Infection and Transmission of Disease in Residential Aged Care and Community Care Settings: Key Risk Factors and Practice Recommendations
Rasika Jayasekara1* and Marija Juraja RN2
1Senior Lecturer, School of Nursing & Midwifery, University of South Australia, South Australia
2Clinical Service Coordinator, The Queen Elizabeth Hospital, South Australia
Submission: March 07, 2019; Published: May 22, 2019
*Corresponding author: Rasika Jayasekara, Senior Lecturer, School of Nursing & Midwifery, University of South Australia, South Australia
How to cite this article: Rasika J, Marija J RN. Infection and Transmission of Disease in Residential Aged Care and Community Care Settings: Key Risk Factors and Practice Recommendations. Adv Biotech & Micro. 2019; 14(1): 555877. DOI: 10.19080/AIBM.2019.14.555877
Abstract
The objective of this study was to conduct a literature review to identify the key risk factors that contribute to the risk of infection and transmission of disease in residential aged care and community care settings. This literature review was conducted using a documented search strategy, inclusion and exclusion criteria, critical appraisal methodology and summary of the evidence. The review method utilizes the National Health and Medical Research Council (NHMRC) 2000 “How to review the evidence systematic identification and review of the scientific literature”; and NHMRC 2009, “NHMRC Level of evidence and grade of recommendations for developers of guidelines. This review included total of 43 studies and 24 guidelines relevant to the review objectives. Included guidelines were developed using available clinical guidelines, literature and expert opinion and based on different countries; Australia (n=11), UK (n=6), USA (n=6) and Netherlands (n=1). This review consists of 43 studies including systematic reviews (n=4), RCTs (n=2), cohort studies (n=13), point prevalence studies (n=11), case control studies (n=7), cross section studies (n=4), and case series (n=2) with various degree of methodological quality. Included studies and guidelines data identified several key factors; Person to person contact/ shared rooms/communal living, hospital stay and antibiotic treatments, indwelling devices, invasive interventions (fingerstick blood glucose monitoring and insulin injections), poor oral and dental hygiene, food contamination and poor nutrition, healthcare workers’ knowledge and varying infection control programs in Residential Aged Care Facilities (RACFs). It is evident that residents who lived in nursing homes were more likely to be colonized with MRSA than those living in independently owned facilities. In addition, the review found several other risk factors including environmental surfaces, unvaccinated residents, non-ambulatory status, poor hand hygiene and rotator/casual employees.
Keywords: Infection; Risk factors; Residential aged care facilities; Older adults
Introduction
The Australian Commission for Safety and Quality in Health Care (ACSQHC) has long recognized the importance of reducing Healthcare Acquired Infections (HAI) through the implementation of various programs. One of those initiatives was the collaborative review and release of the revised new Australian Guidelines for the Prevention and Control of Infection in Healthcare 2010 (AICG) with the National Health and Medical Research Council (NHMRC). This guideline provides core principles for infection prevention and control that are applicable across all areas of healthcare, however hospitals and Residential Aged Care Facilities (RACF) differ in their patient acuity, the availability of medical services, and nurse-to-patient ratios [1,2]. More fundamentally, the focus is different for the resident as the RACF is their home.
The majorities of residents in RACFs are above 65 of age and have unique predispositions to infectious diseases as a result of multiple risk factors including age, chronic diseases, antibiotic utilization, frequent hospitalization, invasive devices, poor nutritional status, cognitive deficits and compromised immunity. There is also a fine balance between risk of infection, isolating residents and the psychological health of the resident. Other contributing factors include the levels of staffing, the education required on standard and transmission-based precautions for staff and residents. Lastly, that any infection prevention methods, must be balanced with other clinical goals and the ongoing enhancement of the residents’ functional status, comfort, and quality of life [3-7].
The residents increasing medical complexity along with the ever-increasing prevalence of antimicrobial-resistant organisms places them at great risk of infection that significantly results in morbidity and mortality for the resident [5,8]. However, given the diversity of RACFs and residents, the management and prevention of infections and antimicrobial resistance is often not as clearly defined as in the acute care facility. This literature review was conducted to inform the development of practice recommendations that will assist healthcare workers and carers implement safe and quality care that promotes and facilitates the overall goal of infection prevention and control which is the creation of safe health care environments through the implementation of practices that minimize the risk of transmission of infectious agents.
Review method
The objectives of this review were to conduct a literature review to identify the key risk factors that contribute to the risk of infection and transmission of disease in residential aged care and community care settings. This literature review was conducted using a documented search strategy, inclusion and exclusion criteria, critical appraisal methodology and summary of the evidence. The review method utilizes NHMRC 2000 “How to review the evidence: systematic identification and review of the scientific literature”; and NHMRC2009, “NHMRC Level of evidence and grade of recommendations for developers of guidelines. The methodology outlined below is based on these guidelines.
Inclusion Criteria
Participants: The review included studies in which patients are described as elderly, geriatric, or older adults, or in which all patients will be aged 55 or over (many North American trials of older adult populations use a cut-off of 55 years). Where possible, participants were categorized as residential aged care or community residents.
Setting
Residential aged care is defined as care services that provide accommodation and support for people who can no longer live at home. Community care is defined as services that are provided which aim to help frail aged people and people with a disability live independently in their own homes and enjoy quality of life for as long as possible, specifically those receiving personal care under the following Department of Health and Aging (DoHA) funded programs Community Aged Care Package (CACP), Extended Aged Care at Home (EACH) and Extended Aged Care at Home (Dementia) (EACHD).
Intervention/risk factors
The review focused on interventions designed to assess the risk of infection and transmission of disease in residential aged care and community care settings. Possible risk factors could be; bed occupancy levels, level of care, staffing ratios, building design, environmental risk, staff and residents knowledge level of infection prevention and control, facilities for cleaning, availability of education and training etc.
Outcomes
The primary outcome measure was;
- Reduction of infection transmission/infection rate.
Search methods for identification of studies
the years 2001to 2011. A three-step search strategy was developed using MeSH terminology and keywords to ensure that all materials relevant to the review are captured. An initial limited search of MEDLINE was undertaken followed by an analysis of the text words contained in the title and abstract, and of the index terms used to describe the article. A second search using all identified keywords and index terms was then undertaken. Thirdly, the reference lists of all identified reports and articles were searched for additional studies.
Electronic searches
The following information sources were searched: Age Line/ AHRQ/CENTRAL (Cochrane Central Register of Controlled Trials, The Cochrane Library)/CINAHL (Cumulative Index to Nursing & Allied Health Literature)/DARE (Database of Abstracts of Reviews of Effects)/EMBASE/Joanna Briggs Institute Systematic Review Library/MEDLINE/TRIP/WHO International Clinical Trials Registry Platform (WHO ICTRP)/NHS Evidence/ISI Web of Knowledge/HTA/NHS EED/SCOPUS/Informit-Health Collection/ APIC
Results
A total of 361studies were identified as potentially relevant to the review question in the first and second steps of the literature search. Based on the title and abstract, 199 papers that were relevant to the review topic were retrieved for evaluation of methodological quality. 162 papers were excluded due to incongruity with the review objectives and/or outcomes. After reviewing the full text of the papers 15 guidelines and 117 studies were excluded. Whilst searching the reference lists of the selected studies (n=65), two papers met the inclusion criteria. Therefore, a total of 43 studies and 24 guidelines were included in the review. Included guidelines were developed using available clinical guidelines, literature and expert opinion and based on different countries; Australia (n=11), UK (n=6), USA (n=6) and Netherlands (n=1). This review consists of 43 studies including systematic reviews (n=4), RCTs (n=2), cohort studies (n=13), point prevalence studies (n=11), case control studies (n=7), cross section studies (n=4), and case series (n=2) with various degree of methodological quality.
Generally, older adults have unique predispositions to infectious diseases as a result of multiple risk factors; [1] impairments in immunity status creates a risk for disease acquisition from specific infectious pathogens (e.g. MRSA, VRE) [9-12]; older adults have an increased prevalence of underlying chronic diseases (e.g., diabetes, vascular disease) that foster risk for common community acquisition including urinary tract infection, pneumonia, and soft tissue infections [3,9,11,12,15-17]. The increased prevalence of functional and cognitive limitations (e.g. impaired swallowing, bladder and bowel incontinence, dementia) [15,18-21].
Key risk factors
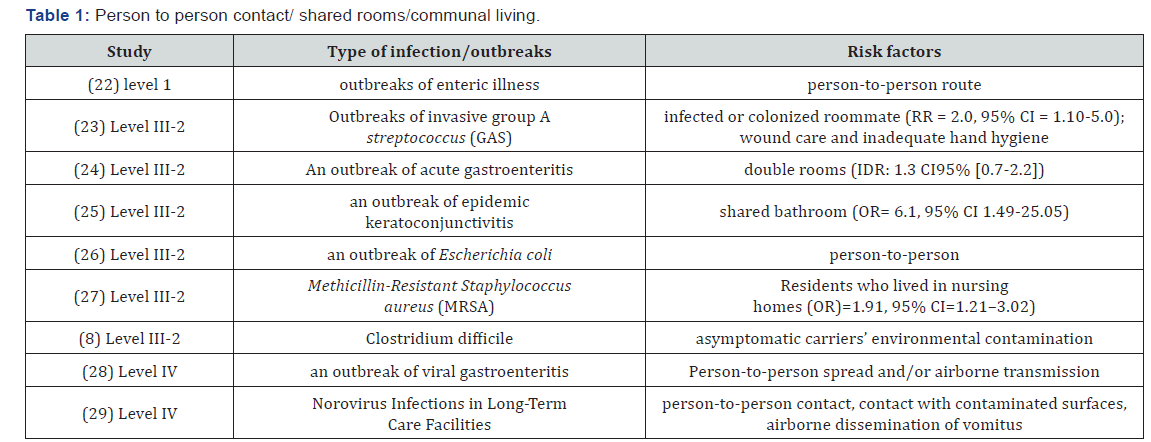
Person to person contact/ shared rooms/communal living
It is evident that residents who lived in nursing homes were more likely to be colonized with MRSA than those living in independently owned facilities. There are several risk factors were also identified in person-to-person infection transmission mainly, infected or colonized roommate, asymptomatic carriers, and communal living such as double rooms and shared bathrooms (Table 1).
Recommendations
a. During outbreaks, controlling residents’ movements, cancelling social events and restricting visitors, excluding ill staff can be recommended.
b. Outbreak management plans should be a part of the infection control standards for accreditation of aged care facilities
c. It is important to educate all staff regarding standardized infection control guidelines for RACFs, which advocate minimizing risk factors for infection
d. It is also important that direct communication throughout the outbreak is maintained with residents and visitors in regard to compliance with hand hygiene and appropriate wearing of protective equipment to minimize the risk of transmission [22-37].
Hospital stay and antibiotic treatments
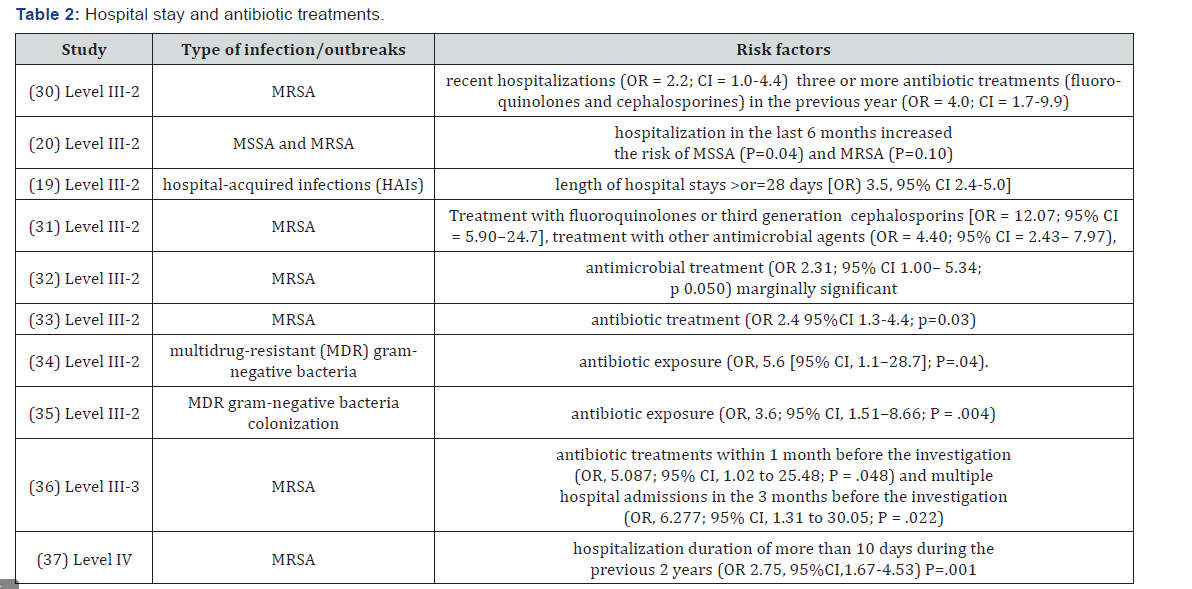
Methicillin-Resistant Staphylococcus Aureus (MRSA) infections have become a major concern in Long Term Care Facilities (LTCF). Patients that have been colonized with MRSA in general hospitals may introduce the organisms into LTCF, and these can become reservoirs for the pathogen. It can be concluded that admission to an acute care hospital within the previous 12 months and prior antimicrobial therapy with broad spectrum agents significantly raised the risk of MRSA colonization in LTCFs (Table 2). A common problem identified in the literature is the failure to distinguish infection and colonization (such as a positive swab culture of a pressure ulcer or a urine culture showing bacteriuria without signs or symptoms of infection) and the treatment of the colonization with antibiotics [4, 14, 38].
Recommendations
a. Infection control measures should be coordinated among different health care settings
b. Development of a nationally agreed minimum criterion for initiation of antibiotic therapy to improve antimicrobial prescribing in RACFs.
c. RACFs should develop antimicrobial stewardship and incorporate them into their infection control programs, including education regarding judicious antibiotic use in RACFs based on clinical needs of the resident [39-45].
Indwelling/invasive devices
Indwelling devices are used to assist with the provision of care for aged care residents due to the increasing level of functional impairment and associated dependency; however these devices such as urinary catheters, subcutaneous catheters, percutaneous enteral gastrostomy tubes, tracheostomy tubes and nasogastric tubes contribute to increase the risk of infection by providing a portal of entry for infections (Table 3).
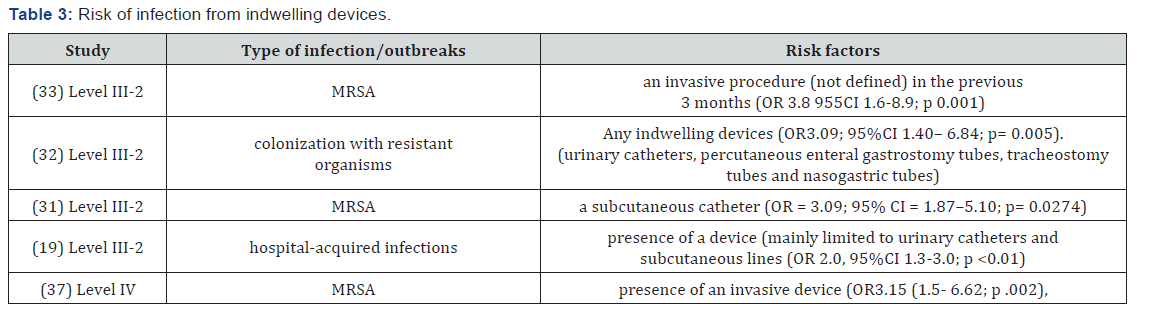
Most guidelines have also identified indwelling devices as risk factors that contribute to the risk of infection in residential aged care and community care settings (Table 1). Many risks could be attributed to the resident acquiring an infection or Multi Resistant Organism (MRO); HCW knowledge or the device, the resident’s cognitive abilities (manipulating the catheter or peripheral intravenous line with contaminated hands) increases the risk of infection and antibiotic utilization. Poor adherence to resident hygiene by HCW increased the risk of device infection, particularly a urinary tract infection. Patient placement within cohort rooms or bathrooms where residents had an indwelling device also placed the resident at risk of acquiring an MRO.
Recommendation
a. Health care workers need to be provided appropriate and ongoing education in the purpose and risk assessment of indwelling devices
b. Residents also need to be provided with education on the care of their device.
Invasive Interventions
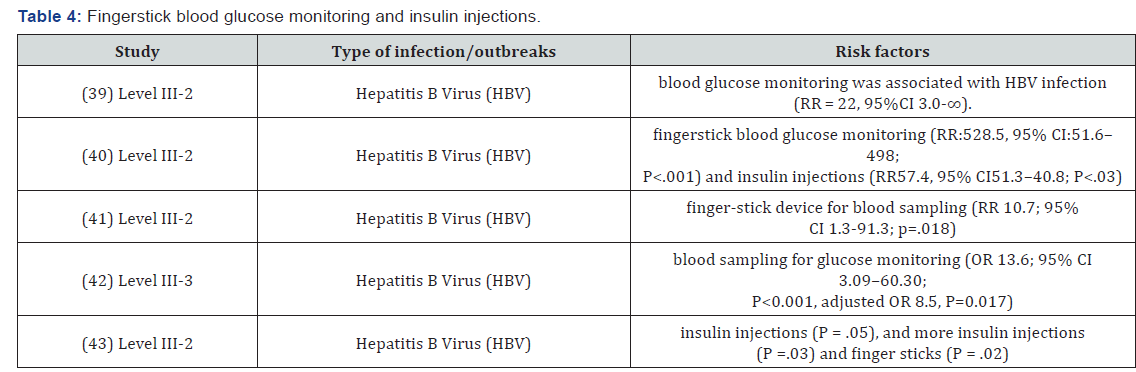
Inappropriate sharing of equipment and inadequate aseptic technique during fingerstick blood glucose monitoring and insulin injections were identified as key risk factors for reported outbreaks of Hepatitis B Virus (HBV) infection in residents of LTCFs with diabetes mellitus (Table 4).
Recommendations
The transmission of the infection could be controlled by restricting the use of finger-stick capillary sampling devices to individual patients or utilizing single use disposable sampling devices, assigning separate glucometers to individual patients
Poor oral hygiene
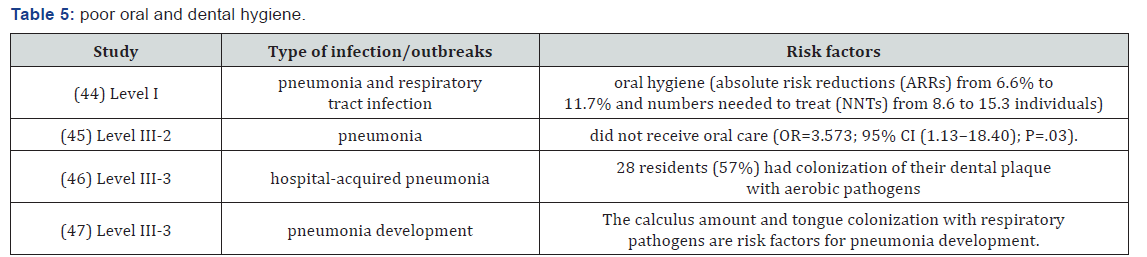
Pneumonia is a common infection in elderly people and the most common cause of mortality from nosocomial infection in elderly patients. Elderly residents in RACFs often have poor oral health due to difficulties in maintaining a sufficient level of personal oral hygiene and difficulties in accessing professional dental care. It is evident that poor oral and dental hygiene is a significant risk factor for pneumonia in residents of RACFs (Table 5).
Recommendations
a. Oral hygiene should be maintained in all residents in aged care/community care facilities to prevent the risk of nursing home–associated pneumonia.
b. Low-quality evidence suggests that professional oral care could reduce mortality due to pneumonia in nursing home residents when compared to usual care [46-48].
Food contamination and poor nutrition
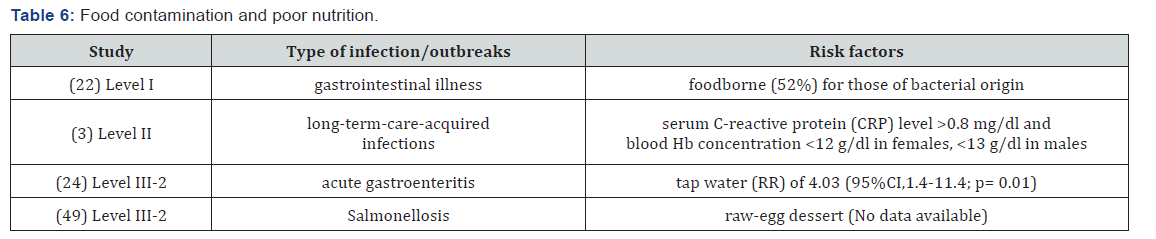
Foodborne disease outbreaks also are common in RACFs, most often caused by Salmonella and E coli, underscoring the importance of proper food preparation and storage. It is evident that older people in RACFs may be more vulnerable to infectious gastroenteritis and food-borne diseases and more likely to experience serious outcomes. Contaminated food particularly puréed food, raw-egg dessert or contaminated tap water can be considered as significant risk factors for infectious gastroenteritis. In addition, poor nutrition status; particularly serum CRP level >0.8 mg/dl and blood Hb concentration <12 g/dl in females, <13 g/dl in males may be risk factors of infection (Table 6).
Recommendations
a. Proper food preparation and storage should be monitored in RACFs
b. Food handling staff should be provided education on food safety standards and hand hygiene.
Other risk factors
It is found that colonized staff who are not aware of their MRSA status and who do not implement good infection control practices may limit the success of measures employed to reduce the spread of MRSA. It has been shown that significant discrepancies remain between infection control best practices and HCWs’ knowledge. Despite the lack of clear evidence, ongoing staff education is a critical element of any infection control program [49].
The ability also to manage an IC program is hindered further when the program is not supported by dedicated infection prevention and control staff, with or without appropriate qualifications. Also, for note, there are no nationally agreed definitions for RACF surveillance. If there is any, they are predominantly small scale, with limited benchmarking, specialist knowledge is required, and data collection is usually meaningless unless it is incorporated in the infection control (IC) program. If there is active surveillance, then for the reporting to be meaningful they must be reported not only at an individual site level but also at a state and national level [50].
The guidelines indicated that the environment also played a significant role in contributing to infection or MRO cross contamination. Having clearly defined schedules for cleaning is important in ensuring that they are carried out at the appropriate frequency. They assisted HCW in determine precisely what cleaning resource are required and if cleaning frequencies are clearly displayed, this can help reassure residents and their family/visitors that cleanliness is seen as an important issue [5, 14, 51]. This review also found several other risk factors that contributed to the risk of infections and transmission of diseases in residential aged care facilities including environmental surfaces [52-54], unvaccinated residents, non-ambulatory status, poor hand hygiene [55] and rotator/casual employees.
Recommendations
a. HCW who undertake management of IC programs require a funding model that supports a standardized program and the necessary resources to implement and sustain these activities.
b. Further exploration of defining standardized national surveillance definitions for RACFs needs to be undertaken and then reported at a state and national level to improve quality healthcare outcomes for the resident.
c. There needs to standardized cleaning guidelines including frequency/schedule of cleaning to reduce HCW confusion, particularly in outbreaks.
Conclusion
Included studies and guidelines data identified several key factors; Person to person contact/ shared rooms/communal living, hospital stay and antibiotic treatments, indwelling devices, invasive interventions (fingerstick blood glucose monitoring and insulin injections), poor oral and dental hygiene, food contamination and poor nutrition, HCWs’ knowledge and varying infection control programs in RACFs. It is evident that residents who lived in nursing homes were more likely to be colonized with MRSA than those living in independently owned facilities.
In addition, the review found several other risk factors including environmental surfaces, unvaccinated residents, non-ambulatory status/poor hand hygiene and rotator/casual employees. Implementing isolation procedures similar to those found in hospitals also may result in undesirable social and psychological implications and functional decline for residents.
The NHMRC 2010 Infection Prevention and Control guideline are generally applicable across most settings in Australia, but from the literature review it has highlighted the need to develop specific guidelines to direct HCWs and Infection Control Professionals (ICPs) in managing IC programs, as well as improving the quality healthcare for the residents within RACF and community.
Acknowledgment
The original review (2011) was supported by the National Health and Medical Research Council (NHMRC) Australia [2011/0161]. This is the updated review [2019] with no funding source.
References
- da Silveira M, da Cunha MLRS, de Souza CSM, Correa AAF, Fortaleza CMCB (2018) Nasal colonization with methicillin-resistant Staphylococcus aureus among elderly living in nursing homes in Brazil: risk factors and molecular epidemiology. Ann Clin Microbiol Antimicrob 17(1):18.
- Perez-Eslava M, Lopez-Ruiz N, Flores-Cebada EM, Rodriguez-Iglesias M, Galan-Sanchez F (2019) Staphylococcus aureus colonization in an institutionalized elderly population in the Bay of Cadiz area, Spain: prevalence and associated risk factors. Med Clin (Barc) 152(4): 141- 144.
- Aquilani R, Zuccarelli GC, Dioguardi FS, Baiardi P, Frustaglia A, et al. (2011) Effects of oral amino acid supplementation on long-term-careacquired infections in elderly patients. Arch Gerontol Geriatr 52(3): e123-128.
- Care Quality Commission (2009) Working together to prevent and control infections A study of the arrangements for infection prevention and control between hospitals and care homes.
- Furuno JP, Kaye KS, Malani PN, Mody L (2010) Implementing long-term care infection control guidelines into practice: A case-based approach. Annals of Long-Term Care 18 (2): 28-33.
- Smith PW, Bennett G, Bradley S, Drinka P, Lautenbach E, et al. (2008) SHEA/APIC Guideline: Infection prevention and control in the longterm care facility. Am J Infect Control 36(7): 504-535.
- Kariya N, Sakon N, Komano J, Tomono K, Iso H (2018) Current prevention and control of health care associated infections in longterm care facilities for the elderly in Japan. J Infect Chemother 24(5): 347-352.
- Riggs MM, Sethi AK, Zabarsky TF, Eckstein EC, Jump RLP, et al. (2007) Asymptomatic carriers are a potential source for transmission of epidemic and nonepidemic Clostridium difficile strains among longterm care facility residents. Clin Infect Dis 45(8): 992-998.
- Communicable Diseases Network Australia (CDNA) (2009) A Practical Guide to assist in the Prevention and Management of Influenza Outbreaks in Residential Care Facilities in Australia. In: Australia Co, editor. Commonwealth of Australia.
- Bayside Health (Victoria) (2007) Antibiotic resistant organisms.
- Mc Culloch J (2007) Infection control guidelines for community settings. Gloucestershire: Health Protection Agency South West.
- Siegel JD, Rhinehart E, Jackson M, Chiarello L, Committee HICPA (2007) 2007 Guideline for Isolation Precautions: Preventing Transmission of Infectious Agents in Health Care Settings. Am J Infect Control 35(10 Suppl 2): S65-164.
- McMullan M, Trinick T (2010) Best practice guidance for the provision of domiciliary eyecare in nursing/residential homes and day care facilities: Best Practice Statement 7 & 8. Guidelines & Audit Implementation Network p. 28.
- NHMRC (2010) Australian Guidelines for the Prevention and Control of Infection in Healthcare.
- Dijkers FWD (2007) Nursing home, residential- and home care MRSA Infection Prevention Working Party.
- High KP, Bradley SF, Gravenstein S, Mehr DR, Quagliarello VJ, et al. (2009) Clinical practice guideline for the evaluation of fever and infection in older adult residents of long-term care facilities: 2008 update by the Infectious Diseases Society of America. Clinical Infectious Diseases 48(2): 149-171.
- Maddock L, Andrews S, Henderson HJ, Trail P, Loades N, et al. (2010) A report on the management of diarrhea in care homes: including an assessment of the implications for recognition and management of residents with Clostridium difficile infection In: Surrey and Sussex Health Protection Unit icw BaSMS.
- Stuart RL, Marshall C, McLaws M-L, Boardman C, Russo PL, et al. (2011) ASID/AICA position statement - Infection control guidelines for patients with Clostridium difficile infection in healthcare settings. Healthcare Infection 16(1): 33-39.
- Brusaferro S, Regattin L, Silvestro A, Vidotto L (2006) Incidence of hospital-acquired infections in Italian long-term-care facilities: a prospective six-month surveillance. J Hosp Infect 63(2): 211-215.
- Lasseter G, Charlett A, Lewis D, Donald I, Howell-Jones R, et al. (2010) Staphylococcus aureus carriage in care homes: Identification of risk factors, including the role of dementia. Epidemiology and Infection 138 (5): 686-696.
- Pop-Vicas A, Mitchell SL, Kandel R, Schreiber R, D Agata EMC (2008) Multidrug-resistant gram-negative bacteria in a long-term care facility: prevalence and risk factors. J Am Geriatr Soc 56 (7): 1276-1280.
- Greig JD, Lee MB (2009) Enteric outbreaks in long-term care facilities and recommendations for prevention: a review. Epidemiol Infect 137(02):145-155.
- Greene CM, Van Beneden CA, Javadi M, Skoff TH, Beall B, et al. (2005) Cluster of deaths from group A streptococcus in a long-term care facility - Georgia, 2001. Am J Infect Control 33 (2): 108-113.
- Luque Fernandez MA, Galmes Truyols A, Herrera Guibert D, Arbona Cerda G, Sancho Gaya F (2008) Cohort study of an outbreak of viral gastroenteritis in a nursing home for elderly, Majorca, Spain, February 2008. Euro surveill 13(51).
- Sendra-Gutierrez JM, Martin-Rios D, Casas I, Saez P, Tovar A, et al. (2004) An outbreak of adenovirus type 8 keratoconjunctivitis in a nursing home in Madrid. Euro Surveill 9(3): 27-30.
- Afza M, Hawker J, Thurston H, Gunn K, Orendi J (2006) An outbreak of Escherichia coli O157 gastroenteritis in a care home for the elderly. Epidemiol Infect 134 (6): 1276-1281.
- Baldwin NS, Gilpin DF, Hughes CM, Kearney MP, Gardiner DA, et al. (2009) Prevalence of methicillin-resistant Staphylococcus aureus colonization in residents and staff in nursing homes in Northern Ireland. J Am Geriatr Soc 57(4): 620-626.
- Miller M, Carter L, Scott K, Millard G, Lynch B, (2002) Norwalk-like virus outbreak in Canberra: implications for infection control in aged care facilities. Commun dis intel Q Rep 26(4): 555-561.
- Rajagopalan S, Yoshikawa TT (2016) Norovirus Infections in Long- Term Care Facilities. J Am Geriatr Soc 64(5): 1097-1103.
- Brugnaro P, Fedeli U, Pellizzer G, Buonfrate D, Rassu M, et al. (2009) Clustering and risk factors of methicillin-resistant staphylococcus aureus carriage in two italian long-term care facilities. Infection 37(3): 216-221.
- Eveillard M, Charru P, Rufat P, Hippeaux M-C, Lancien E, et al. (2008) Methicillin-resistant Staphylococcus aureus carriage in a long-term care facility: hypothesis about selection and transmission. Age Ageing 37(3): 294-299.
- March A, Aschbacher R, Dhanji H, Livermore DM, Böttcher A, et al. (2010) Colonization of residents and staff of a long-term-care facility and adjacent acute-care hospital geriatric unit by multiresistant bacteria. Clinical Microbiol Infection 16(7): 934-944.
- Mendelson G, Yearmack Y, Granot E, Ben-Israel J, Colodner R, et al. (2003) Staphylococcus aureus carrier state among elderly residents of a long-term care facility. Journal of the American Medical Directors Association 4(3): 125-127.
- O Fallon E, Kandell R, Schreiber R, D Agata EMC (2010) Acquisition of multidrug-resistant gramnegative bacteria: Incidence and risk factors within a long-term care population. Infect Control Hosp Epidemi 31(11): 1148-1153.
- O Fallon E, Schreiber R, Kandel R, D Agata E MC (2009) Multidrugresistant gram-negative bacteria at a long-term care facility: Assessment of residents, healthcare workers, and inanimate surfaces. Infection Control and Hospital Epidemiology 30 (12):1172-1179.
- Vovko P, Retelj M, Cretnik TZ, Jutersek B, Harlander T, et al. (2005) Risk factors for colonization with methicillin-resistant Staphylococcus aureus in a long-term-care facility in Slovenia. Infect Control Hosp Epidemiol 26(2): 191-195.
- Barr B, Wilcox MH, Brady A, Parnell P, Darby B, et al. (2007) Prevalence of Methicillin Resistant Staphylococcus aureus Colonization Among Older Residents of Care Homes in the United Kingdom. Infect Control and Hosp Epidemol 28(7): 853-859.
- ACSQHC (2010) Reducing harm to patients from health care associated infection: the role of surveillance 2010 Chapter 13 Residential agedcare facilities.
- Diercke M, Monazahian M, Petermann H, Gerlich WH, Schuttler CG, et al. (2010) Hepatitis B outbreak in a nursing home associated with reusable lancet devices for blood glucose monitoring, Northern Germany 2010. J Med Virol 87(4): 583-588.
- Counard CA, Perz JF, Linchangco PC, Christiansen D, Ganova-Raeva L, et al. (2010) Acute Hepatitis B outbreaks related to fingerstick blood glucose monitoring in two assisted living facilities. J Am Geriatr Soc 58(2): 306-311.
- De Schrijver K, Maes I, Van Damme P, Tersago J, Moes E, et al. (2005) An outbreak of nosocomial hepatitis B virus infection in a nursing home for the elderly in Antwerp (Belgium). Acta Clin Belg 60(2): 63-69.
- Dreesman JM, Baillot A, Hamschmidt L, Monazahian M, Wend UC, et al. (2006) Outbreak of hepatitis B in a nursing home associated with capillary blood sampling. Epidemiol Infect 134(5): 1102-1103.
- Khan AJ, Cotter SM, Schulz B, Hu X, Rosenberg J, et al. (2002) Nosocomial transmission of hepatitis B virus infection among residents with diabetes in a skilled nursing facility. Infect Control Hosp Epidemiol 23(6): 313-318.
- Sjogren P, Nilsson E, Forsell M, Johansson O, Hoogstraate J (2008) A systematic review of the preventive effect of oral hygiene on pneumonia and respiratory tract infection in elderly people in hospitals and nursing homes: effect estimates and methodological quality of randomized controlled trials. Journal of the American Geriatrics Society 56(11): 2124-2130.
- Bassim CW, Gibson G, Ward T, Paphides BM, DeNucci DJ (2008) Modification of the Risk of Mortality from Pneumonia with Oral Hygiene Care. J Am Geriatr Soc 56(9): 1601-1607.
- El-Solh AA, Pietrantoni C, Bhat A, Okada M, Zambon J, et al. (2004) Colonization of dental plaques: a reservoir of respiratory pathogens for hospital-acquired pneumonia in institutionalized elders. CHEST 126(5):1575-1582.
- Hong C, Aung MM, Kanagasabai K, Lim CA, Liang S, et al. (2018) The association between oral health status and respiratory pathogen colonization with pneumonia risk in institutionalized adults. International journal of dental hygiene 16(2): e96-e102.
- Liu C, Cao Y, Lin J, Ng L, Needleman I, et al. (2018) Oral care measures for preventing nursing home-acquired pneumonia. Cochrane database of syst rev 9: Cd012416.
- Roberts-Witteveen AR, Campbell BA, Merritt TD, Massey PD, Shadbolt CT, et al. (2009) Egg -associated Salmonella outbreak in an aged care facility, New South Wales Communicable diseases intelligence 33 (1): 49-52.
- Mody L, Saint S, Galecki A, Chen S, Krein SL (2010) Knowledge of Evidence-Based Urinary Catheter Care Practice Recommendations Among Healthcare Workers in Nursing Homes. J Am Geriatr Soc 58(8):1532-1537.
- (2006) Department of Health United Kingdom. Infection Control Guidance for Care Homes. In: Health.
- O Fallon E, Schreiber R, Kandel R, D Agata EM (2009) Multidrugresistant gram-negative bacteria at a long-term care facility: assessment of residents, healthcare workers, and inanimate surfaces. Infect control hosp epidemiol 30(12): 1172-1179.
- Shams AM, Rose LJ, Edwards JR, Cali S, Harris AD, et al. (2016) Assessment of the Overall and Multidrug-Resistant Organism Bioburden on Environmental Surfaces in Healthcare Facilities. Infect control hosp epidemiol 37(12): 1426-1432.
- Wu HM, Fornek M, Schwab KJ, Chapin AR, Gibson K, et al. (2005) A norovirus outbreak at a long-term-care facility: the role of environmental surface contamination. Infect Control Hosp Epidemiol 26(10): 802- 810.
- Park GW, Williamson KJ, De Bess E, Cieslak PR, Gregoricus N, et al. (2018) High Hand Contamination Rates During Norovirus Outbreaks in Long-Term Care Facilities. Infect Control Hosp Epidemiol 39(2): 219-221.






























