Limb Liposarcoma: Aspects of Diagnostic and Therapeutic Management and Main Prognostic Factors
Oussama Eladaoui*, Mohamed Laffani, Omar Fadili, Abdellah Chrak, Ahmed Reda Haddoun and Mustapha Fadili
Department of Traumatology and Orthopedics (A4) of the Ibn Rochd University Hospital Center of Casablanca, Hassan 2 University of Casablanca, Morocco
Submission:October 06, 2022; Published: October 13, 2022
*Corresponding author: Oussama Eladaoui, Department of Traumatology and Orthopedics (A4) of the Ibn Rochd University Hospital Center of Casablanca, Hassan 2 University of Casablanca, Morocco
How to cite this article: Oussama E, Mohamed L, Omar F, Abdellah C, Ahmed R H, et al. Limb Liposarcoma: Aspects of Diagnostic and Therapeutic Management and Main Prognostic Factors. Ortho & Rheum Open Access J. 2022; 20(4): 556042. DOI: 10.19080/OROAJ.2022.20.556042
Abstract
The liposarcoma of the soft tissue are rare malignant tumors originating from primitive mesenchymal cells. They show a wide variation in histologic, clinical and prognostic features. To evaluate the different aspects of diagnostic and therapeutic management and main prognostic factors of limbs liposarcome, we retrospectively reviewed 20 patients histologically diagnosed with this type of tumor treated in Department of Traumatology and Orthopedics (A4) of the Ibn Rochd University Hospital Center of Casablanca between 2016 and 2022.
The mean age is 50 years old. A masculine predominance has been noticed. The tumefaction of the soft tissue is the main revealing sign with predominance of the lesions localized preferentially in the lower extremity. The thigh is the predilection seat of these tumors. Myxoid liposarcoma is the most frequent histologic sub-types followed by the pleomorphic liposarcoma and well differentiated. The standard radiographics have been practiced in all patients, the echography in ten. The computerized tomography has been practiced in one case. the imaging by magnetic resonance has been realized in all patients. For our patients, the treatment is primarily surgical, consisting in a large excision for majority. Most cases had complete excision margins and were referred for additional radiotherapy. Among the 20 patients in our series, most patients presented a good clinical evolution.
Introduction
Liposarcoma is a malignant soft tissue tumor of mesenchymal origin developed from lipoblast cells at different stages of their differentiation. They represent the most common histological type of soft tissue sarcomas in adults; however, they remain rare tumors [1]. The clinical presentation and the symptoms are not specific. A complete radiological examination is in all cases essential. However, only anatomopathological examination, brings the diagnosis of certainty [2]. The mainstay of treatment remains oncological surgery, which must be wide and deep, usually supplemented by radiotherapy to reduce the risk of recurrence, and possibly by chemotherapy for high-grade tumors with high metastatic potential. The prognosis is variable and depends on several factors.
Our work is devoted to the study of 20 cases of liposarcoma of the limbs, which presented, treated and followed up at the traumatology-orthopedics department at the University Hospital Centre Ibn Rochd of Casablanca. Through this work and a review of the literature, we want to shed light on:
i. The epidemiological profile of liposarcomas.
ii. The clinical, paraclinical and anatomopathologic aspects.
iii. Therapeutic management.
iv. The evolution and the main prognostic factors.
Materials and Methods
The clinical records of our department with the diagnosis of limp soft tissue sarcoma between the 2016 and 2022 were retrospectively reviewed and 20 patients were identified with liposarcoma of the limbs. Age, gender, symptoms, location of the tumor, histopathological diagnosis, treatment modality and disease status were re-examined. The patients with incomplete clinical, radiographic, and pathologic records were excluded.
Results
Patient characteristics
Of the 20 cases studied, the age of the patients at the time of diagnosis varied between 20 and 72 years with an average age of 50 years and a peak frequency concerning the age group over 60 years. There is a predominance of the male sex (11 men compared to 9 women) with a sex ratio =1,22.
Tumor location
Analysis of the distribution of liposarcoma in the limbs shows that it is more frequent in the lower limb than in the upper limb and more particularly in the thigh (14 cases).
Evolution period and reason for consultation
The duration between the onset of symptoms and the consultation varied between 6 months and 2 years with an average of 16 months. Only 1 patient consulted within 6 months, while the rest of the patients presented to the service after 1 year of evolution or more. The first functional sign found in all the patients was the tumor syndrome. A tumor mass, clinically palpable, was found in our 20 cases, painful in 13 cases, and an alteration in general condition was noted in 4 cases.
Clinical Examination
The clinical examination found a palpable mass of variable sizes, greater than 5 cm , the small size of which was specified as 7 cm, and the large one measured 27 cm in the long axis, of soft consistency in four cases and of firm consistency in 16 cases. In the majority of cases, they are regular, only 2 cases had an irregular mass, mobile in 12 patients, fixed in relation to deep planes in six patients and fixed to the two planes (deep and superficial) in 2 cases with skin ulceration in both, painless in 7 cases. Compression signs such as sciatica were observed in two patients. None of the cases in our series showed lymphadenopathy (Figure 1).
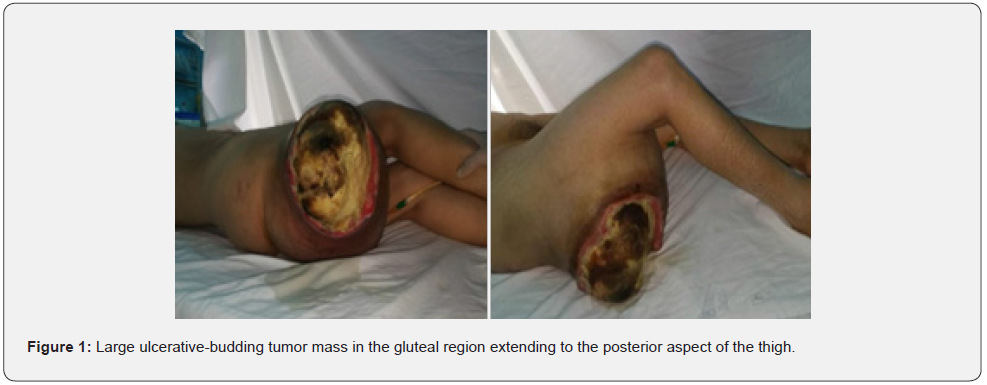
Paraclinical Examinations
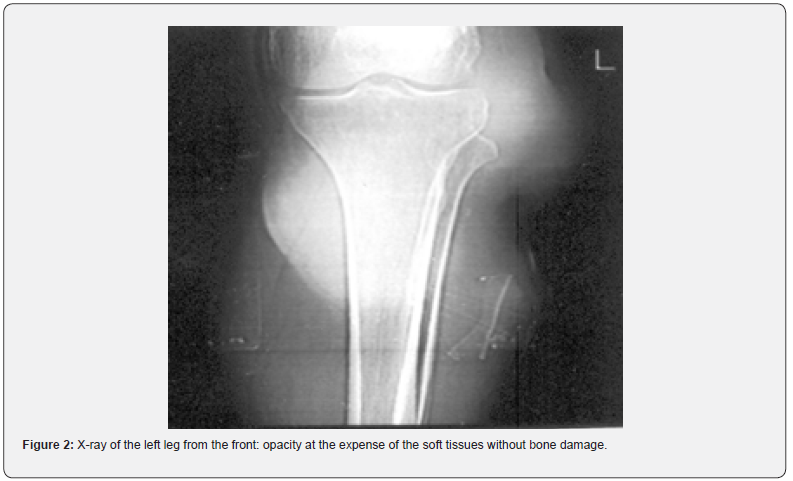
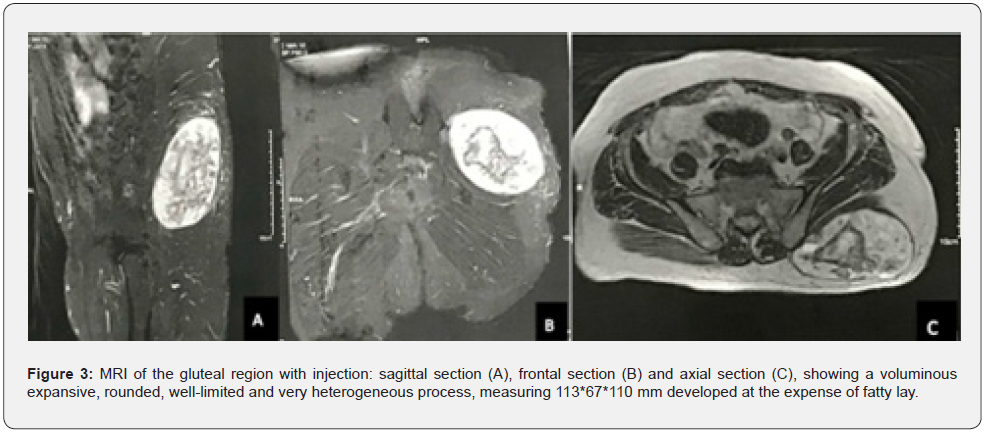
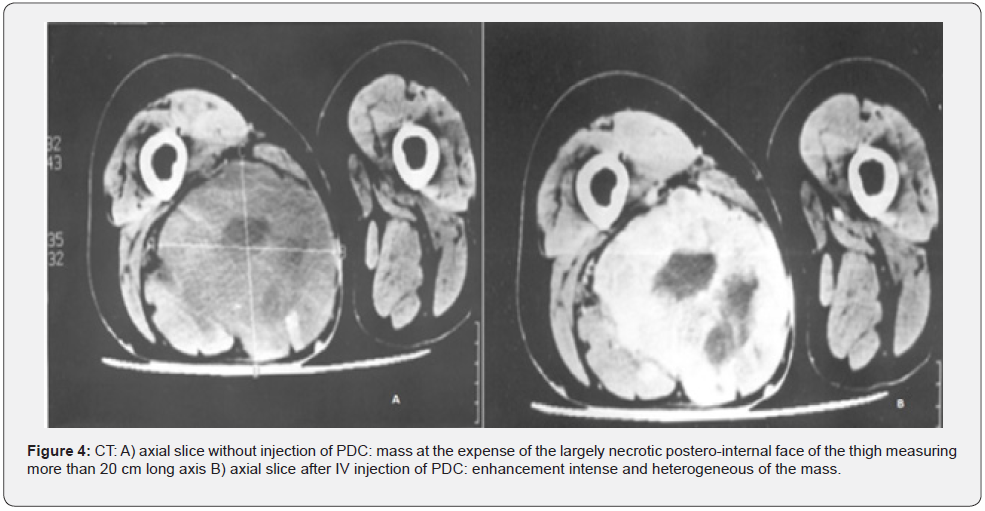
Our series of cases benefited from a well-conducted imaging assessment. Standard radiography was performed in all patients in our series. The majority of radiographs were normal, 5 showed opacity of the soft tissues. (Figure 2). Ultrasound was performed in 10 patients. It allowed to study limits, echostructure, greasy nature, echogenicity, the presence of calcifications and doppler vascularization. All the cases in our series benefited from an MRI (Figure 3), while the CT scan was performed in only one patient (Figure 4). A standard biological assessment was requested in all patients, the biological abnormalities found were Hyperglycemia in a patient, mild anemia in 3 patients, hypercalcemia associated with a decreased parathyroid hormone, probably related to bone damage. It was suppressed during the patient’s hospitalization.
Anatomopathological study
In our study, surgical biopsy was the only examination which led to the diagnosis of certainty of liposarcoma of all our patients; the anatomopathological study of fragments of the biopsy made it possible to show that myxoid liposarcoma was the most common subtype (75%), followed by pleomorphic liposarcoma (15%) then well-differentiated liposarcoma (10%).
12 cases presented an FNCLCC grade II (60%), 5 cases presented a grade III (25%), and 3 cases presented a grade I (15%). An additional immunohistochemical study was carried out in a single patient, whose histological study showed an undifferentiated sarcomatous tumor process, which requires immunohistochemistry to determine the degree of differentiation. The results were: negativity of cytokeratin, desmin, smooth muscle actin, PS100 and CD34, which is in favor of a pleomorphic liposarcoma. The same patient presented a tumor recurrence which was removed for anatomopathological study. The histological study as well as the immunohistochemical study objectified a little differentiated sarcoma which required a molecular biology examination. The study by Fluorescence in situ hybridization (FISH) shows an amplification of the MDM2 gene which is compatible with a liposarcoma.
Assessment of Tumor Extension
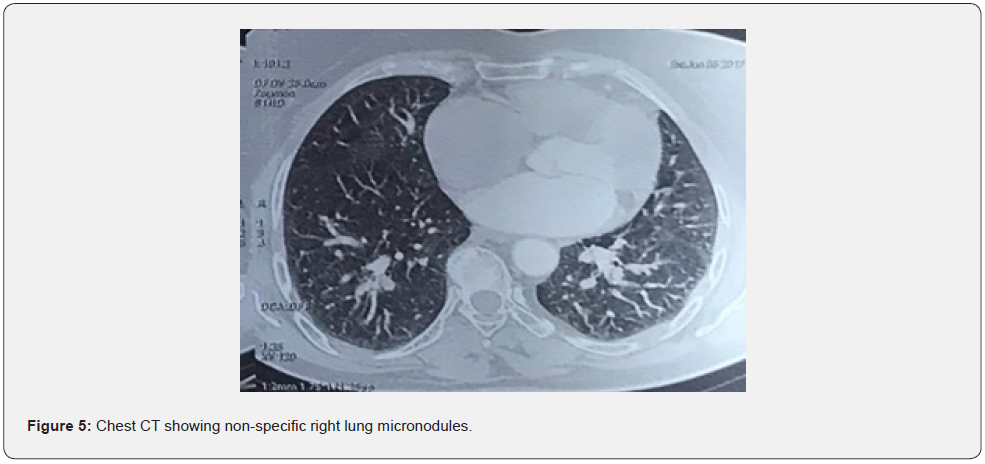
The loco-regional extension was specified by the clinical and paraclinical examination. 2 patients presented with compression of the sciatic nerve, in both cases a myxoid liposarcoma of grade III, one of the gluteal regions and the other of the posterior compartment of the thigh. Metastatic extension was also assessed by clinical and paraclinical examination. A standard chest X-ray was performed in all patients for preoperative assessment. A thoraco-abdomino-pelvic CT scan was requested in 7 patients. In 5 cases, the CT scan was normal. In the other 2, It showed right pulmonary micronodules of non-specific appearance, to be monitored, with no other suspicious lesion detectable (Figure 5). Thus, no metastasis was detected in our case series.
Multidisciplinary Consultation Meeting (MCM)
All cases were presented and discussed in the MCM by a group of specialists including an oncologist, an orthopedic surgeon, a radiologist, and a pathologist. The interest of this meeting was to establish an adequate and adapted care for each patient, including the paraclinical assessment, the tumor biopsy and the therapeutic decision.
Therapeutic Management
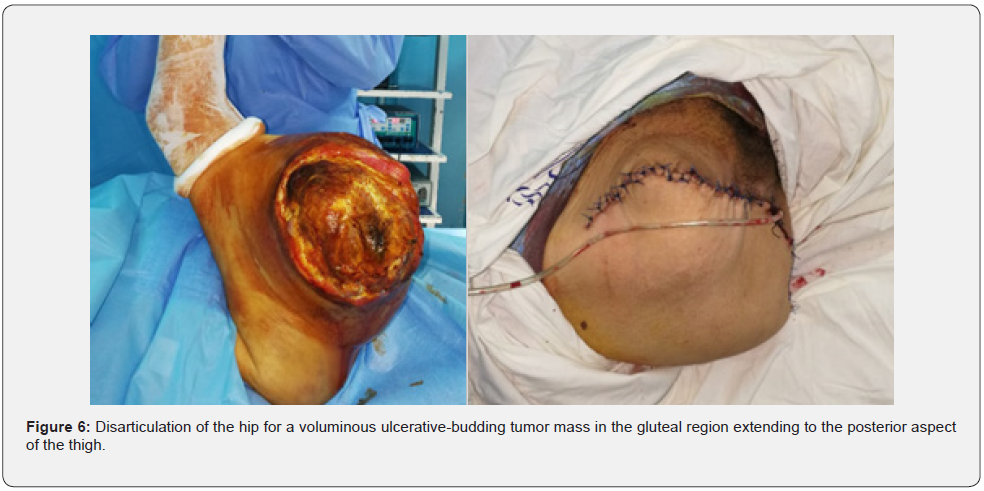
The choice of surgical treatment was based on several elements: the histological type, the grade of the tumor, the location and the general condition of the patient. 19 patients benefited from conservative surgical treatment: it was in 12 cases of a large excision, and in 7 cases of a marginal excision tumor excision, only one patient was treated by radical surgery: disarticulation of the hip (Figure 6). 2 patients were reoperated in our department after a local recurrence (Figure 7).
All patients were operated under general anesthesia. The approach was made directly in the axis of the limb, making it possible to identify the vascular-nervous structures, to remove the biopsy scar and to facilitate surgical revision in the event of recurrence. The surgical specimens were sent for a histological study in order to confirm the diagnosis and to specify whether the excision limits are complete or not. Most cases (90%) had complete excision margins, while in 2 cases they were imprecise. 16 patients were referred to the oncology center of the university hospital center for additional radiotherapy. In our study, the radiation dose delivered was 50- 60GY in five fractions per week of 1.8 to 2GY. The irradiation volume included the operating bed, the scars and the drainage routes. Adjuvant chemotherapy was not indicated in any patient in our series.
Evolution and the main prognostic factors
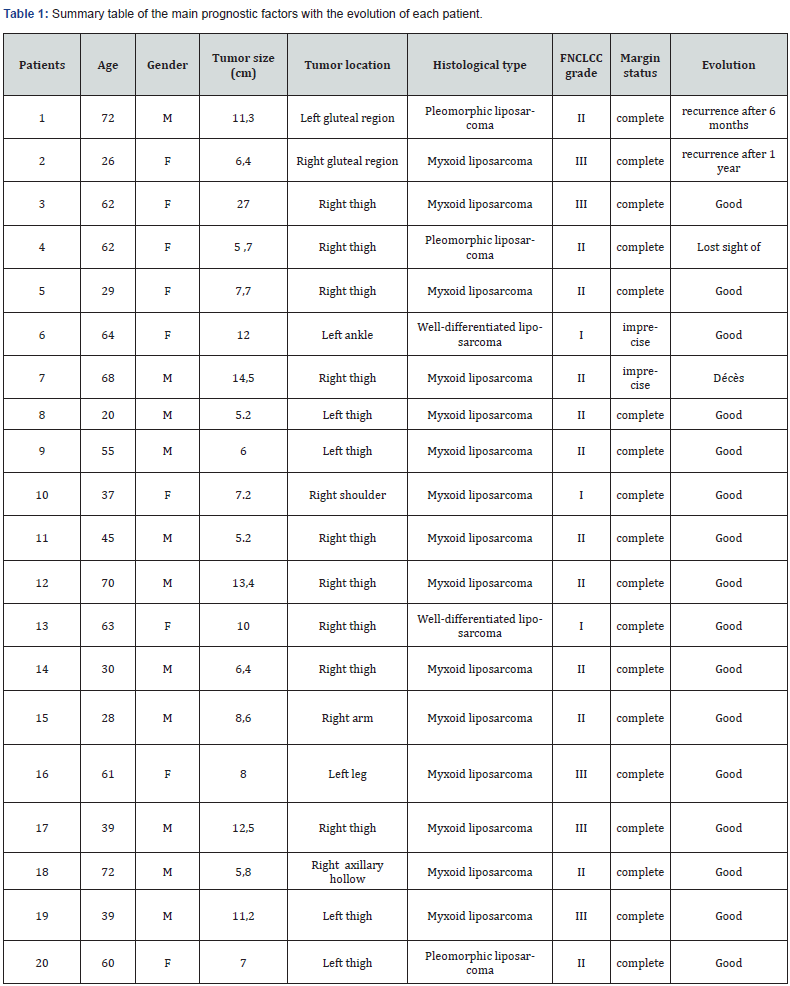
Short term, antibiotic prophylaxis for 48 hours was systematically instituted after surgery in all patients. Only one patient presented an infection of the surgical site after the excision of the tumor recurrence which was large with a significant loss of cutaneous substance. No other patient presented a complication during the postoperative follow-up. Two patients presented with local tumor recurrence, the 2 were repeated and no cases of metastasis were observed. Among the 20 patients in our series, 1 patient died, another was lost to follow-up after surgical revision of the recurrence, while the remaining 18 patients presented a good clinical evolution. Mortality in our series is 12.5%. Our series represents a number of 20 cases of liposarcoma of the limbs including one patient lost sight of what did not allow us no clearing with precision the most impacting prognostic factors, however the table (Table 1) summarizes the evolution in our patients according to the main prognostic factors which are: age, sex, tumor size, histological type, FNCLCC grade, location, and the margin status.
Discussion
Liposarcomas are the most common histological type of soft tissue sarcomas in adults [1]. They present about 15% to 25% of limb sarcomas, yet they remain rare tumors, less than 1% of cancers [2,3]. The annual incidence is estimated at 2.5 per 1 million population [4].
The frequency of the subtypes of liposarcoma varies according to the authors. Well-differentiated and myxoid liposarcomas are by far the most common in the extremities [5]. Myxoid liposarcoma is considered in many studies to be the most frequent liposarcoma of the limbs [6], which is consistent with our results. Liposarcoma is essentially a tumor of adults. The peak incidence varies between 40 and 70 years, with an average age of 55 years. It is exceptional in children [5,7]. The male-female distribution is balanced, a slight male predominance has been reported in some studies [8]. Liposarcomas can develop at any site of the body, the most frequent locations are the extremities (66 to 75% of cases) followed by the retroperitoneum, depending on the histological subtype [2,9]. Localization in the lower limbs is the most frequent according to the authors [10].
The clinic is particularly poor at the time of diagnosis. Liposarcoma of the extremities presents as a deep mass, very often without other symptoms, gradually increasing in size. Other signs develop only when the tumor becomes large enough to exert a mass effect on surrounding structures. These symptoms include pain/sensitivity, oedema, functional impotence or signs related to the compression of the neurovascular bundles (paraesthesia, collateral venous circulation, etc.). The deterioration of the general state can be found at the end of evolution [11]. Several studies find a parallel between the size of the tumor and its malignancy (up to 74% sensitivity of malignancy if the lesion is greater than 5 cm long for De Schepper) [5]. Tung and Davis combined data from three studies and postulated that a diameter less than 3 cm is a reasonable indicator of the benignity of a lesion since this threshold is associated with a positive predictive value of 88%. Conversely, a diameter of 5 cm predicts the malignant nature of a soft tissue mass with a sensitivity of 74%, a specificity of 59% and an accuracy of 66% [12].
Radiological examinations play a key role in the diagnostic and therapeutic assessment, allowing an evaluation of the local and general extension and the search for possible recurrences or metastases [5,13]. MRI is the key examination; it plays an essential role in the exploration of liposarcomas, and it is the examination of choice to distinguish them from other types of soft tissue tumors thanks to the detection of a fatty component. In addition, it brings aspects often very evocative of liposarcoma and allows in some cases to approach the histological subtype. As well as it allows to make the assessment of locoregional extension (bone invasion, soft tissues and vasculonervous reports), essential data for the therapeutic management as well as for the prognosis of these tumours. As well as she keeps interest in the post-therapeutic evolutionary followup [7,14,15].
Functional imaging such as PET scan is beginning to play a more important role as an adjuvant option, it is ideal for the staging of soft tissue malignancies. As well as being useful for evaluating response to treatment and for monitoring residual or recurrent soft tissue masses after treatment [16]. The biopsy is the complementary examination which makes it possible to make the diagnosis and to fix the therapeutic conduct [17]. Surgical biopsy is the reference technique [18]. Two errors must be avoided: taking an insufficient sample, compromising subsequent treatment (hematoma, contamination of healthy tissue) [14,19].
The basic treatment remains carcinological surgery [20,21] supplemented by radiotherapy and possibly by chemotherapy [22]. Given the frequency and apparent oncogenic role of overexpression of MDM2 and CDK4 in well-differentiated and dedifferentiated liposarcoma cases, significant efforts have been made to target these proteins therapeutically. Thus, MDM2 antagonists, CDK4 inhibitors and receptor tyrosine kinase inhibitors have reported promising activity in these subtypes of liposarcomas [23-26]. According to data from the literature, the overall prognosis of liposarcomas depends on the quality of the surgical excision [27], the histological grade [9], the size [4] and the deep location of the tumor [28].
Conclusion
Limb liposarcomas are rare Malignant tumors, although they are the most common subtype of soft tissue sarcomas. This is a histologically and radiologically diverse group of tumors. Its management is multidisciplinary and requires the contribution of an orthopedic surgeon, radiologist, pathologist and oncologist. Imaging (and especially MRI) is an essential element in the diagnostic process, although it does not make it possible to establish the histological diagnosis but directs the diagnosis towards the benign or malignant character, as it is essential to the realization of the extension assessment. The biopsy with the anatomopathological study remains the only confirmatory examination.
The treatment of liposarcomas is essentially based on surgery, which alone can allow excellent control and functionality if it is done in oncological conditions. Surgery is usually combined with radiotherapy to ensure better control, especially in the case of advanced or high-grade tumours. Chemotherapy retains its interest in metastatic tumors. The novelty in the treatment of these tumors is targeted therapy which targets the molecular abnormalities responsible for the tumorigenesis of certain subtypes of liposarcoma. The evolution of liposarcomas is mainly marked by the occurrence of local recurrences and metastases making the prognosis unfavorable. This evolution depends on several factors, in particular: the tumor grade, the quality of the excision, the histological subtype and the location, which must be taken into consideration during management.
Conflict of Interest
All authors have no conflicts of interest to declare.
References
- Terrier P (2012) Les liposarcomes. Annales de Pathologie 32(5): S108‑S
- De Vita A, Mercatali L, Recine F, Pieri F, Riva N, et al. (2016) Current classification, treatment options, and new perspectives in the management of adipocytic sarcomas. Onco Targets Ther 9: 6233‑6246.
- Goldblum JR, Folpe AL, Weiss SW (2019) Enzinger & weiss’s soft tissue tumors. 7th é Elsevier, Philadelphia, USA.
- Henze J, Bauer S (2013) Liposarcomas. Hematol Oncol Clin North Am 27(5): 939‑955.
- Fuchs A, Henrot P, Walter F, Iochum S, Vignaud J, et al. (2002) Tumeurs graisseuses des parties molles des membres et des ceintures de l’adulte. J Radiol J Radiol. 1 janv 8383: 1035‑571035.
- Muratori F, Frenos F, Bettini L, Matera D, Mondanelli N, et al. (2018) Liposarcoma: Clinico-pathological analysis, prognostic factors and survival in a series of 307 patients treated at a single institution. J Orthop Sci 23(6): 1038‑1044.
- El Ouni Salhi F, Jemni H, Trabelsi A, Ben Maitig M, Arifa N, et al. (2010) Liposarcomes des membres : caractéristiques présentes en IRM et leur corrélation avec l’histopathologie. Revue de Chirurgie Orthopédique et Traumatologique 96(8): 970‑977.
- Pearlstone DB, Pisters PW, Bold RJ, Feig BW, Hunt KK, et al. (1999) Patterns of recurrence in extremity liposarcoma: implications for staging and follow-up. 1 janv 85(1): 85‑92.
- Terrier P (2012) Les liposarcomes. Annales de Pathologie. nov 32(5): S108‑S110.
- Soulie D, Boyer B (1995) Coll Liposarcome myxoïde, aspect en IRM. J radiol 1995: 29-36.
- Zafar R, Wheeler Y (2022) Liposarcoma. In: StatPearls. Treasure Island (FL): StatPearls Publishing; mai.
- De Schepper AM, De Beuckeleer L, Vandevenne J, Somville J (2000) Magnetic resonance imaging of soft tissue tumors. Eur Radiol 10(2): 213‑223.
- Murphey MD, Arcara LK, Fanburg-Smith J (2005) Imaging of Musculoskeletal Liposarcoma with Radiologic-Pathologic Correlation. RadioGraphics 25(5): 1371‑1395.
- Taieb S, Ceugnart L, Gauthier H, Penel N, Vanseymortier L (2006) Sarcomes des tissus mous des extrémité Rôle de l’imagerie dans la prise en charge initiale. Cancer/Radiothérapie. 1 févr 10(1): 22‑33.
- Teniola O, Wang KY, Wang WL, Tseng WW, Amini B (2018) Imaging of liposarcomas for clinicians: Characteristic features and differential considerations. J Surg Oncol. mai 117(6): 1195‑1203.
- Kubo T, Furuta T, Johan MP, Ochi M (2016) Prognostic significance of (18)F-FDG PET at diagnosis in patients with soft tissue sarcoma and bone sarcoma; systematic review and meta-analysis. Eur J Cancer 58: 104-111.
- World Health Organization (2013) International Agency for Resarch on Cancer, WHO classification of tumors of soft tissue and bone, 4th IARC Press, Lyon, France.
- Fekkar A, Mc Leer A, Chapuis P, Brichon PY, Chirica M, et al. (2021) Liposarcomes primitifs du tube digestif : diversité des présentations clinicopathologiques et challenges diagnostiques. Annales de Pathologie 1 juill 41(4): 399‑404.
- Stoeckle E, Michot A, Henriques B, Sargos P, Honore C, Ferron G, et al. (2016) Chirurgie des sarcomes des tissus mous des membres et de la paroi du tronc. Cancer/Radiotherapie 20(6): 657‑665.
- Brady MS, Gaynor JJ, Brennan MF (1992) Radiation-associated sarcoma of bone and soft tissue. Arch Surg 127(12): 1379‑1385.
- Robinson E, Neugut AI, Wylie P (1988) Clinical aspects of postirradiation sarcomas. J Natl Cancer Inst. 20 avr 80(4): 233‑240.
- Mssrouri, S Benamr, A Essadel, J Mdaghri, E H Mohammadine, et al. (2006) Liposarcome cervico-médiastinal 1122(5).
- Müller CR, Paulsen EB, Noordhuis P, Pedeutour F, Saeter G, et al. (2007) Potential for treatment of liposarcomas with the MDM2 antagonist Nutlin-3A. Int J Cancer 121(1): 199‑205.
- Singer S, Socci ND, Ambrosini G, Sambol E, Decarolis P, et al. (2007) Gene expression profiling of liposarcoma identifies distinct biological types/subtypes and potential therapeutic targets in well-differentiated and dedifferentiated liposarcoma. Cancer Res 67(14): 6626‑636.
- Dickson MA, Schwartz GK, Keohan ML, D’Angelo SP, Gounder MM, et al. (2016) Progression-Free Survival Among Patients with Well-Differentiated or Dedifferentiated Liposarcoma Treated with CDK4 Inhibitor Palbociclib: A Phase 2 Clinical Trial. JAMA Oncol 2(7): 937‑940.
- Shor AC, Agresta SV, D’Amato GZ, Sondak VK (2008) Therapeutic potential of directed tyrosine kinase inhibitor therapy in sarcomas. Cancer Control. janv 15(1): 47‑54.
- Skubitz KM, Cheng EY, Clohisy DR, Thompson RC, Skubitz APN (2005) Differential gene expression in liposarcoma, lipoma, and adipose tissue. Cancer Invest 23(2): 105‑118.
- Honoré C, Méeus P, Stoeckle E, Bonvalot S (2015) Soft tissue sarcoma in France in 2015: Epidemiology, classification and organization of clinical care. J Visc Surg 152(4): 223‑230.






























