Cutaneous Coverage of the Fingers of the Hand in Severe Injuries
Lazaro Martin Martinez Estupinan1, Leonardo Martinez Aparicio2, Lazaro Martinez Aparicio3, Carlos Osvaldo Arias Calero4, Ana Elena Martinez Suarez5 and Claribel Plain Pazos6
1Doctor in Medical Sciences, II Degree Specialist in Orthopedics and Traumatology, Full Professor, Provincial General University Hospital, Cuba
2Resident of 4th year of Orthopedics and Traumatology, Provincial General University Hospital, Cuba
3I Degree Specialist in Orthopedics and Traumatology, Instructor Professor, Provincial General University Hospital, Cuba
4Resident of 3rd year of Orthopedics and Traumatology, Provincial General University Hospital, Cuba
5Resident of 4th year of Surgery, Provincial General University Hospital “Arnaldo Milian Castro, Cuba
6Iand II Degree Specialist in Comprehensive General Medicine, Faculty of Medical Sciences of Sagua la Grande, Cuba
Submission:December 06, 2022; Published: January 11, 2023
*Corresponding author: Claribel Plain Pazos, Faculty of Medical Sciences of Sagua la Grande, Villa Clara, Cuba
How to cite this article: Lazaro Martin M E, Leonardo Martinez A, Lazaro Martinez A, Carlos Osvaldo Arias C, Ana Elena M S, et al. Cutaneous Coverage of the Fingers of the Hand in Severe Injuries. Ortho & Rheum Open Access J. 2023; 21(1): 556052. DOI: 10.19080/OROAJ.2023.21.556052
Abstract
Introduction: The distal end of the fingers presents a complex anatomy and a fundamental sensory function, the coverage of the skin defects of the fingers of the hand represents a challenge from the anatomical and functional point of view.
Method: A descriptive, non-experimental, longitudinal and prospective study was carried out. The universe of study is made up of 24 patients with distal amputations in 35 fingers. The Allen topographic classification is used for their treatment.
Results: The lesions are more frequent in the non-dominant hand, with an occupational etiology, much more frequent in Allen zone 1, treated with the Atasoy and Kutler flap, with excellent or good results in most of the treated cases.
Conclusion: Distal lesions of the fingers treated by skin coverage surgery evolve favorably.
Keywords: Skin coverage; Finger injury; Atasoy flap
Introduction
The hand is one of the main contributions of ontogeny to the human species, its injuries affect the relationship life, the work life and the psyche of a person. Traumatic injuries frequently affect the fingers and there are multiple medical and/or surgical solutions for this. The repair and coverage of traumatic injuries of the upper limbs with the use of flaps is important to rescue the compromised structures and they can recover the previous functional capacity to be abre to carry out their activities; In addition, the choice of the reconstruction modality must take into account several components, including the origin of the defect and location, level of contamination, availability of donor tissue, and the experience of the surgeon [1].
In the treatment of the loss of skin coverage of the hand, various techniques are used, from directed healing to free flaps, through skin grafts and other local, regional and distant flaps. The coverage strategy depends on several criteria, including the topography of the defect, the affected finger or part of the hand, associated injuries,postoperative rehabilitation needs, the functional requirement, the patient’s work activity and their age all influence the decision. Two All coverage techniques, from simple targeted healing, through skin grafting with or without the use of dermal substitutes, to local or distant flaps, must be known in order to offer the patient the most adapted and appropriate solution. The objective of this work is to delve into the results of skin coverage treatment of distal lesions of the fingers of the hand in our service.
Method
A descriptive, non-experimental, longitudinal and prospective study was carried out from January 2011 to December 2021 at the University General Hospital Sagua la Grande, in cuba. The universe of study is made up of 24 patients with distal amputations in 35 fingers in zones 1, 2, 3 and 4 according to the Allen topographic classification. Theoretical and empirical statistical methods of scientific research were used. In the operative procedure, under pedicular regional anesthesia and after taking the preoperative measures, washing with antiseptic solutions, debridement and adequate hemostasis were performed. Finally, the traumatic defect was resolved using local flaps of the Atasoy or Kutler type, full-thickness grafts, after techniques, or left to heal by secondary intention. For all cases, three-zero monofilament nylon suture with atraumatic needle was used. Tetanus prophylaxis and oral or parental antibiotics were performed depending on the type of injury. The choice of flap to be used was made based on the following parameters: age, professional activity, topography of the defect, finger involved, dominant pad, dominant hand, and level of amputation. The evaluation of the results was made according to a scale of excellent, good, fair or bad, taking into account: scar condition, bone deformity, nail deformity and sensitivity.
Results
In the series of serious injuries, the fingers of the hand, treated with skin coverage, predominate in the non-dominant limb (n=17), in adults between 59 and 78 years where it is more common (Table 1). Table 2 shows how injuries predominate in male patients (n=15), mostly due to occupational injuries, represented by 58.34%. Table 3 shows the distribution of the surgical technique according to the type of lesion according to the Allen classification. The Atasoy or Kutler technique was used (Figure 1) mainly for conditions in zone 1, where the greatest number of affected fingers, followed by lesions in zone 2, unlike lesions that damage zone 3 and 4 where it is not possible to use this type of skin coverage and other techniques or healing by secondary intention are used.
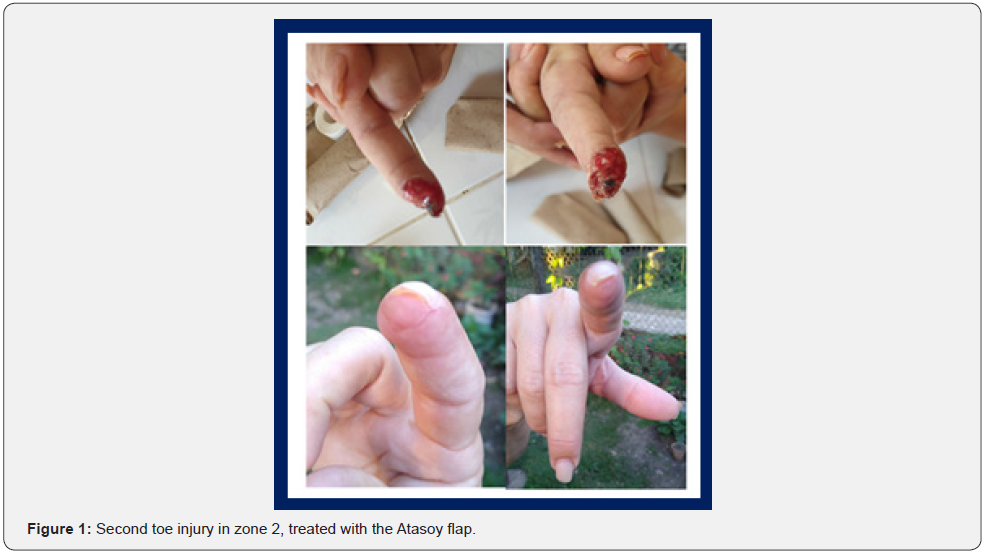
Font. Database.
Font. Database.
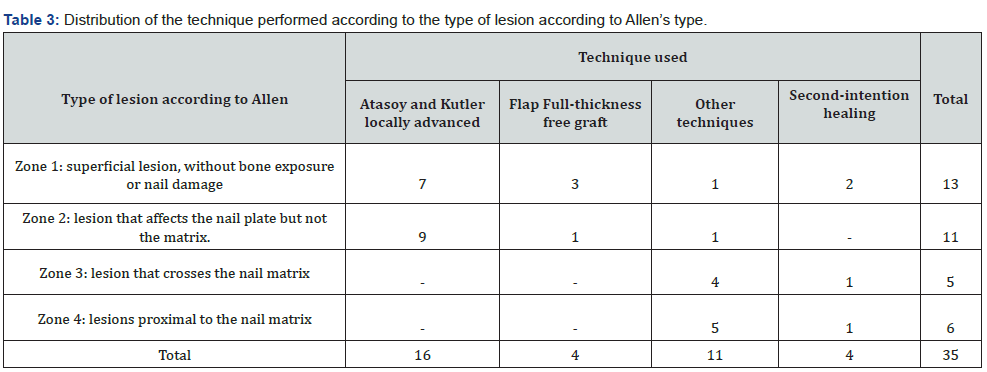
Font. Database.
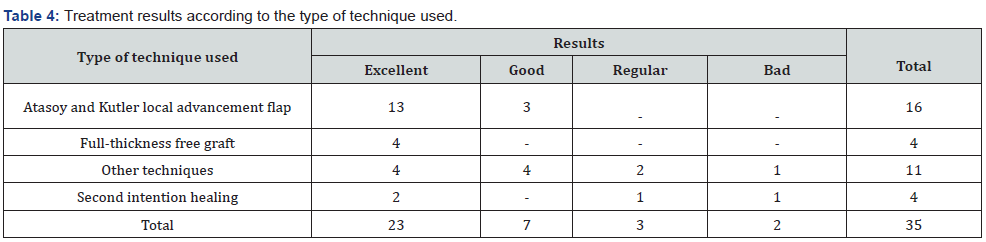
Font. Database.
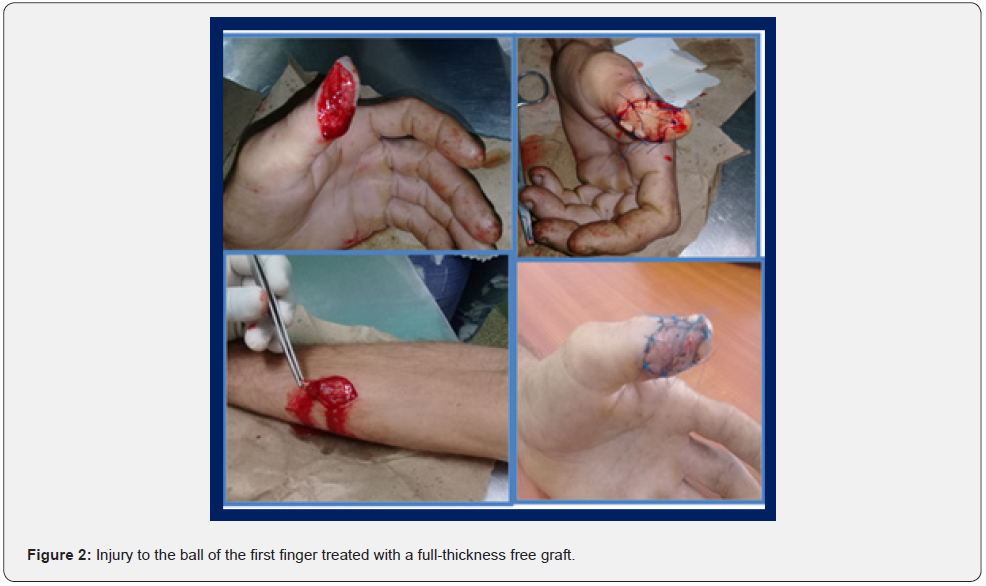
Figure 2 shows the usefulness of the free flap for skin coverage of severe lesions of the external portion of the first finger.
The reason for the particular choice of these types of flaps or coverage was given by a preference of the surgeon, motivated by the observation of efficacy, by the familiarity and skill acquired in performing this type of surgery. Table 4 shows how the results are according to the technique used and in it we see how the majority were excellent or good, mainly where the Atasoy O Kutler technique is used. Only five fingers were evaluated with regular or poor results.
Discussion
The loss of skin coverage and substance distal to the distal interphalangeal joint represents a large part of the surgical emergencies of the hand (30-40%), which is why its aesthetic and functional repercussion is important [3]. The distal end of the fingers has a complex anatomy and essential sensory function. The nail plate is a hard tissue whose function is to protect the back of the finger and aid in sensitivity, as well as allowing better function. The nail bed is a supportive structure attached to the nail and underlying bone that abuts the nail germinal junction. The arrangement of the vessels and nerves at the tips of the fingers requires that their re-implantation, their suturing or their skin coverage be carried out using a very careful technique.
There are several classifications that describe the distal digital amputation; that of Allen and Fassler are the most cited in the studies. Allen takes into account the involvement of the pulp, nail, lunula and distal phalanx dividing it into 4 types [4]
- Zone 1: superficial lesion, without bone exposure or nail damage.
- Zone 2: lesion that affects the nail plate but not the matrix.
- Zone 3: lesion that crosses the nail matrix.
- Zone 4: lesions proximal to the nail matrix.
It is important to know the three elements that must be preserved for the correct function of the pulp: bone integrity, nail integrity, and good condition of the surrounding cellularfat tissue. The coverage of skin defects of the hand represents a challenge from the anatomical and functional point of view; the true reconstruction of this begins with surgical procedures that provide adequate skin and soft tissue coverage.
Distal digital injuries have fostered a great debate regarding their treatment, which can be: surgical or conservative [5]. In short, treatment is always aimed at covering the exposed tissues and epithelializing the pad of the affected finger. For many decades, evidence has existed that secondary scarring can be beneficial and achieves favorable outcomes; however, for different reasons it has lagged behind the surgical option. Multiple protocols and surgical techniques have been designed for coverage of the traumatic hand [6,7].
Multiple treatments have been described for these injuries depending on the type of trauma and the elements involved; They range from coverage flaps, cross finger flaps to treatment by secondary closure. Cayon F et al. use occlusive wet dressing treatment for lesions in the distal region of the fingertips, perform emergency treatment with initial lavage, surgical cleaning, placing solid Vaseline on the lesions and applying an occlusive dressing to keep the injury site isolated from the environment, every week and twice they perform dressings until complete closure of the initial injury, which was observed four weeks later; It was evidenced that the coverage and functionality of the skin were adequate in the treated finger [8].
Healing treatment by second intention is currently a point of controversy in fingertip injuries. The recovery is established in an average time of 20 days. The return time to work activities is estimated at approximately 1 week; except,when it comes to food handling. The appearance of the amputated finger has not prevented this technique from being used; most patients express their agreement with the final result of conservative treatment. The main residual consequence of healing by secondary intention is the deformation of the nail (hook or parrot beak), especially in proximal lesions that lose the bone support that the distal phalanx provides to the nail bed [9].
The non-predominant hand had a percentage of involvement of 68.43% in relation to the predominant hand. According to Blanco Placencia and Pereda Cardoso in their series, [10] zone 3 injuries occurred in 38.15% of the treated fingers and these are the most serious because at this level the stability of the distal fingertip is in danger due to injury to the nail matrix and shortening of bone structure due to injury to the phalangeal tuberosity. However, they mostly use the Atasoy flap (46.05%) and the Kutler flap (34.21%), the reason for the particular choice of these types of flaps was given by a personal preference motivated by the observation of the efficacy of them and for the familiarization and skill acquired in performing this type of flaps.
For Rodríguez Alvarado and collaborators, the mechanism of injury in the patients who participated in the study had a marked distribution, so much so that 70% corresponded to injuries of cutting origin, in relation to 17% of crush injuries and 13% of injuries, attrition injuries [11]. The main post-treatment symptoms of distal toe amputations are intolerance to cold, decreased discriminative sensitivity, and deformities that are unsatisfying in appearance. Heberprot P therapy is emerging as one of the most promising techniques in the future medical arsenal for the repair of damaged or destroyed tissue. In the last decade in Cuba a true regenerative revolution has taken place where Heberprot P is one of them, it provides repairing and regenerative properties of damaged tissues [12].
References
- Foucher G, Daliaserra M, Tilquin B, Sammut ED (1994) The Hueston Flap in Reconstruction of Fingertip Skin Loss: Results in a series of 41 Patients. Thejournal of handsurgery 19(3): 508-515.
- Athlani L, Dautel G (2021) Cobertura cutánea de la mano y de los dedos. EMC - Cirugia Plastica Reparadora y Estetica 29(1): 1-23.
- Gunter G, Klaus DR, Scott L, Manuel H (2017) Fingertip and thumb tip wound: Changing Algorithms for Sensation, Aesthetic and Function. J Hand Surg Am 42(4): 274-284.
- Hoigne D, Hug U, Schurch M, Meoli M, von Wartburg U (2013) Semi-occlusive dressing for the treatment of fingertip amputations with exposed bone: quantity and quality of soft-tissue regeneration. J Hand Surg Eur Vol 39(5): 505-509.
- Sindhu K, DeFroda SF, Harris AP, Gil JA (2017) Management of partial fingertip amputation in adults: Operative and non operative treatment. Injury 48(12): 2643-2649.
- Sebastian N, Rodriguez JC (2018) Design of radial flaps for reconstruction of defects of the hand and study of the perforators that compose them. Cir Plast Iberolatinoam 44(3): 319-328.
- Apa SN, Rodriguez JC (2020) Design of radial flaps for reconstruction of defects of the hand and study of the perforators that compose them. Cir plast iberolatinoam 44(3): 319-328.
- Cayon F, Alegria G, Pacheco J, Carrillo, Larco E, et al. (2020) Secondary healing in distal digital amputation. Case report and bibliographic review. Revista Metro Ciencia 28(1).
- Panattoni JB, De Ona IR, Ahmed MM (2015) Reconstruction of fingertip injuries: Surgical tips and avoiding complications. J Hand Surg Am 40(5): 1016-1024.
- Blanco Placencia H, Pereda Cardoso O (2000) Local flaps in the emergency treatment of distal amputations of the fingers. Rev Cubana Ortop Traumatol 14(1-2): 41-45.
- Rodriguez Alvarado ND, Vargas Diaz RE (2014) Montenegro Mayorga SE, Dajaro Castro LA. Comparative study of surgical techniques for the repair of fingertip defects. Revista de la Facultad de Ciencias Medicas de Guayaquil 17(2).
- Gutierrez Lopez A, Gomez Aguila TM, Choy Fernandez E (2020) Heberprot P in severe hand injury and bipedicle graft to the abdomen. Case presentation. Gac Med Espirit 22(3): 111-118.






























