favor early losses [11,14].
There is no specific treatment for this genetic condition [6,9]. Overall, the proposed strategies aim to preserve erupted teeth the longest time possible [6,9]. Still, life expectancy of dentition is short, and the patient will need periodic adaptations in the oral prosthesis [11,14].
The treatments described for dentin dysplasia type I also include endodontic therapy, periodical curettage and functional space maintainers [6,9,15-17]. Functional rehabilitation with prosthesis, after extraction of all the teeth and cystic curettage, was also identified as an option [18]. In the present case, we opted for the maintenance of the teeth until their exfoliation and a temporary mucosa-supported prosthesis was made, readapted at each new eruption and/or dental exfoliation. The decision of such conduct aims to preserve bone structure for later confection of fixed implant-supported prostheses.
References
- Cherkaoui JI, El Alloussi M, Laarabi FZ, Bouhouche A, Ameziane R, et al. (2013) Inhabitual autosomal recessive form of dentin dysplasia type I in large consanguineous Maroccan family. Eur J Med Genet 56(8): 442444.
- de La Dure Molla M, Philippe Fournier B, Berdal A (2015) Isolated dentinogenesis imperfecta and dentin dysplasia: revision of the classification. Eur J Hum Genet 23(4): 445-451.
- Shields ED, Bixler D, el Kafrawy AM (1973) A proposed classification for heritable human dentine defects with a description of a new entity. Arch Oral Biol 18(4): 543-553.
- Witkop CJ (1988) Amelogenesis imperfecta, dentinogenesis imperfecta and dentin dysplasia revisited: problems in classification. J Oral Pathol 17(9-10): 547-53.
- Komlos G, Joob Fancsaly A, Pataky L, Shkolnik T, Bogdan S, et al. (2015) Difficulties in differential diagnosis of dentin dysplasia. Case report. Fogorv Sz 108(2): 53-56.
- Rocha CT, Nelson Filho P, Silva LA, Assed S, Queiroz AM, et al. (2011) Variation of dentin dysplasia type I: report of atypical findings in the permanent dentition. Braz Dent J 22(1): 74-78.
- Cabay RJ (2014) An overview of molecular and genetic alterations in selected benign odontogenic disorders. Arch Pathol Lab Med 138(6): 754-758.
- Pintor A, Alexandria A, Marques A, Abrahao A, Guedes F, et al. (2015) Histological and Ultrastructure Analysis of Dentin Dysplasia Type I in Primary Teeth: A Case Report. Ultrastruct Pathol 39(4): 281-285.
- Singh A, Gupta S, Yuwanati MB, Mhaske S (2013) Dentin Dysplasia type I. BMJ Case Rep pii: bcr2013009403.
- Ye X, Li K, Liu L, Yu F, Xiong F, et al. (2015) Dentin dysplasia type I-novel findings in deciduous and permanent teeth. BMC Oral Health 15(1): 163.
- Toomarian L, Mashhadiabbas F, Mirkarimi M, Mehrdad L (2010) Dentin dysplasia type I: a case report and review of the literature. J Med Case Rep 4: 1.
- Ozer S, Ozden B, OtanOzden F, Gunduz K (2013) Dentinal dysplasia type I: a case report with a 6-year follow up. Case Rep Dent 2013: 659084.
- Nettem S, Nettemu SK, Basha K, Venkatachalapathi S (2014) Implant based oral rehabilitation of variant model of type I dentinal dysplasia: a rare case report. Dent Res J (Isfahan) 11(4): 513-517.
- Malik S, Gupta S, Wadhwan V, Suhasini GP (2015) Dentin dysplasia type I - A rare entity. Oral Maxillofac Pathol 19(1): 110.
- Brenneise CV, Dwornik RM, Brenneise EE (1989) Clinical, radiographic and histological manifestations of dentin dysplasia, type I: Report of case. J Am Dent Assoc 119(6): 721-723.
- Vieira AR, Modesto A, Cabral MG (1998) Dentinal dysplasia type I:report of an atypical case in the primary dentition. ASDC J Dent Child 65(2): 141-144.
- Shankly PE, Mackie IC, Sloan P (1999) Dentinal dysplasia type I: Report of a case. Int J Paediatr Dent 9(1): 37-42.
- Neumann F, Wurfel F, Mundt T (1999) Dentin dysplasia type I -a case report. Ann Anat 181(1): 138-140.






























