Tongue - Cause and Correction of Anterior Open Bite Malocclusion
A Arif Yezdani*1 and Jabeen Fathima2
1Department of Orthodontics and Dentofacial Orthopaedics, Sree Balaji Dental College and Hospital, India
2Yezdani Dental and Orthodontic Center, India
Submission: February 10, 2017; Published: March 24, 2017
*Corresponding author: Arif Yezdani, MDS, FWFO, Professor & Director, Dept. of Orthodontics and Dentofacial Orthopaedics, Bharath University, Sree Balaji Dental College and Hospital, Narayanapuram, Pallikaranai, Chennai-600100, India, Email: arifyezdani@yahoo.com
How to cite this article: A Arif Yezdani, Jabeen F. Tongue - Cause and Correction of Anterior Open Bite Malocclusion. Adv Dent & Oral Health. 2017; 4(3):555636. DOI: 10.19080/ADOH.2017.04.555636
Abstract
Objective: To evaluate the efficiency of a low lying transpalatal arch along with fixed appliance therapy in the correction of an anterior open bite malocclusion with an orthognathic maxilla and a mildly prognathic mandible with bi-maxillary dento-alveolar protrusion and forward tongue posture.
Methods: Treatment involved strap-up of a pre-adjusted edgewise appliance, Roth’s prescription (0.022 X 0.028 - inch slot), with a low lying transpalatal arch 4mm away from the palatal mucosa, and a non-extraction approach. The case was assessed at start of orthodontic treatment (T1), and end of orthodontic treatment (T2).
Results: At T2, the anterior open bite was corrected and the canines were treated to a class I relation. The proclined maxillary incisors as also the proclined and imbricated mandibular incisors were corrected.
Conclusion: Anterior open bite malocclusion with forward tongue posture was effectively corrected with the use of a low lying transpalatal arch using the forces of the tongue during deglutition and mastication. The proclination of maxillary incisors and proclination and imbrication of mandibular incisors were corrected with the fixed appliance therapy.
Keywords: Low lying transpalatal arch; Tongue forces; Deglutition; Pre-adjusted edgewise appliance therapy
Introduction
Dentofacial morphology is inadvertently influenced by the tongue and that tongue thrusting or forward tongue posture can affect the stomatognathic function and can cause open bite malocclusion [1-3]. Tongue pressure ranges from 41 to 709g/cm2 according to Winders [4] and that constant tongue thrust or forward tongue posture can cause proclination of maxillary and mandibular anterior teeth and /or anterior open bite. Posterior open bite too can be a sequelae of lateral tongue thrust. The role of the tongue and the trans palatal arch (TPA) has been well documented in the literature. The TPA is designed with a loop in its middle portion such that it traverses the entire contour of the palatal mucous membrane. It facilitates anchorage and stabilization of molar, correction of molar rotation, molar intrusion [5,6], molar expansion [7-9] and molar distalization [10]. It has been reported that the tongue during deglutition and mastication inadvertently encourages molar intrusion [11]. Animal studies have shown that TPA can control vertical growth [12]. Finite element analysis studies too suggest that TPA increases molar displacement and controls molar rotation [13]. This case report reiterates the fact that though the tongue could have been the causative factor of the anterior open bite its action on the fabricated TPA in vivo had been reined in to correct what it had caused, namely the anterior open bite.
Case Report
Diagnosis and etiology

A 29 year old male presented with forward placement of the maxillary and mandibular incisors, and anterior open bite with forward tongue posture. Extra oral assessment: The patient had a leptoprosopic face, mildly concave profile, mild anterior divergence, incompetent lips, clinical high mandibular plane angle, with no signs of temporo mandibular joint dysfunction (Figure 1a- 1c). Intra oral assessment: Oral hygiene was satisfactory.


The maxillary arch was U-shaped with severely proclined maxillary incisors. The mandibular arch was also U-shaped with proclination and imbrication of mandibular incisors. Anterior open bite with forward tongue posture was observed. The maxillary and mandibular dental midlines and the skeletal midlines coincided with each other. On both sides the molar relation and canine relation was Class III (Figure 1d-1h).
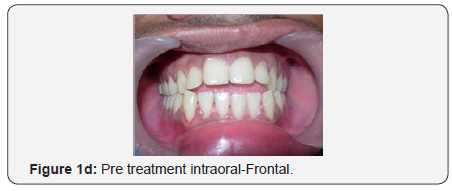
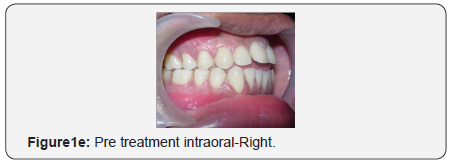
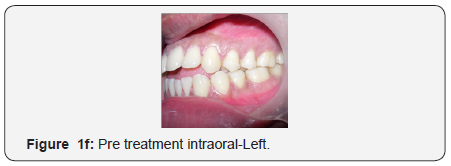
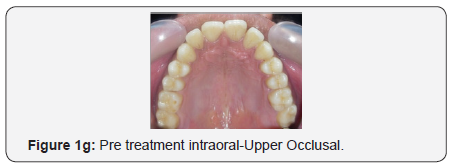
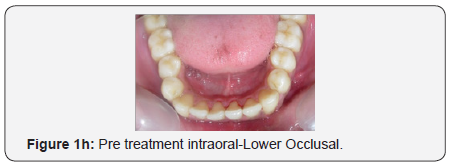
Radiographic assessment: The panoramic radiograph confirmed the presence of all permanent teeth with the exception of missing maxillary and mandibular third molars on the right side and horizontally impacted mandibular third molar on the left side with normal alveolar bone levels. Cephalometric analysis revealed a mild skeletal Class III pattern, with a nearly orthognathic maxilla and a mildly prognathic mandible, with a high mandibular plane angle and severely proclined maxillary and mandibular incisors
Treatment objectives
The main treatment objectives were to improve smile esthetics, soft tissue profile, lip competence and speech. Since the maxilla was orthognathic and the mandible mildly prognathic, and the anterior open bite was dentoalveolar in nature greater emphasis was laid for the correction of the anterior open bite and the retraining of the forward posture of the tongue as also the increased proclination of the maxillary incisors and proclined and imbricated mandibular incisors. A non extraction approach was decided upon.
Treatment alternatives
Micro implants placed palatally between first and second maxillary molars could have been used to intrude the maxillary molars to correct the anterior open bite. However, an attempt was made to correct the anterior open bite with a low lying TPA with retraining of the forward posture of the tongue with lingual buttons bonded to the palatal surfaces of the maxillary incisors along with Roth’s pre adjusted edgewise appliance therapy.
Treatment progress
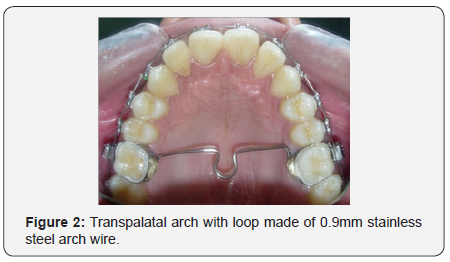
Pre adjusted edgewise brackets (Roth prescription,0.022 x 0.028-inch slot) were bonded, complete with a low lying trans palatal arch made of 0.9 mm stainless steel arch wire, positioned 4 mm away from the palatal surface (Figure 2). Aligning and levelling was done with 0.014 inch nickel titanium wires (Figure 3). It was subsequently upgraded to 0.016x0.022 inch stainless steel arch wires and finished with 0.017x0.025 inch stainless steel arch wires. Lingual bondable buttons were bonded to the palatal surfaces of the maxillary incisors to retrain the tongue and posture it in its normal position.

Results
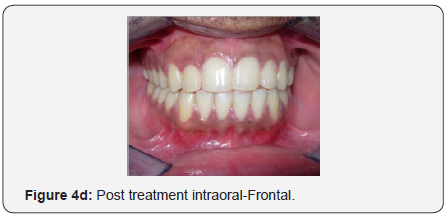
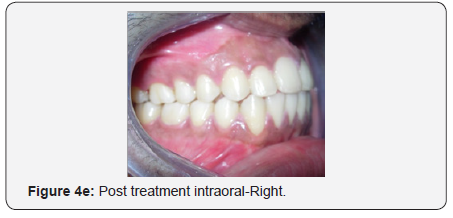
The patient showed remarkable improvement in the correction of the anterior open bite achieved to a great extent by the low lying transpalatal arch which caused molar intrusion during every act of mastication and deglutition. The proclined maxillary incisors and the proclined and imbricated mandibular incisors were corrected and a class I canine relationship was achieved with the fixed appliance therapy. A pleasing soft tissue profile was achieved (Figure 4a-4h).






Discussion
Anterior open bite results due to the combined influence of skeletal, dental, habitual and functional factors. Molar intrusion to correct the anterior open bite can be achieved by high– pull headgear and TPA but their effectiveness has not been demonstrated in clinical studies [14-16]. Microimplants have been understood to bring about absolute intrusion [17] and its use with modified TPA has also been reported in the literature [18]. De-Berardinis et al. [19] used a vertical holding appliance (VHA) which was a modified TPA made by the addition of an acrylic plate which was significant in reducing the percentage of lower anterior vertical face height.
This case validates the evidence-based use of a low lying TPA. Tongue pressure increased when the loop was positioned distally and that maximum pressure was obtained when the loop was placed at the middle of the palatal mucous membrane between the first and second maxillary molars. It has been opined that bolus or fluid is swept backward down the pharynx as the tongue activity is like a wave along its dorsum [20,21].
The TPA interferes with tongue motion around the area of maxillary second molars during the act when the tongue moves upward and backwards toward the hard palate. Chiba et al. [22] in a study to measure the tongue pressure exerted on the loop of TPA during deglutition and the influence of the distance of the loop from the palatal mucosa opined that maximum tongue pressure was observed when the loop was 6mm from the palatal mucosa but for practical applications 4mm was observed to be sufficient. Kaifan Xu et al. [23] in another study also opined that increasing the distance of the pads away from the mucosa leads to augmentation of tongue force. In the case presented the loop of the TPA was kept 4mm away from the palatal mucosa and effective intrusion of the maxillary molars was observed.
Molar intrusion is deemed to be an efficient treatment for an open bite and is effective for anteriorly rotating the mandible to improve the facial profile, especially in hyperdivergent patients as has been observed in various cases that had been reported. Kincaid [24] reported that the average frequency of deglutition per day was 1600 times. Therefore, it seems appropriate to conclude that the tongue can deliver orthodontic forces with considerable frequency to correct the anterior open bite which could be further augmented with the use of anterior open bite elastics with fixed appliance therapy as had been observed in the case treated. The bonded palatal lingual buttons were effective in the training of the faulty posture of the tongue. The patients’ muscle strength and morphology of the tongue during deglutition also plays a very vital role in the treatment prognosis.
Conclusion
TPA with a loop 4mm from the palatal mucosa was effective in the intrusion of the maxillary molars and the subsequent autorotation of the mandible that occurred was found to be the reason for the correction of the anterior open bite. Tongue forces against the TPA during mastication and deglutition could be reined in to correct the anterior open bite malocclusion with finishing and detailing of the teeth concomittantly corrected with fixed appliance therapy.
References
- Kydd WL (1957) Maximum forces exerted on the dentition by the perioral and lingual musculature. J Am Dent Assoc 55(5): 646-651.
- Staub WJ (1961) Malfunction of the tongue. Part II. The abnormal swallowing habit: its causes, effects, and results in relation to orthodontic treatment and speech therapy. Am J Orthod 47(8): 596- 617.
- Christiansen RL, Evans CA, Sue SK (1979) Resting tongue pressures. Angle Orthod 49(2): 92-97.
- Winders RV (1958) Forces exerted on the dentition by the perioral and lingual musculature during swallowing. Angle Orthod 28(4): 226-235.
- McNamara JA, Brudon WL (1993) Orthodontic and orthopedic treatment in the mixed dentition. In: Spivey KB, Skidmore LM (Eds.), Transpalatal arches. 2nd (edn), Need-ham Press Inc., Ann Arbor, Michigan, pp. 179-192.
- Wise JB, Magness WB, Powers JM (1994) Maxillary molar vertical control with the use of transpalatal arches. Am J Orthod Dento facial Orthop 106(4): 403-408.
- Burstone CJ, Koenig HA (1981) Precision adjustment of the transpalatal lingual arch: computer arch form predetermination. Am J Orthod 79(2): 115-133.
- Cetlin NM, Hoeve AT (1983) Non-extraction treatment. J ClinOrthod 17(6): 396-413.
- Root TL (1981) The level anchorage system for correction of orthodontic malocclusions. Am J Orthod 80(4): 395-410.
- Melsen B, Bonetti G, Giunta D (1994) Statically determinate transpalatal arches. J ClinOrthod 28(10): 602-606.
- Yamawaki H, Kawamoto T (1996) Effect of palatal bar on maxillary molars during swallowing. J Osaka Dent Univ 59(1): 53-63.
- Hata M (1993) Effect on the dentofacial complex of Macacairus of functional tongue forces imparted on a palatal bar-tongue forces imparted on palatal bar. J Osaka Dent Univ 27(1): 51-66.
- Bobak V, Christiansen RL, Hillister SJ, Kohn DH (1997) Stress-related molar responses to the transpalatal arch: a finite element analysis. Am J Orthod Dento facial Orthop 112(5): 512-518.
- Gkantidis N, Halazonetis DJ, Alexandropoulos E, Haralabakis NB (2011) Treatment strategies for patients with hyperdivergent Class II Division 1 malocclusion: is vertical dimension affected? Am J Orthod Dentofacial Orthop 140(3): 346-355.
- Zablocki HL, McNamara JA Jr, Franchi L, Baccetti T (2008) Effect of the transpalatal arch during extraction treatment. Am J OrthodDento-facial Orthop 133(6): 852-860.
- Wise JB, Magness WB, Powers JM (1994) Maxillary molar vertical control with the use of transpalatal arches. Am J OrthodDentofacial Orthop 106(4): 403-408.
- Yao CC, Lee JJ, Chen HY, Chang ZC, Chang HF, et al. (2005) Maxillary molar intrusion with fixed appliances and mini-implant anchorage studied in three dimensions. Angle Orthod 75(5): 754-760.
- Lee J, Miyazawa K, Tabuchi M, Kawaguchi M, Shibata M, et al. (2013) Midpalatalminiscrews and high-pull headgear for anteroposterior and vertical anchorage control: cephalometric comparisons of treatment changes. Am J Ortho Dento facial Orthop 144(2): 238-250.
- Deberardinis M, Stretesky T, Sinha P, Nanda RS (2000) Evaluation of the vertical holding appliance in treatment of high-angle patients. Am J Ortho Dento facial Orthop 117(6): 700-705.
- Dubrul EL Sicher (1988) Dubrul’s oral anatomy. In: Dubrul EL (Ed.), Graphic world. 8th (edn), Ishiyaku Euroamerica, St Louis, Missouri, pp. 161-199.
- Nishimura R (1977) An X-ray cinematographical study on position of the dorsum of the tongue in deglutition. Shikagakuhou 77(4): 263-309.
- Chiba Y, Motoyoshi M, Namura S (2003) Tongue pressure on loop of transpalatal arch during deglutition. Am Jm OrthoDento facial Orthop 123(1): 29-34.
- Kaifan Xu, Jingjing Zeng, Tianmin Xu (2016) Effect of an introral appliance on tongue pressure measured by force exerted during swallowing. Am J Ortho Dento facial Orthop 149(1): 55-61.
- Kincaid RM (1951) The frequency of deglutition in man: its relationship to overbite. Angle Orthod 21: 34-43.






























