Abstract
Background: Posterior shoulder dislocations are rare, accounting for only 2–5% of all shoulder dislocations, yet they are frequently missed on initial assessment. Chronic or neglected cases, defined as unreduced dislocations beyond three weeks, present unique diagnostic and therapeutic challenges, particularly when complicated by a reverse Hill–Sachs lesion.
Case Presentation: We report the case of a 42-year-old right-hand dominant male who presented three weeks after an electric shock injury with pain, stiffness, and loss of function in the right shoulder. Imaging revealed a neglected, locked posterior dislocation with a reverse Hill–Sachs lesion involving approximately 30% of the articular surface. Open reduction was performed via a deltopectoral approach. The reverse Hill–Sachs defect was managed with a modified McLaughlin procedure-transfer of the subscapularis tendon into the defect-reinforced with a suture anchor and two cancellous screws. Postoperatively, a structured rehabilitation protocol was followed. At three months, the patient demonstrated painless forward flexion to 110°, abduction to 100°, internal rotation to 25°, and radiographic evidence of stable reduction without re-dislocation.
Discussion: Posterior shoulder dislocations are commonly overlooked due to subtle clinical and radiographic findings. Neglected cases often require open surgical intervention. The choice of surgical procedure depends on the size of the reverse Hill–Sachs lesion: defects <25% may be treated with reduction alone, 25–40% typically require a modified McLaughlin procedure, while >40% defects may necessitate reconstructive grafting or arthroplasty. Literature supports the modified McLaughlin technique as the most reliable joint-preserving option for medium-sized defects.
Conclusion: This case emphasizes the importance of high clinical suspicion, appropriate imaging, and defect-based surgical management in neglected posterior dislocations. The modified McLaughlin procedure remains an effective and reproducible technique for medium-sized reverse Hill–Sachs lesions, providing stable reduction, pain relief, and functional recovery.
Keywords:Posterior shoulder dislocation; Neglected dislocation; Reverse Hill–Sachs lesion; Modified McLaughlin procedure; Electric shock injury
Introduction
Shoulder dislocation is the most common large joint dislocation encountered in clinical practice, but posterior dislocations remain rare, accounting for only 2–5% of all cases [1-3]. Unlike anterior dislocations, posterior dislocations are frequently missed at initial presentation, with reported rates of misdiagnosis as high as 60–79% [4-6]. The clinical presentation is often subtle, and standard anteroposterior radiographs may appear deceptively normal, necessitating additional imaging such as axillary or scapular Y-views and cross-sectional modalities for confirmation [2,6,7]. Posterior dislocations typically occur due to axial loading of the adducted, internally rotated arm or secondary to violent involuntary muscle contractions [3,8,9]. The latter mechanism is classically associated with epileptic seizures and electrical shock injuries, where sudden and powerful contraction of the subscapularis, pectoralis major, latissimus dorsi, and teres major overwhelms the external rotators, forcing the humeral head posteriorly against the glenoid [3,8,10].
A particularly challenging subset of cases involves neglected or chronic posterior shoulder dislocations, defined as those left unreduced for more than three weeks [4,11,12]. In such cases, fibrous tissue, joint capsule contracture, and articular damage make closed reduction virtually impossible. Furthermore, these injuries are often accompanied by a reverse Hill–Sachs lesion, an impression fracture of the anteromedial humeral head that occurs in up to 86% of posterior dislocations [2,13]. The size of this defect largely determines the choice of surgical management. Several surgical options have been described depending on the extent of humeral head involvement. When the defect involves <25% of the articular surface, closed or open reduction alone may suffice [2,5]. For moderate defects (25–40%), the modified McLaughlin procedure-involving transfer of the subscapularis tendon or lesser tuberosity into the defect-has become the treatment of choice [6,15-17].
For larger defects exceeding 40%, particularly in chronic cases or elderly patients, reconstructive procedures with structural bone grafts, rotational osteotomy, or even arthroplasty may be necessary [11,18,19]. The modified McLaughlin technique, first described by Neer in 1970 as an evolution of McLaughlin’s original procedure [5,13], has shown reproducible outcomes with restoration of stability and function in neglected posterior dislocations [14,15-17]. Modern systematic reviews confirm its role as the mainstay treatment for moderate reverse Hill–Sachs lesions, with arthroplasty reserved for more extensive humeral head compromise [20]. In this report, we present a rare case of a neglected locked posterior shoulder dislocation following electrical injury in a 42-year-old male, treated successfully with open reduction and a modified McLaughlin procedure augmented by an anchor and cancellous screw fixation. We also provide a comprehensive review of the literature regarding epidemiology, diagnostic challenges, surgical techniques, and outcomes of neglected posterior dislocations.
Case Report
A 42-year-old right-hand dominant male presented to our department three weeks after sustaining an electric shock injury at home. Immediately following the event, he experienced severe pain and functional limitation in the right shoulder but did not seek medical attention. He presented with persistent pain, stiffness, and inability to elevate the arm.
Clinical Examination Revealed
The shoulder held in internal rotation, loss of the normal shoulder contour with posterior fullness, marked restriction of abduction and forward flexion, external rotation severely limited and painful, and neurovascular examination unremarkable.
Radiological Evaluation
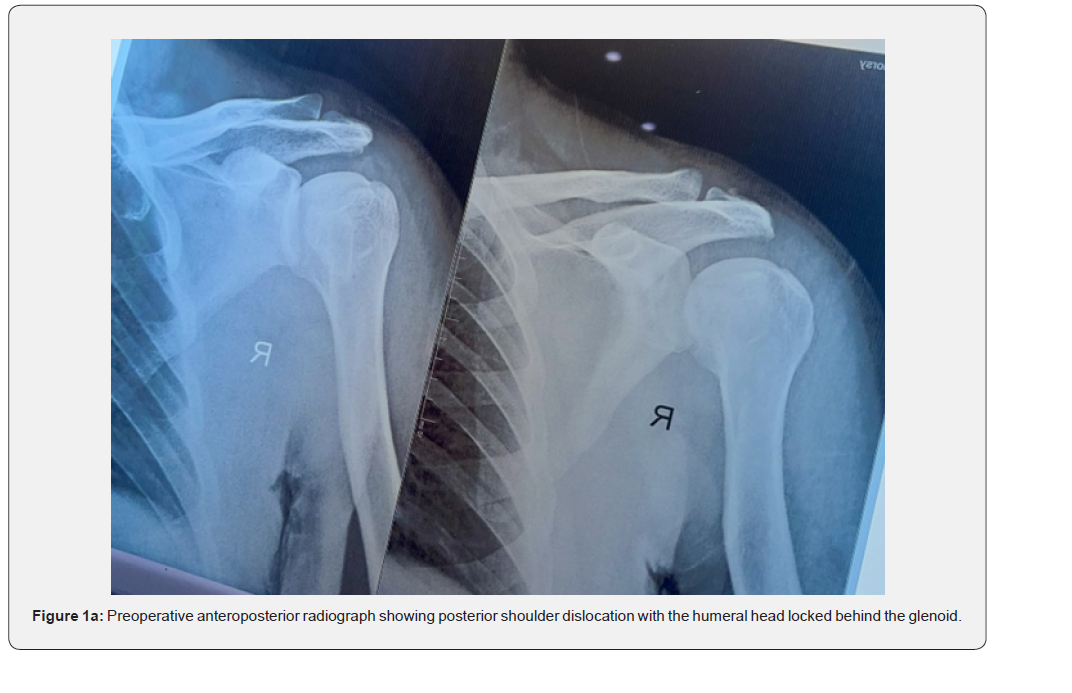
Preoperative anteroposterior and axillary radiographs demonstrated a neglected locked posterior shoulder dislocation with a reverse Hill–Sachs defect (Figure 1a). Computed tomography and MRI confirmed a posteriorly locked humeral head with approximately 30% involvement of the articular surface (Figure 2a–2d).

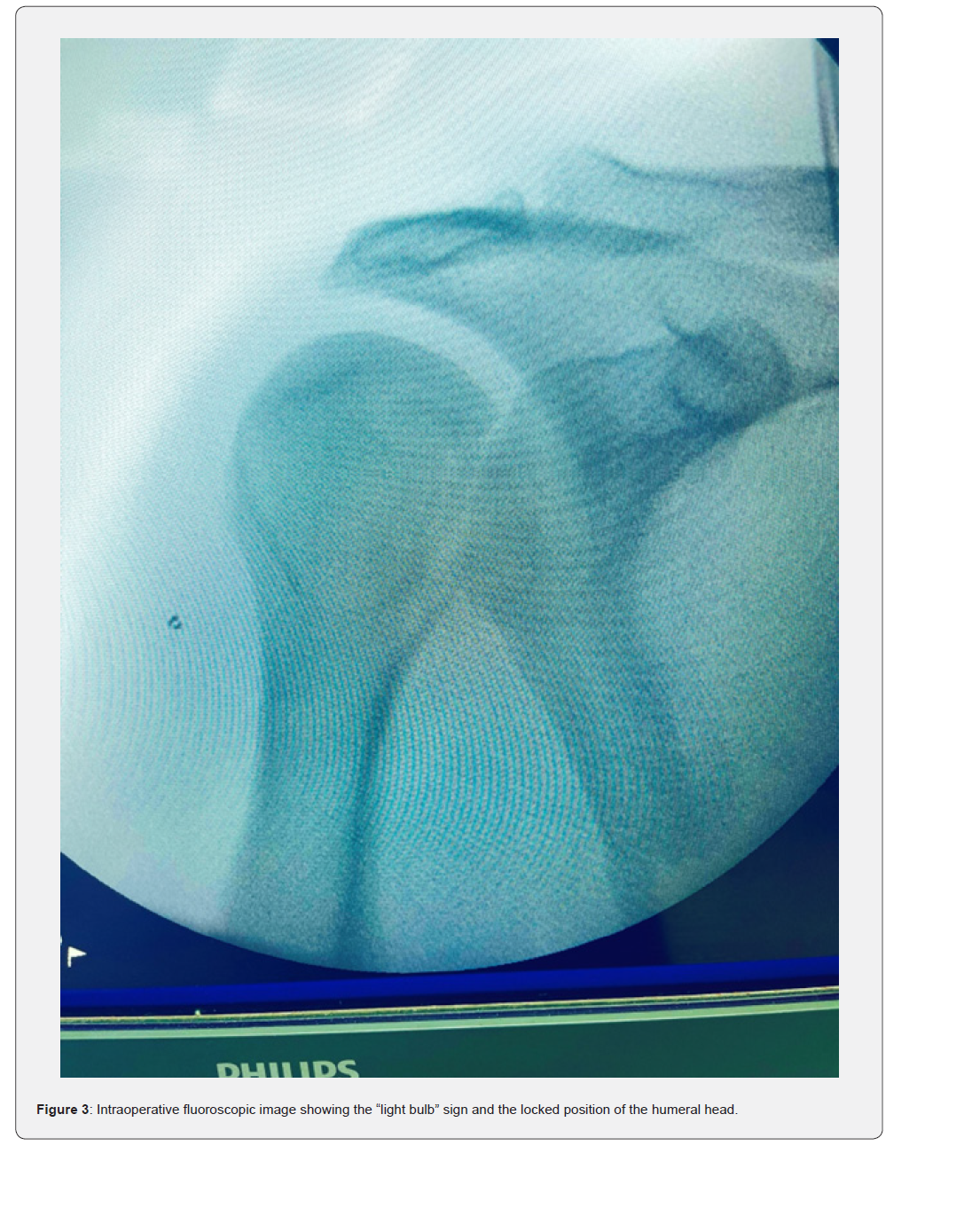
Intraoperative fluoroscopic images further delineated the light bulb sign and locked position of the humeral head (Figure 3).
Surgical Technique
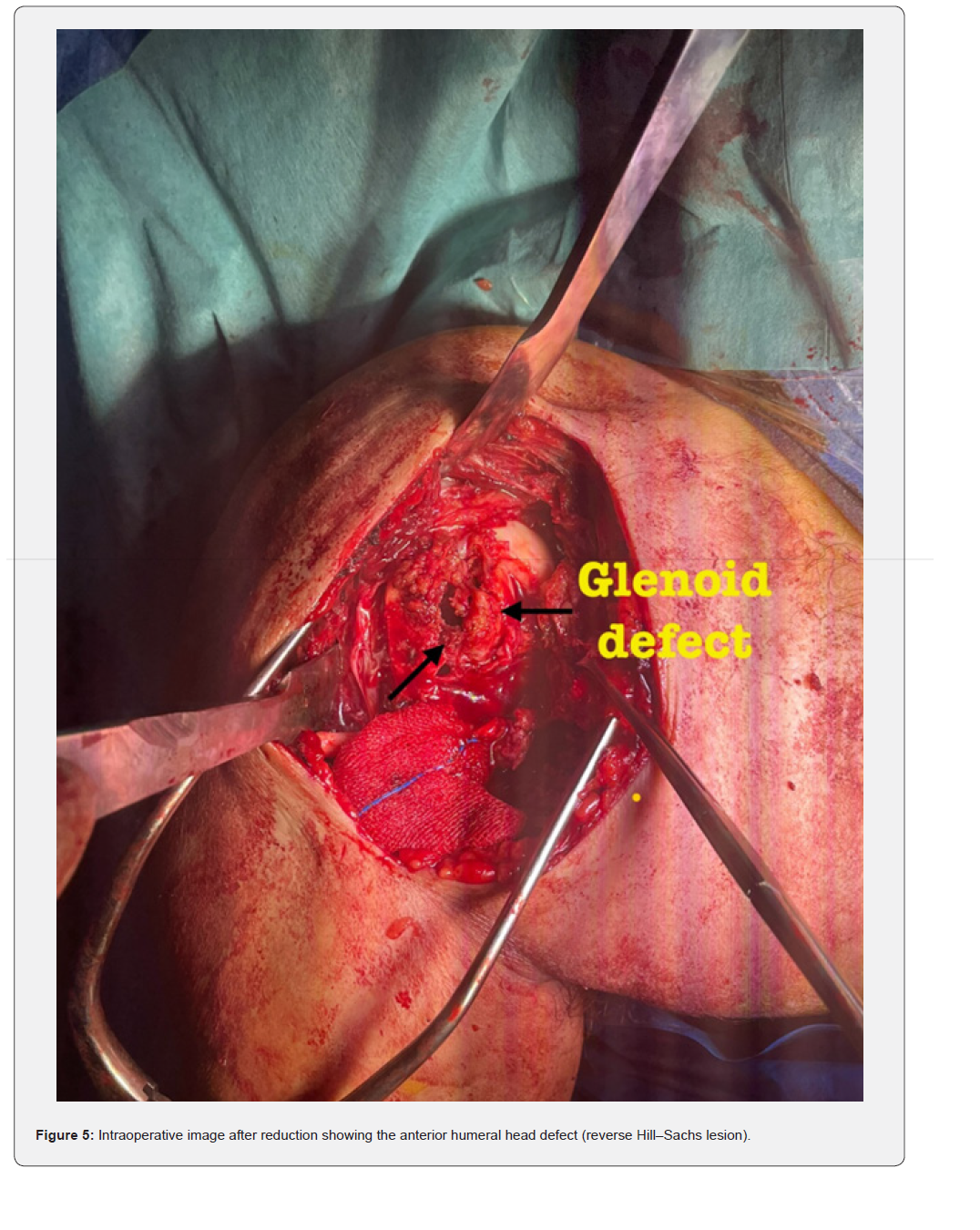
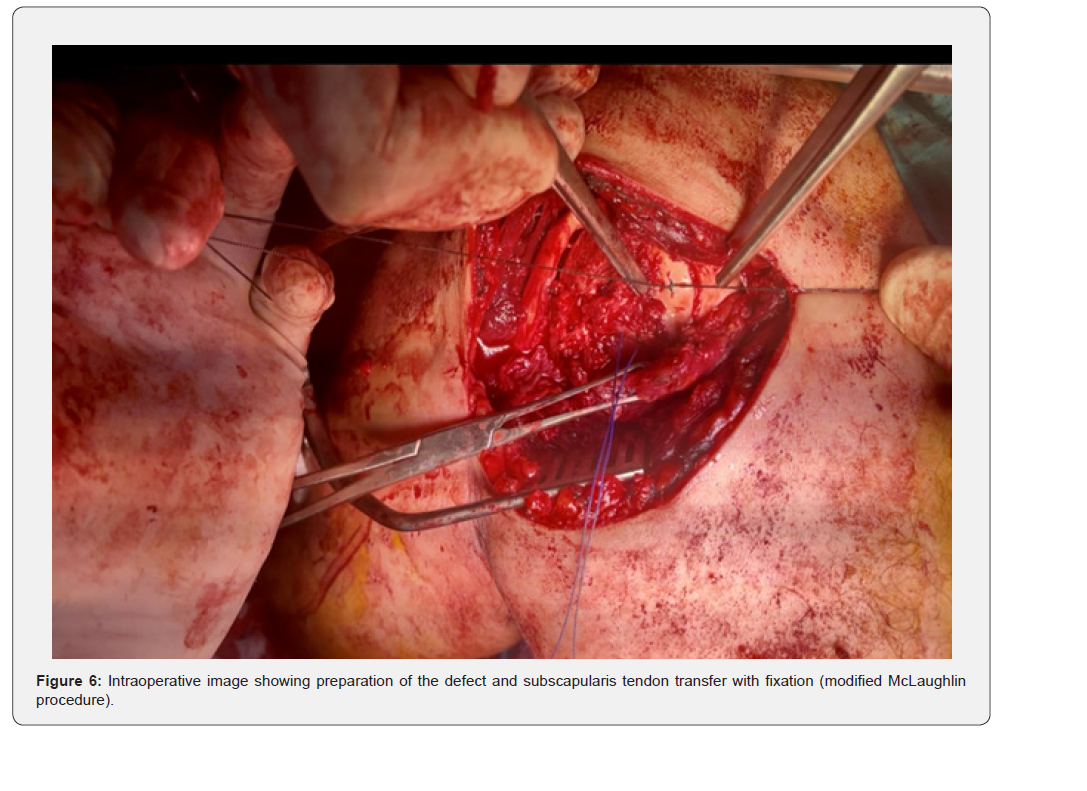
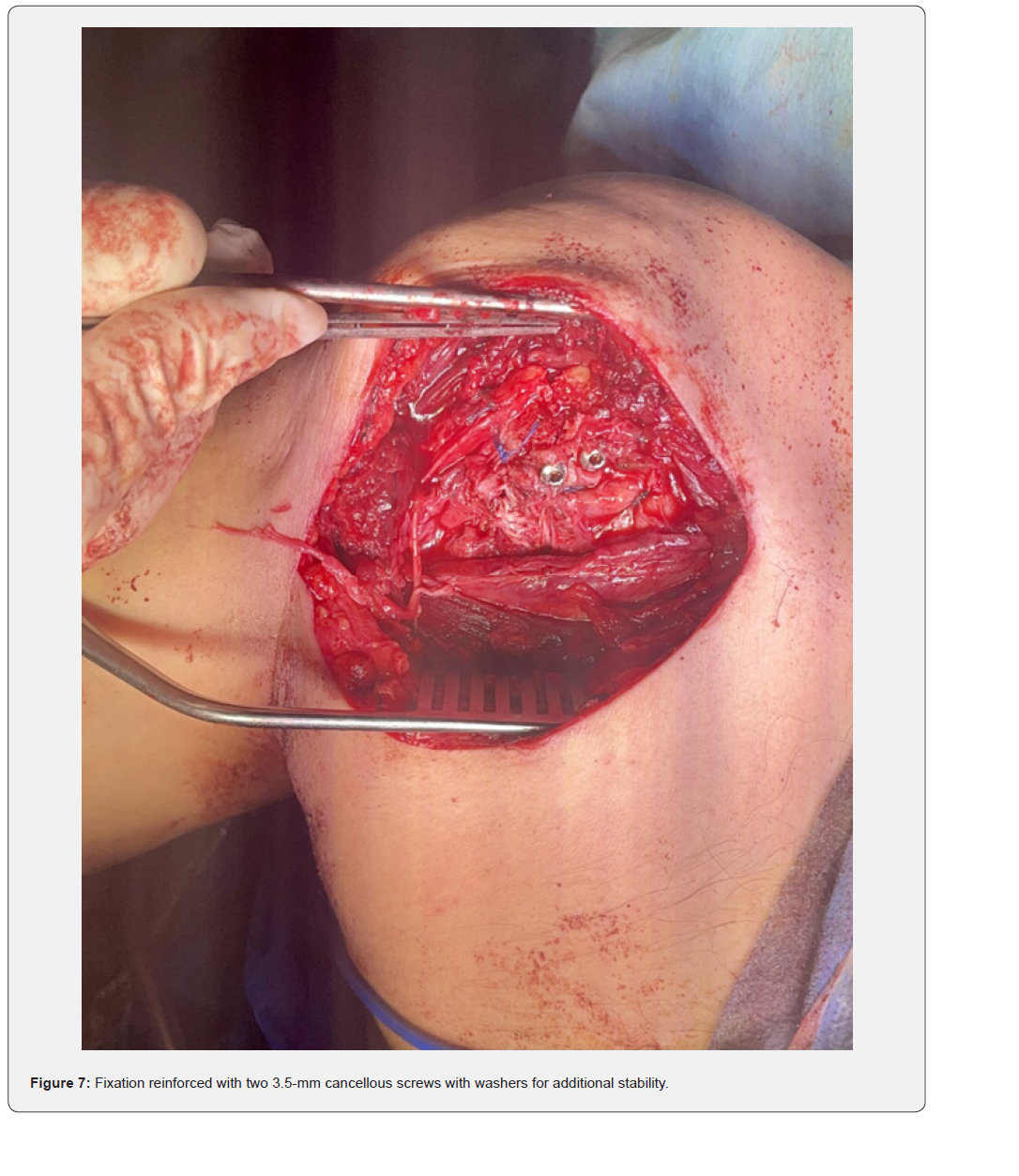
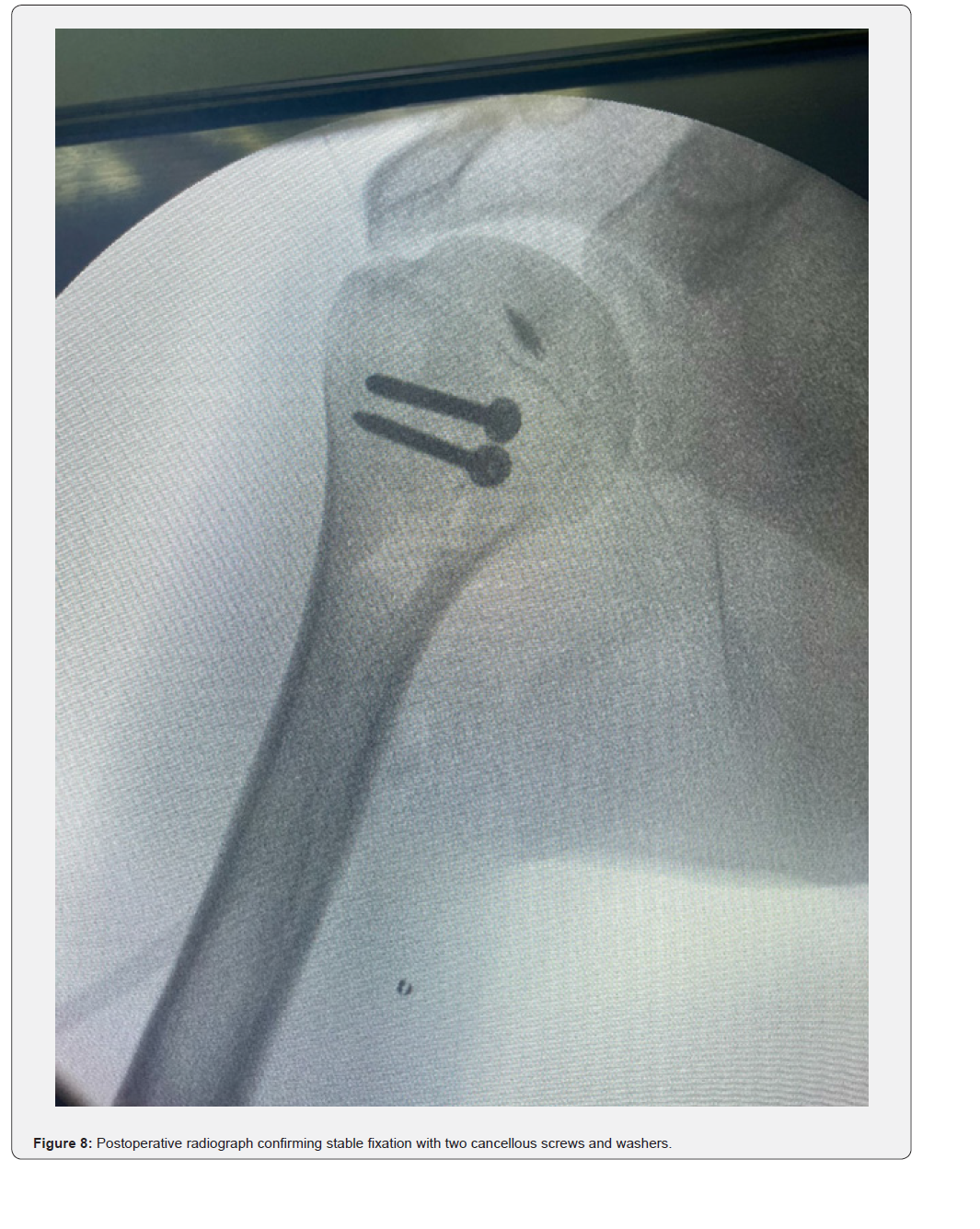
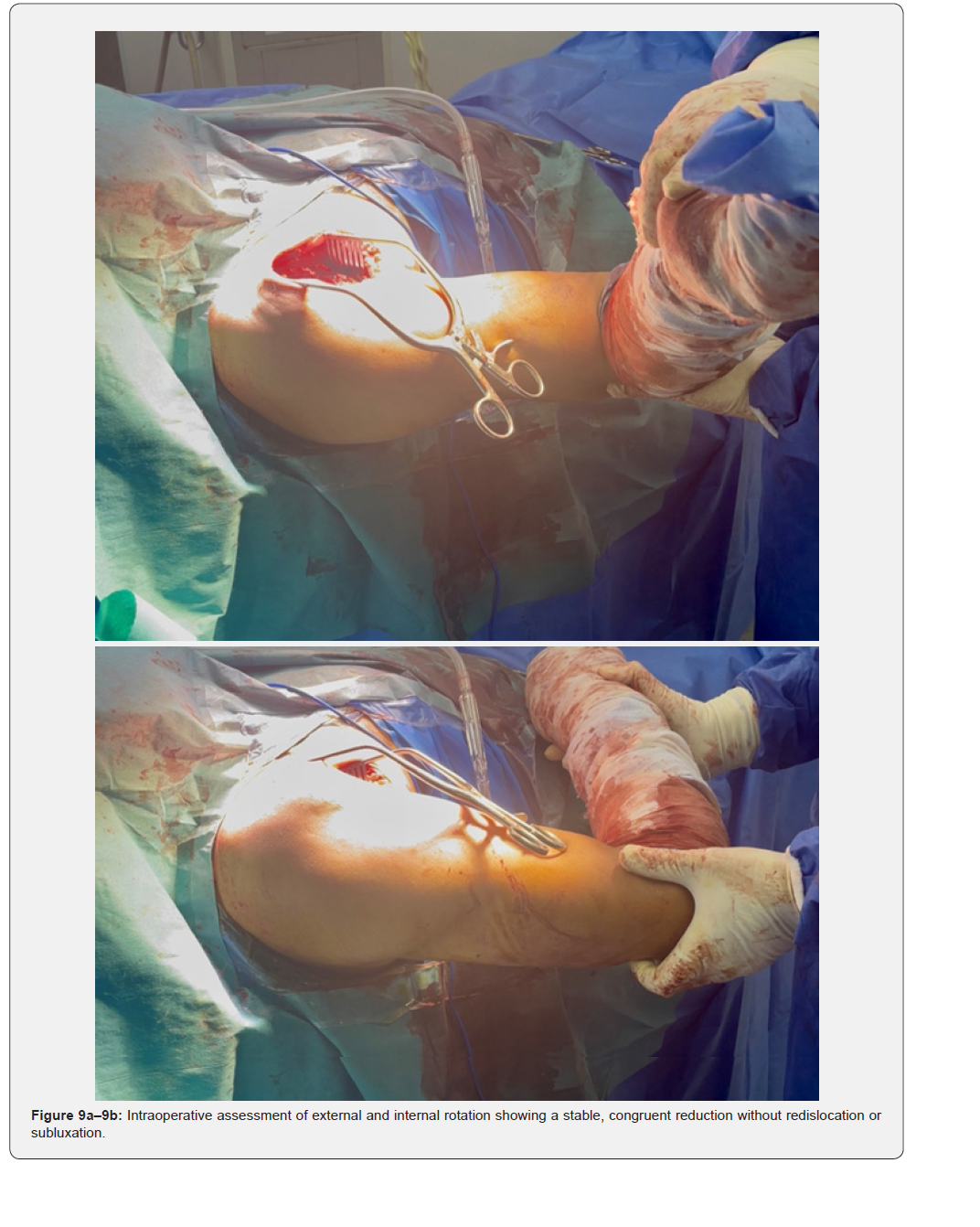
The patient was placed in a beach-chair position under general anesthesia. A standard deltopectoral approach was used. Intraoperatively, the humeral head was found locked posteriorly with fibrous tissue interposition (Figure 4). Open reduction was achieved after careful release of fibrous adhesions and identification of the anterior glenoid defect (Figure 5). The reverse Hill–Sachs defect was managed by a modified McLaughlin procedure: transfer of the subscapularis tendon into the defect using a suture anchor (Figure 6). Fixation was reinforced with two 3.5 mm cancellous screws with washers for stability (Figure 7). Intraoperative fluoroscopy confirmed concentric reduction and stable fixation (Figure 8). External and internal rotation was tested intraoperatively and demonstrated a stable, congruent reduction without evidence of redislocation or subluxation (Figure 9a–9b).

Postoperative Protocol
The shoulder was immobilized in an abduction brace for 4 weeks. Passive pendulum exercises were initiated at 2 weeks. Active-assisted range of motion began at 4–6 weeks. Strengthening exercises commenced at 10–12 weeks postoperatively.
Outcome
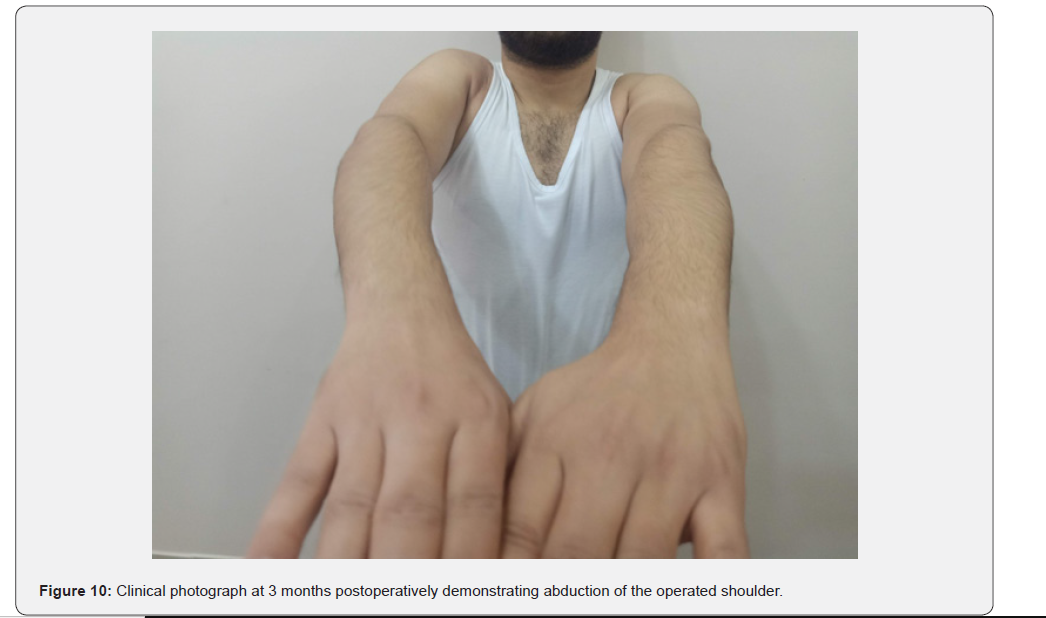
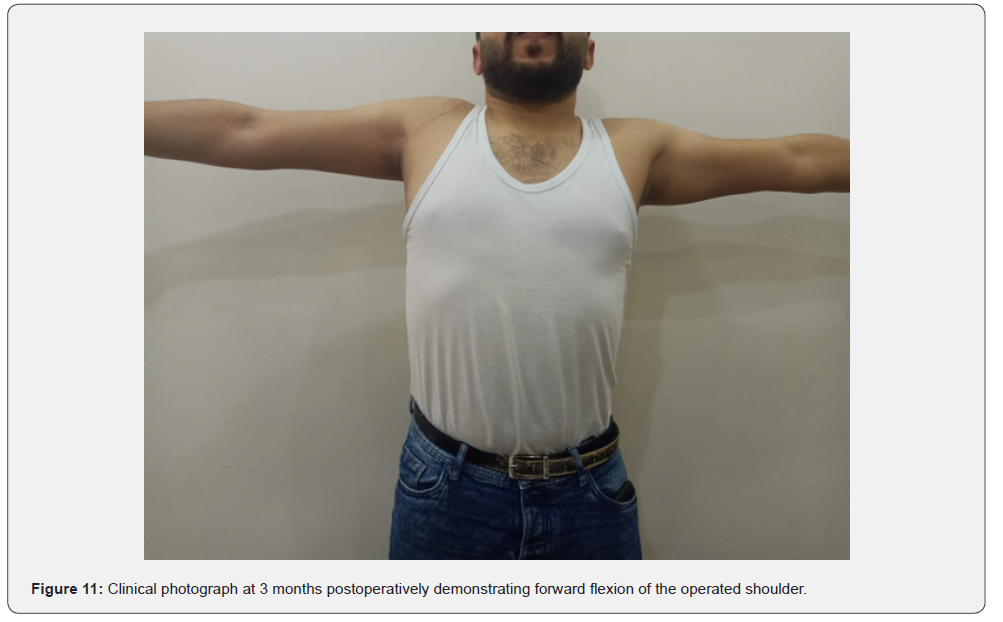
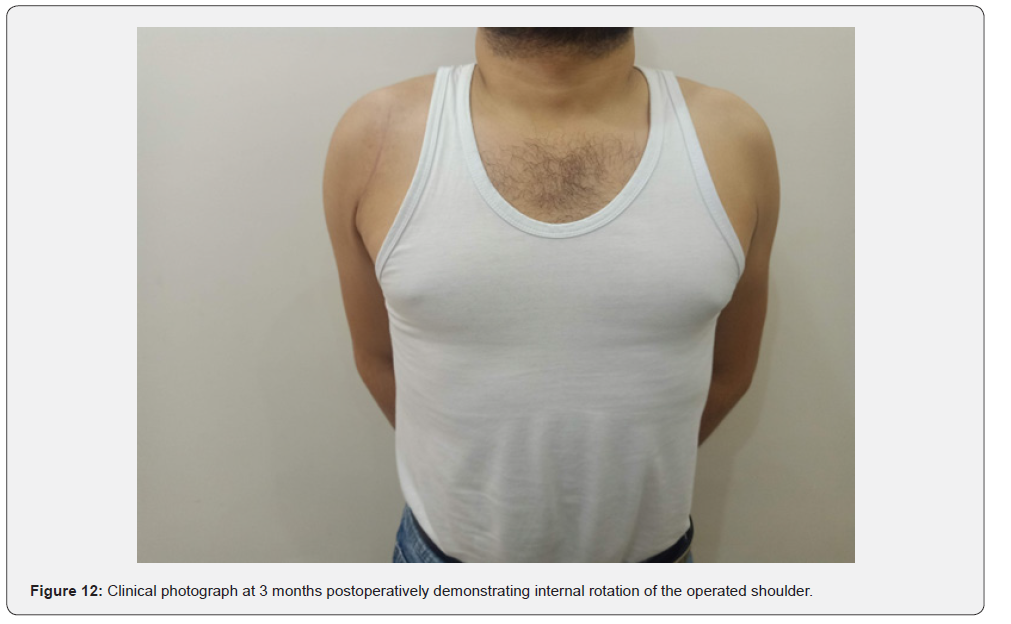
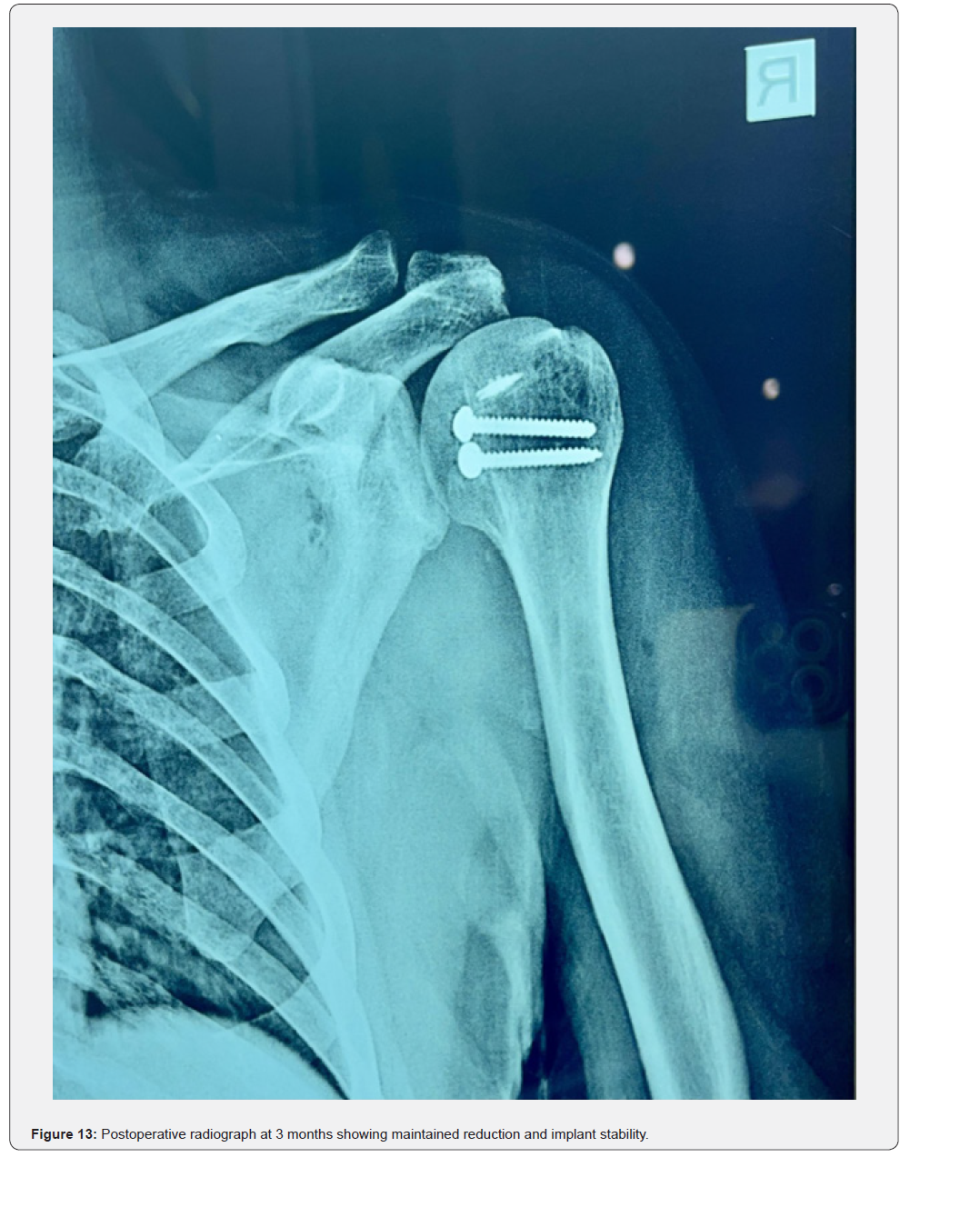
At three months, the patient had regained painless functional mobility with forward flexion to 110°, abduction to 100°, and internal rotation to 25° (Figures 10-12). Postoperative radiographs at three months demonstrated maintained reduction and implant stability without loosening or redislocation (Figure 13). At one-year follow-up, the patient remained pain-free, with forward flexion 140°, abduction 130°, external rotation 20°, and internal rotation 30°. The Constant–Murley score improved from 22 preoperatively to 82, with no evidence of avascular necrosis or post-traumatic arthritis.
Discussion
Posterior shoulder dislocation is an uncommon injury, comprising only 2–5% of all shoulder dislocations [1-3]. It is often under-recognized, with up to 79% of cases missed initial assessment due to subtle radiographic findings and nonspecific clinical signs [4-6]. In our patient, the etiology was an electric shock, a well-documented but relatively rare mechanism compared to epileptic seizures and high-energy trauma [3,8,9].
Mechanism and Pathophysiology
During an electric shock or seizure, violent involuntary contraction of the internal rotators (subscapularis, pectoralis major, latissimus dorsi, trees major) overwhelms the external rotators and posterior capsule, forcing the humeral head posteriorly [3,8,10]. This results in dislocation, and in many cases, an impression fracture of the anteromedial humeral head-the reverse Hill–Sachs lesion-occurs when the humeral head impacts against the posterior glenoid rim [2,13]. In our patient, CT imaging confirmed ~30% articular surface involvement, consistent with a medium-sized reverse Hill–Sachs lesion.
Diagnostic Challenges
Posterior dislocations can be missed if only anteroposterior radiographs are obtained, as the humeral head may appear normally aligned. The axillary view is the most reliable, while scapular Y-view and CT scans aid in confirmation and in quantifying humeral head defects [2,6,7]. In our case, the patient was misdiagnosed initially, and diagnosis was only established three weeks later using both radiographs and CT.
Neglected Dislocations
Neglected or chronic posterior dislocations are defined as those unreduced for more than three weeks [4,11,12]. Chronicity results in fibrous tissue formation, capsular contracture, and irreversible bony changes, rendering closed reduction impossible. These cases pose significant treatment challenges, especially when associated with large reverse Hill–Sachs lesions [11,17,21].
Management Strategies
Figure 14 illustrates a comprehensive management algorithm for posterior shoulder dislocations, designed to assist surgeons in structured clinical decision-making. The pathway begins with confirmation of the diagnosis through standard radiographs, computed tomography, and magnetic resonance imaging to delineate associated bone and soft-tissue injuries. Once confirmed, dislocations are classified as acute (<3 weeks) or chronic (>3 weeks), as chronicity significantly affects treatment feasibility and outcomes. The next critical step is quantifying the reverse Hill– Sachs defect, as defect size remains the principal determinant of surgical strategy: Defects <25%: Closed or open reduction may suffice, occasionally with McLaughlin’s original tendon transfer [2,14]. Defects 25–40%: The modified McLaughlin procedure is recommended, involving transfer of the subscapularis tendon or the lesser tuberosity into the humeral head defect [6,19-21].
This technique provides stability and allows for biological healing. Defects >40%: Options include humeral head reconstruction with autograft or allograft [11,13,19], rotational osteotomy [10], or shoulder arthroplasty in irreparable cases, particularly in older or low-demand patients [18,22]. Our patient had a ~30% defect, making the modified McLaughlin procedure the most appropriate treatment option. We reinforced fixation with two cancellous screws and washers, ensuring stability. The algorithm concludes with a standardized postoperative rehabilitation protocol emphasizing staged mobilization-from sling immobilization and passive motion to progressive activeassisted and active exercises within 3–6 weeks-to restore stability, range of motion, and functional recovery.
Literature Review
McLaughlin [23] first described subscapularis tendon transfer into the defect, while Neer [15] later modified it by transferring the lesser tuberosity, which improved healing and fixation strength. Several studies have reported excellent outcomes with the modified McLaughlin procedure in neglected dislocations: Gerber & Lambert [11] reconstructed large segmental defects with allografts, reporting good long-term outcomes. Diklic et al. [24] treated 13 patients with chronic locked posterior dislocations using open reduction and tendon transfer, achieving satisfactory function. Martinez et al. [25] used Neer’s modification in four neglected cases, reporting stable reductions and pain relief. Kokkalis et al. [15,26] confirmed the efficacy of the modified McLaughlin for medium-sized defects, with good functional results.
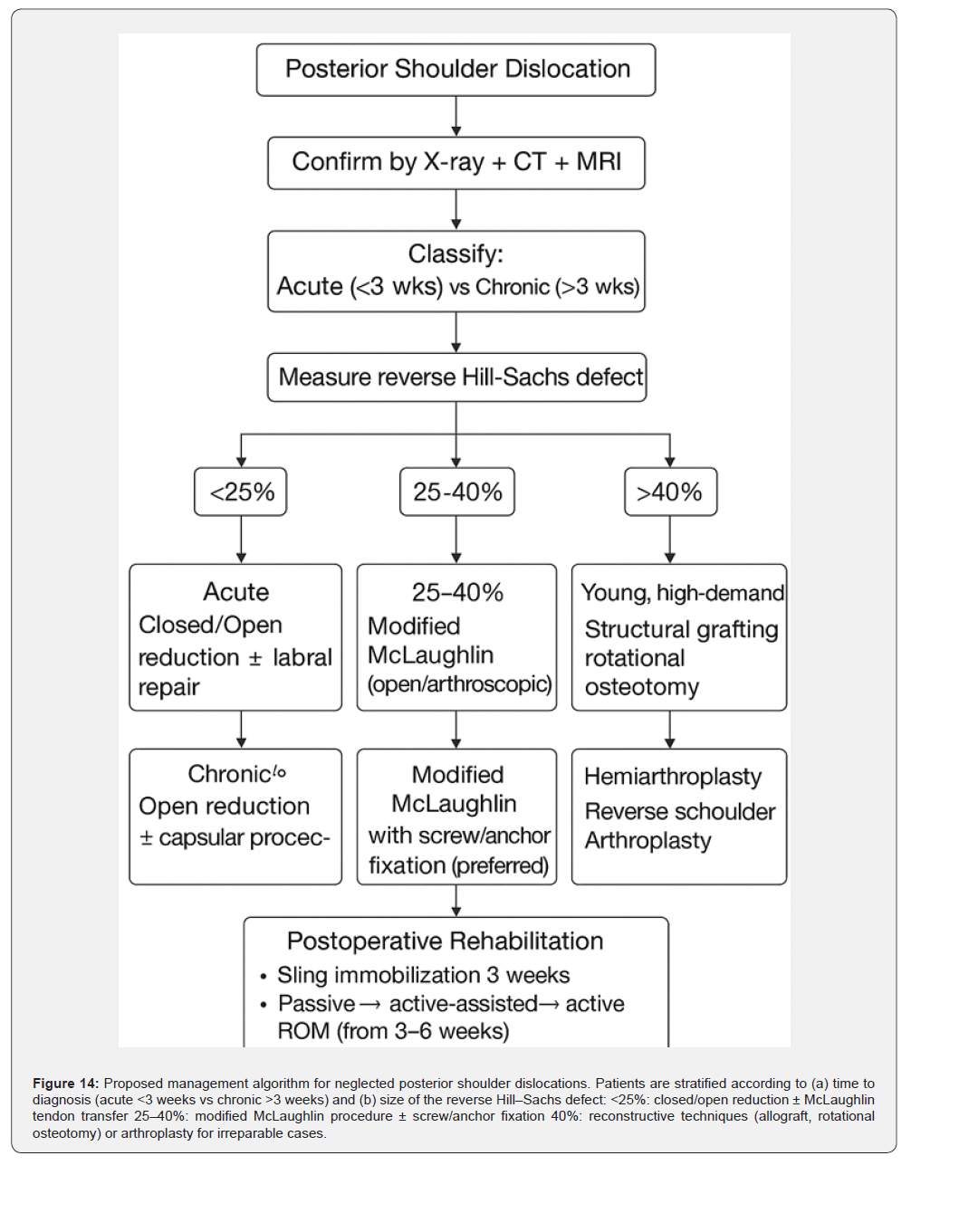
Katthagen et al. [22] emphasized the procedure’s value for locked dislocations with engaging lesions. Saltzman et al. [24], in a systematic review, found the modified McLaughlin procedure to be the most employed technique for moderate lesions, reserving arthroplasty for large defects. Conversely, when humeral head involvement exceeds 40–50%, outcomes with tendon transfer alone are suboptimal, and arthroplasty or reconstructive grafting is recommended [11,18,19]. A comprehensive overview of the major reported series is summarized in Table 1, which demonstrates how time to diagnosis, defect size, and surgical choice directly influence clinical outcome. To guide clinical decision-making, we propose a structured treatment pathway illustrated in Figure 14 (management algorithm), which stratifies patients by defect size and chronicity to optimize surgical selection.

Prognosis and Rehabilitation
Successful outcomes depend not only on the surgical technique but also on a carefully structured rehabilitation program. Immobilization should be followed by staged passive, active-assisted, and strengthening exercises [12,13]. Our patient followed this protocol and achieved functional range of motion by three months. Prognostic factors influencing outcome include defect size, time to diagnosis, fixation stability, and patient compliance with rehabilitation [9,11,21]. Early detection and appropriate management remain the most critical determinants of long-term results.
Relevance of the Present Case
The current case highlights several important points: Rare mechanism: posterior dislocation following electrical injury is uncommon but well-documented. Diagnostic pitfalls: the injury was neglected for three weeks due to initial misdiagnosis. Optimal surgical management: the modified McLaughlin procedure, reinforced with anchors and screws, provided stability for a medium-sized reverse Hill–Sachs lesion. Favorable short-term outcome: in three months, the patient achieved painless functional range of motion and radiographic stability.
Conclusion
Neglected posterior shoulder dislocations with associated reverse Hill–Sachs lesions remain a rare but challenging entity in orthopedic practice. Diagnosis is frequently delayed due to subtle radiographic findings and nonspecific symptoms, especially when the mechanism of injury involves seizures or electrical shock. Our case illustrates the importance of maintaining a high index of suspicion, utilizing advanced imaging such as CT for accurate assessment, and selecting an appropriate surgical strategy based on the size of the humeral head defect. The modified McLaughlin procedure remains a reliable and effective option for defects involving 25-40% of the humeral head, offering joint preservation and restoration of stability.
A structured algorithm (Figure 14) together with evidence from the literature (Table 1) may aid surgeons in selecting the optimal treatment strategy for neglected posterior shoulder dislocations. Early diagnosis, meticulous surgical technique, and structured rehabilitation are key determinants of successful outcomes. Surgeons must remain vigilant in cases of posterior shoulder pain following seizures, trauma, or electrical injury, as prompt recognition and intervention can prevent chronic instability, functional impairment, and the need for arthroplasty [27,28].
Declarations
Consent for publication
Oral informed consent was taken.
Availability of data and material
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Funding: There is no funding source.
Competing interests: The author declare that he has no competing interests.
Acknowledgement: Not applicable.
Conflict of Interest
The author declare that he has no conflict of interest.
References
- Abalo A, Dossim A, Songne B, et al. (2009) Neglected posterior dislocation of the shoulder: functional outcome after open reduction. Int Orthop 33(3): 525-529.
- Chetan S Modi, Laurence Wicks, Kuntrapaka Srinivasan (2009) Reconstruction of humeral head defects with osteochondral autograft for chronic locked posterior dislocation of the shoulder. J Shoulder Elbow Surg 18(4): 544-549.
- Checchia SL, Santos PD, Miyazaki AN (1998) Surgical treatment of chronic posterior dislocation of the shoulder. J Shoulder Elbow Surg 7(1): 53-57.
- Cicak N (2004) Posterior dislocation of the shoulder. J Bone Joint Surg Br 86(3): 324-332.
- Hawkins RJ, Neer CS, Pianta RM, Mendoza FX (1987) Locked posterior dislocation of the shoulder. J Bone Joint Surg Am 69(1): 9-18.
- Kowalsky MS, Levine WN (2008) Traumatic posterior glenohumeral dislocation: classification, pathoanatomy, diagnosis, and treatment. Orthop Clin North Am 39(4): 519-533.
- Sperling JW, Pring ME, Antuna SA, Cofield RH (2004) Shoulder arthroplasty for locked posterior dislocation of the shoulder. J Shoulder Elbow Surg 13(5): 522-527.
- Robinson CM, Seah M, Akhtar MA (2011) The epidemiology, risk of recurrence, and functional outcome after an acute traumatic posterior dislocation of the shoulder. J Bone Joint Surg Am 93(17): 1605-1613.
- Rowe CR, Zarins B (1982) Chronic unreduced dislocations of the shoulder. J Bone Joint Surg Am 64(4): 494-505.
- Shaw JL (1971) Bilateral posterior fracture-dislocation of the shoulder and other trauma caused by convulsive seizures. J Bone Joint Surg Am 53(7): 1437-1440.
- Gerber C, Lambert SM (1996) Allograft reconstruction of segmental defects of the humeral head for the treatment of chronic locked posterior dislocation of the shoulder. J Bone Joint Surg Am 78(3): 376-382.
- Gerber C, Pennington SD, Nyffeler RW (2004) Reverse Hill–Sachs lesion: an operative technique. J Shoulder Elbow Surg 13(5): 605-610.
- Kokkalis ZT, Iliopoulos ID, Antoniou G, Antoniadou T, Mavrogenis AF, et al. (2017) Posterior shoulder fracture-dislocation: an update with treatment algorithm. Eur J Orthop Surg Traumatol 27(3): 285-294.
- Connell DA, Potter HG, Sherman MF, Wickiewicz TL (1994) Injuries of the shoulder posterior stabilizers in athletes. Am J Sports Med 22(2): 261-267.
- Neer CS (1970) Displaced proximal humeral fractures. I. Classification and evaluation. J Bone Joint Surg Am 52(6):1077-1089.
- Raiss P, Edwards TB, Bruckner T, Loew M, Zeifang F, et al. (2012) Reverse shoulder arthroplasty for the treatment of locked posterior dislocation of the shoulder. J Bone Joint Surg Br 94(6): 813-818.
- Robinson CM, Aderinto J (2005) Posterior shoulder dislocations and fracture-dislocations. J Bone Joint Surg Am 87(3): 639-650.
- ML Despeyroux, O Loustau, J J Railhac, N Sans (2008) Imaging of traumatic shoulder injuries. Semin Musculoskelet Radiol 12(2): 149-167.
- Fei Xiong, Qin Yin, Jian Wang, Changbao Wei, Sanjun Gu, et al. (2023) A novel modified McLaughlin surgery for treating locked chronic posterior shoulder dislocation. BMC Musculoskelet Disord 24(1): 114.
- Saltzman BM, Riboh JC, Cole BJ, Romeo AA (2015) Management and outcomes of posterior shoulder instability: a systematic review. J Bone Joint Surg Am 97(6): 470-478.
- Gerber C, Pennington SD, Nyffeler RW (2009) Reverse shoulder arthroplasty. J Am Acad Orthop Surg 17(5): 284-295.
- Katthagen JC, Tahal DS, Millett PJ (2016) Arthroscopic management of locked posterior shoulder dislocations and reverse Hill–Sachs lesions: a case series. Arthroscopy 32(9): 1811-1817.
- McLaughlin HL (1952) Posterior dislocation of the shoulder. J Bone Joint Surg Am 24(3): 584-590.
- Diklic ID, Ganic ZD, Blagojevic ZD, et al. (2010) Treatment of locked chronic posterior dislocation of the shoulder by reconstruction of the defect in the humeral head with an allograft. J Bone Joint Surg Br 92(1): 71-76.
- Martinez AA, Calvo A, Domingo J, Cuenca J, Herrera A (2008) Long-term results of Neer modification for neglected posterior dislocation of the shoulder. J Orthop Trauma 22(9): 603-610.
- Kokkalis ZT, Ballas EG, Mavrogenis AF, Papagelopoulos PJ (2013) Modified McLaughlin technique for neglected locked posterior dislocation of the shoulder. Orthopedics 36(1): e912-916.
- McLaughlin HL, MacLellan DI (1967) Recurrent posterior dislocation of the shoulder. J Trauma 7(2): 191-198.
- Keppler P, Holz U, Thielemann FW, Meinig R (1994) Locked posterior dislocation of the shoulder: treatment using rotational osteotomy of the humerus. J Orthop Trauma 8(4): 286-292.






























