Abstract
Introduction: The global market for knee replacement implants was valued at USD 10.61 billion in 2023 and is projected to reach USD 16.41 billion by 2032. In India, the knee implant market generated USD 264.0 million in 2024 and is expected to reach USD 381.9 million by 2030. India is a significant market for knee replacement surgeries due to factors like a growing aging population and increasing awareness about the benefits of these procedures. It’s estimated that by 2030, over 3 million knee replacements will be performed annually. The most common causes of chronic pain and disability in the knee leading to total knee (TKR) replacement surgery are i) Osteoarthritis, ii) Rheumatoid arthritis and iii) post-traumatic arthritis. A total knee replacement is a surgical procedure that replaces the worn-out or damaged joint of the knee with a prosthesis made of metal, or plastic. The parts of a knee joint that can be replaced include the femur, tibia and patella. TKRS is recommended when treatments with anti-inflammatory medications, lubricating or cortisone injections, and physical therapy have failed to offer relief from pain and stiffness in patients who find performing everyday activities like walking, bending, sitting, or standing an ordeal due to severe knee pain and stiffness. When knee pain continues even while resting or sleeping or when knee swelling does not subside with rest and medicines, or patients with bowed-knee deformity are advised Knee replacement. While 15-20 million individuals with Osteoarthritis, Rheumatoid arthritis and post-traumatic arthritis may benefit with TKR surgery only a fraction (about 10%) can afford it in 2025.
Material & Methods: This article has been prompted by the author’s management of 2 Total Knee replacements for osteoarthritis in the last 3 months and one Rheumatoid arthritis case and another post-traumatic arthritis case over the last 2 years, supported by literature search
Outcomes: All four cases (2 bilateral & 2 unilateral) are leading a comfortable daily life after Total Knee replacement.
Keywords:Disease-modifying antirheumatic drugs; Nonsteroidal anti-inflammatory drugs; Minimally Invasive; Traditional TKR; Rheumatoid arthritis
Abbreviations:OA: Osteoarthritis; RA: Rheumatoid arthritis; PTA: Post Traumatic Arthritis; TKR: Total Knee Replacement; DMARDs: Disease-modifying antirheumatic drugs; NSAIDs: Nonsteroidal anti-inflammatory drugs; TKAP: Total knee arthroplasty Procedure; MITKR: Minimally Invasive TKR; TTKR: Traditional TKR
Introduction
The knee is the largest joint in the body and having healthy knees is required to perform most everyday activities. The knee is made up of- i) The lower end of the femur ii) The upper end of the tibia and the patella known as kneecap. The ends of these three bones are covered with articular cartilage, a smooth substance that protects the bones and enables them to move easily within the joint. The C-shaped wedges called menisci are located between the femur and tibia & act as shock absorbers that cushion the joint. Large ligaments hold the femur and tibia together and provide stability. The long-thigh muscles give the knee strength. If the knee is severely damaged by arthritis or injury, it will be hard for everyone to perform simple activities, like walking or climbing stairs etc. The individual begins to feel pain while sitting or lying down. If nonsurgical treatments like medications and using walking support are not helpful, doctors advise total knee replacement surgery, which is a safe and effective procedure to relieve pain, correct leg deformity, and help you resume normal activities. The most common cause of chronic pain and disability in the knee that leads to total knee replacement surgery include i) Osteoarthritis, a type of arthritis seen in people over 50 years of age, due to the wear and tear of the bones over the years as a person ages, and the cartilage that protects the knee bones wears away causing the bones to rub against one another leading to pain and stiffness of the knee. ii) Rheumatoid arthritis is a condition in which the synovial membrane around the knee joint becomes inflamed & damages the cartilage which cushions and protects the knee joint iii) post-traumatic arthritis- any injury to cartilage or bone of joint leads to premature arthritis. A total knee replacement is a surgical procedure that replaces the worn-out or damaged joint of the knee with a prosthesis made of metal, or plastic. The parts of a knee joint that can be replaced include the femur, tibia and patella (Figure 1).
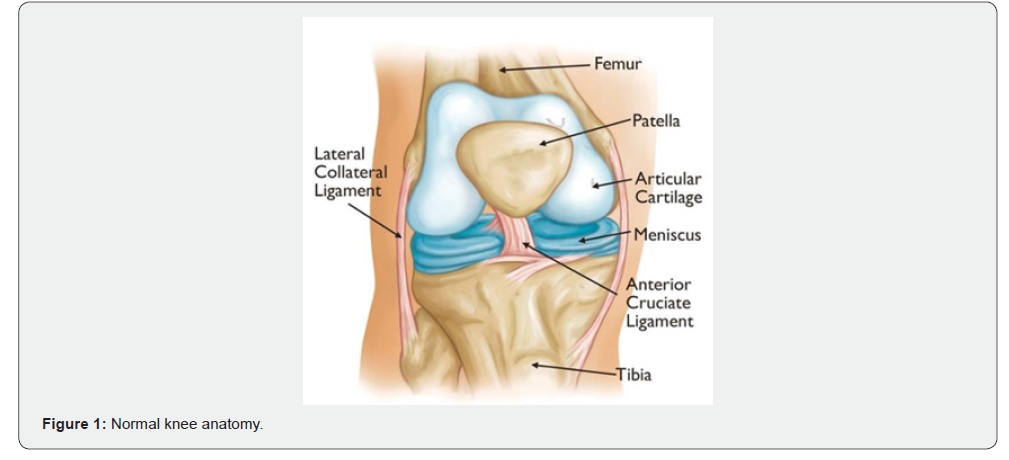
This article is prompted by the author’s management of 2 Total Knee replacements in the last 3 months and another 2 over the last 2 years, supported by literature search.
Case Report
Case 1
Sridhar a Case of Bilateral Osteoarthritis: Sridhar 71 years old male patent, sales executive by profession complained of Bilateral knee pain, for nearly a decade which became more severe in Left knee for 6 months disabling him from routine walking. The pain had an insidious onset, gradually progressing, sharp pain for 6 months which used to aggravate after walking for long distances initially but just 100 meters since a month. He was taking Ibuprofen 400 mg twice or thrice a day whenever pain was severe for 3-5 days. In view of of the severity of pain & analgesics not relieving much, an orthopedic consultation was taken on 30 January 2025. He is a known Hypertensive for a decade and CKD stage 3 patient since 2024. Orthopedical physical examination recorded.
Right Knee: Varus deformity, Quadriceps wasting = FFD+ 10° Tenderness +, Crepitus +, No DNVD, ROM=10-110 deg,
Left Knee: Varus deformity, Quadriceps wasting = FFD+ 10o Tenderness +, Crepitus +, No DNVD, ROM=10-110 deg. Xray of both knees confirmed Osteoarthritis. In consultation with his family a bilateral TKR decided. After a thorough check up and clearance for surgery by Cardiologist and Nephrologist on 1 February 2025, his right knee was operated on 3 February, and the left knee was operated on 6 February 2025 and discharged on 8 February 2025 after training for the exercises. He was made to stand & walk with walker support the very next day after each knee surgery and by the end of a week after the second surgery he started walking without a walker. After 15 days he could climb up and come down 15 steps with the support of the ramp. From the first week of March 2025, he walks without any support & discomfort.
Surgical Procedure
Total Knee Replacement (TKR) under Spinal Anesthesia & Adductor Canal Block: Patient was put in supine position under Spinal Anesthesia, after exposing the knee and draping, a midline incision was made. Skin and subcutaneous tissue were dissected. Medial parapatellar approach used, ACL Meniscus excised. Femoral and Tibia cuts are made using Jig. Flexion and Extension gap assessed and found to be adequate. Trial implants F-2(CR), T-2.5 and insert2.5x8 mm placed and reduction done. The cementing was done. Final implants of Depuy F-2, T 2.5and Inserted 2.5 x8 mm placed and reduced, wash given and wound closed in layers. On the 6th, a similar procedure was done for the left leg. Patent was put on IV fluids and antibiotics and oral analgesics each time. Post operative dressing was done a week after. The wound was clean with no post operative adverse events (Figure 2).
Case 2
TKR for Rheumatoid Arthritis: A lady aged 49 years old, with severe RA for the last 10 years. had had several steroid injections into the Left knee and an arthroscopic debridement of the joint which failed to give her any relief. She had a painfully stiff knee joint which was stuck in 30 degrees of flexion with further movement till just 80 degrees. After basic investigations she was taken for TKR. Following her total knee replacement, she regained full and pain free movement of the joint. She is comfortable doing all her day-to-day activities. Her medications for rheumatoid arthritis will continue to prevent damage to other joints.

Case 3
Total bilateral Knee Replacement of a Lady: Ms. Sandhya aged 72 years was suffering from a Trivial twist in Left knee and 2 weeks of MCL tenderness in December 2023. Her legs had bowed, and muscle wasted was of grade 2. due to The X Ray had shown Gross Osteoarthritis and was advised to undergo Total Knee Replacement. She somehow postponed and was forced to go through TKR, almost simultaneously as Shridhar but by different surgeons in different facilities. The interventions were like the first case. Her recovery was a bit delayed, and she needed physiotherapists assistance for about 2 months (Figure 3).
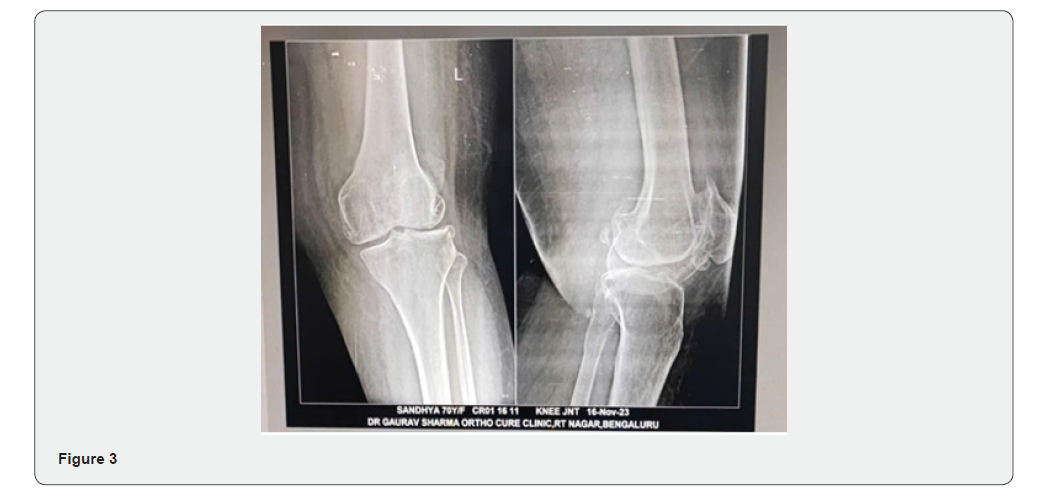
Case 4
TKR for Injured Knee with malunited fracture lower end of femur: A young, healthy 30-year-old male with no co-morbidities met with a two-wheeler accident, fell hitting his right knee on the road in August 2023, resulting in an open distal femur fracture without accompanying neurovascular injuries. He was treated for that injury with irrigation and debridement of the wound with a spanning external fixator of the left knee, kept for three months and wide broad antibiotics until wound healing. After six months the fixator was removed & physiotherapy started with a knee range of motion. However, a nonunion of the medial femoral condyle had happened and he started complaining of severe knee pain with stiffness and lack of full range of motion. The patient complained of severe mechanical pain with knee stiffness after the failure of knee manipulations under anesthesia, and that is when TKR was decided. On the initial examination, mild muscle wasting in the left femur was noticed, and a 3 X 2 cm scar on the medial aspect of the distal femur just proximal to the joint line. No joint effusion was seen. A CAT scan revealed an old non-united fracture of the medial femoral condyle. His MRI showed intact collateral ligaments and extensor mechanism. On 25-2-2024, under spinal anesthesia, an anterior para-patellar approach was made on the left knee, a tourniquet was applied to the proximal thigh but not inflated, and surgical dissection and excision of the severely fibrotic retro-patellar fat pad were done.
The patella was flipped, and excision of the medial, lateral meniscuses & the fibrotic ligaments in the middle compartment were done. An intramedullary guide was used to make the proximal cut of the tibia with a standard measurement of 10 mm of the highest point of the lateral tibial plateau and a posterior slope of 3 degrees. Then femoral exposure was done as a big chunk of the femoral condyle was barely attached to the femur, and as the bone quality of the separate chunk was of no good to be salvaged, it was excised. The chamfer cut was made after sizing the femoral component on the AP diameter. Three degrees of external rotation were made based on the epicondylar axis, ensuring it was parallel to the proximal tibial cut. The box cut was created as the prosthesis was cruciate sacrificing, and the distal femur was prepared for the stem by prober reaming. For the bone loss, the surgeon used three 4.5 mm cancellous screws on the medial aspect of the distal femur to buttress the cement used for bone loss filling. The patellofemoral track was fine, so a negative pressure drain was put in the lateral gutter, and closure on layers was done. The knee range of motion exercises started the next day after surgery with a proper pain control regime. Within two weeks’ patients’ rehabilitation started & wound healed in six weeks, enabling him to walk without pain.
Discussion
A total knee replacement is recommended for patients with severely damaged knee joints due to osteoarthritis, rheumatoid arthritis, post-traumatic arthritis, or injury. Arthritis stiffens the joint, making it painful & harder to walk even for shorter distances. The joint replacement of the knee is considered when medications, exercises, or other therapies failed to relieve pain [4].
Rheumatoid arthritis (RA)
Rheumatoid arthritis is a chronic autoimmune inflammatory disease affecting the joints resulting in pain and stiffness. It affects females more commonly, usually starting in their 30’s. There are reportedly 10 lakh cases diagnosed in India every year and many remain undiagnosed. can be hard to diagnose in its early stages. That’s because the early symptoms can be like those of other common conditions [1]. RA can lead to significant joint damage, often necessitating knee replacement. From 1990 to 2021 in India, the incidence, prevalence, and DALY rates of RA showed an increasing trend, with all age-standardized rates being significantly higher in females than in males. The number of males affected by RA across all age groups increased from 224,505 in 1990 to 704,401 in 2021, while the number of females increased from 594,068 to 2,062,348. In 2024 an estimated 2.5 million TKR surgeries were done in India. The age group of 65–69 years showed the highest incidence rate, while the prevalence peaked at 75–79 years. The forecast results indicate that the age-standardized incidence and DALY rates of RA in India will show an upward trend from 2022 to 2036 [2] (Figure 4).
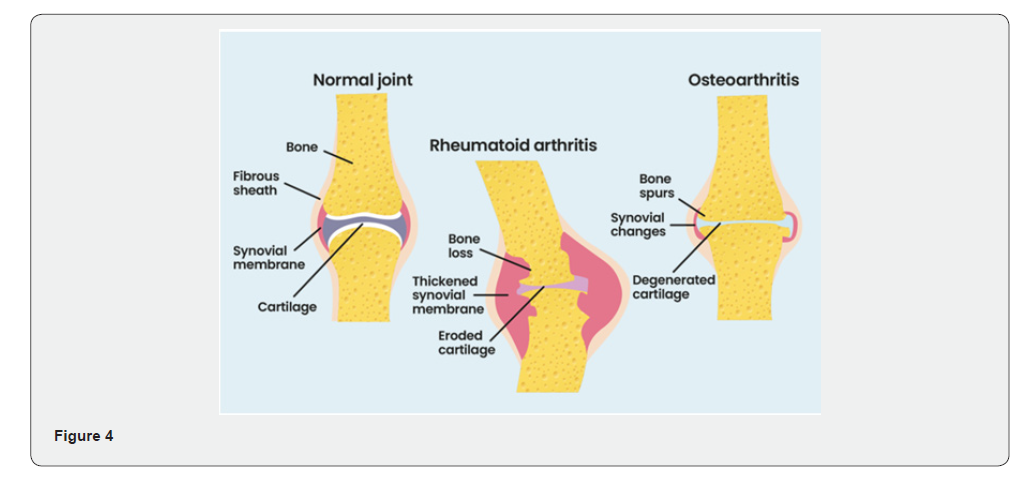
Physical Examination
During the physical exam, the Primary health Care doctor or Orthopedic checks the joints for swelling, redness and warmth, reflexes and muscle strength. Muscle strength general grading system: a) Grade 0: Minimal or no muscle loss. Muscles appear normal b) Grade 1: Mild muscle loss. Muscle appears slightly smaller but still functional c) Grade 2: Moderate muscle loss. Muscles are noticeably smaller, and strength may be reduced d) Grade 3: Severe muscle loss. Muscles are significantly smaller, and strength is markedly diminished. E) Grade 4: Extreme muscle loss. Muscles are severely atrophied, & strength is severely impaired. Basic investigations include -Blood tests, X Rays, MRIs, and Ultrasound or CT scans. Blood Tests are asked for erythrocyte sedimentation rate (ESR), C-reactive protein (CRP) level a higher level which indicate inflammation in the body. Rheumatoid factor and anti-cyclic citrullinated peptide (anti-CCP) antibodies are other tests done. Imaging tests like X-rays are done to track rheumatoid arthritis in the joints over time. MRI scans and ultrasound tests are done for initial diagnosis and how bad the condition is.
Management
There is no cure for rheumatoid arthritis. Joint damage can happen quickly without treatment, but remission, can be given with early treatment with medicines called disease-modifying antirheumatic drugs (DMARDs) [1].
Osteoarthritis (OA)
Osteoarthritis is a degenerative joint disease-causing cartilage breakdown, leading to pain, stiffness, and reduced mobility. There’s no blood test for osteoarthritis, certain tests like joint fluid analysis, help to infer if pain is caused by an inflammatory arthritis, such as rheumatoid arthritis or gout, or an infection rather than osteoarthritis or rule out other causes such as rheumatoid arthritis [3,4]. OA prevalence in India ranges from 22% to 39% among those aged 40 and above (41% 1464 million =600 million) amounting to 132-240 million people, with a higher prevalence among women and increases with age. Assuming 1 quarter of them 40-60 million cases may need Knee replacement. Osteoarthritis Management focuses on symptom relief and improving function, often through a combination of lifestyle changes, exercise, medication, and assistive devices. Pain Relievers like Acetaminophen (Tylenol) help with mild to moderate pain. Nonsteroidal anti-inflammatory drugs (NSAID like ibuprofen or naproxen) reduce both pain and inflammation. In some cases, corticosteroids are injected directly into the joint for short-term pain relief. While 15-20 million individuals with Osteoarthritis may benefit with TKR in India, only a fraction can afford it [3,4]. Recent knee OA studies report a lack of efficacy of Methotrexate and the potential adverse events, it is not recommended for the treatment of painful, inflammatory knee OA.
Post-traumatic Arthritis in Inda (PTOA)
The burden of post-traumatic arthritis (PTOA) in India is significant, with rising rates of knee OA, knee replacement surgery is a crucial treatment option. PTOA accounts for 12% of knee OA & is the third most common indication for TKA [5,6].
Supportive Therapies
In all three conditions’ assistive devices like Canes, walkers, Knee braces provide stability and compression. While knee massagers use heat, vibration, or TENS (transcutaneous electrical nerve stimulation) for pain relief. Heating pads and foam rollers can also be used to reduce pain and muscle soreness and improve mobility. Physical therapies like exercises, electrotherapy, and manual techniques help to improve strength, flexibility, range of motion, and reduce pain [3].
Surgery
In severe cases, or if treatments referred above are not effective, surgery is advised. In India, knee surgeries offered for pain are diverse, including arthroscopy, ligament reconstruction (ACL, PCL), meniscus repair/removal, cartilage repair, and knee replacement (partial or total). Total knee replacement is a common option for severe joint damage, while partial knee replacement focuses on specific compartments.
Total knee arthroplasty Procedure (TKAP)
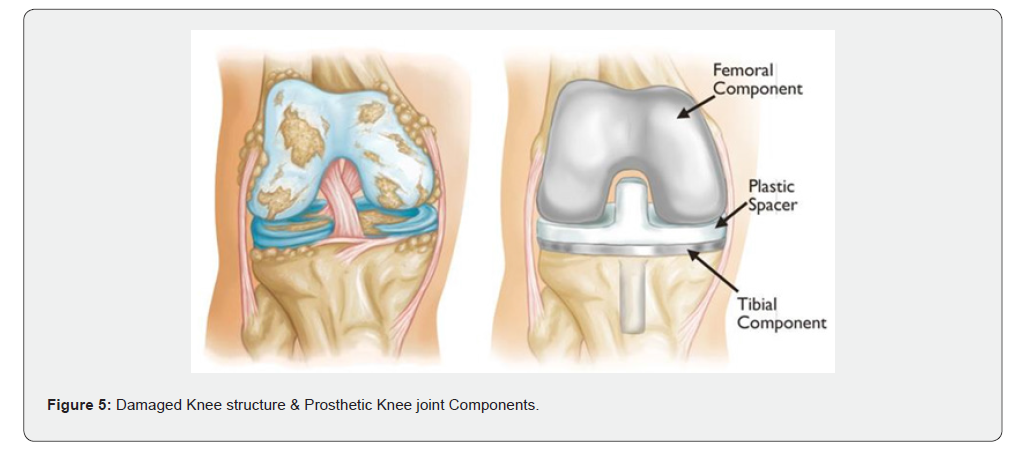
Surgery for replacing the knee joint (also known as total knee arthroplasty-TKAP) is performed either under general anesthesia, or spinal or epidural anesthesia and our case was done epidural anesthesia. The knee is opened through an incision of 8 - 10 inches long. The kneecap is moved so that the damaged part of the cartilage at the end of the Femur, and shin bones Tibia and Fibula are cut and replaced with a metal prosthesis. In between the metal prosthesis, a medical-grade plastic spacer is inserted for a smooth gliding surface. The back portion of the kneecap is replaced with the prosthesis made of strong plastic. After fixing the knee joint prosthetic, pins, screws, or cement is used to secure the new joint in place. In our cases cement was used. The incision is closed & dressed to prevent infection [7,8] (Figure 5).
Advantages of total knee replacement surgery
Total knee replacement surgery (TKRS) relieves knee pain, and the Prosthesis effectively restores the alignment and function of the knee. After a TKR procedure, the patient can lead a normal life and do routine activities independently.
TKR Eligibility Criteria
TKRS is recommended when other treatments like anti-inflammatory medications, lubricating injections, cortisone injections, or physical therapy have failed to offer relief from knee pain and stiffness in patients who find performing everyday activities like walking, bending, sitting, or standing an ordeal due to severe knee pain and stiffness; when knee pain continues even while resting or sleeping; when knee swelling does not subside with rest and medicines, or those with bowed-knee deformity [4].
The Orthopedics Evaluation
An orthopaedic evaluation is performed to assess the condition and determine the best treatment that offers relief from the chronic pain, stiffness, and disability of the knees. An Orthopedic evaluation includes: i) Medical history about general health and about the severity of knee, or hip pain while doing everyday activities ii) A physical examination is performed to assess knee, motion, muscle strength, and overall alignment iii) X-rays help to assess the severity of damage and deformity of the knee iv) Other tests including blood investigations, advanced imaging tests like MRI, etc. are also done.

Outcome: There may be some numbness at the incision site and some level of stiffness which is resolved over some time. Most patients can bend their knees or kneel much better than they would before the implantation. Individuals feel the clicking of the metal & plastic while bending or walking. The new metal implants in the knee will activate metal detectors at airports, malls, etc. Informing about the knee replacement surgery will solve the security issue.
Precautions after Surgery/Possible Complications
After surgery, the patient must avoid injuries, falls, aggressive motion, etc. as they may cause fractures. Light physical activity or exercises may help strengthen and mobilize the new knees. A follow-up after a week and another after one month would suffice. You may have to contact your orthopaedic surgeon in case of a dental procedure that requires taking antibiotics. Make sure not to miss any of your routine follow-up examination and x-rays. Knee surgery is safe and effective, with few post-surgery complications (< 2%) like knee joint infection, Blood clots issues. One of the most common complications of knee replacement surgery like any surgery is the formation of blood clots in the veins of the leg (pelvis, calf, or thigh) which can become life-threatening if they reach lungs or heart via circulation. Medication like blood thinners, early mobilization, stockings, and periodic evaluation of legs will prevent this complication. Infection in the incision site or near the implant may occur within days or weeks of surgery or even after years, while minor infections are generally treated with antibiotics, major infections may require another surgery and antibiotics. Infection in other parts of the (septicemia) body can also spread to the knee joint replacement. Implant components may loosen, and their surface may wear and tear with time even with advanced and improved implants. Scarring the knee, restricting the movements. Rarely, nerves or blood vessels around the knee can get damaged during the surgery [7,8]. Activities to avoid at home/daily routine after both TKR: Significant improvement in pain relief and the ability to perform regular activities are the benefits of the TKR surgeries. Avoiding weight gain, lifting heavy weights, or doing high-intensity exercises like jumping, running, skipping, etc. which cause the implants to loosen and dislocate must be avoided. However, walking, swimming, driving, etc. can be done regularly for several years. Patients are discharged from the hospital within 1 to 5 days and can resume their everyday activities for about 6 weeks post-surgery. Complete recovery may take up to 6 months. The most crucial part of recovery is to avoid strenuous activities, regain strength and mobility with exercises & avoid complications. Healing may take a bit longer in elderly people, or those with underlying medical conditions, or those who smoke and drink alcohol.
Minimally Invasive TKR (MITKR) vs Traditional TKR (TTKR)
More than 90% of knee replacement surgeries are considered successful leading to a recovery patients have Less knee pain and improved knee function. While common, total knee replacement is a major surgery, and recovery requires several days of physical therapy. Minimally invasive knee replacement is an example of evolving efforts in trying to improve outcomes for patients. Minimally invasive total knee replacement offers potential benefits over traditional surgery, including smaller incisions, reduced tissue trauma, and potentially faster recovery, but both approaches can lead to successful pain relief and improved mobility [9]. Total Knee Arthroplasty (TKA) has been described as an effective and successful mode of treatment in alleviation of pain and restoration of function in patients with Rheumatoid Arthritis (RA). The array of bone and soft tissue deformities in RA patients can impact initial success and long-term durability of TKA. Medial Pivot (MP) prosthesis is fixed bearing asymmetric pivoting design that provides anterior-posterior stability without any post and conserves bone on the femoral side. Twenty-six patients (average age 55 years) with end stage arthritis secondary to RA operated with MP prosthesis were retrospectively followed up. At a minimum follow up of three years, all patients were assessed using Knee Society Score (KSS), Oxford Knee Score (OKS), Pain Catastrophizing Scale (PCS) and radiological outcomes. At final follow-up, patients reported significant improvement in mean KSS-Objective and Functional scores, Oxford Knee Score and Pain Catastrophizing Scale (p < 0.05).
The mean range of motion achieved at the end of two years ranged from 0 ͦ (extension) to 109.4 ͦ (full flexion). There was no evidence of loosening or osteolysis at minimum follow up of three years. These results endorse satisfactory clinical and radiological outcomes at minimum follow up of three years following Medial Pivot Prosthetic Knee design in RA patients [8]. TKR for Rheumatoid arthritis is a chronic autoimmune inflammatory disease affecting the joints resulting in pain and stiffness. It affects females more commonly, usually starting in their 30’s. There are reportedly 10 lakh cases diagnosed in India every year and many remain undiagnosed. Management focuses on reducing inflammation, managing pain, and preserving joint function through medication, physical therapy, and lifestyle modifications. There is no cure for rheumatoid arthritis. Joint damage can happen quickly without treatment. But clinical studies show that easing symptoms. If treatment starts early, the long-term damage to the joints can be limited. However, there are many cases who are late seeking treatment or in whom the disease is extremely aggressive. These patients may in their lifetime require injections of steroids into the joints or arthroscopic debridement, and in very advanced cases joint replacement surgery.
Contra-indications for Knee replacement:
a. Systemic infection or is prone to infection. Infection is
considered a serious post-surgical risk, in some cases life-threatening.
b. Significant problems affecting the muscles or soft tissues
surrounding the knee, such as a neuromuscular disorder.
c. medical condition that may interfere with safely administering
anesthesia.
d. Skin condition, such as psoriasis, in the area to be operated
on, as they affect successful healing and increase the likelihood
of infection.
e. Pain associated with arthritis does not severely limit activities
of daily living and/or negatively impact quality of life daily.
f. Certain health problems like uncontrolled diabetes, severe
vascular diseases indicated by a loss of pulse in the leg, skin
ulcers, and/or significant swelling, morbid obesity, poor dentition
with loose teeth, cavities, or gingivitis and Severe anemia, severe
malnutrition, active smoking, need to be addressed prior to elective
total knee replacement to reduce the risk of serious complications
[4].
Cost of Total Knee Replacements
Total knee replacement costs vary significantly between India, the USA, and the UK. In India, the cost is typically much lower, ranging from INR 300,000 to INR 6,00,000 (3500-5000 US$) per knee. Minimal invasive surgeries cost an additional INS 100,000 (US 1K$). Private hospitals in India are often more expensive than government hospitals, based on their star status. The USA has the highest cost, with averages between $32,570 and $70,000, while the UK falls in between with prices ranging from £12,000 to £16,000.
Conclusion
i. Knee OA and Rheumatoid arthritis are major causes of
disability and reduce quality of life, impacting daily activities and
societal productivity.
ii. OA prevalence in India ranges from 22% to 39% among
those aged 40 and above and its prevalence is higher, among women,
and increases with age.
iii. While 15-20 million individuals with Osteoarthritis may
benefit with TKR surgery presenting a significant burden in India,
only a fraction can afford it.
iv. The number of males affected by RA across all age
groups increased from 224,505 in 1990 to 704,401 in 2021, while
the number of females increased from 594,068 to 2,062,348 an
annual increase rate of 7% in men and 8.2% in women.
v. Total Knee Arthroplasty (TKA) is an effective & successful
treatment in alleviation of pain & restoration of function of
knees in patients that do not respond to medicines.
References
- Rheumatoid-arthritis/diagnosis-treatment/https://www.mayoclinic.org/ 04/09/2025.
- Wei Shi, Xinyu Liang, Huafeng Zhang, Hui Li (2025) Burden of rheumatoid arthritis in India from 1990 to 2021: insights from the GBD Database. Front Med (Lausanne) 12: 1526218.
- Osteoarthritis/diagnosis-treatment.
- Saravanan Kandasamy, Rajalakshmi Vadivelu, Sathish Kumar Shanmugam, Balaji S Mahendran (2024) Exploring the Burden of Knee Osteoarthritis in Rural South India Among Adults Aged 40+ Saravanan Cureus 16(11): e73452.
- Post-traumatic arthritis.
- Hesham Saleh, Stephen Yu, Jonathan Vigdorchik, Ran Schwarzkopf (2016) Total knee arthroplasty for treatment of post-traumatic arthritis. World J Orthop 7(9): 584-591.
- Total Knee Replacement.
- Rajesh Malhotra, Ritvik Janardhanan, Sahil Batra (2021) Total Knee Arthroplasty in Rheumatoid Arthritis patients with a medial stabilized prosthesis - A retrospective analysis, J Clin Orthop Trauma 21: 101566.
- Vivek Sood (2014) The Pros and Cons of Minimally Invasive Knee Replacement Surgery. Arthritis-health.






























