Study of Mental Health and Job Burnout and its Relationship with Musculoskeletal Discomfort in the Staff of Cardiology
Pedram Sadoug H Moghanlu1, Shahnaz Tabatabaei2*, Isa Khaheshi3 and Mohamad Hossein Vaziri4
1Master of Science, Shahid Beheshti University of Medical Sciences, Iran
2Department of Ergonomics, Shahid Beheshti University of Medical Sciences, Iran
3Department of Cardiovascular Research Center, Shahid Beheshti University of Medical Sciences, Iran
4School of Public Health and Safety, Shahid Beheshti University of Medical Sciences, Iran
Submission: October 18, 2021; Published: November 17, 2021
*Corresponding author: Shahnaz Tabatabaei, Department of Ergonomics, Shahid Beheshti University of Medical Sciences, Iran
How to cite this article: Pedram S H M, Shahnaz T, Isa K, Mohamad H V. Study of Mental Health and Job Burnout and its Relationship with Musculoskeletal Discomfort in the Staff of Cardiology. J Yoga & Physio. 2021; 9(2): 555756. DOI:10.19080/JYP.2021.09.555756
Abstract
Background: Cardiovascular diseases (CVD) in particular, are coronary complications which cause high numbers of mortality each year. A common intervention technique for these complications is catheterization (angiography). Professionals involved in this technique are exposed to uncomfortable postures, long working hours, and stress, which may result in severe mental health conditions and job burnout. This research aims to study mental health and job burnout and its relationship with musculoskeletal discomfort in the staff of cardiology department, and whether this effect is specific to any working group.
Methods: This case-control study was implemented on a convenience sample of 120 out of 150 physicians and nurses in the cardiology department. The sample group was divided into two groups: those who were working in the Cath lab were selected as case (interventional), and those who were employees in the heart surgery and CCU units were considered as control (non-interventional). Data were collected through a demographic survey, the Nordic Musculoskeletal Questionnaire (NMQ), General Health Questionnaire (GHQ-28), and Maslach Burnout Inventory (MBI-HSS).
Results: Results show that mental health of the staff who reported ankle pain (p=.007) was lower than other groups, and it was significant in control (non-interventional) group (p=.013). Emotional Exhaustion and pain in the ankle (p=.002), Depersonalization and pain in the lower back (p=.001) and the shoulders (p=.032) were found to be significant to non-interventional staff.
Conclusion: It can be concluded that pain in certain body regions of the staff is associated with lower mental health and higher job burnout. In addition, the musculoskeletal symptoms in the ankle of non-interventional group can be a signal for higher possibility of lower mental health and stressful job life, which may qualify them for in-depth psychological and medical interventions.
Keywords: Mental health; Job burnout; Cardiology staff; Musculoskeletal discomfort
Abbreviations: CVD: Cardiovascular Diseases; NMQ: Nordic Musculoskeletal Questionnaire; GHQ: General Health Questionnaire; MBI-HSS: Maslach Burnout Inventory; IP: Interventionalist Professionals; NP: Non-Interventionalists Professionals; PA: Personal Accomplishment; EE: Emotional Exhaustion; DP: Depersonalization
Introduction
Currently cardiovascular diseases are among the most common causes of mortality worldwide. In fact, in the United States alone, 1 in 8.6 death certificates is related to heart diseases and 1 in 6 deaths caused by cardiovascular failures, links to coronary artery disease [1]. Although an official statistic regarding the CVD mortality in Iran is not available, the literature report a 20-45 percent increase in heart-related health conditions [2]. Angiography and Interventional cardiology are common methods to diagnose and manage coronary problems [3]. In modern angiography, due to substantial demand for these procedures hence increased work rate, interventionalist and interventional (Cath lab) staff are exposed to ionizing X-ray radiation, awkward postures and long working hours, while wearing heavy lead aprons and protective shields [4,5]. Several studies hinted at a higher prevalence of musculoskeletal pain among Cath lab specialists and staff [4,6,7]. This makes interventional cardiologists potentially vulnerable to psychological distress which in turn can lead to lower mental health and eventually job burnout. Healthcare providers and most importantly physicians are prone to higher risk of depression and suicidal tendencies comparing to other occupations that indicates their mental health is at risk [8-10]. They are constantly confronted by challenging situations, such as death, pain, patient’s emotional problems and long-term bedridden patients who survive under burdensome treatment methods which have negative impact on healthcare professional’s mental health [11]. The increased job demands besides stressful situations gradually impact on feelings of satisfaction and ultimately may result to job burnout [12,13]. Job burnout can be defined as long-term distress arising from emotional pressure in interpersonal relations at workplace [14]. While burnout occur in almost all occupations, its prevalence in physicians and healthcare professionals is higher comparing to other groups [15]. The most common symptoms at the workplace are objectifying patients or colleagues, diminishing emotional resources, health problems and lack of social support [16,17]. Job burnout has been strongly related to lower overall health, poorer quality of services, sleep problems, substance, and alcohol addiction and work absenteeism [14,18].
The relationship between musculoskeletal disorders and mental health and job burnout factors has been investigated by numerous studies. However, no studies have examined and discussed this relationship between these main variables and whether there are some differences between two groups (interventional and non- interventional) of Cath lab and Heart surgery/Intensive Care Unit regarding their physical and mental health at workplace. Finding the difference between two types of professional groups is the main and innovative idea of this research. The aim of the study is first to determine the prevalence of musculoskeletal symptoms, mental health and job burnout in both groups of Cath lab and Heart surgery/intensive care unit. Then, it compares two groups of interventional (Cath lab) and non-interventional (Heart surgery and intensive care unit) professionals with respect to their musculoskeletal discomfort, mental health and job burnout.
Materials and Methods
Study design
This case-control study was performed on the specialists and nurses in Shahid Modarres Hospital, in which, those working in Cath lab were selected as case (interventionalists) and those active in heart surgery and CCU units were considered as (noninterventional) as control group. Wearing protective lead aprons were considered as the attribute and musculoskeletal pains, mental health status and job burnout level as the outcome. The participants were chosen by convenience sampling from the current workforce at the hospital. Inclusion criteria for case group were continuous use of protective lead aprons, not currently suffering from pre-existing occupational musculoskeletal disorders, not using long-term prescribed sedatives or similar tranquilizers, and at least 2 years of work experience.
Data collection
Data were collected through anonymous self-administered questionnaires. Data collection ran from 20th February until 11th May 2017. Prior to delivering the questionnaires, general information and instructions were explained to the volunteer respondents by the researchers. No identifiable information was collected, and the staff were free to decline. Moreover, approval of Shahid Beheshti University of Medical Sciences’ Ethics Committee was obtained (approval code: IR. SBMU.RETECH.1396.200). The questionnaire bundle was divided into four parts:
a) Part one entailed demographic information such as age, weight, height, gender, education level, work experience in this occupation, job title, daily work hours, psychoactive drug usage, and any previous accident that had incurred musculoskeletal damage.
b) The second part included the Nordic Musculoskeletal Questionnaire (NMQ) [19]. In this questionnaire, pain, discomfort, or numbness in 9 anatomical regions. The respondent ticks a yesno style box against each section corresponding to an anatomical region.
c) Part three utilized General Health Questionnaire (GHQ) [20] Farsi version [21] to determine the overall perception of mental health of staff. In this study, the 28-item version (GHQ-28) was utilized in this study.
d) Part four consisted of Maslach Burnout Inventory- Human Services Survey (MBI-HSS) [22]. This tool helped to measure the burnout level among physicians and nurses in this center. MBI-HSS assesses 3 scopes (subscales) of job burnout on a 7-point Likert scale, by providing 22 items: emotional exhaustion (9 items); depersonalization (5 items); and personal accomplishment (8 items).
Statistical analysis
Demographic data were analyzed by descriptive statistics. The data from all questionnaires were converted to a 1 to 100-point scale, and Kolmogorov–Smirnov test was utilized to confirm normal distribution and lastly, Levene’s test cleared the samples for having equal variances. Student t-test was performed to compare the means of variables. Data were analyzed in SPSS software (V: 19.0, IBM Inc. Armonk, NY). Any p value below .05 was considered as statistically significant.
Results
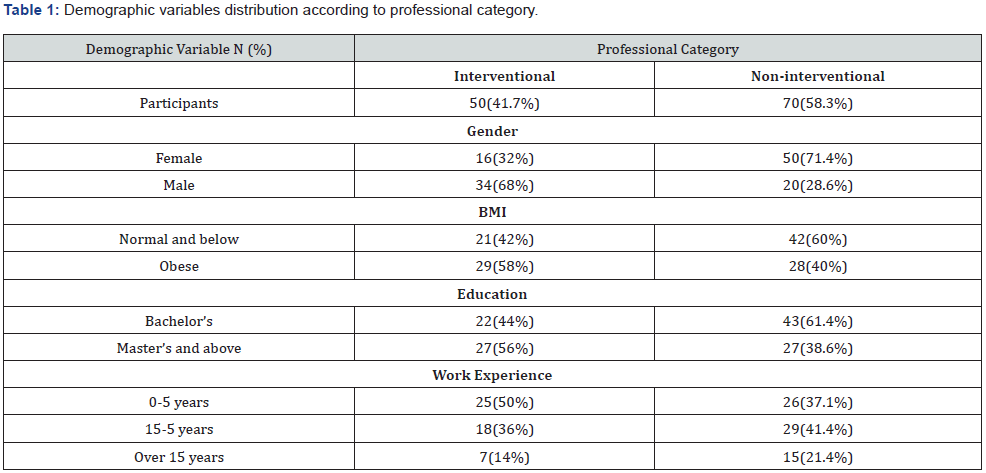
Of 150 questionnaires distributed, 120 were qualified for a final data process which indicates a 70% participation rate. The case group (interventionalist professionals (IP)) comprised of 28 specialists and 22 nurses (50) while 19 specialists and 51 nurses returned the questionnaires in the control group (noninterventionalists professionals (NP)). The Socio-demographic features of the respective categories are displayed in Table 1.
Mental health and musculoskeletal disorders
To examine the relationship between musculoskeletal symptoms prevalence and mental health scores obtained from GHQ-28, we first evaluated the relationship in each body region for both groups, then in case of significant relationship in a body region, separate comparison was performed between IP and NP groups.
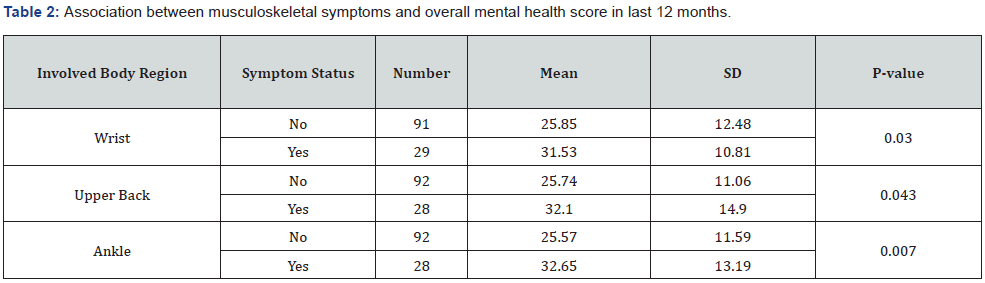
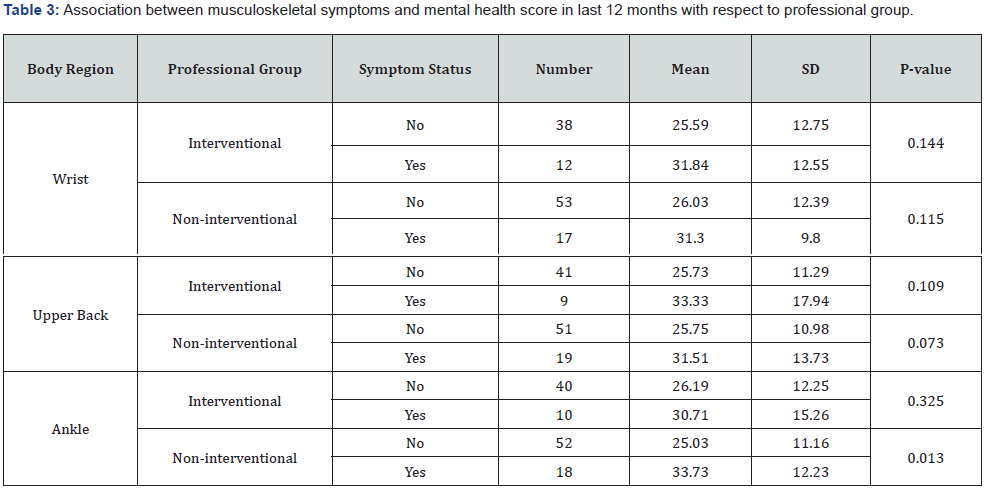
As it is illustrated in Table 2, Student t-test with .05 significance level revealed that mental health score in subjects who have reported a pain in wrist (p=.030), upper back (p=.043), and ankle (p=.007) regions, is higher than those did not. To further elaborate on the differences in mental health score with respect to the professional group, we examined the wrist, upper back and ankle regions to figure out whether this effect is exclusive to any job groups. Table 3 shows that pain and discomfort in the ankle (p=.013) of non-interventional professionals is associated with higher GHQ-28 score, hence with lower perception of mental health.
Musculoskeletal symptoms and burnout syndrome
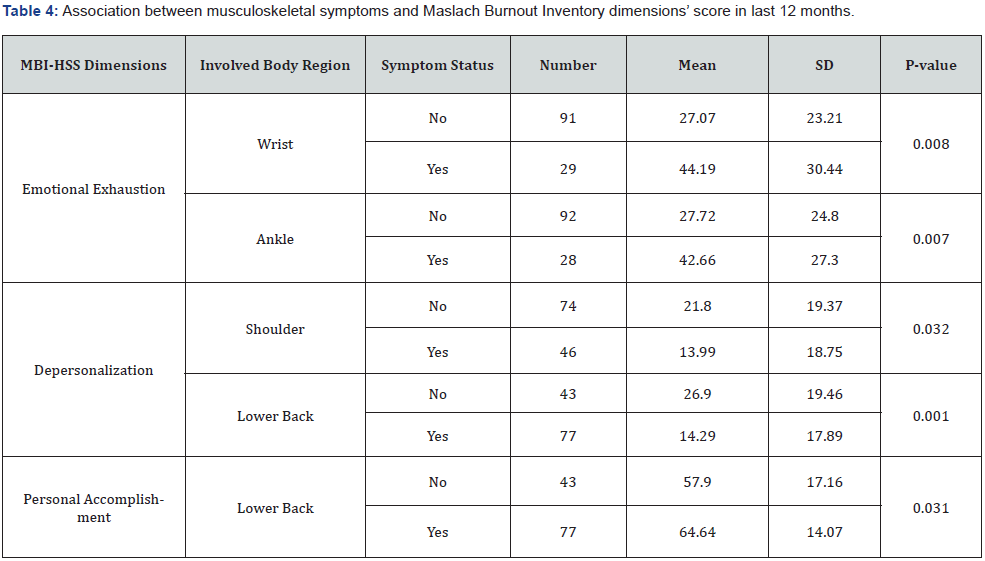
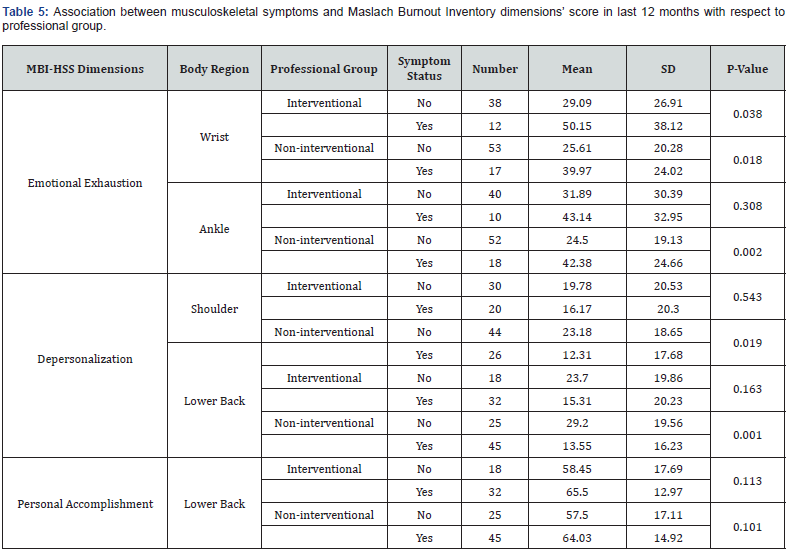
To inquire possible relationship between musculoskeletal discomforts and job burnout using MBI-HSS, we utilized t-test, linking each dimension to results from NMQ. Emotional Exhaustion (EE) dimension scores were closely associated with symptoms in wrist (p=.008) and ankle (p=.007). To find out whether this link is specific to any of the two professional groups, another t-test was utilized. The symptoms in wrist are relevant in both categories (interventional group: p=.038; non-interventional group: p=.018), while EE scores and pain in the ankle was exclusively related to working as non-interventional personnel (p=.002 vs p=.308). The same analysis was performed for Depersonalization (DP) scores. Here, pain in the shoulder (p=.032) and lower back (p=.001) were associated with Depersonalization. The following analysis revealed that only in non-interventional group the relationship is statistically significant (shoulder: p=.019 vs p=.543; lower back: p=.001 vs p=.163). Lastly, lower scores in Personal Accomplishment (PA) dimension was related to discomfort in the lower back (p=.031). No professional group showed specificity in this regard. Table 4 & 5 displays the results of the analysis for musculoskeletal symptoms and their relationship with MBI-HSS dimensions.
Discussion
Previous studies suggest higher levels of musculoskeletal discomfort and pain among Interventional cardiology staff. These studies mostly identified the problem as wearing heavy lead protective shields, awkward postures and long working hours [4,6,23]. Having this in mind, authors of this study aimed to 1) determine a possible effect of musculoskeletal symptoms on mental health and job burnout on Interventional and non- Interventional staff in cardiology department and to 2) present the difference between the two groups. The results showed that a personnel’s overall mental health and her job burnout level, relate to the level of musculoskeletal discomfort that she is experiencing. In a similar study, Melamed introduced job burnout as a predictive factor for pain in the neck/shoulder and low back [24]. In the present paper, we found that the pain in wrist, upper back and ankle is inversely linked to lower mental health, and pain in the ankle is the sole body region that is specific to working in non-interventional setting. The most probable explanation for this observation can be inferred from prolonged standing and continuous circulation while performing their tasks. Furthermore, non-intervention staff relatively suffered more from psychosomatic symptoms and stress which aggravates the ongoing pain. Orme et al. conducted a survey comparing cardiology department personnel that were involved in interventional cardiology procedures and those who were not in respect to occupational hazards associated with this method [7]. They found that the musculoskeletal pain was more common among interventional staff compared to non-interventional group. This contrasts with our findings, and we attribute this variance to smaller size of IP sample. Similarly, Emotional Exhaustion dimension of job burnout is associated with pain in the ankle and is exclusively linked to working as a non-intervention personnel. Due to their constant confrontation with ailing patients and their emotionally under pressure families, heavy workload, patient handling [25] besides standing for hours, nurses and physicians working in such environment feel amplified pain in their ankles. Considering mental health and job burnout scores and their close link with the ankle pain among non-intervention group, we claim that working conditions and demands in non-interventional section of cardiology department is an important factor in developing musculoskeletal disorder in the ankle region of the staff.
The relationship between pain in the shoulder and lower back and Depersonalization was another important finding of the present study. Interestingly, the results were again significant for non-interventional group. In a review article by Costa et al., it was revealed that heavy physical workload and psychosocial factors are among the most important risk factors for pain in the shoulder and lower back [26]. Looking to the stressful nature work life in heart surgery and post-operative care, the professionals in this section dealing with more physical, psychological and social pressures compared to their peers in the catheterization laboratory. The pain in lower back part of the body was associated with high degree of Depersonalization and low Personal Accomplishment. The results partly agree with what d’Errico et al. [27] found in their study about low back pain and its association with presenteeism in nurses. They found that good working climate and procedural justice reduces the risk of low back pain. In a study by Elfering et al. [28] it was shown that emotional demands and level of appreciation can be a good predictor of low back pain in home care nurses. Numerous studies have explored the links between individual characteristics and job burnout in nursing. Canadas-De la Fuente et al. [29] by examining the job burnout level in nursing occupation, has found that neuroticism, extroversion and job commitment are directly correlated to Depersonalization and Personal Accomplishment. Moreover, in a study by Embriaco et al. [30] among critical care nurses, organizational factors were introduced as the most important factor in high prevalence of job burnout among the nurses. Despite this, because of on-site restrictions, we were unable to survey the subjects regarding the individual characteristics, personal life (e.g. family-work confliction) and organizational factors. Future studies should include these factors in their research to inspect the underlying factors more clearly among cardiology department professionals. Even though recent studies hint to prominent role of sleep quality and shifting in health of nursing staff [31,32], to equalize comparison factors in both groups (as interventional group did not work on out of day hours), we did not take non-day shifts and their effects on musculoskeletal and mental health of the staff into account.
Conclusion
The aim of this study was to examine any possible connection between musculoskeletal discomfort and psychological among cardiology department staff. The results hint that prevalence of symptoms in certain regions of the body is closely related to the level of mental health and job burnout. We also found that despite our initial beliefs, it was non-interventional group that demonstrates a significant relationship between musculoskeletal symptoms and mental health status. Most importantly, ankle and mental health and dimensions of Depersonalization and Emotional Exhaustion of job burnout were specifically related with professionals in non-interventional. Hence, it is recommended to consider the prevalence of pain and discomfort symptoms in ankle, as an important indicator of wider psychosocial implications in non-interventional section of cardiology departments.
References
- Lloyd-Jones D, Adams RJ, Brown TM, Mercedes C, Shifan D, et al. (2010) Executive summary: heart disease and stroke statistics-2010 update: A report from the American heart association Circulation 121(7): 948-954.
- Maleki F, Sayehmiri F, Kiani F (2014) Metabolic syndrome prevalence in Iran: a systematic review and meta-analysis. J Kermanshah Univ Med Sci 18: 242-250.
- Lakhan SE, Kaplan A, Laird C (2009) The interventionalism of medicine: Interventional radiology, cardiology, and neuroradiology. Int Arch Med 2(1): 27.
- Goldstein JA, Balter S, Cowley M, John H, Lloyd W K (2004) Occupational hazards of interventional cardiologists: Prevalence of orthopedic health problems in contemporary practice. Catheter. Cardiovasc Interv 63(4): 407-411.
- Smilowitz NR, Balter S, Weisz G (2013) Occupational hazards of interventional cardiology. Cardiovasc Revascularization Med 14(4): 223-228.
- Ross AM, Segal J, Borenstein D, E Jenkins, S Cho (1997) Prevalence of Spinal Disc Disease Among Interventional Cardiologists. Am J Cardiol 79(1): 68-70.
- Orme NM, Rihal CS, Gulati R, David Rh, Ryan JL, et al. (2015) Occupational health hazards of working in the interventional laboratory: A multisite case control study of physicians and allied staff. J Am Coll Cardiol 65(8): 820-826.
- Center C, Davis M, Detre T, Daniel EF, Wendy H, et al. (2003) Confronting depression and suicide in physicians: A consensus statement. JAMA 289(23): 3161-3166.
- ML Goldman, Ravi NS, Carol AB (2015) Depression and suicide among physician trainees: Recommendations for a national response. JAMA Psychiatry 72(5): 411-412.
- Adler NR, Adler KA, Grant Kels JM (2017) Doctors’ mental health, burnout, and suicidality: Professional and ethical issues in the workplace. J Am Acad Dermatol 77(6): 1191-1193.
- Ferrand E, Robert R, Ingrand P (2001) Withholding and withdrawal of life support in intensive-care units in France: a prospective survey. Lancet 357(9249): 9-14.
- Van Mol MMC, Nijkamp MD, Bakker J (2018) Counterbalancing work-related stress? Work engagement among intensive care professionals. Aust Crit Care 31(4): 234-241.
- Rayan A, Sisan M, Baker O (2019) Stress, Workplace Violence, and Burnout in Nurses Working in King Abdullah Medical City During Al-Hajj Season. J Nurs Res 27(3): e26.
- Ribeiro VF, Filho C, Valenti VE, Marcelo F, Luiz CA, et al. (2014) Prevalence of burnout syndrome in clinical nurses at a hospital of excellence. Int Arch Med 7: 22.
- Ramirez AJ, Graham J, Richards MA (1996) Mental health of hospital consultants: the effects of stress and satisfaction at work. Lancet 347(9003): 727-728.
- Meltzer LS, Huckabay LM (2004) Critical Care Nurses’ Perceptions of Futile Care and its Effect on Burnout. Am J Crit 13(3): 202-208.
- Arora M, Asha S, Chinnappa J,Ashish DD (2013) Review article: Burnout in emergency medicine physicians. Emerg Med Australas 25(6): 491-495.
- Leiter MP (1997) The truth about burnout. How Organizations Cause Personal Stress and What to do about It. San Francisco, US.
- Kuorinka I, Jonsson B, Kilbom A (1987) Standardised Nordic questionnaires for the analysis of musculoskeletal symptoms. Appl Ergon 18(3): 233-237.
- Goldberg DP (1972) The detection of psychiatric illness by questionnaire: A technique for the identification and assessment of non-psychotic psychiatric illness. Oxford University Press, New York, USA.
- Rasouli Z, Tabatabaei S (2018) The Reliability and validity of Persian Version of the General Health Questionnaire (CHQ-60) in Industry Staff. Iran Occup Heal 15: 44-54.
- Maslach C, Jackson S (1981) The measurement of experienced Burnout. J Occup Behav 2(2): 99-113.
- Andreassi MG, Piccaluga E, Guagliumi G, Maurizio DG, Fiorenzo G, et al. (2016) Occupational health risks in cardiac catheterization laboratory workers. Circ Cardiovasc Interv 9(4): 1-9.
- Melamed S (2009) Burnout and risk of regional musculoskeletal pain - a prospective study of apparently healthy employed adults. 25(4): 313-321.
- Akbari H, Akbari H, Abadi MBH, Gholami FM, Ghasemi M, et al. (2017) Assessing the risk of manual handling of patients and its relationship with the prevalence of musculoskeletal disorders among nursing staff: performance evaluation of the MAPO And PTAI methods. Iran. Red Crescent Med J 19(2).
- Costa BR, Vieira ER, da Costa BR (2010) Risk factors for work-related musculoskeletal disorders: A systematic review of recent longitudinal studies. Am J Ind Med 53(3): 285-323.
- D Errico A, Viotti S, Baratti A, Bianca M, Anna PB, et al. (2013) Low Back Pain and Associated Presenteeism among Hospital Nursing Staff. J. Occup Health 55(4): 276-283.
- Elfering A, Häfliger E, Celik Z, Simone G (2018) Lower back pain in nurses working in home care: linked to work–family conflict, emotional dissonance, and appreciation? Psychol Health Med 23(6): 733-740.
- Canadas De la FGA, Vargas C, San Luis CC, Inmaculada G, Gustavo RC, et al. (2015) Risk factors and prevalence of burnout syndrome in the nursing profession. Int J Nurs Stud 52(1): 240-249.
- Embriaco N, Papazian L, Kentish BN, Frederic P, Elie A, et al. (2007) Burnout syndrome among critical care healthcare workers. Curr Opin Crit Care 13(5): 482-488.
- Lee CY, Chen HC, Meg TMC, Hsin CL, Lian HH, et al. (2015) The relationships among sleep quality and chronotype, emotional disturbance, and insomnia vulnerability in shift nurses. J Nurs Res 23(3): 225-235.
- Bazazan A, Dianat I, Bahrampour S, Amirhosein T, Hojat Z, et al. (2019) Association of musculoskeletal disorders and workload with work schedule and job satisfaction among emergency nurses. Int Emerg Nurs 44: 8-13.






























