Management of Osteoporotic Vertebral Compression Fractures with Stentoplasty
Abdulrazzaq AlObaid*, Islam Elsayed and Abdulaziz Al-Mutair
Orthopaedic Spine Surgeon, Alrazi Hospital, Kuwait
Submission: April 10, 2017; Published: April 17, 2017
*Corresponding author: Abdulrazzaq Alobaid, Orthopaedic Spine Surgeon, Chief of Spine Surgery Unit, Alrazi Hospital, P.O. Box 1160, Surra- 45172, Kuwait, Tel: (+965) 60606216; Email: dralobaid@hotmail.com; dralobaid@hotmail.com; a_almutair@hotmail.com;
How to cite this article: Abdulrazzaq A, Islam E, Abdulaziz A-M. Management of Osteoporotic Vertebral Compression Fractures with Stentoplasty. Ortho & Rheum Open Access 2017; 6(2): 555684. DOI: 10.19080/OROAJ.2017.06.555684
Abstract
Study Design: A prospective study of clinical and radiographic results after vertebral body stenting (VBS) for treatment of osteoporotic vertebral compression fractures (VCFs).
Objectives: To evaluate the effectiveness of stentoplasty as a new technique to treat symptomatic VCFs.
Background Data: Conventional balloon kyphoplasty is a procedure meant to treat osteoporotic and/or cancer related VCFs. However, there is an inherent technical problem with the amount of reduction. When filling the balloons, an acceptable reduction is achieved. However, the resulting final reduction after cementing is approximately 25% lower due to partial collapse after balloon deflation. To address this issue, a newer technique—based on the principles of balloon kyphoplasty and vascular stenting—has been introduced.
Methods: A total of 52 patients with 73 symptomatic VCFs were enrolled in our study of VBS. Clinical outcomes were measured pre- and postoperatively using the visual analogue scale (VAS), Oswestry Disability Index (ODI), and ambulatory status (AS). All outcomes were assessed before the procedure and at 1, 12, 24, and 36 weeks postoperatively.
Results: The median VAS scores went from 10.0 preoperatively to 1.0 at last follow-up. The preoperative ODI score was 80 preoperatively, but improved to 18 at last follow-up. The ability to move independently and ease of ambulation significantly improved after the procedure (P ≤ 0.001). The median kyphosis angle was 15.0 degrees preoperatively and decreased by a median of 4.5 degrees postoperatively.
Conclusion: Patients with symptomatic VCFs had significant improvements in back pain, function, and quality of life following VBS.
Keywords: Vertebral Body Stenting; Balloon kyphoplasty; Vertebral compression Fracture; Loss of Reduction; Back pain
Introduction
Vertebral compression fractures are frequent, and constitute a common and often debilitating feature of osteoporosis. The incidence of vertebral compression fractures rises with age [1,2]. Due to the increasing elderly population, the treatment of vertebral compression fractures is becoming more and more important. [3-7]. The objective in treating VCFs is the relief of pain and the restoration of spinal function utilizing a minimally invasive therapy. The ideal treatment should result in an immediate relief of fracture-related pain, a satisfying restoration of vertebral body height, and the correction of angular deformity [8-10]. Both vertebroplasty and kyphoplasty lead to immediate pain relief because the broken vertebra is stabilized and further deformity is prevented [9,11,12]. Characteristic complications, such as cement extrusion and pulmonary embolism, are less likely to occur in kyphoplasty due to lower pressure when injecting the cement [13]. In addition, a restoration of height and correction of kyphosis is achieved by filling the kyphoplasty balloons. There are reports of relative restoration of vertebral body height between 0 and 90% and correction in kyphotic angle up to 8.8 in kyphoplasty treated patients [8,14-19].
At the same time, there is a device related problem with the amount of reduction; when filling the kyphoplasty balloons a satisfactory reduction is achieved in many patients. However, the resulting reduction after cementing is approximately 25% lower due to a partial collapse after balloon deflation.13 In order to avoid this loss of height, a newer alternative—one based on the principles of balloon kyphoplasty and vascular stenting—has been developed. Using VBS, the stent remains within the newly created vertebral cavity, and the balloons can be removed after deflation while preventing the vertebral body from collapsing. Thus, in an ideal scenario, a virtually physiological vertebral body height and shape can be restored and preserved. The cavity is then filled with PMMA (Poly-methylemethacrylate) bone cement [20]. We performed a prospective analysis of the first 52 patients treated with VBS at our hospital. They had VCFs at levels T5 to L5 due to osteoporosis; there were 73 VCFs in these 52 patients. The goals of this study were to determine the safety and effectiveness of VBS in improving vertebral body height, decreasing pain, and improving function.
Material and Methods
Patients and Procedure
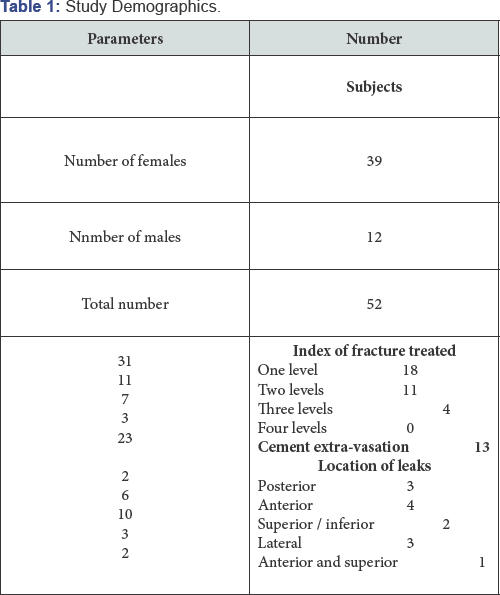
The study included 33 patients (13 male, 39 female) with a follow-up of nine months. The median age was 67 years (range 49-89 years) (Table 1). Subjects were excluded if they had associated spinal stenosis, pedicle fracture, neurologic deficit, an active infection, and severe comorbidities, such as uncorrected coagulopathy. The date of the fracture was determined by a retrospective chart review. During the preoperative visit, the patient was asked to recall a traumatic event or a sudden onset of pain. The interval between the date of fracture and the date of surgery determined the age of the fracture. The age of the fracture could be determined for 55 of the 73 fractures based on this method of data collection. Informed consent was obtained from all patients. A physical examination combined with lateral radiographs, magnetic resonance imaging (MRI) and computerized tomography (CT) were used to diagnose vertebral body compression fractures (VBCFs).
Surgical technique
A radiolucent table (Tru System 7500, Trumpf Medizin Systeme GmbH, Puchheim, Germany), and two C-arm fluoroscopy machines (Fluorostar 7900 Mobile Digital C-Arm, GE OEC Medical Systems GmbH, Wendelstein, Germany) were requested for every vertebral body stenting procedure at our hospital. The two fluoroscopy machines were placed orthogonally across the radiolucent Table 1, and allowed simultaneous viewing of antero-posterior and lateral projections of the spine. This process helped to accelerate the operation and minimize intraoperative contamination. The patients were then taken to the operating room, where general anesthesia was used in 33 procedures and local anesthesia with heavy sedation was utilized for 9 procedures. The patient was carefully turned prone onto the Wilson frame and all bony prominences were protected. To prevent infection, a preoperative single shot IV dose of a third generation cephalosporins was administered. Two fluoroscopy machines were then wheeled into position, and the fractured level was centered in both the antero-posterior and lateral projections before the skin was prepared and the patient was draped. The fluoroscopy machines were also covered with appropriate sterile covers.

A 1-cm incision was made just lateral and superior to both pedicles. Utilizing continuous fluoroscopic guidance, the guide wires were inserted into the superior outer pedicle quadrant using slight manual pressure and controlled blows from a hammer (Figure 1). The working sleeves were applied over a side-opening cannula, and the guide wires were removed. At this stage, any bone fragment that was extracted through the cannula was taken as a biopsy and sent for histopathological examination. A drill was manually twisted in the vertebral body to create a tract for the stents. The vertebral body stents are available in two sizes, {Vertebral body stent (Ø17mm [diameter] x 15 mm[length]) or (Ø17mm [diameter] x 20 mm [length]), Synthes GmbH, Solothurn, Switzerland)}. The stent implants consist of a strong cobalt-chromium alloy that is extensively used in coronary and peripheral artery stenting. The balloon catheters with the attached stents were inserted bilaterally; this was continued until the white indicator on the catheter shaft aligned with the top of the working sleeves. Then the packaging wires were removed.
The prepared VBS inflation systems were connected bilaterally, and the air bubbles were evacuated from the catheters using visual (fluoroscopic) and manometric parameters. Criteria for stopping the balloon inflation are the fracture being reduced, the balloon violating the confines of the bone, the inflation pressure reaching 440 psi, or maximum balloon volume being reached (5ml for 15 mm stent &5.5 ml for 20 mm stent). The balloons were gradually deflated to maintain maximum stent expansion, and then removed through the working sleeves (leaving the stents behind). PMMA cement (Vertecem, Synthes) corresponding to the combined volume of the inflated balloons was inserted bilaterally using the side-opening cannula by Synthes. Cement viscosity was measured by a viscometer (Viscosafe, Synthes) before and during the injection. Each step was performed under fluoroscopic control. The cement was inserted until it infiltrated the bone surrounding the stent. The cannulae were then pulled back slightly, but kept in until the cement hardened. Afterwards, the cannulae were twisted in order prevent any cement from being left in the pedicles.
Radiographic evaluation
Standing films were used to measure kyphosis of the fractured vertebral body (calculated as the angulation between both endplates). In some cases, preoperative standing films could not be obtained due to the patient's level of pain. In these situations, measurements were taken from the available supine films. Kyphotic angles were analyzed from these radiographs using a special software (Centricity PACS-IW 3.7.3.3; GE Healthcare, United Kingdom). Sagittal alignment across the fractured level was calculated using the Cobb technique. Measurements were taken from the superior endplate of the vertebra one level above the treated vertebra to the inferior endplate of the vertebral body one level below the treated vertebra. When non-adjacent levels were treated, separate Cobb angles were measured for each treated level. If adjacent level vertebral fractures were treated, a single Cobb angle measurement across the treated levels was obtained. Thoracic and lumbar fractures were analyzed for alterations in angles of kyphosis and lordosis, respectively. All symptomatic patients underwent MRI. The fractured levels requiring augmentation showed evidence of edema on T2-weighted images and MRI short TI inversion recovery sequences, hence the cause of pain. These were considered for treatment. CT scans were done only on select patients as in most cases enough information could be obtained about the integrity of the posterior wall from the MRI studies. Fluoroscopic and radiographic images were used to monitor extravasation from all treated vertebral levels.
Clinical Outcome measurements
Clinical outcomes were measured pre- and postoperatively using the visual analogue scale (VAS), Oswestry Disability Index (ODI) and ambulatory status (AS). All outcomes were assessed before the procedure and at 1, 12, 24, and 36 weeks after the procedure.
I. VAS: Patients were asked to note their pain on a scale of Q.Q to 10.0 cm, with Q.Q cm being no pain at all and 10.0 cm being the worst pain imaginable.
II. ODI: The ODI is a low back pain questionnaire that assesses the ability of the patient to perform various activities of daily living. The questionnaire consists of 10 categories (pain intensity, personal care, lifting, walking, sitting, standing, sleeping, social life, changing degree of pain, and traveling). Each category includes 6 options, ranked from 0 to 5, representing no limitation to severe limitation. The ODI score is calculated by using the following formula: total score/(5xnumber of questions answered) x 100.21 A lower percentage indicates a better health status.
III. AS: Ambulatory status was categorized as "fully ambulatory" for patients who could ambulate independently without assistance, "assisted ambulation" for patients who required a brace, cane, or walker to maintain mobility, and "not ambulatory" for wheelchair bound or bedridden patients.
Statistical analysis
Statistical analysis was performed using SPSS V17.0 (SPSS Inc, Chicago, Illinois). The data for clinical scores were checked for normality and found to be not normal. Hence, we used Wilcoxon paired rank test to compare two related groups; the Friedman test was used to compare more than two related samples. A P-value of 0.001 was considered to be the cut-off for statistical significance. Median and interquartile ranges were used as descriptive statistics.
Results
A total of 52 patients with 73 VCFs underwent cement augmentation at our hospital from April 2012 to June 2015. Two or more fractures were treated in 22 subjects (46%). Of the 52 subjects enrolled, 4 (9%) did not complete the 9 month follow-up. Two individuals refused to return for follow-up clinic visits (3%), one patient had subsequent medical comorbidities that made compliance impossible (3%), and one patient moved out of the area (3%). This article reports clinical effectiveness measures for the subjects who completed the 9 month follow- up (30). This group included 39 females and 13 males, with a median age of 67 years. Of the patients, 7 (21%) had back pain lasting more than 60 days before the procedure. Of the 73 fractures treated, 6 (4%) were at the thoracic levels and 22 (27%) were at the lumbar levels. The largest concentration of compression fractures was in the thoraco-lumbar spine.
All patients were mobile within the first 48 hours after surgery. Twenty-nine patients were hospitalized for 1-3 days. Due to additional injuries, 7 patients (12%) stayed for a maximum of 10 days. In 33 cases (67%), VBS was performed as an isolated procedure, whereas in 19 patients (33%) the adjacent levels above and below the treated level were reinforced with vertebroplasty or kyphoplasty during the same surgery. Indications for a combined procedure were an advanced stage of osteoporosis as well as significant overall kyphosis of the segments to be treated.
The clinical outcomes
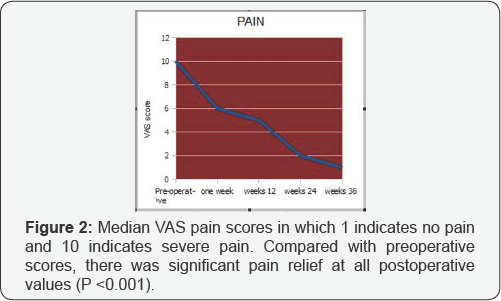
The median VAS scores (Figure 2) went from 10.0 preoperatively to 6.0 (Should you continue with a decimal and a 0, i.e, 6.0, 5.0, etc.?) at one week post-operatively, to 5.0 at 12 weeks following the procedure, and to 2.0 and 1 at 24 weeks and last follow-up, respectively. The preoperative ODI score was 80, improved to 45 at one week postoperatively, decreased to 35 at 12 weeks and to 22 and 18 at 24 weeks and last follow- up, respectively. Both the ability to move independently and ease of ambulation were significantly improved after the procedure (P <0.001). The proportion of patients who were fully ambulatory increased from 24% before surgery to 82% at 1-week postoperatively and to 95% at 9 months postoperatively. The median kyphosis angle was 15.0 degrees before the procedure and decreased by a median of 4.5 degrees after the operation; 76% of patients experienced a reduction in kyphosis of more than 4 degrees (interquartile range was 8.8 degrees). In an analysis of this subgroup of patients, faster pain relief was achieved compared with patients who showed minimal to no reduction in kyphotic angle.
Complications
There were two medical complications reported. Seven days after VBS, a pulmonary embolism was diagnosed in a patient with a history of deep vein thrombosis (no evidence of PMMA leakage to the lungs as indicated on CT angiography). The second patient had peri-operative confusion and generalized weakness that gradually resolved (per a negative brain CT and thorough neurologic exam). Evaluation of intra- and postoperative radiographs revealed extra-vertebral cement leaks in 23 (25%) of the 73 vertebral fractures treated. In five cases, cement leaked into the adjacent intervertebral disc. In six cases, leakage occurred anterior to the vertebral body; in three patients, cement leaked both into the adjacent intervertebral disc and anterior to the vertebra. All polymethylmethacrylate extravasations were asymptomatic. The cement remained in the immediate area of the treated vertebrae, and no medical or surgical intervention was required to remove the extravasated polymethylmethacrylate (Table 1).
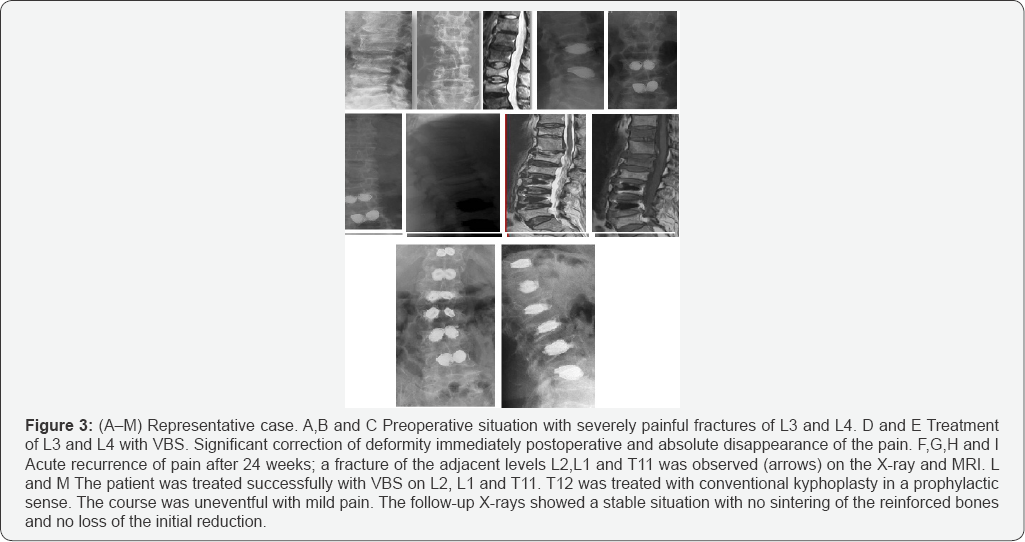
The clinical results of the group with polymethylmethacrylate extravasation did not differ from those subjects in whom it was not observed. The overall reoccurrence rate was 3 out of 48 patients who completed the 9 month follow-up. At 24 weeks following initial fixation, one patient was treated for multilevel fractures, two of which were adjacent to the initial level. The others were remote (Figure 3). The two remaining patients refused any further treatment. At the operative level, no subsequent treatment was warranted, and no additional fractures occurred.
Discussion
Osteoporotic VBCFs are a significant cause of back pain in the elderly. Even though only about one third of all fractures come to the attention of clinicians, the sequelae of VCFs represent a major impact on patients' physical function, quality of life, and survival. As our population ages, the rate of osteoporotic fractures is expected to triple over the next 30 years [21,22]. An ideal treatment for VBCFs would relieve fracture related pain and durably correct the kyphotic deformity of the spinal segment. In most cases, conservative measures are effective; however, one third of vertebral compression fractures result in chronic pain [23,24]. Percutaneous stabilization methods, such as vertebroplasty and kyphoplasty, have been developed to address these painful fractures. Vertebroplasty in its proper sense is not able to restore a kyphotic deformity. However, in fresh fractures [25], positioning of the patient can reduce the deformity to a certain extent, a reduction that can be preserved by cementing the vertebral body (VB).
Kyphoplasty was designed to address the kyphotic deformity and help to realign the spine. It has been reported that kyphoplasty can improve the kyphotic angle in the range of 3.4 to 8.8° degrees [8,19,26]. However, clinically, 34% of kyphoplasties do not result in a demonstrable reduction in kyphotic angle or restoration of vertebral body height [27]. Dudeney et al. [14] report on the treatment of VB fractures in metastatic lesions in 18 patients. They performed 55 kyphoplasty procedures. Of height loss, 34% was restored. (Are you trying to say that height loss was restored in 34% of the 55 patients?) A study by Weisskopf et al. [18] involved 22 patients with a total of 37 VB treated. Kyphosis reduction was achieved in only 4 cases with 8.5° on average.
One reason for inadequate height preservation in kyphoplasty is the loss of vertebral body height after balloon tamp deflation (prior to cement injection) [28,29] Stenting in order to correct a deformed VB has been introduced as a practical method of maintaining the initially gained height, as well as kyphotic angular changes of the vertebrae. Moreover, the stent maintains the size of the created cavity inside the vertebra after balloon removal. However, it could not yet be established that VB height reconstruction and correction of kyphosis are clinically relevant. McKiernan et al. [30] found that quality of life significantly improved in 46 patients following vertebroplasty. Garfin et al. [8] gave an overview on the treatment of the first 340 patients undergoing vertebroplasty. A total of 603 fractures were reduced and reinforced; 90% showed functional and symptomatic improvements. On the other hand, Markus et al. [31] found that there was no correlation between the height reconstruction in the vertebral body affected and quality of life.
This finding underlines the fact that the degree of height reconstruction might not have a significant influence on the quality of life after cement augmentation procedures. In our study, we found that 76% of patients experienced a reduction in kyphosis of more than 4 degrees. In an analysis of this subgroup of patients, faster pain relief was achieved compared with patients who showed minimal to no reduction in kyphotic angle. Furthermore, at the last follow-up, these patients were shown to have improved pain relief and functional capacity. To our knowledge, this is the first report of VBS treated fractures that has a 9 month follow-up. The clinical and radiographic results indicated that the effects of VBS are immediate and dramatic, and showed no evidence of deterioration with time.
Alleviation of pain, reduction in the use of pain medications, and improved mobility occurred within the first few postoperative days and weeks, and remained stable for the entire length of the study. This effect was shown by at least a 4-point decrease in the VAS pain score in 75% of patients at 1 week, 85% by 1 month, and 96% at 9 months. This result supports the earlier findings of rapid pain relief, as well as quality of life (ODI score and AS). In addition, it is noteworthy that clinical outcomes were nearly identical for subjects with age of fractures of more than 60 days, suggesting that older fractures can be successfully treated with VBS. Subsequent fractures occurred in 10% of subjects by 9 months; the majority were adjacent level fractures. The exact cause for subsequent adjacent-level vertebral compression fractures following cement augmentation procedures is still not fully explained. Some investigators [32] have suggested that vertebral body augmentation may alter stiffness, leading to an increased risk of subsequent adjacent-level vertebral compression fractures. However, the biomechanical basis for this theory is poorly documented. Mechanically, the response of the functional spinal unit (2 vertebral bodies with an intervening disc) to a given load is driven by its least stiff component. Because the disc [33] is 5-10 times less stiff than bone, load transfer to adjacent vertebrae is related to the stiffness of the disc, not the bone.
Whether cement augmentation leads to an elevated incidence of new adjacent-level fractures is the subject of ongoing discussion [29,30,32,34] As our patient population was rather small and the follow-up period was relatively short, we were not able to make definitive conclusions about the problem of adjacent level fractures. In our study, all polymethylmethacrylate extravasations were asymptomatic; the cement remained in the immediate area of the treated vertebrae. The early results after VBS are encouraging as the procedure has led to satisfactory improvement in pain, function and kyphosis correction in the treatment of osteoporotic fractures. Finally, we believe that the results of percutaneous VBS in osteoporotic fractures may encourage surgeons to widen the indications and use these techniques to successfully restore the anterior column in traumatic non-osteoporotic fractures in conjunction with posterior instrumentation.
Keypoints
A. One reason for inadequate height preservation in kyphoplasty is the loss of vertebral body height after balloon tamp deflation, prior to cement augmentation. Stenting of a VB in order to correct a deformed VB has been introduced as a practical solution to maintain the initially gained height.
B. This study supports VBS as a safe and effective method of improving vertebral height as well as overall sagittal alignment.
C. Future studies will need to address the efficiency of VBS as a valuable alternative to balloon kyphoplasty. The ideal study should be a direct in-vivo comparison between kyphoplasty and VBS.
References
- Kanis JA, Pitt FA (1992) Epidemiology of osteoporosis. Bone 13: S7- S15.
- Lee YL, Yip KM (1996) The osteoporotic spine. Clin Orthop 323: 91-96.
- Cook DJ, Guyatt GH, Adachi JD, Clifton J, Juniper EF. et al. (1993) Quality of life issues in women with vertebral fractures due to osteoporosis. Arthritis Rheum 36(6): 750-756.
- Gold DT (1996) The clinical impact of vertebral fractures: quality of life in women with osteoporosis.
- Kado DM, Browner WS, Palermo L, Nevitt MC, Genant HK, et al. (1999) Vertebral fractures and mortality in older women: a prospective study. Study of osteoporotic fractures research group. Arch Intern Med 159(11):1215-1220.
- Riggs BL, Melton III LJ (1995) The worldwide problem of osteoporosis: insights afforded by epidemiology. Bone 17(S5): 505S-511S.
- Ryan PJ, Blake G, Herd R, Fogelman I (1994) A clinical profile of back pain and disability in patients with spinal osteoporosis. Bone 15: 27-30.
- Garfin SR, Yuan HA, Reiley MA (2001) Kyphoplasty and vertebroplasty for the treatment of painful osteoporotic compression fractures. Spine 26(14):1511-1515.
- Heini PF (2005) The current treatment—a survey of osteoporotic fractures treatment. Osteoporotic spine fractures: the surgeon's perspective. Osteoporos Int 16(S1): S85-S92.
- ME (2003 Kallmes DF, Jensen) Percutaneous vertebroplasty. Radiology 229(1): 27-36.
- Berlemann U, Franz T, Orler R, Heini PF (2004) Kyphoplasty for the treatment of osteoporotic vertebral fractures: a prospective nonrandomized study. Eur Spine J 13(6): 496-501.
- Einhorn TA (2000) Vertebroplasty: an opportunity to do something really good for patients. Spine 25(9):1051-1052.
- Heini PF, Orler R (2004) Kyphoplasty for treatment of osteoporotic vertebral fractures. Eur Spine J 13:184-192.
- Dudensey S, Lieberman IH, Reinhardt MK, Hussein M (2002) Kyphoplasty in the treatment of osteolytic vertebral compression fractures as a result of multiple myeloma. J Clin Oncol 20(9): 23822387.
- Fourney DR, Schomer DF, Nader R, Chlan-Fourney J, Gokaslan ZL, et al. (2003) Percutaneous vertebroplasty and kyphoplasty for painful vertebral body fractures in cancer patients. J Neurosurg 98(S1): 21-30.
- Ledlie JT, Renfro M (2003) Balloon kyphoplasty: one-year outcomes in vertebral body height restoration, chronic pain and activity levels. J Neurosurg 98(S1): 36-42.
- Theodorou DJ, Theodorou SJ, Duncan TD, Garfin SR, Wong WH (2002) Percutaneous balloon kyphoplasty for the correction of spinal deformity in painful vertebral compression fractures. Clin Imaging 26(1):1-5.
- Weisskopf M, Herlein S, Birnbaum K (2003) Kyphoplasty - a new minimally invasive treatment for repositioning and stabilizing vertebral bodies. Z Orthop Ihre Grenzgeb 141: 406- 411.
- Wong W, Riley MA, Garfin S (2000) Vertebroplasty/kyphoplasty. J Womens Imaging 2: 117-124.?
- Heini PF, Orler R (2004) Vertebroplasty in severe osteoporosis. Technique and experience with multi-segment injection. Orthopade33: 22-30.
- Lavelle WF, Cheney R (2006) Recurrent fracture after vertebral kyphoplasty. Spine J 6(5): 488-493.
- Truumees E (2001) Osteoporosis Spine 26:930-932.
- Pateder DB, Khanna AJ, Lieberman IH (2007) Vertebroplasty and kyphoplasty for the management of osteoporotic vertebral compression fractures. Orthop Clin N Am 38(3): 409-418.
- Riggs BL, Melton LJ III (1995) The worldwide problem of osteoporosis: insights afforded by epidemiology. Bone 17(5) (suppl): 505S-511S.
- McKiernan F, Jensen R, Faciszewski T (2003) The dynamic mobility of vertebral compression fractures. J Bone Miner Res 18: 24-29.
- Ortiz AO, Zoarski GH, Beckerman M (2002) Kyphoplasty. Tech Vasc Interv Radiol 5(4): 239-249.
- Tohmeh AG, Mathis JM, Fenton DC, Levine AM, Belkoff SM (1999) Biomechanical efficacy of unipedicular versus bipedicular vertebroplasty for the management of osteoporotic compression fractures. Spine 24(17): 1772-1776.
- Feltes C, Fountas KN, Machinis T, Nikolakakos LG, Dimopoulos V, et al. (2005) Immediate and early postoperative pain relief after kyphoplasty without significant restoration of vertebral body height in acute osteoporotic vertebral fractures. Neurosurg Focus 18(3): e5.
- Voggenreiter G (2005) Balloon kyphoplasty is effective in deformity correction of osteoporotic vertebral compression fractures. Spine 30(24): 2806-2812.
- Uppin AA, Hirsch JA, Centenera LV, Pfiefer BA, Pazianos AG (2003) Choi IS Occurrence of new vertebral body fracture after percutaneous vertebroplasty in patients with osteoporosis. Radiology 226: 119-124.
- Markus D, Turgay E, Nina T, Quante M (2009) Comparison of kyphoplasty and vertebroplasty in the treatment of fresh vertebral compression fractures. Arch Orthop Trauma Surg 129(10): 1391-1399.
- Fribourg D, Tang C, Sra P, et al. (2004) Incidence of subsequent vertebral fracture after kyphoplasty. Spine 29(20): 2270-2276.
- White A, Panjabi M (1990) Clinical Biomechanics of the Spine. Philadelphia, PA: Lippincott pp: 722.
- Hulme PA, Krebs J, Ferguson SJ, Berlemann U (2006) Vertebroplasty and kyphoplasty: a systematic review of 69 clinical studies. Spine 31(17): 1983-2001.
Bone 18(S3): 185S-189S.






























