Papillary Cyst Adenocarcinoma Arising in a Papillary Cyst Adenoma: A Rare Entity in the Sublingual Gland
Adir Cohen1, Ilana Kaplan2, Gal Frenkel3*, Benjamin Shlomi1 and Vadim Raiser4
1 Department of Oral and Maxillofacial Surgery, Hebrew University, Israel
2Director of the Oral Pathology Service, Sourasky Medical Center and Sackler School of Medicine, Tel-Aviv University, Israel
3Department of Oral and Maxillofacial Surgery, Tel Aviv Sourasky Medical Center, Israel
4Department of Oral and Maxillofacial Surgery, Tel Aviv Sourasky Medical Center, Israel
Submission: September 14, 2016; Published: September 23, 2016
*Corresponding author: Gal Frenkel , Resident, Department of Oral and Maxillofacial Surgery, Aviv Sourasky Medical Center, Weizmann St 6, Aviv-Yafo, Israel, Email: gfrenk@gmail.com
How to cite this article: Adir C, Ilana K, Gal F, Benjamin S, Vadim R. Papillary Cyst Adenocarcinoma Arising in a Papillary Cyst Adenoma: A Rare Entity 004 in the Sublingual Gland. Adv Dent & Oral Health. 2016; 2(3): 555592. DOI: 10.19080/ADOH.2016.02.555592
Abstract
Papillary cyst adenocarcinoma (PCAC) of salivary glands is an extremely rare, low-grade destructive tumor, with a papillary - cystic architecture. PCAC has considerable overlap in microscopic characteristics with the benign variant of papillary cyst adenoma (PCA), where the main difference between the two is the presence of frank invasion into surrounding tissues in PCAC. The present case describes a long -standing lesion multilobulated submucosal mass of 4 cm diameter of the floor of the mouth in a 78 years old female. Histologic analysis reviled infiltrative pattern suggesting malignant pattern. The history of a long duration with a recent increase in size, the encapsulation of most of the tumor periphery and the localized front of invasion, all suggest transformation from PCA to PCAC fiture of PCA.
Conclusion:n:With the results it is concluded that preoperative plasma BNP levels is a reliable indicator for early postoperative morbidity in patients undergoing coronary artery bypass. Keywords:Papillary cystic adenoid carcinoma
Introduction
Papillary cyst adenocarcinoma (PCAC) of salivary glands is an extremely rare, usually low-grade destructive tumor, with a papillary - cystic architecture, first classified as a distinct neoplasm in 1991 by the World Health Organization (WHO) [1] and later by Ellis and auclair [2]. It accounts for less than 0.2% of all salivary gland tumors according to some studies [3,4,5]. Only a single lesion of PCAC of the parotid was described within a series of 834 salivary glands tumors [6]. The sublingual gland is an uncommon location for this lesion [5]. PCAC has considerable overlap in microscopic characteristics with the benign variant of papillary cyst adenoma (PCA), where the main difference between the two is the presence of frank invasion into surrounding tissues in PCAC.
In the following report we present a case diagnosed as papillary cystadenoma of the sublingual gland in an incisional biopsy, which following resection, turned out to have an area of invasion and the final diagnosis was PCAC. The diagnostic challenges in differentiating the benign from the malignant variants are discussed.
Case Report
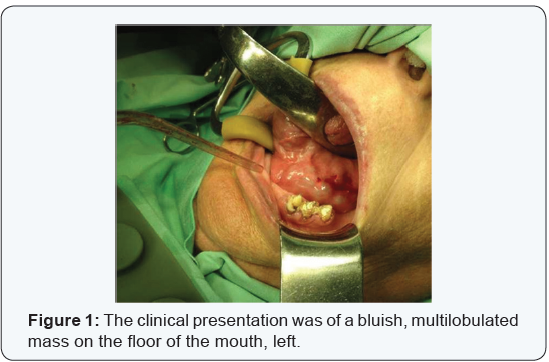
A 78-year-old woman presented with an asymptomatic mass of the floor of the mouth, left side. The patient was aware of lesion in that area which was constant in size for a long duration, and presented some growth 4 month prior to her examination. Clinical examination revealed a multilobulated submucosal mass of 4 cm diameter. It was bluish, firm and the overlying mucosa was intact (Figure 1).
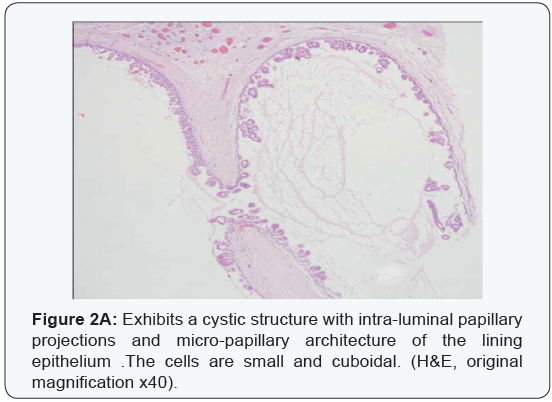
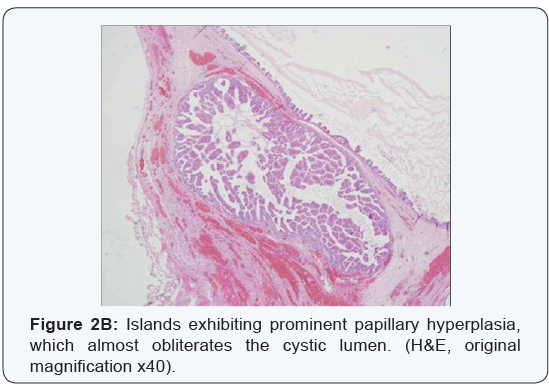
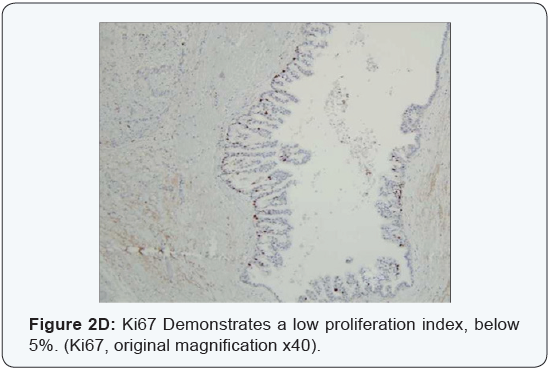
An incisional biopsy was performed, with the provisional diagnoses including pleomorphic adenoma, adenoid cystic carcinoma or mucoepidermoid carcinoma. Microscopic examination exhibited a multicystic architecture, lined by a thin cuboidal epithelium, which proliferated to create small and delicate intra-luminal papillary projections. The cells were uniform, with a bland cytology, without atypia, prominent mitotic activity or necrosis, and thus malignancy was not suspected at this point. The biopsy was signed out as PCA (Figure 2a-2d).
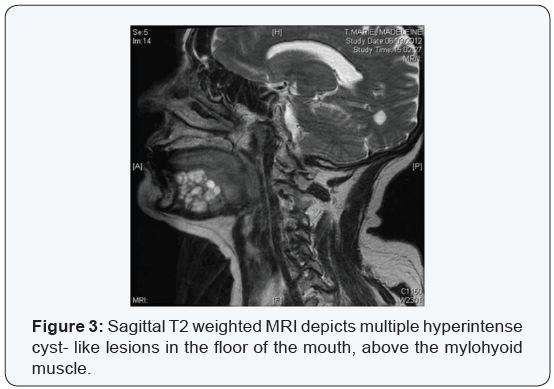
An MRI that was performed in order to define the extent and nature of the lesion. A multicystic mass of 2cm X 3.2 cm X 4.5 cm was identified in the left sublingual space above the mylohyoid muscle. It was well circumscribed, did not involve the mandible and lymph node enlargement was not observed. The left sublingual gland could not be demonstrated in the MRI (Figure 3).
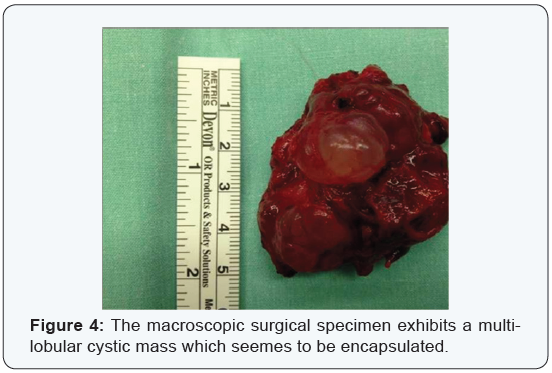
Under general anesthesia, a mucosal incision was preformed above the mass. The lesion seemed to present a distinct capsule, and an extra capsular dissection was carried out, with the mass separating easily of from the surrounding tissues. In the posterior aspect, a firm attachment to the submandibular salivary gland was observed, with no clear demarcation in that area. The surgical specimen seemed macroscopically to be multilobulated, well-circumscribed and encapsulated (Figure 4).
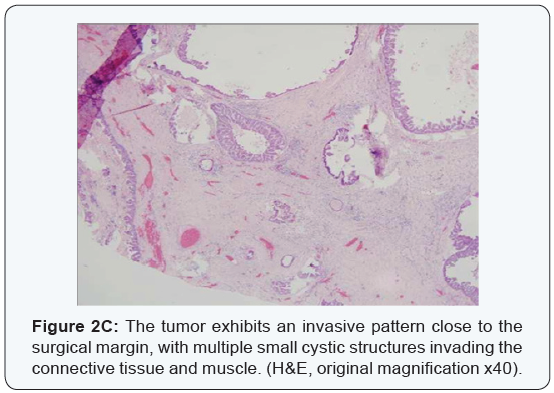
Multiple microscopic sections exhibited essentially the same features described in the initial biopsy, with multiple cystic structures, lined by thin bland cuboidal epithelium with intra-luminal papillary projections. However, while examining the margins it became evident that at least in one area (which corresponded with the posterior aspect), the tumor had an invasive pattern rather than a capsule, with multiple small tumoral cysts and islands invading into the muscle. With this finding the diagnosis was reversed from benign to malignant, and signed-out as PCAC.
Discussion
Cystadenoma is characterized by epithelium-lined cystic masses that contain secretion material, usually serous or mucinous. When the tumor presents both papillary and cystic features it is classified as PCA.
This tumor type is found in the ovaries, pancreas and salivary glands. In the salivary glands it is most frequent in the parotid, with decreasing incidence in submandibular, minor salivary glands and the sublingual gland [7].
The World Health Organization (WHO) described PCA of the salivary glands as a tumor that closely resembles Warthin tumor but without the lymphoid elements, constituting multiple papillary projections arising from undifferentiated epithelium of the intercalated ducts of the glands [1,8].
In this variant the epithelial cells are typically tall and present abundant eosinophilic cytoplasm, similar to Warthin’s tumor. However, some cases present the same cystic papillary architecture, but the cells tend to be small and cuboidal.
Salivary gland PCAC is an extremely rare malignant neoplasm, with a peak of incidence in the 7th - 8th decades. A single case of PCAC was described in a child [9]. The sublingual gland is an uncommon location for this lesion. Foss et al. [6] described only 2 PCAC in the sublingual glands in a series of 57 PCAC cases.
Due to similar architecture and cytology, it may be difficult to distinguish the benign variant (PCA) form PCAC, especially in a biopsy specimen [10]. Both lesions lack overt atypia, necrosis or prominent mitotic figures. In fact, the only definitive feature separating PCA from PCAC is the presence of frank invasion in PCAC, as opposed to complete encapsulation and absence of invasion in PCA.
In the present case, the majority of the surgical specimen was encapsulated clinically, with only one area in which the tumor seemed to be inseparable from the surrounding tissues during surgery. This area corresponded with the microscopic finding of invasion into the peri-tumoral tissue. This fact, coupled with the information the patient was aware of a mass which was constant in size in that area for a long duration, and presented some growth
only 4 months prior to her examination, raises the possibility of malignant transformation to PCAC in a long-standing benign PCA. Similar processes are well recognized in other salivary gland tumors, such as transformation to carcinoma- in- situ in long standing pleomorphic adenoma, however, it has not been described in these rare pair of PCA and PCAC [11].
Hence, once an incisional biopsy of PCA is signed out, especially in long standing large lesions, the surgeon performing the definite treatment and the pathologist should both keep in mind there is a possibility of the lesion exhibiting invasive features in the final surgical specimen, which would than require re-classification from benign (PCA) to malignant (PCAC). Highgrade variants may present cervical lymph node metastases [6,12]. However, occasional cases of low grade PCAC with cervical lymph nodes metastases have also been reported [13]. Local recurrences can occur at an average of 76 months after initial treatment [6]. The treatment of PCA is surgical excision. In most reported cases of PCAC an additional broader excision or postoperative radiotherapy have been suggested and annual revisions for a minimum period of five years [4,5,13,14].
References
- Seifert G, Sobin LH (1992) The World Health Organization’s Histological Classification of Salivary Gland Tumors. A commentary on the second edition. Cancer 70(2): 379-385.
- Ellis GL, Auclair PL (1996) Tumours of the salivary glands. Atlas of Tumour Pathology, 3rd Series. Washington: Armed Forces Institute of Pathology. p. 29.
- Tomioka H, Harada H, Okada N, (2006) Papillary cystadenocarcinoma arising in the floor of the mouth: report of a case. Oral Maxillofac Surg 64(5): 864-867.
- Yamada S, Matsuo T, Baba N, Rokutanda S, Kawasaki G, et al. (2007) High-grade papillary cystadenocarcinoma of the sublingual gland: a case report. J Oral Maxillofac Surg 65(6): 1223-1227.
- Gallego L, Junquera L, Fresno MF, de Vicente JC (2008) Papillary cystadenoma and cystadenocarcinoma of salivary glands: two unusual entities. Med Oral Patol Oral Cir Bucal 13(7): E460-E463.
- Foss RD, Ellis GL, Auclair PL (1996) Salivary gland cystadenocarcinomas. A clinicopathologic study of 57 cases. Am J Surg Pathol 20(12): 1440- 1447.
- Nakagawa T1, Hattori K, Iwata N, Tsujimura T (2002) Papillary cystadenocarcinoma arising from minor salivary glands in the anterior portion of the tongue: A case report. Auris Nasus Larynx 29(1):87-90.
- Alexis JB, Dembrow V (1995) Papillary cystadenoma of a minor salivary gland. J Oral Maxillofac Surg 53(1): 70-72.
- Crocker TP, Kreutner A Jr, Othersen HB Jr, Garvin AJ (1995) Papillary adenocarcinoma of minor salivary gland origin in a child. Arch Otolaryngol 109(12): 827-831.
- Mardi K, Sharma S, Gupta N (2010) Papillary cystadenocarcinoma of submandibular salivary gland: a rare case report. J Cancer Res Ther 6(3): 330-332.
- Maruyama S, Cheng J, Shingaki S, Tamura T, Asakawa S, et al. (2009) Establishment and characterization of pleomorphic adenoma cell systems: an in-vitro demonstration of carcinomas arising secondarily from adenomas in the salivary gland. BMC Cancer 9: 247.
- Koç M, Yanilmaz M, Yildirim H, Gök U, Cobanoğlu B (2010) MRI findings of papillary cystadenocarcinoma of the submandibular gland. Diagn Interv Radiol 16(1): 20-23.
- Shteyer A, Fundoianu-Dayan D (1986) Papillary cystic adenocarcinoma of minor salivary glands. Int J Oral Maxillofac Surg 15(3): 361-364.
- Mardi K, Sharma S, Gupta N (2010) Papillary cystadenocarcinoma of submandibular salivary gland: a rare case report. J Cancer Res Ther 6(3): 330-332.






























