Abstract
A retrospective study evaluates the results of resection of the first row of carpal bones in 12 patients with Kienböck’s disease at Lichtman stages III and IV. Data analysis after an average follow-up of 4 years shows significant improvement in pain, range of motion, and wrist function. These results confirm the value of this surgical approach in improving the patients’ quality of life.
Keywords:Kienböck; Resection; First row; Lishtman stage
Introduction
Kienböck’s disease, or avascular necrosis of the lunate, is a rare and complex degenerative condition of the carpus. This pathology is characterized by the progressive deterioration of the lunate, leading to chronic pain and loss of wrist function. Treatment choices depend on the stage of the disease according to Lichtman’s classification. Among the surgical options for advanced stages (III and IV), resection of the first row of carpal bones (PRC) is an interesting alternative. However, the optimal timing for this intervention remains a topic of debate. This article aims to clarify the criteria for first-row resection based on recent data from scientific literature.
Materials and Methods
The study was conducted on 12 patients diagnosed with Kienböck’s disease between 2017 and 2023. The included patients were at Lichtman stage III or IV and exhibited painful symptoms and functional wrist limitations. All patients underwent resection of the first row of carpal bones. The average follow-up was 4 years. The evaluation criteria included pain (visual analog scale - VAS), range of motion (flexion/extension), wrist strength, and functional wrist score (DASH). The student’s t-test was used to assess differences between preoperative and postoperative values. A significant threshold of p < 0.05 was considered.
Result
Among the 12 patients included in the study:
• 9 were womens (75%).
• 3 were mens (25%).
• The average age was 45 years ± 7 years (range 35 to 58 years).
All patients had functional wrist limitations and inflammatory symptoms.
A radiological assessment consisting of a conventional wrist X-ray in both frontal and lateral views, as well as CT, was performed on all patients, allowing for classification of the patients at stage III and IV of Lichtman (Figure 1). All patients underwent the same surgical technique through a posterior approach. The procedure involved opening the retinaculum and denervation of the NIP (nervus interosseus profundus). A T-shaped arthrotomy was performed, followed by resection using a cold blade while preserving the anterior capsuloligamentous plane (Figure 2). Pain significantly decreased in all patients. The VAS score decreased from an average of 6.5 ± 1.2 before the procedure to 2.3 ± 1.1 at the last follow-up (p < 0.01). This pain reduction was consistently observed throughout the follow-up period. Range of motion (flexion/extension) also showed notable improvement. The average flexion/extension increased from 65° ± 10° preoperatively to 85° ± 8° postoperatively (p = 0.02). This improvement allowed the patients to regain satisfactory functional mobility (Figures 3 & 4). Grip strength significantly improved. It increased from 55% ± 8% of the strength of the healthy side to 72% ± 6% at the last follow-up (p = 0.03). The functional wrist score (DASH) decreased, reflecting an improvement in quality of life. The average score dropped from 32 ± 7 preoperatively to 14 ± 5 postoperatively (p < 0.01). No major complications were reported during the follow-up. One patient developed mild carpal osteoarthritis at 4 years postoperatively, but this did not require further intervention.
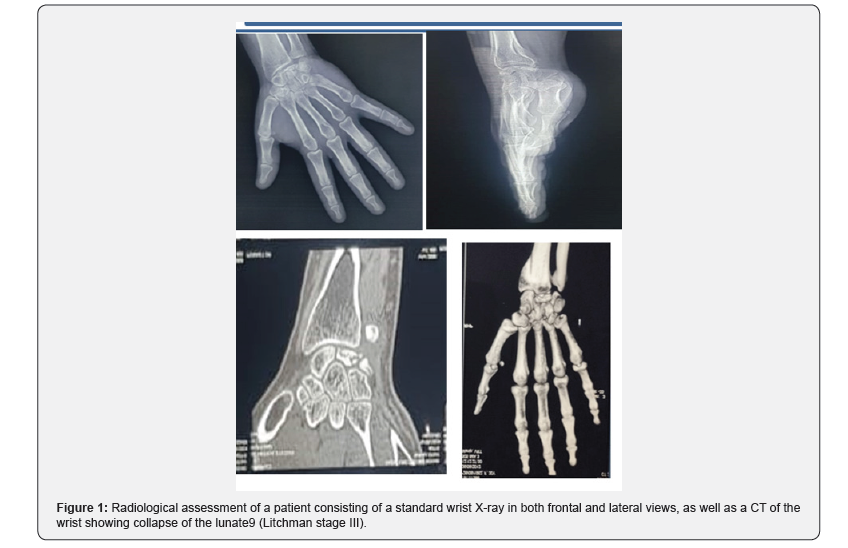
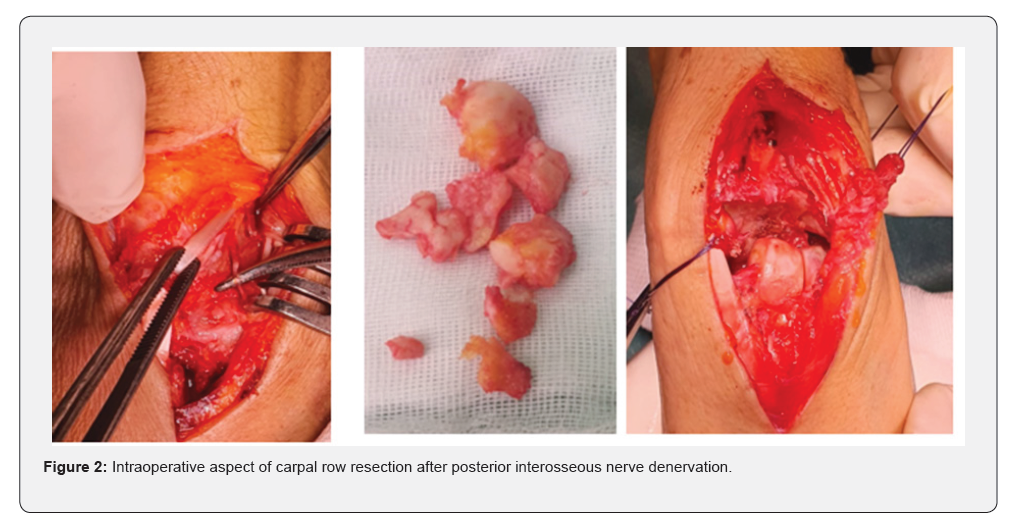
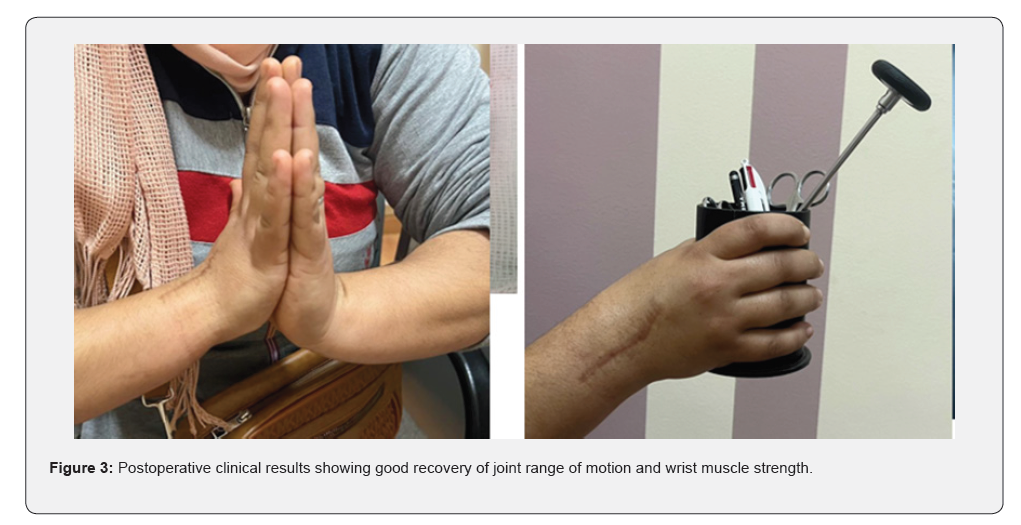
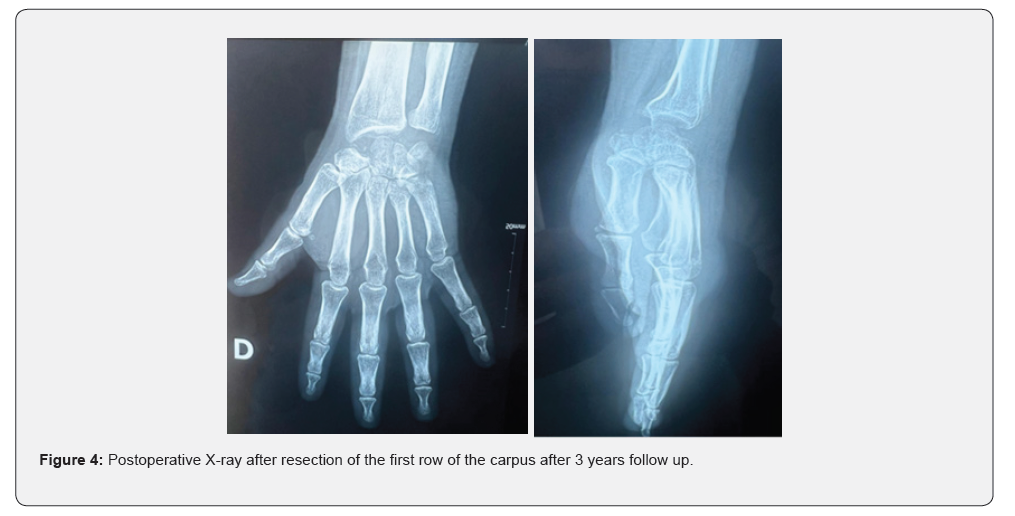
Discussion
Kienböck’s disease was first described in 1910 by Robert Kienböck, an Austrian radiologist, who identified it as avascular necrosis of the lunate associated with painful symptoms and loss of wrist mobility [1]. Initially considered a form of chondromalacia, its pathophysiology has evolved over time, and it is now recognized as a multifactorial condition involving vascular, mechanical, and anatomical anomalies [2]. In 1977, Lichtman proposed a fourstage classification based on the radiographic progression of the disease, which helps adapt therapeutic strategies depending on the severity of bone and joint involvement [2]. With the improvement of imaging techniques and a better understanding of risk factors, new therapeutic approaches, including resection of the first row of carpal bones, have been developed to preserve wrist function and alleviate pain [3]. Kienböck’s disease at stage IV is characterized by advanced destruction of the lunate with arthritic involvement of the radiolunate and midcarpal joints. At this stage, surgical options should aim to relieve pain while maintaining acceptable joint function. Among these options, resection of the first row of carpal bones (PRC) stands out as an effective alternative to total wrist arthrodesis and full joint prostheses. The study by De Smet et al. evaluated the results of PRC in 21 patients with advanced Kienböck’s disease. After an average follow-up of 67 months, 76% of the patients experienced mild or no pain, and grip strength improved from 19 kg to 26 kg (65% of the strength of the unaffected side) [4]. These results highlight that PRC provides significant functional gains, although some patients may experience persistent pain. Furthermore, Marcuzzi et al. studied a variant of PRC combined with the implantation of a pyrocarbon prosthesis (RCPI implant) to preserve wrist stability after bone resection. The average follow-up of 27.6 months showed significant pain reduction, improved range of motion, and satisfactory grip strength, with no major complications such as dislocation or implant fracture [5].

Another study by Kopel confirmed these findings, reporting high patient satisfaction with grip strength representing 77% of the opposite side [6]. However, approximately 20% of patients required secondary surgery, mainly for conversion to arthrodesis. A longer follow-up study by Couturier et al. on 94 RCPI implants showed similar results, with pain reduction and preservation of wrist mobility, but a significant risk of failure requiring conversion to total arthrodesis [7]. These data indicate that, although PRC combined with a pyrocarbon implant offers a reasonable compromise between pain and mobility, it requires careful patient selection and optimized surgical technique. Long-term studies also show that PRC alone may present a risk of symptomatic radiocapitate joint degeneration, especially in patients at stage IV. Croog and Stern report that this risk increases over time and must be considered when choosing this surgical technique [8]. This suggests that prolonged follow-up is necessary to detect late complications and adjust management accordingly.
Conclusion
Resection of the first row of the carpus in Kienböck’s disease can only be considered when the resources of conservative surgery have been exceeded, or from Lichtman stage III onwards. It preserves wrist mobility with a strength greater than or equal to half that of the opposite side, while eliminating pain. results are stable and satisfactory over the long term. This technique should be avoided in young subjects with high functional requirements. Larger comparative studies are needed to support these results. The addition of a pyrocarbon implant, such as the RCPI implant, seems to improve joint stability and prolong functional benefits, although further long-term studies are needed to confirm its effectiveness and durability.
References
- Kienböck R (1910) Über traumatische Malazie des Mondbeins und ihre Folgezustände: Entartungsformen und Kompressionsfrakturen. Fortschritte auf dem Gebiete der Rontgenstrahlen 16: 77-103.
- Lichtman DM, Degnan GG (1993) Staging and its use in the determination of treatment modalities for Kienböck’s disease. Hand Clinics 9(3): 385-404.
- Allan CH, Joshi A, Lichtman DM (2001) Kienböck’s disease: diagnosis and treatment. J Am Acad Orthop Surg 9(2): 128-136.
- De Smet L, Robijns PH, Degreef I (2005) Proximal row carpectomy in advanced Kienböck’s disease. J Hand Surg Br 30(6): 585-587.
- Marcuzzi A, Colantonio F, Petrella G, Ozben H, Russomando A (2017) Stage IV Kienböck’s disease: Proximal row carpectomy and application of RCPI implant. Hand Surg Rehabil 36(2): 102-108.
- Kopel et al. Evaluation of RCPI implant in addition to proximal row carpectomy for advanced wrist arthritis.
- Couturier et al. Long-term results of the RCPI implant in advanced wrist conditions.
- Croog J, Stern P (2012) Long-term outcomes of proximal row carpectomy in Kienböck’s disease stages III and IV. J Hand Surg Am 1(2): 141-148.






























