Multiple Location of the Glomic Tumor in Children: About a Case
El Boulifi N1,2*, Hajjaji A1,2, Cherqaoui MY1,2, Rouaghi H1,2, Cherqaoui A1,2, Bjitro C1,2, Arihi M1,2 and Aboumaarouf M1,2
1Paediatric Orthopaedic Traumatology Department, Abderrahim Harouchi Mother and Child Hospital, Ibn Rochd University Hospital, Casablanca
2Faculty of Medicine and Pharmacy of Casablanca, Hassan II University of Casablanca, Morocco
Submission: May 21, 2024; Published: June 06, 2024
*Corresponding author: Dr. Najlae El Boulifi, Department of Pediatric Surgery, Abderrahim Harouchi Mother and Child Hospital, Ibn Rochd University Hospital, Casablanca, Email: na.elboulifi@gmail.com
How to cite this article: El Boulifi N, Hajjaji A, Cherqaoui MY, Rouaghi H, Cherqaoui A, et al. Multiple Location of the Glomic Tumor in Children: About a Case. Ortho & Rheum Open Access J. 2024; 23(2): 556110. DOI: 10.19080/OROAJ.2024.23.556110
Abstract
Masson’s glomus tumors [TG] are rare benign tumors, developing from Masson’s glomus, a neuromyovascular structure of the body that participates in thermal regulation. We report a case with two locations, the first at the level of the dorsal aspect of the second commissure of the hand and the second at the level of the palmar surface, surgically treated by a biopsy total excision of the mass whose diagnosis had been confirmed by the histopathological study.
Keywords: Glomus tumor; Hand; Child; Digital localization; Treatment of choice
Abbreviations: TG: Glomus Tumor; MRI: Magnetic Resonance Imaging; PDC: Contrast Agent
Introduction
TG is a neuromyo-arterial hamartomatous proliferation that develops from this corpuscle located in the dermo-hypodermic junction, which is the main player in the regulation of cutaneous microcirculation and thermal regulation. These tumors are most often located in the fingers and represent 1 to 5% of all soft tissue tumors of the hand. The diagnosis is often made in the presence of a painful nodule of the extremities, but the diagnostic certainty is histological. The multiple nodular form remains a rare and unusual form in the hand.
Case Report
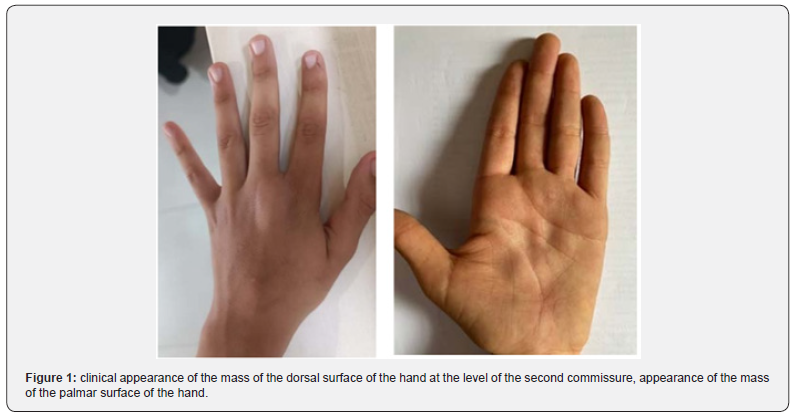
This is a 13-year-old boy, with no particular pathological history, no notion of inbreeding, who consulted for the insidious appearance of two masses, one on the dorsal surface of the second commissure and the other on the palmar side of the left hand evolving over 6 months before and gradually increasing in volume that had become painful. The clinical examination revealed the presence of two soft masses, mobile in relation to the superficial and deep plane and painful on palpation (Figure 1) with normal joint mobility. The examination of the other hand and the general examination did not reveal any abnormalities.
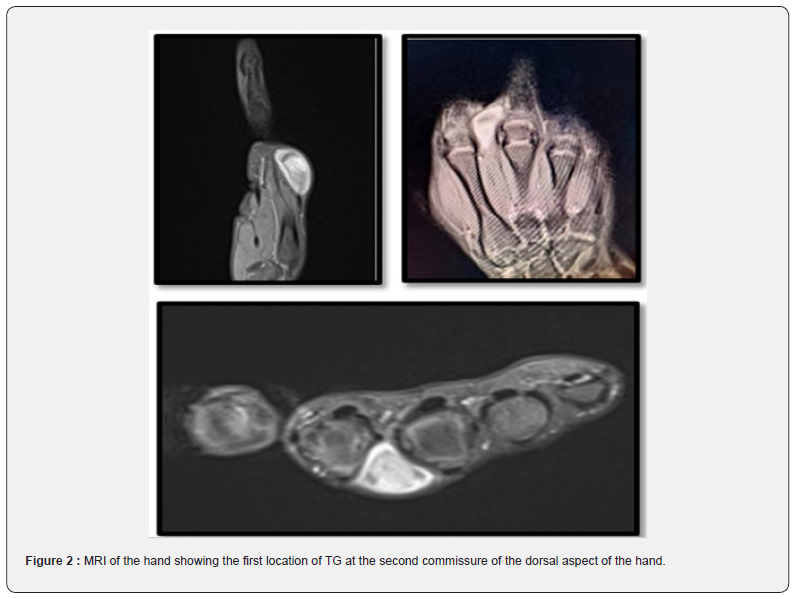
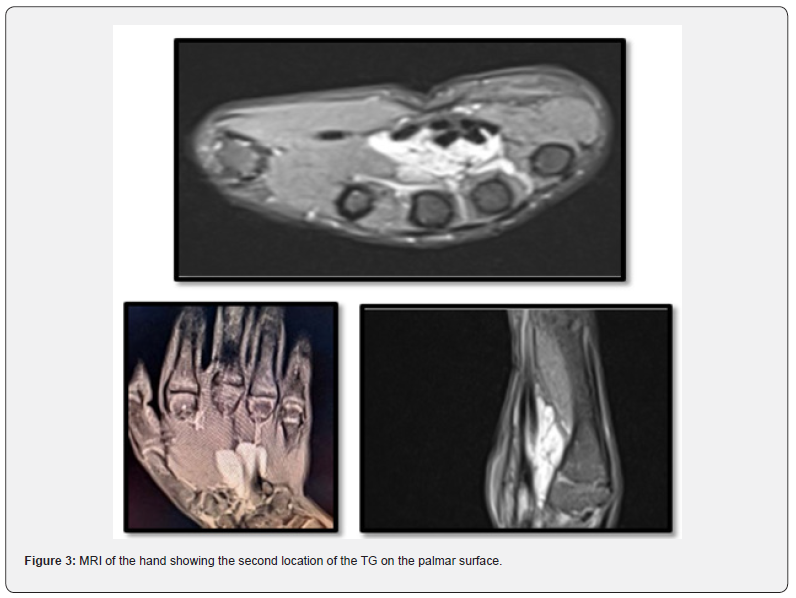
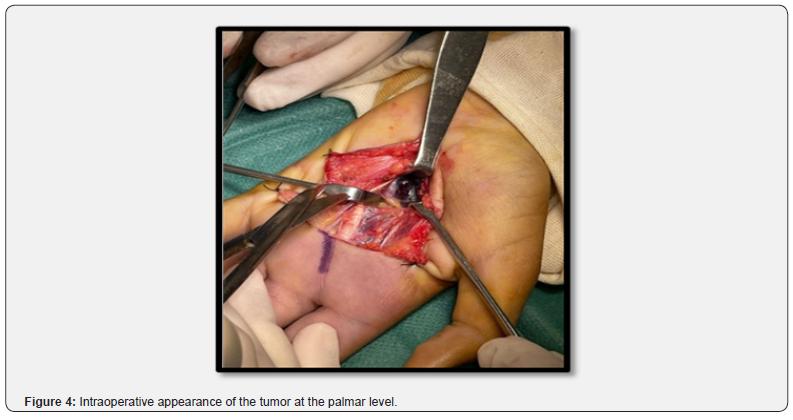
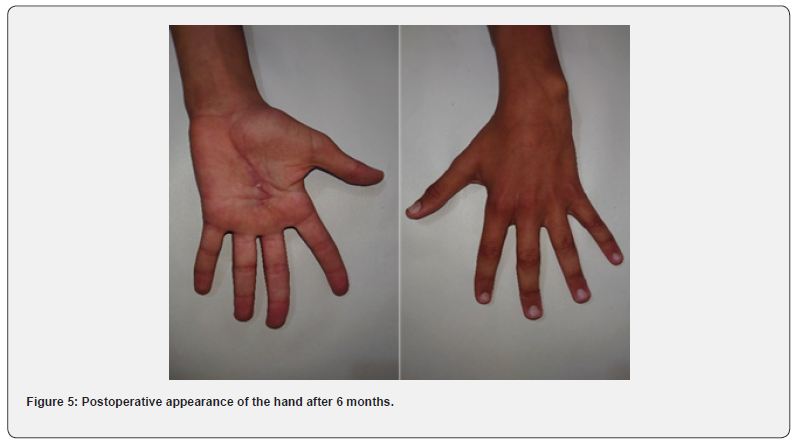
X-rays of the affected hand from the front and 3/4 were normal. The MRI showed a dorsal tissue formation at the level of the2nd commissure of the hand, with regular contours measuring 16x13x27mm in hypo signal T1 and hyper signal T2 enhancing at the PDC with a second formation of the palmar surface measuring 25x 10x26mm (Figures 2 & 3). A biopsy of the two tumor sites was performed. Macroscopic examination revealed a very limited nodular formation of bluish color (Figure 4), the histopathological result confirmed the diagnosis of TG. After a 6- month follow-up, no recurrence or secondary location was found (Figure 5).
Discussion
The first description of TG of the hand was made by Wood and Dimmick in 1812 [1], in the form of "Painful subcutaneous nodules", and it was not until 1924 that Masson [2] specified their origin and gave the name TG. It is a benign tumor developed at the expense of the neuromyoarterial tissue located at the level of the capillaro-venous regulatory anastomoses, which are particularly numerous in the digital extremities. These tumors are rare, ranging in frequency from 1.6% to 5% of all soft tissue tumors in the hand [3]. They mainly affect adults between 30 and 50 years old. Its occurrence in children is exceptional [4], Upton and Coombs found only 9 glomus tumors out of 516 vascular tumors of the upper limb of children [5]. The family history is quite often found given the autosomal dominant mode of inheritance [6].
Digital localization represents 66% of cases (including finger and toe) frequently in the subungua, compared to 33% of extradigital localization including the different parts of the body as well as the viscera (intestinal tract, lung, bone, etc.) [7]. The most frequent extradigital localizations are the hands, feet and forearms [8]. TG is usually solitary; however, it can be multiple [9]. Multiple TGs usually appear in children in extra-digital mode. They are sometimes present from birth [6,9]. Pain is the main reason for consultation in all series, generally localized, throbbing or even disabling, can be spontaneous or caused by contact or even the slightest touch, exacerbated by the cold [9]. However, TG can be painless, especially when it is extra digitally localized. The tumor only becomes visible or palpable after a long evolution. The long delay in diagnosis can also be explained by the rarity of the pathology and the lack of information [10]. Local signs are noted in the form of a spot of a few millimeters that appears by bluish or reddish transparency, rounded or oval [6].
Three tests have a high diagnostic value [11,12]:
i. The Cold-Water Immersion Test: Which triggers a paroxysm of pain when the patient dips their hand in cold water.
ii. The Love Test: Which awakens pain with localized pressure through the application of a pencil tip.
iii. The Hildreth ischemia test: Pathognomonic of TG, based on the disappearance of pain in the tumor area by the creation of an ischemia of the order of 15 seconds with a cuff inflated at the root of the limb around 300 mm Hg.
The place of complementary examinations in the diagnosis is very limited. Thus, standard X-rays are systematically requested to look for bone invasion. Currently, MRI, despite its inaccessibility on a large scale, remains a more efficient examination than ultrasound and arteriography; It can confirm the diagnosis in more than 86% of cases [13]. Diagnostic certainty is provided by histology, which generally shows a proliferation consisting in varying proportions of glomic cells, vascular structures and smooth muscle tissue.
Total tumor removal is always immediately effective and considered the treatment of choice [8,10]. It is advisable to use a direct approach to the mass with good exposure and respect for the principles of skin incisions by avoiding the path of the nerve branches. Recurrences have been reported, they are generally due to incomplete excision, hence the interest in operating on patients without emptying the limb and under magnifying glasses. Sarcomatous transformations have been described but are exceptional, they should be evoked in the presence of a large deep tumor [7,4].
Conclusion
TG is a rare but not exceptional benign tumor that is often misunderstood. The diagnosis is mainly clinical and the treatment is exclusively surgical, the histopathological examination confirms the diagnosis.
Recurrence is exceptional if the excision is complete.
Acknowledgement
The authors declare no conflict of interest in connection with the writing of this article.
References
- Wood WS, Dimmick JE (1977) Multiple infiltrating glomus tumors in children. Cancer 40(4): 1680-1685.
- Masson P (1924) Le glomus neuro-myo-arteriel des régions tactiles et ses tumeurs. Lyon Chi 21: 257-280.
- Vandevender DK, Daley RA (1995) Benign and malignant vascular tumors of the upper extremity. Hand Clin 11(2): 161-181.
- Mravic M, LaChaud G, Nguyen A, Scott MA, Dry SM, et al. (2015) Clinical and histopathological diagnosis of glomus tumor: an institutional experience of 138 cases. Int J Surg Pathol 23(3): 181-188.
- Upton J, Coombs C (1995) Vascular tumors in children. Hand Clin 11(2): 307-337.
- Chatterjee JS, Youssef AHK, Brown RM, Nishikawa H (2005) Congenital nodular multiple glomangioma: a case report. J Clin Pathol 58(1): 102-103.
- Kumar T, Jamal I, Nigam JS, Pandey JK (2020) Malignant glomus tumor of the index finger. Autops Case Rep 10(4): e2020184.
- Lee D-W, Yang J-H, Chang S, Won C-H, Lee M-W, et al. (2011) Clinical and pathological characteristics of extradigital and digital glomus tumours: a retrospective comparative study. J Eur Acad Dermatol Venereol 25(12): 1392-1397.
- Anakwenze OA, Parker WL, Schiefer TK, Inwards CY, Skinner RJ, et al. (2008) Clinical features of multiple glomus tumors. Dermatol Surg 34(7): 884-890.
- Abbassi A, Amrani A, Dendane MA, El Alami Z, El Madhi T, et al. (2012) [Glomus tumor of the finger pulp: an unusual pediatric case]. J Mal Vasc 37(4): 219-221.
- Bhaskaranand K, Navadgi BC (2002) Glomus tumour of the hand. J Hand Surg Br 27(3): 229-231.
- Hildreth DH (1970) The ischemia test for glomus tumor: a new diagnostic test. Rev Surg 27(2): 147-148.
- Drapé JL, Idy-Peretti I, Goettmann S, Guérin-Surville H, Bittoun J (1996) Standard and high-resolution magnetic resonance imaging of glomus tumors of toes and fingertips. J Am Acad Dermatol 35(4): 550-555.






























