Pathology of Cardiovascular System in Patients with Inflammatory Bowel Diseases
Khlynova OV*, Vasilets LM, Tuev AV and Kuznetsova ES
Department of Hospital Therapy, E.A. Vagner Perm State Medical University, Russia
Submission:December 14, 2018;Published: January 17, 2019
*Corresponding author: Khlynova OV, Department of Hospital Therapy, E.A. Vagner Perm State Medical University, 614990, Perm, Petropavlovskaya str 26, Russia
How to cite this article: Khlynova O, Vasilets L, Tuev A, Kuznetsova E. Pathology of Cardiovascular System in Patients with Inflammatory Bowel Diseases. 002 Adv Res Gastroentero Hepatol. 2019; 12(1): 555830. DOI: 10.19080/ARGH.2019.12.555830.
Abstract
The purpose the work was studying of cardiovascular system disease prevalence and structure in persons with the inflammatory bowel diseases (IBD) using Gastroenterology department of the Perm regional hospital as an example. It was the retrospective one-stage research including studying case histories of the patients with ulcerative colitis (UC) and Crohn’s disease (CD) examined and treated in gastroenterological clinic for the period of 2013-2016. There were 291 patients with IBD, chronic cardiovascular pathology was revealed only in 90 patients. Comparative analysis showed that combined diseases were mainly spread in men with UC of middle and advanced age. The most typical for them was combination of UC and ischemic heart disease (50% of cases). Cardiovascular system pathology was 1.5 times more common for women with CD pathology. Besides CD, thromboses of peripheral veins (45% of cases) and myocardial dystrophy (24.5% of cases) were the most frequent pathologies. Due to the small number of patients with IBD and cardiovascular system pathology, it is not possible to claim unambiguously the degree of cardiac disorders in patients with IBD. Thus, it is planned to increase the number of observations to reach statistically optimum conclusion. Studying of this problem is of special practical importance for the possibility to regard patients with IBD as a group of patients with high cardiovascular risk. This will necessitate a number of preventive actions to prevent cardiovascular accidents of fatal and non-fatal character.
Keywords: Ulcerative colitis; Crohn’s; Thromboses; Arrhythmias; Cardiovascular risk
Abbrevations: IBD: Inflammatory Bowel Diseases; CD: Crohn’s Disease; UC: Ulcerative Colitis; HP: Hypertension; IHD: Coronary Heart Disease; HRD: Heart Rhythm Disturbances; HCD: Heart Conductivity Disorders
Introduction
Inflammatory Bowel Diseases (IBD) including disease Crohn’s (CD) and ulcerative colitis (UC) are the most serious chronic gastrointestinal tract diseases [1-4]. They should be considered as general diseases with multiple immune pathology. Because of this, clinicians are always interested not only in the local changes or complications of IBD associated immediately with an inflammation in the digestive tube but also abenteric or system manifestations of diseases [5-11].
It is well known that in certain cases IBD begin with atypical clinical symptoms, namely with nonspecific abenteric disturbances [12]. This presents certain difficulties in their diagnostics and in some cases delays the time of making the correct diagnosis for several years that negatively affects the forecast of a disease. Besides, abenteric manifestations quite often reduce the general quality of life much more, than typical symptoms in certain IBD phenotypes [12]. The general system complications and abenteric manifestations of IBD are traditionally classified by the pathogenic principle:
• Changes occurring due to a system hypersensitization – damage of joints, eyes, skin, oral mucous membrane;
• Caused by bacteremia and an antigenemia in the portal system – liver and biliary tract damages;
• Relapsing in long-lasting disturbances in the large intestine – anemias, electrolyte disorders [11,13-15].
At the same time, IBD abenteric manifestations are, according to different authors, from 5 to 55%. The majority of large studies show higher prevalence of abenteric manifestations in CD in comparison with UC [16]. At the same time, some works show approximately identical frequency of their occurrence in various types of IBD [10].
Considering cardiovascular system pathology in persons with IBD, it is one of the most poorly studied disorders today [17,18]. There are only few reports on coronary artery lesions [19,20], development of vascular atherosclerosis and coronary heart disease [9,21,22], dilated cardiomyopathy [23] and endomyocardial fibrosis [4], and vascular thromboses [24-28] in IBD patients. The problem is whether patients with IBD can be regarded as persons with high risk of cardiovascular accidents that it is mainly associated with the development of the progressive dysfunction of the vascular endothelium in them [29-33].
However, there is still no consensus on the prevalence of cardiovascular system diseases in persons with ШИВ, mechanisms of formation and progressing of endothelial dysfunctions and thrombophilias in UC and CD, and also there is no answer to a question: whether it is necessary to taken into account seriously patients with IBD as a category of patients with high and very high cardiovascular risk. Since non-infection diseases mortality in the world is now due to cardiovascular diseases their prevention is an urgent and significant problem having both in medical, and social significance. The above arguments made the basis for the present research.
Work Purpose
To study prevalence and structure of cardiovascular system diseases in patients with IBD, gastroenterology department of the Perm regional hospital served as an example.
Materials and Methods
It was a retrospective study of 291 case histories of patients with IBD (UC and CD) examined and treated in gastroenterological clinic of the Perm regional hospital during 2013-2016. According to life anamnesis written down according to patients report, results of laboratory and instrumental examination, patients with the accompanying cardiovascular system pathology, including hypertension (HP), coronary heart disease (IHD), heart rhythm disturbances (HRD) and heart conductivity disorders (HCD), system vasculitis, vascular atherosclerotic lesions, thromboembolic disorders were selected. Comparison of the obtained data with literary data on the prevalence of the chosen cardiovascular diseases in the Russian population in general was carried out. The results were statistically processed using the variation statistics method that allowed to present data in the form of mean values and percent. To evaluate reliability of differences Wilcoxon nonparametric method for pair comparisons was used, distinctions were considered reliable at р <0.05.
Discussion
As a result, in 90(30.93%) of 291 patients with IBD (for the period of 2013-2106) had chronic cardiovascular system diseases. They were found in 58 patients with UC (mean age 42.5±14.8 years, 31 men and 27 women) and in 32 patients with CD (mean age of 35.2±12.1 years, 18 men and 14 women). The structure of the revealed cardiovascular system diseases in patients with UC is presented in Figure 1.
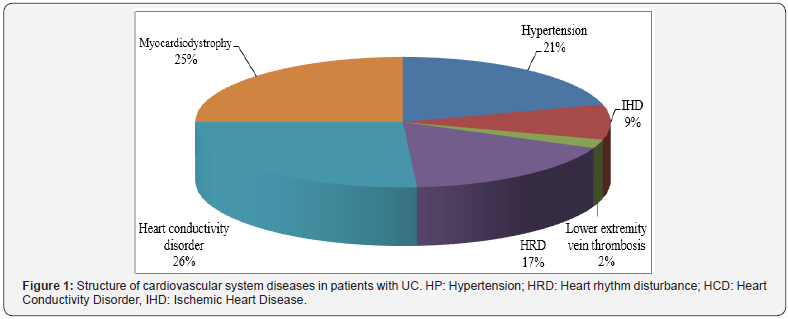
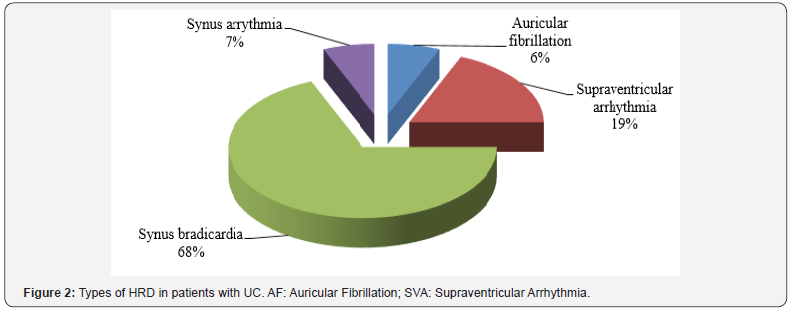
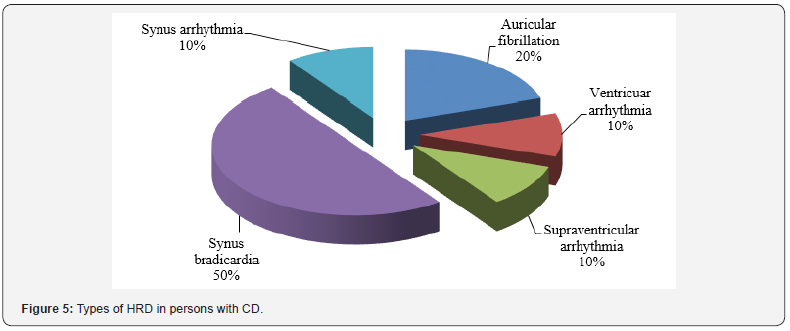
Types of heart rhythm disturbance (HRD) in patients of this group were the following (Figure 2). Types of the heart conductivity disorders (HCD) in patients with UC were also nonuniform (Figure 3). The structure of the revealed diseases of cardiovascular system in persons with CD is presented in Figure 4. Types of HRD in patients with CD are presented in Figure 5.


The gender analysis in groups with IBD and cardiovascular pathologies showed that among persons with UC combined pathology men were twice more affected than women (р =0.032). At the same time in 50% of cases it was IHD, in 25% - HT, in 20% - myocardial dystrophy and in 5% - HRD and HCD, whereas women with UC had another structure of cardiac pathology: HT - in 62% of cases, IHD - in 18.3% of cases, HRD and HCD - in18.7% of cases, myocardial dystrophy – in 1% oа cases. In patients with CD cardiovascular diseases were observed 1.5 times more often in women (р =0.04) than in men. They included thromboses of peripheral veins in 45% of patients, myocardial dystrophy - in 24.5% of cases, HT - in 6.5% of cases, IHD - in 12.3%, HRD and HCD – 11.7% of cases. In men of this subgroup: HCD was registered in 80% of cases, HRD - in 14.8%, HT – 5.2% of cases.
Age distribution of patients with IBD and cardiovascular pathology is presented in Figure 6 & 7. The figure shows that among patients with UC cardiovascular pathology was mainly prevalent in older age group (р =0.041). HT, IHD, HRD and myocardial dystrophy were more common.
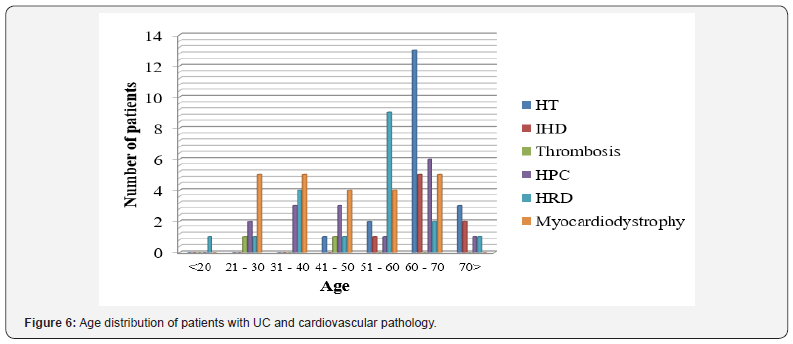
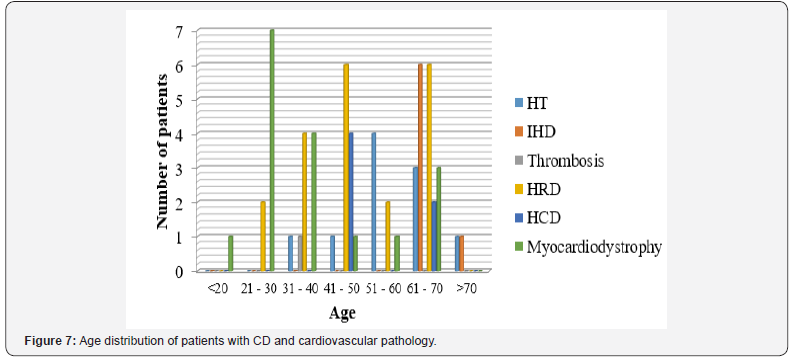
According to Figure 7, it is not possible to state the prevailing age period and incidence of cardiovascular diseases in patients with CD. At present there are no works devoted to this problem, moreover due to small number of selected patients with IBD and cardiovascular system pathology it is not possible to claim unambiguously the degree of prevalence of cardiac disorders in patients with IBD. Therefore, it is planned to continue these studies, increasing the number of observations for receiving statistically optimum conclusions.
In our opinion, this problem is of practical importance for separating patients with IBD in the group with high cardiovascular risk. This will probably necessitate a number of prophylactic measures to prevent cardiovascular diseases of fatal and non-fatal character. The received results could be used in real clinical practice of various experts: therapists, gastroenterologists, cardiologists, general practitioners and vascular surgeons.
Conclusion
a) On the basis of one gastroenterological clinic of the city of Perm as an example it was shown that in patients with IBD of middle age the incidence of cardiovascular system chronic diseases is slightly higher, than in the population of the middle age group.
b) Contrastive analysis showed that predominantly men with UC of middle and old age suffer from combination of diseases. The most typical is the combination of UC and ischemic heart disease (50% of cases).
c) In patients with CD pathology of cardiovascular system is 1.5 times more common in women than in men. Besides CD, the most common pathologies include thromboses of peripheral veins (45% of cases) and myocardial dystrophy (24.5% of cases).
d) Increasing the group of observation will probably result in data allowing to define a special category of patients with IBD for realizing primary preventive measures for cardiovascular diseases.
References
- Zvyagintseva TD (2011) Diagnostics and treatment of chronic colitis: a modern view on the problem. Newspaper “Novosti Meditsiny I Pharmatsii” gastroenterology 367.
- VT Ivashkin (2013) Recommendations on diagnostics and treatment of adult patients with Crohn’s disease. Recommendations of “The Russian gastroenterological association”, LLC Association of Coloproctologists of Russia and “Society on studying of inflammatory bowel diseases” at “Association of coloproctologists of Russia, p. 23.
- VT Ivashkin (2013) Recommendations on diagnostics and treatment of adult patients with ulcer colitis. Recommendations are developed by the commission of experts of LLC Association of Gastroenterologists of Russia, LLC Association of Coloproctologists of Russia and Society on studying of inflammatory bowel diseases at Association of coloproctologists of Russia, p. 25.
- Cromer WE, Mathis JM, Granger DN, Chaitanya GV, Alexander JS (2011) Role of endothelium in inflammatory bowel diseases. World J Gastroenterol 17(5): 578-593.
- Boiko TI (2009) Inflammation and endothelial dysfunction in chronic inflammatory bowel diseases. Russian journal of gastroenterology, hepathology, coloproctology (5): 54.
- Valuiskikh E Yu (2009) Polymorphism of genes regulators of inflammation in Crohn’s disease and nonspecific ulcerative colitis. Bulletin Siberian Branch of the Russian Academy of Medical Science 2(136): 81-89.
- Ilyashenko MG (2012) Phagocytal activity of neutrocytes in patients with inflammatory bowel diseases depending on clinical characteristics of a disease. Applied medicine 7(62): 170-173.
- Konovich EA (2009) Perinuclear anti-neutrophylic cytoplasmatic antibodies in patients with ulcer colitis and Crohn’s disease. Russian journal of gastroenterology, hepathology, coloproctology 19(5): 72-77.
- Alkan E (2014) Atherosclerosis in inflammatory bowel disease. Turk J Gastroenterol 25(Suppl 1): 20-25.
- Hitomi S (2002) Extra intestinal complications of inflammatory bowel disease. J Nat Defense Med College 27(1): 36-42.
- Talbot R, Heppell J, Dozois RR, Beart RW Jr (1986) Vascular complications of inflammatory bowel disease Mayo Clin Proc 61(2): 140-145.
- Vavricka SR, Schoepfer A, Scharl M, Lakatos PL, Navarini A, et al. (2004) Extra-intestinal manifestations of inflammatory bowel disease. J Med Clin 21(8): 1982-1992.
- Andreyev AI (2011) Modern approaches to morphological diagnostics of inflammatory bowel diseases on the material of endoscopic biopsies. Archive of pathology (1): 40-47.
- Kolesov SA (2014) Metabolites of nitrogen oxide, beams of thermal shock 70 and pro-inflammatory cytokines in children with inflammatory bowel diseases. The International Journal of Applied and Basic Researches (4): 75-78.
- Matyukhin AA (2013) Noninvasive assessment of activity of a disease in patients with inflammatory bowel diseases. Herald of new medical technologies. Electronic edition 1: 73.
- Esmon C (2003) Inflammation and thrombosis. J Thromb Haemost 1(7): 1343-1348.
- Boiko TI (2010) State of vascular endothelium function in patients with chronic inflammatory bowel diseases. Suchasna gastoenterologia 1(51): 5-10.
- Grainge MJ (2010) Venous thromboembolism during active disease and remission in inflammatory bowel disease: cohort study. Lancet 375(9715): 657-663.
- Rosello-Diez E, Christian Muñoz-Guijosa, Antonino Ginel, JM Padró (2012) Coronary Artery Aneurysms and Inflammatory Bowel Disease: A Rare Association Case Report. The Open Cardiovascular and Thoracic Surgery 5: 35-37.
- Zheng Y, X Lu, J Li, Reinhardt JD (2014) Impact of remote physiological ischemic training on vascular endothelial growth factor, endothelial progenitor cells and coronary angiogenesis after myocardial ischemia. Int J Cardiol 177(3): 894-901.
- Bernstein CN, Wajda A, Blanchard JF (2008) The incidence of arterial thromboembolic diseases in inflammatory bowel disease: populationbased study. Clin Gastroenterol Hepatol 6(1): 41-45.
- Inamdar SA (2012) Increased risk of coronary artery disease among patients with inflammatory bowel disease. Gastroenterology 142: 792.
- Osterman MT, Yang YX, Brensinger C, Forde KA, Lichtenstein GR (2011) No Increased Risk of Myocardial Infarction Among Patients with Ulcerative Colitis or Crohn’s Disease. Clin Gastroenterol Hepatol 9(10): 875-880.
- Ramazanova AH (2015) Inflammatory bowel diseases and tromboembolic complications: new problem. Applied medicine 2(4): 90-93.
- Ramazanova AH (2014) Changes in a system of hemostasis in patients with inflammatory bowel diseases. Innovative technologies in medicine 1(4): 91-93.
- Bernstein C, Blanchard JF, Houston DS, Wajda A (2001) The incidence of deep venous thrombosis and pulmonary embolism among patients with inflammatory bowel disease. A population-based cohort study. Thromb Haemos 85(3): 430-434.
- Chung WS, Lin CL, Hsu WH, Kao CH (2015) Inflammatory bowel disease increases the risks of deep vein thrombosis and pulmonary embolism in the hospitalized patients: nationwide cohort study. Thromb Res 135(3): 492-496.
- Zezos P, G Kouklakis, F Saibil (2014) Inflammatory bowel disease and thromboembolism. World J Gastroenterol 20(38): 13863-13878.
- Buvaltsev VI (2003) Endothelium dysfunction as a new concept of prevention and treatment of cardiovascular diseases. International medical journal 6(1): 5-9.
- Tretyakova YuI (2015) Features of vascular endothelium state in patients with ulcerative colitis / Yu.I. Tretyakova//Perm medical journal 32(1): 24-29.
- Principi M, Mastrolonardo M, Scicchitano P, Gesualdo M, Sassara M, et al. (2013) Endothelial function and cardiovascular risk in active inflammatory bowel diseases. J Crohns Colitis 7(10): 427-433.
- Rellecke P, Strauer BE (2006) Chronic inflammatory bowel disease and cardiovascular complications. Med Klin 101(Suppl 1): 56-60.
- Schicho R, Marsche G, Storr M (2015) Cardiovascular complications in inflammatory bowel disease. Current drug targets. 16(3): 181-188.






























