Protruded Rode Post Posterior Spinal Fusion in Scoliosis Patient – Case Report
Sulaiman Mohammed Hushlul*, Abdu Zaher Albargi, Abdulaziz Saleh Alharthi and Osama Abdulrahman Alharthi
Degree of Bachelor of Medicine MBBS,UQU, Saudi Arabia board of orthopedic surgery, Saudi Arabia
Submission:February 02, 2023; Published: February 16, 2023
*Corresponding author: Sulaiman Mohammed Hushlul, Degree of Bachelor of Medicine MBBS,UQU, Saudi Arabia board of orthopedic surgery, Saudi Arabia
How to cite this article: Sulaiman Mohammed Hushlul, Abdu Zaher Albargi, Abdulaziz Saleh Alharthi and Osama Abdulrahman Alharthi. Protruded Rode Post Posterior Spinal Fusion in Scoliosis Patient – Case Report. Ortho & Rheum Open Access J. 2023; 21(2): 556059. DOI: 10.19080/OROAJ.2023.21.556059
Abstract
Scoliosis is defined as coronal plane spinal deformity. It is known as the lateral angulation of the vertebra more than 10 degrees which most commonly presents in adolescent girls from age 10 to 18. Scoliosis is divided into two groups which are congenital and idiopathic Scoliosis. We present a case of 18 years old male patient known as mental delayed and cleft palate, complaining of protruded Hardware for three years as post-T4 to L2 Posterior Spinal Fusion who diagnosed as a neuromuscular Scoliosis. The patient lost to follow-up since staples removal and came to the clinic after three years as transferred from primary health care. Upon physical examination, intact motor and sensory exam and normal reflexes, no signs of infection. A serial radiological investigation was ordered, and blood work was done as well. Irrigation and, debridement and hardware removal were performed, the four left proximal pedicle screws were removed. The proximal cutting part of the left rod. Deep tissue culture from different sites was taken for culture and sensitivity, which was positive for staphylococcus Aureus. The patient was kept in the hospital for intravenous antibiotics and seen in the clinic for follow-up. This case report suggests noncompliance can affect the outcome and lead to severe complications. We present a case of protruded rode post scoliosis correction in which underwent removal of loose left four pedicle screws and proximal rode.
Keywords: Non-Idiopathic Scoliosis; Hardware Failure; Protruded Rode; Posterior Spinal Fusion Complication; Infection
Introduction
Scoliosis is a three-dimensional deformity that occurs when the lateral angulation of the vertebra is more than 10 degrees [1]. Scoliosis is divided into two different groups. These are Congenital Scoliosis (CS) and Idiopathic scoliosis (IS) [2]. Congenital Scoliosis occurs at a rate of 0.5-1 per 1000 live births [3]. Although there is no evidence that the long-term effects of scoliosis surgery are superior to the long-term impact of AIS itself, patients can fear the consequences of not undergoing this surgery due to incorrect or insufficient information. The main indication for surgical treatment in patients with AIS is cosmetic. However, spinal surgery may, along with other adverse side effects, cause postoperative clinical deterioration. This complication of surgery has yet to be described in international literature. The surgical management of Scoliosis is associated with significant complications, including blood loss, infection, and neurologic compromise. It has previously been demonstrated that patients with non-idiopathic Scoliosis, especially neuromuscular, have higher rates of infection, blood loss during surgery, and subsequent need for transfusion, than idiopathic scoliosis patients [4]. It should be noted that non-idiopathic patients also have significantly higher medical comorbidities rates than idiopathic patients [5].
Case Presentation
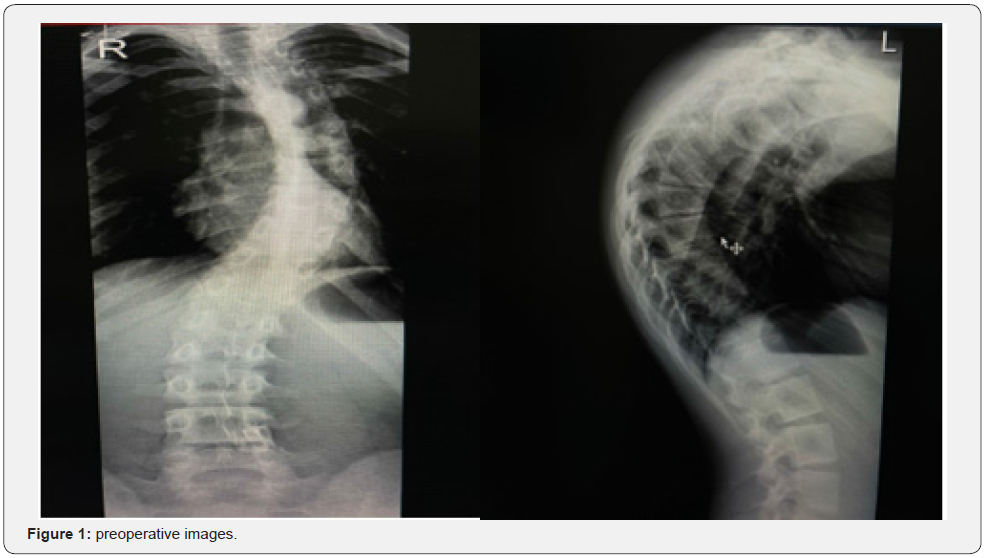
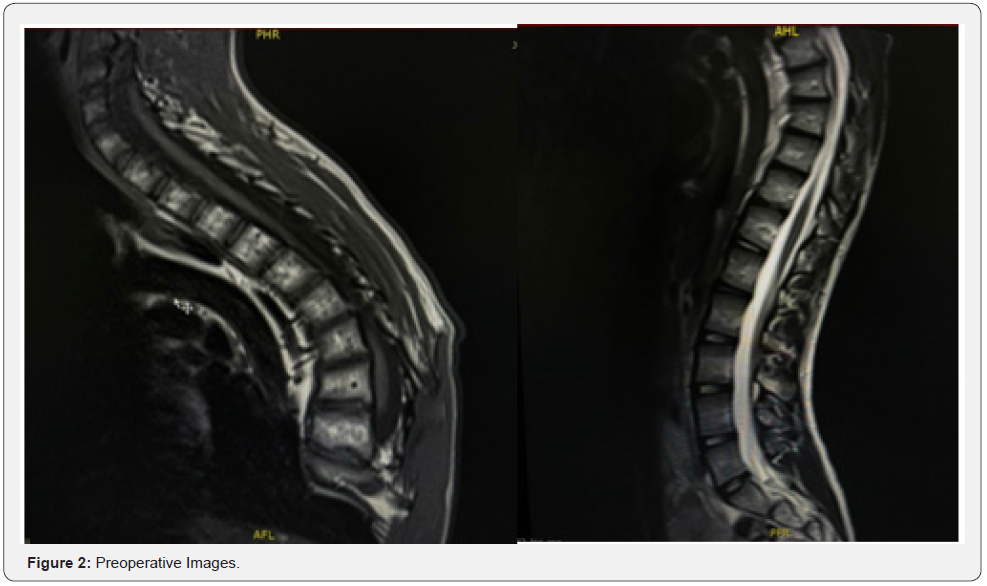
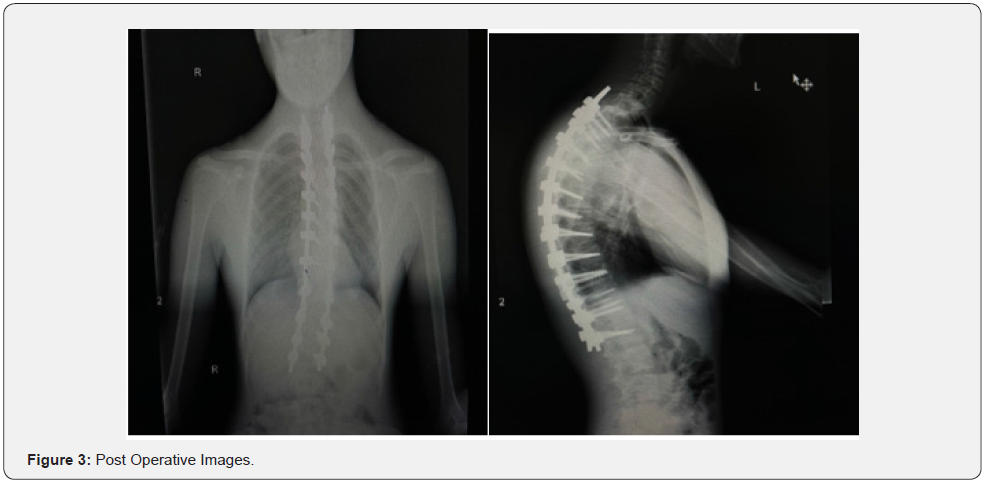
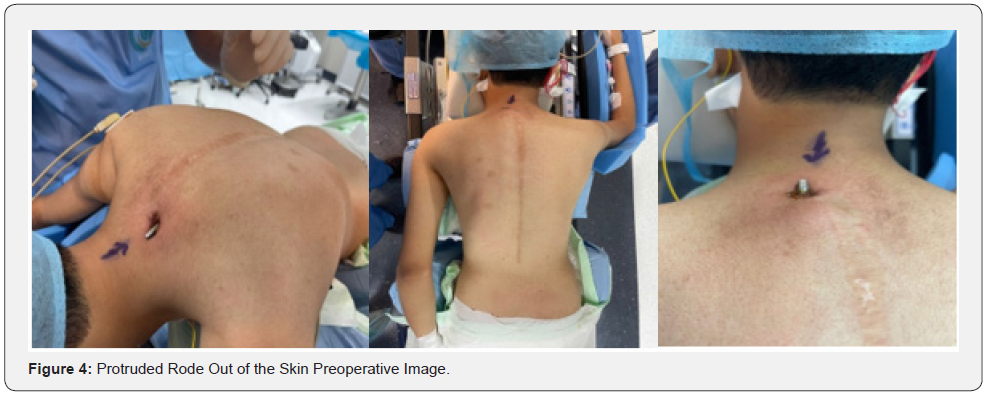
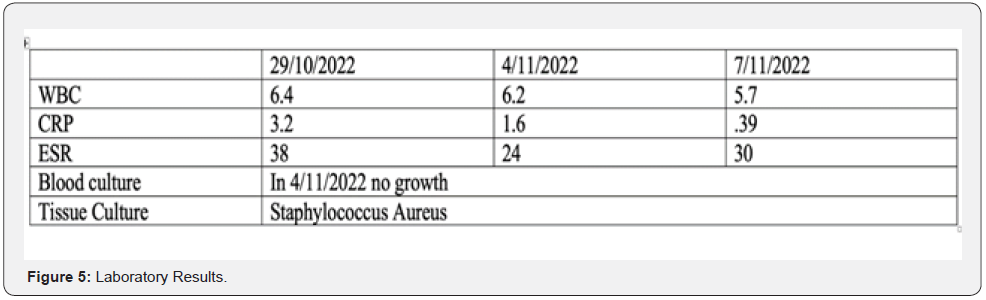
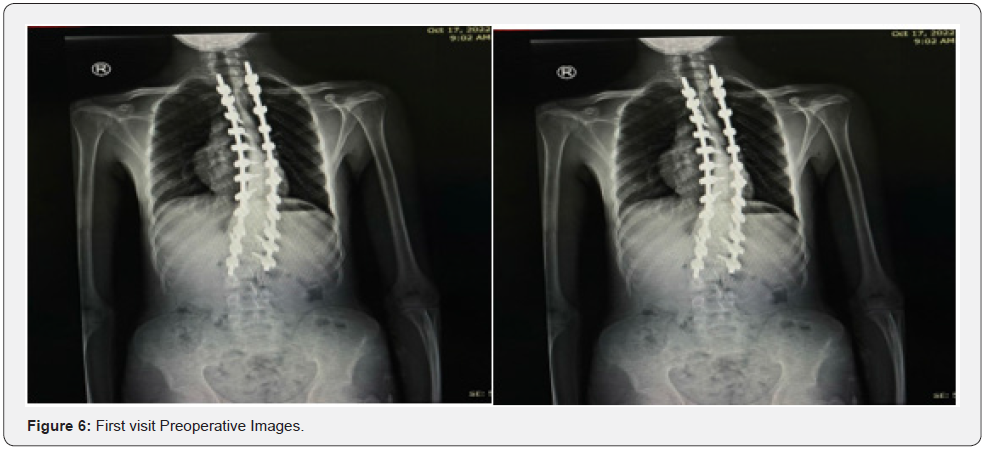
Eighteen years old male patients with a known case of mental retardation and cleft palate presented to the clinic on 27/9/2022 complaining of protruded Hardware in the last three years. Underwent posterior spinal fusion as a case of neuromuscular kyphoscoliosis in 15/10/2018 from T4 to L2. (Figures 1-3). The patient lost to follow-up after staples removal. Then came to the clinic and transferred from primary health care as a case of asymptomatic protruded rode. General examination: vitally stable, normal gait and posture. Obvious protruded rode out of the skin from the back just below the neck 2 cm, with no tenderness, no redness or hotness no discharge around the rod (Figure 4). Motor and sensory upper limb and lower limb intact, normal reflexes. Laboratory investigations and serial scoliosis X-rays were ordered in the clinic (Figures 5 & 6). Discussed with family and explained red flags and complications and preparation for urgent surgery done, Patient Admitted and operated in 30/10/2022.
Operative Technic
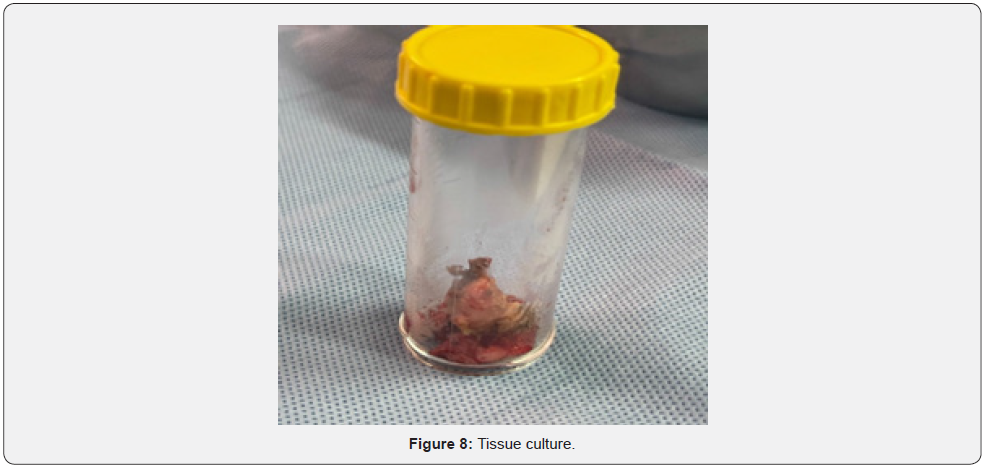
The patient was brought to the holding area, consented and marked done, shifted to the operative room, intubated then moved to Jackson table on a prone position, and Back was washed with soap and water and then prepped and draped in the usual sterile fashion, mark the skin incision using a permanent marker pen, midline longitudinal skin incision made over the previous scar around 40 cm, deep careful dissection done. No obvious bus or devitalized tissue was seen, and the four left proximal pedicle screws were loose and removed. They were cutting the proximal part of the left rod (Figure 7). Deep tissue culture from different sites was taken for culture and sensitivity (Figure 8), irrigation was done using nine litter normal slaine, debridement was done, drain size 18 cc was placed, and the deep layer was closed by vicryl two and subcutaneous tissue closed using 2.0 vicryl and skin closed by staples. Sterile dressing is done, and patient postoperative was stable.

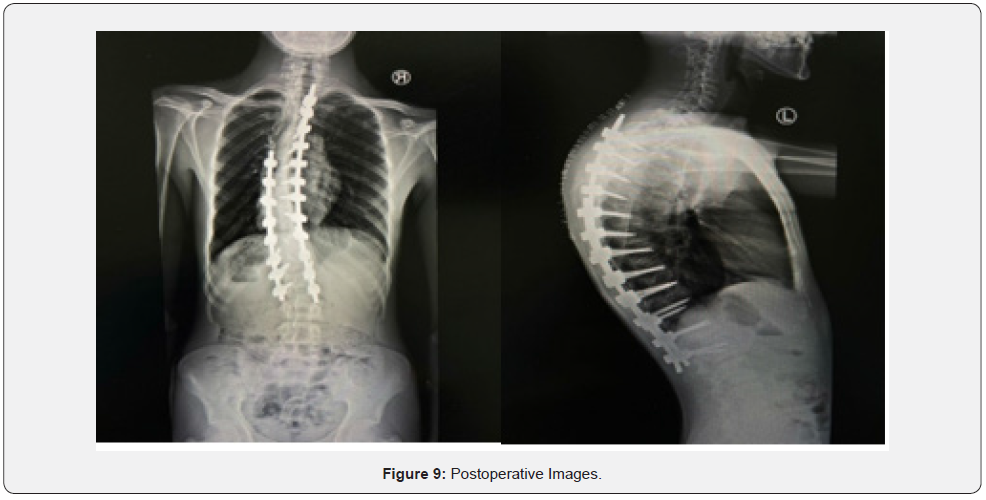
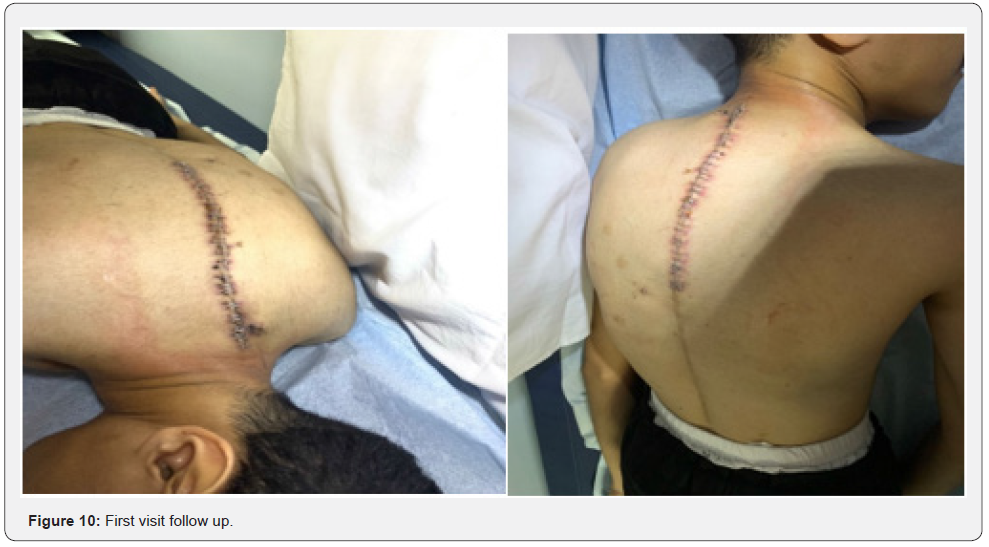
The patient was shifted to a regular bed, and Infectious Disease was consulted for antibiotic type, which was on Ciprofloxacin, and cefazoline (started initially from 30/10/2022 to 7/11/2022)— then changed to cloxacillin (started in 7/11/2022 to 10/11/2022 ) as intraoperative tissue culture was Staphylococcus Aureus. Postoperative x-rays were done and reviewed (Figure 9). The patient has discharged on 10/11/2022 on Cloxacillin 500 mg every six hours per oral for one week as the patient is clinically stable and laboratory-wise improving. First, visit clinic postoperative on 14/11/2022, no new complains, healthy wound no signs of infection or dehiscence, neurological examination intact (Figure 10).
Discussion
Spinal fusion in patients with spinal deformity replaces one pathology (a curved spine) by another (a stiff spine). Therefore, the indication for corrective surgery in patients with spinal deformity is mainly cosmetic. This paradigm is also supported by the fact that signs and symptoms of spinal deformity cannot be changed by spinal fusion [6]. Many articles have been published regarding post-scoliosis correction complications, such as Hawes review [6] lists the complications in the following order:
Death and neurological damage. The incidence of death as a complication of spine surgery for otherwise healthy adolescent and adult patients is reported to be <1% but can also be higher (20%) in the adult population undergoing surgery. Symptoms of neurological damage include partial or total paraplegia, quadriplegia, or peripheral nerve deficit and can emerge a decade after surgery and loss of normal spinal function. In every patient who undergoes spinal fusion surgery, there is an irreversible loss of the average ability of the spine to move. Spinal fusion is correlated with a significantly reduced range of motion over the entire spine, including the non-fused segments [7].
Post-surgery pain, which may develop soon after surgery or after ten years or more, is the primary reason patients must be operated on more than once [6]. Infection and inflammatory processes. Infections introduced into the spinal column during surgery may manifest months or years later [6]. Curvature progression. Some curvatures continue to progress after spinal fusion due to broken rods or other failures of instrumentation [6].
The complexity of spinal surgery is reflected in the diversity of complications that may result in months or years later. Given the time delay and difficulty in diagnosis, it is likely that only a minority of such events are recognized as surgical complications. In one study, 40% of the patients treated surgically as adults required salvage surgery within a follow-up period averaging 55 months after surgery [7].Most of the papers reporting shortterm complications of spinal fusion in patients with Scoliosis are retrospective studies. Just recently, a prospective study on complications has been published, stating the rate of complications being much higher than expected from previous retrospective reviews [8]. Therefore, also the true rate of complications may be higher in the long term than the rate reported so far. In our case, an adolescent patient who had neuromuscular kyphoscoliosis underwent correction from T4 to L2 complicated by protruded rode out of the skin as the patient lost to follow-up, came after three years to the clinic and serial investigations done and planned for surgery. Short-term follow-up showed satisfactory outcomes regarding pain, range of motion, and cosmetic issues in comparison to preoperative. Comparing these findings to the patient with regular follow-up in the literature is of favorable value.
Conclusion
Major spinal surgery has an important risk of severe and different complications, such as massive bleeding and neurologic deficit, and hardware failure. The surgeon must have an organized plan with measures and monitoring aimed at the best possible outcome, following evidence-based recommendations where the benefit exceeds the risks. These techniques may be used successfully in patients whose principles forbid blood transfusion, offering the possibility of surgery fulfilling their personal beliefs. We report this case of an unusual complication of scoliosis correction. This case demonstrates the importance of pre-surgical planning, patient selection, and the importance of patient followup. In the future, we may consider pre-surgical planning and patient selection as a must to avoid noncompliance and unusual complications.
Human Ethics
Consent was obtained by all participants in this study.
Footnotes
The author reports that he has no conflicts of interest in the authorship and publication of this article.
References
- Haleem S, Nnadi C (2018) Scoliosis: a review. Paediatrics and Child Health 28(5): 209-217.
- Giampietro PF, Blank RD, Raggio CL, Merchant S & Jacobsen FS, et al. (2003) Congenital and idiopathic scoliosis: clinical and genetic aspects. Clinical Medicine & Research 1(2): 125-136.
- Cho W, Shepard N & Arlet V (2018) The etiology of congenital scoliosis: genetic vs. environmental: a report of three monozygotic twin cases. European Spine Journal 27(3): 533-537.
- Edler A, Murray DJ & Forbes RB (2003) Blood loss during posterior spinal fusion surgery in patients with neuromuscular disease: is there an increased risk? Paediatr Anaesth 13(9): 818–822.
- Hassan N, Halanski M, Wincek J, Reischman D & Sanfilippo D, et al. (2011) Blood management in pediatric spinal deformity surgery: review of a 2-year experience. Transfusion 51(10): 2133-2141.
- Hawes M (2006) Impact of spine surgery on signs and symptoms of spinal deformity. Pediatr Rehabil 9(4): 318-339.
- Goldberg CJ, Moore DP, Fogarty EE & Dowling FE (2001) Adolescent idiopathic scoliosis: the effect of brace treatment on the incidence of surgery 26(1): 42-47.
- Carreon LY, Puno RM, Lenke LG, Richards BS & Sucato DJ (2007) Non-neurologic complications following surgery for adolescent idiopathic scoliosis. J Bone Joint Surg Am 89(11): 2427–2432.






























