Relationship Between Early Menopause, Estrogens Receptor A Polymorphism, Vitamin D3 Receptor Polymorphisms and Osteoporosis in a Mediterranean Population
Teresa Esposito1, Marianna Chierchia2, Gian Franco Di Martino2, Bruno Varriale*1 and Dante Ronca2
1 Labaratory of Molecular Genetics, Dept. of Experimental Medicine, School of Medicine and Surgery, University of Campania “L. Vanvitelli”, Italy
2Department Multidisciplinary of Medical-Surgical Specialty and Dental Services, School of Medicine and Surgery, University of Campania “L. Vanvitelli”, Italy
Submission: September 05, 2018; Published: September 11, 2018
*Corresponding author: Prof. Dante Ronca, Department Multidisciplinary of Medical-Surgical Specialty and Dental Services, School of Medicine and Surgery, University of Campania “L. Vanvitelli”, Via L. de Crecchio 2, 80138 Naples, Italy.
How to cite this article: Teresa E, Marianna C, Gian F D M, Bruno V, Dante R. Relationship Between Early Menopause, Estrogens Receptor A Polymorphism, Vitamin D3 Receptor Polymorphisms and Osteoporosis in a Mediterranean Population. Nov Tech Arthritis Bone Res. 2018; 3(2): 555608. DOI: 10.19080/NTAB.2018.03.555608
Abstract
In order to clarify the role of candidate genes for the osteoporosis related phenotypes, we have investigated among polymorphism of the ESR1 gene and polymorphism of VDR3 gene in the relation to BMD and bone loss in a population of women of the southern Italy who underwent early (35-45 years old) menopause. The bone mineral density of all subjects was measured by Dual energy x-ray absorptiometry (DEXA). Molecular analyses were performed on ERa and VDR3 genes exons using both sequencing and RFLP technology. All women showed an average DEXA value less than -2,5. We have identified polymorphisms in the coding region of ESR1 gene that is well correlated with the bone status of the affected subjects. Vitamin D3 receptor also presents polymorphisms and is evident only in the affected subjects. The identified polymorphism of ESR1 is present only in osteoporotic patients and absent in normal subjects, such as the vitamin D receptor. Furthermore all the subjects that show such polymorphisms have DEXA values lesser than -2.5 showing a relationship between the above polymorphisms and bone loss. This let us to hypothesize that identification of polymorphism of ESR1 and vitamin D3 receptor could be a tool for early diagnosis of osteoporosis in early menopause woman.
Keywords: Estrogen receptor alpha polymorphism; VDR3 polymorphisms; Osteoporosis; Genetic-linkage; Early menopause.
Introduction
Osteoporosis brings about deterioration in activities of daily living and quality of life of the affected patients. Although fragility fractures resulting from osteoporosis continue to increase in the current aging society, it is assumed that this disease is still undertreated [1,2]. Actually, osteoporosis is defined as a skeletal disorder characterized by compromised bone strength predisposing a person to an increased risk of fracture [3]. In the definition of osteoporosis, low BMD must not be considered as a sole factor of osteoporosis. Infact more clearly the bone strength is determined not only by BMD but also by factors other than BMD [3]. Osteoporosis is a silent condition and there is no clinical tool to assess “bone quality”, so measurement of bone mineral density (BMD) is required to identify patients before fractures occur. There are many techniques for measuring bone mineral density. They fall into 2 main categories: those that use ionizing radiation and those that do not. Ionizing techniques include Dual Energy X-Ray Absorptiometry (DEXA) [4]. Dual Energy X-ray Absorptiometry (DEXA) measure bone density based on differential absorption of 2 x-ray beams by bone and soft tissues. It is the gold standard for detecting and diagnosing osteoporosis, characterized by low bone density and altered bone structure [5,6].
The World Health Organization has established criteria for osteoporosis and osteopenia based on DEXA BMD measurements: osteoporosis is defined as a BMD that is >2.5 standard deviations below the mean BMD for normal young adults (i.e. T-score <–2.5), while osteopenia is defined as BMD that is more than 1 standard deviation but less than 2.5 standard deviation below the mean for normal young adults (i.e. T-score< –1 and> –2.5). Bone mineral density measurement has been the most common test used to screen for and diagnose osteoporosis [7]. BMD measurement of the entire skeleton or specific sites (lumbar spine and proximal femur) using x-ray absorptiometry is based on the absorption of x-rays by the calcium crystals in the bone. It measures the amount of calcium per unit area (grams/square cm) or per unit volume (grams/cubic cm) in the bone. Results of BMD tests are expressed as T-score and Z-score. T-score is the number of standard deviations (SD) from the mean BMD for young (25–45years old) adults. A T-score of -2.5 represents a BMD value that is 2.5 SD below the mean BMD for young adults. Z-score is the number of SDs from the mean BMD value for people of the same age and gender 8. Although it was not intended to be applied to individual patients, the WHO classification works well to define ‘‘normal’’ (T-score -1.0 and above) and “osteoporosis” (T-score -2.5 and below). Several large studies have shown an unacceptably high risk of fracture in patients who have T-scores of -2.5 and below and a significant reduction in fracture risk with treatment, making this threshold an “evidence based” criterion for the diagnosis of osteoporosis and for the initiation of treatment [9,10].
According to its definition, the genes of osteoporosis should be a group of genes contributing to the multiple aspects of pathogenesis. When polymorphisms of genes were significantly and reproducibly associated with bone phenotypes, it must be considered a potential marker although the contribution of each polymorphism to BMD would be small. The multiple factors contributing to the pathogenesis of osteoporosis include genetic and environmental factors. Because decrease in bone mineral density (BMD) is the major clinical indicator and a useful quantitative trait, many association and linkage studies of BMD have been conducted. Although the series of studies showed apparently significant associations, the genes have not been found that can be utilized in clinical practice. Several genes identified in robust genome-wide association studies will be the new cutting edge in genetic studies of osteoporosis [11]. The “essential gene”, responsible for the manifestation of osteoporosis has not yet been identified, despite utilizing the most advanced methods. Some random observations indicate the broader impact of candidate genes for osteoporosis of the skeleton.
Genes are important in determining both peak bone mass and the rate of bone loss in later life. There is agreement that genetic factors are important, however, identifying the relevant genes have yielded inconsistent and conflicting results. Several genes are involved, some of which may be more important in particular ethnic groups than in others [11]. The genetics of osteoporosis has many pitfalls, that prevent application of information to practical osteology. An unanimous consensus has not been reached in the relationship between certain candidate genes and bone phenotypes. A significant disturbing phenomenon is the effect of mutual interactions between genes (e.g. the interaction between ER and VDR) or between a gene and the environment (lifestyle, nutrition, physical activity). The effects of epigenetic factors must also be considered.
The GWAS method can partially overcome those pitfalls: it allows for the identification of a range of candidate genes and an assessment of the impact of their mutual interactions on the appropriate phenotype in a single measurement (genomics). So far, about 20 GWAS studies have recorded the association of genes with bone density, fractures, or skeletal geometry [12]. From the point of further progress in genetics of osteoporosis, the polymorphic variations at multiple loci can be detected in the laboratory. Despite all of the difficulties and numerous unanswered questions, the genetics (genomics) of osteoporosis remains a big challenge for further research in the field of pathogenesis, diagnosis and the personalized treatment of osteoporosis. The regulatory effect of these genes on hormonal parameters needs to be further verified. In this respect here, we have undertaken this study inorder to correlate the single nucleotide polymorphism in the estrogen receptor alpha and in the vitamin D3 receptor and the osteoporotic status in women with early menopause.
Materials and Methods
We have selected in our cohort of subjects (1564) that underwent to osteoporosis a set of women (89) ranging between 35 and 45 years with early menopause symptoms and women (64) ranging between 45 and 55 years in advanced menopause but with no diagnosis of osteoporosis (used as control group). All women were subjected to genetic counseling. All treatments follow the guidelines of our Comitato Etico dell’Azienda Ospedaliera Universitaria of the 2nd University of Naples. The study was performed in accordance with the ethical standards stated in the 1964 Declaration of Helsinki and approved by the local clinical research ethics committee (protocol number 477, 18 November 2013).
Blood Samples
After the counseling and with their written informed consent, blood samples from all women were collected. Blood samples were used for DNA extraction. All women did not undergo to any pharmacological treatment.
BMD Evaluation:
Dual energy x-ray absorptiometry (DEXA) was carried out to all subjects enrolled for the present study. The values for a diagnosis of osteoporosis were to consider ‘‘normal’’ in the subjects with a T-score of -1.0 and above, and “osteoporosis” in those with a T-score of -2.5 and below. A dual energy x-ray absorptiometry (DXA) machine sends a thin beam of low-dose x-rays with 2 distinct energy peaks through the bones of patients. One peak is absorbed mainly by soft tissue and the other by bone. BMD is calculated from the difference in absorption between the bone and the soft tissue. Computer software calculates the numerical density of the bone from the image and compares it with the mean of healthy young adults, and to the age-matched control of the reference population. Intra-instrument reliability was assessed by repeatedly scanning soft tissue phantoms for lean tissue (water) and fat tissue (methanol) using one DPX-Land two identical Prodigy. Intra-instrument reliability, expressed as coefficient of variation, ranged between 0.7% and 5.2% for the DPX-L and 0.4% and 4.5% for the Prodigy, with the lowest coefficients of variation observed when scanning the fat tissue phantom.
Chemicals
All chemicals and glassware were molecular biology grade. Primers for exons amplification and assay kits for steroids were purchased from Sigma (St. Louis, MO).
DNA Extraction
Blood samples were obtained from all participants and genomic DNA was extracted with standard purification protocols [13,14].
Primers and Estrogen Receptor Alpha (Erα) Exon Amplification, Primers and Vitamin D3 Receptor (VD3R) Exons Amplification
Primers were designed (Table 1) from sequences present in GenBank (BC128573.1 for the exon 6 of the Era and from the sequenced gene for the exon 6 and 7 of VD3R and Human Genome Browser. PCR were performed accordingly to the manufacturer of PCR kit Roche (Roche Diagnostics, Italy). Products of amplification reactions were purified with standard methods and used for sequencing. Amplification products were sequenced from both ends.

Sequencing
The product of PCR amplification was sequenced from both strands according to the conditions out-lined by the Big Dye Terminator Kit (PerkinElmer/Applied Biosystem) and runs on ABI 377 Sequencing System (PerkinElmer/Applied Biosystem) [15].
RFLP of Sequenced Exons
Sequenced exons were digested using appropriate restriction enzymes inorder to generate restriction fragments. The exon 6 of the estrogen receptor alpha was digested with Pst1 (New England Biolabs), the exon 6 of the vitamin D3 receptor was digested with ApaI (New England Biolabs), the exon 7 of the vitamin D3 receptor was digested with Bam H1 (New England Biolabs). The restriction fragments were separated onto agarose gel (1.8%) and the electrophoresis results were photographed with appropriate apparatus.
Statistics
Significance of differences was evaluated by using Duncan’s test (at p < 0.05 and p < 0.01) for multi-group comparisons.
Results
It ‘important to note that, of the total number of the subjects who had been referred to the osteoporosis service of our university, only 89 of them underwent to an early onset of menopause. This number of subjects is compatible with the percentage currently found in Southern Italy for patients with early menopause (about 5%). Also, no significant differences were found in BMI between the two experimental groups.
BMD Evaluation
Diagnosis of osteoporosis was based on the BMD obtained with DEXA at the hip (neck of the femur) and spine (vertebral body of L2, L3, and L4), which is considered the gold standard for the noninvasive diagnosis of osteoporosis. The average value of T-score measured with DEXA was -2.8 (T-score range: from -3.7 to -1.98). Our cohort of patients affected by early menopause showed an average value of BMD less of -2,5, while the control group showed an average value of – 0.7 (Table 2)

Era Polymorphism
The analysis of the sequences of amplified exons, show a polymorphism in the exon 6. The base mutations cause the insertion of restriction sequences for the Pst1 enzyme. The restriction fragments generated by the above mutation are of 520 and 177 bp respectively and are shown in Figure 1. In the exon 6, the Glu441 is substituted by Gln. Thus, a basic aminoacid is substituted by a polar one. This polymorphism was found only in the subject that underwent to early menopause.

VD3R Polymorphism
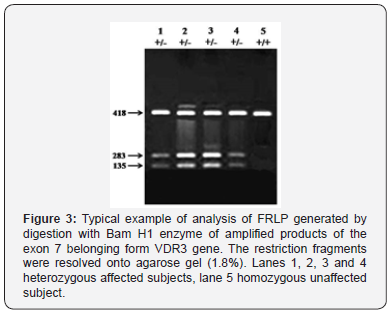
The analyses of the sequences of amplified exons, show a polymorphism in the exons 6 and 7. The base mutation in the exon 6 cause the insertion of a restriction sequence for the ApaI enzyme. The restriction fragments generated by the above mutation are of 550 and 423 bp respectively and are shown in Figure 2. In the exon 6 of VD3R gene cause the substitution of Arg121 by Gly. Thus, a basic amino-acid is substituted by a nonpolar one. As far as it concerns the exon 7, the base mutation causes the insertion of a restriction sequence for the Brahmi enzyme. The restriction fragments generated by this mutation are of 283 and 135 bp respectively and are shown in Figure 3. In this exon of the VD3R receptor gene the mutation causes the substitution of Ser165 by Ile. Thus, a polar amino-acid is substituted by a non-polar one. This polymorphism was found only in the subject that showed an early menopause.

Discussion
Postmenopausal osteoporosis is heterogeneous disorder that appear to be caused by several non-hormonal and hormonal factors. Of non-hormonal factors, age-related bone loss, the degree of bone density achieved in young adult life, and dietary intake and absorption of calcium appear to be important. Hormones that may be important in pathogenesis are parathyroid hormone (PTH), estrogen, 1,25(OH)2D, and possibly calcitonin. Postmenopausal estrogen deficiency accelerates bone loss by increasing responsiveness of bone to endogenous PTH. The resultant increase in release of calcium from bone is associated with normal or low values for serum immune-reactive PTH (iPTH) except for a subset of 15% of the total (which appear to represent a separate population). Some evidence suggests that subnormal calcium absorption, which is a common finding in postmenopausal osteoporosis and which may contribute to negative calcium balance, is caused by decreased conversion of 25-OH-D to 1,25(OH)2D.
The role of steroid hormones in the development and maintenance of bone is a well-established phenomenon. Traditionally the point of view is that estrogens and androgens were the main sex steroids influencing bone maturation and maintenance in women and men, respectively [16]. Studies reported that serum 17b-estradiol well correlated with bone mass density at various sites although also T has some effects [17-23]. It has been shown that serum17b-estradiol is important in the increase in bone mass during the puberty [23]. This claims for a central role of estrogen with respect to skeletal metabolism. In fact, in patients with aromatase deficiency 17b-estradiol levels lesser than 20 pg/ml are required to complete bone maturation and mineralization [ 20,24-26].
The cortical bone size is, at least partly, due to sex steroid exposure in mice [20,21,27]. Studies on the effect of ER activation non-trabecular bone have been performed inorder to better understand which ER is mainly involved in bone development. In these studies, orchidectomized wild type (WT) and ER-inactivated mice were treated with the non-aromatizable androgen dihydrotestosterone (DHT), 17b-estradiol, or vehicle. Both ERa and AR but not ERb activation preserved the amount of trabecular bone. ERa activation resulted both in a preserved thickness and number of trabeculae. ERa is the principal ER for the regulation of both trabecular and cortical bone in female mice [22,28-31]. These observations well correlate with the results obtained from the analysis of polymorphisms of the estrogen receptor alpha. All subjects with early menopause with osteoporosis had a polymorphism of exon6.In the exon 6, the Glu441 is substituted by Gln. Thus a basic amino-acid is substituted by a polar one. This amino acid substitution falls in the steroid-binding domain that to be fully effective, it must have a well-controlled electrical environment. This result may indicate that 17b-estradiol is bound with lower efficiency in the binding pocket of the receptor by decreasing the efficiency of the response to the hormone. Besides ERa studies in postmenopausal Italian women indicate that intragenic polymorphisms make a small, but statistically significant contribution to the heritability of bone mineral density [11].
Among the vitamin D facts, it must been noticed that its metabolite (1,25(OH)2D3) plays a key role in the regulation of bone metabolism. It activates specific receptors (VDR) on osteoblasts and stimulates bone formation. However, in high in vitro concentrations, it activates osteoclastic resorption.1,25(OH)2D3 through VDR also regulates calcium homeostasis in vivo outside of the bone by reducing calcium and phosphorus loss in the kidneys, while stimulating their absorption in the intestines, thereby ensuring adequate bone matrix mineralization [8]. The gene for VDR was the first candidate gene, in which an association with bone mineral density was discovered by Morrison [32]. The effect of the VDR genotype (the TaqI, BsmI and ApaI polymorphisms) on BMD has been found strongest in premenopausal women and decreases with age [33]. Later, however, only 11 isolated studies found an association between VDR and BMD values [34] while other studies (including those using the GWAS method) had negative results. Instead, genes encoding the expression of proteinbinding vitamin D (VDBP) and circulating25(OH)D (CYP2R1) were identified, which predicted the risk of osteoporosis [11,35]. A study of an intragenic polymorphism in VDR led to the suggestion that this gene, mutations in which cause vitamin D-depended rickets type II, could account for as much as 75% of the heritability of bone mineral density [11,23]. It must have also in account that similar studies failed to confirm this observation. In this respect our study carried out in a particular woman population (early menopause) have accounted for clear correlation between VDR polymorphisms and osteoporosis. The ApaI polymorphism in the exon 6 accounts for the substitution of Arg121 by Gly. Thus a basic amino-acid is substituted by a nonpolar one. This substitution falls in the DNA binding domain. Due to the electric properties of Gly (non-polar), this substitution instead of Arg having basic properties, the bind to DNA of the VDR3 receptor could be less efficient.
As far as it concerns BamHI polymorphism the exon 7, the mutation cause the substitution of Ser by Ile. Also, this substitution falls in the ligand binding domain. Also, in this case the electric properties have a remarkable change since a polar amino-acid is substituted by a non-polar one. The binding of the ligand to the receptor induces a conformational change of the ligand binding domain (LBD) with consequent dissociation of co-repressors. Upon ligand binding, VDR forms heterodimer with the retinoid X receptor (RXR) that binds to vitamin D response elements (VDREs), recruits co-activators. This leads to the expression of a large number of genes. Approximately 200 human genes are considered to be primary targets of VDR and even more genes are regulated indirectly. Our hypothesis is that the change Ser165/Ile may affect one of the above effect exerted by ligand. But this must be proved with targeted experiments. It is noteworthy that we found double mutation in the VDR3 receptor only in one subject while only one of the mutations among VDR3 gene described in the present paper has been found in our cohort of affected woman. Interestingly, all affected woman show the polymorphism of ERa gene and at the same time one of the two polymorphism of the VDR3 gene.
From our results its appears that the early menopause is not only closely related to an increased risk of osteoporosis in our southern Italy population but show also a genetic linkage with both ERa and VDR3 polymorphism. It is well known that treatment of osteoporosis with either sex steroids (by antagonizing the effect of PTH on bone resorption) or orally administered calcium with or without vitamin D (by decreasing PTH secretion) decreases bone resorption. Long-term therapy with these agents, however, decreases bone formation; thus, bone loss is only arrested or slowed. Although combined therapy with fluoride and calcium stimulates bone formation and appears to be capable of increasing bone mass, its long-term safety and efficacy in decreasing the occurrence of fractures remain to be demonstrated specially in those subject that undergone to early menopause.
Acknowledgement
This work is dedicated to Professor Anna Cardone, a dearest friend who died prematurely.
Statement
Teresa Esposito, Marianna Chierchia, GianFranco Di Martino, Bruno Varriale, and Dante Ronca declare that they have no conflict of interest.
References
- Kroth PJ, Murray MD, McDonald CJ (2004) Undertreatment of osteoporosis in women, based on detection of vertebral compression fractures on chest radiography. Am J Geriatric Pharmacotherapy 2: 112-118.
- Consensus Development Center (1993) Consensus Development Conference V, 1993. Diagnosis, prophylaxis and treatment of osteoporosis. Am J Med 94: 646-650.
- NIH Consensus Development Panel (2001) NIH consensus development panel on osteoporosis prevention, diagnosis, and therapy. JAMA 285(6): 785-795.
- Watts NB (2004) Fundamentals and pitfalls of bone densitometry using dual-energy X-ray absorptiometry (DXA). Osteoporosis Int 15(11): 847-854.
- Makhdoom A, Rahopoto MQ, Siddiqui KA, Qureshi GA (2014) Detection of osteoporosis by dual energy X-ray absorptiometry. Pak J Med Sci 30(6): 1265-1269.
- Baim S, Wilson CR, Lewiecki EM, Luckey MM, Downs RW, et al. (2005) Precision assessment and radiation safety for dual-energy X-ray absorptiometry: Position paper of the International Society for Clinical Densitometry. J Clin Densitom 8(4): 371-378
- Shore RM, Langman CB, Donovan JM, Conway JJ, Poznanski AK (1995) Bone mineral disorders in children. Evaluation with dual X-ray absorptiometry. Radiology 196(2): 535-540.
- Kanis JA, Melton LJ III, Christiansen C, Johnston CC, Khaltaev N (1994) The diagnosis of osteoporosis. J Bone Miner Res 9(8): 1137-1141.
- Hodgson SF, Watts NB (2003) American Association of Clinical Endocrinologists medical guidelines for clinical practice for the prevention and management of postmenopausal osteoporosis, 2001 Edition, with selected updates for 2003. Endocrine Practice 9(6): 544- 564.
- Kanis JA, Gluer CC (2000) An update on the diagnosis and assessment of osteoporosis with densitometry. Committee of Scientific Advisors, International Osteoporosis Foundation. Osteoporosis Int 11(3): 192- 202.
- Young ID (2002) Genetics for Orthopedic Surgeons – The molecular genetic basis of orthopedic disorders. Remedica Publishing, London.
- Riancho JA, Hernándeze JL (2012) Pharmacogenomics of osteoporosis: A pathway approach. Pharmacogenomics 13(7): 815-829.
- Ausubel FM (1987) Current Protocols in Molecular Biology, Greene/ Wiley–Interscience, New York.
- FritschEF, ManiatisT, SambrookJ (1989) Molecular Cloning: A Laboratory Manual, Cold Spring Harbor Laboratory Press, Cold Spring Harbor, NY.
- Esposito T, Tammaro P, Paolisso G, Varriale B (2015) Hormonal regulation and characterization of MHG30 gene, a desaturase-like gene of hamster harderian gland. J Steroid Biochem Mol Biol 154: 267-73
- Esposito T, Uccello R, Caliendo R, Di Martino GF, Gironi Carnevale UA, et al. (2009) Estrogen receptor polymorphism, estrogen content and idiopatic scoliosis in human: A possible genetic linkage. J Steroid Biochem Mol Biol 116(1-2): 56-60
- Dawson-Hughes B, (2008) Serum 25-hydroxyvitamin D and functional outcomes in the elderly. Am J Clin Nutr 88(23): 537S-540S.
- Buell JS, Hughes DB (2008) Vitamin D and neurocognitive dysfunction: preventing “D” decline? Mol Aspects Med 29(6): 415-422
- Quarles LD (2008) Endocrine functions of bone in mineral metabolism regulation. J Clin Invest118(12): 3820-3828.
- RochiraV, Faustini Fustini M, Balestrieri A, Carani C, (2000) Estrogen replacement therapy in a man with congenital aromatase deficiency: Effects of different doses of transdermal estradiol on bone mineral density and hormonal parameters, J Clin Endocrinol Metab 86(5): 1841-1845.
- Venken K, De Gendt K, Boonen S, Ophoff J, Bouillon R, et al. (2006) Relative impact of androgen and estrogen receptor activation in the effects of androgens on trabecular and cortical bone in growing male mice: A study in the androgen receptor knockout mouse model. J Bone Miner Res 21(4): 576-585.
- Lindberg MK, Moverare S, Skrtic S, Alatalo S, Halleen J, et al. (2002) Two different pathways for the maintenance of trabecular bone in adult male mice. J Bone Miner Res 17: 555-562.
- Takayuki H (2010) Genetic aspects of osteoporosis. J Bone Miner Metab 28(6): 601-607.
- Carani C, Qin K, Simoni M, Faustini Fustini M, Serpente S (1997) Effect of testosterone and estradiol in a man with aromatase deficiency. NewEngl J Med 337: 91-95.
- Bilezikian JP, Morishima A, Bell J, Grumbach MM (1998) Increased bone mass as a result of estrogen therapy in a man with aromatase deficiency, New Engl J Med 339(9): 599-603.
- LanfrancoF, ZirilliL, BaldiM, PignattiE, CorneliG, et al. (2008) A novel mutation in the human aromatase gene: Insights on the relationship among serum estradiol, longitudinal growth and bone mineral density in an adult man under estrogen replacement treatment. Bone 43(3): 628-635.
- Moverare, Venken K, Eriksson AL, ndersson N, Skrtic S, et al. (2003) Differential effects on bone of estrogen receptor a and androgen receptor activation in orchidectomized adult male mice, PNAS 100(23): 13573-13578.
- Lindberg MK, Alatalo SL, Halleen JM, Mohan S, Gustafsson JA, et al. (2001) Estrogen receptor specificity in the regulation of the skeleton in female mice. J Endocrinol 171(2): 229-236.
- Lindberg MK, Weihua Z, Andersson N, Moverare S, Gao H, et al. (2002) Estrogen receptor specificity for the effects of estrogen in ovariectomized mice. J Endocrinol 174(2): 167-178.
- Sims NA, Lacroix CP, Minet D, Vanhulle FC, Kelly GM, et al. (2003) A functional androgen receptor is not sufficient to allow estradiol to protect bone after gonadectomy in estradiol receptor deficient mice. J Clin Invest 111(9): 1319-1327.
- Sim NA, Dupont S, Krust A, Clement Lacroix P, Minet D, et al. (2002) Deletion of estrogen receptors reveals a regulatory role for estrogen receptors-beta in bone remodeling in females but not in males. Bone 30(1): 18-25.
- Morrison NA, Qi J, Tokita A, Kelly PJ, Crofts L, et al. (1994) Prediction of bone density from vitamin D receptor alleles. Nature 367(6460): 284- 287.
- Riggs BL, Nguyen TV, Melton LJ, Kortison NA, O Fallon WM (1995) The contribution of vitamin D receptor gene alleles to the determination of bone mineral density in normal and osteoporotic women. J Bone Miner Res 10(6): 991-996.
- Masi L, Cimaz R, SimoniniG, Bindi G, Stagi S, et al. (2002) Association of low bone mass with vitamin D receptor gene and calcitonin receptor gene polymorphisms in juvenile idiopathic arthritis. J Rheumatol 29(10): 2225-2231.
- Mejia RD, Coral Vazquez RM, Coronel A, Espinosa CL, del Carmen Aguirre Garcia M, (2014) Relation of the estrogen receptor and vitamin D receptor polymorphisms with bone mineral density in postmenopausal Mexican-mestizo women. Gene 537(1): 10-14.






























