Examining the Psychometric Properties of the Bladder Cancer Needs Assessment Survey
Tung-Ming Leung1, Emma K T Benn2, Matthew Galsky3, David M Latini4, Heather H Goltz5, Cheryl T Lee6, Diane Z Quale7, Bente T Jensen8, Afaf Girgis9, Barbara A Given10 and Nihal E Mohamed1*
1Department of Urology and Oncological Science, Icahn School of Medicine at Mount Sinai, USA
2Center for Biostatistics and Department of Population Health Science and Policy, Icahn School of Medicine at Mount Sinai, USA
3Department of Medicine, Hematology and Medical Oncology, Icahn School of Medicine at Mount Sinai, USA
4Department of Urology, Baylor College of Medicine, USA
5Section of Infectious Diseases, Baylor College of Medicine, USA
6Department of Urology, Ohio State University, USA
7Bladder Cancer Advocacy Network, Bethesda, USA
8Department of Urology, Aarhus University Hospital, Denmark
9Centre for Oncology Education and Research Translation (CONCERT), Ingham Institute for Applied Medical Research, South Western Sydney Clinical School, University of New South Wales, Sydney, Australia
10College of Nursing, Michigan State University, USA
Submission: July 28, 2017; Published: August 28, 2017
*Corresponding author: Nihal E Mohamed, Department of Urology, Icahn School of Medicine at Mount Sinai, USA, Tel: 212-241-8858; Fax: 212-876-3246; Email: nihal.mohamed@mountsinai.org
How to cite this article: Tung-Ming L, Emma K T B, Matthew G, David M L, Heather H G. Examining the Psychometric Properties of the Bladder Cancer Needs Assessment Survey. JOJ uro & nephron. 2017; 4(1): 555627. DOI: 10.19080/JOJUN.2017.04.555627
Abstract
Understanding the types and magnitudes of bladder cancer (BC) survivors’ unmet needs and their associated factors is critical to optimizing health care planning for newly diagnosed patients. Unfortunately, measures that assess BC patients’ specific needs are lacking. This study examined the psychometric properties of a new needs assessment survey (BCNAS-32) for BC patients that we developed to address this gap. The BCNAS-32 was based on expert opinion, in-depth interviews of BC survivors and informal caregivers, and literatures on BC outcomes and unmet needs. BC survivors (n=159) were recruited from the Bladder Cancer Advocacy Network (BCAN) to complete a questionnaire that included the BCNAS-32, the supportive care needs survey (SCNS-LF59), functional assessment of cancer therapy bladder cancer scale (FACT-BL), hospital anxiety and depression scale (HADS), coping (BRIEF COPE), social provisions scale (SPS),and general self-efficacy beliefs (GSE) scale. Internal consistency of the BCNAS-32 was examined using exploratory factor analysis, and convergent and discriminant validity analyses. Thirty-two of the 92 items developed were selected by exploratory factor analysis constituting 7 subscales (psychological, health system, physical and daily living, patient care and support, logistics, communication with providers, and communication with partners) with high internal consistency (α range:0.89-0.97)and for the total scale (α=0.94). There was strong evidence of convergent and discriminant validity of the BCNAS-32, as indicated by moderate-to-high correlations with SCNS-LF59 (r=0.90; p<0.001), HADS(r=-0.76; p<0.001), GSE (r=-0.60; p<0.001), SPS (r=-0.66; p<0.001), and Brief COPE scales (r=0.58, p<0.001). These findings suggest that the BCNAS-32 provides a reliable and valid index of BC patients’ needs.
Keywords: Bladder cancer; Unmet needs; Needs assessment; Validation; Quality of life; Radical cystectomy; Supportive care
Abbreviations: MIBC: Muscle Invasive Bladder Cancer; NMIBC: Non-Muscle Invasive Bladder Cancer; TURBT: Transurethral Resection of Bladder Tumor; NCCN; National Comprehensive Cancer Network; HIPPA: Health Insurance Portability and Accountability Act; SD: Standard Deviation; KMO: Kaiser-Meyer-Olkin; BC: Bladder Cancer; BCAN: Bladder Cancer Advocacy Network; SPS: Social Provisions Scale; GSE: General Self-Efficacy Beliefs
Introduction
Bladder Cancer (BC) is the fifth most commonly diagnosed cancer in the US [1,2]. Approximately 75% of BC patients present with non-muscle invasive bladder cancer (NMIBC) and 25% present with muscle invasive bladder cancer (MIBC) [1-3]. About one-tenth to one-quarter of NMIBC patients typically progress to MIBC [2,3]. Currently, the standard treatment for NMIBC is transurethral resection of bladder tumor (TURBT) with or without adjuvant intravesical therapy, whereas radical cystectomy and urinary diversion are generally employed to treat MIBC and high-risk NMIBC refractory to conservative therapy [4]. A tri-modal chemoradiation and orthotopic urinary diversion to mimic natural voiding patterns is used to improve health-related quality of life (HRQoL) [5]. Nonetheless, BC treatment, in general, negatively affects patients’ HRQoL, emotional well being, sexual function, and physical and social functioning [6-8].
Treatment burden for BC patients increases with treatment intensity. MIBC patients who receive cystectomy and urinary diversion have more more physical and psychological treatment burden than NMIBC patients who receive lessintensive treatment (e.g. endoscopic and intravesical therapies) due to the severity of treatment and the requirements for self-care (e.g., utility of stoma appliances and catheters). Research findings have revealed that MIBC patients report worse HRQoL, impaired body image, and difficulties in post-operative self-care than NMIBC patients [9-11]. Traditionally, in men, the prostate and seminal vesicles are removed with the bladder, while in women the urethra, reproductive organs, and anterior vagina are removed along with the bladder [12-16] which increases the physical and emotional impact of treatment on patients’ outcomes by further decreasing the sexual function and increasing negative views of self-image [17].
In spite of the profound effects of BC and its treatment on patients’ outcomes, no study has systematically examined the specific unmet needs of BC patients. Identifying the types and magnitudes of patients’ unmetneeds, as well as their associated factors is vital in providing necessary support to reducing treatment burden and to ultimately guiding design and evaluation of future psychosocial interventions. Personalized health care and clinical care pathways were recently developed to improve BC patients’ outcomes, with an increasing emphasis on HRQoL and psychosocial outcomes (e.g., distress, depression, and anxiety) [18]. To integrate the psychosocial approach into BC care, implementation of routine psychosocial screening for needs assessment is recommended by the National Comprehensive Cancer Network (NCCN) guidelines [19-25]. However, needs assessment measures that are sensitive to BC specific outcomes are lacking and the most commonly used BC patient outcome measures (e.g., HRQoL, distress, anxiety) are not designed to assess specific unmet needs or challenges patients encounter in health care (e.g., informational needs, needs for support, logistic challenges).
This study aims to evaluate the psychometric properties of a new needs assessment survey that we developed to examine the prevalence and intensity of BC patients’ unmet needs throughout their illness experience (i.e., from the time of diagnosis to survivorship). The BCNAS-32 was developed and refined based on expert opinion, in-depth interviews of BC survivors and informal caregivers (described in details in a previous publication) [17], an established theoretical framework (Self- Regulatory Theory; Illness Trajectory Model) [26-28], and input from urologists, ostomy nurses, psychologists, and the Bladder Cancer Advocacy Network.
Methods
Participants
A sample size of at least 50-100 is generally recommended for validation studies [29]. In 2014, a heterogeneous sample of 159 BC patients was recruited from BCAN to complete an online- questionnaire including BC specific needs assessment survey. The inclusion criteria restricted our sample to include BC patients who were English speakers, aged 18-85 years, and able and willing to provide informed consent. Patients who had metastatic disease, cancer recurrence, or other primary cancers at the time of assessment were excluded from the study. These exclusion criteria were selected with the rationale that these patients may have other current unmet needs that could potentially bias our study results by introducing additional factors not inherent to the MIBC and NMIBC experience.
The online questionnaire was designed using the Research Electronic Data Capture (REDCap) software which is a Health Insurance Portability and Accountability Act (HIPPA) approved browser-based software for designing clinical trial studies [30]. All participants read and signed an online consent form before accessing the questionnaire. The questionnaire assessed demographic and clinical characteristics of the study participants, the BC needs assessment survey we developed (BCNAS-32), and psychosocial and functional outcome measures to evaluate the convergent validity (SCNS-LF59) and discriminant validity of the bladder cancer needs assessment survey (FACT-BL, HADS, BRIEF COPE, SPS, and GSF).
Study Measures
The supportive care needs survey long-form (SCNSLF59)
The SCNS-LF59 was developed by The Supportive Care Review Group [31] to assess the care needs of cancer patients regarding specific themes during survivorship: namely psychological (22 items), health system (15 items), physical and daily living (7 items), patient care and support (8 items), sexuality (3 items), and other concerns (4 items). For each aspect, participants are asked to consider their level of need for help with a specific item by choosing one of the following response options: no need-not applicable; no need-already satisfied; low need; moderate need; or high need.
The instructions ask patients to identify needs they may have experienced in the last month as a result of having cancer. The reported face and content validity of this scale were found to be high. Internal reliability coefficients (Cronbach alpha) of all 5 factor-based scales were found to be substantial, ranging from 0.87 to 0.97.
The bladder cancer needs assessment survey (BCNAS-32)
The purpose of the BCNAS-32 was to provide a comprehensive assessment of the multi-dimensional impact of BC on patients’ physical, psychosocial, and functional outcomes and their current needs for support in multiple life areas including but not limited to health care, disease self-management, social support, finance, and logistics. Guided by our qualitative studies, literature reviews, and expert opinion we developed 92 items assessing different dimensions of needs related to individuals’ BC experience.
A priori estimates of BCNAS-32 scale constructs were based on the SCNS-LF59 original five constructs:
i. Psychologic (29 items)-assessing BC patients’ perceived needs for help with psychological and emotional issues, including support for BC related outcomes
ii. Health system and information(16 items)-including needs for information about BC treatment and outcomes, cancer progression and follow-up care
iii. Physical and daily living(8 items)-including needs related to coping with BC and treatment side effects, and challenges in daily living following treatment;
iv. Patient care and support (4 items)-including needs for compassionate health care support, understanding, privacy, and more health care choices; and
v. Sexuality (14 items)-including needs of support with sexual problems and sexual dysfunction. Additional items were developed to address two separate dimensions of patients’ unmet needs that emerged as significant issues during the patient interviews we conducted; 1) logistic needs (9 items) and 2) challenges in communication with providers and caregivers/social partners (12 items).
The functional assessment of cancer therapy - bladder cancer scale (FACT-BL)
The FACT-BL is a BC targeted quality of life instrument, incorporating five functional scales (physical, social/family, emotional, functional, and additional concerns). Items are scored on a 5-point Likert scale from 0 (‘not at all’) to 4 (‘very much’). Prior studies attest to the validity and reliability of data collected using this scale (Alpha: 0.77-0.94) [32].
The hospital anxiety and depression scale (HADS)
The HADS was developed to identify symptoms of anxiety and depression in medically ill patients [33-34]. The questionnaire contains 14 items with four response categories, ranging from 0-3. Higher scores on the two subscales (each consisting of 7 items) indicate a higher level of anxiety or depression. The total score of the HADS ranges from 0-42, and can be used as a global measure of psychological distress [35]. The reported internal consistency for this scale is Alpha: 0.78-0.88 [36].
The coping scale (BRIEF COPE)
The original COPE Inventory was developed to assess a broad range of coping responses including both adaptive and maladaptive coping strategies (e.g., planning, avoidance) [37]. A shorter 28-item set was created from the original 60-item scale to assess 14 demotions (2 items per subscale) of coping strategies [38]. The questionnaire has four response categories, ranging from (I have not been doing this at all: 1) to (I have been doing this a lot: 4) with higher scores indicating more utility of specific coping strategies. The validity and reliability of data collected using this scale is moderate-to-high (Alpha: 0.50-0.90) [39].
The social provisions scale (SPS)
The SPS is an instrument used to perceived social support. This instrument has 24 items to assess six dimensions of perceived support provisions including attachment, social integration, reassurance of worth, reliable alliance, guidance, and opportunity for nurturance. The response scale ranges from (strongly disagree: 1) to (strongly agree: 4) with a higher score indicating better perceived social support. This scale has moderate-to-high validity and reliability (Alpha: 0.50-0.77) [40].
The general self-efficacy beliefs scale (GSE)
The GSE is designed to assess optimistic self-control beliefs (i.e., the belief that one’s actions are responsible for successful outcomes). The scale is uni dimensional consisting of 10 items with high internal consistency (Cronbach’s alphas ranged from 0.76 to 0.90). Item response ranges from (not at all: 1) to (exactly true: 4) with higher scores indicating higher self-efficacy beliefs [41].
Data analyses
Statistical analyses were conducted using R 3.1.3 [42]. First, the data were cleaned and examined for missing values, outliers or extreme values [43]. Next, data were summarized as mean ± standard deviation (SD) for continuous variables and as frequency (percentage) for categorical variables. Statistical significance for all hypothesis tests was evaluated using a type I error rate of 0.05. The reliability of the BCNAS-32 was explored by examining the internal consistency of BCNAS-32 summary subscales and the total scale, with the aim to allocate a Cohen’s Alpha of ≥0.70 as recommended by similar studies [44-45]. Discriminant and convergent validity was investigated by computing r coefficient correlations between the BCNAS-32 summary subscales and the total scale and the FACT-BL, HADS, BRIEF COPE, and the GSE scales. Similar correlation analyses between SCNS-LF59 and FACT-BL, HADS, BRIEF COPE, and the GSE scales were conducted to allow for comparing the emerging correlation coefficients with those resulted from the correlation between BCNAS-32and FACT-BL, HADS, BRIEF COPE, and the GSE scales to provide additional validity assessments.
Missing data analysis and imputation
In order to determine the robustness of the data collected, the percentage and the pattern of the missing data of each of the study scales included in the questionnaire were determined. A percentage of 15-20% of missing data in each scale is considered to be reasonable in psychological studies [46]. The number, percentage, and pattern of missing data in each scale were analyzed using the mice package in R [42]. Polytomous response logistic regression was used to impute missing values for ordered categorical variables. The mean of the imputed numbers was used for each missing value.
Examining the internal consistency of the BCNAS-32
Due to the complexity and variability of BC-related needs within treatment groups and over time, the limited study sample (N = 159) , and the large number of items we developed (92 items) to assess BC related needs, using a one general factor analysis on all the individual items was not statistically meaningful in this small sample [47]. Therefore, principal component analysis (PCA) with varimax rotation was used in assessing the underlying factor patterns of each original subscale we developed to assess BC related needs within each domain.
A first PCA was carried out on the individual items constituting the designed scales to explore the subscales’ internal consistency (i.e., psychologic, health system and information, physical and daily living, patient care and support, sexuality, logistic, and communication with providers and partners) using the psych package in R [48]. The number of factors in each need subscale was determined and subsequently, items for each subscale were selected if they had a factor loading≥0.40 in the main cluster and the factor loading of <0.40 in other clusters. The internal reliability of the selected items in each subscale was evaluated using the Cronbach’s alpha coefficient.
Convergent validity and discriminant validity analysis of the BCNAS-32
Pearson’s correlation coefficients (r) were computed to evaluate the convergent and discriminant validity of the emerging subscales confirmed by the PCA analyses, FACT-BL, HADS, BRIEF COPE, and GSE scales. Correlations were designated as low, moderate, or high, when their absolute values were respectively <0.30, from 0.30-0.50 and ≥0.50 [49].
Determination of proportion of moderate/high unmet needs
The proportion of BC patients with moderate/high unmet need and no/low unmet need was estimated from the mean value of each subscale after transforming the scale to 0-100 score as recommended for the general SCNS-LF59. A mid-point of 50 was used as the cut-off point to separate no/low need and moderate/high need. A score larger than 50 was considered indicative of moderate-high need, otherwise, was considered as no/low need.
Results
Missing data pattern
The percentage of missing data in this study was between 6% to 18% in all the original needs assessment survey subscales and between 0% to 19% in the other scales used in this study including theSCNS-LF59,FACT-BL, HADS, Brief COPE, and GSE scales. No specific pattern of missing values was observed, thus the degree of missing data was assumed to be random.
Sample characteristics
Table 1 shows the demographic and clinical characteristics of the respondents. Of the 159 BC patients, 51% were male and 47% were female. The mean age of the BC patients was 62±9.4 years old. Almost two-third (62%) of the BC patients received cystectomy. Among these, 28% received ileal conduit, 11%continent reservoir, and 26% neobladder. The majority of the patients were married (82%), with children (85%), and with at least some college education or higher degree (88%). Many of the BC patients in this study were retired (43%) or unemployed (43%). A number of the BC patients were in stage I (T1, 37%) or stage II (T2, 25%) of cancer. Fifty-five percent of the patients reported to be in tumor grade of 3. The average time since cystectomy was 42±37.5 months (range: 3-173 months). On average, the respondents had two comorbidities (Table 1). The five most common co-morbidities reported were: hypertension (38%), arthritis (33%), problem with bladder control (27%), hearing loss (17%), and stomach problem (14%) (Data not shown).

Examining the internal consistency and reliability of the BCNAS-32
To ensure that the data was suitable for factor analysis, standard diagnostic tests were run each time. Following recommendations, both the Kaiser-Meyer-Olkin (KMO) test of sampling adequacy criterion (KMO≥0.6) and Bartlett’s test of sphericity criterion (p<0.05) were completed to indicate factorability of the data [47]. Thirty-two out of the 92 newly designed items from the 7 designed sub-scales were selected by exploratory factor analysis using 0.40 as the loading cutoff point [50,51]. Table 2 shows the selected items in each newly designed original subscale based on the factor analyses results.
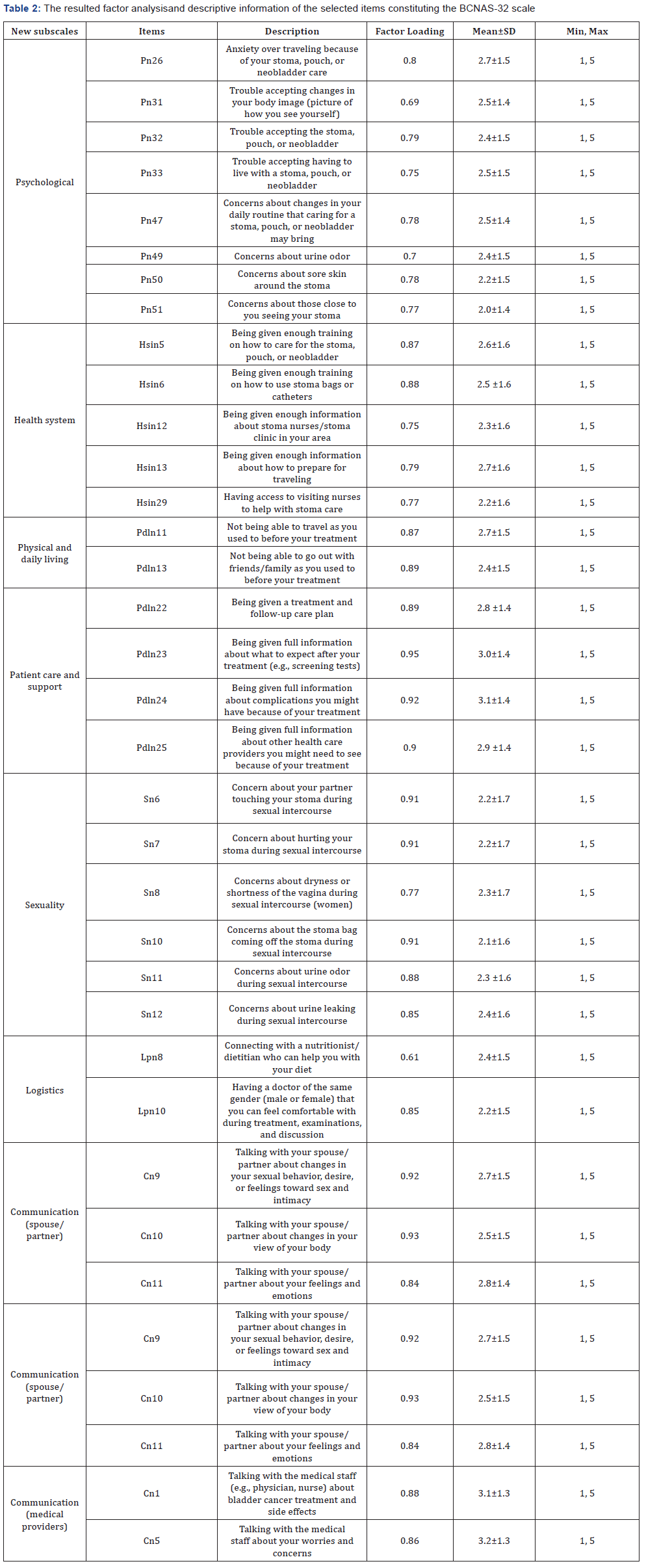
The items in the psychological subscale assess psychological impact of BC treatment on emotional adjustment including worries about BC, and acceptance of a stoma, pouch, or neobladder. Items in health system subscale assess needs of BC specific information and training on self-care strategies. The items in physical and daily living subscale assess the impact of BC treatment on patient’s daily living and lifestyle. Items in patient care and support subscale assess needs of supportive care specific to BC and treatment side effects.
The items in the sexuality subscale assess the impact of BC treatment and side effects on sexual function, body image, and sexual relationships. Items in logistics subscale assess patients’ need for support with transportation, access to communitybased services, and any other logistic issues. Factors analyses of the communication subscale revealed two distinct types of communication modes: communication with providers and communication with partners. The items in communication with spouse/partner subgroup assess challenges and difficulties in talking about changes in sexual behavior, body image, and patients’ feeling and emotions. The items in communication with medical provider assess the difficulties in talking about cancer treatment and BC-related side effects and about patients’ worries and concerns with their medical staff.
To explore the reliability of the BCNAS-32 total and the emerging seven subscales, alpha coefficients were calculated (Table 3). For the seven BCNAS-32 subscales, the mean of alpha coefficients was 0.97 (range: 0.93-0.96). Only two items were selected in the physical and daily living subscale, logistics subscale, and communication (medical provider) subscale, therefore correlation coefficient was used instead of alpha coefficient to describe the internal consistency as recommended [52]. The correlation coefficients of these subscales were physical and daily living (r=0.85, p<0.001), logistics subscale (r=0.57, p<0.001), and communication with provider subscale (r=0.78, p<0.001).

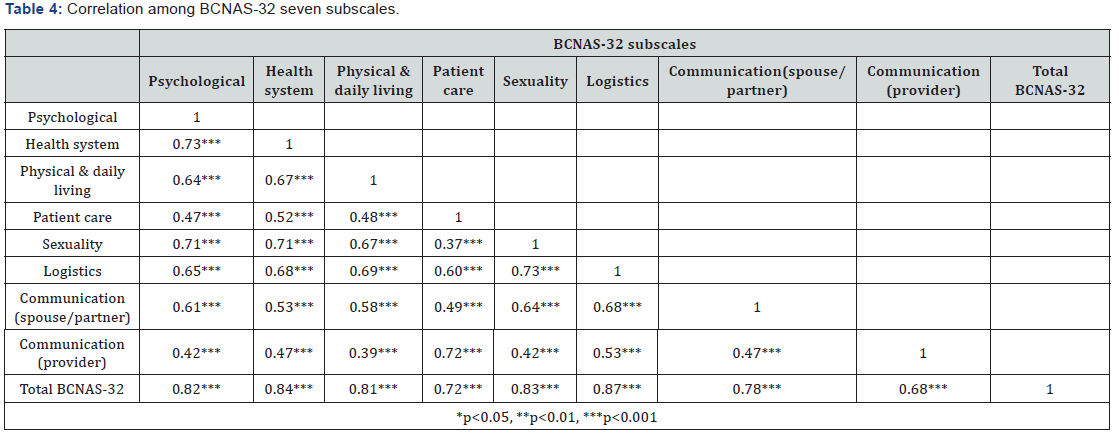
The mean for the total BCNAS-32was 319(range: 0-775, SD=218) and all subscales (range 32-53; SD range: 32-38). Intercorrelation among the seven subscales ranged between 0.37 and 0.73 (Table 4) indicating that these subscales assess related but different dimensions of concerns and care needs while revealing no evidence for multi collinearity (i.e., r≥0.80) [53]. The proportion of moderate/high unmet needs in each subscale using the criteria described in the method section were 29% for psychological, 31% for health system, 30% for physical and daily living, 41% for patient care and support, 25% for sexuality, 24% for logistics, 30% for communication (spouse/partner) and 44% for communication (medical provider) as shown by Table 3.
Examining the convergent validity and discriminant validity of the BCNAS-32
Pearson correlations for BCNAS-32 total and its seven subscales and the SCNS-LF59 total and its 5 subscales were in the expected directions (Table 4). Statistically significant and positive correlations emerged between the BCNAS-32and SCNSLF59 confirming the convergent validity of the BCNAS-32.
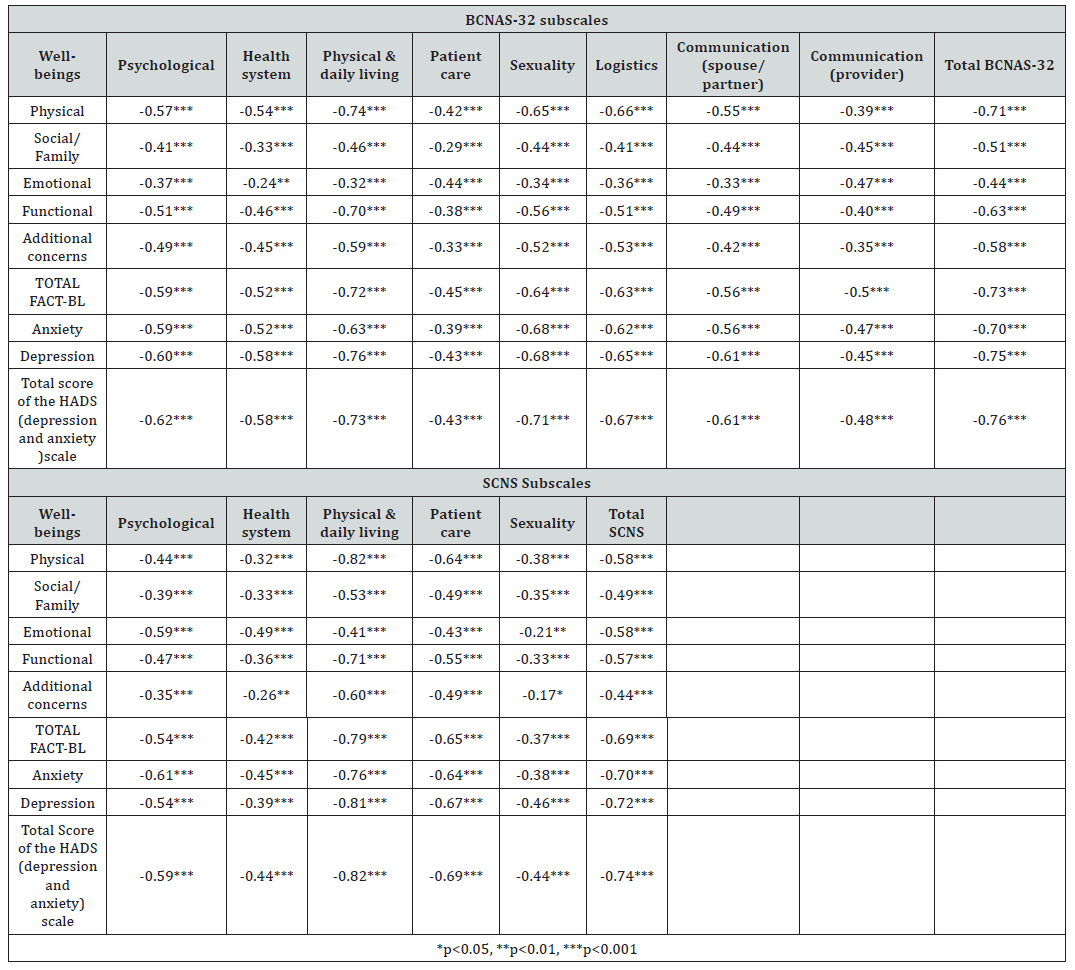
Exploring the discriminant validity of the BCNAS-32 confirmed associations between higher unmet needs as measured by BCNAS-32 and lower levels of HRQoL (r range: -0.74 to -0.24; p<0.001), social support provisions (r range: -0.66 to -0.16; p<0.05), and self-efficacy beliefs (r range: -0.59 to -0.30; p<0.001), and higher levels of maladaptive coping strategies (r range: 0.24 to0.71; p<0.001), depression (r range: -0.76 to -0.43; p<0.001), and anxiety (r range: -0.68 to -0.39; p<0.001) as expected.
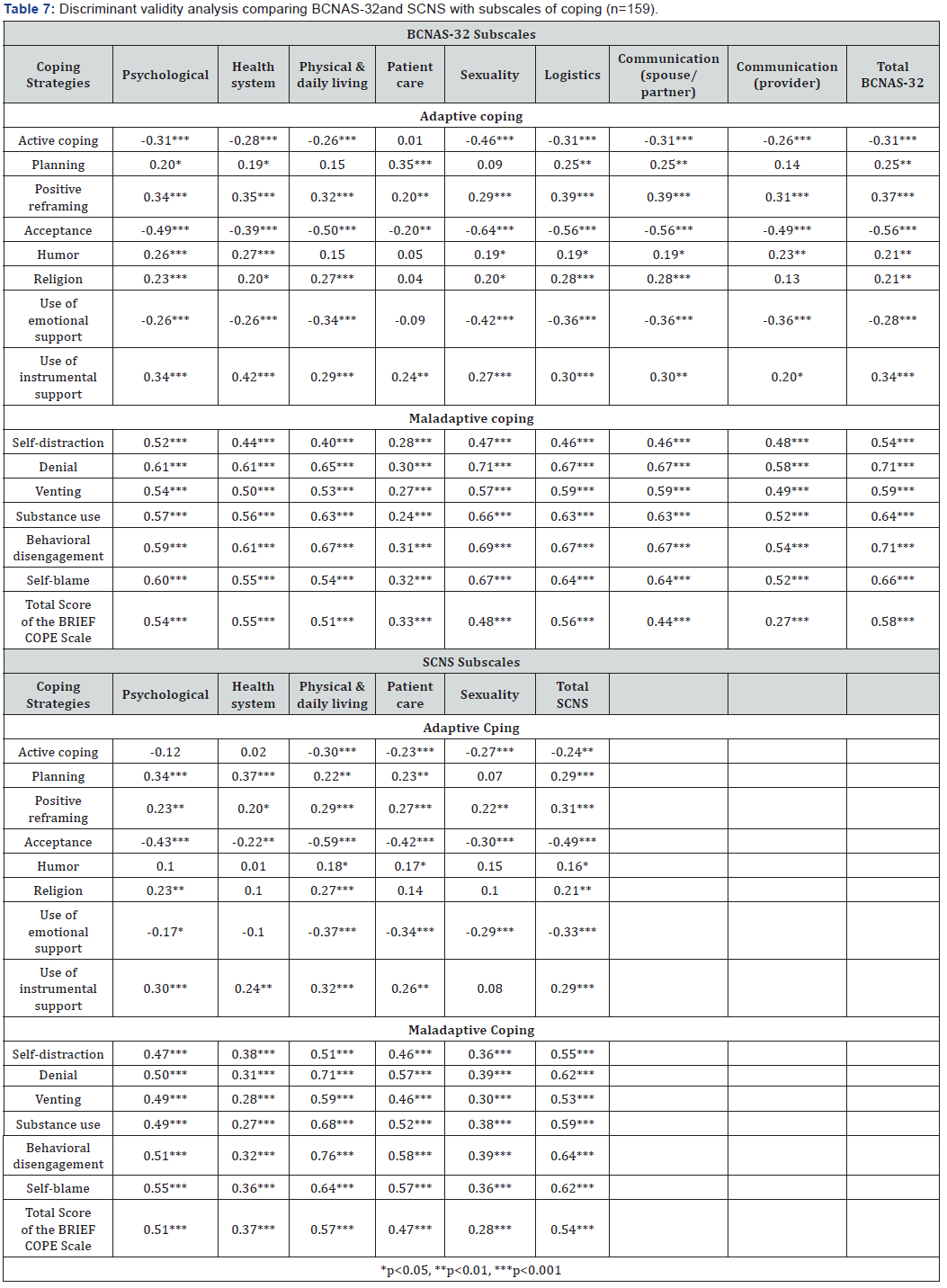
The magnitude and direction of these associations confirm the convergent and discriminant validity of the BCNAS-32 and are similar to those that emerged from examining the associations between the SCNS-LF59, FACT-BL, HADS, GSE, Brief COPE, and SPS, thus further attesting to the validity of the BCNAS-32 (Table 5-7).
Table 5: Correlations between BANSA-32 and FACT-BL and between SCNS-59 and FACT-BL.

Discussion
The current study provides initial evidence for the newly designed BCNAS-32 scale as a suitable measure of unmet needs of BC patients across different phase of the illness trajectory. Although theSCNS-LF59 survey has been commonly used to assess cancer patients’ needs [54], it is a generic measure that is not sensitive for issues specific to BC and treatment outcomes. Developing a disease-specific survey for BC patients to identify their unmet needs is imperative in providing tailored and personalized supportive care for patients.
Identifying such needs allows health care providers to most effectively allocate scarce resources to address patients’ specific unmet needs, improve service quality, and inform the design and evaluation of tailored educational and psychosocial interventions to address these needs. Additionally, from a clinical perspective, identifying patients’ needs will help improve health care service quality, adherence to treatment recommendation and followup care, and increase patient involvement and satisfaction with care.
In this study, we designed 92 new items specific to BC patients’ needs [17]. Exploratory factor analysis was performed to identify and select the most relevant items that explained seven distinguishable components of unmet needs in BC patients (psychological, health system, physical and daily living, patient care and support, sexuality, logistics, and communication) [55,56]. Cronbach’s alpha for each subscale was very high confirming the internal consistency of the identified subscales. Examining the convergent validity of the BCNAS-32 using the SCNS-LF59 showed significant correlations in the expected direction and confirm the convergent validity of the BCNAS-32.
Studies have shown that cancer patients who report high unmet needs also report poor HRQoL [57,58]. As expected, discriminant validity of the BCNAS-32 confirmed these negative associations with different dimensions of HRQoL including physical, functional, social, and emotional. Additionally, analysis of discriminant validity of the BCNAS-32 showed that BC patients with high unmet needs were also more likely to report higher levels of anxiety and depression.
High unmet needs measured by the BCNAS-32 were also associated with maladaptive coping strategies (i.e., self-distraction, denial, venting, substance use, behavioral disengagement, and self-blame), lower levels of self-efficacy beliefs, and low levels of perceived social support measured as attachment, social integration, reassurance of worth, reliable alliance, guidance, and opportunity for nurturance, which is in line with prior findings in need assessment of other cancer populations [59-61].
Our study results also showed that, although the majority of the study participants were >42 months post-BC treatment, significant proportions of these patients reported unmet needs at the time of the online survey including psychological, health system, physical and daily living, patient care and support, sexuality, logistics, communication with partners and provider’s needs. These findings emphasize the need for standardized and frequent screening of patients’ unmet needs across the BC trajectory. Thus BC patients’ needs could be addressed in an efficient manner using available health care resources. Prior research in other cancer populations has shown that psychosocial and health care planning interventions tailored to patients’ unmet needs are effective in improving their quality of life, adherence to cancer treatment, and treatment outcomes [62,63]. For BC patients, interventions could also be provided as standard care to prevent patients from experiencing unmet needs throughout the BC care-continuum. These interventions may include provision of information about BC treatment and potential outcomes, and telephone calls or home visits by social workers and os to my nurses to improve self-care skills and symptom management, and, when warranted, provide crisis intervention.
This study had several limitations. The general recommendation for the number of subjects included in factor analysis is 10 subjects per item of the questionnaire [29]. With 92 items constituting the original bladder cancer need survey, the 159 participants who were included in this study constitute a rather limited research sample [47]. The majority of the study participants were MIBC patients who received cystectomy and urinary diversion. A larger and more diverse sample of BC patients is needed to confirm the structure of the BCNAS-32.
Additionally, this is a cross-sectional study, thus test-retest validity of the emerging components of the BCNAS-32 could not be examined. Furthermore, the study sample consisted of members of BCAN who have access to BCAN’s educational and support resources (e.g., online support groups, patient educational booklets, and online seminars on BC treatment and outcomes). The utility and validity of the BCNAS-32 should further be explored in patients recruited from hospitals and clinics, before the instrument is implemented in clinical practice.
While this study demonstrates rigor of the BCNAS-32 across key psychometric properties, we must acknowledge that other indices were not explored, e.g. known group comparisons, predictive validity, and responsiveness. Consequently, future studies should focus on these aspects, and can strengthen the evidence of validity of the BCNAS-32
Conclusion
This study confirms the internal consistency and validity of BCNAS-32. Further research studies are needed to explore how the use of such a tool can be implemented efficiently in clinical practice to contribute to quality patient-centered care.
Acknowledgement
This study is supported by mentored research scholar grants from the American Cancer Society (121193-MRSG-11-103-01- CPPB), the National Cancer Institute (1R03CA165768-01A1), and Department of Defense award DoD W81XWH-15-1-0532.
We would also like to show our gratitude to the participants in this study and the BCAN survivorship group in providing input on the original version of the scale. We thank Ms. Qainat Shah for her assistance with editing.
References
- American Cancer Society: Cancer Facts and Figures 2011. (2011) Atlanta, Ga: American Cancer Society.
- Noyes K, Singer EA, Messing EM (2008) Healthcare economics of bladder cancer: cost-enhancing and cost-reducing factors. Curr Opin Urol 18(5): 533-539.
- Latini DM, Lerner SP, Wade SW, Lee DW, Quale DZ (2010) Bladder Cancer Detection, Treatment and Outcomes: Opportunities and Challenges. Urology 75(2):334-339.
- Yee DS, Ishill NM, Lowrance WT, Herr HW, Elkin EB (2011) Ethnic differences in bladder cancer survival. Urology 78(3): 544-549.
- Smith ZL, Christodouleas JP, Keefe SM, Malkowicz SB, Guzzo TJ (2013) Bladder preservation in the treatment of muscle-invasive bladder cancer (MIBC): a review of the literature and a practical approach to therapy. BJU Int 112(1): 13-25.
- Cooksley CD, Avritscher EB, Grossman HB, Sabichi AL, Dinney CP, et al (2008) Clinical model of the cost of bladder cancer in the elderly. Urology 71(3): 519-525.
- Sandler HM, Mirhadi AJ (2012) Current Role of Radiation Therapy for Bladder Cancer. Seminars in Oncology 39(5): 583-587.
- Mohamed NE, Chaoprang HP, Hudson S, Revenson TA, Lee CT, et al (2013) Muscle invasive bladder cancer: examining survivor burden and unmet needs.J Urol 191(1): 48-53.
- Bohle A, Balck F, Von Weitersheim J, Jocham D (1996) The quality of life during intravesical bacillus calmette-guerin therapy. J Urol 155(4): 1221-1226.
- Mack D and Frick J (1996) Quality of life in patients undergoing bacilli Calmette-Gue´rin therapy for superficial bladder cancer. Br J Urol 78(3): 369-371.
- Liedberg F, Holmberg E, Holmäng S, Ljungberg B, Malmstrom PU, et al. (2012) Long-term follow-up after radical cystectomy with emphasis on complications and reoperations: a Swedish population-based survey. Scandinavian Journal of Surgery 46(1):14-18.
- Okada Y, Oishi K, Shichiri Y, Kakehi Y, Hamaguchi A, et al. (1997) Quality of life survey of urinary diversion patients: comparison of continent urinary diversion versus ileal conduitnt Int J Urol 4(1): 26-31.
- Turner WH, Studer UE (1997) Cystectomy and urinary diversion. J SurgOncol 13(5): 350-358.
- Hardt J, Filipas D, Hohenfellner R, Egle UT (2000) Quality of life in patients with bladder carcinoma after cystectomy: first results of a prospective study. Quality of Life Research 9(1): 1-12.
- Stein JP, Lieskovsky G, Cote R, Groshen S, Feng AC, et al (2001) Radical cystectomy in the treatment of invasive bladder cancer: long-term results in 1,054 patients. J ClinOncol 19(3): 666-675.
- Clark PE (2002) Urinary diversion after radical cystectomy. Current Science 3(5): 389-402.
- Mohamed NE, Herrera CP, Hudson S, Revenson TA, Lee CT, et al. (2014) Muscle invasive bladder cancer: Examining survivors’ burden and unmet needs. J Urol 191(1): 48-53.
- Warrington L, Absolom K, Velikova G (2015) Integrated care pathways for cancer survivors - a role for patient-reported outcome measures and health informatics. ActaOncol 54(5): 600-608.
- Accreditation Canada (2009) Qmentum Program 2009: Cancer Care and Oncology Services. Canada.
- Breitbart W, Rosenfeld B, Pessin H, Applebaum A, Kulikowski J, et al. (2015) Meaning-centered group psychotherapy: an effective intervention for improving psychological well-being in patients with advanced cancer. J Clin Oncol 33(7): 749-754.
- Holland J, Watson M, Dunn J (2011) The IPOS new International Standard of Quality Cancer Care: integrating the psychosocial domain into routine care. Psychooncology 20(7): 677-680.
- Meyer LA, Nick AM, Shi Q, Wang XS, Williams L, et al. (2015) Perioperative trajectory of patient reported symptoms: a pilot study in gynecologic oncology patients. Gynecol Oncol 136(3): 440-445.
- National Comprenhensive Cancer Network: Distress management (v.1.2008).
- Institute of Medicine (2008) Cancer Care for the Whole Patient: Meeting Psychosocial Health Needs. The National Academies Press.
- Leventhal H, Diefenbach M, Leventhal EA (1992) Illness cognition: Using common sense to understand treatment adherence and affect cognition interactions. Cognitive Therapy and Research 16(2): 143- 163.
- Miller SM, Diefenbach MA (1998) C-SHIP: A cognitive-social health information processing approach to cancer. In: Krantz D (Ed.), Perspective in Behavioral Medicine, Lawrence Erlbaum, pp. 219-244.
- McElduff P, Boyes A, Zucca A, Girgis A (2004) The supportive care needs survey: A guide to administration, scoring and analysis. Newcastle: Centre for Health Research & Psycho-Oncology, England.
- Girgis A, Lambert S, Lecathelinais C (2011) The supportive care needs survey for partners and caregivers of cancer survivors: development andevaluation. Psychooncology 20(4): 387-393.
- Terwee CB, Bot SD, de Boer MR, van der Windt DA, Knol DL, et al. (2007) Quality criteria were proposed for measurement properties of health status questionnaires. J Clin Epidemiol 60(1): 34-42.
- Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, et al. (2009) Research electronic data capture (REDCap) - a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42(2): 377-3781.
- Bonevski B, Sanson-Fisher R, Girgis A, Burton L, Cook P, et al. (2000) Evaluation of an instrument to assess the needs of patients with cancer. Supportive Care Review Group. Cancer 88(1): 217-225.
- Danna BJ, Metcalfe MJ, Wood EL, Shah JB (2016) Assessing Symptom Burden in Bladder Cancer: An Overview of Bladder Cancer Specific Health-Related Quality of Life Instruments. Bladder Cancer. 2(3): 329- 340.
- Spinhoven P, Ormel J, Sloekers PP, Kempen GI, Speckens AE, et al. (1997) A validation study of the Hospital Anxiety and Depression Scale (HADS) in different groups of Dutch subjects. Psychol Med 27(2): 363- 370.
- Zigmond AS, Snaith RP (1983) The hospital anxiety and depression scale. Acta Psychiatr Scand 67(6): 361-370.
- Mitchell AJ, Meader N, Symonds P (2010) Diagnostic validity of the Hospital Anxiety and Depression Scale (HADS) in cancer and palliative settings: a meta-analysis. J Affect Disord 126(3): 335-348.
- Yusoff N, Low WY, Yip CH (2011) Psychometric properties of the Malay Version of the hospital anxiety and depression scale: a study of husbands of breast cancer patients in Kuala Lumpur, Malaysia. Asian Pac J Cancer Prev 12(4): 915-917.
- Carver CS, Scheier MF, Weintraub JK (1989) Assessing coping strategies: a theoretically based approach. J Pers Soc Psychol 56(2): 267-283.
- Carver CS (1997) You want to measure coping but your protocol’s too long: consider the brief COPE. Int J Behav Med 4(1): 92-100.
- Yusoff N, Low WY, Yip CH (2010) Reliability and validity of the Brief COPE Scale (English version) among women with breast cancer undergoing treatment of adjuvant chemotherapy: a Malaysian study. Med J Malaysia 65(1): 41-44.
- Drageset S, Lindstrøm TC (2005) Coping with a possible breast cancer diagnosis: demographic factors and social support. J Adv Nurs 51(3): 217-226.
- Jerusalem M, Schwarzer R, Schwarzer R (1992) Self-efficacy as a resource factor in stress appraisal processes. Self-efficacy: Thought control of action. US: Hemisphere Publishing Corp, USA pp. 195-213.
- R Development Core Team (2008) R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria.
- Van den Broeck J, Cunningham SA, Eeckels R, Herbst K (2005) Data cleaning: detecting, diagnosing, and editing data abnormalities. PLoS Med 2(10): e267.
- Terwee CB, Dekker FW, Wiersinga WM, Prummel MF, Bossuyt PM (2003) On assessing responsiveness of health-related quality of life instruments: guidelines for instrument evaluation. Qual Life Res 12(4): 349-362.
- Bartko JJ (1966) The intraclass correlation coefficient as a measure of reliability. Psychol Rep 19(1): 3-11.
- Enders CK (2003) Using the expectation maximization algorithm to estimate coefficient alpha for scales with item-level missing data. Psychol Methods 8(3): 322-337.
- Schouten B, Hellings J, Van Hoof E, Vankrunkelsven P, Bulens P, et al. (2016) Validation of the flemish CARES, a quality of life and needs assessment tool for cancer care. BMC Cancer 16: 696.
- Revelle W (2017) psych: Procedures for Personality and Psychological Research, Northwestern University, Evanston, Illinois, USA.
- Burns N, Grove SK (2001) The practice of nursing research (4th edn). Philadelphia: WB Saunders, USA.
- Stevens JP (1992) Factor analysis of Variance. Applied Multivariate Statistics for the Social Sciences (2nd edn). Hillsdale, NJ: Erlbaum.
- Matsunaga M (2010) How to Factor-Analyze Your Data Right: Do’s, Don’ts, and How-To’s. International Journal of Psychological Research 3(1):97-110.
- Eisinga R, Grotenhuis M, Pelzer B (2013) The reliability of a two-item scale: Pearson, Cronbach, or Spearman-Brown? Int J Public Health 58(4): 637-642.
- Franke GR (2010) Multicollinearity. Wiley International Encyclopedia of Marketing.
- Richardson A, Medina J, Brown V, Sitzia J (2007) Patients’ needs assessment in cancer care: a review of assessment tools. Support Care Cancer 15(10): 1125-1144.
- Gorsuch RL (1983) Factor Analysis (2nd edn). Hillsdale: Lawrence Erlbaum Associates.
- Kim JO, Mueller CW (1978) Introduction to factor analysis: what it is and how to do it. Beverly Hills, Calif Sage Publications.
- Aranda S, Schofield P, Weih L, Yates P, Milne D, et al. (2005) Mapping the quality of life and unmet needs of urban women with metastatic breast cancer. Eur J Cancer Care (Engl) 14(3): 211-222.
- Molassiotis A, Wilson B, Blair S, Howe T, Cavet J (2011) Unmet supportive care needs, psychological well-being and quality of life in patients living with multiple myeloma and their partners. Psychooncology 20(1): 88-97.
- Lintz K, Moynihan C, Steginga S, Norman A, Eeles R, et al. (2003) Prostate cancer patients’ support and psychological care needs: Survey from a non-surgical oncology clinic. Psychooncology 12(8): 769-783.
- Lev EL, Paul D, Owen SV (1999) Age, self-efficacy, and change in patients’ adjustment to cancer. Cancer Pract 7(4): 170-176.
- McSorley O, McCaughan E, Prue G, Parahoo K, Bunting B, et al. (2014) A longitudinal study of coping strategies in men receiving radiotherapy and neo-adjuvant androgen deprivation for prostate cancer: a quantitative and qualitative study. J AdvNurs 70(3): 625-638.
- Rehse B, Pukrop R (2003) Effects of psychosocial interventions on quality of life in adult cancer patients: meta analysis of 37 published controlled outcome studies. Patient Educ Couns 50(2): 179-186.
- Salonen P, Tarkka MT, Kellokumpu-Lehtinen PL, Astedt-Kurki P, Luukkaala T, et al. (2009) Telephone intervention and quality of life in patients with breast cancer. Cancer Nurs 32(3): 177-190.






























