Unicameral Bone Cyst in Unusual Location - Report of a Case
Sergio Morales Pineiro1, Roberto Mara Cuevas1, Claribel Plain Pazos2*, Leonardo Dominguez Plain3, Luis Crescencio Breton Espinosa4 and Lazaro Martin Martinez Estupinan5
1I and II Degree Specialist in Orthopedics and Traumatology, Assistant Professor, Provincial General University Hospital, Cuba
2I and II Degree Specialist in Comprehensive General Medicine, Faculty of Medical Sciences of Sagua la Grande, Cuba
3Resident of 3rd year of Orthopedics and Traumatology, Provincial General University Hospital, Cuba
4I Degree Specialist in Orthopedics and Traumatology, Assistant Professor, Provincial General University Hospital, Cuba
5Doctor in Medical Sciences, II Degree Specialist in Orthopedics and Traumatology, Full Professor, Provincial General University Hospital, Cuba
Submission: February 10, 2022; Published: February 25, 2022
*Corresponding author: Claribel Plain Pazos, Faculty of Medical Sciences of Sagua la Grande, Villa Clara, Cuba
How to cite this article: Sergio M P, Roberto M C, Claribel P P, Leonardo D P, Luis C B E, et al. Unicameral Bone Cyst in Unusual Location - Report of a Case. Ortho & Rheum Open Access J. 2022; 19(5): 556023. DOI: 10.19080/OROAJ.2022.19.556023
Abstract
Introduction: The unicameral bone cyst is an infrequent benign bone tumor, located preferentially in the metaphyseal-diaphyseal portion of the bones and present in the first decades of life
Objective:To present a patient who was diagnosed with a unicameral bone cyst in an unusual location.
Case presentation: 23-year-old male patient, mixed race, university athlete, who came to the consultation for pain in the right ankle after having practiced sports. The CT scan detected an osteolytic image at the level of the body of the talus towards the peroneal malleolus that did not break the cortex. A modified Gatellier and Chastang posterolateral surgical approach is used, a bone window is opened in the peroneal aspect of the talus, proceeding to curettage of the cyst walls, filling with a cancellous iliac bone graft, the extracted material was sent to the Department of Pathology, obtaining the diagnosis of Unicameral Bone Cyst. (QOU).
Conclusion: The patient evolved satisfactorily incorporating the graft in its entirety and returned to his daily activities after 9 months.
Keywords: Unicameral bone cyst of the talus; Treatment
Introduction
The Unicameral Bone Cyst (UOC) is a benign bone tumor, rare, located preferentially in the metaphyseal-diaphyseal region of the long bones that occurs mainly in childhood, 95% of diagnosed cases occur in the first two decades of life with a 2.5: 1 ratio in favor of the male sex [1,2]. The management of these benign bone tumors is varied, it differs according to the size and its behavior among the treatment variants include periodic observation of the lesion without intervention, decompression of the cyst with cannulated screws or drains, intralesional injection with steroids, curettage of the cyst plus adjuvant therapy, curettage of the cyst with or without open or arthroscopic bone graft, and finally, wide resection that may be necessary in aggressive lesions. All these forms of treatment focus on alleviating pain, promoting cure, and preventing adverse complications such as recurrence and pathological fractures [3,4]. Due to the infrequency of this tumor, the authors of this study aim to present a patient with UOC whose main characteristic is its atypical location as well as the treatment carried out for the solution.
Patient Presentation
A 23-year-old male patient, mixed race, university athlete, practitioner of the 110-meter hurdles modality, who attended the Orthopedic consultation due to pain in the right ankle that began after training carried out as planned.
Physical exam
Normolinean patient Weight: 75 Kg Height: 1.80 cm Pain on flexion-extension, inversion and eversion movements of the right ankle, according to the Visual Analogue Scale (VAS= 2), no crepitus, discoloration or increased volume. When the foot is supported on the lower right limb, the pain increases to one (VAS= 5)
Complementary:
Hb: 14.4 g / l
Hematocrit: 0.48 vol%
Glycemia: 4.5 mmol / l
Creatinine: 89 μmol / l
Erythrosedimentation: 25 mm / h
Alkaline phosphatase: 182 umol / l
Blood group and factor: A +
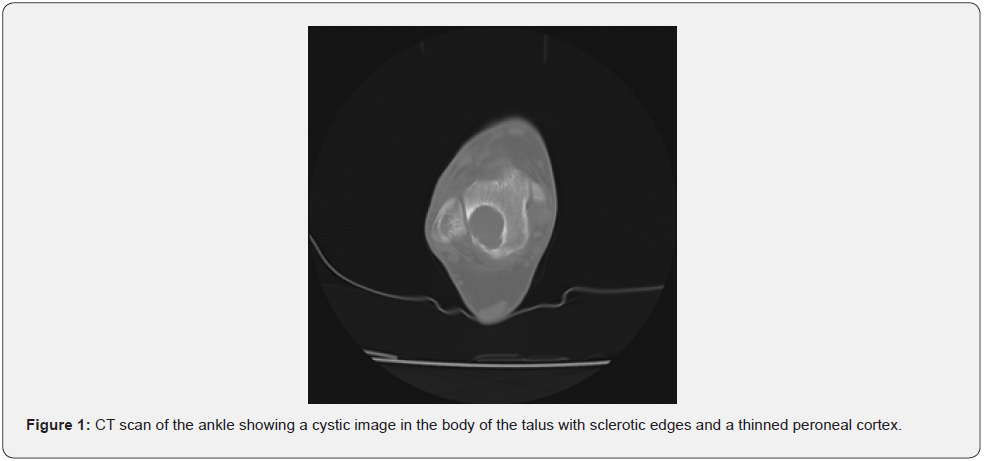
Ankle CT: (Figure 1) It is observed in the body of the talus towards the peroneal side, a well-defined cystic image, eccentric with sclerotic edges with the external cortex very thin but without rupture, measuring 18 X 11 mm. Bony trabeculae are not observed inside.
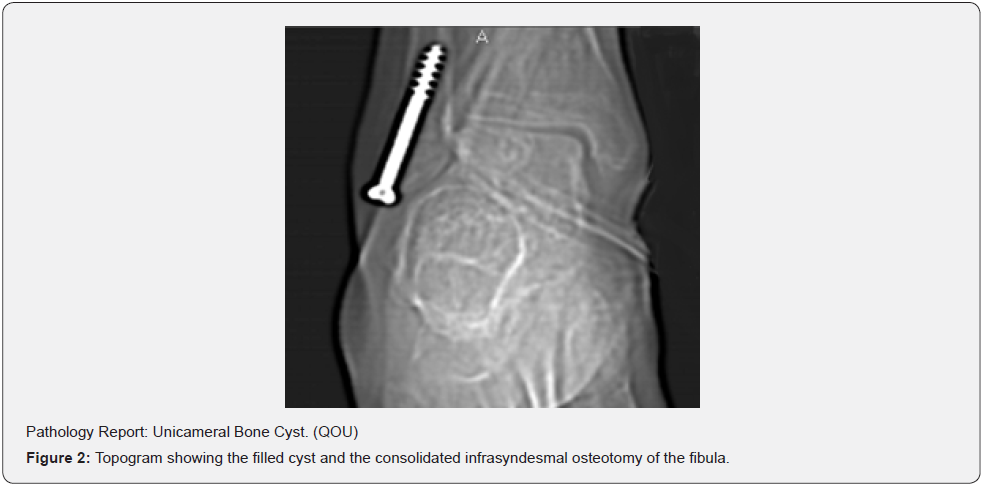
Surgical technique After spinal anesthesia, an ischemic cuff is placed on the thigh, asepsis and antisepsis are performed with Betadine®, field cloths are placed, the skin is incised on the external side of the ankle on the fibula approximately five centimeters long according to Gatellier. y. Chastang [5,6] is decolated by planes exposing the fibula in the distal six centimeters, an infrasyndesmal osteotomy is made, immediately below the tibiofibular syndesmosis and not at 10 centimeters as described by the original technique, the fibula is folded downwards using as it hinges the peroneal talus and peroneal calcaneus ligaments, perfectly exposing the peroneal side of the body of the talus. A periosteal window of approximately one centimeter in diameter is made, evacuating the fluid included in the cyst, proceeding to curettage of the walls from which a sample is taken for biopsy, which is done until the sclerosis of the walls is eliminated, then small perforations in the cavity wall with a two-millimeter Kirchner wire to promote bleeding. A cancellous bone graft is obtained from the ilium by filling the cavity, closing the window, the fibula is replaced, fixing it with a 70 mm long cancellous AO screw (Figure 2). Haemostasis is performed, closure by planes and a plaster boot is placed for six weeks, the cast is removed, and ankle rehabilitation begins without weight bearing for another six weeks. With the evidence of the filling of the cyst (Figure 2), progressive partial support is started subject to the presence or absence of pain. The patient is discharged from the clinic at nine months, not allowing him to practice sports until one year after the operation.
Discussion
The location of the UOC in this patient is very infrequent since the preferential location of these is the metaphyseal-epiphyseal region of the long bones [1,7]. In this case it could be caused because of osteochondral lesions of the body of the talus in embryonic or early stage of life that developed a valve mechanism in the damaged cartilage creating a unidirectional flow of synovial fluid from the joint space through the cartilage towards the bone. subchondral exerting a high intracystic pressure that causes the death of osteocytes, thus favoring the growth of the cyst [8,9].
From the above we can deduce that the cyst already existed long before and that the contingencies to which the talus was subjected in daily life and the rigorous sports training were the conditions for the pain to begin.
Once the surgical treatment was decided as a solution to the problem, a postero-external route was used to approach the talus, initially described in 1924 by Gatellier and Chastang [5] and masterfully by Campbell’s [6] to which a modification was made consisting of making the smallest skin incision (five centimeters) and the infrasyndesmal fibula osteotomy and not 10 centimeters or through the fracture as described by the original technique that was otherwise originally described to repair fracture injuries of the tibial pilon and not for injuries of the talus, thus avoiding injuring the tibiofibular syndesmosis and having to close it with another screw.
Currently, the forms of treatment for these lesions are varied, from simple observation to the injection of autologous bone marrow under radiological vision, through decompression and the performance of curettage and bone grafting [3,4,10]. Although bone marrow injection turns out to be the treatment with the best results, it depends on the site of the injury, the size and the bone affected [10]. In our case, an open curettage and autologous bone graft was performed because it is a difficult access site and there are no other possibilities such as performing the procedure with arthroscopic assistance [1].
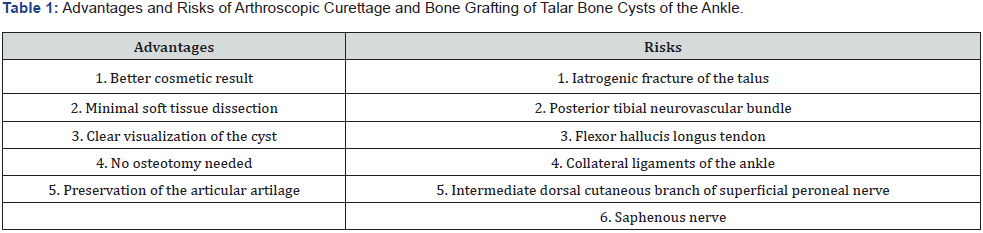
At present, the arthroscopic approach to these injuries is gaining momentum [9-14], a procedure that requires a long learning curve that, although it has advantages, is not without risks [9] as observed in (Table 1). When the filling and bone integration of the graft were certain, progressive partial support was started and sports practice was not authorized until the year after the surgical intervention, thus avoiding the collapse of the body of the talus and the subsequent establishment of osteoarthritis of the tibiotalar joint.
Conclusion
The presentation of UOC in the talus is very infrequent and the surgical solution given to this patient turned out to be satisfactory.
References
- Stoica IC, Pop DM, Grosu F (2017) Unicameral bone cyst of the calcaneus – minimally invasive endoscopic surgical treatment. Case report Rom J Morphol Embryol 58(2): 689–693.
- Kapoor C, Shah M, Soni R, Patwa J, Merh A, et al. (2017) Aneurysmal bone cyst of the proximal femur and its management. A case report. Cureus 9(1): e991.
- Farouk HA, Saladin M, Senna WA, Ebeid W (2018) All-endoscopic management of benign bone lesions; a case series of 26 cases with minimum of 2 years follow-up. SICOT J 4: 50.
- Noordin S, Allana S, Umer M, Jamil M, Hilal K, et al. (2018) Unicameral bone cysts: Current concepts. Ann Med Surg (Lond) 34: 43–49.
- Gatellier J, Chastang L (1924) Access to fractured malleolus with piece chipped off at back. J Chir 24: 513.
- Crenshaw AH (2012) Surgical Techniques and Approaches. En: Canale ST, Beaty JH, editors. Campbell's. Operative Orthopaedics. Elseiver, Phyladelphia, Mosby, USA, p. 3- 125.
- Boude AB, Vasquez LG, Alvarado-Gomez F, Bedoya MC, Rodriguez-Munera A, et al. (2017) A simple bone cyst in cervical vertebrae of an adolescent patient. Case Rep Orthop 2017: 8908216.
- Van Dijk CN, Reilingh ML, Zengerink M, van Bergen C J A (2010) Osteochondral defects in the ankle: Why painful? Knee Surg Sports Traumatol Arthrosc 18(5): 570–580.
- Lui TH (2017) Arthroscopic Curettage and Bone Grafting of Bone Cysts of the Talar Body. Arthrosc Tech 6(1): e7–e13.
- Lee SY, Chung CY, Lee KM, Sung KH, Won SH, et al. (2014) Determining the Best Treatment for Simple Bone Cyst: A Decision Analysis. Clin Orthop Surg 6(1): 62–71.
- Baliga S, Basu Mallick MN, Shrivastava C (2019) Cartilage-sparing Arthroscopic Technique for Curettage and Bone Grafting of Cystic Lesion of Talus –A Case Report. J Orthop Case Rep 9(1): 102–105.
- Zhu X, Yang L, Duan X (2019) Arthroscopically Assisted Anterior Treatment of Symptomatic Large Talar Bone Cyst. J Foot Ankle Surg 58(1): 151–155.
- Baliga S, Mallick MNB, Shrivastava C (2019) Cartilage- sparing arthroscopic technique for curettage and bone grafting of cystic lesion os talus. A case report. J Orthop Case Rep 9(1): 102-105.
- Lui T H (2013) Arthroscopic bone grafting of talar bone cyst using posterior ankle arthroscopy. J Foot Ankle Surg 52: 529–532.






























