Arthroscopic Labral Stabilization with Capsular Mattress Reinforcement Using Suture Anchors
*Tsiouri Chrysi, Mok Daniel H and Chidambaram Ramiah
Aristotle University of Thessaloniki, Greece
Submission: August 28, 2017; Published: September 07, 2017
*Correspondence author: Chrysi Tsiouri, Mitropoleos 63, Aristotle University of Thessaloniki, Greece, Tel:306948056477; Email: xpysat@yahoo.co.uk
How to cite this article: Tsiouri C, Mok Daniel H, Chidambaram R. Arthroscopic Labral Stabilization with Capsular Mattress Reinforcement Using Suture Anchors. Ortho & Rheum Open Access 2017; 8(3): 555738. DOI: 10.19080/OROAJ.2017.08.555738
Introduction
Arthroscopic management of labral pathology has evolved in recent years with advancement in surgical techniques, aided by new instrumentation and implants designed to simplify the repair [1-5]. Results of arthroscopic stabilizations have been recently reported as equal or superior to open stabilizations with high rates of success, patient satisfaction and early return to activity [6-9]. The purpose of this study was to evaluate the early clinical results of labral stabilization with capsular mattress reinforcement using suture anchors that has not been previously described.
Materials and Methods
A retrospective study was performed on sixty-five consecutive shoulders on 62 patients who underwent arthroscopic labral stabilization with capsular mattress reinforcement by the senior author between August 2005 and August 2008. Indications included instability and persistent pain. Age, contact sports, bilateral instability, bony lesions or recurrent dislocations were not exclusion criteria. All patients were followed up. There were 50 male and 12 female patients with mean age of 38 years (1466). The dominant shoulder was involved in 30(48%) cases and the non-dominant in 35 (52%).
Thirty-eight shoulders (58.5%) had dislocated at least once and required reduction. Of those shoulders 17 (26%) had recurrent episodes and six patients (12.3%) had bilateral instability. In 27(41, 5%) shoulders there was persistent pain either gradual (13 cases, 48%) or after an injury in 14 (52%) cases, in five patients with apprehension. Of non-dislocators, two had bilateral symptoms. Four of those patients reported subluxations, two without any injury. Two patients had a glenoid fracture treated conservatively and one had an ORIF for a clavicular fracture. One patient had stabilization of the same shoulder in the past but his symptoms recurred after a fall. Fourteen patients were occupied with heavy manual work, two of them having injured their shoulder at work. There werefour cases that were involved in a RTA, one of those carrying claims. Fifty-six patients are involved in sports, four of them professionally. The patients ‘demographics are summarized in Table 1.
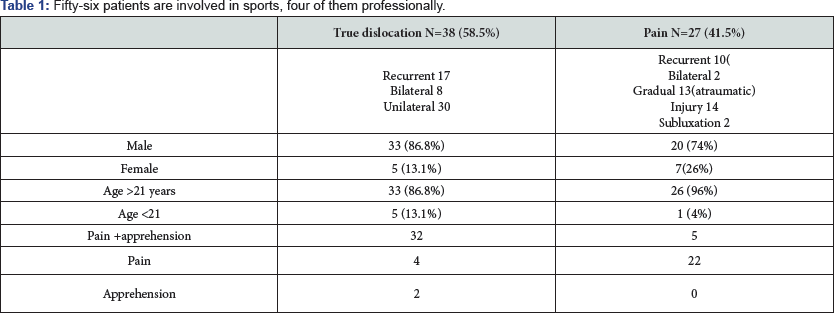
The mean interval between either trauma or initiation of symptoms and surgical procedure was 22 months (0- 132 months). Sixty-three shoulders were painful and thirty-nine were apprehensive. Additional investigations were performed in 26 patients and consisted of 25 MRI scans that showed the labral tears and one CT scan that revealed severe (>30%) Hill Sachs lesion. All sixty-two patients were postoperatively evaluated by telephone interview using the Rowe Score and the Oxford Score for Instability. Statistical analysis was performed using the SPSS 16.0 package for Windows. Statistical significance was set at p<0.05.
Surgical Technique
Under general anaesthetic, the shoulder was assessed for its direction of instability. Arthroscopy was performed with the patient in the lateral decubitus position. The standard posterior viewing portal was used. With the help of a spinal needle, the anterior portal was established in the rotator interval with the cannula inserted above the subscapularis tendon. Further portals were established pending on labral pathology. The superior portal often entered the joint above the long head of biceps tendon (LHB). In this position, the scope or instrument could then work either anterior or posterior to the LHB insertion. In cases with posterior labral tear, posterolateral working portals would then be established along the posterolateral corner of the acromion.

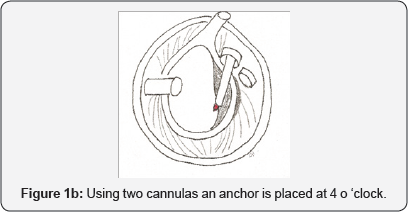
The integrity and quality of the torn labrum detachment was carefully assessed using a probe. Particular attention was paid to possible tears in the adjacent capsule, including its attachment to the humeral head. Using a rasp, any remaining soft tissue in the area of the torn labrum was released from the glenoid neck. Bioabsorbable 3.5mm anchor (Lactoscrew, Biomet) was then inserted at an inclination of 45° into the glenoid surface edge (Figures 1a & 1b).


Introduced through the anterior portal, a 60° IDEAL Suture Grasper (DePuy, Mitek) (Figure 2a) or a 45° or 60° shuttle relay suture passer (Spectrum, Linvatec) was used to pick up capsule adjacent to the labral tear (Figure 2b). Whilst carrying the capsule, the needle of either the Mitek Grasper (Figure 3a) or the Spectrum shuttle relay was re-introduced to pick up the torn labrum on the neck of the glenoid with its point exiting at the edge of the articular surface. In this way, both the capsule and the torn labrum were gathered together. Through the shuttle relay, a #1 PDS (Ethicon) suture was introduced into the joint (Figure 3b). The intra-articular end of this PDS suture was then tied to one of the strands of suture from the anchor (Figure 3c). Removing the shuttle relay and the PDS suture would ensure the suture from the anchor be passed through the damaged labrum and the capsule (Figures 3d & 3e). In a similar manner, the second strand of the suture was retrieved with PDS carrying adjacent part of the capsule and labrum (Figure 3f), thus affecting a mattress repair with reinforcement from the plicated (Figure 4) capsule. Further anchors and mattress repair were added as necessary (Figure 5).





Postoperative Care
The operated arm was immobilized in a sling for up to six weeks (mean 4.5 weeks) that is not removed but for cleansing and exercise that includes active elbow flexion extension pronation supination and passive external rotation (pendulum) exercises of the shoulder. When the sling is removed strengthening and range of movement rehabilitation is commenced. Gradually more muscle groups are added in the program and activities are allowed. Return to contact sports is not recommended until 12 months postoperatively.
Results
Diagnostic arthroscopy revealed Hill Sachs lesions in 18 shoulders (27.6%).Seven (10.7%) were significant (>25%). Glenoid bone defects (Bony Bankart) >25% (18) were found in three shoulders (5%). The labrum was completely absent in parts of the glenoid in 6 shoulders (9%) and there were three (5%) panlabral tears. One patient with a panlabral tear and a 40% Hill Sachs lesion required additional remplissage. In ten shoulders the capsule was lax and in three shoulders it was torn. The mean number of anchors used was 2 (range one to four) aiming at good stability and centralization of the humeral head.
The mean follow up was 32 weeks, (14-49). All patients returned to work after a mean of 6 weeks (0-52) except from two who were preoperatively unemployed for reasons other than their shoulder pathology and a professional rugby player. Manual workers returned to work in a mean of 14 weeks. The mean return to sports as recreational activity was 23 weeks (172) and 16 weeks for those professionally involved in athletics. The mean Rowe score was 91.7 ranging from 30 to 100. According to Rowe score [10], 51 shoulders had excellent results, 9 were graded as good, four as fair and there was one poor outcome. According to the Oxford score [11] (mean 41, range 16 to 44) there were 48 excellent results, ten good, six fair and one poor.
Our poor result is of a patient who was involved in a RTA three years before she underwent arthroscopic stabilization of her anterior 1 to 6.30 labral tear with three anchors. She complains of persistent pain and disability. She has never been back to work as a housewife after the accident when she also suffered eye and neck injuries. Her claim case is currently running.
Fifty-nine (95%) patients are pleased with the results of the operation and would have the other side operated if needed. Two patients are satisfied with the result but unwilling to go through the procedure again and the previously mentioned patient is not pleased. Another patient is not pleased either having however a Rowe score of 80 and an Oxford score of 35. He is unemployed by choice. Two patients complain of reduced extension-external rotation and two of restricted abduction-external rotation but they are all pleased with the outcome.
Regarding our patient factors and the arthroscopic findings, it is interesting that there is significant correlation between recurrent dislocators and, Hill Sachs lesions (Pearson's coef.0.258, p=0.038), partially absent labrum (Pearson's coef 0.306, p=0.016), as one would expect, but not with Panlabral tears or Bony Bankart lesions. There was no statistical difference in the mean Rowe score, Oxford score, return to work or sports between sex, age (when patients grouped as less or more than 21 years old), delay between injury or initial symptoms and surgery. There was no statistical difference in the results when the patient had bilateral shoulder problems, multidirectional instability, or recurrent instability. There was also no difference between those who suffered true dislocation and those whose complaint was pain whether after an injury or gradual. Hill Sachs and Bankart lesions and loss of labral tissue neither influenced the results. The number of anchors used had no effect either but there is a significant correlation between number of anchors used and preoperative recurrent dislocation (Pearson's coef. =0.320, p=0.011) There were three failures (4.5%) were the shoulder redislocated.
Discussion
Arthroscopic capsular plication as means of treating shoulder instability was originally described in 1997 [12]. Since then multiple techniques has been developed [13-15] with satisfactory results reported. Most methods use simple suture technique with the exception of a purse-string method were the knot is tied in a mattress fashion [16-20] and a mattress plication of the inferior capsule that incorporates the IGHL but does not involve the labrum [21]. Results of mattress capsulolabral plication with the use of suture anchors for traumatic instability have not been reported. In most published studies, patients with a history of recurrent dislocations, young patients and those involved in contact sports are excluded [22,23]. Capsular laxity, Bony Bankart >25%, large Hill Sachs lesion are associated with high rates of failure [6,17,21] of up to 75% when anterior hyper laxity or a glenoid compression fracture involving >25% of the glenoid surface were present [18] and are considered contraindications to arthroscopic stabilization by most authors [18,22,23].
A technique of mattress inferior capsular plication with metallic anchors has published midterm results with a 6% failure rate [23] excluding high risk patients. We used Bioabsorbable anchors that have in our opinion many advantages [24-28]. Our study included all patients regardless ofthe previously mentioned demographics or arthroscopic findings. We used our portals as viewing or interventional according to the site of the pathology addressed starting with a standard posterior viewing portal and a sub-bicipital and viewing through those the periphery of the glenoid. With the aid of a spinal needle a third portal will usually be established posterior to the long head of biceps or posteriorly aiming at posterior/inferior labrum. It enables placing an anchor at 6 o 'clock and using one limb to grasp the capsule and labrum at 6.30-7 o 'clock using the posterior portal and viewing from the superior portal posterior to the long head of biceps and the other limb at 5-5.30 o 'clock using our sub-bicipital portal and viewing from the superior portal. When the knot is tied, it lifts the humeral head up. Our technique involves using a 45° or 60° shuttle relay suture passer according to the site of the defect to first pick up the capsule, exit, and then pick up the labrum and exit again thus creating a bumper's effect and a strong capsulelabrum construct and not only the capsule.
This way we are able to balance capsular laxity-labral deficiency or pathology effectively. We do not routinely close the rotator interval since we have found that this may cause extensive loss of external rotation. A 95.5% success rate was noted with forty-seven (88.5%) of shoulders having a good or excellent Oxford score and sixty shoulders (92% ) having a good or excellent Rowe score at final follow up which compares to published results after open procedures [6-9] Opposite to other studies [8,17,21] we found no difference in the scores or patient's return to work or sport with the number of fixation points, possibly because we addressed each shoulder's defect accordingly and due to the variety of our findings. The benefit of the mattress suture technique is that we can address two areas of the capsule from one anchor which will give a wider bumper effect than simple suture technique. Also in the simple suture, the tied suture can cut a poor quality damaged labrum. In the mattress technique, the suture through the capsule will not cut through the labrum. This technique is one of the few published that can address anteroinferior capsular laxity effectively [24-26].
Our three failures occurred after 24 months. The first patient is a 34 year old builder who had recurrent episodes of traumatic (football tackles) dislocations in both his shoulder. His non dominant shoulder redislocated 39 months after arthroscopic stabilization with our technique again after a football tackle. Our findings included a small Hill Sachs lesion (15%) and a torn anterior capsule. Three anchors were used and on last follow up before failure he had an Oxford score of 36 and a Rowe score of 80>His dominant shoulder is stable 53 months after stabilization. The second patient was 14 years old at the time he had his arthroscopic stabilization and now works as a truck loader [27]. He had a history of bilateral recurrent shoulder dislocations. On arthroscopy a large Bankart lesion was found. The stabilization failed after 24 months after trauma and an open later jet procedure was performed that provided stability and pain relief for two years but also failed recently [28]. The third patient is a 28 year old accountant who had a single traumatic episode of anterior dislocation. During arthroscopy an extensive labral tear from 11 posteriorly clockwise to 7 was found and 3 anchors were needed to centralize the humeral head. On his last 24 months follow up he had an Oxford score of 41 and a Rowe score of 100. He was not willing to provide us with any details regarding the redislocation and he has been revised elsewhere.
Conclusion
Capsular-labral plication with the use of suture anchors recreates the labral bumper and tensions the capsule thus restoring shoulder stability. There is no knot in the joint surface allowing for better establishment of the humeral head in the labrum. Our results are intermediate and may deteriorate with time therefore further review has to follow. However, the high success rate shows that it is a reliable technique.
References
- Freeman BL (1992) Recurrent dislocations, in Crenshaw AH (8th edn), Campbell's Operative Orthopaedics St Louis, Mosby Year Book, USA, pp. 1391-1461.
- Abrams JS, Savoie FH, Tauro JC, Bradley JP (2002) Recent advances in the evaluation and treatment of shoulder instability: Anterior, posterior, and multidirectional. Arthroscopy 18: 1-13.
- Stein DA, Jazrawi L, Bartolozzi AR (2002) Arthroscopic stabilization of anterior shoulder instability: A review of the literature. Arthroscopy 18(8): 912-924.
- Kim SH, Ha KI, Park JH, Kim YM, Lee YS, et al. (2003) Arthroscopic posterior labral repair and capsular shift for traumatic unidirectional recurrent posterior subluxation of the shoulder. J Bone Joint Surg Am 85(8): 1479-1487.
- Gartsman GM, Roddey TS, Hammerman SM (2001) Arthroscopic treatment of bi-directional glenohumeral instability: Two- to five-year follow-up. J Shoulder Elbow Surg 10(1): 28-36.
- Cole BJ, L 'Insalata J, Irrgang J, Warner JJ (2000) Comparison of Arthroscopic and Open Anterior Shoulder Stabilization two to six year follow up study. J Bone Joint Surg Am 82(8): 1108-1114.
- Hobby J, Griffin D, Dunbar M, Boileau P (2007) Is arthroscopic surgery for stabilizationof chronic shoulder instability as effective as open surgery? A systematic review and Meta-analysis of 62 studies including 3044 arthroscopic operations. J Bone Joint Surg Br 89(9): 1188-1196.
- Kim SH, Ha KI (2002) Bankart repair in traumatic anterior shoulder instability: Open versus arthroscopic technique. Arthroscopy 18(7): 755-763.
- Fabbriciani C, Milano G, Demontis A, Fadda S, Ziranu F, et al. (2004) Arthroscopic versus open treatment of Bankart lesion of the shoulder: A prospective randomized study. Arthroscopy 20(5): 456-462.
- Rowe CR, Patel D, Southmayd WW (1978) The Bankart procedure: a long-term end-result study. J Bone Joint Surg Am 60(1): 1-16.
- Dawson J, Fitzpatrick R, Carr A (1999) The assessment of shoulder instability The development and validation of a questionnaire. J Bone Joint Surg Br 81(3): 420-426.
- Wichman MT, Snyder SJ (1997) Arthroscopic capsular plication for multidirectional instability of the shoulder. Operative Techniques in Sports Medicine 5(4): 238-243.
- Snyder SJ, Schablin ML (2004) Arthroscopic Capsular Plication Techniques. Techniques in Shoulder and Elbow Surgery 5(4): 193-199.
- Wiley WB, Goradia VK, Pearson SE (2005) Arthroscopic Capsular Plication-Shift. Arthroscopy: The Journal of Arthroscopic and Related Surgery 21(1): 119-121.
- Sekiya JK (2005) Arthroscopic Labral Repair and Capsular Shift of the Glenohumeral Joint: Technical Pearls for a Multiple Pleated Plication Through a Single Working Portal. Arthroscopy 21(6): 766.
- Levy O, Matthews T, Even T (2007) The-Purse-String Technique: An Arthroscopic Technique for Stabilization of Anteroinferior Instability of the Shoulder with Early and Medium-Term Results. Arthroscopy 23(1): 57-64.
- Barber FA, Snyder SJ, Abrams JS, Famnelli GC, Savoie FH (2003) Arthroscopic Bankart reconstruction with a Bioabsorbable anchor. J Shoulder Elbow Surg 12(6): 535-538.
- Boileau P, Vilalba M, Hery JY, Balg F, Aherns P, et al. (2006) Risk Factors for Recurrence of Shoulder Instability After Arthroscopic Bankart Repair. J Bone Joint Surg Am 88(8): 1755-1763.
- Koss S, Richmond JC, Woodward JS (1997) Two- to five-year follow- up of arthroscopic Bankart reconstruction using a suture anchor technique. Am J Sports Med 25(6): 809-812.
- Fleiss DJ (1996) Arthroscopic anterior labral reconstruction using a transglenoid suture technique. Results in active-duty military patients. Am J Sports Med 24(6): 866-867.
- Speer KP, Warren RF, Pagnani M, Warner JJ (1996) An arthroscopic technique for anterior stabilization of the shoulder with a Bioabsorbable tack. J Bone Joint Surg Am 78(12): 1801-1807.
- Stein DA, Jazrawi L, Bartolozzi (2002) AR Arthroscopic stabilization of anterior shoulder instability: A review of the literature. Arthroscopy 18(8): 912-924.
- John M, Nebelung W, Ropke M, Ender SA, Urbach D (2007) Arthroscopic labrum reconstruction with capsular shift in anterior shoulder instability: improved midterm results by using a standardized suprabicipital camera position. Arthroscopy 23(7): 688-695.
- Boileau P, Ahrens P (2003) The TOTS (temporary outside traction suture): a new technique to allow easy suture placement and improve capsular shift in arthroscopic bankart repair. Arthroscopy 19(6): 672677.
- Tauro JC (2000) Arthroscopic inferior capsular split and advancement for anterior and inferior shoulder instability: technique and results at 2- to 5-year follow-up. Arthroscopy 16(5): 451-456.
- Nebelung W, Ropke M, Urbach D, Becker R (2001) A new technique of arthroscopic capsular shift in anterior shoulder instability. Arthroscopy 17(4): 426-429.
- Barber FA, Herbert MA, Coons DA, Boothby MH (2006) Sutures and suture Anchors-Update 2006. Arthroscopy 22(10): 1063-1069.
- Ozbaydar M, Elhassan B, Warner JJ (2007) The Use of Anchors in Shoulder Surgery: A Shift From Metallic to Bioabsorbable Anchors. Arthroscopy 23(10): 1124-1126.






























