An overview of Floating Knee Injuries, Management Approach
Mohammed Saad Alghamdi1, Ali M Alhaddad2, Sulaiman Mohammed Hushlul3, Faisal Omar Alrefaei4 and Mohammed Mubark Haqash4*
1Degree of Bachelor of Medicine MBBS, KAU, Master of Business Administration, MBA, MBSC, PGY5 Resident in Saudi orthopedic program, Saudi Arabia
2Degree of Bachelor of Medicine, NUI, Bachelor of Surgery, Bachelor of Obstetrics MB, BCh, BAO (NUI, RCSI)
saudi arabia board of orthopedic surgery, Saudi Arabia
3Degree of Bachelor of Medicine MBBS , UQU, PGY4 Resident in Saudi orthopedic program, Saudi Arabia
4Degree of Bachelor of Medicine MBBS, UQU, saudi arabia board of orthopedic surgery, Saudi Arabia
Submission:December 20, 2022; Published: January 04, 2023
*Corresponding author: Sulaiman Mohammed Hushlul, Degree of Bachelor of Medicine MBBS , UQU, PGY4 Resident in Saudi orthopedic program, Saudi Arabia
How to cite this article: Mohammed S A, Ali M A, Sulaiman M H, Faisal O A, Mohammed M H. An overview of Floating Knee Injuries, Management Approach. Ortho & Rheum Open Access J. 2023; 21(1): 556051. DOI: 10.19080/OROAJ.2023.21.556051
Abstract
Floating knee injuries are frequently associated with other serious injuries. Our study intends to evaluate the management and treatment of floating knee, as well as associated injuries, treatment techniques, treatment outcomes, and consequences. Electronic search performed on the most widely used biomedical databases, such as Medline. Floating knee with ipsilateral femoral and tibial fracture is a severe injury that is frequently associated with high-energy trauma and a variety of associated injuries that are frequently quite serious, as well as systemic and local effects. When planning treatment, it is critical to consider both the patient’s overall condition and the condition of the limbs. At times, amputation is a viable alternative. It is critical to evaluate injuries and complications before deciding on a surgical procedure. These injuries require the management of a multidisciplinary team with experience.
Introduction
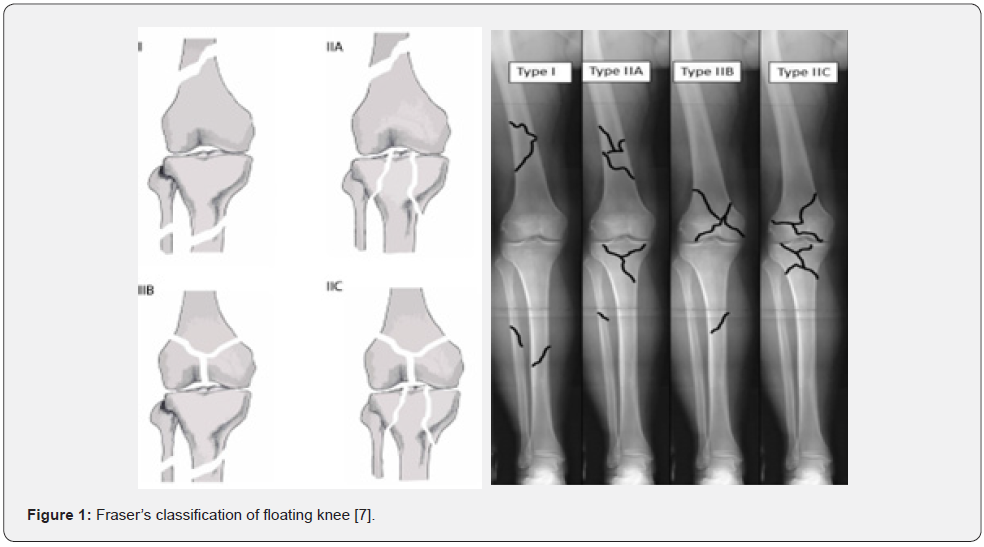
The term “floating knee” may be used to describe fractures of the ipsilateral tibia and femur. These fractures may involve the diaphysis or metaphysis, with the result that the knee becomes “separated” from the remainder of the leg. Although the etiology of this disease is unknown, it is normally uncommon, although it has increased in recent years at the same rate as the number of polytrauma patients affected by high-energy damage. Typically resulting from such an event, floating knee is typically reported by patients who have also sustained major injuries to their upper body, head, abdominal region, arm, or leg [1]. Other complications associated with floating knee injuries include infection, excessive blood loss, embolism, malunion, delayed or nonunion, knee tightness, long-term hospitalization, and inability to bear weight [2]. Vascular injuries are far more frequently related with this type of injury when the fractures occur independently, which occurs in roughly 29 % according to certain research studies [3]. Several other authors believe that these concerns are significantly less common [4]. According to some studies, open floating knees are seen in between 60% and 80% of cases [5]. Additionally, it has been linked to neurological damage and embolism. Blake and McBryde developed the ‘floating knee’ principle in 1975 to explain ipsilateral femur and tibia fractures [6]. While road traffic accidents (RTA) are the primary cause, falls from height (FFH) also account for a significant number of incidents. According to Fraser [7], the FK manifests itself in a variety of ways, according to the involvement of the knee: bi-diaphysis fractures (type I), combined diaphysis and epiphyseal fractures on the same bone (type II A, B), and reciprocal epiphyseal fractures (IIC).
Complications such as compartment syndrome, loss of knee mobility, failure to detect knee ligamentous injury, and the need for amputation do not appear to be uncommon. When both fractures are diaphyseal in nature, as opposed to when one or both are intra-articular, significantly better outcomes and fewer complications are observed [8]. Typically, floating knee injuries occur in conjunction with a variety of other significant injuries. Do these injuries have an effect on how the floating knee is managed and on the final outcome of patients? Our research study will examine the consequences of associated injuries on the management and final outcome of floating knee. Age, sex, mechanism of injury, associated injuries, technique of different treatment approaches, and complications of floating knee are all discussed in this study.
Discussion
Classification
In 1978, Fraser [7] Categorized the floating knee according to the fracture location and the knee involvement (Figure 1). Type 1, fractures in the shafts of the femur and tibia without extension to the knee. Type II, fractures involving the knee, and was further subdivided into: Type II a) (8%) Femur shaft fracture with a tibia plateau fracture. Type II b) (12%) distal intra-articular femur fracture with tibial shaft fracture. Type II c) (9%) distal intraarticular femur fracture with tibia plateau fracture [9].
Preoperative Evaluation and Initial Management
Polytrauma is a common occurrence in patients with floating knees, and involvement of various other body organs is highly speculative. Orthopedic surgeons typically recommend a variety of treatment regimens for floating knee injuries, including very early and aggressive stabilization of both femoral and tibial fractures regardless of the treatment approach [10]. According to some authors, the difficulty rate and death rate remain high regardless of the therapy program used [11].
Generally, the injury is a result of a high-energy impact such as biking injuries, pedestrian , collisions between automobiles. Extremely associated injuries have an average Injury Severity Score (ISS) of greater than 16 [9], with serious head injuries occurring in 14% [13], as well as breast and stomach sores in addition to those of the influenced arm or leg, such as extreme associated soft tissues [14]. Injuries of the popliteal artery affect 7% of cases, and a minimum of the tibia or femur fracture is open in 69% of cases [9]. In 44 percent of patients, involved fractures are discovered. The fatality rate following admission may reach 10% [15]. Lesions of the popliteal artery and/or severely mangled arms or legs, as well as open fractures, may result in amputation in 9% of patients within the first 24 hours of admission. Joint and knee ligament injuries are common, with a laxity of up to 19% [16]. Additionally, fat embolism and compartment syndromes are common [9,17].
For polytrauma patients with hip or long bone fractures, determining the extent of soft tissue injury and the presence of vascular injury or compartment syndrome is critical early in the course of treatment because these complications necessitate immediate treatment, and the outcome will be directly influenced by whether or not treatment is delayed [18]. When examining polytrauma patients, the standard approach is to consider their hemodynamic stability. The term “triad of death” was coined to describe the decompensation caused by acute blood loss, which results in coagulopathy, hypothermia, and acidosis. Avoiding or reversing these elements may prevent fatal exsanguination. Recent research has emphasized the effect of orthopedic injuries on this trio [19].
The optimal time to treat a fracture is contingent upon proper resuscitation. Parameters that are frequently used to assess the resuscitation include urine output, pulse rate, blood pressure as well as lactate and base deficit. Ideally, all of these criteria should be normalized prior to pursuing fracture fixation. It is critical to reverse any type of coagulopathy and to stabilize the core body temperature [18,19]. Patients are classified into four groups throughout the resuscitation stage based on their ability to recover, these criteria are: stable, borderline, unpredictable, and in extremis.
When considering the medical therapy that should be applied to orthopedic injuries, a variety of top priorities must be considered. Prior to any procedure, it is important to preserve the patient’s life and any viable extremity and to keep the operating room time to less than two hours [19,20]. Open fractures must be debrided and stabilized with an external fixator within this critical window. For a fracture on the upper extremities, a splint may suffice. A preliminary amputation may be necessary to save the life of a patient who is in extremis due to an extremity fracture or an open fracture with vascular injury. Certain standards cannot be suggested for every circumstance, as each situation involves a variety of variables.
External fixation as a first step avoids the need for additional lengthy treatments that may exacerbate the “triad of death”. In this regard, treatments lasting longer than six hours are particularly harmful, as they are associated with an increased risk of acute respiratory distress syndrome and the failure of several body organs. Some elements directly related to the job of orthopedic surgeons are associated with negative outcomes; these include several long bone fractures, pelvic injury in the presence of hemorrhagic shock, medical time exceeding 6 hours, and lung artery pressures greater than 6 mm/Hg during intramedullary nailing, which is a measure of significant lung damage [21].
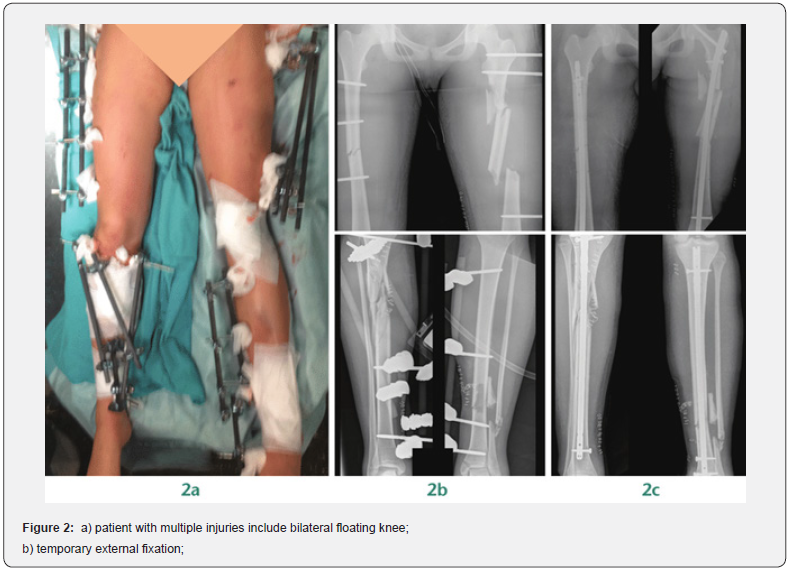
Injuries (head, upper body, or other fractures, as well as vascular injuries) influence medical decision-making regarding the timing and sequence of surgical treatment (Figure 2). It is critical to recognize the injuries associated with floating knee since it may be life threatening. It is necessary to determine the impact on the extremities systems (soft tissue, nerves, vascular, and bone). When they are seriously influenced, the surgeon must choose between preliminary amputation and salvage. The MESS (Mangled Extremity Severity Score) scale takes into account the following factors: (1) skeletal and soft-tissue injuries; (2) limb ischemia; (3) shock; and (4) the age of the patient [22]. This approach has been shown to aid in the clinical management of lesions of this type (Table 1).
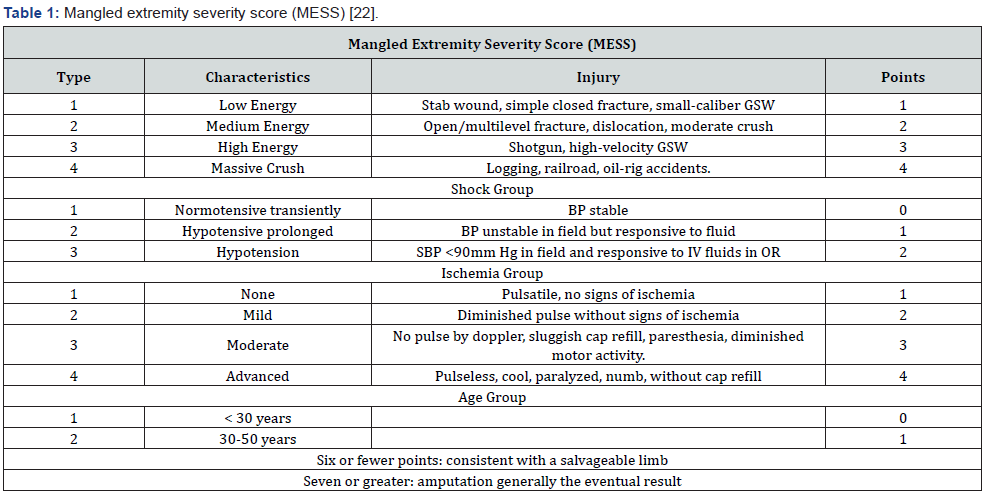
GSW: gunshot wound, BP: blood pressure. SBP: Systolic blood pressure. IV: intravenous. OR: Operation room.
There have been other different evaluation methodologies suggested, but none has been definitively authorized in the decision-making process when it comes to limb or leg salvage versus amputation in the management of patients with severe arm or leg injuries. As a result, further research is needed to better understand the factors that could help decision-making and reduce the frequency of unsuccessful recovery efforts. Recent medical advancements have increased the capability to reconstruct severely wounded arm or legs, to the point where arm or legs that would have been amputated years ago are now routinely handled and recovered. In addition to bone stabilization and debridement of open fractures as well as the utilization of antibiotic and the antibiotic beads [23,24], damage control therapy for floating knee includes the treatment of associated soft tissue injury such as vascular injury or compartment syndrome, where the corresponding fasciotomy should be performed.
Treatment
Typically, a floating knee is treated by nailing both the femur and the tibia . This technique prompted several problems, consisting of fat embolism, pulmonary embolism [25]. Akinyoola et al. reported patients whose treatment was postponed, as well as those who were not treated operatively, faced significantly more difficulties [26].
Orthopedic stabilization of both bones, tailored for each patient and fracture morphology [27] is the most widely accepted conclusive therapy today. The instructions and location of each fracture, the soft tissue condition, the resources available, and the medical condition of the patient, all play a role in determining the most appropriate treatment. The surgical plan is to perform an anterograde femoral nailing first, followed by anterograde tibial nailing. A different procedure has been considered, in which both bones are fixed using a single median parapatellar approach and single incision, utilizing a retrograde femoral nail and also a tibial anterograde nail [28]. Rios et al. researched 43 patients with floating knee injuries were divided into two groups: a treatment group of 25 patients who received retrograde femoral nailing as well as anterograde tibial nailing through a single incision, and a control group of 18 patients who received standard intramedullary anterograde nailing for both the femur and tibia. According to the results, the femoral retrograde technique requires far less preparatory work, anesthetic, and surgical procedure time than the usual anterograde femoral technique; it also results in significantly less blood loss. The single incision procedure, according to these authors, is a safe and also quick treatment that can be used as an alternative therapy for type I floating knee [29].
The femur is initially nailed, and the tibia is temporarily secured with a splint or, in situations of severe comminution, an external fixator. If the tibia was secured first, the femur’s activity and contortion during surgery would cause more harm to the soft tissues and also provide a greater risk to the patient’s general condition, including a larger risk of fat embolism [27,30]. If shortterm fixation is required, fixators that function with MRI scanning are recommended. After temporary stabilization, an MRI of the knee is recommended, preferably if a tendon injury is suspected [31]. A medical assessment of the ligamentous stability of the knee must be performed under anesthesia following the last fixation.
The vascular injury of fractures around the knee, primarily of the popliteal artery, is an injury that occurs in around 29% of floating knees, with amputation occurring in up to 21% of cases [32]. An evaluation of the peripheral pulses by physical examination, and obtaining an ankle brachial pressure index, utilizing the Doppler ultrasonography exam, as well as the careful use of angiography, should be included in a neurovascular evaluation of polytrauma patients. Although vascular injury may be overlooked during the initial physical examination, it might occur during the first 24 hours due to the progression of arterial thrombosis. After the short-term fixation of unpredictable fractures, vascular repairing surgical procedures should be performed as soon as possible [33].
Complications
Treatment for floating knee has inconsistent results, with a high prevalence of complications. Systemic injuries, such as a pulmonary embolism, fat embolism, kidney failure, or lesions in the head, chest, or stomach, as well as the consequences of other injuries, are among the most common. Regional effects may include pain, ligamentous laxity, decreased articular flexibility, delayed union or nonunion, osteomyelitis, or even amputation of the arm or leg [34]. Type II floating knee is associated with a more severe diagnosis, more open injuries, and a higher amount of systemic harm [35]. Kao et al. discovered that floating knee injuries have been linked to a high likelihood of complications and death, regardless of the treatment regimen used. These issues are linked to age (more common in patients aged 60-89 years), injury type (greater in-kind II floating knee, according to the Fraser classification), and location (higher in the tibial plateau, distal tibia, and open fractures) [36].
Conclusion
Floating knee with ipsilateral femoral and tibial fracture is a serious injury that is usually caused by a high-energy injury and a slew of other injuries, many of which are also quite serious, as well as systemic and local consequences. It is critical to consider the patient’s overall problem as well as the condition of the limbs while arranging therapy. Amputation can be a good alternative in some cases. Before settling on a surgical approach, it’s critical to evaluate injuries and complications. That is, severe injuries must be managed by a multidisciplinary team with extensive knowledge.
References
- Rethnam U, Yesupalan R S, Nair R (2007) The floating knee: epidemiology, prognostic indicators & outcome following surgical management. J Trauma Manag. Outcomes 1(1): 2.
- Elmrini A, Elibrahimi A, Agoumi O, Boutayeb F, Mahfoud M, et al. (2006) Ipsilateral fractures of tibia and femur or floating knee. Int Orthop 30: 325-328.
- Paul GR, Sawka MW, Whitelaw GP (1990) Fractures of the ipsilateral femur and tibia: emphasis on intra-articular and soft tissue injury. J Orthop Trauma 4(3): 309–314.
- Kao FC, Tu Y K, Hsu KY, Su JY, Yen CY, et al. (2010) Floating knee injuries: a high complication rate. Orthopedics 33(1): 14.
- Kumar R (2011) The floating knee injury. J Clin Orthop Trauma 2(2): 69-76.
- Blake R, McBryde A Jr (1975) The floating knee: ipsilateral fractures of the tibia and femur. South Med J 68(1): 13-16.
- Fraser RD, Hunter GA, Waddell JP (1978) Ipsilateral fracture of the femur and tibia. J. Bone Joint Surg. Br 60-B(4): 510–515.
- Lundy DW, Johnson KD (2001) "Floating knee" injuries: ipsilateral fractures of the femur and tibia. J Am Acad Orthop Surg 9(4): 238-245.
- Pietu G, Jacquot F, Feron J-M, et les membres du GETRAUM (2007) Le genou flottant: étude rétrospective de 172 cas. [The floating knee: a retrospective analysis of 172 cases. Revue de Chirurgie Orthopédique 93(6): 627-634.
- Veith RG, Winquist RA, Hansen ST Jr (1984) Ipsilateral fractures of the femur and tibia. A report of fifty-seven consecutive cases. J Bone Joint Surg Am 66(7): 991-1002.
- Ostrum RF (2000) Treatment of floating knee injuries through a single percutaneous approach. Clin Orthop Relat Res (375): 43-50.
- Karlstrom G, Olerud S (1977) Ipsilateral fracture of the femur and tibia. J Bone Joint Surg Am 59(2): 240-243.
- van Raay JJ, Raaymakers EL, Dupree HW (1991) Knee ligament injuries combined with ipsilateral tibial and femoral diaphyseal fractures: the “floating knee”. Arch Orthop Trauma Surg 110(2): 75-77.
- Paul GR, Sawka MW, Whitelaw GP (1990) Fractures of the ipsilateral femur and tibia: emphasis on intra-articular and soft tissue injury. J Orthop Trauma 4(3): 309-314.
- Dwyer AJ, Paul R, Mam MK, Kumar A, Gosselin RA (2005) Floating knee injuries: long-term results of four treatment methods. Int Orthop 29(5): 314-318.
- Paul GR, Sawka MW, Whitelaw GP (1990) Fractures of the ipsilateral femur and tibia: emphasis on intra-articular and soft tissue injury. J Orthop Trauma 4: 309-314.
- Adamson GJ, Wiss DA, Lowery GL, Peters CL (1992) Type II floating knee: ipsilateral femoral and tibial fractures with intraarticular extension into the knee joint. J Orthop Trauma 6(3): 333-339.
- Crist BD, Ferguson T, Murtha YM, Lee MA (2013) Surgical timing of treating injured extremities: an evolving concept of urgency. Instr. Course Lect 62: 17-28.
- Pape HC, Giannoudis PV, Krettek C, Trentz O (2005) Timing of fixation of major fractures in blunt polytrauma: role of conventional indicators in clinical decision making. J Orthop Trauma 19(8): 551–562.
- Shafi S, Elliott AC, Gentilello L (2005) Is hypothermia simply a marker of shock and injury severity or an independent risk factor for mortality in trauma patients? Analysis of a large national trauma registry. J Trauma 59(5): 1081–1085.
- Fulkerson EW, Egol K A (2009) Timing issues in fracture management: a review of current concepts. Bull. NYU Hosp Jt Dis 67(1): 58–67.
- Helfet DL, Howey T, Sanders R, Johansen K (1990) Limb salvage versus amputation. Preliminary results of the Mangled Extremity Severity Score. Clin Orthop Relat Res 256: 80–86.
- Putnis S, Khan WS, Wong J M (2014) Negative pressure wound therapy - a review of its uses in orthopaedic trauma. Open Orthop J 8: 142–147.
- Decoster T.A., Bozorgnia S. Antibiotic beads. J Am Acad Orthop Surg 2008;16(11): 674–678.
- Veith RG, Winquist RA, Hansen ST Jr (1984) Ipsilateral fractures of the femur and tibia. A report of fifty-seven consecutive cases. J. Bone Joint Surg Am 66(7): 991–1002.
- Akinyoola AL, Yusuf M B, Orekha O Challenges in the management of floating knee injuries in a resource constrained setting. Musculoskelet. Surg 97(1): 45–49.
- Lundy DW, Johnson KD (2001) “Floating knee” injuries: ipsilateral fractures of the femur and tibia. J Am Acad Orthop Surg 9(4): 238–245.
- Gregory P, DiCicco J, Karpik K, DiPasquale T, Herscovici D, et al. (1996) Ipsilateral fractures of the femur and tibia: treatment with retrograde femoral nailing and unreamed tibial nailing. J Orthop Trauma 10(5): 309–316.
- Rios JA, Ho-Fung V, Ramirez N, Hernandez RA (2004) Floating knee injuries treated with single-incision technique versus traditional antegrade femur fixation: a comparative study. Am J Orthop 33(9): 468–472.
- Ostrum RF, Tornetta P III, Watson JT, Christiano A, Vafek E (2014) Ipsilateral proximal femur and shaft fractures treated with hip screws and a reamed retrograde intramedullary nail. Clin Orthop Relat Res 472(9): 2751–2758.
- Levy BA, Dajani KA, Whelan DB, Stannard JP, Fanelli GC, et al. (2009) Decision making in the multiligament-injured knee: an evidence-based systematic review. Arthroscopy 25(4): 430-438.
- Perron AD, Brady WJ, Sing RF (2001) Orthopedic pitfalls in the ED: vascular injury associated with knee dislocation. Am J Emerg Med 19(7): 583-588.
- Medina O, Arom GA, Yeranosian MG, Petrigliano FA, McAllister DR (2014) Vascular and nerve injury after knee dislocation: a systematic review. Clin Orthop Relat Res 472(9): 2621–2629.
- Kumar R (2011) The floating knee injury. J Clin Orthop Trauma 2(2): 69-76.
- Kao FC, Tu YK, Hsu KY, Su JY, Yen CY, et al. (2010) Floating knee injuries: a high complication rate. Orthopedics 33(1): 14.
- Adamson GJ, Wiss DA, Lowery GL, Peters CL (1992) Type II floating knee: ipsilateral femoral and tibial fractures with intraarticular extension into the knee joint. J Orthop Trauma 6(3): 333–339.






























