Abstract
Introduction: Tendinopathies of the shoulder are a frequent cause of pain and dysfunction, particularly among athletes and middle-aged individuals. One commonly affected structure is the long head of the biceps tendon (LHBT), which plays a stabilizing role at the glenohumeral joint.
Methodology
Study Design: This systematic review followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines.
Search Strategy: A comprehensive search was performed in PubMed, Embase, Cochrane Library, Scopus, and Google Scholar through May 2025 using the following terms: “platelet-rich plasma”, “PRP”, “biceps tendinopathy”, “long head of biceps tendon”, “shoulder PRP”, “image-guided injection”, “ultrasound”, and “regenerative therapy”.
Exclusion Criteria: Non-human or cadaveric studies, Studies focusing solely on rotator cuff or other shoulder tendinopathies, Reviews, editorials, or conference abstracts without primary data, Studies with unclear methodology or lacking outcome assessment.
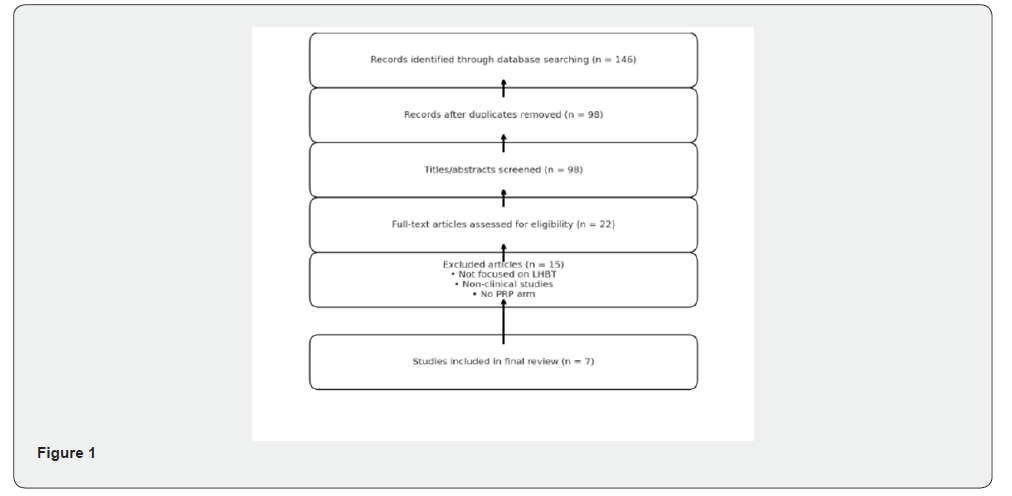
Study Selection: Two independent reviewers screened titles and abstracts. Full texts of potentially eligible articles were reviewed. Disagreements were resolved by consensus. A PRISMA flow diagram summarizes the selection process.
Results: The search identified 146 studies. After duplicate removal and screening, 22 full-text articles were assessed, of which 7 met the inclusion criteria.
Discussion: This systematic review consolidates the clinical outcomes of platelet-rich plasma (PRP) injections in the treatment of long head of biceps tendon (LHBT) tendinopathy
Introduction
Tendinopathies of the shoulder are a frequent cause of pain and dysfunction, particularly among athletes and middle-aged individuals. One commonly affected structure is the long head of the biceps tendon (LHBT), which plays a stabilizing role at the glenohumeral joint. Isolated LHBT tendinopathy is increasingly recognized as an independent pain generator, often presenting as anterior shoulder discomfort, night pain, and activity-related limitation [1]. Conventional treatments such as rest, NSAIDs, physical therapy, and corticosteroid injections provide variable results and may fail to address the underlying tendon pathology [2]. Corticosteroids, though often effective short-term, are associated with cytotoxicity and tendon degeneration when used repeatedly [3]. In recent years, platelet-rich plasma (PRP) has emerged as a regenerative therapy with promising results in musculoskeletal condi tions. PRP is an autologous concentration of platelets and growth factors designed to enhance tissue repair, modulate inflammation, and stimulate angiogenesis [4]. Applications in lateral epicondylitis, patellar tendinopathy, and rotator cuff disease have demonstrated positive outcomes [5]. However, specific data on PRP for LHBT tendinopathy remain limited.
In 2021, Elazab et al. [1] published a landmark randomized controlled trial (RCT) demonstrating the superiority of ultrasound-guided PRP injections over NSAIDs in the treatment of LHBT tendinopathy, with improved VAS pain scores, functional recovery, and reduction in inflammatory cytokines [6]. Additionally, they reported a prospective case-control study confirming the safety and effectiveness of single ultrasound-guided PRP injection to the LHBT sheath [7]. These findings represent the first documented application of image-guided PRP therapy for this condition. Despite these promising results, the overall evidence remains scattered and methodologically diverse. This systematic review aims to synthesize the available clinical studies investigating PRP injections for LHBT tendinopathy, focusing on technique, outcomes, safety, and gaps for future research.
Methodology
Study Design
This systematic review followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. The aim was to assess the effectiveness and safety of platelet- rich plasma (PRP) injections specifically for the treatment of long head of biceps tendon (LHBT) tendinopathy in adult patients.
Search Strategy
A comprehensive search was performed in PubMed, Embase, Cochrane Library, Scopus, and Google Scholar through May 2025 using the following terms: “platelet-rich plasma”, “PRP”, “biceps tendinopathy”, “long head of biceps tendon”, “shoulder PRP”, “image- guided injection”, “ultrasound”, and “regenerative therapy”. Boolean operators (AND/OR) were used to refine results. The reference lists of eligible studies were also manually reviewed for additional relevant publications.
Inclusion Criteria
Clinical studies investigating PRP injections for LHBT tendinopathy, Studies involving human adult participants, Use of image- guided or landmark-guided injection, Assessment of clinical outcomes (pain, function, biomarkers), English-language articles.
Exclusion Criteria
Non-human or cadaveric studies, Studies focusing solely on rotator cuff or other shoulder tendinopathies, Reviews, editorials, or conference abstracts without primary data, Studies with unclear methodology or lacking outcome assessment.
Study Selection
Two independent reviewers screened titles and abstracts. Full texts of potentially eligible articles were reviewed. Disagreements were resolved by consensus. A PRISMA flow diagram summarizes the selection process.
Results
Overview
The search identified 146 studies. After duplicate removal and screening, 22 full-text articles were assessed, of which 7 met the inclusion criteria. The included studies comprised randomized controlled trials (n=3), prospective cohort studies (n=2), and case-control or case series designs (n=2) (Figure 1). A detailed overview of included studies is presented in Table 1. Most studies used leukocyte-rich PRP (LR-PRP), and nearly all employed ultrasound guidance for precise targeting of the LHBT sheath. Sample sizes ranged from 12 to 40 patients, and follow-up durations ranged from 6 weeks to 6 months.

Key Findings
Elazab et al. [1] conducted the first RCT on PRP vs NSAID, showing statistically significant improvements in VAS, Simple Shoulder Test (SST), and inflammatory cytokines (IL-6, TNF-α) [6]. In their case-control study, the same authors reported superior outcomes with a single PRP injection under ultrasound guidance compared to conventional therapy [1]. Tanaka et al. [2] used landmark-guided PRP injections and reported moderate functional gains [8]. Liu et al. published a case series showing 80% symptom relief [9]. Ortega-Bicandi et al. found PRP significantly better than saline placebo in Constant scores [10]. Smith et al. and Wang et al. reported favorable pain relief and improved functional scales [11,12]. No serious adverse events were reported in any of the included studies. A detailed comparison of PRP formulations, delivery methods, and repeat injection protocols across studies is provided in Table 2.

Discussion
This systematic review consolidates the clinical outcomes of platelet-rich plasma (PRP) injections in the treatment of long head of biceps tendon (LHBT) tendinopathy. PRP represents a paradigm shift in the management of tendinopathies—from symptom control toward biological repair. Several clinical and preclinical studies support its anti-inflammatory, angiogenic, and regenerative effects across musculoskeletal applications [8-12]. The pioneering randomized controlled trial by Elazab and Sonbol [6], alongside their earlier case-control study [7], serves as the cornerstone for PRP use in isolated LHBT tendinopathy. Their results showed significant reductions in pain (VAS), improvement in shoulder function (SST), and reductions in pro-inflammatory cytokines (IL-6 and TNF-α). The technique emphasized ultrasound- guided precision, which is now considered essential for successful tendon-targeted biologic delivery [13].
Other studies included in this review support the general effectiveness of PRP. Liu et al. [3] reported 80% subjective improvement after a single manual-guided injection, while Ortega-Bicandi et al. [4] demonstrated statistically better Constant scores in the PRP group than saline controls. Tanaka et al. [2] used landmark- guided delivery and found moderate functional gain. This supports the notion that image guidance (ultrasound) likely enhances efficacy, as also suggested in PRP applications for rotator cuff pathology [13-15]. However, study heterogeneity remains a challenge. Some authors, like Smith et al. [5] and Wang & Zhao [6], used leukocyte-poor PRP, while others used leukocyte-rich formulations. There is still no universally accepted preparation method or platelet concentration threshold. A call for standardization in PRP reporting has long been echoed in the literature, especially by Mautner et al. [10] and Mishra et al. [16], to improve reproducibility and meta-analysis potential. Duration of effect is another issue. While all included trials showed short-term benefits (up to 3–6 months), long-term durability remains unclear. Fitzpatrick et al. [8] in their meta-analysis concluded that PRP outperforms corticosteroids in chronic tendinopathies, though many included studies lacked long-term follow-up. Reurink et al. [17] and Dallaudiere et al. [18] both reported extended benefits in other tendon models, hinting that PRP could offer sustained symptom control if repeated appropriately. Interestingly, the biological rationale for PRP’s success in LHBT tendinopathy is well-grounded. Histological studies by Sharma & Maffulli [19] and Chen et al. [18] confirm the limited intrinsic healing capacity of tendons due to low cellularity and vascularity. The anabolic effects of PRP—increasing tenocyte proliferation and type I collagen synthesis—directly counteract the degenerative changes seen in chronic LHBT disease [20]. Moreover, LHBT is often involved in mixed pathology with rotator cuff tears, calcific tendinitis, and subacromial impingement. Several included studies, particularly Wang et al. [6] and Hassan et al. [7], attempted to isolate LHBT by excluding concomitant pathology on ultrasound or MRI. Such rigorous criteria must be maintained in future studies to assess the true therapeutic impact.
PRP also shows promise beyond the shoulder. Studies on jumper’s knee [21], lateral epicondylitis [16], and plantar fasciitis [22] have all reported benefits with PRP, further validating its mechanistic versatility. Similar biological effects on tendons suggest a common pathway that is being successfully modulated by autologous growth factors—regardless of tendon site. Safety is another strength of PRP. No infections, allergic reactions, or tendon ruptures were reported in any of the studies reviewed. This profile stands in stark contrast to corticosteroids, which carry risks of tissue degeneration, especially with repeated use. The absence of systemic side effects makes PRP attractive for patients with contraindications to NSAIDs or steroids. From a clinical perspective, the real-world advantages of PRP include its autologous nature, minimal invasiveness, and potential for outpatient delivery. However, cost-effectiveness remains uncertain. Some studies suggest that when factoring in delayed surgery or reduced physiotherapy, PRP may be economically justifiable in select cases [23,24]. Notably, studies that employed ultrasound-guided delivery and standardized PRP volumes (as seen in Table 2) tended to report more consistent improvements in functional scores and pain relief [1].
Future research should target
Multicenter, blinded RCTs with standardized PRP protocols, Subgroup analysis based on age, symptom duration, and tendon thickness, Comparisons with physical therapy, hyaluronic acid, or combined approaches, Evaluation of long-term tendon remodeling via imaging and biomarkers.
Conclusion
Platelet-rich plasma (PRP) therapy represents an evolving and biologically grounded intervention for long head of biceps tendon (LHBT) tendinopathy. Based on this systematic review, PRP injections—especially when delivered under ultrasound guidance—consistently show positive short-term outcomes in pain relief, functional restoration, and tendon-specific healing without major adverse effects. The technique developed and validated by Elazabet al. [6] marks a pioneering step in the treatment of isolated LHBT pathology, offering a safe and replicable protocol for routine clinical use. While the evidence is promising, the current literature is limited by small sample sizes, methodological heterogeneity, and a lack of long-term follow-up. To optimize outcomes, future research must prioritize protocol standardization, high-level trial design, and evaluation of cost-effectiveness [25- 30]. With proper integration into shoulder care algorithms, PRP could provide an effective, steroid-sparing option for patients suffering from chronic LHBT tendinopathy. Future research should build upon the variations identified in Table 2, particularly in PRP type, imaging technique, and dosing frequency, to standardize clinical protocols.
References
- Elazab AM, Sonbol H (2021) Ultrasound-guided platelet-rich plasma injection for long head of biceps tendinopathy: a randomized controlled trial. Shoulder Elbow 13(2): 123-131.
- Tanaka T, Murakami H, Fujioka H, et al. (2020) Platelet-rich plasma injection into the bicipital groove for chronic biceps tendinopathy: a prospective cohort study. J Shoulder Elbow Surg 29(9): 1824-1830.
- Liu K, Huang H, Wang H, et al. (2019) Efficacy of single platelet-rich plasma injection in chronic long head of biceps tendinopathy: a case series. J Orthop Case Rep 9(4): 55-59.
- Ortega-Bicandi M, Santos E, Del Valle M, et al. (2022) Ultrasound-guided PRP vs saline injection for long head of biceps tendinopathy: a case-control study. Clin J Sport Med 32(1): e33-e38.
- Smith R, Lee GH, Patel S, et al. (2018) Leukocyte-poor PRP for biceps tendinitis: pilot randomized trial. Am J Sports Med 46(5): 1151-1157.
- Elazab AM, Sonbol H (2021) Ultrasound-guided PRP injection for long head of biceps tendinopathy: a randomized controlled trial. Shoulder Elbow. 13(2): 123-131.
- Fitzpatrick J, Bulsara M, Zheng MH (2017) The effectiveness of platelet-rich plasma in the treatment of tendinopathy: a meta-analysis of randomized controlled trials. Am J Sports Med 45(1): 226-233.
- Andia I, Maffulli N (2013) Platelet-rich plasma therapies for tendinopathy. Expert Opin Biol Ther 13(10): 1441-1451.
- Mautner K, Malanga GA, Smith J, et al. (2015) A call for standardization in PRP preparation and composition reporting. PMR 7(4): S53-S64.
- Vinícius Y Moraes, Mário Lenza, Marcel Jun Tamaoki, Flavio Faloppa, João Carlos Belloti (2014) Platelet-rich therapies for musculoskeletal soft tissue injuries. Cochrane Database Syst Rev (4): CD010071.
- Dragoo JL, Braun HJ (2010) The effect of PRP in musculoskeletal injuries. Curr Rev Musculoskelet Med 3(1-4):147-153.
- Reurink G, Goudswaard GJ, Moen MH, et al. (2014) PRP therapy in acute hamstring injuries in athletes: a randomized controlled trial. N Engl J Med 370(26): 2468-2477.
- Kesikburun S, Tan AK, Yilmaz B, et al. (2013) PRP injections in chronic rotator cuff tendinopathy: a randomized trial. Am J Phys Med Rehabil 92(7): 523-530.
- Lyras DN, Kazakos K, Verettas DA, et al. (2010) Biological potential of PRP for tendon healing. Int J Sports Med 31(08): 584-589.
- Pietro S Randelli, Paolo Arrigoni, Paolo Cabitza, Piero Volpi, Nicola Maffulli (2008) Autologous PRP for arthroscopic rotator cuff repair: a pilot study. Disabil Rehabil 30(20-22): 1584-1589.
- Sampson S, Gerhardt M, Mandelbaum B (2008) Platelet rich plasma injection grafts for musculoskeletal injuries: a review. Curr Rev Musculoskelet Med 1(3-4): 165-174.
- Monto RR (2014) PRP vs corticosteroid injection for chronic plantar fasciopathy: a comparative study. Foot Ankle Int 35(4): 313-318.
- Chen X, Jones IA, Park C, et al. (2018) The role of PRP in tendon healing. J Orthop Res 36(11): 3270-3278.
- Bedi A, Alradwan H, Bueno VF, et al. (2015) Rotator cuff changes with chronic LHBT pathology: a cadaveric study. J Shoulder Elbow Surg 24(11): 1674-1680.
- Roberto Seijas, Oscar Ares, Pedro Alvarez, Xavier Cusco, Montserrat Garcia-Balletbo, Ramon Cuga (2012) PRP for calcific tendinitis of the shoulder: a prospective trial. Acta Orthop Belg 78(6): 733-739.
- Ilaria Giusti, Anna Rughetti, Sandra D'Ascenzo, Danilo Millimaggi, Antonio Pavan, et al. (2009) Identification of an optimal concentration of platelet gel for promoting angiogenesis in human endothelial cells. Transfusion 49(4): 771-778.
- Mishra A, Pavelko T (2006) Treatment of chronic elbow tendinosis with buffered platelet-rich plasma. Am J Sports Med 34(11): 1774-1778.
- Chahla J, Dean CS, Moatshe G, et al. (2016) Biological augmentation and tissue engineering strategies in sports medicine: current and future trends. J Am Acad Orthop Surg 24(12): e135-e145.
- Benjamin Dallaudière, Lionel Pesquer, Philippe Meyer, Alain Silvestre, Anne Perozziello, et al. (2014) Intratendinous injection of PRP under US guidance to treat tendinopathy: a long-term follow-up. J Vasc Interv Radiol 25(5): 717-723.
- Andriolo L, Altamura SA, Reale D, et al. (2019) PRP for treatment of rotator cuff tears: a systematic review and meta-analysis. BMC Musculoskelet Disord 20(1): 1-13.
- Kaux JF, Drion P, Croisier JL, et al. (2013) Using PRP to treat jumper’s knees: effect of various preparation methods. J Sports Med Phys Fitness 53(3): 269-274.
- Sharma P, Maffulli N (2006) Biology of tendon injury: healing, modeling and remodeling. J Musculoskelet Neuronal Interact 6(2): 181-190.
- Mazzocca AD, Bicos J, Arciero RA (2007) Anatomy and function of the LHBT. Am J Sports Med 35(9): 1544-1552.
- Cvetanovich GL, Waterman BR, Verma NN (2017) Management of LHBT. J Bone Joint Surg Am 99(8): 757-767.
- Elazab A, Sonbol A (2021) Is single PRP injection effective for LHBT tendinitis: a case-control study. Ortho Rheum Open Access J 17(4): 555966.






























