Biomechanics Before and After Hip Replacement
Tim Maggs1* and Alexandros Siozos2
1DC, Director, Maggs Sports Chiropractic Biomechanics and Wellness Center Director, Sports Injuries and Biomechanics, USA
2MD, Consultant in Orthopaedic Surgery, Private Practice, Greece
Submission: October 21, 2022; Published: November 04, 2022
*Corresponding author: Tim Maggs, DC, Director, Maggs Sports Chiropractic Biomechanics and Wellness Center Director, Sports Injuries and Biomechanics, USA
How to cite this article: Tim M, Alexandros S. Biomechanics Before and After Hip Replacement. Ortho & Rheum Open Access J. 2022; 20(4): 556044. DOI: 10.19080/OROAJ.2022.20.556044
Mini Review
Hip replacement surgeries take place so often that they occur in every city every day in the US. According to the Rheumatology advisor article, researchers project that the total annual counts of total hip arthroplasty could increase by 34% in 2020 to 498,000 replacements, by 75% in 2025 to 652,000 replacements, by 129% in 2030 to 850,000 replacements, and by 284% in 2040 to 1,429,000 replacements [1]. Most people see this surgery as inevitable, an end stage treatment. What we fail to ask is, why did one hip falter while the other did not. This question may help researchers gain information towards the prevention of hip degeneration rather than its replacement.
Hip degeneration is determined by many factors, including genetics, biomechanics, trauma, repetitive activities, body weight, conditioning and more. For this paper, we want to look at the biomechanics to explore the possibilities of delaying degeneration and reducing the need for hip replacement. Every human being has structural imbalances [2], such as leg length differences, foot pronation differences, etc. These are the precursors to joint overload, whether it be the knee, hip, or lumbar spine. Increased loading of any muscle, tendon, ligament, or joint will predispose that tissue to advanced and accelerated degeneration [3].
Musculoskeletal healthcare in the U.S. is mostly reactive. There are no standardized examinations for the masses that look at factors such as pronation of the feet, increased Q angles of the knees, leg length, femoral head height or overall alignment and balance. The system in the US addresses musculoskeletal issues only after a patient is injured, in pain or disabled and health insurers support this reactive approach as coverage occurs only after a patient suffers with pain. To make matters worse, any type of maintenance care or maintenance treatment is not only frowned upon but discouraged by insurance companies. Tests such as MRI’s can be extremely difficult to gain insurance approval unless the patient qualifies with extreme medical findings. It can be difficult upon routine physical examination to determine if there are findings such as disc bulge or herniation unless the patient is also suffering with foot drop, incontinence or any other extreme findings. Fortunately, much like a colonoscopy, MRI’s can detect musculoskeletal breakdown and degeneration sooner and corrective treatments can be recommended prior to the need for fusion or discectomy. Ignoring these early findings is part of the reason patients in the U.S. have had to rely upon opioid treatments for severe pain relief.
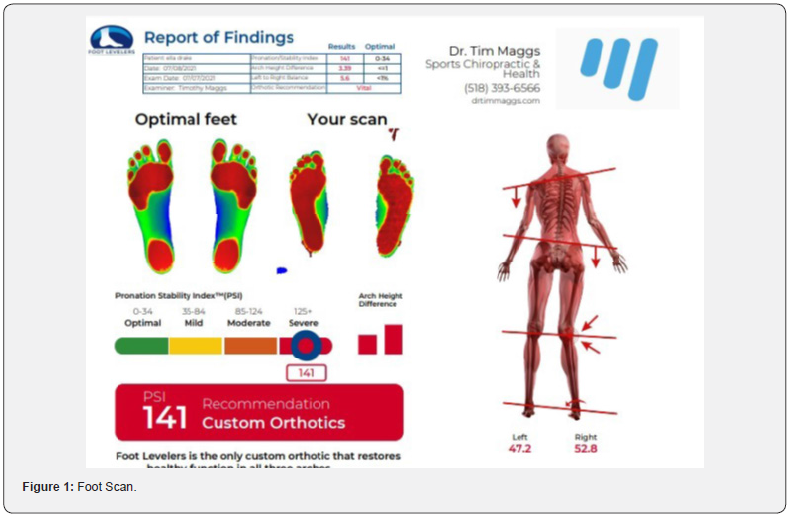
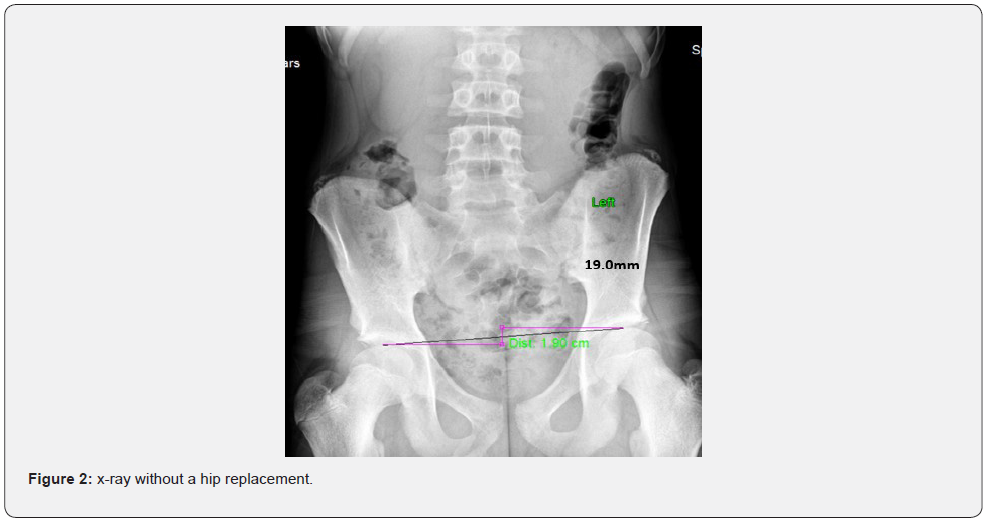
Testing that can be performed that may identify hip overload could begin with digital laser foot scans. This test identifies the amount of space under each foot in the standing position to determine if there is collapse of one or more arches of each foot as well as determining the symmetry of collapse (Figure 1). Symmetry, or asymmetry, of the feet could alert an examiner of biomechanical imbalances that may exist. A study of four hundred patients showed that 99.5% had moderate to severe pronation [4]. Further testing would include an A-P lumbosacral digital x-ray to determine femoral head height with the patient barefoot and in the standing position (Figure 2). Studies have shown that while barefoot, 64% of patients had femoral head height difference (fhhd) of >3mm. 42% of patients had fhhd >5mm [5].
Fhhd is the result of two anatomical findings: the unilateral or bilateral collapse of the feet and leg length. When the collapse and asymmetries of the feet are addressed by putting the patient into custom orthotics, a 2nd A-P L-S x-ray would suggest only a leg length difference if fhhd occurs. The same study showed that 61% of patients wearing custom orthotics had >3mm in fhhd while 40% had >5mm in fhhd. This suggests that custom orthotics provides beneficial contributions at improving overall loading of the body but does truly little at changing fhhd.
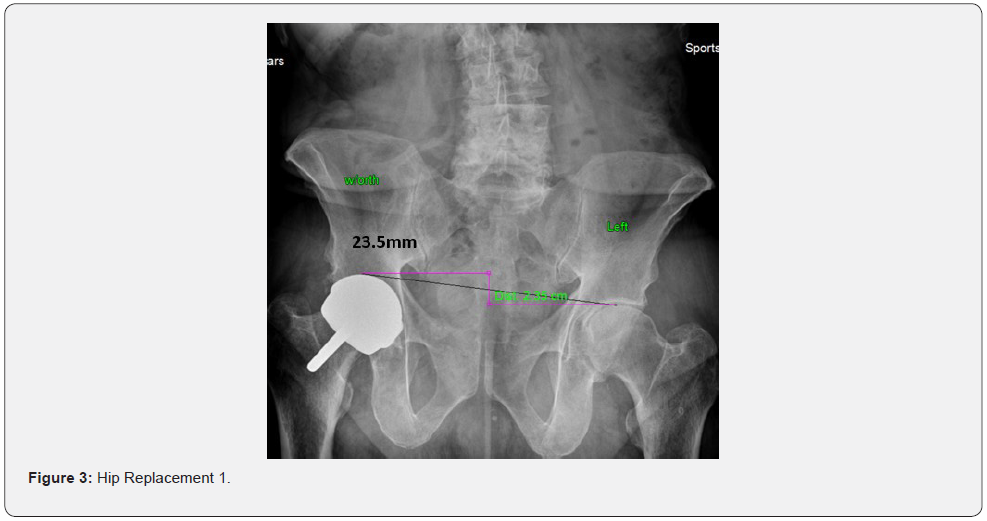
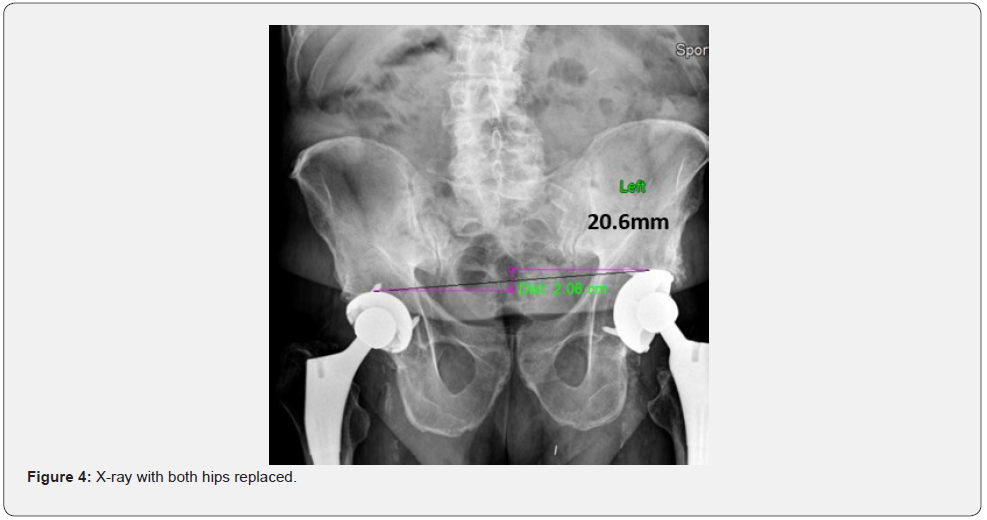
More alarming findings on this study showed that correction of the feet with custom orthotics showed an increase (rather than decrease) in fhhd on the second x-ray 22% of the time. This might suggest that x-ray inclusion, as well as digital foot scans, should be routine on all physical examinations. When a patient is a candidate to undergo a hip replacement surgery almost no surgeon searches for leg length discrepancies either pre- or postoperatively. A-P L-S x-rays taken on patients who have had one or both hips replaced show significant differences in femoral head height (Figures 3 & 4).
Future Studies
Once a patient has been examined and a fhhd >3mm has been determined, an appropriate sized lift is placed underneath the heel of the orthotic on the low fh side. No studies yet have been done to determine if this simple procedure is the best, or even if it is correct. The appropriate response may be more complicated and further testing may need to be done. The goal is for all patients to support their feet with an orthotic device to create symmetry in the arches, to prevent further collapse, and to obtain the most levelling of the femoral heads possible. Lift therapy is recommended up to 7mm and adding to the entire sole of the shoe is recommended if the lift needs to be greater than 7mm.
References
- Jasvinder A Singh, Shaohua Yu, Lang Chen, John D Cleveland (2019) Rates of Total Joint Replacement in the United States: Future Projections to 2020–2040 Using the National Inpatient Sample. J Rheumatol 46(9): 1134-1140.
- Tim Maggs D, Steven B M, Alexandros S M (2020) When Correcting the Collapse of Arches of the Feet with Custom Orthotics, are Other Areas of the Body Effected? A Revolutionary Approach towards Reduced Injuries and Better Outcomes by Ortho & Rheum Open Access J 17(1): 555953.
- Lorena Canosa-Carro, Maria Bravo-Aguilar, Vanesa Abuíin-Porras, Jaime Almazan-Polo, Guillermo García-Pérez-de-Sevilla, et al. (2022) Current understanding of the diagnosis and management of the tendinopathy: An update from the lab to the clinical practice. Disease-a-Month 68(10): 101314.
- Tim Maggs D, Steven B M, Alexandros S M (2021) Are the biomechanics of the feet considered enough in their contributory relationship to leg length and femoral head height difference? Advanced technology provides new information by. Ortho & Rheum Open Access J 17(5): 555974.
- Tim Maggs, Steven B, Alexandros S (2021) Is Prescribing Custom Orthotics Enough to Prevent and Treat Musculoskeletal Injuries and Degeneration? What if we Integrated Biomechanical X-ray Measurements with the Laser Foot Scan Procedure? Could this Reduce Injuries Even More? Ortho & Rheum Open Access J 17(4): 555970.






























