Salivary Glucose: A Metabolic Disease Marker and a Risk Factor for Oral Disease Development
J Max Goodson*
The Forsyth Institute, USA
Submission: March 23, 2017; Published: April 13, 2017
*Corresponding author: J Max Goodson, The Forsyth Institute, 245 First Street, Cambridge, MA 02140, USA, Tel: 617-892-8266; Fax: 617-262-4021; Email: mgoodson@forsyth.org
How to cite this article: J Max G. Salivary Glucose: A Metabolic Disease Marker and a Risk Factor for Oral Disease Development. Adv Dent & Oral Health. 2017; 4(3): 555640. DOI: 10.19080/ADOH.2017.04.555640
Abstract
The existence of glucose in saliva as a step in development of metabolic disease including diabetes has not received adequate recognition as an oral disease risk factor. Hyperglycemia, the driving function for appearance of salivary glucose is rare in children and appears mainly in adulthood. The presence of salivary glucose modifies salivary microbial composition and affects both dental caries and gingivitis. Data on salivary pH as a surrogate measure is reviewed to suggest that pH indicator paper could serve as a surrogate chairside diagnostic of hyperglycemia.
Keywords: Glucose, Saliva; Hyperglycemia; Dental caries, Gingivitis
Hyperglycemia
Hyperglycemia is a defining characteristic of diabetes and also occurs in pre-diabetic states. Normal blood glucose levels are between 70 and 100mg/dL. Blood levels of greater than 100mg/dL glucose are recognized as being hyperglycemic. Glucose levels of greater than 125mg/dLare recognized as being diabetic. Impaired glucosetolerance (fasting glucose > 110mg/dL) was investigated in a large cohort of individuals (112,960 Japanese) including a wide age span (14-94) over 15 years. From these data (Figure 1) we see that impaired glucose tolerance occurred in males before females but levels do not become an important factor in the population until around the age of 30. Even though this characteristic would likely differ considerably among world populations, the point here is that hyperglycemia occurs as individuals become adult and is rare in children. Most hyperglycemic children would be those with Type 1 diabetes. In a study of 10-year old Kuwaiti children Goodson et al. [1], only 2% of the children had salivary glucose values that would suggest hyperglycemia.

Salivary Glucose

Glucose appears in the saliva of individuals (Figure 2) with hyperglycemia Hartman et al. [2]. This model predicts that normal blood glucose does not result in salivary glucose. When blood levels exceed 84.8mg/dL, measureable glucose appeared in saliva. When blood values exceed 100mg/dL, saliva concentrations exceed 1.13mg/dL. It is generally recognized that diabetics have higher salivary concentrations of glucose than in normal subjects Mascarenhas et al. [3]. These values would likely differ considerably among different populations.
When dentists speak, of salivary glucose, it is usually associated with consumption of sweets. Sucrose is cleared from the oral cavity with a halftime of 2.2 minutes Dawes [4]. So, within 5 halftimes (11 minutes) there is essentially no sucrose remaining in the mouth. In contrast, when glucose is excreted into saliva due to metabolic disease, it is present for the entire waking period. Even though salivary glucose concentration in diabetics is low (around 1-3mg/dL) it is present all day. Hence, oral diseases based on bacteria that metabolize glucose would likely be augmented.
Salivary Glucose and Oral Bacteria
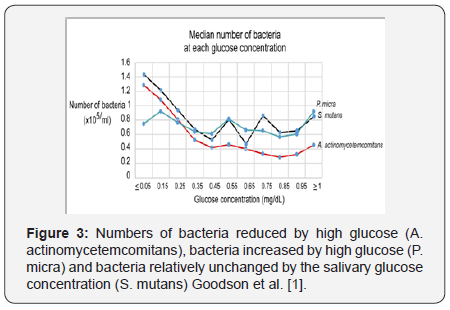
One of the effects of high glucose is a modification of the salivary microbiota (Figure 3). Most salivary bacteria are reduced by high salivary glucose Goodson et al. [1], some to a greater degree than others. A. actinomycetemcomitans is among the most sensitive to salivary glucose. S. mutans and P micra by comparison are relatively resistant to change by salivary glucose. Hence, one effect of salivary glucose is to change the oral microbial composition. It is proposed that this reduction in bacterial numbers is the result of salivary acidification by the conversion of salivary glucose to short-chain fatty acids.
The measurement of bacterial numbers is a crude measure of bacterial effect. It is likely that he continuous presence of glucose in saliva would also modify the metabolic nature of many oral bacteria. For example, glutamate oxaloacetate transaminase (GOT) and glutamate pyruvate transaminase (GPT) levels in saliva were different in diabetics compared to non-diabetics Verma et al. [5].
Salivary Glucose and Clinical Response
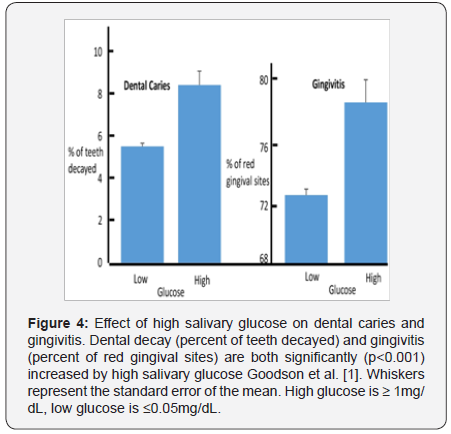
The effects of high salivary glucose on oral disease are a significant increase in both dental caries and gingivitis (Figure 4). The number of carious lesions per tooth increased from 5.43% decayed to 8.35% decayed. The gingival redness increased from 72.55% of sites to 78.58%. Measurement of salivary glucose is technically difficult because of its low concentration (often less than 1mg/dL and seldom more than 3mg/dL). In our studies of Kuwaiti children, we used a glucose oxidase method with a fluorescent label implemented on a robotic chemical platform. In addition, we boiled samples to denature enzymes such as catalyse that interfered with our assay and to kill bacteria that might consume glucose in the saliva sample. A chairside equivalent of this assay has not been devised. There may be, however, a reasonable chairside surrogate measure for salivary glucose, namely salivary pH (Table 1).
Salivary Ph and Diabetes
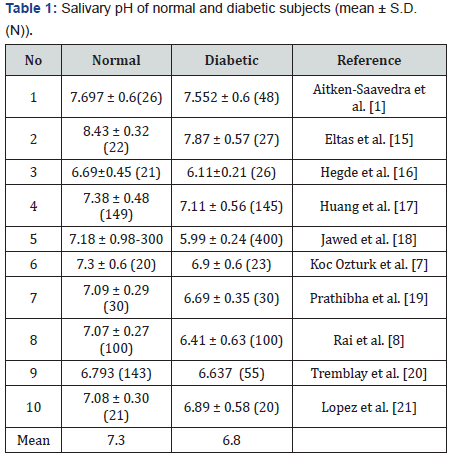
Casual inspection of the data of Table 1 would suggest that a salivary pH lower than 7 could be diabetic. It has been suggested that salivary pH could be used as a simple screening measure for detection of metabolic syndrome or diabetes Aitken-Saavedra et al. [6]. Reported differences are of sufficient magnitude to be measured by pH paper Koc Ozturk et al. [7]; Rai et al. [8] where it served as a simple chairside diagnostic. There are other conditions associated with lowered saliva pH. These include oral cancer Ramya et al. [9] and ionizing radiation exposure Vuotila et al. [10], mouth breathing Choi et al. [11], bulimia Paszynska et al. [12], gastroesophageal reflux disease Preetha et al. [13] and consumption of juices and cola-based beverages Tenuta et al. [14].
Conclusion
The added intraoral disease risk associated with hyperglycemia found in both diabetic and prediabetic states should be a recognized oral disease risk factor that may be evaluated by measurement of saliva pH.
References
- Goodson JM, Hartman ML, Shi P, Hasturk H, Yaskell T, et al. (2017) The salivary microbiome is altered in the presence of a high salivary glucose concentration. PloS one 12(3): e0170437.
- Hartman ML, Goodson JM, Barake R, Alsmadi O, Ariga J, et al. (2015) Salivary glucose concentration exhibits threshold kinetics in normalweight, overweight, and obese children. Diabetes Metab Syndr Obes 8: 9-15.
- Mascarenhas P, Fatela B, Barahona I (2014) Effect of diabetes mellitus type 2 on salivary glucose--a systematic review and meta-analysis of observational studies. PloS one 9(7): e101706.
- Dawes C (2008) Salivary flow patterns and the health of hard and soft oral tissues. J Am Dent Assoc 139: 18S-24S.
- Verma M, Metgud R, Madhusudan AS, Verma N, Saxena M, et al. (2014) A comparative study of glutamate oxaloacetate transaminase (got) and glutamate pyruvate transaminase (gpt) levels in the saliva of diabetic and normal patients. Biotech Histochem 89(7): 529-534.
- Verma M, Metgud R, Madhusudan AS, Verma N, Saxena M, et al. (2014) A comparative study of glutamate oxaloacetate transaminase (got) and glutamate pyruvate transaminase (gpt) levels in the saliva of diabetic and normal patients. Biotech Histochem 89(7): 529-534.
- Koc OL, Ulucan K, Akyuz S, Furuncuoglu H, Bayer H, et al. (2012) The investigation of genetic polymorphisms in the carbonic anhydrase vi gene exon 2 and salivary parameters in type 2 diabetic patients and healthy adults. Mol Biol Rep 39(5): 5677-5682.
- Rai K, Hegde AM, Kamath A, Shetty S (2011) Dental caries and salivary alterations in type i diabetes. J Clin Pediatr Dent 36(2): 181-184.
- Ramya AS, Uppala D, Majumdar S, Surekha C, Deepak KG (2015) Are salivary amylase and ph - prognostic indicators of cancers?. J Oral Biol Craniofac Res 5(2): 81-85.
- Vuotila T, Ylikontiola L, Sorsa T, Luoto H, Hanemaaijer R, et al. (2002) The relationship between mmps and ph in whole saliva of radiated head and neck cancer patients. J Oral Pathol Med 31(6): 329-338.
- Choi JE, Waddell JN, Lyons KM, Kieser JA (2015) Intraoral ph and temperature during sleep with and without mouth breathing. J Oral Rehabil 43(5): 356-363.
- Paszynska E, Slopien A, Weglarz M, Linden RW (2015) Parotid salivary parameters in bulimic patients - a controlled clinical trial. Psychiatr Pol 49(4): 709-720.
- Preetha A, Sujatha D, Patil BA, Hegde S (2015) Oral manifestations in gastroesophageal reflux disease. Gen Dent 63(3): e27-31.
- Tenuta LM, Fernandez CE, Brandao AC, Cury JA (2015) Titratable acidity of beverages influences salivary ph recovery. Brazilian oral research, pp. 29.
- Eltas A, Tozoglu U, Keles M, Canakci V (2012) Assessment of oral health in peritoneal dialysis patients with and without diabetes mellitus. Perit Dial Int 32(1): 81-85.
- Hegde A, Shenoy R, D’Mello P, Smitha A, Tintu A, et al. (2010) Alternative markers of glycemic status in diabetes mellitus. Biomedical Research 21(3): 252-256.
- Huang JH, Liu Y, Liu HW (2012) comparative study on oral candidal infection in individuals with diabetes mellitus and impaired glucose regulation. Zhonghua Kou Qiang Yi Xue Za Zhi 47(6): 335-339.
- Jawed M, Khan RN, Shahid SM, Azhar A (2012) Protective effects of salivary factors in dental caries in diabetic patients of pakistan. Exp Diabetes Res 2012: 947304.
- Prathibha KM, Johnson P, Ganesh M, Subhashini AS (2013) Evaluation of salivary profile among adult type 2 diabetes mellitus patients in south india. J Clin Diagn Res 7(8): 1592-1595.
- Tremblay M, Brisson D, Gaudet D (2012) Association between salivary ph and metabolic syndrome in women: A cross-sectional study. BMC oral health 12(1): 40.
- Lopez ME, Colloca ME, Paez RG, Schallmach JN, Koss MA, et al. (2003) Salivary characteristics of diabetic children. Braz Dent J 14(1): 26-31.
- Kuzuya M, Ando F, Iguchi A, Shimokata H (2007) Age-specific change of prevalence of metabolic syndrome: Longitudinal observation of large japanese cohort. Atherosclerosis 191(2): 305-312.






























