Slipped Capital Femoral Epiphysis -A Mini Review
Jonathan Reddy, Arun Hulsoore, Emil Genistopher, Abhay Gahukamble and Thomas Palocaren*
Department of Paediatric Orthopaedics, Christian Medical College, Vellore, TN, India
Submission: January 31, 2024; Published: February 09, 2024
*Corresponding author: Thomas Palocaren, Professor and Head, Department of Paediatric Orthopaedics, Christian Medical College, Vellore, India, Email: thomaspalox@cmcvellore.ac.in
How to cite this article: Jonathan Reddy, Arun Hulsoore, Emil Genistopher, Abhay Gahukamble and Thomas Palocaren*. Slipped Capital Femoral Epiphysis -A Mini Review. Ortho & Rheum Open Access J. 2024; 22(1): 556099. DOI: 10.19080/OROAJ.2024.22.556099
Abstract
Keywords: Slipped capital femoral epiphysis; Dunn’s procedure; In situ pinning; Surgical hip dislocation; Chondrolysis; Avascular necrosis
Abbreviations: SCFE: Slipped Capital Femoral Epiphysis; PI: Pelvic Incidence; AVN: Avascular Necrosis; SHD: Surgical Hip Dislocation
Mini Review
Slipped capital femoral epiphysis (SCFE)is the most common hip disorder affecting adolescents in the age group of 9-16 years occurring in 10.8 per 100,000 children [1], with male-to-female ratios of 3: 1 [2]. In Classical Varus SCFE, the femoral head stays in the acetabulum while femoral neck and the metaphysis moves antero-superiorly whereas in Valgus SCFE the femoral head tilts superolaterally relative to the femoral neck but remains within the acetabulum (Figure 1a & 1b) [3]. Etiology is multifactorial including mechanical, endocrine, and genetic factors. Mechanically unfavorable situations can occur secondary to excessive shear forces, a weak growth plate, or both [4]. Gebhart et al explored variations in two common anatomical measurements, namely pelvic incidence (PI) and acetabular retroversion, and their correlations with post-SCFE deformities, to add to many other implicated factors already proposed such as increased femoral retroversion and increased physeal obliquity, They argued that individuals with a smaller PI might experience an anterior tilt of the pelvis to maintain typical lumbar lordosis and ensure a balanced sagittal alignment of the spine. This forward tilt could lead to increased stress on the anterior aspect of the hip joint, transmitting the stress across the physis of the proximal femur. The heightened stress, combined with other mechanical factors like obesity, physeal sloping angle, femoral retroversion, and the size of the epiphyseal tubercle, could potentially contribute to the development of SCFE [5].
The conventional image of an overweight, hypogonadal male with adiposogenital syndrome is no longer considered universal especially in the Indian subcontinent where endocrinopathies and vitamin D deficiency have been implicated as factors [6]. Despite the prevalent association with hormonal imbalance, there is a lack of substantial evidence supporting hormonal alterations in most patients, even those who conform to the stereotypical image of an overweight, hypogonadal male with chronic bilateral slipped epiphysis [7]. The initiation of slip typically takes place during the phase of rapid growth, but the age of onset is subject to ongoing change. Recent trends indicate a tendency for this period to occur earlier, reflecting a shift in the age profile of individuals experiencing SCFE [8]. The widely accepted classification for SCFE typically categorizes cases as either “stable” or “unstable,” primarily based on the patient’s ability to walk with or without crutches, Additional symptoms may include a mild limp, gait featuring external rotation of the foot, restricted internal rotation of the hip, or a fixed position in external rotation and flexion of the hip, often identified as the Drehmann sign. Conversely, a patient with unstable SCFE typically experiences intense hip pain almost rendering the patient’s inability to stay upright with or without crutches [9].
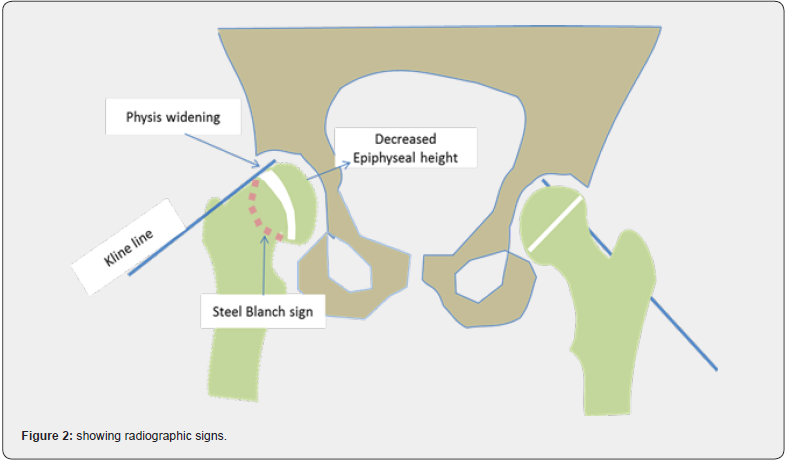
Radiographic evaluation should include anteroposterior and frog-leg views of both hips. In cases of unstable SCFE, a comparative analysis with the unaffected side is crucial. Various radiographic signs (Figure 2) can indicate SCFE, including physis widening, a relative reduction in the height of the epiphysis, absence of intersection of the epiphysis by a lateral cortical line along the femoral neck (referred to as Klein’s line), and the detection of double density at the metaphysis (known as the Steel sign, attributed to the posterior slip of the epiphysis) [10]. The magnitude of slip is measured using Southwick’s method, which evaluates the extent of sliding by measuring the angle between the head and femoral diaphysis on anteroposterior and axial X-ray projections. This angle is then compared with the corresponding angle on the unaffected side in cases of unilateral involvement or with established normal values for instances of bilateral participation (145° in anteroposterior projection and 18° in axial projection). The degree of sliding is characterized as mild when the angle deviation is less than 30°, moderate if the angle falls between 30° and 60°, and severe if the difference exceeds 60° [11].

Treatment
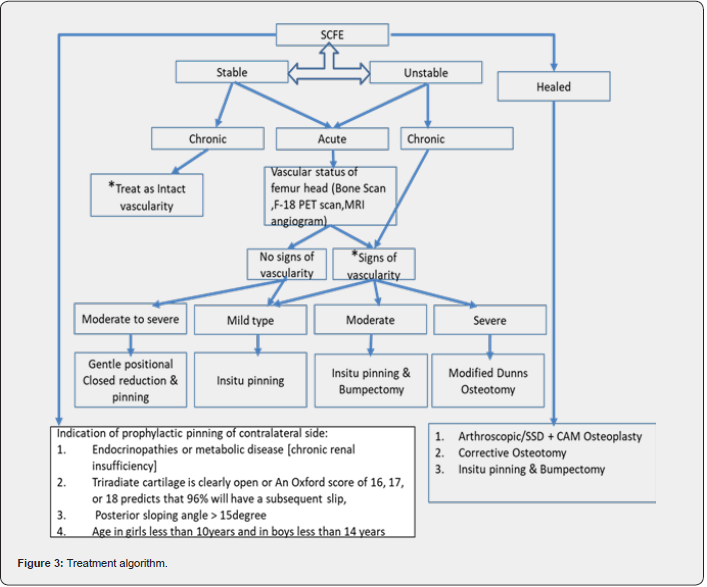
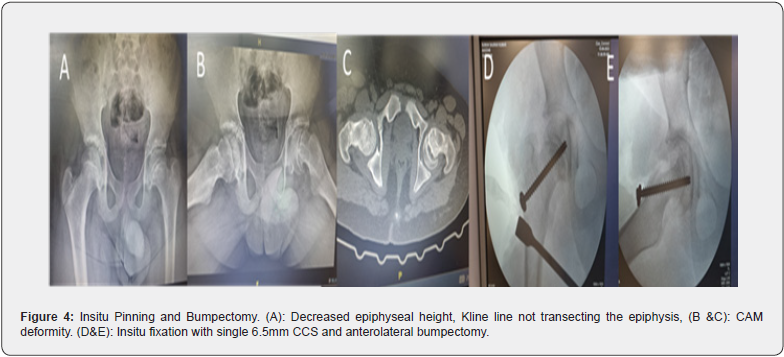
Most authors agree that once SCFE is diagnosed, surgical treatment is indicated, but significant controversies remain regarding the best treatment [12]. The goals of management are to stabilize and prevent additional slippage and correct the deformity, to prevent the dreaded complications such as osteonecrosis and chondrolysis. The classical approach to treating mild SCFE involves percutaneous in situ-fixation of the epiphysis, however, for moderate to severe type of deformity, there has been no consensus due to the introduction of new treatment approaches such as anatomic realignment and modified Dunn’s osteotomy over the last 2 decades. At our center the treatment approach has evolved over the years and now we have formulated an algorithm based on the severity of slip, stable or unstable, and acute or chronic type (Figure 3). Percutaneous in situ fixation technique is designed to prevent further displacement until the eventual closure of the growth plate. It is a widely employed method for both stable and unstable SCFE cases, irrespective of the degree of deformity [13]. The optimal placement for a single screw in the treatment of SCFE is in the center of the neck and perpendicular to the growth plate, at least 3 threads of the screw across the physis (Figure 4). As the severity increases the epiphysis is placed more posterior and the entry point becomes more anterior to cross the physis perpendicularly, starting the entry medial to the intertrochanteric line makes the screw head intra-articular and later present as anterior impingement pain. Penetration of screw and intra-articular pins causes chondrolysis and this incidence has reduced with the advent of intraoperative fluoroscopy [14]. The use of a single fully threaded stainless screw is advocated for in-situ pinning as titanium cannulated screws can prove difficult to remove, a phenomenon attributed to the propensity of bone growth over the screw head., Considering this, several authors have advocated for the use of fully threaded (no-cutback mechanism) stainless-steel screws. This recommendation is grounded in the belief that stainless-steel screws may reduce the likelihood of bone overgrowth, potentially easing the process of removal of screws [15]. The other most important factor that one needs to take in consideration is the timing of surgery especially in cases of unstable SCFE, as there is a growing body of evidence indicating that early intervention, within 24 hours, is likely to result in a lower rate of avascular necrosis (AVN) [16].
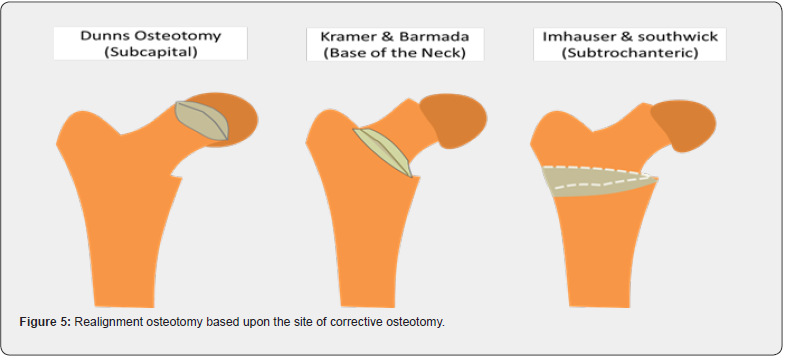
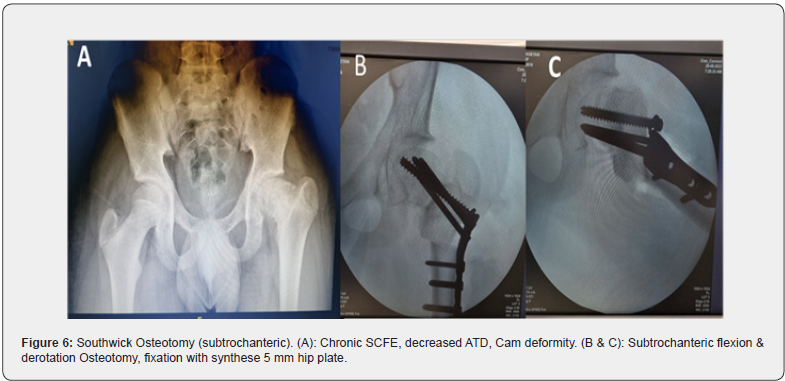
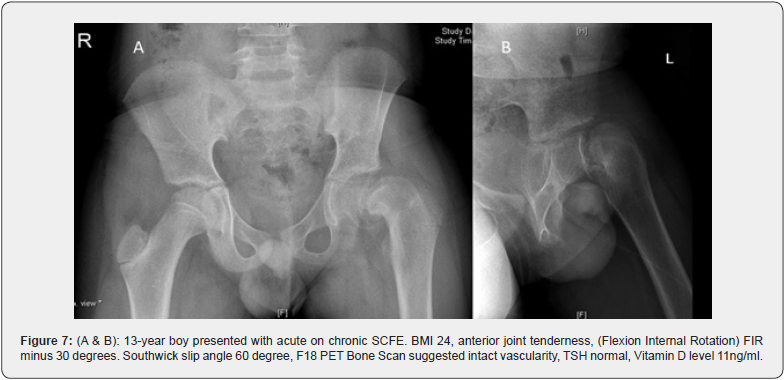
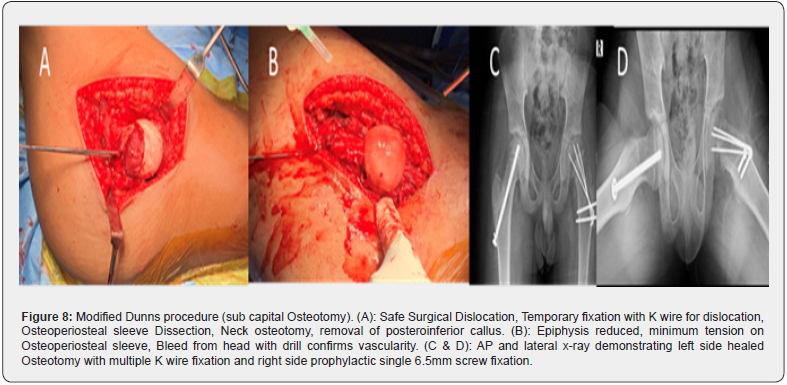
There is no consensus about uniform treatment guidelines in patients with moderate to severe slips. The technique introduced by Ganz namely the Surgical Hip Dislocation (SHD) technique for anatomical realignment /osteochondroplasty has become more widely used [17]. This technique allows an anatomic reorientation of the epiphysis protecting retinacular vessels and epiphyseal vascularization [18]. Historically for severe slips various named realignment osteotomy were described based upon the site of corrective osteotomy (Figure 5 & Figure 6). Initially, modified dunn osteotomy didn’t gain acceptance as a choice of treatment for severe slip due to the high incidence of iatrogenic AVN up to 40% [19]. However, with better knowledge of the vascularity of the femoral head, modified dunn osteotomy has become an alternative for the management of acute unstable SCFE (Figure 7a & 7b (preop), Figure 8a-d( intraop & post op)). The incidence of bilateral SCFE varies between 14% and 63% , This risk can escalate to as high as 80% when SCFE is diagnosed at a very young age and reaches up to 100% when endocrinopathies are associated [20]. Prophylactic pinning of the contralateral clinically normal hip is typically done for very young children, and individuals with endocrinopathies [21].
Complications
The potential complications include progression of the slip, instability, growth arrest, residual deformity, chondrolysis, and osteonecrosis of the femoral epiphysis [22]. Avascular necrosis (AVN) is a dreaded complication in acute unstable SCFE. Numerous studies have revealed AVN rates ranging from 6% to 58% in unstable SCFE, whereas the rate approaches zero in stable SCFE. Various factors contribute to the development of AVN, including hip instability with epiphyseal separation from the metaphysis, delayed time from presentation to surgery, the severity of the slip, younger age, a short duration of prodromal symptoms, increased intracapsular pressure, and the chosen surgical technique. The assessment of risk factors associated with AVN in SCFE has been studied and female sex and slip magnitude at presentation have been implicated as predisposing factors for AVN [23].
Conclusion
Management of SCFE, especially the moderate and severe variety, has lacked consensus over recent years due to the evolving treatment options including capital realignment techniques and the advent of minimally invasive techniques such as hip arthroscopy. In situ fixation, involving pins or screws through the physis has been the standard of care for the treatment of stable SCFE, however, the advent of modern reconstructive procedures has provided alternatives in the case of acute unstable slips which have a higher risk for avascular necrosis. These realignment procedures themselves carry a risk of iatrogenic AVN but if these procedures can be made safer with intraoperative monitoring of the blood supply of the femoral head, it can emerge as a suitable alternative to in-situ pinning which has been long considered as the” standard of care” for management of SCFE.
Future research must focus on decreasing the rates of development of AVN and treatment of these complications reducing the need for future arthroplasty and reconstructive procedures in these patients.
Conflict of Interest
The authors have no conflicts of interest to disclose.
References
- Lehmann CL, Arons RR, Loder RT, Vitale MG (2006) The epidemiology of slipped capital femoral epiphysis: an update. J Pediatr Orthop 26(3): 286-290.
- Loder RT (1996) The demographics of slipped capital femoral epiphysis. An international multicenter study. Clin Orthop Relat Res 322: 8-27.
- Loder RT, O’Donnell PW, Didelot WP, Kayes KJ (2006) Valgus slipped capital femoral epiphysis. J Pediatr Orthop 26(5): 594-600.
- Alshryda S, Jones S, Banaszkiewicz P (2014) Postgraduate paediatric orthopaedics: the candidate’s guide to the FRCS (Tr and Orth) examination. Cambridge: Cambridge University Press.
- Gebhart JJ, Bohl MS, Weinberg DS, Cooperman DR, Liu RW (2015) Pelvic incidence and acetabular version in slipped capital femoral epiphysis. J Pediatr Orthop 35(6): 565-570.
- Madhuri V, Arora SK, Dutt V (2013) Slipped capital femoral epiphysis associated with vitamin D deficiency: a series of 15 cases. Bone Joint J 95-B (6): 851-854.
- Wells D, King JD, Roe TF, Kaufman FR (1993) Review of slipped capital femoral epiphysis associated with endocrine disease, J Pediatr Orthop 13(5): 610-614.
- Loder RT, Starnes T, Dikos G (2006) The narrow window of bone age in children with slipped capital femoral epiphysis: a reassessment one decade later. J Pediatr Orthop 26(3): 300-306.
- Loder RT, Richards BS, Shapiro PS, Reznick LR, Aronson DD (1993) Acute slipped capital femoral epiphy- sis: the importance of physeal stability. J Bone Joint Surg Am 75(8): 1134-1140.
- Herman MJ, Martinek M (2015) The limping child. Pediatr Rev 36(5): 184-197.
- Southwick WO (1967) Osteotomy through the lesser trochanter for slipped capital femoral epiphysis. J Bone Joint Surg Am 49(5): 807-835.
- Loder RT (2001) Unstable slipped capital femoral epiphysis. J Pediatr Orthop 21(5): 694-699.
- Loder RT, Dietz FR (2012) What is the best evidence for the treatment of slipped capital femoral epiphysis? J Pediatr Orthop 32(Suppl 2): S158-S165.
- Kibiloski LJ, Doane RM, Karol LA, Haut RC, Loder RT (1994) Biomechanical analysis of single- versus double-screw fixation in slipped capital femoral epiphysis at physiological load levels. J Pediatr Orthop 14(5): 627-630.
- Dragoni M, Heiner AD, Costa S, Gabrielli A, Weinstein SL (2012) Biome- chanical study of 16-mm threaded, 32-mm threaded, and fully threaded SCFE screw fixation. J Pediatr Orthop 32(1): 70-74.
- Kohno Y, Nakashima Y, Kitano T, Taichi I, Atsushi K, et al. (2017) Is the timing of surgery associated with avascular necrosis after unstable slipped capital femoral epiphysis? A multicenter study. J Orthop Sci 22(1): 112-115.
- Ganz R, Gill TJ, Gautier E, Ganz K, Krügel N, et al. (2001) Surgical dislocation of the adult hip a technique with full access to the femoral head and acetabulum without the risk of avascular necrosis. J Bone Joint Surg Br 83(8): 1119-1124.
- Ricciardi BF, Sink EL (2014) Surgical hip dislocation: techniques for success. J Pediatr Orthop 34(Suppl 1): S25-S31.
- Upasani VV, Matheney TH, Spencer SA, Kim YJ, Millis MB, et al. (2014) Complications after modified Dunn osteotomy for the treatment of adolescent slipped capital femoral epiphysis. J Pediatr Orthop 34(7): 661-667.
- Loder RT, Aronson DD, Greenfield ML (1993) The epidemiology of bilateral slipped capital femoral epiphysis. A study of children in Michigan. J Bone Joint Surg Am 75: 1141-1147.
- Anghilieri FM, Morelli I, Peretti GM, Verdoni F, Curci D (2022) Role of the prophylactic fixation of contralateral unaffected hip in paediatric unilateral slipped capital femoral epiphysis: a systematic review. EFORT Open Rev 7(2): 164-173.
- Roaten J, Spence DD (2016) Complications related to the treatment of slipped capital femoral epiphysis. Orthop Clin North Am 47(2): 405-413.
- Thomas P, Holmes L, Rogers K, Kumar Shanmuga J (2010) Outcome of In Situ Pinning in Patients with Unstable Slipped Capital Femoral Epiphysis: Assessment of Risk Factors Associated with Avascular Necrosis. J Pediatr Orthop 30(1): 31-36.






























