Painful Abdominal Mass with Undetected Growth in a 46-years-Old Man
Bárbara L Sotelo, Fernando Oliva, Juan José Domínguez, José Manuel Vilches and José Antonio Andrés
Department of Orthopaedic Surgery and Traumatology, Puerta del Mar University Hospital, Spain
Submission: November 19, 2016; Published: November 28, 2016
*Corresponding author: Bárbara L Sotelo, Department of Orthopaedic Surgery and Traumatology, Puerta del Mar University Hospital, Spain, Europe, Tel:; Email:dra.sotelo@yahoo.es; fernandolivamoya@gmail.com; uaj0@hotmail.com; jomavil7@hotmail.com; jaandres@ono.com
How to cite this article: Bárbara L S, Fernando O, Juan J D, José M V, José A A. Painful Abdominal Mass with Undetected Growth in a 46-years-Old Man. Ortho & Rheum Open Access J. 2016; 3(5): 555623. DOI: 10.19080/OROAJ.2016.03.555623
Abstract
Malignant fibrous histiocytoma (MFH) is a soft-tissue sarcoma characterized by a high rate of metastases or recurrence. The treatment of retroperitoneal sarcomas are challenging because of its rarity and frequent presentation with advance disease in an anatomically complex location. We report a case in a 46-years-old-man who presented left lower abdominal pain with a palpable mass in the left flank. A computed tomography (CT) scan demonstrated a large, well-circumscribed mass in the left iliopso as compartment extending to the root of thigh and to left femoral head. A primary surgical approach was decided and we report here the radical retroperitoneal tumor surgery with resection of the psoas major muscle. Tumor excision was performed in a piece with negative margins. The patient received postoperative radiotherapy and has been followed for three years and is free of recurrence. We review this tumor in the retroperitoneum, and discuss its diagnosis, pathogenesis, and treatment.
Keywords: Abdominal pain; Malignant fibrous histiocytoma; Retroperitoneal space; Thigh; Sarcoma
Introduction
Retroperitoneal soft-tissue sarcomas are rare tumors with an incidence of 0.5 to 1 new cases per 100.000 inhabitants per year [1]. Malignant fibrous histiocytoma (MFH) is the most common subtype of soft-tissue sarcoma. In the retroperitoneal space , MFH represents from 7 to 30% of sarcomas. Generally occurs in 50-70 year-old people [2,3]. This entity affects both sexes, most of the tumors are located at the extremities , its predilection for the thigh was reported in various studies [4,5], almost half are subcutaneous [6],and only 16% appears in the retroperitoneum [6,7]. Overall prognosis is influenced by tumor size, grading and resected margins, being negative microscopic margins the most favorable prognostic factor. We think that the case that we report is interesting because the few published cases located in the thigh and retroperitoneum and his treatment.
Case Description
A 46-years-old male patient was referred to our department with a two month history of left lower abdominal pain. It was located, nonradiating , presented at night , it didn ́t increased with the movement, tended to be relieved with nonesteroidal anti-inflammatory drugs. On physical examination a well-defined firm mass was palpable in the left flank, adherent to deep planes. He limited the hip flexion and started feeling numbness in the left anterior thigh. There was no antecedent of trauma or constitutional symptoms. A plain radiograph of the pelvis was normal. Ultrasound showed a solid tumor on the left inguinal ring in relation with the iliopsoas muscle.
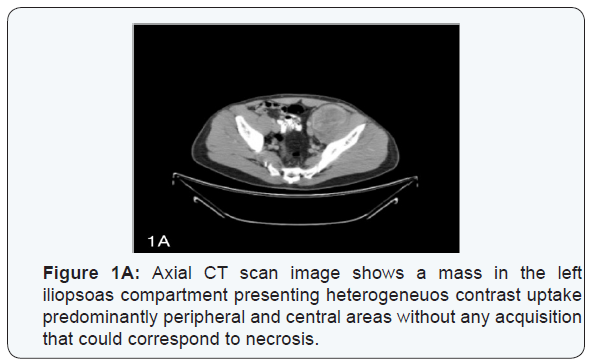
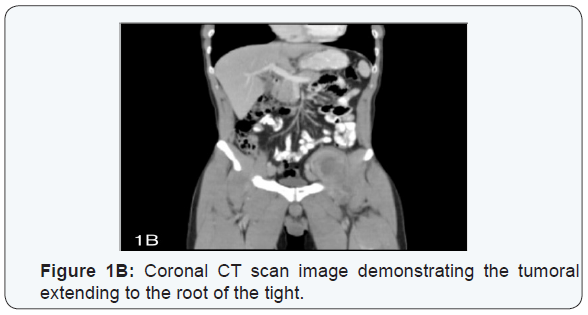
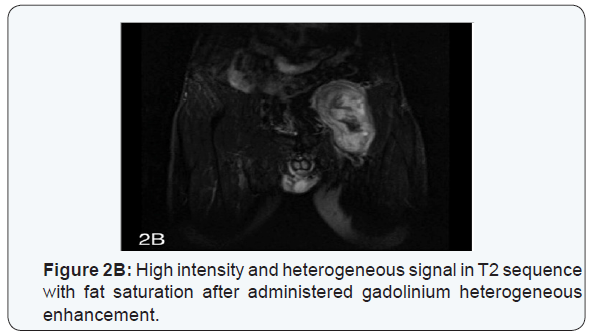
CT scan of the abdomen demonstrated a well- circumscribed mass in the left iliopsoas compartment extending to the root of thigh and to left femoral head, measuring 120x60x70 mm (Figures 1A-1B). Therefore, MR imaging showed a heterogeneous hypointense signal on T1 sequence in T2 sequence heterogeneous enhancement after having administered gadolinium (Figures 2A-2B). Scintygraphy didn ́t show metastatic spread and arteriography didn ́t display the formation of new blood vessels. We decide to do a surgical approach through an abdominoinguinal incisión [8] (Figure 3A).
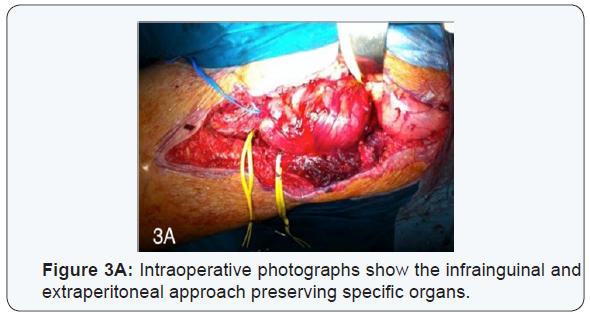
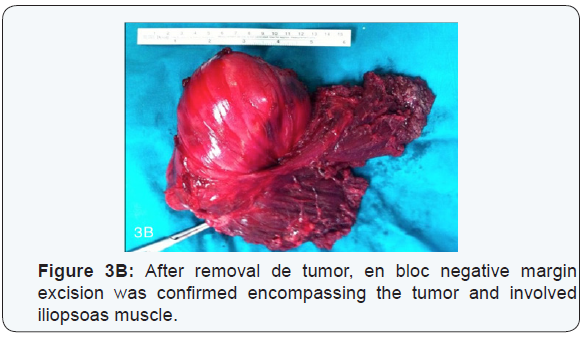
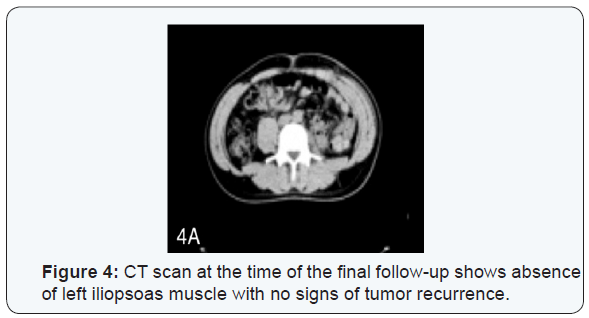
Tumor excision performed in a piece preserving specific organs. Intraoperative findings showed a single specimen of 190x130x90 mm encompassing the tumor and involved iliopsoas muscle, achieving macroscopically complete resection (Figure 3B) Histopathological examination of the specimen reported that microscopic margins were negative and the three femoral lymph nodes showed absence of tumoral infiltration. Postoperative radiotherapy was offered in the adjuvant setting in the dose of 6o Gy. Now, our patient has been followed for 36 months and is free of recurrence (Figure 4), with slight hypoesthesia in the left anterior thigh.
Discussion
MFH is one of the common soft-tissue sarcoma [2-9]. The symptom reported are painless mass, weight loss and abdominal, back or hip pain [2]. Very often, it can rise for longer periods of time [6,10,11]. In the diagnostic of the patient, adequate physical exam and images are important. Ultrasound provides a diagnostic in only 60% of cases [12,13]. Contrast CT is the initial investigation for evaluation and findings containing areas of low attenuation with loss of fat plane and mild contrast enhancement. Histopathological examination confirmed the diagnosis of MFH. MFH is a sarcoma, composed of tumor cells without evidence of an specific differentiation, both histiocytic and fibrous elements [14]. MFH has been categorized into storipleomorphic, mixoid, inflammatory, giant cell and angiomatoid variants [4,15,16].
Inmunohistochemical analyses shows tumor cells positive for vimentin, and negative for cytokeratins, desmin, S-100 protein, actins, c-kit and CD34. We decided an abdominoinguinal incision, the anterolateral abdominal wall muscles were divided along the iliac crest and the ligament 1-2 cm lateral to the femoral artery too. We did an extensión of the incisión to the left of the midline from the pubic symphysis to the pubic tubercle dividing the anterior rectus sheath, rectus muscle and peritoneum, then we extended transversely from the pubic tubercle to the midinguinal point and finally vertically into the femoral triangle over the approximate course of the femoral vessels [8].
Conclusion
We eliminated the tumor at the expense of removed all the iliopsoas muscle.The differential diagnosis based on clinical examination and radiological imaging and it includes softtissue sarcoma, metastatic tumors, abscess and haemorrhagic process.The most common malignant tumors in this area are metastases such testicular, renal, bladder and prostate tumors [17]. Differentiation from lipomatous tumour, leiomyosarcoma, and lymph node metastasis, is difficult. CT-guided biopsy is the alternative in the retroperitoneal space [1,7] and the diagnosis is mainly based on histologic and immunohistochemical findings.
Abscess may include fever and chills. CT features includes postcontrast enhancement of the peripheral abscess wall [12]. It is possible the presence of purulent material by diagnostic needle aspiration. Haemorrhage is rare and usually occurs secondary to trauma or from involvement of the psoas muscle in abdominal aortic aneurysm rupture [13]. The managementwas determined in a multidisciplinary team based on the imaging of the tumor and its surrounding structures. Surgery requires complete resection because it is the most important risk factor for local recurrence.
Debulking surgery is reserved for unresectable chemoresistant tumors. Several studies have shown the value of adjuvant radiation either postoperatively or preoperatively in lowering the incidence of local recurrence [18,19]. Systematic chemotherapy can be useful when used in a neoadjuvant manner in selected patients with technically unresectable tumors that could potentially be rendered resectable by downsizing. The prime cause of death is distant metastases and occurred within the first 2 years. After surgery a periodic follow up observation should be performed for the early detection of localrecurrence and metastasis. A long-term follow-up with regular chest X-ray and CT scans of the abdomen is mandatory.
- “Each autor certifies that he or she or a member of his or her immediately family has no comercial associations (eg, consultancies, stock ownership, equity interest, patent/ licensing arrangements, etc) that might pose a conflicto of interest in connection with the submitted article.”
- “Each autor certifies that his or her institution has approved the reporting of this case report and that all investigations were conducted in conformity with ethical principles of research”.
References
- Trans-Atlantic RPS Working Group (2015) Management of Primary Retroperitoneal Sarcoma (RPS) in the Adult: A Consensus Approach From the Trans-Atlantic RPS Working Group. Annals of Surgical Oncology 22(1): 256-263.
- Ko SH, Cha JR, Lee KJ (2012) Recurrent malignant fibrous histiocytoma in psoas muscle:a case report. Asian Spine J 6(3): 211-215.
- Atmatzidis KS, Pavlidis TE, Galanis IN, Papaziogas BT, Papaziogas TB (2003) Malignant fibrous histiocytoma of the abdominal cavity:report of a case. Surg Today 33(10): 794-796.
- Kaplan M, Iyiköşker HI (2012) A new complication of retained surgical gauze: development of malignant fibrous histiocytoma-report of a case with a literature review. World J Surg Oncol 10(1): 139.
- Salemis NS, Gourgiotis S, Tsiambas E, Panagiotopoulos N, Karameris A,et al. (2010) Primary intra-abdominal malignant fibrous histiocytoma: a highly aggressive tumor.J Gastrointest Cancer 41(4): 238-242.
- Peiper M, Zurakowski D, Knoefel WT, Izbicki JR (2004) Malignant fibrous histiocytoma of the extremities and trunk: an institutional review. Surgery 135(1): 59-66.
- Karki B, Xu YK, Wu YK, Zhang WW (2012) Primary malignant fibrous histiocytoma of the abdominal cavity: CT findings and pathological correlation. World J Radiol 4(4): 151-158.
- Karakousis CP (2010) Refinements of surgical technique in soft tissue sarcomas. J Surg Oncol 101(8): 730-738.
- T Nishida, NishiyamaN, Kawata Y, Yamamoto T, et al. (2005) Mediastinal Malignant Fibrous Histiocytoma Developing From a Foreign Body Granuloma. Jpn J Thorac Cardiovasc Surg 53(10): 583-586.
- Kenny JB, Widdowson DJ, Carty AT, Williams CE (1990) Malignant involvement of the iliopsoas muscle: CT appearances. Eur J Radiol 10(3): 183-187.
- Behranwala KA, A’Hern R, Thomas JM (2004) Primary malignant tumors of the iliopsoas compartment. J Surg Oncol 86(2): 78-83.
- Cronin CG, Lohan DG, Meehan CP, Delappe E, McLoughlin R,et al. (2008) Anatomy, pathology, imaging and intervention of the iliopsoas muscle revisited. Emerg Radiol 15(5): 295-310.
- Daly BD, McPhillips M, Leung AW, Evans RM, Metreweli C (1992) Ultrasound, computed tomography and magnetic resonance in the investigation of iliopsoas compartment disease. Australas Radiol 36(4): 294-299.
- Al-Agha OM, Igbokwe AA (2008) Malignant fibrous histiocytoma: between the past and the present. Arch Pathol Lab Med 132(6): 1030- 1035.
- Coindre JM, Mariani O, Chibon F, Mairal A, De Saint Aubain Somerhausen N et al. (2003) Most malignant fibrous histiocytomas developed in the retroperitoneum are dedifferentiated liposarcomas: a review of 25 cases initially diagnosed as malignant fibrous histiocytoma. Mod Pathol 16(3): 256-262.
- Fletcher CD, Gustafson P, Rydholm A, Willén H, Akerman M (2001) Clinicopathologic re-evaluation of 100 malignant fibrous histiocytomas: prognostic relevance of subclassification J Clin Oncol 19(12): 3045-3050.
- Spillane AJ, Thomas JM (1999) Surgical aspects of iliopsoas compartment tumours.Eur J Surg Oncol 25(4): 389-391.
- Enneking WF, Spanier SS, Goodman MA (1980) A system for the surgical staging of musculoskeletal sarcoma.Clin Orthop Relat Res 415: 4-18.
- Karakousis CP, Zografos GC (2002) Radiation therapy for high grade soft tissue sarcomas of the extremities treated with limb-preserving surgery. Eur J Surg Oncol 28(4): 431-436.






























