How Common is Laterality-Deficits in Patients Attending Outpatient Physiotherapy with Lower Extremity Injuries?
Adriaan Louw*1, Alex Birely2, Daniel Kaschke2, Brad Tracy3, Hailey Louw4, Kevin Farrell2
1Evidence in Motion, USA
2Department of Physical Therapy Education, St Ambrose University, USA
3Evidence in Motion, USA
4Department of Mathematics, Northwestern College, USA
Submission: April 08, 2022; Published: April 25, 2022
*Corresponding author: Adriaan Louw, PhD, Evidence in Motion, 618 Broad Street, Suite B, Story City, USA
How to cite this article: Adriaan L, Alex B, Daniel K, Brad T, Hailey L. How Common is Laterality-Deficits in Patients Attending Outpatient Physiotherapy with Lower Extremity Injuries?. J Yoga & Physio. 2022; 9(5): 555773. DOI:10.19080/JYP.2021.09.555773
Abstract
Introduction: Alterations in cortical body maps (body schema), have been tied to the initiation and maintenance of a pain state. One clinical test of altered body schema is left-right discrimination or laterality, which is abnormal in people with chronic pain. To date, the prevalence of these changes in clinical practice has not been studied or reported.
Materials and Methods: Patients attending outpatient physiotherapy for lower extremity injuries were recruited for the study. Following completion of consent and demographic data collection, patients completed two laterality tests of the foot. Mean score of two tests of foot laterality accuracy and speed was collected for each patient. Laterality scores were compared to current normative data to determine patients presenting with abnormal values and which clinical presenting signs and symptoms correlate to abnormal laterality scores.
Results: Forty patients (female 22), participated in the study. Fourteen patients (35%) recorded an abnormal laterality score (speed or accuracy), indicating a relative high prevalence of laterality issues in patients attending outpatient physiotherapy for lower extremity injuries. Older patients and patients identifying as female were more predictive of poor laterality score, compared to other demographic and clinical variables including duration and intensity of pain, immobilization and surgery.
Conclusion: Laterality deficits are common in patients attending outpatient physiotherapy for lower extremity disorders. Older adults and patients identifying as female have a higher chance of recording an abnormal laterality score. Clinicians should recognize this, test for it and use it as a guide in their treatment planning.
Keywords: Pain; Physiotherapy; Laterality; Body Schema
Abbreviations: GMI: Graded Motor Imagery; PT: Physiotherapy; S1: Primary Somatosensory Cortex
Introduction
Traditional pain models often associate injury, various disease processes, inflammation, emotional stressors, etc., with a human’s pain experience [1,2]. Emerging neuroscience research has shown that altered body maps (schema) in the brain may also be associated with human pain experiences [3,4]. It is now well established that the physical body of a person is represented in the brain by a network of neurons, often referred to as a representation of that particular body part in the brain or homunculus [5-8]. This representation refers to the pattern of activity that is evoked when a particular body part is stimulated.
One of the most studied regions of the brain associated with representation is the primary somatosensory cortex (S1) [5-8]. Body schema is thus an integrated neural representation of the body [9]. These neuronal representations of body parts are dynamically maintained, which plays a significant role in a person’s pain experience as well as treatment options [3,10-14]. It is proposed that movement therapy (i.e., exercise, Feldenkrais, yoga, Pilates, etc.) or tactile treatments (i.e., manual therapy, massage, dry needling, etc.), can strengthen these maps, which in turn may ease pain and disability [15-17].
It has been shown that patients with pain display different body schema maps than people with no pain [3,10-14]. Growing evidence additionally supports the notion of these body schema maps expanding or contracting thus essentially increasing or decreasing the body map representation in the brain, most notably in patients with complex regional pain syndrome, phantom limb pain, and chronic low back pain [3,7,18,19]. The clinical importance is that these changes in shape and size of body maps seem to correlate to increased pain and disability [10,20]. Although various factors have been linked to the development of this altered cortical representation of body maps in S1, it is believed that issues such as neglect and decreased use of the painful body part [18], may be a significant source of the altering of body maps [21,22]. A vicious cycle soon emerges between decreased movement, cortical reorganization, and increased pain [18].
In research settings, altered representation of S1 is studied using various forms of advanced brain imaging [11]. In clinical practice, some tests are available to similarly infer changes in the cortical maps, including two-point discrimination, localization, and laterality [15,23,24]. Laterality testing is the process whereby an individual is presented with either a left or right image of an affected body part and they must report if it’s left or right [25-27]. In normal, pain-free adults, normative data has been established for hands, feet, back and neck [23,25]. In people experiencing pain, especially chronic pain, there is a delay (slower ability to identify left/right) and less accuracy [25-27]. It has been postulated that cortical smudging of the S1, neglect and pain influence these measures [4]. When laterality is abnormal, a structured, series of laterality treatments (test becomes the treatment), referred to as graded motor imagery (GMI) is used to normalize these measures with the intent to decrease pain and disability [28,29]. Current evidence for GMI for complex pain states is emerging as a evidence-based approach for people in pain [30].
Given that laterality is an emerging approach in rehabilitation and movement science, there are various unknowns. One of the unknowns is what percentage of patients attending physiotherapy (PT) present with laterality deficits? How common is this phenomenon? The aim of this study was to determine what percentage of patients attending outpatient PT with lower extremity injuries present with a laterality deficit? Secondary analysis established if other presenting variables at the initial visit correlated to laterality deficits.
Methods
Patients
The study design called for a convenience sample of patients attending outpatient PT with lower extremity pain (knee, ankle and foot) to be recruited, complete a demographic survey and a laterality test. Institutional review board approval was be obtained from St. Ambrose University for this study. Participation was entirely voluntary, and the patient had to consent to being part of the study. In order to participate, patients must have presented with a primary complaint of knee, ankle or leg pain, over the age of 18 and proficient in reading and writing the English language. Two outpatient PT clinics where two St. Ambrose orthopedic residents worked served as data collection sites. Data was collected at each clinic over a 4-month period.
Instrument
Two distinct data sets were collected per patient
a) Demographics: In line with previous similar studies, demographic data was collected including age, gender, employment status, education background, pain experience, pain rating (numeric pain rating scale), family history of persistent pain, location of pain, amount of sleep per night, amount of exercise per week, if they smoke, weight, height, family history of depression and having had imaging for their leg pain [31,32].
b) Laterality: In order the assess the speed and accuracy of laterality, a laterality application (Recognise™-noigroup.com) was be used for the foot. For testing, patients started a test of alternating foot images with no cofounding background or texture (vanilla feet) for 60 seconds. The program automatically tracked and reported on the speed and accuracy of the test. In line with previous laterality studies [33], two tests were completed by the patient and the mean score used as their final measure. Normative data for accuracy has been reported as > 80% and recognition speed of 2 seconds / image with a standard deviation of 0.5 [34].
Procedure
New patients attending PT with lower extremity pain (knee, ankle and foot) were recruited for the study. Patients were provided with an explanation of the purpose of the study and informed their participation is entirely voluntary. If patients agreed, they were provided a demographic survey to complete and then participated in laterality testing using a tablet with the Recognise™ foot module pre-loaded. Upon completion of each of the two tests, the results were entered onto the paper demographic sheets to ensure demographic data coincide with the relevant patients. Upon completion of data collection, data was entered manually into a Microsoft Excel™ spreadsheet for data analysis by an independent statistician.
Analysis
Microsoft Excel™ was used to enter data into spreadsheets and explore summary statistics such as counts, means, ranges, and percentages. RStudio Cloud version 1.4 of RStudio IDE was used in analysis what variables lead to a “yes” response as to whether the patient scored overall abnormality. Height and weight were originally recorded in foot-inches and pounds. These values were converted to meters and kilograms, then used to calculate each patient’s body-mass index. Variables recorded as factors with more than two levels were converted into binary variables indicating whether the patient answered “yes” to the variable in question. Additionally, not applicable values were replaced with the mean variable value for numeric variable types, and the most occurring value for factor variable types (binary). Finally, binary variables were converted to factors while remaining observations were kept numeric. Logistic regression was used in determining what variables were the best predictors of overall abnormality. Bayesian Information Criteria was used in determining the lowestscoring model to find what best predicted overall abnormality. Post-hoc power analysis was used to determine the replicability of the findings and showed a high level of power near 1 with df = 36.
Results
Patients

Forty patients attending outpatient PT for lower extremity pain participated in the study (Table 1). The mean pain rating was 4.4 on the numeric pain rating scale, with a mean duration of pain 8.32 months.
Laterality
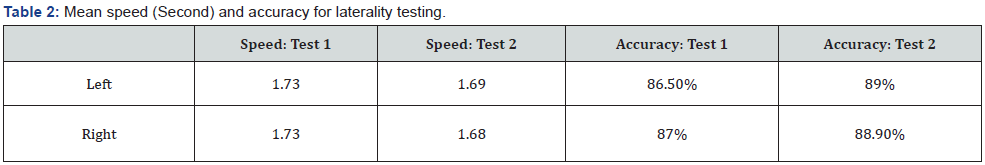
Fourteen patients (35%) recorded a score on the laterality test considered as abnormal (> 2.5 seconds per image and/or accuracy less than 80%). Mean speed and accuracy are found in Table 2. Five patients scored abnormal on speed which was also (100%) accompanied by an abnormal accuracy score for those patients. Nine patients scored abnormal on the accuracy test but not abnormal on the speed test. Logistic regression revealed that only age and gender were associated with abnormal laterality scores. Older age (ß =0.05, Pr = 0.06) and being female (ß =1.52, Pr =0.06) was associated with a higher likelihood of scoring an abnormal laterality test.
Discussion
This is the first study exploring the prevalence of laterality deficits in patients attending outpatient PT for lower extremity pain and /or dysfunction. The results from this study show that laterality deficits are prevalent in one in three patients attending outpatient PT in this study population. GMI, which aims to target cortical changes in the brain associated with pain, has primarily been studied in phantom limb pain and complex regional pain syndrome [18,19,35]. Both these clinical presentations, however, are quite rare [18,19,35]. In recent years, studies started showcasing more and more clinical presentations associated with disturbed body schema, including chronic low back pain, obesity, aging, immobilization and more [36-38]. These studies, however, did not look into the prevalence of these distortions, but rather the presence of altered body schema. The results from this current study are surprising, as it indicates one in three patients attending outpatient PT for a lower extremity injury has some deficit in terms of laterality testing, be it accuracy or speed. This finding is clinically important, as clinicians often view body schema alterations as very rare events confined to a small percentage of patients only presenting with complex pain states such as complex regional pain syndrome or phantom limb pain. In this study, focusing on lower extremity injuries, common conditions such as knee pain, ankle sprain, foot pain and knee replacement presented with laterality deficits. In the US alone over 5 million knee replacements are performed annually [39,40], with many of those patients attending outpatient PT [41]. These results would indicate that laterality deficits, possibly indicative of altered body schema maps, is far more prevalent and can be a significant factor in the initiation and/or maintenance of a pain state in patients attending outpatient PT.
Previous studies have implicated that the presence and intensity of pain, as well as immobilization with a cast or brace is associated with cortical map changes and possibly initiate or maintain a pain state [4,37,42]. In this study, however, this was not found to be the case. Even though this is a small sample size of patients, the presence of pain, intensity of pain, duration of pain, history of undergoing surgery, body mass index, using an assistive device and having been immobilized did not correlate with a poorer laterality test. Older age was associated with poorer laterality scores, which concurs with previous research tying aging to altered body schema [37]. Although pregnancy has been tied to body schema changes [36], gender as a stand-alone has not previously been implicated in altered body schema, warranting further examination.
The study contains various limitations. First, the sample size is small and larger studies will be needed to extrapolate on the findings. This study focused on lower extremity injuries (knee, ankle and foot) and prevalence for other laterality deficits in PT are unknown, thus cautioning extrapolation of these findings. Laterality is only one clinical measure associated with proposed cortical map changes. Other tests should be done to correlate laterality findings with these tests, including twopoint discrimination, localization and even more advanced brain imaging studies. This study, similar to current neuroscience research, infer laterality deficits are associated with cortical body map schema alterations, but future studies will need to be done to strengthen this correlation. Finally, the presence of laterality deficits does not provide information of prognosis or treatment, which must be further explored.
Conclusion
Laterality deficits associated with altered body schema is very common, presenting in one of three patients attending outpatient PT with lower extremity injuries. Older patients and patients identifying as female were more likely to present with an abnormal laterality measurement in PT for a lower extremity injury. Future, larger scale studies are needed to expand on this research including prevalence of other pain states attending outpatient PT and other predictive variables.
References
- Moseley GL (2007) Reconceptualising pain acording to modern pain sciences. Physical Therapy Reviews 12(3): 169-178.
- Gifford LS (1998) Pain, the tissues, and the nervous system. Physiotherapy 84(1): 27-36.
- Lotze M and GL Moseley (2007) Role of distorted body image in pain. Curr Rheumatol Rep 9(6): 488-496.
- Moseley GL, L Gallagher and A Gallace (2012) Neglect-like tactile dysfunction in chronic back pain. Neurology 79(4): 327-332.
- Wand BM (2011) Cortical changes in chronic low back pain: current state of the art and implications for clinical practice. Manual therapy 16(1): 15-20.
- Penfield W and E Boldrey (1937) Somatic, motor and sensory representation in the cerebral cortex of man as studied by electrical stimulation. Brain 60(4): 389-443.
- Flor H (2000) The functional organization of the brain in chronic pain, in Progress in Brain Research. J Sandkühler, B Bromm, and GF Gebhart. Elsevier, Netherlands.
- Stavrinou ML (2007) Temporal dynamics of plastic changes in human primary somatosensory cortex after finger webbing. Cereb Cortex 17(9): 2134-2142.
- Holmes NP and C Spence (2004) The body schema and the multisensory representation(s) of peripersonal space. Cogn Process 5(2): 94-105.
- Flor H (1997) Extensive reorganisation of primary somatosensory cortex in chronic back pain patients. Neurosci Lett 244(1): 5-8.
- Maihofner C (2003) Patterns of cortical reorganization in complex regional pain syndrome. Neurology 61(12): 1707-1715.
- Moseley GL (2008) I can't find it! Distorted body image and tactile dysfunction in patients with chronic back pain. Pain 140(1): 239-243.
- Moseley GL (2005) Distorted body image in complex regional pain syndrome. Neurology 65(5): 773.
- Flor H, T Elbert, W Mühlnickel, C Pantev, C Wienbruch et al. (1998) Cortical reorganisation and phantom phenomena in congenital and traumatic upper-extremity amputees. Exp Brain Res 119(2): 205-212.
- Louw A (2015) Immediate effects of sensory discrimination for chronic low back pain: a case series. New Zealand Journal of Physiotherapy p: 60-65.
- Louw A (2017) The effect of manual therapy and neuroplasticity education on chronic low back pain: a randomized clinical trial. J Man Manip Ther 25(5): 227-234.
- O'Neill M (2021) A Case-Series of Dry Needling as an Immediate Sensory Integration Intervention. J Man Manip Ther13: 1-7.
- Marinus J (2011) Clinical features and pathophysiology of complex regional pain syndrome. Lancet Neurol 10(7): 637-648.
- Giummarra MJ, GL Moseley (2011) Phantom limb pain and bodily awareness: current concepts and future directions. Curr opin anaesthesiol 24(5): 524-31.
- Lloyd D (2008) Differences in low back pain behavior are reflected in the cerebral response to tactile stimulation of the lower back. Spine 33(12): 1372-1377.
- Beggs S (2010) Peripheral nerve injury and TRPV1-expressing primary afferent C-fibers cause opening of the blood-brain barrier. Mol pain 6: 74.
- Flor H (1997) Extensive reorganization of primary somatosensory cortex in chronic back pain patients. Neurosci Lett 224(1): 5-8.
- Zimney K (2020) Comparison of reliability and efficiency of two modified two-point discrimination tests and two-point estimation tactile acuity test. Physiother Theory Pract 38(1): 235-244.
- Catley MJ (2013) Assessing tactile acuity in rheumatology and musculoskeletal medicine--how reliable are two-point discrimination tests at the neck, hand, back and foot? Rheumatology 52(8): 1454-1461.
- Elsig S (2014) Sensorimotor tests, such as movement control and laterality judgment accuracy, in persons with recurrent neck pain and controls. A case-control study. Manual Therapy 19(6): 555-561.
- Moseley GL (2004) Why do people with complex regional pain syndrome take longer to recognize their affected hand? Neurology 62(12): 2182-2186.
- Moseley GL (2005) Experimental hand pain delays recognition of the contralateral hand--evidence that acute and chronic pain have opposite effects on information processing? Brain Res Cogn Brain Res 25(1): 188-194.
- Shepherd M, Louw A, Podolak J (2020) The clinical application of pain neuroscience, graded motor imagery, and graded activity with complex regional pain syndrome-A case report. Physiother Theory Pract 36(9): 1043-1055.
- Moseley GL (2006) Graded motor imagery for pathologic pain. Neurology 67(12): 2129-2136.
- Daly AE, AE Bialocerkowski (2009) Does evidence support physiotherapy management of adult Complex Regional Pain Syndrome Type One? A systematic review. Eur J Pain 13(4): 339-353.
- Louw AR, A Mendoza G, Kassal F, Brennan J, Louw H, et al. (2011) Depression and patients attending outpatient physical therapy with musculoskeletal pain and disability. MOJ Orthop Rheumatol 13(6): 126-129.
- Louw A, HD Weber B, Shuda D, Obert C, Louw H, et al. (2021) Central Sensitization in Patients Attending Physical Therapy for Musculoskeletal Disorders. Phys Med Rehabil Int.
- Zimney KJ (2018) The reliability of card-based and tablet-based left/right judgment measurements. Musculoskelet Sci Pract 33: 105-109.
- Moseley GL (2012) The Graded Motor Imagery Handbook. Adelaide Noigroup Publications.
- Goh EL, S Chidambaram, D Ma (2017) Complex regional pain syndrome: a recent update. Burns trauma 5(1): 2.
- Beales D (2016) Disturbed body perception, reduced sleep, and kinesiophobia in subjects with pregnancy-related persistent lumbopelvic pain and moderate levels of disability: An exploratory study. Man Ther 21: 69-75.
- Falling C, R Mani (2016) Ageing and obesity indices influences the tactile acuity of the low back regions: A cross-sectional study. Man Ther 23: 25-31.
- Meugnot A, Y Almecija, L Toussaint (2017) The embodied nature of motor imagery processes highlighted by short-term limb immobilization. Exp Psychol 61(3): 180-186.
- Maradit Kremers H (2015) Prevalence of Total Hip and Knee Replacement in the United States. J Bone Joint Surg Am 97(17): 1386-1397.
- Singh JA (2019) Rates of Total Joint Replacement in the United States: Future Projections to 2020-2040 Using the National Inpatient Sample. J Rheumatol 46(9): 1134-1140.
- Han AS (2015) Early rehabilitation after total knee replacement surgery: a multicenter, noninferiority, randomized clinical trial comparing a home exercise program with usual outpatient care. Arthritis Care Res (Hoboken) 67(2): 196-202.
- Moseley GL (2014) Intense pain soon after wrist fracture strongly predicts who will develop complex regional pain syndrome: prospective cohort study. J Pain 15(1): 16-23.






























